Abstract
Rationale
A typical antipsychotics (APDs), e.g. olanzapine and risperidone, have been reported to be effective adjunctive treatment for depression if selective serotonin (5-HT) reuptake inhibitors (SSRIs) alone are ineffective.
Objectives and methods
We utilized microdialysis in awake, freely moving rats to study the effect of risperidone in combination with citalopram, an SSRI, on extracellular 5-HT, dopamine (DA), and norepinephrine (NE) efflux in rat medial prefrontal cortex (mPFC).
Results
Risperidone (1.0 mg/kg, s.c.), given alone, significantly increased 5-HT, DA, and NE concentrations in the mPFC. Citalopram (10 mg/kg, s.c.), by itself, produced a significant increase in 5-HT levels only. The combination of risperidone and citalopram produced significantly greater increases in efflux of both DA and NE than risperidone alone. However, the effect of this combination on extracellular 5-HT concentrations was not significantly different than that of citalopram alone. The augmentation of DA and NE efflux induced by risperidone plus citalopram could be partially blocked by the selective 5-HT1A antagonist, WAY 100635 (0.2 mg/kg, s.c.).
Conclusions
The results suggest that the ability of atypical APDs to augment the therapeutic efficacy of SSRIs in major depression and treatment-resistant depression may be due, at least in part, to potentiation of SSRI-induced increases in cortical DA and NE. The contributions of 5-HT1A receptor stimulation and 5-HT2A and alpha2 adrenergic receptor antagonism to this augmentation are discussed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Major depression occurs in up to 10% of the population (Kerr et al. 2000; Amsterdam and Hornig-Rohan 1996). Antidepressant drug treatment is effective, as monotherapy, in around 50–70% of patients (Fava and Davidson 1996; Shelton 1999). Various combinations of different classical antidepressants, e.g., selective serotonin (5-HT) reuptake inhibitors (SSRIs), norepinephrine (NE) reuptake inhibitor, tricyclic antidepressants (TCAs), and monoamine oxidase inhibitors (MAOIs), are sometimes effective in the treatment of depressed patients who fail to respond to a single type of antidepressants (Fava and Davidson 1996; Frazer 1997; Ferrier 1999; Nelson 1999; Fava 2001; Shelton 2003).
Augmenting antidepressant drugs with antipsychotic drugs, especially atypical antipsychotics (APDs), e.g., clozapine, olanzapine, quetiapine, risperidone, ziprasidone, and zotepine, which produce minimal extrapyramidal side effects, has also been found to be effective and tolerable in some patients with treatment-resistant depression (TRD) (Parker and Malhi 2001; Fava 2001; Thase 2002; Shelton 2003; Barbee et al. 2004). For example, some such patients with inadequate response to either fluoxetine, fluvoxamine, or paroxetine, three SSRIs, showed marked improvement following the addition of risperidone (O’Connor and Silver 1998; Ostroff and Nelson 1999; Hirose and Ashby 2002), as did augmentation of TRD patients who failed to respond to tranylcypromine, a MAOI (Stoll and Haura 2000), or milnacipran, an inhibitor of both 5-HT and NE uptake (Tani et al. 2004). The combination of fluoxetine and olanzapine was also found to be more effective than either agent alone in depressed patients who had not responded to fluoxetine alone (Shelton et al. 2001; Corey-Lisle et al. 2003; Tohen et al. 2003; Shi et al. 2004).
Early concepts of the basis for antidepressant drug response suggested that regulating normal function of one or more monoamine neurotransmitters, e.g., 5-HT, NE, or DA, accounted for their effect (Blier et al. 1990; Zemlan and Garver 1990; Leonard 1996; Meltzer 1990). Consistent with this, atypical APDs used as augmentation agents in TRD, e.g., clozapine, olanzapine, and risperidone, increase DA and NE efflux in the prefrontal cortex (Hertel et al. 1996; Zhang et al. 2000; Li et al. 1998). It is possible that these effects also occur in the human prefrontal cortex (PFC), a brain region important for regulating mood, cognition, and social behavior, functions that are compromised in depression (Davidson et al. 2002). The effects of an SSRI alone, an atypical APD alone, or their combination on cortical 5-HT, DA, and NE efflux have been studied. As summarized in Table 1, combinations of an APD (e.g., clozapine, olanzapine, perospirone, quetiapine, or risperidone) with one of the following SSRIs, fluoxetine, fluvoxamine or sertraline, increased DA or NE efflux in rat PFC (Zhang et al. 2000; Koch et al. 2004; Denys et al. 2004; Yoshino et al. 2004).
There are multiple possible bases for the ability of risperidone to augment the efficacy of an SSRI in TRD. Risperidone has a high affinity for dopamine D2, serotonin 5-HT1D, 2A, 2C; α1- and α2-adrenergic; and histamine H1 receptors (Schotte et al. 1996; Richelson and Souder 2000; Table 3). Microdialysis studies have found that risperidone alone increases DA and NE (Zhang et al. 2000), as well as 5-HT, in PFC (Hertel et al. 1996, 1997; Ichikawa et al. 1998). Citalopram, which has the most selective effect on blockade of 5-HT reuptake among all the SSRIs currently available for treatment (Owens et al. 2001; Gobert et al. 1999; Millan et al. 2001), significantly increased extracellular 5-HT, but not DA and NE, levels in rat PFC (Invernizzi et al. 1997; Bymaster et al. 2002; Zhang et al. 2000). We hypothesized that the combination of risperidone and citalopram would produce significantly greater increase in extracellular DA, NE, and 5-HT concentrations in PFC than either drug alone. We also hypothesized that WAY 100635, a 5-HT1A antagonist, which blocks the effects of atypical APDs on DA and NE efflux (Ichikawa and Meltzer 1999; Ichikawa et al. 2001b, 2002), would have a similar effect on the combination of risperidone and citalopram.
