Abstract
Background
The subthalamic nucleus (STN) has only recently been considered to have a role in reward processing. In rats, inactivation of the STN by lesion or high-frequency stimulation (HFS) decreases motivation for cocaine but increases motivation for sucrose. For ethanol, the effect of STN lesion depends on the individual’s baseline intake; decreasing motivation for ethanol in rats with lower ethanol intake, while increasing motivation for ethanol in rats with higher—but still limited—ethanol intake. However, the involvement of the STN in behaviour more closely resembling some aspects of alcohol use disorder has not been assessed. This study aimed to determine the effect of STN lesions on the escalation of ethanol intake, subsequent increases in the motivation to “work” for ethanol and the choice of ethanol over a non-drug alternative.
Results
We found that STN lesion prevented increases in ethanol intake observed during intermittent ethanol access and after a long period of ethanol privation. STN lesion also decreased the motivation to work for ethanol after escalated intake. Surprisingly, STN lesion increased the choice of alcohol over saccharin. This was associated with a blunting of the hedonic responses to the taste of the reinforcement alternatives.
Conclusion
These results evidence the involvement of the STN in different ethanol-motivated behaviours and therefore position the STN as an interesting target for the treatment of alcohol use disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although pharmacological treatments for alcohol use disorder exist, they often have poor therapeutic efficacy or heterogeneous outcomes. The therapeutic use of lesions in the treatment of alcoholism (Li et al. 2012) is problematic due to concerns originally raised in the 1950s; primarily, those off-target consequences of ablations are irreversible. Thus, interest in reversible and adaptable deep brain stimulation techniques has grown as a neurosurgical treatment alternative for mental illnesses (Pelloux and Baunez 2013). High-frequency stimulation (HFS) of the nucleus accumbens (NAc) has already been tested in alcoholic patients and appears to have therapeutic benefit (Müller et al. 2009). However, the NAc is involved in all motivated behaviours, including those directed toward non-drug, natural sources of satisfaction (Cardinal and Everitt 2004). The optimal treatment of addiction would be one that reduces the desire for drugs without disrupting the desire for natural reward. Preclinical studies have shown a decrease in motivation for food after NAc HFS (Van der Plasse et al. 2012; Guercio et al. 2014). Accordingly, limbic symptoms are sometimes observed in patients with deep stimulation of the NAc (for review, see Pelloux and Baunez 2013).
An alternative target for neurosurgical intervention is the subthalamic nucleus (STN). Inactivation of the STN, by lesion or HFS, in rats reduces the motivation for cocaine in a similar manner to inactivation of the NAc. However, STN inactivation is quite different from NAc inactivation, in that STN inactivation increases motivation for food in rats (Baunez et al. 2005; Rouaud et al. 2010). In agreement, Parkinsonian patients, who develop abusive intake of their dopaminergic medication, reduce this intake once treated with STN HFS for their motor symptoms (Witjas et al. 2005; Lhommee et al. 2012; Eusebio et al. 2013), while evidencing weight gain (Barichella et al. 2003). In addition, remission from obsessive compulsive disorders following STN HFS (Mallet et al. 2002; Mallet et al. 2008) has further strengthened the interest of targeting the STN for HFS in treating psychiatric disorders, especially pathologies characterized by a compulsive behaviour and impaired impulse control. Therefore, the possibility of targeting the STN in the treatment of substance use disorder remains of particular interest (for review, see Pelloux and Baunez 2013).
HFS reduces the activity of neurons within a target structure, while also stimulating fibres passing near the site (McCracken and Grace 2007). Lesion of the STN in animal models can produce the same desirable behavioural consequences of HFS (Limousin et al. 1995) and therefore is useful to establish the potential benefit of targeting this structure. The use of lesions is also of interest in its own right, as this may be the only treatment option for patients who cannot be offered DBS (Lévêque et al. 2013).
In the case of alcohol, our laboratory has previously studied ethanol drinking in rats and found that lesion of the STN had mixed effects on motivation for ethanol, which depended upon the baseline intake of the individual (decreasing motivation in low ethanol drinkers and increasing motivation in high ethanol drinkers) (Lardeux and Baunez 2008). However, this manipulation was performed in rats with moderate levels of ethanol. The present study aimed to expand this previous study by manipulating the STN in rats with escalated ethanol consumption and behaviour which more closely resembles some of the defining aspects of substance use disorders observed in humans. The primary measures of interest were the escalation of ethanol intake, the subsequent increase in motivation to “work” for ethanol and the choice of ethanol over a non-drug alternative.
The repeated self-administration of intoxicating levels of ethanol results in an escalation of drug intake, which can lead to loss of control over drug consumption, one of the hallmark features of substance use disorders (Koob et al. 2004). When given ethanol intermittently, rats show an escalation of ethanol intake to levels which produce pharmacologically relevant blood ethanol concentrations, able to cause intoxication and equivalent to levels obtained in selectively in-bred alcohol preferring rats (Simms et al. 2008; Bell et al. 2006; Wise 1973). The recurring cycles of intoxication and deprivation in this simple preparation show similarities to binge drinking observed in human suffering alcohol use disorder, therefore granting it some validity as a preclinical model of alcohol use disorders (for review Carnicella et al. 2014). Previous data have shown that STN inactivation does not affect ethanol consumption in rats with moderate, non-escalated intake but does alter escalated intake of heroin (Wade et al. 2017). The question remains whether this effect generalizes to escalated ethanol intake. In addition to the escalation of drug intake, substance use disorder is also characterized by the appearance of other defining features. For example, a great deal of time is devoted to obtaining or consuming the drug (DSM-V, American Psychiatric Association 2013). We thus aimed to clarify the effect of manipulating the STN on the motivation for ethanol after escalated intake. To address this, we measured motivation in a progressive ratio (PR) schedule of reinforcement. However, as pointed out by Ahmed (2010), an important feature of substance use disorders is the choice of drug to the exclusion of alternatives for reinforcement. Therefore, we also assessed the discrete choice between ethanol and saccharine, using the same design used by Ahmed et al. for cocaine or heroin. In these studies, most rats prefer sweet solutions (e.g., saccharine) over cocaine (Lenoir et al. 2007) or heroin (Lenoir et al. 2013). Notably, in contrast to cocaine and heroin that are mainly injected, ethanol is commonly ingested. Giving exclusive choice between ethanol or sweet solutions presents three advantages: (i) the consummatory responses are similar for each reinforcer, (ii) the consummatory response for each reinforcer recruits the same sensory modalities and (iii) the affective responses to the taste of each reinforcer can be monitored by parallel assessment of taste reactivity.
