Abstract
Rationale
The selective serotonin reuptake inhibitors (SSRIs) and the serotonin and noradrenaline reuptake inhibitors (SNRIs) increase synaptic levels of serotonin, leading to an increased activation of a multitude of specific postsynaptic 5-HT receptors. However, it is not yet known which 5-HT receptor subtypes mediate the therapeutic effects of antidepressants.
Methods
The effects of the SSRI, paroxetine and the SNRI, venlafaxine were evaluated in the mouse four plates test (FPT).
Results
Paroxetine administered intraperitoneally (IP) (0.5, 2–8 mg/kg) potently augmented the number of punished passages accepted by mice in this paradigm. The effects of paroxetine (8 mg/kg) were not reversed by the selective 5-HT2C receptor antagonist, RS 10-2221 (0.1 mg/kg and 1 mg/kg) or the selective 5-HT2B/2C receptor antagonist SB 206553 (0.1 mg/kg and 1 mg/kg), at doses which lack an effect when administered alone. In contrast, the selective 5-HT2A receptor antagonist, SR 46349B (0.1 mg/kg and 1 mg/kg) completely abolished the paroxetine-induced increase in punished passages. The acute administration of venlafaxine induced an anxiolytic-like effect in the FPT at the doses of 2–16 mg/kg. This effect was reversed by the 5-HT2B/2C receptor antagonist as did SR 46349B, for both doses administered. Our results strongly suggest that activation of 5-HT2A receptors is critically involved in the anxiolytic activity of paroxetine, whereas the 5-HT2A and 5-HT2B receptors are involved in the anti-punishment action of venlafaxine in the FPT. The co-administration of selective 5-HT2A, 2B, 2C receptor agonists (DOI, 0.06 mg/kg and 0.25 mg/kg; BW 723C86, 0.5 mg/kg and 2 mg/kg and RO 60-0175, 0.06 mg/kg and 0.25 mg/kg), respectively, was subsequently investigated. The effects of sub-active doses of paroxetine (0.25 mg/kg and 1 mg/kg) were augmented by BW 723C86 and RO 60-0175 receptor agonist challenge. The anti-punishment effects of venlafaxine (0.25 mg/kg and 1 mg/kg) were potentialised only by DOI co-administration.
Conclusion
These results indicate that the co-administration of 5-HT2 receptor agonists with paroxetine and venlafaxine may provide a powerful tool for enhancing the clinical efficacy of these antidepressants.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Even though it is now well established that selective antidepressants (ADs) possess anxiolytic properties, their underlying neuropharmacological mechanism of action is still not understood (Zohar and Westenberg 2000; Bourin and Lambert 2002; Bourin et al. 2002; Nemeroff 2003; Vaswani et al. 2003). Owing to their 5-HT re-uptake inhibiting effects, SSRIs and SNRIs increase synaptic levels of 5-HT (Fuller 1994; Kreiss and Lucki 1995; Beyer et al. 2002; Lambert and Bourin 2002; Ables and Baughman 2003; Felton et al. 2003), leading to an increased activation of a multitude of specific postsynaptic serotonin (5-HT) receptors (e.g. 5-HT1A, 5-HT1D, 5-HT2A, 5-HT2C and 5-HT3 receptors). However, it is not yet known which 5-HT receptor subtypes mediate the therapeutic effects of antidepressants and whether different 5-HT receptor subtypes are involved in their anxiolytic actions.
The following study was carried out to explore the anxiolytic-like profile of two different classes of antidepressants; paroxetine, a selective serotonin reuptake inhibitor (SSRI), and venlafaxine, a serotonin and noradrenaline reuptake inhibitor (SNRI), in the mouse model of anxiety; the four plates test (FPT). This model is based on the suppression by punishment of a simple innate ongoing behaviour, i.e. the exploration of novel surroundings, of the mouse. Both compounds are licensed in most areas for the treatment of GAD and have become established as first-line therapies as shown by randomised, double-blind studies (Davidson et al. 1999; Gelenberg et al. 2000; Rickels et al. 2000) and a large placebo-controlled, flexible-dosage trial (Pollack et al. 2001).
