Abstract
Tri- and dipeptides are transported in the kidney by PEPT1 and PEPT2 isoforms. The aim of this study was to investigate differences in transport kinetics between renal brush border (BBMV) and outer medulla (OMMV) membrane vesicles (where PEPT1 and PEPT2 are sequentially available) for a range of di- and tripeptides and peptidomimetic drugs. This was accomplished through the use of the potential-sensitive fluorescent dye 3,3′-dipropylthiacarbocyanine iodide [DiS–C3-(3)]. BBMV and OMMV were prepared from the rat kidney using standard techniques. The presence of PEPT1 in BBMV and PEPT2 in OMMV was confirmed using Western blotting. Fluorescence changes were measured when extravesicular medium at pH 6.6 containing 0–1 mM substrates was added to a cuvette containing vesicles pre-equilibrated at pH 7.4 and 2.71 μM DiS-C3-(3). An increase in fluorescence intensity occurred upon substrate addition reflecting the expected positive change in membrane potential difference. Of the range of substrates studied, OMMV manifested the highest affinity to cefadroxil and valacyclovir (K m 4.3 ± 1.2 and 11.7 ± 3.2 µM, respectively) compared to other substrates, whilst the BBMV showed a higher affinity to Gly-His (K m 15.4 ± 3.1 µM) compared to other substrates. In addition, OMMV showed higher affinity and capacity to Gly-Gln (K m 47.1 ± 9.8 µM, 55.5 ± 2.8 ΔF/s/mg protein) than BBMV (K m 78.1 ± 13.3 µM and 35.5 ± 1.7 ΔF/s/mg protein, respectively). In conclusion, this study successfully separated the expression of PEPT1 and PEPT2 into different vesicle preparations inferring their activity in different regions of the renal proximal tubule.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The generation and regulation of a membrane potential difference is a dynamic process and fundamentally crucial to many physiological functions. For example, the energy released from ATP hydrolysis is used by the Na+, K+ ATPase to transport three Na+ ions out of the cell in exchange for two K+ ions pumped into the cell (Blostein 1999). This, in combination with the passive potassium and chloride fluxes, creates a negative membrane potential difference that favours the entry of sodium ions. This electrochemical gradient generates the driving force that facilitates the efficient absorption of many nutrients and some important drugs (Faller 2008; Jorgensen 1986). The reabsorption of amino acids in the kidney proximal tubule is a vital process to the body’s protein balance. Small peptides in the form of 2-3 amino acids are transported by the H+-dependent transporters PEPT1 (low-affinity/high-capacity) and PEPT2 (high-affinity/low-capacity) (Daniel and Kottra 2004). The translocation of di- and tripeptides by these cotransporters is forced by a transmembrane electrochemical proton gradient. This is mainly facilitated by the apical Na+–H+ exchanger (NHE3), which acidifies the lumen to around pH 6.7–6.8 by continuously secreting H+ across the brush border membrane (Daniel and Kottra 2004; Vieira and Malnic 1968). The resultant H+ inward electrochemical gradient can then be utilised by PEPT cotransporters to force the uptake of any of the naturally occurring 400 dipeptide and 8000 potential tripeptide combinations into the proximal tubule cells (Anderson and Thwaites 2010; Rubio-Aliaga and Daniel 2008). PEPT transporters are also capable of transporting a vast range of peptidomimetic drugs including β-lactam antibiotics of the aminocephalosporin (e.g. cefadroxil) and penicillin (e.g. ampicillin) classes; some antiviral (e.g. valacyclovir) and anti-tumour drugs (e.g. δ-amino-levulinic acid and γ-glutamyl-l-cysteine); and selected angiotensin-converting enzyme (ACE) inhibitors (e.g. captopril) (Brandsch et al. 2008).
PEPT1 and PEPT2 transporters are heterogeneously distributed in the renal proximal tubule, as PEPT1 is confined to segment 1, while PEPT2 is restricted predominantly to the later S3 segments (Shen et al. 1999). PEPT2 was found in higher quantity than PEPT1 (Leibach and Ganapathy 1996; Smith et al. 1998), and hence it was suggested that PEPT2 is the main cotransporter for the uptake of peptides and peptidomimetic drugs (Shen et al. 1999). Several studies using either transfected cell lines with PEPT1 and PEPT2 (Terada et al. 1997) or BBMV (Ries et al. 1994; Takahashi et al. 1998) revealed that β-lactam antibiotic containing an α-amino group (e.g. cefadroxil) had much higher affinity to the renal PEPT2. However, the relative contribution of the native PEPT1 and PEPT2 isoforms in transporting oligopeptides and peptidomimetic drugs in the renal proximal tubule is not clear yet. It was suggested that further studies investigating the distribution and expression level of PEPT1 and PEPT2 and also their contribution to the tubular reabsorption are needed for differentiating between their roles (Takahashi et al. 1998).
