Abstract
While much research focuses on the range of signals detected by the osteoblast lineage that originate from endocrine influences, or from other cells within the body, there are also multiple interactions that occur within this family of cells. Osteoblasts exist as teams and form extensive communication networks both on, and within, the bone matrix. We provide four snapshots of communication pathways that exist within the osteoblast lineage between different stages of their differentiation, as follows: (1) PTHrP, a factor produced by early osteoblasts that stimulates the activity of more mature bone-forming cells and the most mature osteoblast embedded within the bone matrix, the osteocyte; (2) sclerostin, a secreted factor, released by osteocytes into their extensive communication network to restrict the activity of younger osteoblasts on the bone surface; (3) oncostatin M, a member of the IL-6/gp130 family of cytokines, expressed throughout osteoblast differentiation and acting to stimulate osteoblast activity that works on a different receptor in the mature osteocyte compared to the preosteoblast; and (4) Eph/ephrins, cell-contact-dependent kinases, and the osteoblast-lineage-specific interaction of EphB4 and ephrinB2, which provides a checkpoint for entry to the late stages of osteoblast differentiation and restricts RANKL expression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The skeleton is continually renewed and reshaped throughout life by the coordinated actions of multiple cell types. During bone remodeling, bone formation occurs on discrete surfaces where osteoclastic resorption has previously occurred. Cell-to-cell communication between both cell types is required for the skeleton to achieve the desired external and internal shape, thereby conferring appropriate strength needed for physiological activity with minimal risk of fracture. This communication is mediated by a system of regulatory factors produced by the cells that populate the bone multicellular unit (BMU). This includes the lineages that give rise to osteoblasts and osteoclasts. In this review, we will focus on factors secreted by the osteoblast lineage and proteins expressed on their cell membranes and describe their paracrine or autocrine influences on osteoblast and osteocyte function.
The Osteoblast Lineage In Vitro and In Vivo
We use the term osteoblast lineage to include all cells along the continuum that exists between cells with the capacity and commitment to differentiate into active bone-forming osteoblasts and those cells that were active bone-forming osteoblasts at an earlier time point. This population therefore includes committed osteoblast precursors, preosteoblasts, active bone-forming osteoblasts and osteocytes, both those embedded in the osteoid matrix and those fully differentiated osteocytes embedded within the mineralized matrix. These cells would also include lining cells, reported to be final stage osteoblasts, that sit, flattened on the bone matrix, apparently guarding the bone matrix against osteoclastic activity.
Osteoblast lineage cells are derived from mesenchymal stem cells; originally identified in vitro as colony-forming fibroblasts [1]. These cells also have the capacity to differentiate to chondrocytes or adipocytes [2]. A precise definition of a committed osteoblast precursor is elusive, but expression of Runt-related transcription factor 2 (Runx2) and Osterix (Osx) are absolutely required for bone formation to occur [3, 4] indicating that these two factors at least are required for osteoblast commitment.
Active bone-forming osteoblasts in vivo are engaged in forming osteoid on the bone surface. An important characteristic of active osteoblasts is that, in vivo, these cells do not operate in isolation, or even in small groups of two or three cells. In contrast, bone forming surfaces are lined by a seam of osteoid, on the surface of which resides a team of osteoblasts, with similar nuclear–cytoplasmic alignment, and extensive sites of contact between team members. Formation of mineralized nodules in cell culture also depends on a critical mass of differentiated osteoblasts, with a cobblestone appearance and extensive cell–cell contact, before matrix deposition occurs [5–7]. The requirement of cell-cell contact by bone-forming osteoblasts, reiterates the importance of cadherins and gap junctions (discussed elsewhere in this issue) but also suggests that paracrine and autocrine control mechanisms may be important for osteoblast differentiation and bone formation.
While osteoblasts are readily detected in tissue sections, they are more difficult to identify in vitro because they cannot be observed lining an osteoid seam. For this reason cell culture systems rely on osteoblast marker genes to define the stages of differentiation reached by the cultured cells. Genes that reflect early osteoblast commitment include Runx2 [8] and Osx [4]. The osteoblast produces abundant levels of collagen I (Col1a1), alkaline phosphatase (Alp), and parathyroid hormone receptor (Pth1r) [9]. Osteocalcin (Bglap) [10] and bone sialoprotein (Ibsp) [11] are expressed when the osteoblasts enter a more mature stage of osteoblast differentiation including the early osteocytic stage. This is then followed by expression of osteocyte genes such as Dentin matrix protein-1 (Dmp1) [12], Matrix extracellular phosphoglycoprotein (Mepe) [13] and Sclerostin (Sost) [14] as the cells continue to differentiate into mature osteocytes (Fig. 1).
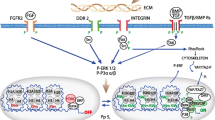
Paracrine influences on the osteoblast lineage throughout differentiation. Top Patterns of expression of paracrine factors within the lineage. Ligands such as oncostatin M (OSM), ephrinB1 and ephrinB2 are expressed at relatively stable levels throughout differentiation, while parathyroid hormone-related protein (PTHrP) is down-regulated during differentiation, and sclerostin is up-regulated as osteoblasts reach osteocytic differentiation. Some receptor expression levels are relatively stable, such as glycoprotein 130 (gp130), OSM receptor (OSMR), leukemia inhibitory factor receptor (LIFR) and EphB4, while PTH receptor (PTHR1) is up-regulated during osteoblast differentiation. Center Differentiating osteoblast lineage and genes expressed from the preosteoblast to the osteocytic stage. These include Runx2, osterix (Osx), collagen 1α1 (Col1a1), alkaline phosphatase (Alpl), osteocalcin (Bglap), bone sialoprotein (Ibsp), dentine–matrix protein-1 (Dmp1), matrix extracellular phosphoglycoprotein (Mepe) and sclerostin (Sost). Bottom Stages at which the discussed paracrine factors influence osteoblast function. PTHrP stimulates osteoblasts at a late stage of differentiation. OSM stimulates osteoblast commitment at an early stage, through OSMR, and inhibits sclerostin in osteocytes through LIFR. Within the osteoblast lineage, EphrinB1:EphB2 influences the transition from Runx2 expression to Osx expression, while ephrinB2:EphB4 signaling allows the transition to Alpl expression. Sclerostin, while expressed by osteocytes, influences osteoblast activity from an early stage of differentiation but may also have direct effects on the mature osteocyte
Osteoblast lineage cells have also been described in a canopy over BMUs in human tissue sections. These cells were identified as osteoblasts by their expression of late osteoblast markers including osteocalcin [15]. The cells form a continuous layer over regions of bone remodeling, perhaps as a result of lifting from the bone surface. In this manner, they are currently thought to make a sealed zone in which bone remodeling and paracrine communication can occur in isolation from the rest of the marrow milieu. While these cells may also contribute directly to paracrine and autocrine control of osteoblast differentiation, this contribution has been difficult to separate from the influence of the rest of the lineage because they have not been described in species other than human, and are not observed in cell culture.
Factors that modify osteoblast behavior have been shown to play essential roles within the osteoblast lineage based on in vivo mouse genetic knockout modeling experiments, cell culture studies, or by familial human genetic analysis of patients with particular bone disorders. These factors have the potential to serve as new targets for therapies for skeletal disorders including osteoporosis. In this review we will discuss the evidence for paracrine/autocrine regulation of the osteoblast lineage by parathyroid hormone-related protein (PTHrP), sclerostin, the gp130 family of cytokines, particularly oncostatin M (OSM), and members of the Eph/ephrin family.
