Abstract
Introduction
Even low-grade astrocytomas infiltrate the entire brain, a feature that precludes their successful therapy. So to assess the invasive potential of astrocytoma is very important. The aim of this study was determine whether there is a significant correlation between the results of 1H-magnetic resonance spectroscopy (1H-MRS) and tumor invasive potential of astrocytoma, which is reflected by expression of matrix metalloproteinase-2 (MMP-2).
Methods
The 1H-MRS spectra of 41 histologically verified astrocytomas were obtained on a 3-T MR scanner. According to the World Health Organization classification criteria for central nervous system tumors, there were 16 low-grade astrocytomas (2 pilocytic astrocytomas, 14 grade II astrocytomas) and 25 high-grade astrocytomas (5 anaplastic astrocytomas, 20 glioblastomas).The choline/N-acetylaspartate (Cho/NAA) and choline/creatine (Cho/Cr) ratios were calculated. Of the 41 astrocytomas, 19 (8 low-grade and 11 high-grade) were analyzed immunohistochemically. Expression of MMP-2 was determined using streptavidin-peroxidase complex (SP) staining which was quantified by calculating its calibrated opacity density (COD) using an image analysis system. The correlations between metabolite ratios and the quantitative data from the immunohistochemical tests in the 19 astrocytomas were determined.
Results
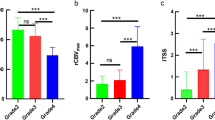
The Cho/NAA and Cho/Cr ratios of high-grade astrocytoma were both significantly greater than those of low-grade astrocytoma (t = −6.222, P = 0.000; t = −6.533, P = 0.000, respectively). MMP-2 COD values of high-grade astrocytomas were also significantly greater than those of low-grade astrocytomas (t = −5.892, P = 0.000). There were strong positive correlations between Cho/NAA ratio and MMP-2 COD (r = 0.669, P = 0.002), and between Cho/Cr ratio and MMP-2 COD (r = 0.689, P = 0.001).
Conclusion
1H-MRS is helpful in evaluating the invasiveness of astrocytomas and predicting prognosis preoperatively by determining the Cho/NAA and Cho/Cr ratios.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Astrocytoma is the most common intracranial tumor. Although it is classified into four grades according to its biological activity, even low-grade astrocytomas infiltrate the entire brain, a feature that precludes their successful therapy [1]. The invasiveness of astrocytoma is proportional to its malignancy. It has been proved that the infiltrating growth pattern of astrocytoma is closely associated with the antigen, matrix metalloproteinase-2 (MMP-2) [2–5]. The higher the level of expression of this antigen, the higher the tumor grade. MR spectroscopy (MRS) is able to reveal metabolic changes of disease noninvasively. Previous studies have revealed that the grade of astrocytoma can be determined by 1H-MRS and the grade is positively correlated with cellular proliferation [6–8]. The aim of this study was to explore the relationship between MMP-2 expression and the 1H-MRS results in astrocytomas of different grades to determine whether 1H-MRS could be used to evaluate the invasiveness of astrocytoma.
Materials and methods
Patients
Enrolled in this study were 41 patients (15 women and 26 men, aged 14–73 years, mean age 45 years) with pathologically confirmed astrocytomas. According to the World Health Organization classification criteria for central nervous system tumors, there were 16 low-grade astrocytomas (2 pilocytic astrocytomas, 14 grade II astrocytomas) and 25 high-grade astrocytomas (5 anaplastic astrocytomas, 20 glioblastomas). None of the patients had undergone any treatment before MRS examination. All patients were operated on within 7 days after the MRS examination. The study was approved by our institutional review board and informed consent was obtained from all patients.
