Abstract
Objective
Atacicept, a recombinant fusion protein, blocks the activity of BLyS (a B-lymphocyte stimulator) and APRIL (a proliferation-inducing ligand) and may be a potential treatment for B-cell-mediated diseases. This study assesses the safety, pharmacokinetics (PK) and pharmacodynamics (PD) of atacicept.
Methods
In this Phase I study, healthy male volunteers received a single subcutaneous dose of atacicept (2.1, 70, 210 or 630 mg) or placebo and were monitored over 7 weeks for injection-site pain, local tolerability, vital signs, echocardiography, haematology, coagulation, blood chemistry, serum virology, urinalysis and PK/PD markers [lymphocyte cell counts, BLyS–atacicept complex, immunoglobulin G (IgG), IgM].
Results
Atacicept was well tolerated at all doses (n = 23). There were no clinically significant changes in vital signs or laboratory parameters during the study. Treatment-emergent adverse events (AEs) were mainly mild or moderate in severity, and all were transient, resolving without any clinical sequelae. There was no evidence of any relationship between atacicept dose and the incidence of AEs. Local tolerability was good. Serum atacicept peaked 16 h after dosing, and the area under the concentration-time curve increased in an approximately dose-related manner. The 70-, 210- and 630-mg doses of atacicept demonstrated a dose-dependent biological effect on IgM levels, which was apparent up to 210 days post-dose. There were no treatment-related effects on IgG levels or lymphocyte subpopulations.
Conclusions
These results showed that single subcutaneous doses of atacicept were well tolerated in healthy volunteers, demonstrated non-linear PK and were biologically active, according to IgM levels.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Atacicept (formerly known as TACI-Ig) is a recombinant fusion protein containing the extracellular, ligand-binding portion of the transmembrane activator and CAML-interactor (TACI) receptor and the Fc portion of human immunoglobulin G (IgG) [6]. Atacicept acts as an antagonist to BLyS, a B-lymphocyte stimulator also known as BAFF [B-cell-activating factor of the tumour necrosis factor (TNF) family], and APRIL (a proliferation-inducing ligand), both of which are related members of the TNF ligand superfamily. Both BLyS and APRIL signal through TACI and BCMA (B-cell maturation antigen) receptors, and BLyS also has a high affinity for BAFF-R (BAFF receptor) [1]. In addition, APRIL can bind with low affinity to heparin-sulphate proteoglycans [8, 10]. Through binding to these receptors, BLyS and APRIL are known to regulate B-cell maturation, differentiation and survival (normal or malignant B-cells) [3, 6, 7, 12, 13]. BLyS and APRIL may also co-stimulate T-cells under certain conditions [11].
Most likely as a result of these effects on B- and T-cell function, BLyS and APRIL appear to play an important role in the development of autoimmune conditions. Transgenic mice engineered to express high levels of BLyS exhibit immune cell disorders and symptoms similar to those seen in humans with the autoimmune disorder systemic lupus erythematosus (SLE) [6] and Sjögren’s syndrome [4]. Furthermore, elevated levels of BLyS have been correlated with the onset and progression of disease in a strain of mice that spontaneously develops SLE-like symptoms [6]. Similar elevations in BLyS have been observed in humans with various autoimmune disorders, including SLE and rheumatoid arthritis (RA) [2, 15]. In addition, increased levels of both BLyS and APRIL have been observed in the arthritic joints of patients with inflammatory arthritis [14].
BLyS and APRIL have also been implicated in B-cell malignancies. Both of these molecules are expressed by malignant myeloma cells as well as by surrounding cells in the tumour environment [3]. BLyS and APRIL enhance the survival of the malignant cells via autocrine and paracrine loops [3]. Based on this evidence, agents that block the activity of BLyS and/or APRIL seem to be an attractive therapeutic approach for the treatment of autoimmune diseases and B-cell malignancies.