Materials and methods
Animals
Male Sprague–Dawley albino rats (Zivic-Miller Laboratories, Porterville, PA, USA) weighting 250–300 g were used throughout the study. Rats were housed two per cage and maintained in a controlled 12-h:12-h light–dark cycle and under constant temperature at 22°C, with free access to food and water.
Surgery and microdialysis
Rats were anesthetized with a combination (i.p.) of chloral hydrate (172 mg/kg) and pentobarbital (35.6 mg/kg) and mounted in a stereotaxic frame (Stoetling, Wood Dale, IL, USA). Stainless guide cannula (21 G) with a dummy probe were placed and fixed by cranioplastic cement (Plastic One, Roanoke, VA, USA) onto the cortex dorsal to the medial PFC (mPFC). Stereotaxic coordinate of probe, when implanted, was A +3.2, L −0.8 (10° inclination), V −5.5 mm, relative to the bregma. The incisor bar level was − 3.0 mm, according to the atlas of Paxinos and Watson (1986). Concentric-shaped dialysis probes were constructed according to the details described elsewhere (Ichikawa and Meltzer 1999; Ichikawa et al. 2001a). The hollow fiber dialysis membrane (polyacrylonitrile/sodium methalysulfonate polymer, 310 μm o.d., 220 μm i.d., molecular weight cut-off 40,000, AN69 HF, Hospal) was used, and the length of exposed nonglued surface for dialyzing was 2.0 mm.
Three to five days following cannulation, the dialysis probes were implanted into the rat mPFC under slight anesthesia with methalysulfonate (Metofane, Pitman-Moore, Mundelein, IL, USA). For systemic administration of drugs or vehicle, a catheter constructed from microbore Tygon tubing (TGY-010, 0.03′ o.d., 0.01′ i.d.; Small Parts Inc., Miami Lakes, FL, USA) was implanted subcutaneously in the intrascapular space of the rats. Rats were then housed individually overnight in dialysis cages with overnight perfusion (0.3 μl/min) of the probe, then the perfusion rate was raised to 1.5 μl/min at the morning of the day the dialysis was carried out. One hour after the perfusion at 1.5 μl/min of the probe, dialysate samples were collected every 30 min for measuring dialysate 5-HT, DA, and NE concentration. The perfusion medium was Dulbecco’s phosphate-buffered saline solution (Sigma, St. Louis, MO, USA) including Ca2+ (138 mM NaCl, 8.1 mM Na2HPO4, 2.7 mM KCl, 1.5 mM KH2PO4, 0.5 mM MgCl, 1.2 mM CaCl2, pH 7.4). Samples collected were analyzed online on a high-performance liquid chromatography (HPLC) system. After stable baseline values in the dialysates were obtained (the monoamine contents on the last three consecutive 30-min samples within a variation of 10%), each drug or vehicle was administered subcutaneously to the rats. The effect of the drug on monoamines release was monitored for another 180 min (30 min for each sample; six samples were collected post drug administration). The location of the dialysis probes were verified at the end of each experiment by manual brain dissection and with 100 μm brain slices (OTS-4000, FHC, Bowdoinham, ME, USA). The procedures applied in these experiments were approved by the Institutional Animal Care and Use Committee of Vanderbilt University in Nashville, TN, USA.
Biochemical assay
Determination of 5-HT
Concentration of 5-HT in dialysate samples were determined by HPLC with electrochemical detection (HPLC-ECD). The 5-HT was separated on a reversed-phase column (XTerra 3.5 μm C18, 1.0×100 mm, Waters Co., Milford, MA, USA). The composition of mobile phase was 50 mM NaH2PO4 (pH 6.0), 20% (v/v) methanol, 8% (v/v) acetonitrile, 450 mg/l sodium dodecyl sulfate, 1 mM Na2EDTA, 10 mM NaCl, and 500 μl/l triethylamine. An electrochemical detection controller (LC-4C, BAS, West Lafayette, PA, USA) with a unijet amperometric detector cell (MF-9080, BAS) set at +320 mV vs an Ag/AgCl reference electrode was used to detect 5-HT. All reagents used for HPLC-ECD analytical or HPLC grade were purchased from Fisher Scientific (Pittsburgh, PA, USA) and Sigma.
Determination of DA and NE
Samples were directly applied onto an HPLC-ECD. DA and NE were simultaneously separated on a reversed-phase column (BDS Hypersil 3 μM C18, 1.0×100 mm, Keystone Scientific, Bellefronte, PA, USA) at 35°C maintained by column heater (LC-22C Temperature Controller, BAS). The mobile phase consisted of 24 mM anhydrous citric acid, 75 mM sodium acetate trihydrate, 0.5 mM sodium salt, 1.8 mM sodium dodecyl sulfate, 4% methanol, and 8% acetonitrile and was pumped at the flow rate of 0.38 ml/min by LC-10AD (Schimadzu, Japan). A unijet working electrode (MF-1003, BAS) was set at 180 mV (LC-4C, BAS) vs an Ag/AgCl reference electrode.