While it is known that the taste of ethanol, especially at high concentration, is initially aversive in rats (Kiefer and Dopp 1989), the question remains whether affective appraisal of the ethanol solution would change after escalated intake. Thus, we measured the orofacial responses to non-contingent ethanol exposure both before and after escalation of ethanol intake. Considering the role of the STN in the hedonic valuation of sweetened solutions, and affective processes in general (Pelloux et al. 2014; Péron et al. 2013), we aimed to determine whether STN lesion would modify affective responses to ethanol (Pelloux et al. 2014).
We hypothesised that STN lesion would reduce the rewarding effects of ethanol (i.e. decreases the escalated intake) and reduce the motivation for ethanol (i.e. reduces willingness to “work” for ethanol following intermittent access to ethanol). We further hypothesised that reduced reinforcement derived from ethanol would mean that STN lesioned rats would show a reduction in their choice of ethanol over saccharin. We also hypothesised that STN lesion after escalation would blunt conditioned hedonic responses elicited by the taste of ethanol.
Material and methods
Subjects
Sixty-two male outbred Long Evans rats (Janvier, Le Genest St Isle, France), weighing ~320 g upon arrival, were housed in pairs in polycarbonate cages (L = 40 cm, W = 25 cm, H = 18 cm) and maintained under a 12-h light/dark cycle (lights on at 7:00 a.m.) at a constant temperature (21 ± 1 °C), with free access to laboratory chow (Scientific Animal Food & Engineering, Augy, France) and water. All procedures were conducted in accordance with the European Community Council Directive of November 24, 1986 (86/609/EEC), and the National French Agriculture and Forestry Ministry (decree 87–849). It has received the approval by the local ethics committee.
General procedure
As illustrated in Fig. 1, 1 week after arrival, 40 rats were allowed intermittent access to ethanol (experiments 2 and 3), while the remaining 22 rats received surgery (experiment 1). Sham and STN lesioned rats from the first experiment were implanted with intraoral fistula for measurement of hedonic and aversive orofacial reactions to presentation of novel, increasing concentrations of ethanol (5, 10 and 20% v/v). Two days later, the same rats had intermittent access of ethanol solution for 12 sessions, after which they were sacrificed and their brains were collected.
Flowchart of the simplified experimental procedure. For details, see “Materials and methods” section
Rats from the second and third experiments were given 15 sessions of intermittent access to ethanol and then underwent surgery. The rats were left to recover in their homecage for 20 days and then re-exposed to ethanol in five intermittent access sessions. The population was then divided in two groups. One group was assessed for instrumental performance under a fixed ratio schedule of reinforcement for 10 days and under a progressive ratio (PR) schedule of reinforcement for a further 10 days. The other group was assessed for discrete choice between ethanol and saccharin. Once completed, the animals in experiment 3 were implanted with intraoral fistulae for assessment of taste reactivity for these two agents 2 days later.
Surgeries
Subthalamic nucleus manipulation
Rats weighting no less than 380 g were anaesthetised with subcutaneous injection of 30 mg (100 mg/mL) ketamine (Imalgene, Merial, Lyon, France) and 8.5 μg (85 μg/mL) Medetomidine (Domitor, Janssen, Issy-les-Moulineaux, France) and placed in the stereotaxic frame (David Kopf Instruments, Tujunga, USA). Bilateral 30-gauge stainless-steel injector needles connected by Tygon tubing (internal diameter 0.25 mm, Saint Gobain performance plastics) to a 10-μL Hamilton microsyringe (Bonaduz, Switzerland) fixed on a micropump (CMA, Kista, Sweden) were stereotaxically positioned into the STN (anteroposterior −3.7, lateral ±2.4 from bregma, dorsoventral −8.35 from skull, with tooth bar set at −3.3 mm) (Paxinos and Watson 2005). Rats in the STN lesioned group were subjected to axon-sparing excitotoxic lesions, made by infusing 0.5 μL of 53 mM of ibotenic acid (9.4 μg/μL, Abcam Biochemical, Cambridge, UK), while sham-injected control rats received bilateral injections of vehicle solution (phosphate buffer, 0.1 M) over 3 min.
2.3.2. Intraoral fistula implantation
A 6-cm length of PE-100 tubing was implanted using similar procedure as that used by Roitman et al. (2008) and as described previously (Pelloux et al. 2014). Rats were allowed at least 1 week to recover from surgery.
Affective responses to ethanol before (experiment 1) or after escalated ethanol intake (experiment 3): taste reactivity
Apparatus, procedure and analysis were similar to those described previously (Pelloux et al. 2014). Briefly, for two habituation days, each rat was connected to the fistula and placed into a cylinder for 2 min. Then, 1 mL of water was then injected in the mouth over 30 s. On day 3, 30-s infusions of increasing concentrations of ethanol (5, 10 and 20% v/v) were administered, separated by 2-min wash-out periods. In experiment 3, a fourth day was added, where animals received a single 30-s saccharin (0.2 M) injection.
Sessions were recorded and later were manually scored for hedonic (rhythmic tongue protrusions) and aversive responses (nose rubbing, wet dog shakes and gapes) occurring during the 30-s infusion periods.