Preclinical studies have shown that atacicept treatment decreases levels of B-cells and antibody production, and also inhibits the development of autoimmune disease in mouse models of SLE and RA [5, 6]. Recent data have demonstrated the ability of another agent targeting BLyS and APRIL (a BCMA-Fc fusion protein, not yet in clinical development) to delay the progression of clinical symptoms in a mouse model of multiple sclerosis [9].
The purpose of this paper is to describe the results from the first Phase I study of atacicept in humans conducted as part of its clinical development programme. In this study, the systemic and local tolerability of atacicept administered as a single subcutaneous dose was assessed in healthy male volunteers. The pharmacokinetics (PK) and markers of the biological activity of atacicept were also evaluated.
Methods
This Phase I, double-blind, dose-escalating, sequential-dose study of atacicept in healthy volunteers was conducted at LCG Bioscience, Bourn, UK. The study protocol was approved by the Cambridge Local Research Ethics Committee, and the study was performed according to the principles of Good Clinical Practice and the Declaration of Helsinki. All volunteers gave written, informed consent.
Study participants
Healthy male volunteers were assessed for eligibility at a pre-study screening visit carried out within 14 days prior to the start of the study. Participants were eligible if they were aged 18–50 years, with a body weight of at least 60 kg and a body mass index (BMI) of up to 28 kg/m2. All participants were required to have vital signs within normal ranges: body temperature, 35.0–37.0°C; systolic blood pressure (BP), 90–140 mmHg at rest (supine), ≤20 mmHg drop after standing for 3 min; diastolic BP, 50–90 mmHg at rest (supine), ≤10 mmHg drop after standing for 3 min; heart rate at rest (supine), 40–90 beats per minute. To be eligible for the study, participants were required to be non-smokers and not to have smoked in the past 3 years. Participants were asked to use contraceptive methods for the duration of the study.
Owing to the expected immunosuppressant properties of atacicept, the medical history of the participant was assessed at the screening visit, paying particular attention to any previous infective episode, recent infective illnesses and/or concomitant conditions that may have affected the immune system. Volunteers were excluded from the study if they showed any clinically significant abnormalities in pre-study safety laboratory tests (taking particular care over any indicators of infective conditions).
Other exclusion criteria were: any clinically significant abnormality on the 12 leads resting electrocardiogram (ECG); history or presence of drug or alcohol abuse; positive serology results [hepatitis B surface antigen (not due to vaccination), hepatitis C virus or human immunodeficiency virus]; history or presence of hypertension or other significant cardiovascular abnormality; history or presence of kidney disease; any acute infection within the 3 weeks prior to dosing; definite or suspected personal history or family history of adverse drug reaction or hypersensitivity to drugs (particularly those with a chemical structure similar to atacicept); presence or history of any serious allergy (i.e. requiring hospitalization or systemic treatment); loss or donation of more than 400 ml of blood within 12 weeks prior to study entry; use of any prescription drugs within 2 weeks of study drug administration; use of over-the-counter medication (except multi-vitamins) within 1 week of study drug administration; immunization or immunoglobulin treatment in the 3 months before screening; administration of any investigational medicinal product within 12 weeks prior to study.
Interventions
Study participants were randomized into four groups, each containing six volunteers. In each group, one individual was randomized to receive placebo (phosphate-buffered saline) and the rest received a single subcutaneous dose of atacicept. The randomization list was generated by the study statistician on a programme developed in-house using the SAS system (SAS, Cary, N.C.). Individuals who were deemed eligible for study participation were allocated a randomization number in sequential, chronological order, immediately before dosing, according to the randomization list provided by the sponsor.
Study participants were admitted on the night before the study drug was administered. The study drug was administered the following morning after an overnight fast, and participants remained in the clinic until 24 h post-dose. The dose of atacicept was sequentially escalated from one group to the next: Group 1, 2.1 mg (equivalent to 0.03 mg/kg for a 70-kg person); Group 2, 70 mg (1 mg/kg); Group 3, 210 mg (3 mg/kg); Group 4, 630 mg (9 mg/kg). Each treatment group was dosed no less than 21 days after the previous group. Each 2.1- or 70-mg dose was administered as a single 1-ml injection, the 210-mg dose was administered as 2 × 1-ml injections, and the 630-mg dose was administered as 5 × 1-ml injections.