PTHrP: Endocrine in Pathology, Paracrine in Physiology
PTHrP was initially discovered to be released into the circulation at high levels in 80 % of humoral hypercalcemia of malignancy cases [16]. PTHrP can also enter the circulation during lactation [17] and in fetal life [18]. In the rest of life, PTHrP is not detected in the serum, but is expressed locally by many cells within different tissues [19] where it acts in a paracrine manner. Within the osteoblast lineage, PTHrP is expressed by osteoblast progenitors in bone and bone marrow [20, 21]. As these cells mature and differentiate, PTHrP expression levels decrease [22]. This contrasts with the expression of its receptor (parathyroid hormone receptor 1–PTH1R) that it shares with parathyroid hormone (PTH) [23]. PTH1R levels increase as osteoblast progenitors mature into osteoblasts and terminally differentiate into osteocytes [21]. Thus, paracrine PTHrP released from early stage osteoblasts would influence the function of late-stage osteoblasts and osteocytes [24].
A physiological role of PTHrP in bone formation was first demonstrated when its specific deletion from the osteoblast lineage resulted in a phenotype of low bone formation and low bone mass [25]. Consistent with the ability of PTHrP to stimulate RANKL expression, these mice also showed impaired osteoclast formation. Strikingly, PTHrP-deficient osteoblasts were hyper-responsive to anabolic PTH treatment, suggesting that paracrine PTHrP may also limit the anabolic action of therapeutic PTH [25]. This phenotype, and its similarity with that of PTHrP haploinsufficient mice [26], has culminated in a model where PTHrP produced by osteoblast progenitors acts through PTH1R on committed preosteoblasts to enhance their differentiation into mature matrix-producing osteoblasts and osteocytes [27], and promotes their survival [25]. This anabolic action of PTHrP has been proposed to be the paracrine physiological equivalent of the pharmacological anabolic agent, PTH [28]. Such a paracrine action is consistent with detection of PTHrP in preosteoblasts that reside in the superficial layer above bone-forming osteoblasts in developing bone and in wound healing [22].
While the regulation of PTHrP expression has been well studied in the context of breast cancer because of its pro-metastatic action [29] and in chondrocytes because of its role in bone development [30], little work has focused on the regulation of PTHrP within the osteoblast lineage. Presumably the same factors that stimulate PTHrP expression in breast cancer and chondrocyte differentiation would also stimulate it in osteoblasts. An example is hedgehog signaling, which promotes osteoblast differentiation and stimulates PTHrP expression in osteoblasts [31], breast cancer cells [32, 33], and chondrocytes [34, 35].
The local anabolic action of PTHrP has meant that the study of genes regulated by PTHrP in osteoblasts may reveal novel anabolic pathways for the skeleton. The rest of this review will discuss several proteins regulated by PTHrP (and PTH) in the osteoblast lineage that have been found to have anabolic action in bone: sclerostin, the signal transducer gp130 and ephrinB2.
Sclerostin: A Signal from the Mature Matrix-Embedded Osteocyte to the Active Osteoblast
One of the most fascinating communication pathways in the osteoblast lineage is osteocytic production of sclerostin [36] and its inhibition of the bone-forming activity of osteoblasts. Sclerostin was first identified when loss of function mutations within its coding gene (SOST) were shown to associate with the high bone mass phenotype of Sclerosteosis [37]. Large deletions downstream of the SOST coding region that cause loss of sclerostin expression were identified in a similar syndrome of Van Buchem disease, a phenotype that was reproduced in a genetic mouse model containing the same mutation [38–40]. What was particularly interesting about these patients was that inhibition of sclerostin activity led to an increase in bone mass that was not associated with osteosarcoma, pointing to a potential therapeutic pathway: inhibition of sclerostin might be an anabolic therapy for osteoporosis. This has made investigations into the action and regulation of sclerostin all the more important, and research into this pathway has proceeded very rapidly.
Sclerostin is a Wnt antagonist that is expressed by osteocytes in mineralized bone, particularly in the most deeply embedded mature osteocytes [14, 41]. Although most work has focused on the secretion of sclerostin from the osteocyte and its potential paracrine role, sclerostin has been detected in other organs and in the cartilage [42]. This suggests paracrine roles in other organ systems such as in the aortic intima where it may inhibit mineralization [43]. Its ability to enter the circulation also suggests a systemic action may be possible [44].
Mouse genetic studies have confirmed that sclerostin inhibits osteoblast-mediated bone formation [36, 40, 45, 46] primarily by binding to the Wnt receptors LRP4, LRP5 and LRP6, thereby inhibiting Wnt-β-catenin signaling [47–51]. The importance of this pathway of sclerostin action is underscored by the knowledge that some human mutations in LRP5 associated with high bone mass impair sclerostin binding to LRP5 [47, 48]. An intriguing question is whether sclerostin limits bone formation by acting only on matrix-producing osteoblasts, or also has autocrine action on the osteocyte. There is evidence for both of these roles. The relative importance of the different LRP proteins with which sclerostin interacts remains unclear, but has been extensively reviewed recently [52].
That sclerostin influences osteoblast differentiation is well established. The increase in bone mass, rather than only an increase in bone material density, that is observed in the absence of sclerostin signaling indicate that matrix production, the main action of bone surface osteoblasts, is increased. And, in mice deficient in sclerostin, osteoblast numbers are higher than in controls [45] indicating enhanced osteoblast differentiation. Furthermore, in vitro studies found that treatment of the mouse stromal cell line C3H10T1/2 with sclerostin inhibited alkaline phosphatase activity, a characteristic of matrix-producing osteoblasts [36] and inhibited mineralization of human MSCs, an outcome that would be anticipated because of the impaired osteoblast differentiation [36]. This osteoblastic mode of action of sclerostin is based on the understanding that once secreted by the osteocyte, sclerostin travels through the lacunar-canalicular network to the bone surface where it influences matrix production by surface-dwelling osteoblasts.
Osteocyte-specific targeting of genetic mutations in mouse models is now routinely used to investigate the role of osteocytes in controlling both bone formation and resorption. Of relevance to the autocrine/paracrine action of sclerostin, the LRP5 high bone mass mutations that interfere with sclerostin binding have been genetically introduced to osteocytes using a DMP1-Cre. In this model, bone formation rate and bone mass were both significantly greater confirming that it is the binding of sclerostin to LRP5 that is an autocrine mechanism by which bone formation is inhibited [53]. Some caution in interpretation is required because DMP1-Cre is also active in bone surface osteoblasts [54] and it remains controversial to what extent this needs to be considered [55]. Certainly, this result confirms that the interaction of sclerostin with LRP5 that inhibits bone formation is a lineage-specific paracrine interaction.
Further evidence that sclerostin acts on the osteocyte itself is that Wnt signaling activation, detected in adult TOPgal reporter mice, is more readily detected in osteocytes than osteoblasts [56]. In addition, stimulation of bone formation by experimental mechanical loading reduces sclerostin expression [57], suggesting that sclerostin mediates the anabolic action of mechanical loading. Data to support this has been that deletion of sclerostin, or antibody-based inhibition, protects mice from bone loss after unloading [46, 58]. Further correlative data supports this concept: for example, mechanical loading in mice lacking periostin neither increased bone formation nor reduced sclerostin expression [59]. Proof will be found if mechanical loading is unable to stimulate bone formation in sclerostin deficient mice; this outcome may be complicated by the already very high bone mass of these animals.