Paroxetine, a phenylpiperidine derivative, is a chiral SSRI but is marketed as its active (S)-enantiomer. It is the most potent inhibitor of the reuptake of 5-HT, a very weak inhibitor of noradrenaline uptake but is still more potent at this site than the other SSRIs (Rasmussen and Brosen 2000; Bourin et al. 2001). Venlafaxine is a dual 5-HT and noradrenaline (NA) reuptake inhibitor which has been claimed to have a faster onset of antidepressant action and superior clinical efficacy than for other comparable drugs as shown by randomised, double-blind studies (Nierenberg 2001; Stahl et al. 2002) and a randomised clinical trial with placebo controls (Ninan 2000). The pharmacology of venlafaxine is dose dependent: namely, at low doses it is essentially an SSRI; at medium to high doses, additional NA reuptake inhibition occurs; and at very high doses, some DA reuptake inhibition also occurs (Stahl 1998). Venlafaxine is a bicyclic phenylthylamine and has no significant affinity for 5-HT1, 5-HT2, histamine H1, muscarinic receptors, α1, α2 and β adrenoceptors, dopamine or opiate receptors in the rat brain (Muth et al. 1986; Cusack et al. 1994; Millan et al. 2001a; Briley 2003).
Conflicting results have been reported for the anxiolytic-like effects of acute paroxetine and venlafaxine administration in animal models of anxiety (Hascoët et al. 2000a; Borsini et al. 2002; Prut and Belzung 2003; Sanchez 2003). However, few detailed comparative evaluations of the role of 5-HT receptors in the anxiolytic effects of these compounds using a broad range of selective 5-HT receptor ligands have been described.
Thus after exploring the potential anxiolytic-like profile of these two drugs in the anxiety model, we evaluated the contribution of particular 5-HT2 receptor subtypes in these anxiolytic actions. 5-HT2 receptor antagonists employed included the 5-HT2A receptor antagonist, SR 46349B, the 5-HT2B/2C receptor antagonist, SB 206553 and the 5-HT2C receptor antagonist RS 10-2221 (Nic Dhonnchadha et al. 2003).
Enhancement of the synaptic availability of 5-HT appears to be a critical component of the mechanism underlying the actions of ADs. The antidepressant effect of SSRIs can be enhanced by co-administration of non-specific 5-HT2 receptor antagonists including mianserin, olanzapine and trazodone using clinical double-blind studies (Rosen et al. 1999; Ferreri et al. 2001). Recently the addition of drugs with prominent but non-specific 5-HT2 receptor antagonist properties (risperidone, olanzapine, mirtazapine and mianserin) to SSRIs has been shown to enhance therapeutic responses in patients with treatment-refractory obsessive compulsive disorder (McDougle et al. 2000). It has been suggested that the simultaneous blockade of 5-HT2A receptors and an activation of an unknown constellation of other 5-HT receptors indirectly as a result of 5-HT uptake inhibition might have greater therapeutic efficacy than either action alone. Few animal studies have been carried out for the potential synergistic action of 5-HT2 ligands and ADs in anxiety models. Co-administration of the 5-HT2C receptor antagonist (irindalone) and paroxetine in the light/dark paradigm (Mork and Hogg 2002) was shown to augment the anxiolytic-like effects of acute paroxetine administration. It was equally suggested that the co-administration of mirtazapine (an α2, 5-HT2, 5-HT3 and H1 receptor antagonist) and paroxetine induces an earlier increase in 5-HT transmission (Besson et al. 2000).
In this study we equally investigated the effects of the co-administration of inactive doses of 5-HT2 receptor agonists and antagonists with sub-active doses of paroxetine and venlafaxine in the FPT. Locomotor activity studies were conducted in parallel to investigate the effects of drug administration on the spontaneous motor activity of mice and to discount stimulant or sedative doses.