Drugs
Risperidone (Sigma) was dissolved in 0.1 M tartaric acid solution and was adjusted to pH 6–7 with 0.1 N NaOH. Citalopram hydrobromide (Janssen, Titasville, NJ, USA) and WAY 100635 (Sandoz, Basel, Switzerland) were both dissolved in deionized water. Vehicle or drugs were administered subcutaneously through the implanted catheter in a volume of 1.0 ml/kg to randomly assigned rats. The drug doses of risperidone and citalopram used in this study were consistent with that used in the report of Zhang et al. (2000).
Data analysis
Only results derived from healthy rats with correctly positioned dialysis probes were used in the data analysis. Mean predrug baseline levels (time −60, −30, and 0) were designated as 100%. The net area under the curve (AUC) was calculated from the absolute net increase for a 180-min period after subtracting each predrug baseline value by ANOVA. Repeated measure ANOVA followed by Fisher’s protected least significant difference post hoc pairwise comparison procedure and one-way ANOVA were used to determine group differences (StatView 4.5 for the Macintosh). A probability of less than 0.05 (p<0.05) was considered significant in the present study. All results are given as mean±SEM.
Results
Basal extracellular 5-HT, DA, and NE levels in the rat mPFC
There were no significant differences in basal extracellular 5-HT, DA, and NE levels in rat mPFC among the various treatment groups. Basal extracellular 5-HT, DA, and NE levels in all rats used in this study (mean±SEM) were 0.105±0.01 (N=22), 0.109±0.01 (N=29), and 0.157±0.03 (N=27) nM (pmol/ml), respectively. Vehicle administration did not affect basal levels of these monoamines in this region.
Effect of citalopram and risperidone, alone and in combination, on extracellular 5-HT, DA, and NE levels in rat mPFC
As shown in Fig. 1, citalopram alone (10 mg/kg, s.c.) significantly increased extracellular 5-HT levels (F(1,8)=26.00, p<0.001, net AUC=136±46), but had no effects on DA and NE concentrations. The net AUC data for all studies are summarized in Fig. 2. Risperidone (1.0 mg/kg, s.c.), given alone, produced a modest but significant increase in extracellular 5-HT levels (F(1,9)=9.35, p=0.003, net AUC =30±11). However, it produced markedly greater increases in both DA (F(1,8)=22.33, p<0.001, net AUC=77±18) and NE (F(1,8)=46.39, p<0.001, net AUC=166±28) concentrations. The combination of citalopram and risperidone significantly elevated DA (net AUC 241±15) and NE (net AUC 340±36) levels compared with risperidone alone (DA: F(1,8)=21.89, p<0.001; NE: F(1,9)=11.84, p<0.001). These effects were significantly greater than risperidone alone (net AUCs, DA=77±18, NE=166±28). The combination of risperidone and citalopram on 5-HT efflux in rat mPFC (net AUC=122±36) was not significantly different from that of citalopram alone (F(1,8)=1.027, P=0.3134).
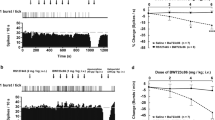
Time course of the effects of administration of vehicle and citalopram (10 mg/kg, s.c.), risperidone (1.0 mg/kg, s.c.) alone or in combination, and WAY 100635 (0.2 m/kg, s.c.) plus citalopram and risperidone on extracellular concentrations of a norepinephrine (NE), b dopamine (DA), and c serotonin (5-HT) in rats prefrontal cortex. Values are shown as mean±SEM of the percentage of predrug baseline of 5–7 rats. Citalopram alone significantly increased the 5-HT level [F(1,8)=26.00, p<0.001] and had no effects on DA and NE levels. Risperidone produced a modest, but significant, increase in 5-HT [F(1,9)=9.351, p=0.003]. Meanwhile, risperidone could significantly increase both DA [F(1,8)=22.33, p<0.001] and NE [F(1,8)=46.39, p<0.001]. Coadministration of citalopram and risperidone also could increase 5-HT in rat mPFC, but was not significantly different with citalopram and risperidone alone, respectively. The combination of citalopram and risperidone significantly elevated DA and NE concentrations, compared with risperidone alone [For DA: F(1,8)=21.89, p<0.001; for NE: F(1,9)=11.84, p<0.001]. WAY 100635 (0.2 mg/kg, s.c.) partly inhibited DA and NE increase induced by citalopram plus risperidone [DA: F(1,10)=20.00, p<0.001; NE: F(1.9)=13.00, p<0.001] compared with coadministration of citalopram and risperidone
Changes in extracellular concentrations of serotonin (5-HT), dopamine (DA), and norepinephrine (NE) in prefrontal cortex of rats after administration of vehicle and citalopram, risperidone alone or in combination. Values are the average of AUC (mean±SEM) of each group post drugs injection in 180 min. **p<0.01, ***p<0.001, compared with vehicle group; ##p<0.01, ###p<0.001, compared with risperidone alone; &&&p<0.001, compared with citalopram risperidone group
Effect of WAY 100635 on the augmentation of citalopram and risperidone on mPFC DA and NE efflux
The selective 5-HT1A antagonist WAY 100635, at a dose of 0.2 mg/kg (s.c.) given 5 min before citalopram administration, partly but significantly inhibited the DA (net AUC=88±13) and NE (net AUC=173±18) increase induced by citalopram plus risperidone (net AUCs: DA=241±15, NE=340±36) (DA: F(1,10)=20.00, p<0.001; NE: F(1, 9)=13.00, p<0.001), compared with coadministration of citalopram and risperidone.