Escalation of ethanol intake: intermittent access to ethanol
Animals were isolated and had free access to food and water. A bottle of 20% ethanol (v/v) was presented for a 14-h session (from 7:00 p.m. to 9:00 a.m.) concurrent with water access (i.e. a two-bottle choice). The ethanol bottle was weighed before and after presentation, in order to estimate consumption. Following ethanol presentation, rats were subjected to 58 h without ethanol, before the next session began. The placement of the bottles in the cage was alternated from session to session to control for side preferences.
Assessing motivation for ethanol with FR1 and PR schedules of reinforcement
Apparatus
Each of the four operant conditioning chambers (29.5 × 32.5 × 23.5 cm; Med Associates, Georgia, VT, USA) was placed within a sound-attenuating and light-attenuating enclosure equipped with a ventilation fan that also masked external noise. Chambers were equipped with two 4-cm-wide retractable levers that were mounted in one sidewall 12 cm apart and 8 cm above the grid floor. Above each lever was a cue light (2.5 W, 24 V). A houselight (2.5 W, 24 V) was located at the level of the ceiling and, just under, there was a buzzer (3.5 kHz). On the opposite wall, there were two recessed magazines (3.8-cm high and 3.8-cm wide and 5.5 cm from the grid floor) containing each a single cup liquid receptacle with an 18-gauge pipe, connected via Tygon tubing to a 10-mL syringe mounted on a Razel infusion pump (Semat Technical, UK) located outside the outer enclosure. Entry into each magazine was detected by the interruption of an infrared photo-beam. The operant conditioning chambers were controlled by MED IV PC software.
Procedure
After ethanol magazine training, rats were trained to press on levers located on one side of the operant box and collect the reinforcer (0.1 mL of 20% ethanol solution) in the recessed magazine on the opposite side of the operant box. In experiment 2, both right and left levers were presented but pressing on only one of them (counterbalanced across rats) resulted in ethanol delivery, coupled with onset of the 2-s stimulus light (located directly above the pressed lever) according to a continuous schedule of reinforcement (fixed ratio 1 (FR1)). Rats were trained for 10 consecutive days, and daily sessions ended when rats had obtained 100 rewards or 30 min had elapsed. Rats were then subjected to a PR schedule of reinforcement for 10 consecutive days. In this task, the number of lever presses required to obtain a single reward began at one, and increased by five, after the completion of every three ratios (i.e. 1, 1, 1, 5, 5, 5, 10, 10, 10, 15, 15, 15…), as previously used with ethanol (Lardeux and Baunez 2008). Ratio completion resulted in the delivery of 0.1 mL of 20% ethanol and the onset of the stimulus light. The session ended if the rat failed to lever press for 5 min or if 90 min had elapsed. For each session, the value reached during the last ratio and the number of rewards obtained were recorded.
Assessing choice between ethanol and a non-drug alternative using a discrete choice procedure
In experiment 3, once magazine training was completed, rats were subjected to a discrete choice procedure, where 0.1 mL of 0.2% saccharin or 20% ethanol was available in a mutually exclusively choice. As previously described (Pelloux et al. 2014), sessions began with four sampling trials separated by 1-min time outs. For each sampling trial, only one of the two levers was available. Once pressed, it was retracted with the onset of the corresponding 2-s conditioned stimulus (buzzer or light, counterbalanced among rats) and the delivery of the corresponding reward (0.125 mL of saccharin or ethanol). On the following sampling trial, the other lever was presented and this sequence of two sampling trials was repeated once, so that each option was experienced twice. Then, for 20 trials, both levers were inserted. Responding on one lever resulted in the retraction of both levers and the reward chosen delivered in the corresponding receptacle.
Histological assessment
At the end of the experiments, rats were euthanized with pentobarbital sodium (Dolethal, Vetoquinol, Lure, France, 73 mg/mL, 1.5 mL i.p.). Their brains were removed, frozen in isopentane (Sigma-Aldrich) and kept at −80 °C, then they were sectioned coronally at 50-μm thickness with a cryostat. Sections were later stained with Cresyl Violet (Fluka Chemika) to assess location and extent of the lesion.
Statistical analyses
Results were analysed through mixed analyses of variance. Each ANOVA was preceded by a Mauchly’s test of sphericity to confirm homogeneity of variance. When sphericity was violated, a Huynh-Feldt correction factor was applied to the degree of freedom and the residual, in order to reduce type I error.
During intermittent access to ethanol, the relative preference for ethanol was calculated as the volume of ethanol consumed divided by the total volume of liquids consumed (i.e. water and ethanol) and multiplied by 100. The relative preference for ethanol and the ethanol intake (g/kg/14 h) across intermittent exposure to ethanol (all experiments) and between the last 5 days before surgery and the 5 days after surgery (experiments 2 and 3) were compared between sham and STN lesioned animals using mixed two-way ANOVA with “group” (sham or STN lesion) as between subject factor and “Sessions” as within subject factor. ANOVA was followed by Bonferroni post hoc comparison when appropriate. This same analysis was performed on post-escalation performance of sham and STN lesioned animals (number of reinforcements and the number of magazine entries) under FR1 and PR schedules of reinforcement. In experiment 3, this same analysis was again performed on saccharin preference, which was computed as the number of choices for saccharin minus the number of choices for ethanol over the total number of choices.
Affective responses to ethanol were assessed by positive and negative orofacial responses. Mixed three-way ANOVAs with “group” (sham or STN lesion) as between subject factor and “concentration” (5, 10 and 20%) and “type of affective responses” (positive or negative) as within subject factors were performed separately for rats presented ethanol for the first time and for rats tested post-escalation. Similar mixed three-way ANOVAs with “ethanol history” (first exposure or after escalation) as a between subject factor instead of “type of affective responses” were performed for each type of response (positive and negative). Further post hoc evaluations were conducted using mixed two-way ANOVAs with “group” as between subject factor and “concentration” as within subject factor for both ethanol history and for both types of affective responses. Finally, positive or aversive responses after escalated intake were further analysed separately with mixed two-way ANOVAs with “group” as between subject factor and “type of reinforcer” (ethanol or saccharin) as within subject factor. For the correlation analyses, we performed Spearman correlations tests between affective responses and the saccharine preference. For all statistical tests, the significance level was pre-determined at α = 0.05.
