Abstract
The aim of this study was to clarify the association of clinical characteristics of unexplained syncope with the outcome of the head-up tilt test (HUT) in children. A total of 47 patients with unexplained syncope were classified into two groups according to their outcomes of HUT: the positive response group and the negative response group. We reviewed their clinical data as well as the results of HUT and analyzed them with logistic regression method. The results showed that the incidence of positive responses to HUT was higher in girls than in boys (8/22 vs 10/7, p < 0.05). Compared with fainted children younger than 12 years of age, 12- to 16-year-old adolescents with unexplained syncope had a high positive outcome of HUT (30 vs 72.9%, p < 0.05). Compared with fainted children with negative response of HUT, children with positive response to HUT often had syncope in special circumstances (e.g., prolonged standing, anxiety and fright, and morning exercise), and they often had prodrome, such as pallor, lightheadedness, and nausea (28/30 vs 8/17, p < 0.05). However, the number and duration of syncopal spells did not relate to the positive responses to HUT. The logistic regression analysis showed that three factors significantly influenced the outcome of HUT: predisposing factors of syncope, prodrome of syncope, and age (p < 0.05; OR = 32.9434, 17.7281, and 2.7842, respectively). Hence, if pubertal girls with unexplained syncope had clear predisposing factors and prodromes, they were likely to have positive responses to HUT, and they were likely to be clinically considered as having vasovagal syncope.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Syncope is one of the most common problems in clinical pediatrics. Its reported incidence is variable. Some investigators have indicated that as many as half of young adults recalled at least one episode in their past, whereas the incidence of those seeking medical attention was approximately 126 per 100,000 [2]. Vasovagal reflex has been identified as the most common cause of unexplained syncope [9]. The head-up tilt test (HUT) has been used in the diagnosis of patients of both sexes, all ages, and with a very wide range of severity [3, 4]. The number of syncopal spells varies from one to thousands, and the duration of the history of syncope varies from days to decades. However, whether there are any relations between the clinical characteristics and the outcome of HUT remains unclear. We therefore prospectively studied 47 children with unexplained syncope undergoing standardized passive tilt test to determine whether the age and sex of the patients and the number, duration, and frequency of syncopcal spells could predict HUT outcome.
Materials and Methods
Patients
The records of all patients referred for evaluation of syncope who underwent HUT at the Department of Pediatrics, the First Hospital of Peking University between January 1995 and December 2000 were retrospectively reviewed. All syncopal patients had normal findings on evaluation, which consisted of a complete medical history, physical examination, orthostatic blood pressure determination, complete blood cell count, urinalysis, measurement of blood electrolyte and glucose, 12-lead electrocardiogram (ECG), echocardiography, thoracic X-ray, electroencephalogram, and cranial computed tomography (CT) scan. The patients were classified into two groups according to their outcomes of HUT: the positive response group and the negative response group.
Head-Up Tilt Test
Informed parental consent was obtained for each patient. All patients were asked to stop the administration of drugs that could affect the automatic nerve function for at least 3 days and to fast for 12 hours before the tilt test. The tilt test was preceded by 5 minutes of observation in a supine position, and blood pressure, heart rate, and ECG were recorded before the tilt test. A 60° tilt was used for subjects until the positive reaction occurred or for 45 minutes. Blood pressure, heart rate, and 12-lead ECG were monitored continuously when patients felt uncomfortable during the test. Children were placed in a supine position as soon as the positive response occurred. First-aid drugs were available at all times.
Estimation of Positive Response
Either syncope or severe presyncope occurring during the tilt test associated with at least one of the following symptoms was considered a positive response:
-
1
Systolic blood pressure <80 mmHg or a decrease >15 mmHg and/or diastolic blood pressure <50 mmHg
-
2
Bradycardia [heart rate <75 beats per minute (bpm) for 4- to 6-year-old children, <65 bpm for 7- or 8-year-old children, <60 bpm for 8-year-old or older children] or sinus arrest >3 seconds
-
3
Second-degree or higher atrioventricular block
-
4
Atrioventricular junctional rhythm, including escape rhythm and accelerated idiorhythm
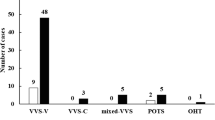
Presyncope was the state of lightheadedness associated with at least one of the following symptoms: decreased vision or audition, nausea, vomiting, heavy sweating, and unsteady steps. There were three patterns of positive response according to the changes in blood pressure and heart rate: (1) the cardioinhibitory pattern, which was characterized by a rapid decrease in heart rate, presenting as bradycardia; (2) the vasodepressor pattern, with a rapid decrease in blood pressure; and (3) the mixed pattern, in which both blood pressure and heart rate decreased during the tilting [7].
Statistical Analysis
Differences for continuous variables between normally distributed groups were examined for statistical significance with a two-sample t-test and with the Mann–Whitney U-test for nonparametrically distributed values. Analysis was then performed and the validity of conclusions independently confirmed with logistic regression analysis. Fisher’s exact test was used for contingency tables and the chi-square was used for larger tables. The statistical ability of variables to predict HUT outcome was determined with logistic regression analysis.
