Abstract
Bystander effect, a known phenomenon in radiation biology, where irradiated cells release signals which cause damage to nearby, unirradiated cells, has not been explored in electroporated cells yet. Therefore, our aim was to determine whether bystander effect is present in electroporated melanoma cells in vitro, by determining viability of non-electroporated cells exposed to medium from electroporated cells and by the release of microvesicles as potential indicators of the bystander effect. Here, we demonstrated that electroporation of cells induces bystander effect: Cells exposed to electric pulses mediated their damage to the non-electroporated cells, thus decreasing cell viability. We have shown that shedding microvesicles may be one of the ways used by the cells to mediate the death signals to the neighboring cells. The murine melanoma B16F1 cell line was found to be more electrosensitive and thus more prone to bystander effect than the canine melanoma CMeC-1 cell line. In B16F1 cell line, bystander effect was present above the level of electropermeabilization of the cells, with the threshold at 800 V/cm. Furthermore, with increasing electric field intensities and the number of pulses, the bystander effect also increased. In conclusion, electroporation can induce bystander effect which may be mediated by microvesicles, and depends on pulse amplitude, repetition frequency and cell type.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ionizing radiation causes oxidation of the molecules in the irradiated cells. This can further lead to cell death, carcinogenesis and mutation, which are the main biological effects of radiation (Hall and Giaccia 2006). In the recent years, it has been discovered that the unirradiated cells in the vicinity of the irradiated cells also express biological changes, typical for irradiation exposure. This phenomenon was termed bystander effect and is thought to be the result of signals received from nearby irradiated cells (Hall and Giaccia 2006). It was first described by Nagasawa and Little (1992) who observed biological damage in a higher number of cells irradiated by low-dose alpha particles than would be expected if only the cells hit by alpha particles were damaged. The damage in the unirradiated cells consists of telomere aberrations, DNA damage and cell death (Hall and Giaccia 2006). Signals which cause damage of the neighboring cells can be released either through gap junctions (Azzam et al. 1998) or as extracellular soluble substrates (Mothersill and Seymour 1998) and may be in the form of soluble substrates, such as reactive oxygen species (Klammer et al. 2015) and cytokines (Hei et al. 2008), or they may travel to the bystander cells via microvesicles (Kumar Jella et al. 2014). Microvesicles are extracellular fragments of cell membrane containing different proteins, RNA molecules and other agents, which can influence various signaling pathways in the target cells, including pathways leading to oncogenesis, cell death or activation of the immune response (Al-Mayah et al. 2012; Kumar Jella et al. 2014).
In radiation therapy, bystander effect is gaining increasing attention, due to its spatial potentiation of the local tumor response, as well as the increase in normal tissue damage (Baskar 2010; Hatzi et al. 2015). Furthermore, it may indirectly (by the involvement of the immune response) negatively influence the growth of distant tumors (Marín et al. 2015; Deng et al. 2016).
Bystander effect was also implicated in therapy with chemotherapeutic agents (Gorman et al. 2009; Marín et al. 2015). Therefore, the contribution of bystander effect, in addition to radiation therapy, is possible also with other ablative therapies. One of them is electrochemotherapy (Yarmush et al. 2014) which combines the use of chemotherapeutic drugs (bleomycin or cisplatin) with the application of electric pulses (electroporation) to the tumors, to increase drug delivery to the tumor cells (Rols 2006; Orlowski et al. 1988; Mir et al. 1991; Heller et al. 1997). Electroporation, in this case, is a drug delivery system, inducing short-lasting reversible structural changes in the cell membrane, but it does not itself induce cell death (i.e., reversible electroporation). Reversible electroporation can also be used for the delivery of nucleic acid molecules in gene therapy (gene electrotransfer) (Neumann et al. 1982; Yarmush et al. 2014). Exposure of the cells to longer trains of pulses leads to irreversible damage to the cell membrane and causes cell death. Irreversible electroporation can also be used in the treatment of tumors (Davalos et al. 2005; Miller et al. 2005; Edd et al. 2006; Kos et al. 2015).
Bystander effect in electroporated cells has not been explored yet. It may have implication on the therapeutic effectiveness of electrochemotherapy, irreversible electroporation as well as on gene electrotransfer. Therefore, our aim was to determine whether bystander effect is present in electroporated melanoma cells in vitro, as measured by cell viability and release of microvesicles as potential indicators of the bystander effect.
