Abstract
Background
There are few studies describing acetaminophen (APAP) cerebrospinal fluid (CSF) concentrations in children. This current study was undertaken in children—from neonates to adolescents—in order to investigate age-related changes in the plasma to CSF equilibration half-time (Teq) of APAP.
Methods
Children (n=41) 1 week to 18 years of age undergoing (semi) elective surgery for placement or revision of a ventriculo-peritoneal shunt or insertion of a temporary external ventricular drain received a loading dose of 30–40 mg/kg APAP 1 h before scheduled surgery. Blood and CSF samples for APAP concentration analysis were collected during surgery. In those children with a temporary external drain, blood and CSF sampling were extended into the postoperative period. APAP and CSF pharmacokinetics were estimated using non-linear mixed-effects models. Size was standardized to a 70-kg person using allometric "1/4 power models".
Results
Median (25–75th percentile) age and weight of the patients included in this study were 12 months (3–62 months) and 10.0 kg (5.8–20.0 kg). Median (25–75th percentile) time between APAP loading dose administration and collection of blood samples and median time (25–75th percentile) between APAP loading dose and collection of CSF were, respectively, 125 min (95–210 min) and 133 min (33–202 min). The population mean Teq, standardized to a 70-kg person, was 1.93 h (CV 43%), an estimate similar to that described in adults (2.1 h). There was no relationship between age and Teq other than that predicted by size. APAP plasma concentrations ranged from 0.0 mg/l to 33.0 mg/l, APAP CSF concentrations ranged from 0.0 mg/l to 21.0 mg/l.
Conclusion
Size rather than blood–brain-barrier maturation determines Teq changes with age in children. We predict a neonate (3.5 kg), 1-year-old child (10 kg), 5-year-old child (20 kg), 10-year-old child (30 kg) and adult (70 kg) to have Teq values of 0.9, 1, 1.4, 1.6, and 1.93 h, respectively.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
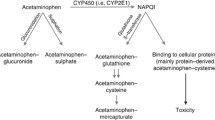
The mechanism of action of acetaminophen (APAP) analgesia is multifactorial. It is known to be a potent inhibitor of prostaglandin synthesis within the central nervous system (CNS) but also acts peripherally by blocking impulse generation within the bradykinin-sensitive chemoreceptors responsible for the generation of nociceptive impulses. APAP is also thought to have an analgesic effect by antagonising N-methyl-d-aspartate (NMDA) and substance P in the spinal cord [1, 2]. The analgesic effect involves an inhibitory action on spinal nitric oxide (NO) mechanisms [3]. APAP's antipyretic effect is mediated through inhibition of prostaglandin E2 in the brain [4]. These temporal dysequilibriums have been modeled using delayed effects with an effect compartment. The equilibration half-time between plasma and effect compartment is reported as 53 min (CV 217%) for analgesia and 71 min (CV 10%) for anti-pyresis in children (mean±SD 9.0±3.0) [5, 6].
Reduction of cerebrospinal fluid (CSF) prostaglandin concentrations in animals after APAP administration might be responsible for APAP's analgesic effect [7, 8]. Consequently, the amount of APAP reaching the CNS and causing inhibition of prostaglandin synthesis may mirror its analgesic effect. APAP CSF concentrations are dependent on APAP plasma concentrations and the permeability of the blood–brain barrier (BBB) to this molecule. Debate exists concerning BBB permeability changes with age [9]. There are few APAP CSF pharmacokinetic studies in adult humans [10, 11] and only one study in children previously reported by Anderson et al. [12]. However, seven of the nine children studied by Anderson et al. [12] suffered traumatic brain injury that may have influenced BBB permeability.
This current study was undertaken in children from neonates to adolescents in order to investigate age-related changes. The results were compared with the results of the study performed by Anderson et al. [12] to examine the influence of traumatic brain injury and its possible disruption of the BBB on the plasma–CSF equilibration half-time (Teq).
Methods
Patients and methods
After approval of the medical ethics committee of the ErasmusMC Rotterdam, informed consent was obtained from the parents of children participating in this study. Children aged between 0 years and 18 years undergoing placement or revision of a ventriculo-peritoneal (VP) shunt or insertion of a temporary external ventricular drain were considered for enrolment. Exclusion criteria were pre-existent liver- or kidney disorders, known allergy to APAP and traumatic brain injury.