Results
Histology
The sites and extent of lesions were characterized by a neuronal loss and associated gliosis and are illustrated in Fig. 2. Three out of 13 in experiment 1, 3 out of 12 in experiment 2 and 5 out of 12 animals in experiment 3 were excluded from the STN lesioned group for unsatisfactory lesions, being either too restricted or outside the STN. The 10 STN lesioned rats in experiment 1 were compared to nine sham controls, the nine STN lesioned rats in experiment 2 compared to seven sham controls and the seven STN lesioned rats in experiment 3 compared to eight sham controls.
Left panel: schematic representations of the subthalamic lesions on standardized sections of the rat brain. The numbers adjoining each section refer to distances from bregma (adapted from Paxinos and Watson 2015). Right panel: picture from a representative lesion. The STN is delineated by the dashed line. It lays above the cerebral peduncle (cp)
Experiments 1, 2 and 3: escalation of ethanol consumption: intermittent access to ethanol
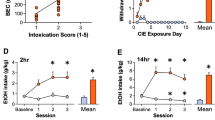
Rats subjected to STN lesions or sham surgeries prior to any ethanol experience showed different ethanol intake throughout intermittent presentation of 20% ethanol solution [group effect: F(1, 17) = 4.5, p < 0.05]. Sham rats progressively increased intake [session effect: F(6.4, 51.2) = 4.1, p < 0.01] as previously described (Wise 1973). Their increase in intake differed from the first exposure from session 9 onward [ps ≤ 0.001]. In contrast, STN lesioned rats maintained stable ethanol intake [F(4.4, 39.8) < 1, not significant (NS)]. This led to a significant difference in intake between groups on session 11 [p < 0.05] (Fig. 3a). Similarly, sham and STN lesioned rats differed in the relative “preference” for ethanol throughout intermittent access sessions [group effect: F(1, 187) = 4.3, p = 0.05]. Sham rats progressively increased their relative preference for ethanol [session effect: F(9.6, 76.9) = 4.8, p < 0.001]. The preference was significantly greater than during the first exposure from session 10 onward [ps < 0.001]. In contrast, STN lesioned animals had stable intake [F(4.9, 44.2) < 1, NS] (Fig. 3c). Sham and STN lesion rats differed for the last two sessions [p < 0.05].
a Mean ethanol intake and c mean relative "preference" for ethanolacross the 12 sessions of intermittent access to ethanol in sham (n = 9, white dots) and STN lesioned animals (n = 10, black dots) for which surgeries were performed before any ethanol presentation. b Mean ethanol intake and d mean relative "preference" for ethanolacross the 25 sessions of intermittent access to ethanol of sham (n = 15, white bars) and STN lesioned animals (n = 16, black bars) for which surgeries were performed once ethanol intake was escalated (after the 20th days). a Significant differences between sham and lesioned animals Bonferroni p < 0.05. b Significantly different from session 1 Bonferroni ps < 0.05
Animals for which STN or sham lesions were performed after having escalated ethanol intake and preference [session effect: F(4, 111.2) = 12.6, p < 0.001; F(6.5, 181.8) = 20.5, p < 0.001, respectively, for ethanol intake and ethanol preference] had comparable escalated intake and preference before surgery [group effect F(1, 392) < 1, NS; F(1, 392) < 1, NS; group × session interaction F(3.9, 111.2) < 1, NS, and F(6.5, 181.8) < 1, NS]. Consecutively, STN lesioned rats significantly differed from their sham counterparts when intermittently re-exposed to 20% ethanol solution after 20 days post-surgical recovery [group × session interaction: F(4.1, 114.5) = 2.7, p < 0.05 and F(5.3, 148) = 2.4, p < 0.05, respectively, for ethanol intake and ethanol “preference”]. Sham animals kept increasing their intake [F(3.9, 54.1) = 2.7, p < 0.01] at re-exposure, while consumption remained stable in the STN lesion group [F(9, 126) = <1, NS] (Fig. 3b).
Experiment 2: motivation for ethanol: FR1 and PR performance
STN lesion and sham rats had similar ethanol intake under FR1 schedule of reinforcement [group effect F(1, 126) = 4, NS; group × session interaction: F(6.3, 88.6) = 1, NS] (Fig. 4a). Both groups consumed around 1 ± 0.1 g/kg over the 30-min session. However, STN lesioned rats made less magazine entries than sham rats [group effect: F(1, 126) = 5.9, p < 0.05] (Fig. 4c).
L eft panels: mean ± SEM number of ethanol reinforcers earned (a) and number of magazine entries (c) per session under a fixed ratio schedule of reinforcement in sham (n = 7, white dots) and STN lesioned animals (n = 9, black dots). Right panels: mean ± SEM number of ethanol reinforcers earned (b) and number of magazine entries (d) under a progressive ratio schedule of reinforcement in sham (n = 7, white dots) and STN lesioned animals (n = 9, black dots). Asterisk: significant group effect, mixed two-way ANOVA, p < 0.05
Under the PR schedule of reinforcement, the number of reinforcements earned remained stable across days [session effect: F(7.4, 104) = 1.1, NS]. Lesioned rats earned significantly less ethanol than sham rats [group effect: F(1, 126) = 4.9: p < 0.05] (Fig. 4b). Sham rats consumed on average 0.23 ± 0.02 g/kg/session and STN lesioned rats 0.2 ± 0.01 [T(14) = 1.8: p < 0.05]. The average break point was stable over the 10 days [session effect: F(7.7, 107.7) = 1.2, NS] and tended to be lower for STN lesioned rats than for sham controls [9 ± 1 vs 12 ± 1, respectively; group effect: F(1, 14) = 4.3, p = 0.06]. Magazine entries were not different between groups [group effect: F(1, 126) = 2, NS; group × session interaction: F(6.3, 88.6) = 1.2, NS] (Fig. 4d).