Materials and Methods
Cell Lines
Cell lines were cultured at 37 °C in a 5 % CO2 humidified atmosphere. Canine malignant melanoma cell line CMeC-1 [obtained as a kind gift from Inoue et al. (2004)] was cultured in RPMI 1460 medium (Gibco, Thermo Fisher Scientific, MA, USA). Murine malignant melanoma cell line B16F1 (American Type Culture Collection, Manassas, VA, USA) was cultured in Advanced Minimum Essential Medium (AMEM, Gibco, Thermo Fisher Scientific). Both media were supplemented with 5 % fetal bovine serum (FBS, Thermo Fisher Scientific), 10 mM/l l-glutamine (Thermo Fisher Scientific), 100 U/ml penicillin (Grünenthal, Aachen, Germany) and 50 mg/ml gentamicin (Krka, Novo Mesto, Slovenia).
Cell Irradiation
After trypsinization, 2 × 105 cells were plated on 6-cm Petri dishes and incubated for 5 h. Cells were irradiated with 0.5, 2 and 5 Gy at the dose rate 1 Gy/min using Gulmay Medical System Darpac 3300 X-ray unit (Gulmay Medical Ltd, Shepperton, UK) with a filter consisting of Cu thickness of 0.55 mm and Al thickness of 1.8 mm.
Electroporation
After trypsinization, the cells were resuspended in ice-cold electroporation buffer (EP buffer; 125 mM sucrose, 10 mM K2HPO4, 2.5 mM KH2PO4, 2 mM MgCl2 × 6H2O), the use of which prevents cell death during electroporation (Potter and Heller 2003). For electroporation, 1 × 106 cells in 50 µl (a mixture of 10 µl of endotoxin-free water and 40 µl of cell suspension in EP buffer) were placed between two parallel stainless steel plate electrodes with 2-mm gap in between and exposed to electroporation pulses generated by the electric pulse generator GT-01 (Faculty of Electrical Engineering, University of Ljubljana, Slovenia) or ELECTRO cell B10 HVLV (Leroy Biotech, Saint-Orens-de-Gameville, France). For reversible electroporation, eight square wave pulses with amplitude over distance ratio (electric field intensity) from 400 to 1600 V/cm, duration 100 µs and frequency 1 Hz were applied. For irreversible electroporation, 80 square wave pulses with electric field intensity 1300 V/cm, duration 100 µs and frequency 1 Hz were applied.
Evaluation of Bystander Effect
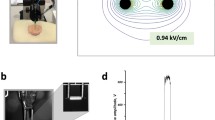
Bystander effect was evaluated by medium transfer method first described by Mothersill and Seymour (1997) (Fig. 1). Irradiated-cell conditioned medium (ICCM) and electroporated-cell conditioned medium (ECCM) were harvested 5 h after irradiation or electroporation. Cells, dead cells and cellular debris which are normally found in cell conditioned media were removed from the ICCM or ECCM by means of differential ultracentrifugation. Briefly, both conditioned media were centrifuged first at 300×g for 10 min, then at 500×g for 10 min and lastly at 1000×g for 20 min (as described in Bobrie et al. 2012; Colombo et al. 2014). To evaluate the presence of bystander effect in untreated cells exposed to either ICCM or ECCM, 2 × 104 cells per well were plated in a 96-well microtiter plate and incubated for 24 h. Then, the cell medium was aspirated from the wells and conditioned media were added to the wells for 24 h. To determine the bystander effect, cell viability was measured by the addition of 10 µl of Presto Blue reagent (Thermo Fisher Scientific) per well. Fluorescence intensity was measured after 1 h according to manufacturer’s recommendations using a fluorescence microplate reader (Tecan, Männedorf, Switzerland).
Evaluation of Cell Electrosensitivity
Cell electrosensitivity was evaluated by plating the cells in 96-well microtiter plate immediately after the electroporation, incubating them for 52 h and performing the Presto Blue assay as described above.