Discussion
The present study supported our hypotheses that citalopram would potentiate the risperidone-induced increases in both mPFC DA and NE levels. It did not potentiate the efflux of 5-HT. WAY 100635, a selective 5-HT1A antagonist, partially inhibited the augmentation of mPFC DA and NE efflux induced by the combination of risperidone and citalopram.
Since there is considerable evidence that decreased cortical noradrenergic, serotonergic, and dopaminergic functions are involved in the etiology of depression (see Elhwuegi 2004for review), the enhanced effect of risperidone and citalopram on DA and NE efflux, together with a modest but nonpotentiated increase in 5-HT efflux in rat PFC, may explain, in part, the augmented therapeutic efficacy of this combination in TRD treatment. Consistent with previous reports, risperidone (1.0 mg/kg, s.c.) alone increased extracellular 5-HT, DA, and NE concentrations (150, 200, and 300% of base levels, respectively) in rat mPFC (Ichikawa et al. 1998, 2001b, 2002; Zhang et al. 2000). Furthermore, citalopram (10 mg/kg), given alone, increased 5-HT (250% of base level), but not DA and NE concentrations in mPFC, consistent with previous reports (Invernizzi et al. 1997; Bymaster et al. 2002). In the present study, citalopram potentiated risperidone-induced increases in cortical DA and NE (400 and 500% of base levels), but not 5-HT (250%) concentrations. By contrast, risperidone has previously been reported to augment fluoxetine-induced increase in cortical DA, but not NE or 5-HT (Zhang et al. 2000). These results suggest that risperidone plus citalopram are more effective in increasing efflux of cortical monoamines than risperidone plus fluoxetine. Since serotoninergic activity was not enhanced to a greater extent than that produced by citalopram alone, it seems reasonable to conclude that the greater increases in DA and NE efflux may be more important for the greater efficacy of the combination in TRD than 5-HT efflux, which may still contribute. Of course, the effects of the combined treatments on other potential mechanisms of antidepressant action such as signal transduction mechanisms and neurogenesis (Duman, 2004) need to be further studied.
Citalopram, like fluoxetine, increased extracellular 5-HT concentrations (Table 1). Endogenous 5-HT has also been shown to increase DA efflux in mPFC (Matsumoto et al. 1999; Iyer and Bradberry 1996). However, citalopram, unlike fluoxetine (Tanda et al. 1994; Jordan et al. 1994), did not increase extracellular DA and NE levels in rat prefrontal cortex, as previously reported by Bymaster et al. (2002) and Koch et al. (2002). This suggests that the increased DA and NE efflux induced by fluoxetine alone is unlikely to be secondary to its effect on 5-HT efflux since citalopram, the most selective SSRI (Sanchez and Hytell 1999), produces greater increase in 5-HT efflux than fluoxetine (Bymaster et al. 2002; Felton et al. 2003), but citalopram had no effect on extracellular DA and NE concentrations. Moreover, local infusion of citalopram into the mPFC markedly increased extracellular 5-HT at 0.1–10 μM, while having little or no effect on DA efflux, clearly showing that extracellular 5-HT concentrations can be substantially increased by SSRIs in the frontal cortex without any concomitant changes in extracellular DA (Pozzi et al. 1999). Evidence has been obtained that inhibition of NE uptake in the frontal cortex enhances the extracellular concentrations of DA as well as NE (Carboni et al. 1990; Pozzi et al. 1994), providing the possible mechanism of the effect of fluoxetine to enhance DA efflux (Pozzi et al. 1999; also see Table 2). Koch et al. (2002) argued that the increase in extracellular DA by R-fluoxetine maybe also be due to its antagonism of 5-HT2C receptors.
Among the atypical APDs, aripiprazole, clozapine, quetiapine, and ziprasidone are 5-HT1A partial agonists, but risperidone and olanzapine are not. Nevertheless, all of these APDs, as well as the former group, produce comparable increases in DA release in the mPFC of rats by a mechanism which can be blocked by pretreatment with the 5-HT1A antagonist WAY 100635, suggesting that direct or indirect 5-HT1A agonism is an important component of the action of all APDs, which are 5-HT2A/D2 antagonists (Ichikawa et al. 2001b, 2002; Meltzer et al. 2003). Stimulation of 5-HT1A receptors by citalopram-induced efflux of 5-HT may partly explain the greater effect of the combination of citalopram and risperidone on DA efflux in PFC. This hypothesis is consistent with our previous studies which demonstrated that combined administration of the 5-HT1A agonist R()-8-OH-DPAT with either a selective 5-HT2A antagonist, MDL 100907, or D2 antagonist S(-)-sulpiride, could augment DA efflux in rat PFC (Ichikawa and Meltzer 1999; Ichikawa et al. 2001b). A similar mechanism may contribute to enhanced NE efflux since systemic administration of 5-HT1A receptor agonists increase NE efflux in the rat PFC through activation of postsynaptic 5-HT1A heteroreceptors (Hajos-Korcsok et al. 1999; Ago et al. 2002; Owen and Whitton 2003). The results of the present study also showed that the 5-HT1A antagonist WAY 100635 could partly inhibit the augmentation of combined administration of risperidone and citalopram on both DA and NE efflux in mPFC, providing additional evidence to support this hypothesis. It has been suggested that the combination of 5-HT2A antagonism and 5-HT1A agonism may potentiate antidepressant action (Hatanaka et al. 1996). However, the fact that the effect of WAY 100635 on DA release was only partial suggests that other mechanisms may be involved.