Materials and methods
Animals
All studies employed male Swiss mice (from the Janvier breeding centre, France) housed in groups of 18 per cage for 4–6 days before experimentation. A standard 12:12 light cycle was employed with lights on at 0700 and lights off at 1900 hours. Naive animals weighing approximately 20±2 g (4 weeks old) on day of testing were randomly allotted to experimental cages. All experiments are carried out between 0700 and 1200 hours, in darkened quiet rooms. Animals are used once for each experiment. All experiments were conducted in accordance with the ethical rules of the French Ministry of Agriculture for experiments with laboratory animals (no. 87.848).
Compounds utilised
5-HT2 receptor agonists
DOI-hydrochloride [(±)-1-(2,5-dimethoxy-4-iodophenyl)-2-aminopropane] (Sigma, France); BW 723C86 hydrochloride [α-methyl-5-(2-thienylmethoxy)-1H-indole-3-ethanamine] (Tocris, France); RO 60-0175 hydrochloride [(s)-2-(6-chloro-5fluoroindol-1-yl)-1-methylethylamine hydrochloride] (Roche, Switzerland).
5-HT2 receptor antagonists
SR 46349B [2-propen-1-one, 1-(2-fluorophenyl)-3-(4-hydroxyphenyl)-O-[2-(dimethylamino)ethyl]oxime] (Sanofi Recherche, France); RS 10-2221 hydrochloride [8-[5-2,4-dimethoxy-5-(4-trifluoromethylphenylsulphonamido)phenyl-5-oxopentyl]-1,3,8-triazaspiro[4,5]decane-2,4-dione] (Tocris, France); SB 206553 hydrochloride [(N-3-pyridinyl-3,5-dihydro-5-methyl-benzo[1,2-b:4,5-b′]dipyrrole-1[2H]carboxamide) hydrochloride] (Sigma, France).
Antidepressants
Paroxetine HCl [(3S-trans)-3[(1,3-benzodioxol-5-yloxy)methyl-4-(4-floorophenyl)-piperidine] (SmithKline Beecham, France), venlafaxine [1-[2-(Dimethylamino)-1-(4-methoxyphenyl)ethyl]cyclohexanol] (Wyeth-Avert, France).
BDZ ligands
Alprazolam [8-Chloro-1-methyl-6-phenyl-4H-(1,2,4)-triazolo(4,3-a)(1,4)benzodiazepine] (Sigma, France), and diazepam [(7-chloro-1-methyl-5-phenyl-3H-1,4-benzodiazepine-2[1H]-one)] (Sigma, France).
Drug preparation
DOI, RO 60-0175, SB 206553, paroxetine and venlafaxine were dissolved in distilled water. BW 723C86, RS 10-2221, diazepam, and alprazolam were suspended in a solution of distilled water with 5% of Tween 80 (Merck, Germany).
For dose effect studies all compounds were administered 30 min before testing via the intraperitoneal (IP) route, in a dosing volume of 0.5 ml/20 g of bodyweight. For interaction and association studies pre-treatment compounds were administered IP 45 min before testing and treatment compounds IP 30 min before testing. Control animals received distilled water.
Behavioural models
General procedure
All tests were performed in a quiet, darkened room. The mice (n=10 for each group) were placed in holding cages in this room at least 1 h before the test in order to reduce any neophobic response to the test-room environment. After injection (vehicle or treatment), mice were placed in their holding cages. Mice were only used once and were not handled during the housing period. Mice were always tested in a soiled apparatus and no cleaning occurred between trials, but rather at the end of each daily test. For all procedures, observers were unaware of the treatments and all experiments were performed in a randomised manner.
Locomotor activity (actimeter test)
The spontaneous activity of naïve animals was recorded using a photoelectric actimeter (Boissier and Simon 1965). This actimeter consists of a stainless steel apparatus containing transparent cages in which the animals’ horizontal activity is measured by light beams connected to a photoelectric cell. The activity is recorded during a 10-min test period. The actimeter test is performed independently of the anxiety tests in order to examine the effect of the drugs on the spontaneous locomotor activity of mice.