Clonogenic Assay
The ICCM and the ECCM of the cells exposed to electric field intensities of 1000, 1200 and 1400 V/cm were harvested 5 h after the electroporation. The control cells were plated in 6-cm Petri dishes in 4 ml of the harvested ECCM at a density of 200 cells per Petri dish. After 5 (for CMeC-1) or 6 (for B16F1) days, when the colonies were formed (groups of 50 cells were considered a colony), they were stained with crystal violet solution (Sigma-Aldrich, St. Louis, MO, USA) and counted. The plating efficiency and surviving fraction were calculated. Plating efficiency is defined by the ratio of the number of colonies to the number of cells plated and the surviving fraction as the number of colonies that form after the treatment (Franken et al. 2006).
Cell Electropermeability
Cell electropermeability was measured using propidium iodide (PI) uptake measurement. The cells were prepared for electroporation as described above. Prior to electroporation, 7.5 µl of 100 µM PI (Sigma-Aldrich, St. Louis, MO, USA) was added to 67.5 µl cell suspension, and then, the cells were immediately exposed to electric pulses as described above. After electroporation, the cells were incubated at room temperature for 5 min. Then, 25 µl of the cell suspension was resuspended in 1 ml 0.01 M phosphate buffered saline (PBS) and PI uptake was measured immediately by FACSCanto II flow cytometer (BD Biosciences). Fluorescence was detected with the bandpass filters 488/10 for forward and side scatter (FSC and SSC) and 585/42 for PI.
Measurement of Microvesicles
The amount of microvesicles in the ECCM was measured using flow cytometric measurements. Data acquisition and analysis were performed by the FACSCanto 10c flow cytometer (BD Biosciences) equipped with a high-power (20 mW) 488-nm laser. The presence of particles was determined by FSC/SSC parameter (bandpass filters 488/10), set at logarithmic gain. The FS threshold was set to 400, and the SS threshold was set to 200. At least 20,000 events were recorded for each sample analysis. Calibrating beads (Flow-Count Fluorospheres, Beckmann Coulter) of 10 μm size and known concentration (1 × 106 beads/ml) were used to determine the amount of microvesicles in the sample. The results are given by the ratio between the number of events corresponding to microvesicles and the number of events corresponding to beads.
Statistical Analysis
Statistical analysis and graphical presentation were performed using SigmaPlot Software (Systat Software, London, UK). The arithmetic mean (AM) and standard error of the mean (SEM) were calculated for all the experimental groups. The data of the experimental groups were normalized to the control groups. Statistically significant differences between experimental groups were determined using one-way analysis of variance (one-way ANOVA) followed by a Holm–Sidak test. The difference between experimental groups was considered significant if the p value was less than 0.05.
Results
Evaluation of Bystander Effect After Irradiation
The exposure to the ICCM obtained from cells irradiated with graded X-ray doses (0.5–5 Gy) significantly reduced the reproductive viability of untreated CMeC-1 cells to 82.0–67.8 % and the reproductive viability of B16F1 cells to 86.9–64.5 %, in comparison with the viability of the control cells (Fig. 2a). The amount of microvesicles in the ICCM after irradiation increased by 5.8–52.1 % for CMeC-1 cells and by 9.8–17.2 % for B16F1 cells, compared to the control media. Exposure of the untreated CMeC-1 cells to ICCM, obtained from cells irradiated with 5 Gy, resulted in a significant increase in formation of microvesicles (Fig. 2b).
Survival fraction of CMeC-1 and B16F1 cells after exposure to irradiated-cell conditioned medium obtained from cells irradiated with graded X-ray doses (IR dose) (a) and the amount of microvesicles in the medium of CMeC-1 and B16F1 cells after irradiation (b). The data are normalized to the pertinent control group. Data represent AM ± SEM of at least three independent experiments. *p < 0.05 compared to the pertinent control group. The dashed line represents the relative amount of microvesicles in the control medium
Electrosensitivity of CMeC-1 and B16F1 Cells
Viability of CMeC-1 cells was not affected after exposure to increasing amplitudes of electric pulses (Fig. 3a), whereas viability of B16F1 cells was reduced to 73.8–85.4 % of the control cells, after reversible electroporation at the higher electric field intensities (above 800 V/cm). At 1600 V/cm, the decrease in cell viability was statistically significant (Fig. 3a). After exposure to a higher number of electric pulses (80 pulses), irreversible electroporation significantly decreased viability to 48.5 ± 6.7 % for CMeC-1 cells and to 9.9 ± 5.2 % for B16F1 cells (Fig. 3b), showing that B16F1 cells were more electrosensitive than CMeC-1 cells.