There is extensive evidence that 5-HT1A receptor-mediated responses are potentiated by coadministration of a 5-HT2A receptor antagonist (Ashby et al. 1994; Ichikawa et al. 2001a; Meltzer and Maes 1995; Willins and Meltzer 1997). The atypical antipsychotic drugs related to risperidone are either direct or indirect 5-HT1A agonists and 5-HT2A antagonists (Ichikawa et al. 2002). The combination of 5-HT reuptake blockade and 5-HT2A antagonism, either in a single antidepressant such as YM992, or from the combined administration of the selective 5-HT2A antagonist MDL 100907, which has no effect on NE and 5-HT levels when given alone, and citalopram, significantly increased mPFC NE efflux, despite no further increase in 5-HT efflux, compared with citalopram treatment alone (Hatanaka et al. 2000a,b). Moreover, long-term administration of YM992 leads to an increased firing activity of NE neurons, resulting from 5-HT reuptake inhibition plus 5-HT2A antagonism, which might confer additional benefits in affective and anxiety disorders (Szabo and Blier 2002). Thus, 5-HT1A agonism and 5-HT2A antagonism may both be factors in the augmentation of SSRIs by APDs for the treatment of depression. However, MDL 100907 did not enhance fluoxetine’s effects on DA or NE efflux in PFC (Zhang et al. 2000), whereas it did increase the effect of citalopram (Hatanaka et al. 2000a,b). These results may partly explain why citalopram plus risperidone augmented both DA and NE but not 5-HT efflux in the present study, compared with fluoxetine plus risperidone, which have been reported not to have a synergistic effect on extracellular NE levels (Zhang et al. 2000). These results suggest that all SSRIs may not be equally effective as combination therapy for TRD and that citalopram may have particular advantages.
Adrenergic α2 blockade may also contribute to the ability of the combination of risperidone and citalopram to increase DA and NE efflux in mPFC. Adrenergic α2 autoreceptors located on both the dendrites and terminals of frontocortical adrenergic pathways exert a pronounced tonic, inhibitory influence upon the efflux of DA and NE in the PFC (Gobert et al. 1998). It has been reported that buspirone, via activation of 5-HT1A and blockade of α2 receptors, facilitated fluoxetine-stimulated dialysate levels of DA and NE, but not 5-HT, in the frontal cortex (Gobert et al. 1999). Furthermore, idazoxan, an α2-adrenoceptor antagonist, potentiated the ability of raclopride, a D2 receptor antagonist, to increase DA efflux in the mPFC (Hertel et al. 1999). H1 receptor blockade may also be involved in the augmentation of DA and NE efflux by the combination of risperidone and citalopram. NE concentration in perfusates of the paraventricular nucleus (PVN) have been reported to be significantly increased by the addition of the histamine H1-receptor antagonist triprolidine to the perfusate, which suggests that histamine has an inhibitory effect on NE release from hypothalamic nerve terminals in the PVN (Kurose and Terashima 1999). Citalopram and risperidone also have high affinities for histamine H1 receptors (Tables 2, 3).
As summarized in Table 1, monoamine efflux in PFC is augmented by different combinations of APDs and SSRIs. The results reported here provide new evidence for the basis for the efficacy of combined treatment with APDs and SSRIs in TRD treatment, namely, their synergistic effect on both DA and NE release in rat PFC. Since risperidone plus fluoxetine augmented only cortical DA levels (Zhang et al. 2000), the possibility that risperidone combined with citalopram might be more effective than risperidone and fluoxetine in TRD patients should be studied. The ability of the combination of SSRI and APDs to potent DA and NE efflux also suggests it would be of interest to test the ability of the combination to improve cognitive deficits and negative symptoms in schizophrenia, which have been suggested to result, in part, from diminished dopaminergic and catecholaminergic activity in the cortex and hippocampus (Meltzer and McGurk 1999).
In conclusion, the ability of atypical antipsychotics to augment the therapeutic efficacy of SSRIs in major depression and treatment-resistant depression may be due, in part, to potentiation of SSRI-induced effluxes in cortical DA and NE. In our opinion, further preclinical and clinical studies of combinations of other antipsychotic drugs, including typical antipsychotic drugs, with various types of antidepressant drugs are indicated.