Spectroscopy
Two-dimensional (2-D) multivoxel 1H-MRS was performed on a 3-T MR scanner (Excite II; GE Signa, Milwaukee, Wis.) using a point-resolved spectroscopic sequence (PRESS). The bird-cage head coil was used for all examinations (TR/TE 1,000/144 ms, number of excitations 1, field of view 24, matrix 16×16, slice thickness 6 mm, interslice gap 1 mm). According to the manufacturer’s protocol, axial T2-weighted (T2-W) images were scanned for region of interest (ROI) selection. In order to avoid surrounding contamination (skull, air cavities, CSF, etc) as much as possible, a ROI including lesion and contralateral normal tissue was selected. Shimming and water suppression were performed automatically by the MR scanner. When the standard of full width at half maximum (FWHM) <15 and water suppression >95% were fulfilled, the scan started. The duration time was 260 s. The data were postprocessed on the GE ADW4.2 workstation using FUNCTOOL 3.1 software by two experienced neuroradiologists. A 1.5×1.5-cm voxel was placed in the homogeneous portion of lesions. Then spectrum was generated automatically. The signal intensity of various metabolite peaks was evaluated using integrals of each peak as a measure of its intensity. The integration limits of the respective peaks were manually defined before computerized calculations. For calculation of metabolite ratios, the integrals of metabolites in the same voxel were used. The spectra were analyzed for the signal intensity of N-acetylaspartate (NAA), choline (Cho) and creatine (Cr). Cho/NAA and Cho/Cr ratios were calculated.
Immunohistochemistry
The tumor was surgically removed from all patients. The tumor was resected en bloc when possible or in several parts otherwise. In 19 of the 41 patients, the tissue sample nearest the spectroscopic voxel was visually identified during sectioning by comparison with MR images and was used for MMP-2 immunostaining. A sample from each of the 19 patients (8 grade II astrocytomas, 4 anaplastic astrocytomas, 7 glioblastomas) was fixed in 10% neutral formalin and embedded in paraffin wax. The samples were then deparaffinized using dimethyl benzene and ethyl alcohol. Reagents including MMP-2 monoclonal antibody, a streptavidin-peroxidase (SP) test kit and a 3,3′-diaminobenzidine tetrahydrochloride dying test kit were provided by Beijing Zhongshan Biotech Corporation. Immunohistochemical testing was performed using SP complex staining according to the instructions in the manual. Brown particles in the cytoplasm were considered to indicate MMP-2 expression. To quantify MMP-2 expression, Image-Pro plus 4.1 image analysis software was used to determine the calibrated opacity density (COD) of the immune reaction products. Ten ×100 magnification fields of each slice were selected randomly, and the mean COD was calculated.
Statistics
SPSS 12.0 software was used for statistical analysis. All quantitative data are expressed as means±standard deviation. Differences in the expression of MMP-2 and the Cho/NAA and Cho/Cr ratios between low- and high-grade astrocytomas were evaluated using an unpaired t-test. Linear regression analysis was performed to assess the relationship between the MMP-2 COD and the Cho/NAA and Cho/Cr ratios. Differences with P<0.05 were considered to be statistically significant.
Results
All patients tolerated the MRS examination and all spectra obtained were satisfactory. The Cho/NAA ratios in the 16 low-grade astrocytomas ranged from 1.080 to 2.683, with a mean of 1.559±0.419, whereas in the 25 high-grade astrocytomas the ratios ranged from 1.370 to 8.000, with a mean of 4.247±2.095. The difference was statistically significant (t = −6.222, P = 0.000). The Cho/Cr ratios in the 16 low-grade astrocytomas ranged from 1.317 to 2.693, with a mean of 1.793±0.386, whereas in the 25 high-grade astrocytomas the ratios ranged from 1.457 to 6.910, with a mean of 3.809±1.465. The difference was statistically significant (t = −6.533, P = 0.000; Table 1; Figs. 1 and 2). Using a Cho/NAA ratio of 2.0 as a threshold, 88.0% of high-grade astrocytoma (22/25) and 93.8% of low-grade astrocytomas (15/16) were diagnosed correctly, and using a Cho/Cr ratio of 2.0 as a threshold, 92.0% high-grade astrocytomas (23/25) and 87.5% low-grade astrocytomas (14/16) were diagnosed correctly.