Results
Forty-seven patients were reviewed. The average age was 11.1 ± 2.2 years (range, 5–16 years). There were 18 males and 29 females. The positive response group included 30 patients, of whom 8 were male and 22 were female; the negative response group included 17 patients, of whom 10 were male and 7 were female. Females dominated those with a positive HUT outcome (p = 0.029). Children who had a positive response to HUT often did so in special circumstances, such as prolonged standing, anxiety and fright, and emotional stress (p = 0.004). They often had prodrome such as pallor, lightheadedness, and nausea (p = 0.001), but the frequency of syncopal spells and duration of attacks of syncope did not influence the HUT outcome. There was no significant difference in baseline supine heart rates and blood pressure between patients with positive and those with negative tilt tests (Table 1). For each of the prespecified variables, patients were allocated into near quintiles, and the effects of the variables on HUT outcome were determined by categorical analyses. There were no significant effects of any of the measures of estimation of severity on HUT outcome, but the ages of subjects significantly influenced HUT outcome (p = 0.032). Twelve- to 16-year-old adolescents with unexplained syncope had higher positive outcome with HUT than those younger than 12 years old (Tables 2,3,4). In logistic regression analysis, three factors significantly influenced the outcome of HUT: predisposing factors, prodrome of syncope, and age (p < 0.05; OR = 32.9434, 17.7281, and 2.7842, respectively) (Table 5).
Discussion
Syncope is a common clinical problem caused by a wide variety of diseases. In some cases, syncope that reoccurs frequently, with normal findings on routine examination of cardiac and central nervous systems, is considered an unexplained syncope. The most common pattern of unexplained syncope in children is vasovagal syncope [2]. Since HUT was introduced to diagnose unexplained syncope in children, it has been regarded as one of the important diagnostic criteria. We analyzed the data on unexplained syncopcal children in recent years to determine the influential factors on HUT. The results of the study showed that the likelihood of a positive response to HUT was markedly higher in pubertal girls than in boys, and that conventional measures of estimation of severity did not influence HUT outcome. Furthermore, children with a positive response to HUT were likely to have clear predisposing factors and prodromes compared with negative responders.
Association of Age and Sex with HUT Outcome
According to our study, age exhibited effects on the response to HUT in patients with syncope. In this study, we found that the positive rates of HUT at the age of 11–16 years and <11 years were 72.9 and 30.0%, respectively. The difference was statistically significant. These results are similar to those of Sheldon’s studies, who found that all patients aged 12–20 years old had positive responses, whereas only 61% of patients aged 61–88 years had positive responses [11]. This was also consistent with the report from Driscoll and colleagues [2], which found that the peak age range for syncope was 15–19 years. Our data showed that sex also affected the responses in children with syncope undergoing HUT. Female patients were more likely to have a positive outcome than male patients. In our study, the positive response group consisted of 30 patients, of whom 22 were female, whereas the negative response group consisted of 17 patients, of whom only 7 were female. The findings are in accordance with those of Driscoll et al.’s [2] study, in which the incidence of positive response in HUT was higher in girls than in boys. According to our study, pubertal girls with unexplained syncope had a trend to positive response to HUT. In previous studies, it was found that age could alter autonomic tone [6, 12]. Therefore, we postulated that the autonomic nervous system in pubertal girls often had inadequate sympathovagal balance.
Predisposing Factors of Syncope and HUT Outcome
Predisposing factors also had an influence on the outcome of HUT. In our study, more than 90% of children with syncope had predisposing factors before syncope in the positive response group; However, in the negative group only 52% of patients had predisposing factors before syncope. Using regression analysis, it was found that predisposing factors significantly influenced the outcome of HUT. In patients with predisposing factors, the OR was 32.943, suggesting that the possibility of positive response of HUT in patients with predisposing factors was 32.6434 times higher than that of those who did not have predisposing factors. Predisposing factors before syncope in the positive response group consisted of the following conditions: suddenly getting up in the morning, prolonged standing, or emotional stress. This accorded with the pathophysiology of vasovagal syncope (VVS). In general, VVS resulted from inappropriate output from the autonomic nervous system leading to symptomatic change in blood pressure and heart rate. This typically occurs while patients are standing. This response appears to be triggered by vigorous contractions of an underfilled ventricle due to pooling of blood in the lower part of the body that stimulates ventricular mechanoreceptor, as might normally occur with systemic hypotension. The result is a surge in afferent neural traffic that triggers a central reflex to cause abrupt inhibition of peripheral sympathetic tone, resulting in hypotension and bradycardia. This is also called the Bezold–Jarish reflex [1]. When patients get up in the morning or stand for long periods of time, there is venous pooling in the lower extremities, which decreases left ventricular filling, and further syncope may develop.