In the past, BBMV have been a popular method for studying the characteristics of di- and tripeptide transport by PEPT1 and PEPT2 (Daniel et al. 1991; Ries et al. 1994; Takahashi et al. 1998). This is partly because the absence of metabolic machinery allows the accumulation of the intact substrate in the intravesicular space to be measured. Traditionally, such experiments have involved the measurement of radioisotope flux (Daniel et al. 1991; Ries et al. 1994; Takahashi et al. 1998) or DiS-C3-(5) (Plášek et al. 1994). We have developed a method of measuring the kinetic parameters for the uptake of some di- and tripeptide and selected peptidomimetic drugs into renal BBMV and OMMV via the use of the fluorescent potential-sensitive dye, 3,3′-dipropylthiacarbocyanine iodide [DiS-C3-(3)]. In a previous publication, we showed that DiS-C3-(3) could be used to detect changes in membrane potential difference in renal membrane vesicles but did not measure the kinetics of substrate transport (Alghamdi and King 2012). The reason why it is important to measure the transport kinetics in different regions of the kidney is predicting the bioavailability of different substrates and drugs or where genetic variations exist in the transporters and their expression.
Materials and Methods
Chemicals and Kidneys
All chemicals and reagents used in this study were obtained from SIGMA, Chem-Supply AppliChem, Santa Cruz Biotechnology or GE Healthcare and were of analytical quality. Kidneys were obtained from 6- to 7-month-old male Wistar rats, which were sacrificed by stunning and cervical dislocation. The kidneys were snap frozen in liquid nitrogen and then transferred to a − 80 °C freezer until used for the preparation of BBMV and OMMV. This study was approved by the Animal Ethics committee of the University of New England and complies with the Guide for the care and use of laboratory Animals published by the US National Institute of Health (NIH Publication No. 85-23, revised 1996).
Isolation of BBMV and OMMV and Quality Control
The BBMV and OMMV were isolated by the two-step Mg++/EGTA precipitation method (Biber et al. 1981; Brown et al. 1993; Daniel et al. 1991). BBMV were prepared from ~ 0.5- to 1-mm-thick slices of superficial cortex, while OMMV were prepared from slices of outer medulla, which are characterised by having red stripes (Kragh-Hansen and Sheikh 1984; Smith et al. 1998). The integrity of the purified vesicles was examined using marker enzyme assays. The enrichments of alkaline phosphatase and leucine aminopeptidase for BBMV were 13.51 ± 2.07 and 12.82 ± 1.32 fold and those for OMMV were 11.3 ± 0.75 and 17.23 ± 2.4 fold, respectively. These values of enzyme enrichments indicate good, noncontaminated vesicles (Biber et al. 1981). Protein concentration was quantified using Bradford’s method (Brown et al. 1993).
After isolating the vesicles and before placing them in the − 80 °C freezer, they were suspended in buffer 1 (intravesicular medium) containing (in mM) 100 mannitol, 100 KH2PO4 and 10 HEPES (pH 7.4 with TRIS) and centrifuged at 31,000×g for 20 min at 4 °C (Daniel et al. 1991). The supernatant was discarded and the pellet was re-suspended with the same solution and pre-equilibrated using freeze–thaw fractionation (Donowitz et al. 1987). The transport buffer (buffer 2) (extravesicular medium) contained (in mM) 100 mannitol, 100 KH2PO4 and 10 2-(N-Morpholino)ethanesulphonic acid (MES, pH 6.6 with TRIS).
Western Blot Analysis
As PEPT1 and PEPT2 are located in different segments of the kidney (superficial cortex and outer medulla, respectively) (Shen et al. 1999), Western blot was used to confirm the positive/negative expression in the isolated BBMV and OMMV. BBMV and OMMV containing 45 µg protein/sample were mixed in Eppendorf tubes with the loading buffer (3×) containing 6% sodium dodecyl sulphate (SDS), 0.3% bromophenol blue, 30% glycerol, 5% β-mercaptoethanol and 150 mM Tris–HCl (pH 6.8). They were transferred to a boiling water bath at 100 °C for 5 min. After that, the tube contents were loaded onto Mini-PROTEAN Bio-Rad Gels 4-20% and the first well was always loaded with 5 µl of Precision Plus Protein Standards as a molecular weight control ladder. Gels were run at 120 V constant voltage for 40-90 min. The gels were then blotted with nitrocellulose membrane (semi-dry system) at 120 mA for 3 h. The membranes were stripped for 15 min as described by Kaur and Bachhawat (2009) and incubated overnight with blocking buffer 5% skim milk dissolved in TBS-T buffer containing (in mM) 150 NaCl, 20 Tris–HCl (pH 7.5) and 0.1% Tween 20. The membranes were then incubated with either mouse monoclonal anti-PEPT1 for 1 h at room temperature (RT) or with goat polyclonal anti-PEPT2 overnight at 4 °C. This was followed by an hour’s incubation with HRP-conjugated goat anti-mouse and mouse anti-goat IgG, respectively, at RT. Between probing with the primary and secondary antibodies and after incubation with the secondary antibodies, the membranes were washed three times for 10 min with TBS-T buffer. Protein bands were detected using ECL™ Western Blotting Analysis System (GE Healthcare) according to the manufacturer’s instructions. Scanned pictures of Hyperfilm ECL were taken using BIO-RAD GEL DOC EQ system. The membranes were transferred to a stripping buffer containing (in mM) 100 β-mercaptoethanol, 62.5 Tris–HCl (pH 6.7) and 2% SDS at 55 °C for 30 min, followed by 2 × 10 min washes with TBS-T. Then they were incubated with the blocking buffer and reprobed with anti-β-actin (mouse monoclonal) antibodies, following the steps described above. This was used as a loading control and it was confirmed that each lane had equal amounts of protein loaded into it (results not shown).