Four plate test
This apparatus (Bioseb, Chaville, France) consists of a cage (18×25×16 cm) floored by four identical rectangular metal plates (8×11 cm) separated from one another by a gap of 4 mm. The plates are connected to a device that can generate electric footshocks (0.6 mA; 0.5 s). Following a 15-s habituation period, the animal is subjected to an electric shock when crossing (transition) from one plate to another, i.e. two legs on one plate and two legs on another (Boissier et al. 1968). The number of punished crossings is calculated for a period of 60 s. An anxiolytic substance is capable of augmenting the number of punished passages.
Statistical analysis
Drug alone studies
Statistical comparisons were performed initially via an one way analysis of variance (ANOVA) for independent groups, after verifying the normality of distribution by a Kolmogorof–Smirnov non-parametric test. If any statistical change was observed, data were further analysed using post hoc comparisons, with a Dunnett’s test, to detect eventual differences between control and treated groups. Data were deemed significant when P<0.05. The effects of diazepam and alprazolam, included as internal standards in the anxiety model, were compared to the control group via a Student’s t-test (P<0.05).
Interaction or association studies
For interaction and association studies, a two-way ANOVA (pre-treatment×treatment) was employed for global analysis purposes. If the ANOVA showed a significant difference between groups (P<0.05), a Sidak post hoc comparison test was performed to compare the effects of pre-treatment on treatment administered.
Results
Behavioural effects of paroxetine
Acute administration of paroxetine in the actimeter test
Paroxetine (1–32 mg/kg) did not increase locomotor activity [F(6,64)=2.112; P=0.064] in comparison to the control group (Table 1).
Acute administration of paroxetine in the FPT
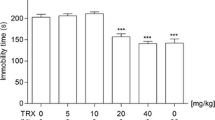
Paroxetine (0.25–8 mg/kg) increased the number of punished passages of mice in this test [F(6,69)=17.120; P<0.001] for the doses of 0.5, 2, 4 and 8 mg/kg. Alprazolam (0.25 mg/kg) also increased the number of punished passages of mice (P<0.001) (Fig. 1).
Effects of acute administration of paroxetine and venlafaxine, IP 30 min in the FPT. The results are cited as means±SEM (n=10). Statistical analysis was performed by a one-way ANOVA followed by a Dunnett’s test for comparisons between treated groups and control group ***P<0.001, **P<0.01, *P<0.05. A Student’s t-test was used for statistical analysis between the alprazolam group and control group: ^^^P<0.001
Behavioural effects of venlafaxine
Acute administration of venlafaxine in the actimeter test
Venlafaxine (1–64 mg/kg) increased locomotor activity at the dose of 64 mg/kg [F(7,72)=5.506; P<0.001] in comparison to the control group (Table 1).
Acute administration of venlafaxine in the FPT
Venlafaxine (0.25–16 mg/kg) increased the number of punished passages of mice in this test [F(7,79)=7.445; P<0.001] for the doses of 2, 4, 8 and 16 mg/kg. Alprazolam (0.25 mg/kg) also increased the number of punished passages of mice (P<0.001) [(Fig. 1)].
Behavioural effects of 5-HT2 receptor antagonists and paroxetine
Acute administration of SR 46349B a 5-HT2A receptor antagonist and paroxetine in the FPT
The administration of paroxetine (8 mg/kg) significantly increased the number of punishments accepted by mice [F(1,54)=66.339; P<0.001] in this test. Although ANOVA showed an overall effect on the number of punishments accepted in this test [F(2,54)=17.241; P<0.001], SR 46349B (0.1 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted in this test in comparison to the vehicle treated group after post hoc analysis (P>0.05). An interaction between the two treatments was observed [F(2,54)=9.181; P<0.001] and both doses of SR 46349B antagonised the anti-punishment effects of paroxetine. Diazepam (1 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Fig. 2).