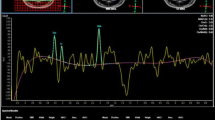
A 52-year-old male patient with grade II astrocytoma. a T2-W image for ROI selection. Voxel 1 is located in the homogeneous part of tumor. b Spectrum of voxel 1. There is no lipid peak, and the Cho/NAA and Cho/Cr ratios are both smaller than 2.0. c Expression of MMP-2 (SP, ×400). There are subtle brown particles in the cytoplasm, which indicates weak expression of MMP-2
A 65-year-old male patient with glioblastoma. a T2-W image for ROI selection. Voxel 1 is located in the homogeneous part the of tumor. b Spectrum of voxel 1. The Cho/NAA and Cho/Cr ratios are both greater than 2.0. The lipid peak is obvious. c Expression of MMP-2 (SP, ×400). There is clear brown staining throughout most of the cytoplasm
The levels of expression of MMP-2 in the 8 low-grade astrocytomas ranged from 0.155 to 0.274, with a mean of 0.196±0.046, whereas in the 11 high-grade astrocytomas the levels of expression ranged from 0.284 to 0.443, with a mean of 0.338±0.056. The difference was statistically significant (t = −5.892, P = 0.000; Figs. 1c and 2c). In 19 astrocytomas analyzed immunohistochemically, the Cho/NAA and Cho/Cr ratios were significantly positively correlated with the expression of MMP-2 (r = 0.669, P = 0.002; r = 0.689, P = 0.001, respectively; Figs. 3 and 4).
Discussion
1H-MRS can reveal metabolic changes in vivo noninvasively, which makes it possible to obtain important biochemical information at the molecular level in intracranial tumors which cannot be provided by conventional structural analysis. The astrocytoma is the most common primary intracranial neoplasm, arising from abnormal hyperplasia of gliocytes. The gliocytes encroach on the normal neurons during tumor growth.
NAA (measured at 2.02 ppm) is synthesized mainly in the neuronal somata and axons, and is recognized as a putative internal neuronal marker. The concentration of NAA reflects the status of the neurons. Stadlbauer et al. have reported that malignancy of gliomas tends to increase with decreasing NAA [9]. In the present study, we found various levels of decrease in NAA in astrocytomas. This finding could reflect the fact that the neurons had been damaged and replaced by tumor, leading to a decrease in the number of neurons and a decline in the concentration of NAA.
Cho (measured at 3.21 ppm) is a membrane metabolite and an increase in its level mainly reflects an acceleration in cellular membrane metabolism, such as turnover or synthesis. The concentration of Cho represents the total choline content which includes choline, phosphorylcholine, phosphatidylcholine and glycerophosphorylcholine. Therefore, the Cho signal intensity always increases in astrocytomas and increases more obviously with the increasing malignancy. The elevation in the Cho peak found in the present study was due not only to rapid cellular proliferation, as a result of increased mitosis, leading to an abnormal increase in membrane metabolism [10, 11], but also to the turnover of cellular membrane because of the invasiveness of the tumor. Meyerand et al. [12] found that there is a significant difference in the Cho/Cr ratio between grade II astrocytoma and high-grade astrocytoma (anaplastic astrocytoma and glioblastoma), but no obvious difference between the two types of high-grade astrocytoma was seen. Dowling et al. [13] calculated the ratio of Cho in tumor to that in contralateral healthy tissue, and suggested that the increase in Cho paralleled the deterioration in clinical status. A follow-up showed that the increase in Cho was more than 45% in patients showing deterioration, while that in stable patients was no more than 35%. Li et al. [14] have reported that the survival of young patients with a lower Cho/Cr ratio preoperatively, even if the tumor is fairly big and the symptoms are obvious, is relatively long, and after surgery if the Cho/NAA ratio in older patients and the Cho/Cr ratio in young patients show a striking increase, the prognosis is poor. Wu et al. [15] reported a patient with low-grade glioma. The MR and perfusion imaging findings suggested that it was a benign astrocytoma. Only the Cho/Cr ratio showed a clear increase. After 2 years the tumor had evolved into a glioblastoma. The authors suggest that when the MRS and perfusion imaging findings are discrepant, close follow-up is critical.
Total Cr, which is expressed as a single high peak in vitro at 3. 03 ppm, represents the sum of creatine and phosphocreatine, which are present in vivo as two adjoining peaks (at 3.03 and 3.94 ppm). Cr probably plays a role in maintaining energy-dependent systems in brain cells by serving as a reserve of high-energy phosphates and as a buffer in adenosine triphosphate and adenosine diphosphate reservoirs. Its content has been reported to be rather stable in normal and pathologically altered brain tissue. Thus, Cr is frequently taken as an internal standard or reference peak to estimate changes in other metabolites.