In addition to its role in inhibiting Wnt signaling, there is also evidence that sclerostin acts specifically to regulate the bone mineralization process by increasing the production of matrix extracellular phosphoglycoprotein (MEPE), and inhibiting production of PHEX [60]. This action is thought to be restricted to late stage osteoblasts/osteocytes; however, whether this is a carryover of sclerostin-inhibited osteoblast differentiation or an independent effect specifically on the osteocyte is not yet clear.
Sclerostin expression is inhibited by a range of factors. In addition to its inhibition by mechanical loading, sclerostin is inhibited by paracrine factors that stimulate bone formation. These include gp130 family cytokines [61], PTHrP [42], prostaglandin E2 [62] and hypoxia [63]. The inhibition of sclerostin expression by these factors is rapid, presumably reflecting a direct effect on osteocytic gene expression. In other cases, sclerostin expression levels are low because of an earlier block in osteoblast differentiation, as seen in mouse models with osteoblast-specific deletion of osterix [64]. These concepts are discussed at length in our earlier review [42]. The importance of suppressing sclerostin for the anabolic action of factors that stimulate bone formation is not yet fully resolved, but much work has focused on the importance of sclerostin in the anabolic action of pharmacological intermittent PTH treatment [65, 66] because PTH rapidly inhibits sclerostin expression [67, 68]. Experiments of stimulating bone formation with PTH in sclerostin deficient mice have been carried out, and while complicated by the high bone mass phenotype of the sclerostin KO mouse, it was clear that PTH could still stimulate bone formation in both trabecular and cortical compartments [69, 70]. As a clue to the physiological importance of PTH or PTHrP-induced inhibition of sclerostin, mice in which their shared receptor (PTH1R) was deleted in osteocytes exhibited a very mild bone phenotype, with no detectable alteration in biochemical markers of bone formation, despite increased sclerostin expression [71]. This indicates that in the context of normal bone remodeling, the role of osteocytic PTH1R signaling, and by extension, PTH1R-mediated inhibition of sclerostin is a minor one.
Oncostatin M: a Paracrine Osteoblast-Lineage Stimulus that Acts Through Stage-Specific Receptors
Within the skeleton, the prevailing opinion has been that interleukin 6 (IL-6) family cytokines (the cytokines that signal through gp130) function mainly as inflammation-associated cytokines that stimulate osteoclast formation by stimulating osteoblastic RANKL expression [72]. Indeed, the main function of IL-6 in the skeleton is to amplify osteoclast formation in conditions such as inflammatory arthritis and estrogen deficiency [73, 74]. This cytokine family also includes interleukin 11 (IL-11), leukemia inhibitory factor (LIF), cardiotrophin-1 (CT-1) and oncostatin M (OSM), all of which also increase osteoclast formation by stimulating osteoblastic RANKL production. There has also been evidence from the earliest days that some members of this family stimulate bone formation, as revealed by Metcalf et al in 1989, who observed high bone mass in mice overexpressing LIF [75].
Because the gp130 receptor itself is so promiscuous the specificity of action of each cytokine that signals through it depends on the formation of ligand-specific multi-component complexes. For example, IL-6 forms a complex that includes the IL-6-specific receptor subunit (IL-6R) bound to a homodimer of gp130; a similar complex is used by IL-11 (with IL-11R in place of IL-6R). The majority of cytokines that signal through gp130 act through a heterodimer of gp130 bound to the LIF receptor (LIFR). Naturally, this means that LIFR is not specific for LIF at all! The specificity of ligand action through gp130:LIFR is further modified by the addition of other ligand-specific receptors to the complex (such as ciliary-neurotrophic factor receptor—CNTFR). A full description of each gp130 family member and its role in bone can be found in our earlier reviews [76, 77]. Here we will focus on Oncostatin M (OSM) because it is expressed at all stages of committed osteoblast differentiation in vivo, and it forms two different receptor complexes depending on the stage of osteoblast differentiation [61]. OSM forms a complex either with a heterodimer of gp130 and LIFR, or a heterodimer of gp130 and OSMR [78]. While it was originally thought that these complexes were only biologically important in human cells because of the low binding affinity of murine OSM for LIFR [79], our recent work indicates that murine OSM has biological effects through both complexes. Furthermore, the downstream effects initiated by these receptor complexes are different, and the ability of OSM to signal through LIFR may be an osteocyte-specific effect.
OSM was originally thought to be largely a product of activated macrophages, with its role in bone thought to be mainly a stimulus of bone destruction in the context of inflammation because it is a very potent stimulus of osteoclast formation in the co-culture system [72], and of RANKL expression in osteboalsts [80, 81]. It was surprising then that OSMR deletion in mice did not moderate the effects of experimental inflammatory arthritis on bone destruction [73]. More recently, we have reported that OSM is also expressed throughout the osteoblast lineage: in bone-forming osteoblasts, bone lining cells and in osteocytes [61]. The osteoblast lineage, including osteocytes, also express both receptor subunits required for gp130 activation by OSM: OSMR and LIFR [61]. In uncommitted progenitors, OSM stimulated the osteoblast commitment genes C/EBPβ and C/EBPδ, and inhibited adipogenic genes C/EBPα and PPARγ, through OSMR. Confirmation that OSM promotes osteoblast commitment through OSMR came from a phenotypic analysis of OSMR null mice which revealed low osteoblast numbers and a high level of marrow adipogenesis [61]. In osteocytes, OSM strongly inhibited sclerostin expression, an action that, surprisingly, was not blocked by OSMR deletion, and was found to be mediated by LIFR. Because sclerostin is the only gene known to be regulated by OSM:LIFR, this signaling pathway may be specific to the osteocyte. No significant up-regulation of LIFR mRNA levels was detected when osteoblasts were differentiated in vitro to the stage of osteocytic gene expression [61]. This raises the possibility that additional components required for complex formation of OSM:LIFR exist in osteocytes, but not in osteoblasts at earlier stages of differentiation. Whether OSM:LIFR signaling occurs in other murine cells outside of the skeleton is not yet known.
The inhibition of sclerostin by OSM:LIFR signaling is also achieved by other gp130 cytokines that act through LIFR [61]. These include CT-1, an osteoclast-derived coupling factor [82], and LIF, which is expressed by a wide range of cells including chondrocytes and osteoblasts [77]. Genetic deletion of CT-1 and LIF both lead to reduced osteoblast differentiation and a low level of bone formation in remodeling bone [82, 83]. This highlights the importance of gp130:LIFR signaling in osteoblast differentiation. The family of cytokines that signal through CNTFR:LIFR complexes do not inhibit sclerostin expression nor stimulate bone formation [84].
Although CT-1 and LIF inhibit sclerostin through LIFR, this is the same receptor complex through which they stimulate RANKL production. How can OSM inhibit sclerostin through LIFR, but not stimulate RANKL? This suggests that there are structural differences in the OSM:gp130:LIFR complex that allow it to activate a different set of signaling pathways from LIF:gp130:LIFR. Discovering this pathway could lead to a novel method to increase bone mass by specifically inhibiting sclerostin without stimulating RANKL. The crystal structure of the OSM:gp130:LIFR complex has not yet been solved, but a comparison with the complexes formed by CT-1 and LIF with gp130:LIFR may provide clues as to how such a specific pathway can be activated.
It is striking that the effects of LIFR signaling in osteoblast lineage cells are very similar to the effects of PTH1R signaling. LIF, OSM, CT-1, PTH and PTHrP all increase RANKL and stimulate osteoclast formation, and all of these agents inhibit sclerostin and stimulate bone formation. It has been known for many years that PTH induces expression of gp130, LIF and IL-6 [85], and we recently observed that OSMR expression is also stimulated by PTH, while paradoxically LIFR expression is reduced [86]. Given that gp130 neutralizing antibodies impair the stimulatory effect of PTH on osteoclast formation in the presence of osteoblasts in vitro [87] an interesting question that remains is whether the actions of PTH depend on signaling of these cytokines in the osteoblast lineage.