Effects of acute administration of SR 46349B (IP 45 min pre-test) and paroxetine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, versus control group and +++p<0.001 versus vehicle+Parox group). A Student’s t-test was used for statistical analysis between the diazepam group and control group: ^^^P<0.001
Acute administration of SB 206553 a 5-HT2B/2C receptor antagonist and paroxetine in the FPT
The administration of paroxetine (8 mg/kg) significantly increased the number of punishments accepted by mice in this test, [F(1,54)=120.045; P<0.001]. SB 206553 (0.1 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted in this test [F(2,54)=2.161; P>0.05]. Co-administration of SB 206553 with paroxetine failed to alter the anti-punishment effects of paroxetine [F(2,54)=2.654; P>0.05]. Diazepam (1 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Fig. 3).
Effects of acute administration of SB 206553 (IP 45 min pre-test) and paroxetine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, versus control group). A Student’s t-test was used for statistical analysis between the diazepam group and control group: ^^^P<0.001
Acute administration of RS 10-2221 a 5-HT2C receptor antagonist and paroxetine in the FPT
The administration of paroxetine (8 mg/kg) significantly increased the number of punishments accepted by mice in this test, [F(1,54)=118.905; P<0.001]. RS 10-2221 (0.1 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted by mice in this test [F(2,54)=4.046; P<0.05] after post hoc analysis in comparison with the control group. Co-administration of RS 10-2221 with paroxetine failed to alter the anti-punishment effect of paroxetine [F(2,54)=3.037; P>0.05]. Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Fig. 4).
Effects of acute administration of RS 10-2221 (IP 45 min pre-test) and paroxetine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, versus control group). A Student’s t-test was used for statistical analysis between the alprazolam group and control group: ^^^P<0.001
Behavioural effects of 5-HT2 receptor antagonists and venlafaxine
Acute administration of SR 46349B a 5-HT2A receptor antagonist and venlafaxine in the FPT
The administration of venlafaxine (8 mg/kg) significantly increased the number of punishments accepted [F(1,54)=19.120; P<0.001]. SR 46349B (0.1 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted in this test in comparison to the vehicle treated group after post hoc analysis (P>0.05), despite a significant effect of the ANOVA [F(2,54)=11.395; P<0.001]. An interaction between the two treatments was observed [F(2,54)=8.684; P<0.001] and both doses of SR 46349B antagonised the anti-punishment effects of venlafaxine. Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001) [(Fig. 5)].
Effects of acute administration of SR 46349B (IP 45 min pre-test) and venlafaxine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, versus control group and ++p<0.01, +++P<0.001 versus vehicle+Venla. group). A Student’s t-test was used for statistical analysis between the alprazolam group and control group: ^^^P<0.001
Acute administration of SB 206553 a 5-HT2B/2C receptor antagonist and venlafaxine in the FPT
The administration of venlafaxine (8 mg/kg) significantly increased the number of punishments accepted [F(1,54)=24.680; P<0.001] (Fig. 6). SB 206553 (0.1 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted by mice in this test [F(2,54)=1.415; P>0.05]. An interaction between the two treatments was observed [F(2,54)=11.868; P<0.001] and both doses of SB 206553 antagonised the anti-punishment effects of venlafaxine. Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001).
Effects of acute administration of SB 206553 (IP 45 min pre-test) and venlafaxine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, versus control group and ++P<0.01, versus vehicle+Venla. group). A Student’s t-test was used for statistical analysis between the alprazolam group and control group: ^^^P<0.001
Acute administration of RS 10-2221 a 5-HT2C receptor antagonist and venlafaxine in the FPT
The administration of venlafaxine (8 mg/kg) significantly increased the number of punishments accepted [F(1,54)=38.976; P<0.001] (Fig. 7). RS 10-2221 (0.1 mg/kg and 1 mg/kg IP 45 min pre-test) had no effect on the number of punishments accepted in this test [F(2,54)=1.432; P>0.05] after sole administration. Co-administration of RS 10-2221 with venlafaxine failed to alter the anti-punishment effect of venlafaxine [F(2,54)=1.016; P>0.05]. Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001).