The original dose specified in the protocol for Group 1 was 21 mg (0.3 mg/kg) and was selected based on findings from pre-clinical studies. However, because of a dilution error, the actual dose administered was 2.1 mg (0.03 mg/kg). The local Ethics Committee was informed, and this error was not considered to adversely affect the safety of the participants.
Assessments
Demographic and medical history data were recorded at the pre-study visit. After dosing, participants were required to return to the clinic for safety assessments and for PK and pharmacodynamic (PD) blood sampling up to a final post-study visit, which took place 7 weeks ± 2 days post-dose.
Participants were monitored continuously during the study for the occurrence of adverse events (AEs), coded using the preferred terms of the Medical Dictionary for Regulatory Activities (MedDRA), noting the duration, severity and relationship to the study drug. During the 7 weeks post-dose, injection-site pain (visual analogue scale; VAS) and local tolerability were evaluated, and laboratory assessments were conducted at regular intervals.
Blood samples for PK markers (free drug and BLyS–atacicept complex) were taken at pre-dose, and at 0.5, 1, 2, 4, 6, 8, 12, 16, 24, 36, 48, 72, 120, 168, 336, 504, 672, 840, 1008 and 1176 h post-dose. Blood samples for PD markers (lymphocyte cell counts, IgG and IgM levels) were taken at pre-dose, and at 168, 336, 504, 672, 840, 1008 and 1176 h post-dose. Individuals who received atacicept and had levels of BLyS–atacicept complex above baseline (defined as pre-dose) at 7 weeks (1176 h) post-dose underwent additional PK/PD sampling (except lymphocytes) at approximately 1-month intervals. The study was unblinded prior to this extension phase of the study.
Serum concentrations of anti-atacicept binding antibodies were measured at study day 1, at 7 weeks post-dose and at the final visit.
Assays
Serum concentrations of atacicept, BLyS–atacicept complex, IgG and IgM were measured using enzyme-linked immunosorbent assays (ELISAs).
The free atacicept concentration ELISA format utilized two monoclonal antibodies to TACI-Fc5: a non-neutralizing (capture) antibody and a neutralizing (revealing) antibody, conjugated to biotin. The lower limit of quantification (LLOQ) of this assay was 15.9 ng/ml; precision, as measured by inter-assay variability, was <15%, and the accuracy was between −20 and 9.7%.
As the exact stoichiometry of the BLyS–atacicept complex is unknown, the concentration measurements are presented in units per millilitre. The BLyS–atacicept assay had a LLOQ of 2.5 U/ml; precision was <11%, and the accuracy was between −8.6 and 4.6%.
Measurements to assess IgG and IgM levels were carried out using SYNCHRON CX Systems utilizing standard clinical Ig assays.
Lymphocyte cell counts (CD5, T-cells; CD4, T-helper cells; CD8, cytotoxic T-cells; CD19, B-cells; IgD, mature B-cells; CD138, plasma cells) were measured using fluorescence-activated cell sorting (FACS).
Statistical and PK/PD analyses
All participants who received at least one dose of study drug were included in the safety population. Treatment-emergent AEs (TEAEs) were defined as those events occurring or worsening after investigational product administration until the post-study visit.
All data from all participants were included in the PK/PD analyses. Serum concentration versus time profiles and PK parameters for atacicept were computed using non-compartmental analysis (NCA) using WinNonLin software, ver. 4.1. Values below the LLOQ before the first measurable concentration were set to zero; those after the last measurable concentration were treated as missing data.
PD response was evaluated as the percentage change from baseline for IgG, IgM, immature B-cells, mature B-cells, total T-cells, T-helper cells and cytotoxic T-cells.