Fluorescence Measurements of Substrate Transport
These measurements were carried out at 20–24 °C in a fluorescence spectrophotometer (Perkin-Elmer LS 55), preset with 5 nm slit width and excitation and emission wavelengths of 557 and 575 nm, respectively, and the cuvettes used had a pathlength of 2 mm. Fluorescence intensity (in arbitrary units) was recorded at 0.02-s intervals for about 80 s and displayed on a digital screen as a plot of fluorescence versus time (see Fig. 2 for an example).
Experiments were started by mixing appropriate volumes of buffer 2, 4 µl from a 541 µM stock (2.71 µM final concentration) DiS-C3-(3) and sufficient vesicles to obtain a constant protein concentration of 45 µg (maintaining a dye-to-protein ratio of 19.4 µg/mg (Cassano et al. 1988; Wright et al. 1981) to a total volume of 800 µl into an Eppendorf tube. This Eppendorf tube was gently mixed using a pipette. The total volume was then divided into two matched cuvettes (each had 396 µl): one for the sample, whilst the other served as the control, both of which were placed into the fluorimeter, and the fluorescence followed for 50 s to enable stabilisation of the signal. A series of concentrations of the substrates were made as stock solutions so that a constant volume of 4 µl was added to each sample, as the addition of different volumes could cause variations in fluorescence intensity. After adding the substrates (e.g. Gly-Gln), the fluorescence was measured for approximately another 50 s until the fluorescence had stabilised. Graphs of the fluorescence measured (in arbitrary units) versus time (in 0.02 s) were plotted and are shown in Fig. 2. To the control samples no substrates were added.
Data Analysis and Presentation
The readings for the first period during which fluorescence was stable (approx. 50 s) were removed from all samples, as this period was used to check whether the system was in the steady state. After that, all data were normalised and each sample was corrected for the changes of fluorescence due to the addition of the substrate by subtracting the trace obtained for the corresponding control samples. Then the average of these corrected readings for each concentration was plotted. The total change in fluorescence intensity was then calculated by subtracting the intensity at the start of the transport to the intensity at the plateau. This was then repeated for different substrate concentrations. The readings were then plotted against their corresponding substrate concentrations and fitted using a Michaelis–Menten curve (R 2 values that demonstrated a goodness of fit > 90) and the equation (\(V = \frac{{V_{\hbox{max} } [S]}}{{K_{\text{m}} + [S]}}\)), which was then used to calculate V max and K m. V max values were calculated as ΔF/0.02 s/45 µg protein, which were converted to ΔF/s/mg protein. Student’s t test was then applied using the following equations: \(t = \frac{{{\text{Difference between the two means}}}}{{{\text{SE of the difference}} }}\) and \({\text{SE}}\;{\text{difference}} = \sqrt {\frac{{{}_{\text{S}}^{2} A}}{{n_{\text{A}} }} + \frac{{{}_{\text{S}}^{2} B}}{{n_{\text{B}} }}}\) to illustrate significant differences between kinetic values. All of the results presented are mean ± SE of n = 6–8 samples. P values < 0.05 were considered to be statistically significant.
Results
Confirmation of the Sequential Distribution of PEPT1 and PEPT2 in BBMV and OMMV, Respectively
All vesicles used in this study were examined by Western blot to confirm the correct distribution of PEPT1 and PEPT2. PEPT1, PEPT2 and β-actin protein bands were detected in BBMV and OMMV with the molecular weights of 75, 85 and 43 kDa, respectively. As shown in the upper panel of Fig. 1, PEPT1 was present in the first 2 lanes, which were loaded with BBMV, while it was absent in lanes 3–11 where OMMV were loaded. The middle panel of Fig. 1 shows that PEPT2 was absent in lanes 4–6 and 8–11 in which BBMV were loaded, while PEPT2 bands were clearly shown in the lanes loaded with OMMV.