EPH/Ephrin Cellular Communication: Contact-Dependent Communication at Specific Stages Within Osteoblast Differentiation
Originally discovered and identified as a trans-membrane protein in an Erythropoietin-producing human hepatocellular carcinoma cell line [88], the Eph/ephrin family constitute the largest family of receptor tyrosine kinases (RTKs) and is composed of 14 Eph receptors and 8 ephrin (Eph receptor interacting protein) ligands within mammals [89, 90]. Two features make the Eph/ephrin family distinct from other RTKs: (1) both receptor and ligand are membrane-bound, so their signaling is mediated by direct cell-to-cell interaction, and (2) receptor–ligand interactions generate bidirectional signaling where forward signaling through the Eph receptor and reverse signaling through the ephrin ligand occur at the same time [91].
Interactions between Eph receptors and their ligands can be quite complex, as a high degree of promiscuity exists both within and between the A and B subclasses that exist. These subclasses are based on how the ephrin ligands are tethered to the cell membrane. The ephrinA subclass bind with a glycosylphosphatidylinositol (GPI) anchor, and ephrinB ligands by a transmembrane domain [90]. The Eph receptors are classified as either EphA or EphB based on their initially identified affinity to ephrinA or ephrinB ligands [89]. Following dimerization of Eph and ephrin, oligomerization and clustering allows bidirectional signaling to occur.
Within the osteoblast lineage, many of the A and B class receptors and ligands are expressed [92, 93], and the roles of each member in bone formation are only beginning to be understood. Much attention has been given to the possibility of heterotypic interactions (i.e. between two cell types) of Eph/ephrins within the BMU between osteoblasts and osteoclasts [93]. In this review we will focus on the role of the Eph family as homotypic paracrine factors within the osteoblast lineage.
Eph:ephrin interactions induce cell adhesion and repulsion, two processes that are critical for cranial suture formation during embryonic skeletal development. Normally, suture closure occurs when mesenchymal cells migrate into the suture region and differentiate into osteoblasts. Attractive and repulsive cues between osteogenic and neural crest cells residing in the mesoderm boundary are required for this to occur at the appropriate stage of skull growth. The importance of repulsive cues generated by Eph/ephrins within the osteoblast lineage has been shown with EphA4. This receptor does not appear to regulate osteoblast differentiation, but delays migration of EphA4-expressing osteogenic cells into the cranial suture until an appropriate stage of development is reached [94]. This occurs by repulsion signals generated between these cells and the cells at the mesoderm boundary that express ephrinA2 and ephrinA4, two receptors for EphA4 [95]. Thus, mice with deletion of EphA4 display early suture closure in their developing skull (craniosynostosis) [95].
Craniofrontonasal syndrome is caused by mutations in the ephrinB1 encoding gene EFNB1 [96], a phenotype that has been reproduced in female mice heterozygous for a global deletion of ephrinB1. Studies in the mouse model showed that this is caused by defective differentiation of the osteogenic mesenchyme that gives rise to osteoblasts [97], rather than to their reduced migration [94]. This finding parallels those observed when ephrinB1 is conditionally deleted from the osteoblast lineage, where the resulting phenotype indicated that ephrinB1 interaction with EphB2 in osteoblasts stimulates their differentiation and bone-forming ability [98]. Although 30 % of these mice died before birth, those that survived had shorter femurs, low bone mineral density and a low level of bone formation. Enhancing ephrinB1 reverse signaling in bone marrow stromal cells with a clustered form of EphB2 caused a dramatic up-regulation of ALP activity and fourfold increase in osterix mRNA compared to control cells after 6 days of treatment. Long bones from osteoblast-targeted conditional ephrinB1 deficient mice had low levels of both Osx and Alp expression compared to control littermates; earlier markers (Runx2 and Msx1) were not altered, and later markers were not investigated. EphrinB1 is therefore required at least for the expression of early osteoblast markers such as Osx and Alp downstream of Runx2. Stimulation of ephrinB1 reverse signaling with clustered EphB2 was shown to increase Osx expression by nuclear translocation of TAZ (transcriptional coactivator with PDZ-binding motif). These studies suggest that reverse signaling by ephrinB1 is required for normal osteoblast differentiation during development and postnatal life. However, as a result of the bidirectional nature of ephrin/Eph signaling, deletion of ephrinB1 may also diminish forward signaling through EphB2. Thus the observed effects of ephrinB2 deletion on osteoblast differentiation may be due to either reduced reverse signaling by ephrinB1, or reduced forward signaling through EphB2. To complicate matters further, reduced expression of ephrinB1 ligand may also promote signaling of EphB2 through its other ligands expressed in osteoblasts (ephrinA5 [99] and ephrinB2 [100]) due to reduced competition with ephrinB1. Studies of ligand and receptor phosphorylation will be required to resolve these questions.
Osteoblasts and osteocytes also express the ephrinB2 ligand [93] and among all ephrin/Eph family members, it is the only one to be stimulated by PTH and PTHrP in the osteoblast lineage [101]. Like ephrinB1, ephrinB2 is expressed stably throughout osteoblast differentiation [101]. The paracrine interaction between ephrinB2 and one of its receptors EphB4 in osteoblasts has subsequently been shown to stimulate the late stages of osteoblast differentiation, and to support their capacity to mineralize [101, 102]. In vitro studies initially showed that pharmacological blockade of ephrinB2/EphB4 interaction (blocking both reverse and forward signaling) in osteoblasts reduced both their mineralization [101, 102] and their expression of late markers of osteoblast differentiation [101–103], indicating an osteoblast-lineage-specific effect of the ephrinB2/EphB4 interaction. Osteoblast markers from the stage of Alkaline phosphatase (Alpl) production were all inhibited by this blockade, indicating an ephrinB2/EphB4-dependent checkpoint required for late stage osteoblast differentiation. The same blockade strategy in vivo increased osteoblast numbers; even in mice that already had high osteoblast numbers due to PTH treatment. Despite this increase in osteoblast numbers and osteoid production, there was no increase in the level of bone mineralizing activity [103]. This suggests that although osteoblasts with reduced ephrinB2/EphB4 signaling are still capable of responding to spatial cues to produce osteoid, they have a reduced capacity to mineralize [103]. This impairment in osteoblast function is consistent with the reduced expression of late stage osteoblast markers in vitro, suggesting that it is the homotypic/autocrine action of ephrinB2/EphB4 within the osteoblast lineage that is most important for osteoblast differentiation.
Even though ephrinB2/EphB4 inhibition of cultured osteoblasts inhibited late markers of osteoblast differentiation, it also increased RANKL expression [103]. In the context of PTH treatment in vivo, this led to an increase in the number of osteoclasts and a loss of the PTH anabolic effect. The increase in osteoclast formation was recapitulated in co-culture experiments between hematopoietic precursors and osteoblasts [103]. In combination this data suggests that ephrinB2 and EphB4 interaction within the osteoblast lineage acts both to promote late osteoblast differentiation and to restrain osteoclast formation within the BMU.