Electropermeability of CMeC-1 and B16F1 Cells
The increase in uptake of PI after the electroporation was used as an indicator of electropermeability of the cells. The threshold of 50 % electropermeabilization for CMeC-1 cells was reached at electric field intensity of 1400 V/cm, whereas for B16F1 cells this threshold was at the electric field intensity of 1200 V/cm. Furthermore, the electropermeabilization at the highest electric field intensity (1600 V/cm) was only 68.9 ± 6.3 % in CMeC-1 cells and 94.3 ± 3.6 % in B16F1 cells (Fig. 4). These results prove that B16F1 cell line was more electropermeable than CMeC-1 cell line.
Formation of Microvesicles
The amount of microvesicles in the ECCM as measured by flow cytometry did not significantly differ from the control cell medium after reversible or irreversible electroporation of CMeC-1 cells (Fig. 5a). On the contrary, the amount of microvesicles in ECCM after reversible electroporation of B16F1 cells was increasing with higher electric field intensities. Also, the amount of microvesicles in the ECCM after irreversible electroporation of B16F1 cells was significantly increased to 345.5 ± 42.3 % of the control (Fig. 5b). These results show that after electroporation, B16F1 cells produced more microvesicles compared to the CMeC-1 cells.
Amount of microvesicles in the medium of CMeC-1 and B16F1 cells exposed to reversible (a) or irreversible electroporation (b) normalized to the pertinent control group. The data represent AM ± SEM of at least three independent experiments. *p < 0.05 compared to the pertinent control group. The dashed lines represent the relative amount of microvesicles in the control media
Evaluation of Bystander Effect After Electroporation
Bystander effect was evaluated by viability assay and by clonogenic assay. After exposure of the non-treated cells to the ECCM for 24 h, reversible electroporation did not affect viability of the CMeC-1 cells. In the B16F1 cells, the viability was non-significantly reduced to 84.4–91.9 % (Fig. 6a). In addition, the ECCM of irreversible electroporation slightly and non-significantly decreased the viability of the CMeC-1 cells to 98.1 ± 3.1 %, but on the contrary, the viability of B16F1 cells was significantly reduced to 84.7 ± 3.0 % (Fig. 6b).
Viability of CMeC-1 and B16F1 cells after exposure to electroporated-cell conditioned medium (ECCM) of reversible electroporation (a) and irreversible eletroporation (b) normalized to the pertinent control group. The data represent AM ± SEM of three independent experiments. *p < 0.05 compared to the pertinent control group
Secondly, the reproductive viability of CMeC-1 and B16F1 cells was evaluated by clonogenic assay. Although the ECCM of reversible electroporation decreased the survival fraction of both cell lines to 90 %, the significance level was reached only in B16F1 cells, due to the smaller variability in the results (Fig. 7). These results prove that bystander effect is present after electroporation of B16F1 cells with a threshold at 800 V/cm, but not after electroporation of CMeC-1 cell line.
Survival fraction of CMeC-1 (a) and B16F1 (b) cells after exposure to electroporated-cell conditioned medium (ECCM) of reversible electroporation normalized to the control groups. The data represent AM ± SEM of three independent experiments. *p < 0.05 compared to the pertinent control group. Representative images of colonies of CMeC-1 and B16F1 cells exposed to control medium (control) and to ECCM (ECCM 1400 V/cm) (c)
Discussion
This study demonstrates that electroporation of cells can induce bystander effect. Cells exposed to electric pulses can mediate signal to the non-electroporated cells, thus reducing the viability of the non-treated cells. We have shown that microvesicle shedding may be one of the ways used by the cells to mediate the death signals to the neighboring cells. In this study, we have also shown that the occurrence of bystander effect depends on the cell line; the murine melanoma B16F1 cell line was more electrosensitive and thus more prone to bystander effect than the canine melanoma CMeC-1 cell line. In B16F1 cell line, bystander effect was present at the level of electropermeabilization of the cells, with the threshold at 800 V/cm. Furthermore, with increasing electric field intensities and the increase in the number of pulses, the bystander effect was more pronounced.