Measurement of Fluorescence Changes as a Function of Time upon the Addition of Extravesicular Medium With or Without 1000 µM Gly-Gln
Figure 2 shows the result of a single experiment representative of 7 such experiments for renal BBMV and OMMV. A sharp decrease in fluorescence was seen as soon as 1000 µM Gly-Gln was added, followed by an increase and a plateau with a largely unchanging fluorescence level that continued for the rest of the experiment. This general pattern was observed in all experiments when different concentrations of substrates were delivered to both BBMV and OMMV. When the same volume of extravesicular buffer containing no Gly-Gln was added to both BBMV and OMMV, there was a similar decrease in fluorescence followed by a plateau (Fig. 2). This pattern of fluorescence was seen in all vesicles, except for at a low concentration of some substrates (10–50 µM) delivered to OMMV which showed a slightly smaller decrease in fluorescence than the control, followed by a sharp increase in fluorescence.
Changes in fluorescence intensity measured upon Gly-Gln (1000 µM) addition to either BBMV or OMMV. Controls (no substrate addition) for these samples were run as indicated in this graph. The arrow indicates the point at which Gly-Gln was added. Data shown are taken from a single experiment representative of 7 such experiments
Kinetics of Substrate Uptake into BBMV and OMMV
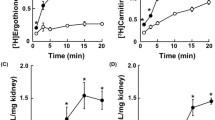
Figures 3, 4 and 5 shows the comparison of the Michaelis–Menten curves for the transport kinetics of a range of substrates measured using an extravesicular pH of 6.6. When comparing the transport of Gly-Gln (circles, dashed line), Gly-His (squares, continuous line) and cefadroxil (triangles, bold dashed line) in BBMV (Fig. 3), the V max value for Gly-His transport was significantly higher than that for Gly-Gln transport (57.3 ± 2.1 ΔF/s/mg protein and 35.5 ± 1.7 ΔF/s/mg protein, respectively, P = 0.001). Similarly, the K m value for Gly-His transport was significantly lower than that for Gly-Gln (15.4 ± 3.1 and 78.1 ± 13.3 μM, respectively, P = 0.002). Cefadroxil (Fig. 3) had an affinity for the transporters situated between Gly-His and Gly-Gln (34.1 ± 8.4 μM) but with a much higher capacity (82.7 ± 5.67 ΔF/s/mg protein) than for the two dipeptides.
Change in fluorescence (ΔF/0.02 s, > 0) as a function of substrate concentration delivered to the BBMV at pH 6.6. Squares joined with a continuous line represent the values obtained for Gly-His. Circles joined with a dashed line represent the values obtained for Gly-Gln. Triangles joined by a bold dashed line represent the values for cefadroxil. Curves were fitted according to the Michaelis–Menten equation. Data shown are mean ± SE, where n = 8
Change in fluorescence (ΔF/0.02 s, > 0) as a function of substrate concentration delivered to the OMMV at pH 6.6. Squares joined with a continuous line represent the values obtained for Gly-His. Circles joined with a dashed line represent the values obtained for Gly-Gln. Triangles joined with a bold dashed line represent the values for Gly-Gly-His. Curves were fitted according to the Michaelis–Menten equation. Data shown are mean ± SE, where n = 8
Change in fluorescence (ΔF/0.02 s, > 0) as a function of substrate concentration delivered to the OMMV at pH 6.6. Squares joined with a continuous line represent the values obtained for valacyclovir. Circles joined with a dashed line represent the values obtained for cefadroxil. Triangles joined with a bold dashed line represent the values for δ-amino-levulinic acid. Curves were fitted according to the Michaelis–Menten equation. Data shown are mean ± SE, where n = 6
The same trend for the transport of two dipeptides was observed in OMMV (Fig. 4) compared to BBMV, with a K m significantly lower for Gly-His transport (squares, continuous line) than for Gly-Gln transport (circles, dashed line) (12.5 ± 3.1 μM and 47.1 ± 9.8 μM, respectively, P = 0.012) and a decrease (although not significant) in V max between Gly-His and Gly-Gln (61.1 ± 2.5 ΔF/s/mg protein and 55.5 ± 2.8 ΔF/s/mg protein, respectively, P = 0.1). However, unlike the BBMV, cefadroxil had a significantly higher transporter affinity (4.3 ± 1.2 μM) than both dipeptides (squares, continuous line; Fig. 4). In addition, the K m value for Gly-Gly-His transport (triangles, dashed line) (47.5 ± 6.65 μM) was significantly lower than for Gly-His transport (P = 0.002) but similar to the Gly-Gln transport. However, the V max value for Gly-Gly-His transport (75.9 ± 2.33 ΔF/s/mg protein) was significantly higher than for Gly-His (P = 0.0034) and Gly-Gln (P = 0.0006) transport.