Earlier data indicated that stimulation of EphB4 forward signaling rather than ephrinB2 reverse signaling within the osteoblast lineage induces osteoblast differentiation and mineralization [93]. This result seems perplexing because PTH and PTHrP, as anabolic influences on osteoblasts, increase only the expression of ephrinB2. However, separating these two effects is technically challenging. Genetic deletion of EphB4 to block forward signaling would also reduce ephrinB2 reverse signaling because binding of receptor to ligand activates signaling in both directions; and the pharmacological inhibitors described above also inhibit both directions of signaling. Activation of ephrinB2 reverse signaling [104] and ephrinB2 overexpression [105] have both recently been reported to determine commitment of MSCs to the osteoblast lineage, a role that is thought to be important for bone injury and repair [106]. The relative contributions of ephrinB2 reverse signaling and EphB4 forward signaling to bone mineralization and the support of osteoclast formation by osteoblasts are yet to be resolved.
Summary and Conclusion
There are a number of specific communication pathways that function at different stages of differentiation within the osteoblast lineage (Fig. 1). PTHrP produced by early osteoblasts stimulates activity of mature cells, and acts on osteocytes where it inhibits sclerostin expression. Sclerostin, produced by osteocytes, acts in the opposite direction to inhibit the activity of bone forming osteoblasts. Other contributors include OSM, which is produced at all stages of osteoblast differentiation, and is not strongly regulated, but in early osteoblasts it stimulates differentiation through actions mediated by the OSMR, while in osteocytes it inhibits sclerostin through the LIFR. Finally, ephrinB2 and EphB4 are expressed on osteoblast cell membranes throughout osteoblast differentiation, and ephrinB2 expression is stimulated in those osteoblasts that express the PTH1R. This interaction controls both osteoblast commitment and promotes late stages of osteoblast differentiation, an effect mediated within the osteoblast lineage. A full understanding of how paracrine factors influence different stages of osteoblast differentiation and unique aspects of their bone forming activity will provide much new information for developing agents that can stimulate bone formation where it is needed, during fracture healing and in osteoporosis, or to suppress bone formation in disorders such as osteosarcoma and heterotopic ossification.
References
Friedenstein AJ, Chailakhjan RK, Lalykina KS (1970) The development of fibroblast colonies in monolayer cultures of guinea-pig bone marrow and spleen cells. Cell Tissue Kinet 3:393–403
Bianco P, Robey PG, Simmons PJ (2008) Mesenchymal stem cells: revisiting history, concepts, and assays. Cell Stem Cell 2:313–319
Ducy P, Starbuck M, Priemel M, Shen J, Pinero G, Geoffroy V, Amling M, Karsenty G (1999) A Cbfa1-dependent genetic pathway controls bone formation beyond embryonic development. Genes Dev 13:1025–1036
Nakashima K, Zhou X, Kunkel G, Zhang Z, Deng JM, Behringer RR, de Crombrugghe B (2002) The novel zinc finger-containing transcription factor osterix is required for osteoblast differentiation and bone formation. Cell 108:17–29
Ecarot-Charrier B, Glorieux FH, van der Rest M, Pereira G (1983) Osteoblasts isolated from mouse calvaria initiate matrix mineralization in culture. J Cell Biol 96:639–643
Abe Y, Akamine A, Aida Y, Maeda K (1993) Differentiation and mineralization in osteogenic precursor cells derived from fetal rat mandibular bone. Calcif Tissue Int 52:365–371
Gerber I, ap Gwynn I (2001) Influence of cell isolation, cell culture density, and cell nutrition on differentiation of rat calvarial osteoblast-like cells in vitro. Eur Cell Mater 2:10–20
Komori T, Yagi H, Nomura S, Yamaguchi A, Sasaki K, Deguchi K, Shimizu Y, Bronson RT, Gao YH, Inada M, Sato M, Okamoto R, Kitamura Y, Yoshiki S, Kishimoto T (1997) Targeted disruption of Cbfa1 results in a complete lack of bone formation owing to maturational arrest of osteoblasts. Cell 89:755–764
Aubin JE, Liu F, Malaval L, Gupta AK (1995) Osteoblast and chondroblast differentiation. Bone 17:77S–83S
Sims NA, White CP, Sunn KL, Thomas GP, Drummond ML, Morrison NA, Eisman JA, Gardiner EM (1997) Human and murine osteocalcin gene expression: conserved tissue restricted expression and divergent responses to 1,25-dihydroxyvitamin D3 in vivo. Mol Endocrinol 11:1695–1708
Aubin JE (2001) Regulation of osteoblast formation and function. Rev Endocr Metab Disord 2:81–94
Toyosawa S, Shintani S, Fujiwara T, Ooshima T, Sato A, Ijuhin N, Komori T (2001) Dentin matrix protein 1 is predominantly expressed in chicken and rat osteocytes but not in osteoblasts. J Bone Miner Res 16:2017–2026
Gowen LC, Petersen DN, Mansolf AL, Qi H, Stock JL, Tkalcevic GT, Simmons HA, Crawford DT, Chidsey-Frink KL, Ke HZ, McNeish JD, Brown TA (2003) Targeted disruption of the osteoblast/osteocyte factor 45 gene (OF45) results in increased bone formation and bone mass. J Biol Chem 278:1998–2007
van Bezooijen RL, Roelen BA, Visser A, van der Wee-Pals L, de Wilt E, Karperien M, Hamersma H, Papapoulos SE, ten Dijke P, Lowik CW (2004) Sclerostin is an osteocyte-expressed negative regulator of bone formation, but not a classical BMP antagonist. J Exp Med 199:805–814
Andersen TL, Sondergaard TE, Skorzynska KE, Dagnaes-Hansen F, Plesner TL, Hauge EM, Plesner T, Delaisse JM (2009) A physical mechanism for coupling bone resorption and formation in adult human bone. Am J Pathol 174:239–247
Suva LJ, Winslow GA, Wettenhall RE, Hammonds RG, Moseley JM, Diefenbach-Jagger H, Rodda CP, Kemp BE, Rodriguez H, Chen EY et al (1987) A parathyroid hormone-related protein implicated in malignant hypercalcemia: cloning and expression. Science 237:893–896
Grill V, Hillary J, Ho PM, Law FM, MacIsaac RJ, MacIsaac IA, Moseley JM, Martin TJ (1992) Parathyroid hormone-related protein: a possible endocrine function in lactation. Clin Endocrinol 37:405–410
Kovacs CS, Lanske B, Hunzelman JL, Guo J, Karaplis AC, Kronenberg HM (1996) Parathyroid hormone-related peptide (PTHrP) regulates fetal-placental calcium transport through a receptor distinct from the PTH/PTHrP receptor. Proc Natl Acad Sci USA 93:15233–15238
Strewler GJ (2000) The physiology of parathyroid hormone–related protein. N Engl J Med 342:177–185