The determination of bystander effect in our study was performed using medium transfer method, which was first described by Mothersill and Seymour in 1997 and has since been used as one of the standard methods in a number of studies describing radiation-induced bystander effect (Hei et al. 2008; Yang et al. 2005; Baskar 2010). In this study, we have tested this method on two different tumor cell lines. After obtaining positive results, showing the presence of bystander effect after irradiation of cells, we used this method to evaluate bystander effect after electroporation.
It has already been shown that non-targeted effects of irradiation may be mediated by several different factors released by the irradiated cells, for example by reactive oxygen species or cytokines and also by the release of microvesicles (Klammer et al. 2015; Hei et al. 2008; Kumar Jella et al. 2014; Al-Mayah et al. 2012). Furthermore, the importance of extracellular microvesicles in cancer treatment is gaining recognition as there is emerging evidence of their role in intercellular communication through which they influence the functioning of the non-targeted cells (El-Andaloussi et al. 2013). The mechanism of the formation of extracellular vesicles is not yet clearly understood, but it is thought that several different mechanisms, such as endosomal sorting complex required for transport (ESCRT) machinery, are involved, which contribute to the specific composition of the vesicles (Ogorevc et al. 2013; El-Andaloussi et al. 2013; Bobrie et al. 2011). There is also the increasing number of studies describing the mechanisms of microvesicles’ effects as they reach the non-targeted cells. Microvesicles contain proteins and RNA molecules, which can act on the non-targeted cells and influence cell growth (Valadi et al. 2007; Skog et al. 2008) and interact with the immune system (Théry et al. 2009; Davis 2007).
In the CMeC-1 and B16F1 cell lines, we have observed the bystander effect, as the cell survival after exposure to ICCM obtained from cells irradiated with graded X-ray doses decreased. In the CMeC-1 cell line, the bystander effect was accompanied by the increased formation of microvesicles at higher doses of irradiation. However, in the B16F1 cell line, the formation of microvesicles did not increase after irradiation, which indicates that in this line, the bystander effect is mediated by mechanisms other than microvesicle shedding. Since in our and in other studies increased microvesicle formation has been observed after cell irradiation in some of the cell lines (Al-Mayah et al. 2012; Kumar Jella et al. 2014), we decided to use this parameter to further evaluate the bystander effect after electroporation.
In electroporation, the formation of extracellular microvesicles has not been studied yet; however, it has been shown that electroporation can cause intracellular vesiculation (Ben-Dov et al. 2012). We hypothesize that there might be similar mechanisms involved in the formation of extracellular microvesicles which we have observed after electroporation in this study. We obtained increasing amount of the microvesicles with the increasing electric field intensity and with the number of pulses applied. This might be due to greater impact on the cell membrane by the more intense pulse application. In our study, we measured the amount of particles smaller than 0.5 μm. Larger particles, such as dead cells and cell debris, were removed from the conditioned medium by means of differential ultracentrifugation (Bobrie et al. 2012; Colombo et al. 2014). However, we cannot exclude that a fraction of these particles was cell debris. Nevertheless, due to the time frame of the measurements, it is unlikely that the particles were apoptotic bodies.
Both ionizing radiation and electroporation can result in changes in the cell membrane structure and function (Valerie et al. 2007; Orlowski et al. 1988). Ionizing radiation causes oxidation of the plasma membrane-associated proteins which in turn leads to structural and functional changes of the cell membrane (Valerie et al. 2007). Application of electric pulses to cells causes the formation of short-lived pores in the cell membrane and increases its permeability (Orlowski et al. 1988; Son et al. 2014; Tarek 2005). Also, it has been shown that both therapies can cause vesiculation on the plasma membrane as described above.
In our study, the bystander effect and increase in the formation of microvesicles after electroporation were present only in one of the cell lines tested. The absence of the bystander effect in CMeC-1 cells could be explained by their lower electrosensitivity (Lampreht et al. 2015). Electrosensitivity of cell lines depends on several parameters, including on the cell size, shape and other intracellular physiological properties (Agarwal et al. 2007; Cemazar et al. 1998), which might be responsible for the difference in the electrosensitivity of the cell lines used in our study. In this aspect, it is important to evaluate the electroporation-induced bystander effect in other tumor cell lines.
Recently, a growing interest in bystander effect in the field of radiation therapy can be observed, due to emerging studies showing that bystander effect can cause potentiation of the local tumor response, as well as the increase in normal tissue damage (Baskar 2010; Hatzi et al. 2015). If we compare these findings in radiation therapy with electroporation-based therapies, we can speculate on the implication of bystander effect on the therapeutic effectiveness of electrochemotherapy, irreversible electroporation and on gene electrotransfer.