In the present research, comprising 41 astrocytomas of different grades, the Cho/NAA and Cho/Cr ratios in high-grade astrocytomas were significantly higher than in low-grade astrocytomas. The results of this study are consistent with those of previous studies. Moreover, the results further verified the correlation between an increase in Cho signal and tumor proliferation and metabolism.
One of the major pathophysiological features of human astrocytomas is their ability to diffusely invade surrounding brain tissues. The rapid dissemination of single tumor cells throughout the brain renders these tumors incurable by surgical removal even when combined with adjuvant radiation and either chemotherapies or immunotherapies [16], and also underlies their great propensity for recurrence. Invasion of glioma cells involves the attachment of invading tumor cells to the extracellular matrix (ECM), disruption of ECM components, and subsequent cell penetration into adjacent brain structures. This is accomplished in part by tumor-secreted MMPs that degrade the ECM at the tumor-invasive front to overcome the ECM barrier [2]. MMPs are a family of 22 ECM-modifying enzymes [3]. Upregulation of MMP-2 has been found in glioma cell lines and in specimens of high-grade glioma [4], and its activation has been linked to enhanced glioma invasion in several in vitro and in vivo model systems [2, 5]. Takahashi et al. [17] have suggested that if there is a lack of MMP-2, the glioma becomes smaller and degeneration of tumoral vessels and necrosis occurs. On the other hand, to some extent the growth of glioma could activate MMP-2 to induce vascular genesis and maintain the angioarchitecture.
The present study showed significant positive correlations between the Cho/NAA and Cho/Cr ratios and MMP-2 COD. With increasing malignancy, MMP-2 is increasingly activated and the ECM is disrupted. So the ability of the astrocytoma to invade the normal brain tissue intensifies. Then more and more neurons are broken down. The damage to the cellular membranes causes an increase in Cho concentration. These are the possible reason for our results, and suggest that 1H-MRS could be used to evaluate the invasiveness of astrocytoma and help in deciding the treatment strategy and in estimating the prognosis.
En bloc tumor resection allows histological examination of the specimen for MMP-2 expression in nearly same region as the MRS voxel. This, however, is not always possible, so finally we had only 19 specimens for immunohistochemical analysis, even though we could not guarantee the concordance. An image-guided technique, which was not applied in the present study for the purpose of tissue sampling, would improve the spatial correlation between the samples examined by MRS and those for histological examination.
Although MRS is a noninvasive technique which can provide metabolic information on disease at the molecular level, it has not been integrated into routine MR protocols so far. One of the main reasons is that most studies simply focus on comparing MRS with pathological grade. Little research has been carried to investigate the usefulness of MRS at the protein, molecular and even genomic levels. There have been only a few such studies in recent years. Shimizu et al. [6] found a clear positive correlation between Ki-67 labeling index and Cho/Cr ratio and a negative correlation between Ki-67 labeling index and NAA/Cho ratio in homogeneous gliomas. However, Gupta et al. [7] found no relationship between Cho level and Ki-67 (MIB-1) labeling index, but did find a positive correlation between nuclear density and Cho level. Nafe et al. [18] also found no correlation between Cho level and Ki-67 labeling index, but did find a positive correlation between lipid level and Ki-67 labeling index. No study comparing MRS findings and MMP-2 expression has yet been reported. This study did show strong positive correlations between MRS findings and MMP-2 expression, suggesting that 1H-MRS is also helpful in evaluating the infiltrating potential of astrocytomas and in predicting prognosis.