References
Ago Y, Sakaue M, Baba A, Matsuda T (2002) Selective reduction by isolation rearing of 5-HT1A receptor-mediated dopamine release in vivo in the frontal cortex of mice. J Neurochem 83:353–359
Amsterdam JD, Hornig-Rohan M (1996) Treatment algorithms in treatment-resistant depression. Psychiatr Clin North Am 19:371–386
Ashby CR Jr, Edwards E, Wang RY (1994) Electrophysical evidence for a functional interaction between central 5-HT2 and 5-HT1A receptors in the rat medial prefrontal cortex: a iontophoretic study. Synapse 17:173–181
Barbee JG, Conrad EJ, Jamhour NJ (2004) The effectiveness of olanzapine, risperidone, quetiapine, and ziprasidone as augmentation agents in treatment-resistant major depressive disorder. J Clin Psychiatry 65:975–981
Blier P, De Montigny C, Chaput Y (1990) A role for the serotonin system in the mechanism of action of antidepressant treatments: preclinical evidence. J Clin Psychiatry 51(Suppl):14–21
Bymaster FP, Zhang W, Carter PA, Shaw J, Chernet E, Phebus L, Wong DT, Perry KW (2002) Fluoxetine, but not other selective serotonin uptake inhibitors, increases norepinephrine and dopamine extracellular levels in prefrontal cortex. Psychopharmacology (Berl) 160:353–361
Carboni E, Tanda GL, Frau R, Di Chiara G (1990) Blockade of the noradrenaline carrier increases extracellular dopamine concentrations in the prefrontal cortex: evidence that dopamine is taken up in vivo by noradrenergic terminals. J Neurochem 55:1067–1070
Corey-Lisle PK, Birnbaum H, Greenberg P, Marynchenko M, Dube S (2003) Economic impact of olanzapine plus fluoxetine combination therapy among patients treated for depression: a pilot study. Psychopharmacol Bull 37:90–98
Davidson RJ, Pizzagalli D, Nitschke JB, Putnam K (2002) Depression: perspectives from affective neuroscience. Annu Rev Psychol 53:545–574
Denys D, Klompmakers AA, Westenberg HG (2004) Synergistic dopamine increase in the rat prefrontal cortex with the combination of quetiapine and fluvoxamine. Psychopharmacology (Berl) 176:195–203
Duman RS (2004) Depression: a case of neuronal life and death? Biol Psychiatry 56:140–145
Elhwuegi AS (2004) Central monoamines and their role in major depression. Prog Neuropsychopharmacol Biol Psychiatry 28:435–451
Fava M (2001) Augmentation and combination strategies in treatment-resistant depression. J Clin Psychiatry 62(Suppl 18):4–11
Fava M, Davidson KG (1996) Definition and epidemiology of treatment-resistant depression. Psychiatr Clin North Am 19:179–200
Felton TM, Kang TB, Hjorth S, Auerbach SB (2003) Effects of selective serotonin and serotonin/noradrenaline reuptake inhibitors on extracellular serotonin in rat diencephalons and frontal cortex. Naunyn Schmiedebergs Arch Pharmacol 367:297–305
Ferrier IN (1999) Treatment of major depression: is improvement enough? J Clin Psychiatry 60(Suppl 6):10–14
Frazer A (1997) Antidepressants. J Clin Psychiatry 58(Suppl 6):9–25
Gobert A, Rivet JM, Audinot V, Newman-Tancredi A, Cistarelli L, Millan MJ (1998) Simultaneous quantification of serotonin, dopamine and noradrenaline levels in single frontal cortex dialysates of free-moving rats reveals a complex pattern of reciprocal auto- and heteroreceptor mediated control release. Neuroscience 84:413–429
Gobert A, Rivet JM, Cistarelli L, Melon C, Millan MJ (1999) Buspirone modulates basal and fluoxetine-stimulated dialysate levels of dopamine, noradrenaline and serotonin in the prefrontal cortex of freely moving rats: activation of serotonin1A receptors and blockade of α2-adrenergic receptors underlie its actions. Neuroscience 93:1251–1262
Hajos-Korcsok E, Mcquade R, Sharp T (1999) Influence of 5-HT1A receptors on central noradrenergic system activity: microdialysis studies using MDL 73005EF and its enantiomers. Neuropharmacology 38:299–306
Hatanaka K, Nomura T, Hidaka K, Takeuchi H, Yatsugi S, Fujii M, Yamaguchi T (1996) Biochemical profile of YM992, a novel selective serotonin reuptake inhibitor with 5-HT2A receptor antagonistic activity Neuropharmacology 35:1621–1626
Hatanaka K, Yatsugi S, Yamaguchi T (2000a) Effect of acute treatment with YM992 on extracellular serotonin levels in the rat frontal cortex. Eur J Pharmacol 395:23–29
Hatanaka K, Yatsugi S, Yamaguchi T (2000b) Effect of acute treatment with YM992 on extracellular norepinephrine levels in the rat frontal cortex. Eur J Pharmacol 395:31–36
Hertel P, Fagerquist MV, Svensson TH (1999) Enhanced cortical dopamine output and antipsychotic-like effects of raclopride by α2 adrenoceptor blockade. Science 286:105–107
Hertel P, Nomikos GG, Iurlo M, Svensson TH (1996) Risperidone: regional effects in vivo on release and metabolism of dopamine and serotonin in the rat brain. Psychopharmacology (Berl) 124:74–86