Results
Study participants
A total of 35 volunteers were screened, of whom 23 were eligible for inclusion in the study. The study investigator in consultation with the sponsor considered a study size of 23 to be sufficient, without affecting the outcome of the study. These 23 individuals were randomized into four groups, with six participants in each group, except for the 630 mg group (n = 5). All 23 participants completed the study, and the 19 individuals who received atacicept were asked to return for additional monthly assessments as part of the extension study. Of these, 18 individuals completed the extension phase and one participant was lost to follow-up (consent withdrawn).
All study participants were Caucasian, had a mean [standard deviation (SD)] age of 31.1 (7.3) years and a mean (SD) BMI of 24.8 (2.4) kg/m2. The four active treatment groups and placebo group were similar in terms of baseline demographic characteristics (Table 1).
Concomitant medications
Concomitant medications were taken by 11/23 participants during the 7 weeks after dosing (mostly aspirin- or paracetamol-based products) and by 15/19 participants during the extension phase.
Safety
During the main study period (7 weeks post-dose), 52 AEs were reported by 17 study participants. Of these events, 48 were TEAEs (Table 2), the majority of which were mild in severity (44/48, 92%; moderate: 4/48, 8%). All TEAEs were transient, resolving without clinical sequelae. Of the TEAEs, 16/48 (33%) were considered to be possibly related to the investigational treatment; the remainder were considered unlikely to be related (16/48; 33%) or unrelated (16/48; 33%) to the investigational treatment. Paracetamol was used to manage six of these TEAEs occurring in four individuals. The most frequent events were headache, sore throat (pharyngolaryngeal pain) and head cold (nasopharyngitis; Table 2). There was no evidence of any relationship between dose of atacicept and any AE.
During the extension period, 51 AEs were reported by 16 study participants. All 51 of these AEs were classed as mild (32/51, 63%), moderate (16/51, 31%) or severe (3/51, 6%) in intensity, were transient and resolved without any clinical sequelae. The most frequent events were headache (15 events) and head cold (8 events). All TEAEs during the extension phase were coded as being unrelated to the investigational treatment. During the main study and extension phase there were no deaths, no serious or life-threatening AEs and no withdrawals due to AEs.
Injection-site pain and local tolerability
Injection-site pain immediately after injection was reported by 16 participants. The highest VAS scores for pain were observed in the 210 mg group (55 mm) and the 630 mg group (64 mm).
Prolonged redness (mild) associated with injection was reported for all participants in the 630 mg group and for one individual in the 210 mg group. The most likely cause for the greater incidence of prolonged redness in the higher dose groups was the greater number of injections and higher injection volume compared with the 2.1 mg and 70 mg groups. Acute redness (mild) was reported in the 210 mg group (six individuals), 630 mg group (five individuals) and 70 mg group (two individuals). Moderate redness was reported by one individual in the 70 mg group. Swelling (mild) was reported by one individual in the 210 mg group. No bruising or itching was reported for any of the participants.
Laboratory assessments
During the main study, two individuals in the 70 mg group (active treatment) had a drop in BP (>20 mmHg systolic and >10 mmHg diastolic) at 1 h post-dose. Both individuals were asymptomatic and, therefore, the events were not considered to be clinically significant. Vital signs and ECG measurements for all other participants were considered to be within the normal range, or not clinically significant during the main study and the extension phase.
One individual in the 210 mg group (active treatment) showed an elevated white blood cell count and a low neutrophil count at 120 h post-dose, but both parameters returned to within the normal ranges by 168 h post-dose. Haematology and coagulation values were within the normal range, with no clinically significant changes for all other participants throughout the main study and extension phase. None of the changes in blood biochemistry that resulted in values outside the normal range were considered to be clinically significant. No participants tested positive for any of the virology tests. None of the positive urinalysis results were considered to be clinically significant.
PK analyses
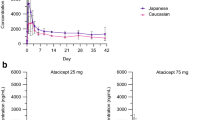
The median PK profiles for free atacicept and the BLyS–atacicept complex are given in Figs. 1 and 2. The NCA results are presented in Tables 3 and 4, respectively.