When comparing peptidomimetic drug substrates in OMMV, the K m value of cefadroxil was significantly lower than that of δ-amino-levulinic (P = 0.001), but close to statistical significance with valacyclovir (P = 0.06; Fig. 5). Also, the V max value was significantly higher for cefadroxil than those for other two drugs (P = 0.002 and 0.001, respectively, Table 1).
A complete list of the K m and V max values for all substrates measured in BBMV and OMMV is shown in Table 1. This shows that the V max value for Gly-Gln transport in BBMV was significantly lower than that for Gly-Gln (P = 0.001) transport in OMMV. Also, the transport of Gly-Gln in OMMV exhibited a higher affinity than that in BBMV, although not significant (P = 0.09). However, while the same trends were observed for V max and K m in the case of Gly-His, the differences between BBMV and OMMV were not significant. In addition, there was no significant difference in V max for cefadroxil transport between BBMV and OMMV. However, the K m value for cefadroxil transport in OMMV was significantly lower than that in BBMV (P = 0.001).
Discussion
The reabsorption of important nutrients in the kidney occurs mostly in the proximal tubule where the proton-dependent PEPT1 and PEPT2 cotransporters are located. The electrochemical gradient created by the inward cation and membrane potential difference is the main force driving these reabsorptive processes. Indeed, the transport of these substrates by PEPT1 and PEPT2 is well defined to be a proton-dependent process in which translocation of the substrate is accompanied by hydrogen ions. Measuring the membrane potential difference could provide important insights into the renal functions for nutrient handling, wastes and also the pharmacokinetics of many drugs. Several studies have shown the possible applications of cyanine dyes as a membrane fluorescent biosensor on BBMV (Beck and Sacktor 1978; Cassano et al. 1988; Kragh-Hansen et al. 1982; Ries et al. 1994; Vayro and Simmons 1996; Wright et al. 1981). Some studies used extracellular pH 6.5–6.8 (Daniel et al. 1991; Kottra et al. 2013) similar to the physiological level to create an inward H+ gradient for activating these transporters. By following these studies, the H+ gradient was created by adjusting the pH of the extravesicular and intravesicular media to 6.6 and 7.4, respectively (~ 6.7 across the membrane). This is based on the hypothesis that in these pH environments and with increasing concentration of substrates delivered to either BBMV or OMMV, the corresponding increases in the fluorescence signal (positive membrane potential difference) would result from a greater influx of protons, which would reflect the translocation of the substrates (Figs. 2, 3, 4 and 5). These changes in fluorescence are similar to those observed in the study conducted by Ries et al. (1994); however, they used a different membrane potential-sensitive dye DiS-C3-(5), and they did not isolate different regions of the proximal tubule representing PEPT1 and PEPT2 (BBMV and OMMV, respectively). Therefore, this prompted us to develop a method for measuring the membrane potential difference by DiS-C3-(3) while transporting substrates across BBMV and OMMV.
In this study, the potential application of DiS-C3-(3) dye as a biosensor for the membrane potential difference in BBMV and OMMV was validated using the following experiments: (1) investigating the addition of the extravesicular medium (pH 6.6, without substrate), which resulted in an instantaneous decrease in fluorescence intensity followed by a steady plateau (Fig. 2). This initial change in intensity is likely due to the perturbation of the sample by the addition of the medium (Ries et al. 1994), as when larger volumes were added a larger negative deflection was observed (results not shown). The resulting plateau indicates that there were no changes in the membrane potential and hence no transport occurred across the membrane for the control samples (Fig. 2); (2) investigating the addition of the extravesicular medium (pH 6.6) containing Gly-Gln to the same vesicles, which resulted in the same decrease as in the control ones, but followed by an increase in the fluorescence signal which then reached plateau. This increase in fluorescence intensity indicated depolarisation of the membrane potential, which is most likely due to the translocation of the substrates with H+ across the membrane (Fig. 2) (Ries et al. 1994).
Chen et al. (1999) demonstrated that although PEPT1 and PEPT2 showed high sequence homology (approx. 50%), there were considerable differences in terms of substrate affinity, stoichiometry and effects of depolarisation and hyperpolarisation. They demonstrated that PEPT2 can be inactivated by either increasing the pH or hyperpolarisation. Another study conducted by Daniel et al. (1991) used similar vesicle preparations isolated from the brush border membrane of the kidney and investigated the transport of just two concentrations of Gly-Gln 0.1 μM and 1 mM as a function of pH gradients. They showed that Gly-Gln transport depends on the presence of a transmembrane pH gradient, although the high-affinity transporter PEPT2 was significantly more sensitive to pH than the low-affinity transporter PEPT1. In this study, BBMV and OMMV represent S1 and S3 of the proximal tubule, respectively (where PEPT1 and PEPT2 are, respectively, located), and this heterogeneous distribution of these transporters was confirmed by Western blot (Fig. 1) (Shen et al. 1999). At pH 6.6, both BBMV and OMMV demonstrated a change in membrane potential difference, which is likely to be due to the transport of the substrate across the membrane. The physiological pH level in S3 was measured to be 6.7–6.8 ((Vieira and Malnic 1968), where NHE3 is highly active to acidify the lumen (Daniel and Kottra 2004), so the nature of these transporters requires such environment. This can also give valuable insights regarding the differences between two important regions of the kidney in terms of small peptide handling and pharmacokinetics at different pH values.