All children (n=41) were given a rectal loading dose of 30–40 mg/kg APAP 1 h before scheduled surgery. Anesthesia was induced using thiopentone, propofol, etomidate or sevoflurane. Before tracheal intubation, children received 2–5 μg/kg fentanyl. Tracheal intubation was facilitated with vecuronium or suxamethonium. Breathing was controlled and anesthesia was maintained using O2/N2O or O2/air and isoflurane 0.5–1%. Before incision, children were given a further 2–5 μg/kg fentanyl. Extra doses of 2 μg/kg fentanyl were administered if heart rate and/or mean arterial blood pressure were greater than 10% above baseline values measured 10 min after tracheal intubation. A blood sample for APAP plasma concentration analysis was collected directly after induction. A CSF sample for APAP CSF concentration analysis was collected during shunt insertion or revision.
Postoperatively, patients received APAP suppositories according to hospital standard dosing schedules. CSF sampling was extended to the postoperative period in patients undergoing insertion of a temporary external ventricular drain (n=5). The sampling schedule in these patients was adjusted to the clinical circumstances of the individual patients and based on pain scores validated for this population [13].
APAP suppositories contained 60, 120, 240, 500 or 1000 mg APAP in a triglyceride base (Pharmachemie, Haarlem, The Netherlands). Loading dose (30–40 mg/kg) was dependent on available suppository size.
CSF sampling
In patients with VP shunts, it was only possible to collect a single CSF and blood sample, taken during surgery. Further CSF sampling was possible in five patients with external ventricular drains. These patients were given 45.5–108.0 mg/kg/24 h APAP rectally in divided doses, including the pre-operatively administered rectal loading dose. Plasma and CSF sampling was intermittent and varied from half hourly for 4 h to two to five hourly for 68 h.
APAP assay
Plasma and CSF samples were stored at 4°C until analysis. APAP plasma and CSF concentrations were determined using fluorescence polarization immunoassay (ADX systems, Abbott Laboratories, North Chicago, IL) (ErasmusMC Rotterdam). The APAP plasma determination limit was 1.0 mg/l, which was defined as the lowest measurable concentration which can be distinguished from zero with 95% confidence. Precision was measured at APAP plasma concentrations of 15, 35 and 150 mg/l; 55 samples of each concentration were assayed to determine coefficients of variation at these concentrations (CV=SD/mean; RSD=CV*100%). RSD at these concentrations were 7.22%, 3.37% and 3.11%, respectively. The APAP plasma concentration range in which accuracy was measured was 10–150 mg/l.
Modeling
Population parameter estimates were obtained using a non-linear mixed effects model (NONMEM) [14]. This model accounts for population parameter variability (between and within subjects) and residual variability (random effects) as well as parameter differences predicted by covariates (fixed effects). The population parameter variability in model parameters was modeled by a proportional variance model. Additive terms characterized the residual unknown variability for plasma and CSF concentrations. This error model assumes that the residual variability is of the same order of magnitude over the whole range of measurements. The population mean parameters, between subject variance and residual variance were estimated using NONMEM version V release 1.1. Estimation used the first-order conditional estimate method with the interaction option and ADVAN 6 with Tol=5. Convergence criterion was three significant digits. A FORTRAN F77 compiler (Watcom version 10.6) was used with an Intel Celeron 333 MHz CPU under MS Windows 98.
A first-order input, first-order elimination, two-compartment link model was used to describe the time course of plasma and CSF drug concentrations. The model is shown schematically in Fig. 1.
Diagram of cerebrospinal fluid (CSF) pharmacokinetic model. Ka absorption rate constant (/h), V/F central compartment volume (l), C plasma concentration (mg/l), CL/F clearance from central compartment (l/h), Ccsf cerebrospinal fluid concentration (mg/l), PC csf/plasma partition coefficient, Keq equilibration rate constant (/h). The Keq can be expressed as Ln2/Teq
The relevant differential equations were:
where Agut is the amount of drug in the gut at any one time. This amount is assumed equal to the dose at time zero. Ka is the absorption rate constant (/h); V is the central compartment volume (l); C is the plasma concentration (mg/l); CL is the clearance from the central compartment (l/h); Ccsf is the cerebrospinal fluid concentration (mg/l).