Free atacicept profiles of the participants from the lowest dose arm (2.1 mg) of the study were below or close to the limit of detection of the assay and displayed high variability. They are therefore unreliable and presented for information purposes only. This result is probably due to the fact that a significant portion of the lowest 2.1-mg dose is bound to the two atacicept ligands (BLyS and APRIL) and, therefore, is not detected by the free drug assay. The main PK evaluations are based primarily on the 70-, 210- and 630-mg dose groups.
Consistent multiphasic free drug PK profiles were observed at the different dose levels, with a fairly rapid absorption phase for this class of molecule, a distribution phase lasting 1–2 weeks and a long terminal phase. The median t max (time to maximum serum concentration) was 16 h (range: 12–36 h) for 70-, 210- and 630-mg doses (free atacicept; Table 3, Fig. 1). Increases in Cmax (maximum serum concentration) were clearly greater than dose proportional across the dose range tested, as evidenced by the increase in the dose-normalized Cmax with increasing dose, and the area under the concentration-time curve (AUC)–dose relationship also appeared to be non-linear, leading to a decrease in apparent clearance with increasing dose. The overall median terminal half-life (t ½) of atacicept was 12.4 days and increased slightly in the higher dose arms. The latter may be partly a consequence of the sampling scheme and the high proportion of terminal values below the LLOQ with the lower dose arms. The apparent clearance (CL/F) showed a tendency to decrease, from 23.2 l/day after the 70-mg dose to 14.5 l/day after the 630-mg dose.
Compared with free atacicept levels, which peaked 16 h after dosing, the BLyS–atacicept complex serum levels increased slowly after atacicept administration, peaking between 14 and 35 days after dosing (Fig. 2). The BLyS–atacicept complex serum levels persisted for significantly longer than free atacicept and were measurable for up to 210 days after dosing (versus 47 days for free atacicept). The maximum BLyS–atacicept complex serum concentrations displayed a trend towards saturation of the complex levels with increasing single doses (saturation evident at or above the 210-mg dose).
PD analyses
Despite the large variations in the median IgM change from baseline profiles, the 70-, 210- and 630-mg doses induced a reduction in IgM serum concentrations (Fig. 3), while the placebo and the 2.1-mg dose had no effect. The greatest IgM reductions of up to 23% of baseline (range: 12–25%) at 35 days post-dose were observed in the 630 mg group: after 47 days, i.e. when free atacicept serum levels were no longer quantifiable, IgM serum levels were still decreased. After 100–150 days post-administration, IgM levels recovered to within approximately 10% of baseline values.
Both the IgM drop and the duration of the effect suggested the existence of dose-dependence. To clarify this point, the AUC for the percentage decrease from baseline of IgM was calculated from the median IgM change from baseline profiles of the 70, 210 and 630 mg dose groups. Figure 4 displays the relationship between the dose level and the measure of response AUC over the first 6 months.
Relationship between the dose level and the measure of response [area under the curve (AUC) for the IgM percentage decrease from baseline was calculated from the individual IgM change from baseline profiles over 6 months]. Bars represent mean values with SE. A negative decrease represents an increase
There was no apparent effect of treatment upon IgG serum concentrations (Fig. 5). The lymphocyte counts following a single dose of atacicept also displayed highly variable profiles that made it difficult to detect emerging patterns.
Discussion
We report results from the first Phase I study to evaluate the administration of atacicept in healthy volunteers. These results showed that a single subcutaneous dose of atacicept was well tolerated by healthy male volunteers at doses of up to 630 mg. There were no clinically significant changes in the vital signs or laboratory parameters during the 7 weeks after dosing. TEAEs were mainly of mild or moderate severity, and all were transient, resolving without any clinical sequelae. There was no evidence of any relationship between atacicept dose and the incidence of AEs. Local tolerability was good, with only mild cases of redness (moderate redness was reported in one individual), one case of mild swelling, and no cases of bruising or itching. There was a greater incidence of injection-site redness in the highest two dose groups (210 and 630 mg), but this was probably related to the number and volume of injections.