Moseley JM, Hayman JA, Danks JA, Alcorn D, Grill V, Southby J, Horton MA (1991) Immunohistochemical detection of parathyroid hormone-related protein in human fetal epithelia. J Clin Endocrinol Metab 73:478–484
Suda N, Gillespie MT, Traianedes K, Zhou H, Ho PW, Hards DK, Allan EH, Martin TJ, Moseley JM (1996) Expression of parathyroid hormone-related protein in cells of osteoblast lineage. J Cell Physiol 166:94–104
Kartsogiannis V, Moseley J, McKelvie B, Chou ST, Hards DK, Ng KW, Martin TJ, Zhou H (1997) Temporal expression of PTHrP during endochondral bone formation in mouse and intramembranous bone formation in an in vivo rabbit model. Bone 21:385–392
Juppner H, Abou-Samra AB, Freeman M, Kong XF, Schipani E, Richards J, Kolakowski LF Jr, Hock J, Potts JT Jr, Kronenberg HM et al (1991) A G protein-linked receptor for parathyroid hormone and parathyroid hormone-related peptide. Science 254:1024–1026
Martin TJ (2005) Osteoblast-derived PTHrP is a physiological regulator of bone formation. J Clin Invest 115:2322–2324
Miao D, He B, Jiang Y, Kobayashi T, Soroceanu MA, Zhao J, Su H, Tong X, Amizuka N, Gupta A, Genant HK, Kronenberg HM, Goltzman D, Karaplis AC (2005) Osteoblast-derived PTHrP is a potent endogenous bone anabolic agent that modifies the therapeutic efficacy of administered PTH 1–34. J Clin Invest 115:2402–2411
Amizuka N, Karaplis AC, Henderson JE, Warshawsky H, Lipman ML, Matsuki Y, Ejiri S, Tanaka M, Izumi N, Ozawa H, Goltzman D (1996) Haploinsufficiency of parathyroid hormone-related peptide (PTHrP) results in abnormal postnatal bone development. Dev Biol 175:166–176
Carpio L, Gladu J, Goltzman D, Rabbani SA (2001) Induction of osteoblast differentiation indexes by PTHrP in MG-63 cells involves multiple signaling pathways. Am J Physiol Endocrinol Metab 281:E489–E499
Martin TJ, Sims NA (2013) Integrating endocrine and paracrine influences on bone: lessons from parathyroid hormone and parathyroid hormone-related protein. In: Thakker RW, Whyte MP, Eisman JA, Igarashi T (eds) Genetics of bone biology and skeletal disease. Academic Press, New York, pp 53–68
McCauley LK, Martin TJ (2012) Twenty-five years of PTHrP progress: from cancer hormone to multifunctional cytokine. J Bone Miner Res 27:1231–1239
Kronenberg HM (2006) PTHrP and skeletal development. Ann N Y Acad Sci 1068:1–13
Mak KK, Bi Y, Wan C, Chuang PT, Clemens T, Young M, Yang Y (2008) Hedgehog signaling in mature osteoblasts regulates bone formation and resorption by controlling PTHrP and RANKL expression. Dev Cell 14:674–688
Johnson RW, Nguyen MP, Padalecki SS, Grubbs BG, Merkel AR, Oyajobi BO, Matrisian LM, Mundy GR, Sterling JA (2011) TGF-beta promotion of Gli2-induced expression of parathyroid hormone-related protein, an important osteolytic factor in bone metastasis, is independent of canonical Hedgehog signaling. Cancer Res 71:822–831
Sterling JA, Oyajobi BO, Grubbs B, Padalecki SS, Munoz SA, Gupta A, Story B, Zhao M, Mundy GR (2006) The hedgehog signaling molecule Gli2 induces parathyroid hormone-related peptide expression and osteolysis in metastatic human breast cancer cells. Cancer Res 66:7548–7553
Lanske B, Karaplis AC, Lee K, Luz A, Vortkamp A, Pirro A, Karperien M, Defize LH, Ho C, Mulligan RC, Abou-Samra AB, Juppner H, Segre GV, Kronenberg HM (1996) PTH/PTHrP receptor in early development and Indian hedgehog-regulated bone growth. Science 273:663–666
Vortkamp A, Lee K, Lanske B, Segre GV, Kronenberg HM, Tabin CJ (1996) Regulation of rate of cartilage differentiation by Indian hedgehog and PTH-related protein. Science 273:613–622
Winkler DG, Sutherland MK, Geoghegan JC, Yu C, Hayes T, Skonier JE, Shpektor D, Jonas M, Kovacevich BR, Staehling-Hampton K, Appleby M, Brunkow ME, Latham JA (2003) Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J 22:6267–6276
Brunkow ME, Gardner JC, Van Ness J, Paeper BW, Kovacevich BR, Proll S, Skonier JE, Zhao L, Sabo PJ, Fu Y, Alisch RS, Gillett L, Colbert T, Tacconi P, Galas D, Hamersma H, Beighton P, Mulligan J (2001) Bone dysplasia sclerosteosis results from loss of the SOST gene product, a novel cystine knot-containing protein. Am J Hum Genet 68:577–589
Staehling-Hampton K, Proll S, Paeper BW, Zhao L, Charmley P, Brown A, Gardner JC, Galas D, Schatzman RC, Beighton P, Papapoulos S, Hamersma H, Brunkow ME (2002) A 52-kb deletion in the SOST-MEOX1 intergenic region on 17q12–q21 is associated with van Buchem disease in the Dutch population. Am J Med Genet 110:144–152
Balemans W, Patel N, Ebeling M, Van Hul E, Wuyts W, Lacza C, Dioszegi M, Dikkers FG, Hildering P, Willems PJ, Verheij JB, Lindpaintner K, Vickery B, Foernzler D, Van Hul W (2002) Identification of a 52 kb deletion downstream of the SOST gene in patients with van Buchem disease. J Med Genet 39:91–97
Loots GG, Kneissel M, Keller H, Baptist M, Chang J, Collette NM, Ovcharenko D, Plajzer-Frick I, Rubin EM (2005) Genomic deletion of a long-range bone enhancer misregulates sclerostin in van Buchem disease. Genome Res 15:928–935
Poole KE, van Bezooijen RL, Loveridge N, Hamersma H, Papapoulos SE, Lowik CW, Reeve J (2005) Sclerostin is a delayed secreted product of osteocytes that inhibits bone formation. FASEB J 19:1842–1844
Sims NA, Chia LY (2012) Regulation of sclerostin expression by paracrine and endocrine factors. Clin Rev Bone Miner Metab 10:98–107
Didangelos A, Yin X, Mandal K, Baumert M, Jahangiri M, Mayr M (2010) Proteomics characterization of extracellular space components in the human aorta. Mol Cell Proteomics 9:2048–2062
Modder UI, Clowes JA, Hoey K, Peterson JM, McCready L, Oursler MJ, Riggs BL, Khosla S (2011) Regulation of circulating sclerostin levels by sex steroids in women and in men. J Bone Miner Res 26:27–34
Li X, Ominsky MS, Niu QT, Sun N, Daugherty B, D’Agostin D, Kurahara C, Gao Y, Cao J, Gong J, Asuncion F, Barrero M, Warmington K, Dwyer D, Stolina M, Morony S, Sarosi I, Kostenuik PJ, Lacey DL, Simonet WS, Ke HZ, Paszty C (2008) Targeted deletion of the sclerostin gene in mice results in increased bone formation and bone strength. J Bone Miner Res 23:860–869
Lin C, Jiang X, Dai Z, Guo X, Weng T, Wang J, Li Y, Feng G, Gao X, He L (2009) Sclerostin mediates bone response to mechanical unloading through antagonizing Wnt/beta-catenin signaling. J Bone Miner Res 24:1651–1661
Ellies DL, Viviano B, McCarthy J, Rey JP, Itasaki N, Saunders S, Krumlauf R (2006) Bone density ligand, sclerostin, directly interacts with LRP5 but not LRP5G171 V to modulate Wnt activity. J Bone Miner Res 21:1738–1749