In our experiments, different concentrations of small peptides containing 2-3 amino acids and selected peptidomimetic drugs were delivered to BBMV and OMMV pre-equilibrated with the extravesicular buffer and DiS-C3-(3) dye at pH 6.6. This aimed to investigate the kinetic transport parameters (K m and V max) in two important regions of the renal proximal tubule (S1 and S2) using DiS-C3-(3) dye. When the buffer (pH 6.6) containing the substrates was added to the vesicles (BBMV or OMMV) pre-equilibrated with DiS-C3-(3) dye and the signal corrected for the addition of buffer (control), the fluorescence intensity increased indicating depolarisation change of the membrane potential, which is therefore most likely due to the translocation of the substrates with H+ across the membrane (from Figs. 3, 4 and 5).
PEPT1 and PEPT2 cotransporters are heterogeneously distributed in the rat kidney, suggesting a sequential process in the flux of peptides and peptide-like drugs in the proximal tubule of the nephron, initially by a low-affinity/high-capacity cotransporter, followed by a high-affinity/low-capacity cotransporter. Since PEPT2 was found in larger abundance than PEPT1 in the kidney (Leibach and Ganapathy 1996; Smith et al. 1998), it was expected that peptides and peptidomimetic drugs are predominately transported by PEPT2 (Shen et al. 1999). This assumption is supported by PEPT2 knockout mouse studies showing that PEPT2 protein is responsible for transporting about 85% of dipeptides (Daniel and Rubio-Aliaga 2003; Ocheltree et al. 2005) and about 95% of cefadroxil (Shen et al. 2007). In most cases, PEPT2 demonstrates higher affinity than PEPT1 in transporting peptidomimetic drugs such as β-lactam antibiotics, which contain an α-amino group and a p-hydroxyphenyl group in their chemical configuration, at therapeutic concentrations (Inui et al. 2000; Takahashi et al. 1998). This is in agreement with our findings that OMMV (where PEPT2 is located) have a higher affinity for most substrates compared to BBMV (PEPT1), with cefadroxil having the highest affinity (Table 1). This value is comparable and in a good correlation with previous studies reporting that cefadroxil had a very high affinity for PEPT2 in the transfected cell line LLC-PK1 (Terada et al. 1997) and to the native PEPT2 in BBMV isolated from rat kidneys (Inui et al. 2000; Ries et al. 1994; Takahashi et al. 1998) where the transported K m and K i values were around 3 µM. Valacyclovir had the second highest affinity in OMMV (Table 1), and when comparing it with cefadroxil, the former contains an α-amino group and a p-hydroxyphenyl group, while the latter contains just an α-amino group. In contrast, δ-amino-levulinic acid, which does not contain these groups, showed the lowest affinity in OMMV (Table 1). These results are in good agreement with the literature (Brandsch et al. 2008), confirming that these functional groups in the chemical structure can play an important role in the recognition of substrates by PEPT2. Also, it suggests that S3 is the predominant region for transporting these substrates at low therapeutic concentration while competing with the hydrolysed small peptides in the kidney.
On the other hand, in OMMV the transport of Gly-His (a positively charged dipeptide) demonstrated significantly higher affinity than Gly-Gln (a neutral dipeptide) and Gly-Gly-His (a tripeptide), but showed significantly higher capacity for Gly-Gly-His (Table 1). Although the transport of Gly-Gln by OMMV was significantly higher in affinity and capacity than BBMV, no significant changes in affinity or capacity were observed between BBMV and OMMV for Gly-His (Table 1). This could be explained by the charge-to-peptide stoichiometry of PEPT1 for acidic and neutral peptides, which is 1:1, and its preference for positively charged dipeptides (Brandsch et al. 2008; Steel et al. 1997), while the proton-to-substrate stoichiometry of PEPT2 for neutral peptides is 2:1 (Chen et al. 1999). The extracellular pH plays a substantial role in increasing the affinity of both anionic and cationic compounds, such that decreasing the extracellular pH increases the affinity of anionic and neutral compounds, whereas increasing extracellular pH decreases the affinity of the cationic ones (Amasheh et al. 1997). It is clear that changing the pH and peptide charge can play a substantial role in determining the transport by PEPT1 and PEPT2. Therefore, one explanation of the higher transport affinity and capacity of Gly-Gln (neutral dipeptide) by OMMV (Table 1) is that the proton-to-substrate stoichiometry is 2:1, and also that the positively charged dipeptide can increase the affinity and capacity of these transporters at physiological pH.