APAP is not bound to plasma proteins. Concentrations were measured in serum (containing protein that contributes to total volume) and CSF (without protein). Consequently, a partition coefficient was required to model the data. The partition coefficient estimate is similar to the alcohol partition coefficient between CSF and serum measured in rats [15] and would be predicted for drugs that distribute in plasma water but which do not bind to plasma proteins [16] because plasma water occupies 90% of plasma by volume. PC is the CSF/ plasma partition coefficient and accounts for protein concentration differences between plasma and CSF; Teq is the equilibration half time (h) between plasma and CSF.
APAP was administered as an extra vascular dose and both clearance and distribution volume is confounded by bioavailability. Frectal/oral is used to refer to the relative bioavailability of the suppository compared with the oral formulation.
Children with traumatic brain injury
Plasma and CSF time–concentration data from nine children with external ventricular shunts, originating from the study published by Anderson et al. [12], were included in the analysis of the data from this study in order to examine the influence of traumatic brain injury and its possible disruption of the BBB on the plasma-CSF Teq. Seven of these nine children suffered traumatic brain injury. All nine children were ventilator dependent and required external ventricular drains for the management of raised intracranial pressure. These children were given APAP elixir [40 mg/kg, 250 mg/5 ml, SmithKline Beecham (NZ) Ltd, Auckland, NZ], instilled down a nasogastric feeding tube and both arterial blood and CSF sampled at hourly intervals for the first 4 h and then two hourly for the subsequent 6 h.
A separate additive term was used to characterize the residual unknown variability for plasma and CSF concentrations from each study.
Quality of fit
The quality of fit of the pharmacokinetic model to the data was assessed by visual examination of plots of observed versus predicted concentrations. Models were nested and an improvement in the objective function was referred to the Chi-squared distribution to assess significance, e.g., an objective function change (ΔOBJ) of 3.84 is significant at α=0.05.
Covariate analysis
The parameter values were standardized for a body weight of 70 kg using an allometric model [17].
where Pi is the parameter in the ith individual, Wi is the weight in the ith individual and Pstd is the parameter in an individual with a weight Wstd of 70 kg. The PWR exponent was 0.75 for clearance, 1 for distribution volumes and 0.25 for time-related indices [18, 19, 20, 21].
Interpreting sparse pharmacokinetic data
It was not possible to collect data to obtain time–concentration profiles on current study patients—often only a single plasma APAP sample was collected from each patient. Consequently, a larger data set from a previous study reported by Anderson et al. investigating age-related APAP pharmacokinetics (n=221) [22] was included to perform the population analysis.
Results
Population demographics
In this current study, 41 children participated: 21 boys and 20 girls. The eligible number of patients was 47. Six children were excluded because informed consent was not obtained due to either language difficulties (n=1) or to parental belief that there was no advantage gained for their child to participate in this study (n=5). Median age (25–75th percentile) and weight of the children participating was 12 months (3–62 months) and 10.0 kg (5.8–20.0 kg), respectively. Median (25–75th percentile) APAP loading dose was 32.3 mg/kg (25.3–42.5 mg/kg). Median (25–75th percentile) time between APAP loading dose administration and collection of blood samples and median time (25–75th percentile) between APAP loading dose and collection of CSF samples were, respectively, 125 min (95–210 min) and 133 min (33–202 min). Twenty-three children underwent VP shunt insertion, thirteen children had a VP shunt revision and five children underwent insertion of a temporary external ventricular drain. There were 114 observations. APAP plasma concentrations ranged from 0.0 mg/l to 33.0 mg/l, APAP CSF concentrations ranged from 0.0 mg/l to 21.0 mg/l.
Parameter estimates
Parameter estimates with covariate analyses are shown in Table 1 and Table 2. Pharmacokinetic estimates and maturational half-lives of V/Foral and CL/Foral were similar to those reported previously [23]. The population mean Teq, standardized to a 70-kg person, was 1.35 h (CV 108%). Figure 2 shows individual Bayesian Teq predictions and their relationship to age for the complete pooled data set. These predictions are based on maximum a posteriori Bayesian estimates of the parameters for each specific individual using their observed data. No relationship between age and Teq was determined. The mean Teq from the previous data from Anderson et al. [12] was lower (Teq 0.71 h, CV 105%) than that from the current study population (Teq 1.93 h, CV 43%). Two children from the previous study by Anderson et al. [12] had a Teq greater than 2.5 h (Fig. 2). These two children both had posterior fossa pathology, as opposed to the remaining children who suffered traumatic brain injury.