Effects of acute administration of RS 10-2221 (IP 45 min pre-test) and venlafaxine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, versus control group). A Student’s t-test was used for statistical analysis between the alprazolam group and control group: ^^^P<0.001
Behavioural effects of 5-HT2 receptor agonists and paroxetine
Acute administration of DOI a 5-HT2A receptor agonist and paroxetine in the FPT
Although the ANOVA was statistically significant [F(2,81)=15.969; P<0.001 and F(2,81)=13.019; P<0.001, respectively], DOI (0.06 mg/kg and 0.25 mg/kg) and paroxetine (0.25 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted in this test, after post hoc analysis (P>0.05), in comparison to the control group. No interaction between the two treatments was observed [F(4,81)=1.225; P>0.05]. Diazepam (1 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Table 2).
Acute administration of BW 723C86 a 5-HT2B receptor agonist and paroxetine in the FPT
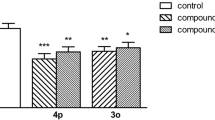
BW 723C86 (0.5 mg/kg and 2 mg/kg) and paroxetine (0.25 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted by mice in this test [F(2,81)=16.864; P<0.05] and [F(2,81)=36.483; P<0.05], respectively, after post hoc analysis in comparison to the control group. There was an interaction however between the two treatments [F(4,81)=4.537; P<0.05]. Both doses of BW 723C86 (0.5 mg/kg and 2 mg/kg) and paroxetine 1 mg/kg administration increased the number of plate crossings in comparison to the appropriate paroxetine group. Diazepam (1 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Fig. 8).
Effects of acute administration of BW 723C86 (IP 45 min pre-test) and paroxetine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, *P<0.05 versus control group and +++P<0.001 versus vehicle+Parox. group). A Student’s t-test was used for statistical analysis between the diazepam group and control group: ^^^P<0.001
Acute administration of RO 60-0175 a 5-HT2C receptor agonist and paroxetine in the FPT
The administration of RO 60-0175 (0.25 mg/kg and 1 mg/kg) and paroxetine (0.25 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted by mice in this test [F(2,81)=5.286; P<0.05] and [F(2,81)=14.792; P<0.05], respectively, in comparison to the control group after post hoc analysis. There was an interaction between the two treatments [F(4,81)=4.717; P<0.05]. The co-administration of RO 60-0175 (1 mg/kg) and paroxetine (0.25 mg/kg) significantly increased the number of punished passages accepted by mice, in comparison to the appropriate paroxetine control group. Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Fig. 9).
Effects of acute administration of RO 60-0175 (IP 45 min pre-test) and paroxetine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, **P<0.01, *p<0.05 versus control group and +++P<0.001 versus vehicle+Parox. group). A Student’s t-test was used for statistical analysis between the alprazolam group and control group: ^^^P<0.001
Behavioural effects of 5-HT2 receptor agonists and venlafaxine
Acute administration of DOI a 5-HT2A receptor agonist and venlafaxine in the FPT
The administration of DOI (0.06 mg/kg and 0.25 mg/kg) and venlafaxine (0.25 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted by mice in this test, after post hoc analysis (P>0.05), in comparison to the control group despite significant ANOVA [F(2,81)=21.797; P<0.001] and [F(2,81)=9.933; P<0.001], respectively. An interaction between the two treatments was observed [F(4,81)=2.936; P<0.05]. The co-administration of both doses of DOI (0.06 mg/kg and 0.25 mg/kg) and venlafaxine 0.25 mg/kg increased the number of punished passages accepted by mice in comparison to the appropriate control group, as did DOI (0.25 mg/kg) in association with venlafaxine (1 mg/kg). Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Fig. 10).