In this study, we have measured the transport kinetics of neutral and positively charged small peptides and selected peptidomimetic drugs delivered to BBMV and OMMV using the membrane potential difference-sensitive dye DiS-C3-(3). This is the first report to infer the relative contribution of the S1 and S3 segments from the renal proximal tubule (which are represented by BBMV and OMMV containing PEPT1 and PEPT2 cotransporters, respectively) to the tubular reabsorption of these substrates in the kidney. These findings could provide valuable insights regarding the transport efficiency between these different substrates and between PEPT1 and PEPT2 in handling nutrients and peptide-like drugs. This could be of importance when considering substrate or drug distribution in the body.
References
Alghamdi OA, King N (2012) Novel application of the dye, DiS-C3-(3) as a biosensor of the renal membrane potential difference. Int J Biosci Biochem Bioinform 9(4):282–286
Amasheh S, Wenzel U, Boll M, Dorn D, Weber WM, Clauss W, Daniel H (1997) Transport of charged dipeptides by the intestinal H+/peptide symporter PepT1 expressed in Xenopus laevis oocytes. J Membr Biol 155(3):247–256
Anderson CM, Thwaites DT (2010) Hijacking solute carriers for proton-coupled drug transport. Physiology 25(6):364–377. doi:10.1152/physiol.00027.2010 (Bethesda, MD)
Beck JC, Sacktor B (1978) Membrane potential-sensitive fluorescence changes during Na+-dependent d-glucose transport in renal brush border membrane vesicles. J Biol Chem 253(20):7158
Biber J, Stieger B, Haase W, Murer H (1981) A high yield preparation for rat kidney brush border membranes. Different behaviour of lysosomal markers. Biochem Biophys Acta 647(2):169–176
Blostein R (1999) Structure-function studies of the sodium pump. Biochem Cell Biol 77(1):1–10. doi:10.1139/o99-018
Brandsch M, Knutter I, Bosse-Doenecke E (2008) Pharmaceutical and pharmacological importance of peptide transporters. J Pharm Pharmacol 60(5):543–585. doi:10.1211/jpp.60.5.0002
Brown CD, King N, Simmons NL (1993) Co-expression of an anion conductance pathway with Na(+)-glucose cotransport in rat renal brush-border membrane vesicles. Pflugers Arch 423(5–6):406–410
Cassano G, Maffia M, Vilella Storelli C (1988) Effects of membrane potential on Na Cotransporters in eel intestinal brush-border membrane vesicles: studies with fluorescent dye. J Membr Biol 101:225–236
Chen XZ, Zhu T, Smith DE, Hediger MA (1999) Stoichiometry and kinetics of the high-affinity H+-coupled peptide transporter PepT2. J Biol Chem 274(5):2773–2779
Daniel H, Kottra G (2004) The proton oligopeptide cotransporter family SLC15 in physiology and pharmacology. Pflugers Arch 447(5):610–618. doi:10.1007/s00424-003-1101-4
Daniel H, Rubio-Aliaga I (2003) An update on renal peptide transporters. Am J Physiol Ren Physiol 284(5):F885–F892. doi:10.1152/ajprenal.00123.2002
Daniel H, Morse EL, Adibi SA (1991) The high and low affinity transport systems for dipeptides in kidney brush border membrane respond differently to alterations in pH gradient and membrane potential. J Biol Chem 266(30):19917–19924
Donowitz M, Emmer E, McCullen J, Reinlib L, Cohen ME, Rood RP, Madara J, Sharp GW, Murer H, Malmstrom K (1987) Freeze-thaw and high-voltage discharge allow macromolecule uptake into ileal brush-border vesicles. Am J Physiol 252(6 Pt 1):G723–G735
Faller LD (2008) Mechanistic studies of sodium pump. Arch Biochem Biophys 476(1):12–21. doi:10.1016/j.abb.2008.05.017
Inui K, Terada T, Masuda S, Saito H (2000) Physiological and pharmacological implications of peptide transporters, PEPT1 and PEPT2. Nephrol Dial Transplant 15(Suppl 6):11–13
Jorgensen P (1986) Structure, function and regulation of Na, K-ATPase in the kidney. Kidney Int 29(1):10–20
Kaur J, Bachhawat AK (2009) A modified Western blot protocol for enhanced sensitivity in the detection of a membrane protein. Anal Biochem 384(2):348–349. doi:10.1016/j.ab.2008.10.005