Balemans W, Piters E, Cleiren E, Ai M, Van Wesenbeeck L, Warman ML, Van Hul W (2008) The binding between sclerostin and LRP5 is altered by DKK1 and by high-bone mass LRP5 mutations. Calcif Tissue Int 82:445–453
Li X, Zhang Y, Kang H, Liu W, Liu P, Zhang J, Harris SE, Wu D (2005) Sclerostin binds to LRP5/6 and antagonizes canonical Wnt signaling. J Biol Chem 280:19883–19887
Semenov M, Tamai K, He X (2005) SOST is a ligand for LRP5/LRP6 and a Wnt signaling inhibitor. J Biol Chem 280:26770–26775
Leupin O, Piters E, Halleux C, Hu S, Kramer I, Morvan F, Bouwmeester T, Schirle M, Bueno-Lozano M, Fuentes FJ, Itin PH, Boudin E, de Freitas F, Jennes K, Brannetti B, Charara N, Ebersbach H, Geisse S, Lu CX, Bauer A, Van Hul W, Kneissel M (2011) Bone overgrowth-associated mutations in the LRP4 gene impair sclerostin facilitator function. J Biol Chem 286:19489–19500
Baron R, Kneissel M (2013) WNT signaling in bone homeostasis and disease: from human mutations to treatments. Nat Med 19:179–192
Cui Y, Niziolek PJ, MacDonald BT, Zylstra CR, Alenina N, Robinson DR, Zhong Z, Matthes S, Jacobsen CM, Conlon RA, Brommage R, Liu Q, Mseeh F, Powell DR, Yang QM, Zambrowicz B, Gerrits H, Gossen JA, He X, Bader M, Williams BO, Warman ML, Robling AG (2011) Lrp5 functions in bone to regulate bone mass. Nat Med 17:684–691
Xiong J, Onal M, Jilka RL, Weinstein RS, Manolagas SC, O’Brien CA (2011) Matrix-embedded cells control osteoclast formation. Nat Med 17:1235–1241
Xiao Z, Dallas M, Qiu N, Nicolella D, Cao L, Johnson M, Bonewald L, Quarles LD (2011) Conditional deletion of Pkd1 in osteocytes disrupts skeletal mechanosensing in mice. FASEB J 25:2418–2432
Hens JR, Wilson KM, Dann P, Chen X, Horowitz MC, Wysolmerski JJ (2005) TOPGAL mice show that the canonical Wnt signaling pathway is active during bone development and growth and is activated by mechanical loading in vitro. J Bone Miner Res 20:1103–1113
Robling AG, Niziolek PJ, Baldridge LA, Condon KW, Allen MR, Alam I, Mantila SM, Gluhak-Heinrich J, Bellido TM, Harris SE, Turner CH (2008) Mechanical stimulation of bone in vivo reduces osteocyte expression of Sost/sclerostin. J Biol Chem 283:5866–5875
Tian X, Jee WS, Li X, Paszty C, Ke HZ (2011) Sclerostin antibody increases bone mass by stimulating bone formation and inhibiting bone resorption in a hindlimb-immobilization rat model. Bone 48:197–201
Bonnet N, Standley KN, Bianchi EN, Stadelmann V, Foti M, Conway SJ, Ferrari SL (2009) The matricellular protein periostin is required for sost inhibition and the anabolic response to mechanical loading and physical activity. J Biol Chem 284:35939–35950
Atkins GJ, Rowe PS, Lim HP, Welldon KJ, Ormsby R, Wijenayaka AR, Zelenchuk L, Evdokiou A, Findlay DM (2011) Sclerostin is a locally acting regulator of late-osteoblast/preosteocyte differentiation and regulates mineralization through a MEPE-ASARM-dependent mechanism. J Bone Miner Res 26:1425–1436
Walker EC, McGregor NE, Poulton IJ, Solano M, Pompolo S, Fernandes TJ, Constable MJ, Nicholson GC, Zhang JG, Nicola NA, Gillespie MT, Martin TJ, Sims NA (2010) Oncostatin M promotes bone formation independently of resorption when signaling through leukemia inhibitory factor receptor in mice. J Clin Invest 120:582–592
Genetos DC, Yellowley CE, Loots GG (2011) Prostaglandin E2 signals through PTGER2 to regulate sclerostin expression. PLoS One 6:e17772
Genetos DC, Toupadakis CA, Raheja LF, Wong A, Papanicolaou SE, Fyhrie DP, Loots GG, Yellowley CE (2010) Hypoxia decreases sclerostin expression and increases Wnt signaling in osteoblasts. J Cell Biochem 110:457–467
Yang F, Tang W, So S, de Crombrugghe B, Zhang C (2010) Sclerostin is a direct target of osteoblast-specific transcription factor osterix. Biochem Biophys Res Commun 400:684–688
Kramer I, Keller H, Leupin O, Kneissel M (2010) Does osteocytic SOST suppression mediate PTH bone anabolism? Trends Endocrinol Metab 21:237–244
Sims NA (2010) Building bone with a SOST–PTH partnership. J Bone Miner Res 25:175–177
Keller H, Kneissel M (2005) SOST is a target gene for PTH in bone. Bone 37:148–158
Bellido T, Ali AA, Gubrij I, Plotkin LI, Fu Q, O’Brien CA, Manolagas SC, Jilka RL (2005) Chronic elevation of parathyroid hormone in mice reduces expression of sclerostin by osteocytes: a novel mechanism for hormonal control of osteoblastogenesis. Endocrinology 146:4577–4583
Kramer I, Loots GG, Studer A, Keller H, Kneissel M (2010) Parathyroid hormone (PTH) induced bone gain is blunted in SOST overexpressing and deficient mice. J Bone Miner Res 25:178–189
Robling AG, Kedlaya R, Ellis SN, Childress PJ, Bidwell JP, Bellido T, Turner CH (2011) Anabolic and catabolic regimens of human parathyroid hormone 1–34 elicit bone- and envelope-specific attenuation of skeletal effects in Sost-deficient mice. Endocrinology 152:2963–2975
Powell WF Jr, Barry KJ, Tulum I, Kobayashi T, Harris SE, Bringhurst FR, Pajevic PD (2011) Targeted ablation of the PTH/PTHrP receptor in osteocytes impairs bone structure and homeostatic calcemic responses. J Endocrinol 209:21–32
Tamura T, Udagawa N, Takahashi N, Miyaura C, Tanaka S, Yamada Y, Koishihara Y, Ohsugi Y, Kumaki K, Taga T, Kishimoto T, Suda T (1993) Soluble interleukin-6 receptor triggers osteoclast formation by interleukin 6. Proc Natl Acad Sci USA 90:11924–11928
Wong PK, Quinn JM, Sims NA, van Nieuwenhuijze A, Campbell IK, Wicks IP (2006) Interleukin-6 modulates production of T lymphocyte-derived cytokines in antigen-induced arthritis and drives inflammation-induced osteoclastogenesis. Arthritis Rheum 54:158–168
Poli V, Balena R, Fattori E, Markatos A, Yamamoto M, Tanaka H, Ciliberto G, Rodan GA, Costantini F (1994) Interleukin-6 deficient mice are protected from bone loss caused by estrogen depletion. EMBO J 13:1189–1196
Metcalf D, Gearing DP (1989) Fatal syndrome in mice engrafted with cells producing high levels of the leukemia inhibitory factor. Proc Natl Acad Sci USA 86:5948–5952
Sims NA, Walsh NC (2010) GP130 cytokines and bone remodelling in health and disease. BMB Rep 43:513–523
Sims NA, Johnson RW (2012) Leukemia inhibitory factor: a paracrine mediator of bone metabolism. Growth Factors 30:76–87
Mosley B, De Imus C, Friend D, Boiani N, Thoma B, Park LS, Cosman D (1996) Dual oncostatin M (OSM) receptors. Cloning and characterization of an alternative signaling subunit conferring OSM-specific receptor activation. J Biol Chem 271:32635–32643