Some studies speculate that tumor regression can be achieved by activation of the intracellular DNA sensors by gene electrotransfer through activation of the immune response (Heller et al. 2013). Although in our study we demonstrated the presence of bystander effect in vitro, we can speculate that the same process is occurring also in vivo. Therefore, the observed phenomenon of tumor regression after DNA electrotransfer may be partly related to bystander effect, since the factors causing bystander effect may influence the tumor environment by affecting the tumor and immune cells. In this relation, the difference in the response between electrochemotherapy in immunocompetent and in immunodeficient organisms can be attributed to bystander effect, evoked by electroporation or electrochemotherapy (Sersa et al. 1997). Furthermore, this can be the starting point for the manipulation of the tumor environment by adjuvant immunotherapy or immune checkpoint inhibitors (Sersa et al. 2015; Calvet et al. 2014; Forde et al. 2014).
To conclude, we have shown that bystander effect can be present after electroporation in vitro. The electroporated cells can mediate signals to the non-electroporated cells, thus inducing a decrease in cell viability of the non-electroporated cells. We have shown that formation of extracellular microvesicles may be one of the ways used by the cells to mediate their damage to the neighboring cells. Finally, occurrence of bystander effect depends on electric field intensity, the number of electric pulses applied and also on the electrosensitivity of the cells.
References
Agarwal A, Zudans I, Weber EA, Olofsson J, Orwar O, Weber SG (2007) Effect of cell size and shape on single-cell electroporation. Anal Chem 79:3589–3596
Al-Mayah AHJ, Irons SL, Pink RC, Carter DRF, Kadhim MA (2012) Possible role of exosomes containing RNA in mediating nontargeted effect of ionizing radiation. Radiat Res 177:539–545
Azzam EI, de Toledo SM, Gooding T, Little JB (1998) Intercellular communication is involved in the bystander regulation of gene expression in human cells exposed to very low fluences of alpha particles. Radiat Res 150:497–504
Baskar R (2010) Emerging role of radiation induced bystander effects: cell communications and carcinogenesis. Genome Integr 1:13
Ben-Dov N, Rozman Grinberg I, Korenstein R (2012) Electroendocytosis is driven by the binding of electrochemically produced protons to the cell’s surface. PLoS One 7:e50299
Bobrie A, Colombo M, Raposo G, Théry C (2011) Exosome secretion: molecular mechanisms and roles in immune responses. Traffic 12:1659–1668
Bobrie A, Colombo M, Krumeich S, Raposo G, Théry C (2012) Diverse subpopulations of vesicles secreted by different intracellular mechanisms are present in exosome preparations obtained by differential ultracentrifugation. J Extracell Vesicles 1:18397
Calvet CY, Famin D, Andre FM, Mir LM (2014) Electrochemotherapy with bleomycin induces hallmarks of immunogenic cell death in murine colon cancer cells. OncoImmunology 3:e28131
Cemazar M, Jarm T, Miklavcic D, Lebar AM, Ihan A, Kopitar NA, Sersa G (1998) Effect of electric-field intensity on electropermeabilization and electrosensitivity of various tumor-cell lines in vitro. Electro Magnetobiol 17:263–272
Colombo M, Raposo G, Théry C (2014) Biogenesis, secretion, and intercellular interactions of exosomes and other extracellular vesicles. Annu Rev Cell Dev Bi 30:255–289
Davalos R, Mir LM, Rubinsky B (2005) Tissue ablation with irreversible electroporation. Ann Biomed Eng 33:223–231
Davis DM (2007) Intercellular transfer of cell-surface proteins is common and can affect many stages of an immune response. Nat Rev Immunol 7:238–243
Deng L, Liang H, Fu S, Weichselbaum RR, Fu Y (2016) From DNA damage to nucleic acid sensing: a strategy to enhance radiation therapy. Clin Cancer Res 22:20–25