Hertel P, Nomikos GG, Schilstrom B, Arborelius L, Svensson TH (1997) Risperidone dose-dependently increases extracellular concentrations of serotonin in the rat frontal cortex: role of α2-adrenoceptor antagonism. Neuropsychopharmacology 17:44–55
Hirose S, Ashby CR Jr (2002) An open pilot study combining risperidone and a selective serotonin reuptake inhibitor as initial antidepressant therapy. J Clin Psychiatry 63:733–736
Ichikawa J, Meltzer HY (1999) R()-8-OH-DPAT, a serotonin 1A receptor agonist, potentiated S(-)-sulpiride-induced dopamine release in rat medial prefrontal cortex and nucleus accumbens but not striatum. J Pharmacol Exp Ther 291:1227–1232
Ichikawa J, Kuroki T, Dai J, Meltzer HY (1998) Effects of antipsychotic drugs on extracellular serotonin levels in rat medial prefrontal cortex and nucleus accumbens. Eur J Pharmacol 351:163–171
Ichikawa J, Dai J, Meltzer HY (2001a) DOI, a 5-HT2A/2C receptor agonist, attenuates clozapine-induced cortical dopamine release. Brain Res 907:151–155
Ichikawa J, Ishii H, Bonaccorso S, Fowler WL, O’Laughlin IA, Meltzer HY (2001b) 5-HT2A and D2 receptor blockade increased cortical DA release via 5-HT1A receptor activation: a possible mechanism of atypical antipsychotic-induced cortical dopamine release. J Neurochem 76:1521–1531
Ichikawa J, Li Z, Dai J, Metlzer HY (2002) Atypical antipsychotic drugs, quetiapine, iloperidone, and melperone, preferentially increase dopamine and acetylcholine release in rat medial prefrontal cortex: role of 5-HT1A receptor agonism. Brain Res 956:349–357
Invernizzi R, Velasco C, Bramante M, Longo A, Samanin R (1997) Effect of 5-HT1A receptor antagonist on citalopram-induced increase in extracellular serotonin in the frontal cortex, striatum and dorsal hippocampus. Neuropharmacology 36:467–473
Iyer RN, Bradberry CW (1996) Serotonin-mediated increase in prefrontal cortex dopamine release: pharmacological characterization. J Pharmacol Exp Ther 277:40–47
Jordan S, Kramer GL, Zukas PK, Moeller M, Petty F (1994) In vivo biogenic amine efflux in medial prefrontal cortex with imipramine, fluoxetine, and fluvoxamine. Synapse 18:294–297
Kerr EA, McGlynn EA, Van Vorst KA, Wickstrom SL (2000) Measuring antidepressant prescribing practice in a health care system using administrative data: implications for quality measurement and improvement. Jt Comm J Qual Improv 26:203–216
Koch S, Perry KW, Nelson DL, Conway RG, Threlkeld PG, Bymaster FP (2002) R-fluoxetine increases extracellular DA, NE, as well as 5-HT in rat prefrontal cortex and hypothalamus: an in vivo microdialysis and receptor binding study. Neuropsychopharmacology 27:949–959
Koch S, Perry KW, Bymaster FP (2004) Brain region and dose effects of an olanzapine/fluoxetine combination on extracellular monoamine concentrations in the rat. Neuropharmacology 46:232–242
Kurose Y, Terashima Y (1999) Histamine regulates food intake through modulating noradrenaline release in the para-ventricular nucleus. Brain Res 828:115–118
Leonard BE (1996) New approaches to the treatment of depression. J Clin Psychiatry 57(Suppl 4):26–33
Li XM, Perry KW, Wong DT, Bymaster FP (1998) Olanzapine increased in vivo dopamine and norepinephrine release in rat prefrontal cortex, nucleus accumbens and striatum. Psychopharmacology (Berl) 136:153–161
Matsumoto M, Togashi H, Mori K, Ueno K, Miyamoto A, Yoshioka M (1999) Characterization of endogenous serotonin-mediated regulation of dopamine release in the rat prefrontal cortex. Eur J Pharmacol 383:39–48
Meltzer HY (1990) Role of serotonin in depression. Ann N Y Acad Sci 600:486–500
Meltzer HY, Maes M (1995) Effect of pindolol pretreatment on MK-212-induced plasma cortical and prolactin responses in normal men. Biol Psychiatry 38:310–318
Meltzer HY, McGurk SR (1999) The effects of clozapine, risperidone, and olanzapine on cognitive function in schizophrenia. Schizophr Bull 25:233–255
Meltzer HY, Li Z, Kaneda Y, Ichiwaka J (2003) Serotonin receptors: their key role in drugs to treat schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry 27:1159–1172
Millan MJ, Gorbert A, Lejeune F, Newman-Tancredi A, Rivet JM, Auclair A, Peglion JL (2001) S33005, a novel ligand at both serotonin and norepinephrine transporters: I. receptor binding, electrophysiological, and neurochemical profile in comparison with venlafaxine, reboxetine, citalopram, and clomipramine. J Pharmacol Exp Ther 298:565–580
Nelson JC (1999) A review of efficacy of serotonergic and noradrenergic reuptake inhibitors for treatment of major depression. Biol Psychiatry 46:1301–1308
O’Connor M, Silver H (1998) Adding risperidone to selective serotonin reuptake inhibitor improves chronic depression. J Clin Psychopharmacol 18:89–91
Ostroff RB, Nelson JC (1999) Risperidone augmentation of selective serotonin reuptake inhibitors in major depression. J Clin Psychiatry 60:256–259