Individual Bayesian Teq (plasma to CSF equilibration half-time) predictions (standardized to a 70-kg person) and their relationship to age for the complete pooled data set. Predictions from the current data set are shown as x. Predictions from data from Anderson et al. are shown as Δ. Standardized Teq does not change with age
The type of surgery (VP shunt versus external ventricular drain) had no effect on individual Bayesian Teq predictions. The covariance of the pharmacokinetic parameters, expressed as the correlation of population parameter variability was low (Table 3).
The individual Bayesian predictions for plasma and CSF concentration are compared with those observed in Fig. 3a, b. These predictions are based on maximum a posteriori Bayesian estimates of the parameters for each specific individual using their observed data. Figure 4a, b demonstrates the quality of fit for pharmacokinetic data over the study time period—each subject's data is connected by a line.
The residual errors (mg/l) for the plasma concentration data were 3.4 and 3.2 for the current data and from Anderson et al. [12], respectively. The residual errors (mg/l) for the CSF concentration data were 4.3 and 2.0 for the current data and from Anderson et al. [12], respectively.
Discussion
This study estimates a population plasma to CSF Teq of 1.93 h (standardized to a 70-kg person) for APAP in children of all ages—an estimate similar to the Teq of 2.1 h determined from naive pooled adult data collected by Bannwarth et al. [10]. Patients in that study were adults (n=43) with rheumatic and nerve-root compression pain. They were given an intravenous pro-drug of APAP (propacetamol) and a single CSF APAP concentration was measured. Data were modeled with the MKMODEL program [23] using the same equations as in this current study and in the study performed by Anderson et al. [12]. Our current data do not support the concept of an increased permeability in the BBB in early infancy. We have recently expanded this view in relation to opioids [24]. Children with traumatic brain injury, however, did have a lower Teq—consistent with disruption of the BBB.
Size was the first covariate used in our current analysis. This deliberate choice was based on known biological principles. A lot of physiological, structural and time-related variables can be predicted within and between species with weight exponents of 0.75, 1 and 0.25, respectively [20]. We have used physiological time, rather than chronological time, to define standardized Teq. The concept of physiological time was developed as a consequence of allometry [25]. For example, most mammals have the same number of heartbeats and breaths in their life span. The difference between small and large animals is that smaller animals have faster physiologic processes and, consequently, a shorter life span. West et al. [18, 19] have used fractional geometry to mathematically explain the allometric power exponents. The "1/4 power laws" were derived from a general model that describes how essential materials are transported through space-filled fractional networks of branching tubes [18]. These design principles are independent of detailed dynamics and explicit models and should apply to virtually all organisms [19]. Consequently, we might expect a neonate (3.5 kg), 1-year-old child (10 kg), 5-year-old child (20 kg), 10-year-old child (30 kg) and an adult (70 kg) to have chronological Teq values of 0.9, 1, 1.4, 1.6 and 1.93 h, respectively (Fig. 5), which would result in a more rapid onset of effect in younger children. This is consistent with the speed of onset of other drugs due to distribution to an effect compartment [26]. This covariate should be factored into investigations of APAP effect. We might, for example, expect maximum fever reduction after APAP elixir to occur earlier in 1-year olds than in 10-year olds.
The plasma to CSF Teq is longer than the effect compartment Teq estimated for analgesia (53 min, CV 217%) [5] and for anti-pyresis (71 min, CV 10%) [6] in children. These data suggest that the CSF compartment is not the effect compartment responsible for these actions. Anti-pyresis is mediated through prostaglandins in the hypothalamus and analgesia through both prostaglandin synthesis and by antagonising NMDA and substance P in the spinal cord. Our data suggest that analgesic and anti-pyretic effects occur earlier than APAP concentration changes in the CSF.