Experiment 1 and 3 affective responses to ethanol
During the initial taste reactivity test, two lesioned rats were excluded due to patency failure of the intraoral fistula. Animals exposed for the first time to ethanol exhibited much more aversive than hedonic responses to intraoral passive infusions of ethanol [effect of type of affective response: F(1, 30) = 5.5, p < 0.05]. In contrast to sham animals, STN lesioned animals showed general blunted responses to the taste of ethanol [group effect: F(1, 30) = 18, p < 0.01] (Fig. 5a).
Mean ± SEM number of aversive and hedonic reactions to increasing concentration of ethanol (5, 10 and 20% v/v) presented for the first time (a) or following escalated ethanol intake (b) in sham (n = 9 and 7, respectively, white bars) and STN lesioned (n = 8 and 7, respectively, black bars) animals. Double asterisk: significant group effect, mixed three-way ANOVA, p < 0.01. Number sign: significant effect of type of affective responses, mixed three-way ANOVA, p < 0.05. Dollar sign: significant effect of ethanol history, mixed three-way ANOVA, p < 0.001
After having escalated their ethanol intake, animals showed reduced aversive responses compared to animals experiencing the taste of ethanol for the first time [effect of ethanol history: F(1, 27) = 14.9, p < 0.001]. No difference in aversive responses between sham and lesioned animals was observed at this later stage [group effect: F(1, 27) = 3, NS; group × concentration interaction: F(1.7, 46.6) < 1, NS] (Fig. 5b).
In contrast to aversive reactions, no significant changes in the hedonic reactions occurred after escalation of ethanol intake [effect of ethanol history: F(1, 27) < 1, NS; ethanol history × concentration interaction: F(1.7, 44.7) = 2.7, NS]. STN lesions did not affect hedonic responses [effect of group: F(1, 27) = 1.3, NS; group × concentration interaction: F(1.7, 44.7) < 1, NS; group × ethanol history: F(1, 27) < 1, NS; group × ethanol history × concentration interaction: F(1.7, 44.7) < 1, NS].
Experiment 3: discrete choice
Since preferences of subgroups trained with conditioned stimuli of different modality (buzzer versus light) were not significantly different [effect of stimulus modality: F(1, 209) = 1.6, NS; stimulus modality × session interaction F(19, 209) < 1, NS], results were pooled and further analysed across conditions. When given mutually exclusive choice between ethanol and saccharin, sham and STN lesion rats strikingly differed regarding their choice [group effect: F(1, 13) = 7.3, p < 0.05; group × session interaction: F(8.6, 112.1) = 2.1, p < 0.05]. Indeed, sham animals expressed steady choice for saccharin [session effect: F(8.6, 59.9) < 1, NS], while lesioned animals transiently expressed preference for ethanol [F(6.2, 37.4) = 2.7, p < 0.05], followed by indifference (Fig. 6a).
a Mean ± SEM index of the preference for saccharin (positive score) or ethanol (negative score) solutions (expressed as the number of choices for saccharin–choices for ethanol on the total number of choices) for sham controls (white dots, n = 8) and STN lesioned rats (black dots, n = 7) that have previously escalated their ethanol intake. The dashed line represents the indecision point and any value above the grey area corresponds to significant preference for saccharin while any value below the grey area represents significant preference for the ethanol solution. Asterisk: significant group effect, mixed two-way ANOVA, p < 0.05. b Mean ± SEM number of aversive and hedonic reactions to intraoral infusion of 20% v/v ethanol or 0.2 M saccharin solutions following escalated ethanol intake in sham (n = 8, white bars) and STN lesioned (n = 7, black bars) animals. Asterisk: significant group effect, mixed two-way ANOVA, p < 0.05
Differential taste reactivity to the reinforcing liquids in sham and STN lesioned animals was investigated to account for the contrasted choice between groups. There was a significant interaction between the group and the type of response assessed [F(1, 12) = 10.1, p < 0.05]. There were very few aversive reactions to ethanol and saccharin solutions, and no significant differences were observed between groups [group effect: F(1, 12) = 2.5, NS; group × type of reinforcer interaction: F(1, 12) < 1, NS]. In contrast, STN lesioned rats exhibited fewer hedonic responses to both saccharin and ethanol compared to sham rats [group effect: F(1, 12) = 7.4, p < 0.05] (Fig. 6b).
The stabilized saccharine preference averaged across the last 15 days was not significantly correlated with the number of hedonic or aversive responses to saccharine or ethanol (ρs(12) < 0.41, NS).
Discussion
The results of this study suggest that inactivation of the STN is beneficial for reducing some features of alcohol use disorders. In line with our hypotheses, lesions of the STN prevented escalation of ethanol intake and rebound intake after deprivation following escalation. STN lesions, when performed after escalation of ethanol intake, also reduced motivation for ethanol in the progressive ratio (PR) schedule of reinforcement. However, contrary to our hypotheses, STN lesions shifted preference away from saccharin, toward ethanol. This was associated with a general blunting of affective responses to tastants.