Ichihara M, Hara T, Kim H, Murate T, Miyajima A (1997) Oncostatin M and leukemia inhibitory factor do not use the same functional receptor in mice. Blood 90:165–173
Fu Q, Jilka RL, Manolagas SC, O’Brien CA (2002) Parathyroid hormone stimulates receptor activator of NFkappa B ligand and inhibits osteoprotegerin expression via protein kinase A activation of cAMP-response element-binding protein. J Biol Chem 277:48868–48875
Kim S, Yamazaki M, Shevde NK, Pike JW (2007) Transcriptional control of receptor activator of nuclear factor-kappaB ligand by the protein kinase A activator forskolin and the transmembrane glycoprotein 130-activating cytokine, oncostatin M, is exerted through multiple distal enhancers. Mol Endocrinol 21:197–214
Walker EC, McGregor NE, Poulton IJ, Pompolo S, Allan EH, Quinn JM, Gillespie MT, Martin TJ, Sims NA (2008) Cardiotrophin-1 is an osteoclast-derived stimulus of bone formation required for normal bone remodeling. J Bone Miner Res 23:2025–2032
Poulton IJ, McGregor NE, Pompolo S, Walker EC, Sims NA (2012) Contrasting roles of LIF in murine bone development and remodeling involve region-specific changes in vascularization. J Bone Miner Res 27:902–912
McGregor NE, Poulton IJ, Walker EC, Pompolo S, Quinn JM, Martin TJ, Sims NA (2010) Ciliary neurotrophic factor inhibits bone formation and plays a sex-specific role in bone growth and remodeling. Calcif Tissue Int 86:261–270
Greenfield EM, Gornik SA, Horowitz MC, Donahue HJ, Shaw SM (1993) Regulation of cytokine expression in osteoblasts by parathyroid hormone: rapid stimulation of interleukin-6 and leukemia inhibitory factor mRNA. J Bone Miner Res 8:1163–1171
Walker EC, Poulton IJ, McGregor NE, Ho PW, Allan EH, Quach JM, Martin TJ, Sims NA (2012) Sustained RANKL response to parathyroid hormone in oncostatin M receptor-deficient osteoblasts converts anabolic treatment to a catabolic effect in vivo. J Bone Miner Res 27:902–912
Romas E, Udagawa N, Zhou H, Tamura T, Saito M, Taga T, Hilton DJ, Suda T, Ng KW, Martin TJ (1996) The role of gp130-mediated signals in osteoclast development: regulation of interleukin 11 production by osteoblasts and distribution of its receptor in bone marrow cultures. J Exp Med 183:2581–2591
Hirai H, Maru Y, Hagiwara K, Nishida J, Takaku F (1987) A novel putative tyrosine kinase receptor encoded by the eph gene. Science 238:1717–1720
Eph Nomenclature Committee (1997) Unified nomenclature for Eph family receptors and their ligands, the ephrins. Cell 90:403–404
Pasquale EB (2008) Eph–ephrin bidirectional signaling in physiology and disease. Cell 133:38–52
Murai KK, Pasquale EB (2003) ‘Eph’ective signaling: forward, reverse and crosstalk. J Cell Sci 116:2823–2832
Irie N, Takada Y, Watanabe Y, Matsuzaki Y, Naruse C, Asano M, Iwakura Y, Suda T, Matsuo K (2009) Bidirectional signaling through ephrinA2–EphA2 enhances osteoclastogenesis and suppresses osteoblastogenesis. J Biol Chem 284:14637–14644
Zhao C, Irie N, Takada Y, Shimoda K, Miyamoto T, Nishiwaki T, Suda T, Matsuo K (2006) Bidirectional ephrinB2–EphB4 signaling controls bone homeostasis. Cell Metab 4:111–121
Ting MC, Wu NL, Roybal PG, Sun J, Liu L, Yen Y, Maxson RE Jr (2009) EphA4 as an effector of Twist1 in the guidance of osteogenic precursor cells during calvarial bone growth and in craniosynostosis. Development 136:855–864
Merrill AE, Bochukova EG, Brugger SM, Ishii M, Pilz DT, Wall SA, Lyons KM, Wilkie AO, Maxson RE Jr (2006) Cell mixing at a neural crest–mesoderm boundary and deficient ephrin–Eph signaling in the pathogenesis of craniosynostosis. Hum Mol Genet 15:1319–1328
Wieland I, Jakubiczka S, Muschke P, Cohen M, Thiele H, Gerlach KL, Adams RH, Wieacker P (2004) Mutations of the ephrin-B1 gene cause craniofrontonasal syndrome. Am J Hum Genet 74:1209–1215
Davy A, Bush JO, Soriano P (2006) Inhibition of gap junction communication at ectopic Eph/ephrin boundaries underlies craniofrontonasal syndrome. PLoS Biol 4:e315
Xing W, Kim J, Wergedal J, Chen ST, Mohan S (2010) Ephrin B1 regulates bone marrow stromal cell differentiation and bone formation by influencing TAZ transactivation via complex formation with NHERF1. Mol Cell Biol 30:711–721
Himanen JP, Chumley MJ, Lackmann M, Li C, Barton WA, Jeffrey PD, Vearing C, Geleick D, Feldheim DA, Boyd AW, Henkemeyer M, Nikolov DB (2004) Repelling class discrimination: ephrin-A5 binds to and activates EphB2 receptor signaling. Nat Neurosci 7:501–509
Himanen JP, Rajashankar KR, Lackmann M, Cowan CA, Henkemeyer M, Nikolov DB (2001) Crystal structure of an Eph receptor–ephrin complex. Nature 414:933–938
Allan EH, Hausler KD, Wei T, Gooi JH, Quinn JM, Crimeen-Irwin B, Pompolo S, Sims NA, Gillespie MT, Onyia JE, Martin TJ (2008) EphrinB2 regulation by PTH and PTHrP revealed by molecular profiling in differentiating osteoblasts. J Bone Miner Res 23:1170–1181
Martin TJ, Allan EH, Ho PW, Gooi JH, Quinn JM, Gillespie MT, Krasnoperov V, Sims NA (2010) Communication between ephrinB2 and EphB4 within the osteoblast lineage. Adv Exp Med Biol 658:51–60
Takyar FM, Tonna S, Ho PW, Crimeen-Irwin B, Baker EK, Martin TJ, Sims NA (2013) EphrinB2/EphB4 inhibition in the osteoblast lineage modifies the anabolic response to parathyroid hormone. J Bone Miner Res 28:912–925
Arthur A, Zannettino A, Panagopoulos R, Koblar SA, Sims NA, Stylianou C, Matsuo K, Gronthos S (2011) EphB/ephrin-B interactions mediate human MSC attachment, migration and osteochondral differentiation. Bone 48:533–542
Tierney EG, McSorley K, Hastings CL, Cryan SA, O’Brien T, Murphy MJ, Barry FP, O’Brien FJ, Duffy GP (2013) High levels of ephrinB2 over-expression increases the osteogenic differentiation of human mesenchymal stem cells and promotes enhanced cell mediated mineralisation in a polyethyleneimine–ephrinB2 gene-activated matrix. J Control Release 165:173–182
Arthur A, Panagopoulos RA, Cooper L, Menicanin D, Parkinson IH, Codrington JD, Vandyke K, Zannettino AC, Koblar SA, Sims NA, Matsuo K, Gronthos S (2013) EphB4 enhances the process of endochondral ossification and inhibits remodeling during bone fracture repair. J Bone Miner Res 28:926–935
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have stated that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Tonna, S., Sims, N.A. Talking among Ourselves: Paracrine Control of Bone Formation within the Osteoblast Lineage. Calcif Tissue Int 94, 35–45 (2014). https://doi.org/10.1007/s00223-013-9738-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-013-9738-2