Serum levels of free atacicept displayed multi-phase behaviour with fairly rapid absorption for this class of drugs (median t max approximately 16 h after dosing), distribution phase(s) lasting 1–2 weeks and a prolonged terminal phase, characterized by terminal half-lives of 2 weeks or longer. The PK of free atacicept is non-linear as characterized primarily by greater than dose-proportional increases in Cmax and AUC. Serum levels of BLyS–atacicept complex increased slowly after atacicept administration, peaking between 14 and 35 days after dosing. BLyS–atacicept complex levels close to the peak persisted for significantly longer than those for free atacicept and were measurable for up to 210 days after dosing (versus 47 days for free atacicept). The evidence of non-linearity in this PK variable was much better displayed than was the case with the free atacicept, with a trend towards saturation of the complex levels with increasing single doses being most evident at or above the 210-mg dose.
The non-linearities observed in the free atacicept and the BLyS–atacicept complex are typical for saturable binding kinetics between the drug and its ligand, BLyS. Establishing the point of binding saturation is of major importance, especially when considering dose levels and dosing frequency for multiple dosing regimens. It is clear that exceeding doses beyond the complex saturation point will bring about little benefit in terms of BLyS inhibition. Although APRIL–atacicept complexes were not measured in this study, the same rationale applies to APRIL inhibition as well. It has to be considered, however, that adequate long-term inhibition of BLyS and APRIL will be required to maintain the saturation of their binding by atacicept all the time and in all body compartments. Therefore, the dose levels and frequency design for chronic dosing should take into account the holistic dynamic complexity of pre-dose ligand homeostasis in blood and peripheral compartments, endogenous BLyS and APRIL production at various body locations, as well as the kinetic redistribution processes of both the drug and the ligands once atacicept is administered.
The three highest doses of atacicept (70, 210 and 630 mg) had a PD effect on IgM levels, which was apparent up to 210 days post-dose. In the highest dose group (630 mg), IgM levels had reduced by up to 23% of baseline at 2 weeks post-dose. This effect is consistent with the mechanism of action of atacicept in BLyS and APRIL inhibition. Therefore, even with a single dose, atacicept started displaying signs of biological activity. The fact that there were no treatment-related effects on IgG levels or lymphocyte subpopulations after a single dose may signal that further doses are required to affect those more inert biomarkers. This hypothesis will be tested in multiple-dose studies with target populations.
In conclusion, our results demonstrated that single subcutaneous doses of atacicept were well-tolerated and demonstrated biological activity in healthy volunteers, as evidenced by the PD response in IgM levels. Further investigation of atacicept for the treatment of patients with autoimmune diseases and B-cell malignancies is ongoing.
References
Bossen C, Schneider P (2006) BAFF, APRIL and their receptors: Structure, function and signaling. Semin Immunol 18:263–275
Cheema GS, Roschke V, Hilbert DM, Stohl W (2001) Elevated serum B lymphocyte stimulator levels in patients with systemic immune-based rheumatic diseases. Arthritis Rheum 44:1313–1319
Dillon SR, Gross JA, Ansell SM, Novak AJ (2006) An APRIL to remember: novel TNF ligands as therapeutic targets. Nat Rev Drug Discov 5:235–246