To evaluate the effect of STN inactivation on escalation of ethanol intake, we gave rats intermittent access to highly concentrated ethanol solutions, in free choice with water. We found that sham control animals increased progressively their ethanol consumption across intermittent presentation to reach a consumption of about 4 g/kg/14 h. This level of consumption in Long Evans rats is similar to that observed by others (Simms et al. 2008). Notably, STN lesions prevented escalation of ethanol intake across intermittent access presentation. In experiments 2 and 3, animals with escalated ethanol intake were left to recover for 20 days after STN lesion or sham surgeries without access to ethanol. When intermittently re-exposed to ethanol, sham control rats further increased their intake. Increases in voluntary ethanol intake after a period of deprivation are commonly defined as the ethanol deprivation effect (Sinclair and Senter 1968). We observed that STN lesion prevented the increase in ethanol intake following the 20 days of ethanol deprivation. Therefore, lesions of the STN consistently precluded the increase in ethanol drinking resulting from deprivation, whatever the length (2 or 20 days) of deprivation enforced.
The analysis of consummatory behaviour suggests ethanol’s rewarding properties were reduced in STN lesioned animals. A similar conclusion could be drawn from analysing operant responding. STN lesioned animals showed a reduced number of magazine entries during FR1 responding. Anticipatory and perseverative nose poke responding in the food magazine is disrupted by outcome devaluation and hence sensitive to the motivational value of the outcome (Morrison et al. 2015; Baunez and Robbins 1997). This suggested reduced motivation for ethanol in STN lesioned rats that was further evidenced by reduced performance under PR. In line with these results, our laboratory previously reported that STN lesion decreases motivation for cocaine, measured by PR responding (Baunez et al. 2005).
We also found that STN lesions reduced the affective appraisal of ethanol. When infants, monkeys or rats are presented bitter or sour solutions on the lips or in the mouth, they express gapes, head shakes or nose rubbing. These orofacial responses are elicited specifically by solutions that are normally avoided. In contrast, solutions that are normally foraged (such as those containing sweet compounds) elicit different orofacial responses such as rhythmic tongue protrusions (Berridge 2000). Here, we evidenced aversive responding to the passive intraoral injection of ethanol in sham rats that were never exposed to ethanol. Importantly, STN lesions reduced these responses, therefore generalizing the previously described role of the STN in mediating affective responses to hedonic solutions, to include affective response to aversive tastants (Pelloux et al. 2014). These effects unlikely resulted from oral motor impairment. On the contrary, if any effect, STN inactivation should be expected to facilitate orofacial responses since it relieves oral motor deficit in Parkinsonian patients (Gentil et al. 2000). In addition, transient oral dyskinesia can be induced by inactivation of the STN (Mehta et al. 2005), although none were observed in the present experiments. Finally, potential motor effects of STN inactivation cannot account on its own for the affective blunt evidenced in other procedures, where motor responses have limited involvement (Pelloux et al. 2014).
After they had escalated their ethanol intake, rats displayed a significant reduction in aversive responses, suggesting that ethanol became less aversive. Sham rats exhibited a small increase in hedonic responding. Low level of hedonic responding exhibited by sham animals is in line with a previous study in animals continuously presented with low concentrations of ethanol (Kiefer and Dopp 1989). Despite the low level of hedonic responding exhibited by sham animals, lesioned rats showed even lower number of tongue protrusions to ethanol. Importantly, the blunted affective responding of STN lesioned animals was not limited to ethanol. We observed that STN lesioned rats also evidenced clear blunted responses to the hedonic taste of the sweet compound saccharin, in line with what was observed with sucrose in a previous study (Pelloux et al. 2014).
The altered affective appraisal of saccharin and ethanol solutions following STN lesion may explain the effects on choice between these two reinforces in the discreet choice paradigm. We observed that most sham rats, even after having escalated their ethanol intake, preferred saccharin. These results are in line with those of Ahmed’s lab showing preference of saccharine over cocaine persists despite escalation of cocaine self-administration (Ahmed 2010) but contrasts the finding that preference shifts away from saccharin toward heroin following heroin escalation. Why escalation of heroin but not escalation of cocaine or ethanol can shift preference toward the drug alternative remains unknown.
We found that STN lesioned animals displayed a temporary preference for ethanol. This preference unlikely results from increased motivation for ethanol, since STN lesioned rats reduced motivation under the PR. More likely, this preference emerged as a result of reduced motivation for saccharin. Saccharin is a sweetener devoid of any caloric intake, and so, its reinforcing effect relies solely on its hedonic taste. In rats with STN lesion which experience blunted affective responses to tastants, saccharin would be expected to cease functioning as a viable non-drug alternative. In contrast, ethanol has caloric value that contributes to its rewarding properties (Richter 1940). It is therefore highly possible that sham rats chose saccharin for its taste and STN lesioned chose ethanol for its caloric properties. Similarly, we previously found that when given the choice between saccharine and glucose solutions, saccharine is sweet tasting devoid of any calories whereas glucose is high in calories with a blander taste, STN lesioned animals developed a preference for glucose over saccharin (Pelloux et al. 2014) in contrast to sham animals which maintained a preference for saccharine. Furthermore, it has also been consistently demonstrated that inactivating the STN using lesion or high-frequency stimulation increases motivation for the sweetened and caloric tastant, sucrose (Baunez et al. 2005; Rouaud et al. 2010). The facilitating effect of STN inactivation on responding for sucrose encourages further studies to evaluate the benefit of inactivating the STN in reducing choice for the drug in favour of natural rewards with relevance for survival (e.g. caloric foods).
More generally, this study interrogates the importance of the STN affective blunt in substance use disorders. While the affective appraisal seems involved in the choice between the drug and a hedonic alternative, the affective appraisal of ethanol does not seem to be as relevant for its initial moderate consumption. Blunted aversive responding following lesion of the STN is not associated with greater ethanol intake during the initial exposure, in line with previous data showing no effect of STN lesion on the consumption of lower concentration (5%) ethanol (Lardeux and Baunez 2008). In addition, insensitivity to the aversive taste of ethanol in STN lesioned rats does not promote escalation of ethanol intake. It has been demonstrated that the blunting of affect induced by STN lesion includes the blunting of negative emotional states (Pelloux et al. 2014). An interesting possibility that remains to be tested is whether the ability of STN manipulations to reduce escalated drinking is in part due to a disruption of the negative emotional states which have been hypothesised to drive compulsive-like drinking (Tunstall et al. 2017).