References
Bjorkman R, Hallman KM, Hedner J, Hedner T, Henning M (1994) Acetaminophen blocks spinal hyperalgesia induced by NMDA and substance P. Pain 57:259–264
Bjorkman R (1995) Central antinociceptive effects of non-steroidal anti-inflammatory drugs and paracetamol. Experimental studies in the rat. Acta Anaesthesiol Scand Suppl 103:1–44
Piletta P, Porchet HC, Dayer P (1991) Central analgesic effect of acetaminophen but not of aspirin. Clin Pharmacol Ther 49:350–354
Coceani F (1991) Prostaglandins and fever: facts and controversies. In: Mackowial PA (ed) Fever: basic mechanisms and management. Raven Press, New York, pp 59–70
Anderson BJ, Woollard GA, Holford NH (2001) Acetaminophen analgesia in children: placebo effect and pain resolution after tonsillectomy. Eur J Clin Pharmacol 57:559–569
Brown RD, Kearns GL, Wilson JT (1998) Integrated pharmacokinetic–pharmacodynamic model for acetaminophen, ibuprofen, and placebo antipyresis in children. J Pharmacokinet Biopharm 26:559–579
Anti-inflammatory and immunosuppressant drugs. (1999) In: Rang HP, Dale MM, Ritter JM (eds) Pharmacology, 4th edn. Churchill Livingstone, pp 229–247
Flower RJ, Vane JT (1972) Inhibition of prostaglandin synthetase in brain explains the anti-pyretic activity of paracetamol (4-acetamidophenol). Nature 240:410–411
Ward RM (2000) Opioid tolerance to sedation and analgesia. Pediatr Res 47:705–706
Bannwarth B, Netter P, Lapicque F, et al (1992) Plasma and cerebrospinal fluid concentrations of paracetamol after a single intravenous dose of propacetamol. Br J Clin Pharmacol 34:79–81
Moreau X, Le Quay L, Granry JC, Boishardy N, Delhumeau A (1993) Pharmacokinetics of paracetamol in the cerebrospinal fluid in the elderly. Therapie 48:393–396
Anderson BJ, Holford NH, Woollard GA, Chan PL (1998) Paracetamol plasma and cerebrospinal fluid pharmacokinetics in children. Br J Clin Pharmacol 46:237–243
van Dijk M, de Boer JB, Koot HM, Tibboel D, Passchier J, Duivenvoorden HJ (2000) The reliability and validity of the COMFORT scale as a postoperative pain instrument in 0- to 3-year-old infants. Pain 84:367–377
Beal SL, Sheiner LB, Boeckmann A (1999) NONMEM user's guide. University of California, Division of Pharmacology, San Francisco
Danhof M, Hisaoka M, Levy G (1985) Kinetics of drugs action in disease state XII: effect of experimental liver diseases on the pharmacokinetics of phenobarbital and ethanol in rats. J Pharm Sci 74:321–324
Walle AJ, Gruner O, Niedemayer W (1980) Measurements of total bodywater in patients on maintenance hemodialysis using an ethanol dilution technique. Nephron 26:286–290
Holford NHG (1996) A size standard for pharmacokinetics. Clin Pharmacokinet 30:329–332
West GB, Brown JH, Enquist BJ (1997) A general model for the origin of allometric scaling laws in biology. Science 276:122–126
West GB, Brown JH, Enquist BJ (1999) The fourth dimension of life: fractal geometry and allometric scaling of organisms. Science 284:1677–1679
Peters HP (1983) Physiological correlates of size. In: Beck E, Birks HJB, Conner EF (eds) The ecological implications of body size. Cambridge University Press, Cambridge, pp 48–53
Prothero JW (1980) Scaling of blood parameters in animals. Comp Biochem Physiol A67:649–657
Anderson BJ, Woollard GA, Holford NH (2000) A model for size and age changes in the pharmacokinetics of paracetamol in neonates, infants and children. Br J Clin Pharmacol 50:125–134
Holford NHG (1994) MK model. Biosoft, Cambridge
van Lingen RA, Simons SH, Anderson BJ, Tibboel D (2002) The effect of analgesia in the vulnerable infant during the perinatal period. Clin Perinatol 19:511–534
Boxenbaum H (1982) Interspecies scaling, allometry, physiological time, and the ground plan of pharmacokinetics. J Pharmacokinet Biopharm 10:201–227
Anderson BJ, Meakin GH (2002) Scaling for sizesome implications for paediatric anaesthesia dosing. Paediatr Anaesth 12:502–519
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
van der Marel, C.D., Anderson, B.J., Pluim, M.A.L. et al. Acetaminophen in cerebrospinal fluid in children. Eur J Clin Pharmacol 59, 297–302 (2003). https://doi.org/10.1007/s00228-003-0622-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-003-0622-2