Edd JF, Horowitz L, Davalos RF, Mir LM, Rubinsky B (2006) In-vivo results of a new focal tissue ablation technique: irreversible electroporation. IEEE Trans Biomed Eng 53:1409–1415
El-Andaloussi S, Mäger I, Breakefield XO, Wood MJ (2013) Extracellular vesicles: biology and emerging therapeutic opportunities. Nat Rev Drug Discov 12:347–357
Forde PF, Sadadcharam M, Hall LJ, O’Donovan TR, de Kruijf M, Byrne WL, O’Sullivan GC, Soden DM (2014) Enhancement of electroporation facilitated immunogene therapy via T-reg depletion. Cancer Gene Ther 21:349–354
Franken NAP, Rodermond HM, Stap J, Haveman J, van Bree C (2006) Clonogenic assay of cells in vitro. Nat Protoc 1:2315–2319
Gorman S, Tosetto M, Lyng F, Howe O, Sheahan K, O’Donoghue D, Hyland J, Mulcahy H, O’Sullivan J (2009) Radiation and chemotherapy bystander effects induce early genomic instability events: telomere shortening and bridge formation coupled with mitochondrial dysfunction. Mutat Res 669:131–138
Hall EJ, Giaccia AJ (2006) Radiobiology for the radiologist. Lippincott Williams & Wilkins, Philadelphia, pp 35–36
Hatzi VI, Laskaratou DA, Mavragani IV, Nikitaki Z, Mangelis A, Panayiotidis MI, Pantelias GE, Terzoudi GI, Georgakilas AG (2015) Non-targeted radiation effects in vivo: a critical glance of the future in radiobiology. Cancer Lett 356:34–42
Hei TK, Zhou H, Ivanov VN, Hong M, Lieberman HB, Brenner DJ, Amundson SA, Geard CR (2008) Mechanism of radiation-induced bystander effects: a unifying model. J Pharm Pharmacol 60:943–950
Heller R, Gilbert R, Jaroszeski MJ (1997) Electrochemotherapy: an emerging drug delivery method for the treatment of cancer. Adv Drug Deliv Rev 26:185–197
Heller L, Todorovic V, Cemazar M (2013) Electrotransfer of single-stranded or double-stranded DNA induces complete regression of palpable B16.F10 mouse melanomas. Cancer Gene Ther 20:695–700
Inoue K, Ohashi E, Kadosawa T, Hong SH, Matsunaga S, Mochizuki M, Nishimura R, Sasaki N (2004) Establishment and characterization of four canine melanoma cell lines. J Vet Med Sci 66:1437–1440
Klammer H, Mladenov E, Li F, Iliakis G (2015) Bystander effects as manifestation of intercellular communication of DNA damage and of the cellular oxidative status. Cancer Lett 356:58–71
Kos B, Voigt P, Miklavcic D, Moche M (2015) Careful treatment planning enables safe ablation of liver tumors adjacent to major blood vessels by percutaneous irreversible electroporation (IRE). Radiol Oncol 49:234–241
Kumar Jella K, Rani S, O’Driscoll L, McClean B, Byrne HJ, Lyng FM (2014) Exosomes are involved in mediating radiation induced bystander signalling in human keratinocyte cells. Radiat Res 181:138–145
Lampreht U, Kamensek U, Stimac M, Sersa G, Tozon N, Bosnjak M, Brozic A, de Sá Oliveira GG, Nakagawa T, Saeki K, Cemazar M (2015) Gene electrotransfer of canine interleukin 12 into canine melanoma cell lines. J Membr Biol 248:909–917
Marín A, Martín M, Liñán O, Alvarenga F, López M, Fernández L, Büchser D, Cerezo L (2015) Bystander effects and radiotherapy. Rep Pract Oncol Radiother 20:12–21
Miller L, Leor J, Rubinsky B (2005) Cancer cells ablation with irreversible electroporation. Technol Cancer Res Treat 4:699–706
Mir LM, Belehdradek M, Domenge C, Orlowski S, Poddevin J, Schwab G, Luboinnski B, Paoletti C (1991) Electrochemotherapy, a new antitumor treatment: first clinical trial. C R Acad Sci III Sci Vie 313:613–618
Mothersill C, Seymour C (1997) Medium from irradiated human epithelial cells but not human fibroblasts reduces the clonogenic survival of unirradiated cells. Int J Radiat Biol 71:421–427
Mothersill C, Seymour C (1998) Cell–cell contact during gamma irradiation is not required to induce a bystander effect in normal human keratinocytes: evidence for release during irradiation of a signal controlling survival into the medium. Radiat Res 149:256–262