Whether the rats are dependant after intermittent access in the present study is debatable. Previous data have evidenced that a subpopulation of rats shows compulsive ethanol intake, that is despite quinine adulteration of the ethanol solution, after 2 months of intermittent access, as performed in this study (Spoelder et al. 2015). However, other studies have demonstrated the emergence of compulsive ethanol intake only after 3 to 4 months and not 1.5 months of intermittent access (Hopf et al. 2010). The interest of targeting the STN for the treatment of alcohol use disorder evidenced here remains to be demonstrated in “dependent” subjects, i.e. rats displaying physical and psychological ethanol dependence for instance after repeated ethanol vapour intoxication.
This study also interrogates the importance of affective processes in substance use disorders and especially the relevance of mitigating affectivity in the treatment of substance use disorders. The insular cortex, a structure that projects to the STN (Berendse and Groenewegen 1991), is proposed to interpret interoceptive stimuli and convert them into emotional states (Damasio 2000). Notably, inactivation of the insular cortex reduces craving for cocaine in rats (Contreras et al. 2007). This agrees with clinical data reporting smoking cessation after brain damage involving the insula (Naqvi et al. 2007). Similarly, affective blunting following STN inactivation may show a therapeutic potential in pathologies characterized by exacerbated affective processes such as addictive disorders, where disturbed emotions, for instance craving and anxiety, contribute to the maintenance of drug use. This remains even more interesting when we consider that inactivation of the STN spares motivated behaviours when the focus of reinforcement is relevant for survival (Baunez et al. 2005; Rouaud et al. 2010), likely allowing addicted individuals to reallocate behaviours toward essential activities. As a conclusion, these results evidence an important role of the STN in alcohol use disorders, further supporting the STN as an interesting target for the treatment of addictive disorders.
References
Ahmed SH (2010) Validation crisis in animal models of drug addiction: beyond non-disordered drug use toward drug addiction. Neurosci Biobehav Rev 35(2):172–184
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders, 5th edn. American Psychiatric Association, Washington
Barichella M, Marczewska AM, Mariani C, Landi A, Vairo A, Pezzoli G (2003) Body weight gain rate in patients with Parkinson's disease and deep brain stimulation. Mov Disord 18:1337–1340
Baunez C, Robbins TW (1997) Bilateral lesions of the subthalamic nucleus induce multiple deficits in an attentional task in rats. Eur J Neurosci 9(10):2086–2099
Baunez C, Dias C, Cador M, Amalric M (2005) The subthalamic nucleus exerts opposite control on cocaine and natural rewards. Nat Neurosci 8:484–489
Bell RL, Rodd ZA, Lumeng L, Murphy JM, McBride WJ (2006) The alcohol-preferring P rat and animal models of excessive alcohol drinking. Addict Biol 11:270–288
Berendse HW, Groenewegen HJ (1991) The connections of the medial part of the subthalamic nucleus in the rat: evidence for a parallel organization. In: Bernardi G, Carpenter MB, Di Chiara G, Morelli M, Stanzione P (eds) The basal ganglia III. Plenum, New York, pp 89–98
Berridge KC (2000) Measuring hedonic impact in animals and infants: microstructure of affective taste reactivity patterns. Neurosci Biobehav Rev 24:173–198
Cardinal RN, Everitt BJ (2004) Neural and psychological mechanisms underlying appetitive learning: links to drug addiction. Curr Opin Neurobiol 14:156–162
Carnicella S, Ron D, Barak S (2014) Intermittent ethanol access schedule in rats as a preclinical model of alcohol abuse. Alcohol 48:243–252
Contreras M, Ceric F, Torrealba F (2007) Inactivation of the interoceptive insula disrupts drug craving and malaise induced by lithium. Science 318:655–658
Damasio A.R., 2000. The feeling of what happens: body and emotion in the making of consciousness. Harcourt; New York.
Eusebio A, Witjas T, Cohen J et al (2013) Subthalamic nucleus stimulation and compulsive use of dopaminergic medication in Parkinson’s disease. J Neurol Neurosurg Psychiatry 84:868–874
Gentil M, Garcia-Ruiz P, Pollak P, Benabid AL (2000) Effect of bilateral deep-brain stimulation on oral control of patients with parkinsonism. Eur Neurol 44(3):147–152
Guercio LA, Schmidt HD, Pierce RC (2014) Deep brain stimulation of the nucleus accumbens shell attenuates cue-induced reinstatement of both cocaine and sucrose seeking in rats. Behav Brain Res 281:125–130
Hopf FW, Chang SJ, Sparta DR, Bowers MS, Bonci A (2010) Motivation for alcohol becomes resistant to quinine adulteration after 3 to 4 months of intermittent alcohol self-administration. Alcohol Clin Exp Res 34(9):1565–1573
Kiefer SW, Dopp JM (1989) Taste reactivity to alcohol in rats. Behav Neurosci 103(6):1318–1326
Koob GF, Ahmed SH, Boutrel B, Chen SA, Kenny PJ, Markou A, O'Dell LE, Parsons LH, Sanna PP (2004) Neurobiological mechanisms in the transition from drug use to drug dependence. Neurosci Biobehav Rev 27:739–749
Lardeux S, Baunez C (2008) Alcohol preference influences the subthalamic nucleus control on motivation for alcohol in rats. Neuropsychopharmacology 33:634–642
Lenoir M, Serre F, Cantin L, Ahmed SH (2007) Intense sweetness surpasses cocaine reward. PLoS One 2(8):e698