Groom J, Kalled SL, Cutler AH, Olson C, Woodcock SA, Schneider P, Tschopp J, Cachero TG, Batten M, Wheway J, Mauri D, Cavill D, Gordon TP, Mackay CR, Mackay F (2002) Association of BAFF/BLyS overexpression and altered B cell differentiation with Sjögren’s syndrome. J Clin Invest 109:59–68
Gross JA, Dillon SR, Mudri S, Johnston J, Littau A, Roque R, Rixon M, Schou O, Foley KP, Haugen H, McMillen S, Waggie K, Schreckhise RW, Shoemaker K, Vu T, Moore M, Grossman A, Clegg CH (2001) TACI-Ig neutralizes molecules critical for B cell development and autoimmune disease: impaired B cell maturation in mice lacking BLyS. Immunity 15:289–302
Gross JA, Johnston J, Mudri S, Enselman R, Dillon SR, Madden K, Xu W, Parrish-Novak J, Foster D, Lofton-Day C, Moore M, Littau A, Grossman A, Haugen H, Foley K, Blumberg H, Harrison K, Kindsvogel W, Clegg CH (2000) TACI and BCMA are receptors for a TNF homologue implicated in B-cell autoimmune disease. Nature 404:995–999
Hahne M, Kataoka T, Schroter M, Hofmann K, Irmler M, Bodmer JL, Schneider P, Bornand T, Holler N, French LE, Sordat B, Rimoldi D, Tschopp J (1998) APRIL, a new ligand of the tumor necrosis factor family, stimulates tumor cell growth. J Exp Med 188:1185–1190
Hendriks J, Planelles L, de Jong-Odding J, Hardenberg G, Pals ST, Hahne M, Spaargaren M, Medema JP (2005) Heparan sulfate proteoglycan binding promotes APRIL-induced tumor cell proliferation. Cell Death Differ 12:637–648
Huntington ND, Tomioka R, Clavarino C, Chow AM, Linares D, Mana P, Rossjohn J, Cachero TG, Qian F, Kalled SL, Bernard CC, Reid HH (2006) A BAFF antagonist suppresses experimental autoimmune encephalomyelitis by targeting cell-mediated and humoral immune responses. Int Immunol 18:1473–1485
Ingold K, Zumsteg A, Tardivel A, Huard B, Steiner QG, Cachero TG, Qiang F, Gorelik L, Kalled SL, Acha-Orbea H, Rennert PD, Tschopp J, Schneider P (2005) Identification of proteoglycans as the APRIL-specific binding partners. J Exp Med 201:1375–1383
Mackay F, Leung H (2006) The role of the BAFF/APRIL system on T cell function. Semin Immunol 18:284–289
Moore PA, Belvedere O, Orr A, Pieri K, LaFleur DW, Feng P, Soppet D, Charters M, Gentz R, Parmelee D, Li Y, Galperina O, Giri J, Roschke V, Nardelli B, Carrell J, Sosnovtseva S, Greenfield W, Ruben SM, Olsen HS, Fikes J, Hilbert DM (1999) BLyS: member of the tumor necrosis factor family and B lymphocyte stimulator. Science 285:260–263
Schneider P, MacKay F, Steiner V, Hofmann K, Bodmer JL, Holler N, Ambrose C, Lawton P, Bixler S, Acha-Orbea H, Valmori D, Romero P, Werner-Favre C, Zubler RH, Browning JL, Tschopp J (1999) BAFF, a novel ligand of the tumor necrosis factor family, stimulates B cell growth. J Exp Med 189:1747–1756
Tan SM, Xu D, Roschke V, Perry JW, Arkfeld DG, Ehresmann GR, Migone TS, Hilbert DM, Stohl W (2003) Local production of B lymphocyte stimulator protein and APRIL in arthritic joints of patients with inflammatory arthritis. Arthritis Rheum 48:982–992
Zhang J, Roschke V, Baker KP, Wang Z, Alarcon GS, Fessler BJ, Bastian H, Kimberly RP, Zhou T (2001) Cutting edge: a role for B lymphocyte stimulator in systemic lupus erythematosus. J Immunol 166:6–10
Acknowledgements
We would like to than Mauro Bertolino of Merck Serono for his valuable assistance in data analysis. This trial was sponsored by Merck Serono S.A. (Geneva, Switzerland), which is developing atacicept in various indications in collaboration with Zymogenetics, Inc. (Seattle, Wash., USA). The procedures in this study complied with the current laws of the country in which they were performed (UK).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Munafo, A., Priestley, A., Nestorov, I. et al. Safety, pharmacokinetics and pharmacodynamics of atacicept in healthy volunteers. Eur J Clin Pharmacol 63, 647–656 (2007). https://doi.org/10.1007/s00228-007-0311-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-007-0311-7