Nagasawa H, Little JB (1992) Induction of sister chromatid exchanges by extremely low doses of α-particles. Cancer Res 52:6394–6396
Neumann E, Schaefer-Ridder M, Wang Y, Hofschneider PH (1982) Gene transfer into mouse lyoma cells by electroporation in high electrical fields. EMBO J 1:841–845
Ogorevc E, Kralj-Iglic V, Veranic P (2013) The role of extracellular vesicles in phenotypic cancer transformation. Radiol Oncol 47:197–205
Orlowski S, Behradek J Jr, Paoletti C, Mir LM (1988) Transient electropermeabilization of cells in culture. Increase in the cytotoxicity of anticancer drugs. Biochem Pharmacol 37:4724–4733
Potter H, Heller R (2003) Transfection by electroporarion. Curr Protoc Mol Biol. doi:10.1002/0471142727.mb0903s62
Rols MP (2006) Electropermeabilization, a physical method for the delivery of therapeutic molecules into cells. Biochim Biophys Acta 1758:423–428
Sersa G, Miklavcic D, Cemazar M, Belehradek J Jr, Jarm T, Mir LM (1997) Electrochemotherapy with CDDP on LPB sarcoma: comparison of the anti-tumor effectiveness in immunocompetent and immunodeficient mice. Bioelectrochem Bioenerg 43:279–283
Sersa G, Teissie J, Cemazar M, Signori E, Kamensek U, Marshall G, Miklavcic D (2015) Electrochemotherapy of tumors as in situ vaccination boosted by immunogene electrotransfer. Cancer Immunol Immunother 64:1315–1327
Skog J, Wurdinger T, van Rijn S, Meijer DH, Gainche L, Sena-Esteves M (2008) Glioblastoma microvesicles transport RNA and proteins that promote tumour growth and provide diagnostic biomarkers. Nat Cell Biol 10:1470–1476
Son RS, Smith KC, Gowrishankar TR, Vernier PT, Weaver JC (2014) Basic features of a cell electroporation model: illustrative behavior for two very different pulses. J Membr Biol 247:1209–1228
Tarek M (2005) Membrane electroporation: a molecular dynamics simulation. Biophys J 88:4045–4053
Théry C, Ostrowski M, Segura E (2009) Membrane vesicles as conveyors of immune responses. Nat Rev Immunol 9:581–593
Valadi H, Ekstrom K, Bossios A, Sjostrand M, Lee JJ, Lotvall JO (2007) Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat Cell Biol 9:654–659
Valerie K, Yacoub A, Hagan MP, Curiel DT, Fisher PB, Grant S, Dent P (2007) Radiation-induced cell signaling: inside-out and outside-in. Mol Cancer Ther 6:789–798
Yang H, Asaad N, Held KD (2005) Medium-mediated intercellular communication is involved in bystander responses of X-ray-irradiated normal human fibroblasts. Oncogene 24:2096–2103
Yarmush ML, Golberg A, Sersa G, Kotnik T, Miklavcic D (2014) Electroporation-based technologies for medicine: principles, applications, and challenges. Annu Rev Biomed Eng 16:295–320
Acknowledgments
This work was financially supported by the Slovenian Research Agency (Program No. P3-0003, Project Nos. J3-4211, J3-6793, J3-4259, J3-6796) and conducted within the scope of LEA EBAM (French-Slovenian European Associated Laboratory: Pulsed Electric Fields Applications in Biology and Medicine) and COST Action. We would also like to thank Mira Lavric (Institute of Oncology Ljubljana, Ljubljana, Slovenia) for her help with the cell culturing, Ilija Vojvodic and Alenka Vavtar (Institute of Oncology Ljubljana, Ljubljana, Slovenia) for their help with the irradiation of the cells and Andreja Brozic and Simon Bucek (Institute of Oncology Ljubljana, Ljubljana, Slovenia) for their help with flow cytometric measurements.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Prevc, A., Bedina Zavec, A., Cemazar, M. et al. Bystander Effect Induced by Electroporation is Possibly Mediated by Microvesicles and Dependent on Pulse Amplitude, Repetition Frequency and Cell Type. J Membrane Biol 249, 703–711 (2016). https://doi.org/10.1007/s00232-016-9915-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00232-016-9915-0