Kottra G, Spanier B, Verri T, Daniel H (2013) Peptide transporter isoforms are discriminated by the fluorophore-conjugated dipeptides beta-Ala- and d-Ala-Lys-N-7-amino-4-methylcoumarin-3-acetic acid. Physiol Rep 1(7):e00165. doi:10.1002/phy2.165
Kragh-Hansen U, Sheikh MI (1984) Serine uptake by luminal and basolateral membrane vesicles from rabbit kidney. J Physiol 354:55–67
Kragh-Hansen U, Jorgensen KE, Sheikh MI (1982) The use of potential-sensitive cyanine dye for studying ion-dependent electrogenic renal transport of organic solutes. Spectrophotometric measurements. Biochem J 208(2):359–368
Leibach FH, Ganapathy V (1996) Peptide transporters in the intestine and the kidney. Annu Rev Nutr 16:99–119. doi:10.1146/annurev.nu.16.070196.000531
Ocheltree SM, Shen H, Hu Y, Keep RF, Smith DE (2005) Role and relevance of peptide transporter 2 (PEPT2) in the kidney and choroid plexus: in vivo studies with glycylsarcosine in wild-type and PEPT2 knockout mice. J Pharmacol Exp Ther 315(1):240–247. doi:10.1124/jpet.105.089359
Plášek J, Dale RE, Sigler K, Laskay G (1994) Transmembrane potentials in cells: a diS-C3(3) assay for relative potentials as an indicator of real changes. Biochem Biophys Acta 1196:181–190
Ries M, Wenzel U, Daniel H (1994) Transport of cefadroxil in rat kidney brush-border membranes is mediated by two electrogenic H+-coupled systems. J Pharmacol Exp Ther 271(3):1327–1333
Rubio-Aliaga I, Daniel H (2008) Peptide transporters and their roles in physiological processes and drug disposition. Xenobiotica 38(7–8):1022–1042. doi:10.1080/00498250701875254
Shen H, Smith DE, Yang T, Huang YG, Schnermann JB, Brosius FC III (1999) Localization of PEPT1 and PEPT2 proton-coupled oligopeptide transporter mRNA and protein in rat kidney. Am J Physiol 276(5):F658–F665
Shen H, Ocheltree SM, Hu Y, Keep RF, Smith DE (2007) Impact of genetic knockout of PEPT2 on cefadroxil pharmacokinetics, renal tubular reabsorption, and brain penetration in mice. Drug Metab Dispos 35(7):1209–1216. doi:10.1124/dmd.107.015263
Smith DE, Pavlova A, Berger UV, Hediger MA, Yang T, Huang YG, Schnermann JB (1998) Tubular localization and tissue distribution of peptide transporters in rat kidney. Pharm Res 15(8):1244–1249
Steel A, Nussberger S, Romero M, Boron W, Boyd C, Hediger M (1997) Stoichiometry and pH dependence of the rabbit proton-dependent oligopeptide transporter PepT1. J Physiol 498(Pt 3):563
Takahashi K, Nakamura N, Terada T, Okano T, Futami T, Saito H, Inui KI (1998) Interaction of beta-lactam antibiotics with H+/peptide cotransporters in rat renal brush-border membranes. J Pharmacol Exp Ther 286(2):1037–1042
Terada T, Saito H, Mukai M, Inui K (1997) Recognition of beta-lactam antibiotics by rat peptide transporters, PEPT1 and PEPT2, in LLC-PK1 cells. Am J Physiol 273(5 Pt 2):F706–F711
Vayro S, Simmons NL (1996) An effect of Ca2+ on the Intrinsic Cl(-)-conductance of rat kidney cortex brush border membrane vesicles. J Membr Biol 150(2):163–173
Vieira F, Malnic G (1968) Hydrogen ion secretion by rat renal cortical tubules as studied by an antimony microelectrode. Am J Physiol 214(4):710–718
Wright SH, Krasne S, Kippen I, Wright EM (1981) Na+-dependent transport of tricarboxylic acid cycle intermediates by renal brush border membranes. Effects on fluorescence of a potential-sensitive cyanine dye. Biochem Biophys Acta 640(3):767–778
Acknowledgements
This work was supported by the Saudi Ministry of Higher Education and University of New England. We would like to thank Mr. Brian Cross and Mr. Jonathon Clay for their excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Apart from the funding sources (listed on the title page), the authors declare that they have no other conflicts of interest.
Rights and permissions
About this article
Cite this article
Alghamdi, O.A., King, N., Jones, G.L. et al. Kinetic Measurements of Di- and Tripeptide and Peptidomimetic Drug Transport in Different Kidney Regions Using the Fluorescent Membrane Potential-Sensitive Dye, DiS-C3-(3). J Membrane Biol 250, 641–649 (2017). https://doi.org/10.1007/s00232-017-9990-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00232-017-9990-x