Lenoir M, Cantin L, Vanhille N, Serre F, Ahmed SH (2013) Extended heroin access increases heroin choices over a potent nondrug alternative. Neuropsychopharmacology 38:1209–1220
Lévêque M, Carron R, Régis JM (2013) Radiosurgery for the treatment of psychiatric disorders: a review. World Neurosurg 80(3–4):S32.e1–S32.e9
Lhommee E, Klinger H, Thobois S et al (2012) Subthalamic stimulation in Parkinson’s disease: restoring the balance of motivated behaviours. Brain 135:1463–1477
Li N, Wang J, Wang XL, Chang CW, Ge SN, Gao L, Wu HM, Zhao HK, Geng N, Gao GD (2012) Nucleus accumbens surgery for addiction. World Neurosurg 80(3–4):S28.e9–S28.19
Limousin P, Pollak P, Benazzouz A et al (1995) Effect of Parkinsonian signs and symptoms of bilateral subthalamic nucleus stimulation. Lancet 345:91–95
Mallet L, Mesnage V, Houeto JL et al (2002) Compulsions, Parkinson's disease, and stimulation. Lancet 360:1302–1304
Mallet L, Polosan M, Jaafari N et al (2008) Subthalamic nucleus stimulation in severe obsessive–compulsive disorder. N Engl J Med 359:2121–2134
McCracken CB, Grace AA (2007) High-frequency deep brain stimulation of the nucleus accumbens region suppresses neuronal activity and selectively modulates afferent drive in rat orbitofrontal cortex in vivo. J Neurosci 27:12601–12610
Mehta A, Menalled L, Chesselet MF (2005) Behavioral responses to injections of muscimol into the subthalamic nucleus: temporal changes after nigrostriatal lesions. Neuroscience 131(3):769–778
Morrison SE, Bamkole MA, Nicola SM (2015) Sign tracking, but not goal tracking, is resistant to outcome devaluation. Front Neurosci 9:468
Müller UJ, Sturm V, Voges J et al (2009) Successful treatment of chronic resistant alcoholism by deep brain stimulation of nucleus accumbens: first experience with three cases. Pharmacopsychiatry 42:288–291
Naqvi NH, Rudrauf D, Damasio H, Bechara A (2007) Damage to the insula disrupts addiction to cigarette smoking. Science 315:531–534
Paxinos G, Watson C (2005) The rat brain in stereotaxic coordinates, 5th edn. Academic, San Diego
Paxinos G, Watson C (2013) The rat brain in stereotaxic coordinates, 7th edn. Academic Press, Cambridge
Pelloux Y, Baunez C (2013) Deep brain stimulation for addiction: why the subthalamic nucleus should be favoured. Curr Opin Neurobiol 23:713–720
Pelloux Y, Meffre J, Giorla E, Baunez C (2014) The subthalamic nucleus keeps you high on emotion: behavioral consequences of its inactivation. Front Behav Neurosci 5(8):414
Péron J, Frühholz S, Vérin M, Grandjean D (2013) Subthalamic nucleus: a key structure for emotional component synchronization in humans. Neurosci Biobehav Rev 37:358–373
Richter CP (1940) Alcohol as food. Quarterly Journal of Studies on Alcoholism 1:650–661
Roitman MF, Wheeler RA, Wightman RM, Carelli RM (2008) Real-time chemical responses in the nucleus accumbens differentiate rewarding and aversive stimuli. Nat Neurosci 11:1376–1377
Rouaud T, Lardeux S, Panayotis N et al (2010) Reducing the desire for cocaine with subthalamic nucleus deep brain stimulation. Proc Natl Acad Sci 107:1196–1200
Simms JA, Steensland P, Medina B et al (2008) Intermittent access to 20% ethanol induces high ethanol consumption in Long-Evans and Wistar rats. Alcohol Clin Exp Res 32:1816–1823
Sinclair JD, Senter RJ (1968) Development of an alcohol-deprivation effect in rats. Q J Stud Alcohol 29:863–867
Spoelder M, Hesseling P1, Baars AM, Lozeman-van't Klooster JG, Rotte MD, Vanderschuren LJ, Lesscher HM (2015) Individual variation in alcohol intake predicts reinforcement, motivation, and compulsive alcohol use in rats. Alcohol Clin Exp Res 39(12):2427–2437
Tunstall BJ, Carmack SA, Koob GF, Vendruscolo LF (2017) Dysregulation of brain stress systems mediates compulsive alcohol drinking. Current Opinion in Behavioral Sciences 13:85–90
Van der Plasse G, Schrama R, van Seters SP et al (2012) Deep brain stimulation reveals a dissociation of consummatory and motivated behaviour in the medial and lateral nucleus accumbens shell of the rat. PLoS One 7:e33455
Wade CL, Kallupi M, Hernandez DO, Breysse E, de Guglielmo G, Crawford E, Koob GF, Schweitzer P, Baunez C, George O (2017) High-frequency stimulation of the subthalamic nucleus blocks compulsive-like re-escalation of heroin taking in rats. Neuropsychopharmacology. doi:10.1038/npp.2016.270
Wise RA (1973) Voluntary ethanol intake in rats following exposure to ethanol on various schedules. Psychopharmacologia 29:203–210
Witjas T, Baunez C, Henry JM et al (2005) Addiction in Parkinson’s disease: impact of subthalamic nucleus deep brain stimulation. Mov Disord 20:1052–1055
Acknowledgements
This study has been supported by Centre National de la Recherche Scientifique, Aix-Marseille Université, Institut de Recherche et d’Etude sur les Boissons, Agence Nationale de la Recherche (Grant ANR-09-MNPS-028-01), ANR Grant 2010-NEUR-005-01 in the framework of the ERA-Net NEURON), Fondation pour la Recherche Medicale (DPA20140629789). CB and YP declare having no competing financial interests.
The authors would like to thank Brendan Tunstall for his helpful comments on the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pelloux, Y., Baunez, C. Targeting the subthalamic nucleus in a preclinical model of alcohol use disorder. Psychopharmacology 234, 2127–2137 (2017). https://doi.org/10.1007/s00213-017-4618-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-017-4618-5