References
Rooprai HK, Rucklidge GJ, Panou C, Pilkington GJ (2000) The effects of exogenous growth factors on matrix metalloproteinase secretion by human brain tumour cells. Br J Cancer 82:52–55
Chintala SK, Tonn JC, Rao JS (1999) Matrix metalloproteinases and their biological function in human gliomas. Int J Dev Neurosci 17:495–502
Brinckerhoff CE, Matrisian LM (2002) Matrix metalloproteinases: a tail of a frog that became a prince. Nat Rev Mol Cell Biol 3:207–214
Yong VW, Power C, Forsyth P, Edwards DR (2001) Metalloproteinases in biology and pathology of the nervous system. Nat Rev Neurosci 2:502–511
Lampert K, Machein U, Machein MR, Conca W, Peter HH, Volk B (1998) Expression of matrix metalloproteinases and their tissue inhibitors in human brain tumors. Am J Pathol 153:429–437
Shimizu H, Kumabe T, Shirane R, Yoshimoto T (2000) Correlation between choline level measured by proton MR spectroscopy and Ki-67 labeling index in gliomas. AJNR Am J Neuroradiol 21:659–665
Gupta RK, Cloughesy TF, Sinha U, Garakian J, Lazareff J, Rubino G (2000) Relationships between choline magnetic resonance spectroscopy, apparent diffusion coefficient and quantitative histopathology in human glioma. J Neurooncol 50:215–226
Chen J, Huang SL, Li T, Chen XL (2006) In vivo research in astrocytoma cell proliferation with 1H-magnetic resonance spectroscopy: correlation with histopathology and immunohistochemistry. Neuroradiology 48:312–318
Stadlbauer A, Gruber S, Nimsky C, Fahlbusch R, Hammen T, Buslei R, Tomandl B, Moser E, Ganslandt O (2006) Preoperative grading of gliomas by using metabolite quantification with high-spatial-resolution proton MR spectroscopic imaging. Radiology 238:958–969
Möller-Hartmann W, Herminghaus S, Krings T, Marquardt G, Lanfermann H, Pilatus U, Zanella FE (2002) Clinical application of proton magnetic resonance spectroscopy in the diagnosis of intracranial mass lesions. Neuroradiology 44:371–381
Fountas KN, Kapsalaki EZ, Vogel RL, Fezoulidis I, Robinson JS, Gotsis ED (2004) Noninvasive histologic grading of solid astrocytomas using proton magnetic resonance spectroscopy. Stereotact Funct Neurosurg 82:90–97
Meyerand ME, Pipas JM, Mamourian A, Tosteson TD, Dunn JF (1999) Classification of biopsy-confirmed brain tumors using single-voxel MR spectroscopy. AJNR Am J Neuroradiol 20:117–123
Dowling C, Bollen A, Noworolski SM, McDermott MW, Barbaro NM, Day MR (2001) Preoperative proton MR spectroscopy imaging of brain tumors: correlation with histopathologic analysis of resection specimens. AJNR Am J Neuroradiol 22:604–612
Li X, Jin H, Lu Y, Oh J, Chang S, Nelson SJ (2004) Identification of MRI and 1H MRSI parameters that may predict survival for patients with malignant gliomas. NMR Biomed 17:10–20
Wu WC, Chen CY, Chung HW, Juan CJ, Hsueh CJ, Gao HW (2002) Discrepant MR spectroscopic and perfusion imaging results in a case of malignant transformation of cerebral glioma. AJNR Am J Neuroradiol 23:1775–1778
Hu B, Guo P, Fang Q, Tao HQ, Wang D, Nagane M, Huang HJ, Gunji Y, Nishikawa R, Alitalo K, Cavenee WK, Cheng SY (2003) Angiopoietin-2 induces human glioma invasion through the activation of matrix metalloprotease-2. Proc Natl Acad Sci U S A 100:8904–8909
Takahashi M, Fukami S, Iwata N, Inoue K, Itohara S, Itoh H (2002) In vivo, glioma growth requires host derived matrix metalloproteinase 2 for maintenance of angioarchitecture. Pharmacol Res 46:155–163
Nafe R, Herminghaus S, Raab P, Wagner S, Pilatus U, Schneider B (2003) Preoperative proton-MR spectroscopy of gliomas – correlation with quantitative nuclear morphology in surgical specimen. J Neurooncol 63:233–245
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, K., Li, C., Liu, Y. et al. Evaluation of invasiveness of astrocytoma using 1H-magnetic resonance spectroscopy: correlation with expression of matrix metalloproteinase-2. Neuroradiology 49, 913–919 (2007). https://doi.org/10.1007/s00234-007-0271-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-007-0271-8