Prodrome of Syncope and HUT Outcome
In our study, prodrome of syncope also affected the outcome of HUT. In the positive response group, 90.3% of patients had prodrome of syncope. Using regression analysis, it was determined that patients with prodrome of syncope had an OR of 17.7281, indicating that the possibility of a positive response of HUT these patients was 17.7281 higher than that of those without prodrom of syncope. Richard and Daniel [8] found that for most children with syncopal spells, if they had prodrome of syncope, especially dizziness, nausea, perspiration, etc., with normal findings on routine examination of cardiac and central nervous systems, they could be empirically diagnosed with VVS. Our data showed that many patients with a positive response to HUT experienced dizziness, pallor, nausea, flashing lights, and perspiration before the syncopal event.
Estimation of Severity and HUT Outcome
HUT outcome did not reflect the clinical burden of syncope. The estimation of syncope frequency and duration of syncopal spells could predict clinical the course of illness, correlate with reductions in quality of life, and determine which patients should be treated [10, 13]. We postulated that patients with a worse clinical history are more likely to faint during tilt testing, but the findings of our study did not support this hypothesis. Therefore, HUT may indicate whether patients have VVS, but it did not reflect the severity of the disorder in VVS patients. This finding was consistent with Levine’s [5] study, He found that patients with a history consistent with VVS had comparable outcomes regardless of the results of HUT. Hence HUT is only a method of diagnosis; it cannot be used to determine whether patients should be treated.
Conclusion
According to our study, patients with VVS can be identified with a careful history and HUT. If pubertal girls with unexplained syncope had clear predisposing factors and prodromes, they were likely to have positive responses to HUT, and they could be clinically considered as having VVS.
References
P Blair MD Grubb (1999) ArticleTitlePathophysiology and differential diagnosis of neurocardiogenic syncope. Am J Cardiol 84 3Q–9Q Occurrence Handle10568555
DJ Driscoll SJ Jacobsen CJ Porter PC Wollan (1997) ArticleTitleSyncope in children and adolescents. J Am Coll Cardiol 29 1039–1045 Occurrence Handle10.1016/S0735-1097(97)00020-X Occurrence Handle1:STN:280:ByiB2cvkt1U%3D Occurrence Handle9120157
CL Johnsrude (2000) ArticleTitleCurrent approach to pediatric syncope. Pediatr Cardiol 21 522–531 Occurrence Handle10.1007/s002460010130 Occurrence Handle1:STN:280:DC%2BD3M%2Fltl2rtA%3D%3D Occurrence Handle11050276
D Junbao M Zhao L Wanzhen et al. (1999) ArticleTitleA study on head-up tilt test for the diagnosis of unexplained syncope in children. Cardiovasc Eng 4 8–10
MM Levine (1999) ArticleTitleNeurally mediated syncope in children: results of tilt testing, treatment, and long-term follow-up. Pediatr Cardiol 20 331–335 Occurrence Handle10.1007/s002469900479 Occurrence Handle1:STN:280:DyaK1MzntlCisA%3D%3D Occurrence Handle10441686
LA Lipsiz J Mietus GB Moody AL Goldberger (1990) ArticleTitleSpectral characteristics of heart rate variability before and during postural tilt: relations to aging and risk of syncope. Circulation 81 1830–1810
G Muller BJ Deal JF Strasburger DW Benson Jr (1993) ArticleTitleUsefulness of metoprolol for unexplained syncope and positive response to tilt testing in young persons. Am J Cardiol 71 592–595 Occurrence Handle10.1016/0002-9149(93)90517-G Occurrence Handle1:STN:280:ByyC2srjsVE%3D Occurrence Handle8438747
S Richard M Daniel (1999) ArticleTitleIndication, methodology, and classification of results of tilt-table testing. Am J Cardiol 84 10Q–16Q Occurrence Handle10.1016/S0002-9149(99)00692-X Occurrence Handle10568556
JK Ronald (1999) syncope. P Gillette A Garson (Eds) Clinical Pediatric Arrthythmias, 2nd edn. Saunders Philadelphia 251–286
S Rose ML Koshman R McDonald et al. (1996) ArticleTitleHealth-related quality of life in patients with neuromediated syncope. Can J Cardiol 12 131–138
RS Sheldon (1994) ArticleTitleEffects of aging on response to isoprotenol tilt-table testing in patients with syncope. J Am Coll Cardiol 19 773–779
R Sheldon (1994) ArticleTitleEffects of aging on responses to isoprotenol tilt-table testing in patients with syncope. Am J Cardiol 7 459–463 Occurrence Handle10.1016/0002-9149(94)90903-2
R Sheldon S Rose P Flanagan ML Koshman S Killam (1996) ArticleTitleRisk factors for syncope recurrent after a positive tilt table test in patients with syncope. Circulation 93 973–981 Occurrence Handle1:STN:280:BymC2sbgt1w%3D Occurrence Handle8598089
Acknowledgements
This work was supported by Capital Medical Development Foundation of China Grant 2001-3037.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Qingyou, Z., Junbao, D., Jianjun, C. et al. Association of Clinical Characteristics of Unexplained Syncope with the Outcome of Head-Up Tilt Tests in Children. Pediatr Cardiol 25, 360–364 (2004). https://doi.org/10.1007/s00246-003-0513-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-003-0513-4