Owen JC, Whitton PS (2003) Reboxetine modulates norepinephrine efflux in the frontal cortex of the freely moving rat: the involvement of alpha 2 and 5-HT1A receptors. Neurosci Lett 348:171–174
Owens MJ, Knight DL, Nemeroff CB (2001) Second-generation SSRIs: human monoamine transporter binding profile of escitalopram and R-fluoxetine. Biol Psychiatry 50:345–350
Parker G, Malhi G (2001) Are atypical antipsychotic drugs also atypical antidepressants. Aust N Z J Psychiatry 35:631–638
Paxinos G, Watson C (1986) The rat brain in stereotaxic coordinates. Academic, New York
Pozzi L, Invernizzi R, Cervo L, Vallebuona F, Samanin R (1994) Evidence that extracellular concentrations of dopamine are regulated by noradrenergic neurons in the frontal cortex of rats. J Neurochem 63:195–200
Pozzi L, Invernizzi R, Garavaglia C, Samanin R (1999) Floxetine increases extracellular dopamine in the prefrontal cortex by a mechanism not dependent on serotonin: a comparison with citalopram. J Neurochem 73:1051–1057
Richelson E, Souder T (2000) Binding of antipsychotic drugs to human brain receptors focus on newer generation compounds. Life Sci 68:29–39
Sanchez C, Hyttel J (1999) Comparison of the effects of antidepressants and their metabolites on reuptake of biogenic amines and on receptor binding. Cell Mol Neurobiol 19:467–489
Schotte A, Janssen PF, Gommeren W, Luyten WH, Van Gompel P, Lesage AS, De Loore K, Leysen JE (1996) Risperidone compared with new and reference antipsychotic drugs: in vitro and in vivo receptor binding. Psychopharmacology (Berl) 124:57–73
Shelton RC (1999) Treatment options for refractory depression. J Clin Psychiatry 60(Suppl 4): 57–61
Shelton RC (2003) The use of antidepressants in novel combination therapies. J Clin Psychiatry 64(Suppl 2):14–18
Shelton RC, Tollefson GD, Tohen M, Stahl S, Gannon KS, Jacobs TG, Buras WR, Bymaster FP, Zhang W, Spencer KA, Feldman PD, Meltzer HY (2001) A novel augmentation strategy for treating resistant major depression. Am J Psychiatry 158:131–134
Shi L, Namjoshi MA, Swindle R, Yu X, Risser R, Baker RW, Tohen M (2004) Effects of olanzapine alone and olanzapine/fluoxetine combination on health-related quality of life in patients with bipolar depression: secondary analyses of a double-blind, placebo-controlled, randomized clinical trial. Clin Ther 26:125–134
Stoll Al, Haura G (2000) Tranylcypromine plus risperidone for treatment-refractory major depression [letter]. J Clin Psychopharmacol 20:495–496
Szabo ST, Blier P (2002) Effects of serotonin (5-hydroxytryptamine, 5-HT) reuptake inhibition plus 5HT (2A) receptor antagonism on the firing activity of norepinephrine neurons. J Pharmacol Exp Ther 302:983+IBM-991
Tanda G, Carboni E, Fran R, Di Chiara G (1994) Increase of extracellular dopamine in the prefrontal cortex: a trait of drugs with antidepressant potential? Psychopharmacology (Berl) 115:285–288
Tani K, Takei N, Kawai M, Suzuki K, Sekine Y, Toyoda T, Minabe Y, Mori N (2004) Augmentation of milnacipran by risperidone in treatment for major depression. Int J Neuropsychopharmacol 7:55–58
Thase ME (2002) What role do atypical antipsychotic drugs have in treatment-resistant depression. J Clin Psychiatry 63:95–103
Tohen M, Vieta E, CalabreseJ, Ketter TA, Sachs G, Bowden C, Mitchell PB, Centorrino F, Risser R, Baker RW, Evans AR, Beymer K, Dube S, Tollefson GD, Breier A (2003) Efficacy of olanzapine and olanzapine-fluoxetine combination in the treatment of bipolar depression. Arch Gen Psychiatry 60:1079–1088
Willins DL, Meltzer HY (1997) Direct injection of 5-HT2A receptor agonists into medial prefrontal cortex produced a head-twitch response in rats. J Pharmacol Exp Ther 282:699–706
Yoshino T, Nisijima K, Shioda K, Yui K, Katoh S (2004) Perospirone, a novel atypical atypical antipsychotic drug, potentiates flouxetine-induced increases in dopamine levels via multireceptor actions in the rat medial prefrontal cortex. Neurosci Lett 364:16–21
Zhang W, Perry KW, Wong DT, Potts BD, Bao JQ, Tollefson GD, Bymaster FP (2000) Synergistic effects of olanzapine and other antipsychotic agents in combination with fluoxetine on norepinephrine and dopamine release in rat prefrontal cortex. Neuropsychopharmacology 23:250–262
Zemlan FP, Garver DL (1990) Depression and antidepressant therapy: receptor dynamics. Prog Neuropsychopharmacol Biol Psychiatry 14:503–523
Acknowledgements
Supported, in part, by grants from Janssen Pharmaceuticals and the Ritter and William K. Warren Foundations.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Huang, M., Ichiwaka, J., Li, Z. et al. Augmentation by citalopram of risperidone-induced monoamine release in rat prefrontal cortex. Psychopharmacology 185, 274–281 (2006). https://doi.org/10.1007/s00213-005-0206-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-005-0206-1