Effects of acute administration of DOI (IP 45 min pre-test) and venlafaxine (IP 30 min pre-test), on the number of punishments accepted by mice in the FPT. The data are cited as means±SEM, (n=10). Statistical analysis was performed by a two-way ANOVA followed by a Sidak test (***P<0.001, *P<0.05 versus control group and +++P<0.001, ++P<0.01 versus vehicle+Venla. group). A Student’s t-test was used for statistical analysis between the alprazolam group and control group: ^^^P<0.001
Acute administration of BW 723C86 a 5-HT2B receptor agonist and venlafaxine in the FPT
The administration of BW 723C86 (0.5 mg/kg and 2 mg/kg) and venlafaxine (0.25 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted by mice in this test, [F(2,81)=1.186; P>0.05] and [F(2,81)=1.855; P>0.05], respectively. There was no interaction between the two treatments [F(4,81)=0.905; P>0.05]. Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Table 2).
Acute administration of RO 60-0175 a 5-HT2C receptor agonist and venlafaxine in the FPT
The administration of RO 60-0175 (0.25 mg/kg and 1 mg/kg) and venlafaxine (0.25 mg/kg and 1 mg/kg) had no effect on the number of punishments accepted by mice in this test [F(2,81)=1.141; P>0.05] and [F(2,81)=0.952; P>0.05], respectively, in comparison to the control group. There was no interaction between the two treatments [F(4,81)=1.298; P>0.05]. Alprazolam (0.25 mg/kg) significantly increased the number of punished passages of mice (P<0.001) (Table 2).
Discussion
This study compared the behavioural profiles of two clinically used ADs, the SSRI paroxetine and the SNRI venlafaxine in a mouse model of anxiety, the FPT. This research demonstrated that paroxetine (0.5, 2, 4, and 8 mg/kg) and venlafaxine (2, 4, 8 and 16 mg/kg) dose dependently increased plate crossing, the order of potency being similar to that found in a previous study (Hascoët et al. 2000a). The magnitude of response was slightly greater for paroxetine. This may be due to differences in the inhibitory potencies for 5-HT re-uptake of both compounds, i.e. in vitro IC50=1 nmol/l for paroxetine and IC50=39 nmol/l for venlafaxine. Differences also exist for the re-uptake inhibitory potencies for NA and DA, respectively: IC50=350 and 5100 nmol/l for paroxetine and IC50=213 and 2,800 nmol/l for venlafaxine (Kent 2000). The correlation between these in vitro values and the in vivo effects of each compound remains ambiguous. Recent microdialysis studies demonstrated a significantly greater increase in extracellular 5-HT in the prefrontal cortex of mice by venlafaxine (8 mg/kg, IP) in comparison to paroxetine (1, 4 and 8 mg/kg, IP) (David et al. 2003). The extrapolation of these results to behavioural responses remains difficult (Deakin et al. 1993), as the question persists as to whether or not the same reaction occurs when mice (subsequent to venlafaxine or paroxetine administration), are subjected to the FPT.
The acute administration of paroxetine has produced anxiolytic-like effects in a few animal models of anxiety; the mouse FPT, the mouse L/D paradigm; isolation-induced vocalisation in rats; shock-induced vocalisations in rats, schedule-induced polydipsia and the mouse defense test battery (Njung’e and Handley 1991; Winslow and Insel 1991; Woods et al. 1993; Hashimoto et al. 1996; Schreiber et al. 1998; Hascoët et al. 2000a,b; Beijamini and Andreatini 2003). No effects have been reported in conflict procedures in rats and the social interaction paradigm (Petersen and Lassen 1981; Lightowler et al. 1994; Duxon et al. 2000) while anxiogenic-like effects have been documented in the rat EPM and L/D test (Sanchez and Meier 1997; Kõks et al. 2001) and the mouse EPM (Nic Dhonnchadha et al., unpublished data).
The acute administration of venlafaxine has not been as extensively studied in anxiety models but has, however, produced anxiolytic-like effects in the mouse FPT; isolation-induced vocalisations in guinea pigs and marble burying behaviour in mice (Hascoët et al. 2000a; Rupniak et al. 2000; Millan et al. 2001b). One major problem in interpreting these results concerns the analgesic effect of AD drugs (they have been widely used in the treatment of chronic pain). However, in animal experiments, systemic administration of ADs have yielded confusing results in tests of nociception. Theoretically, a possible analgesic action could account for the effects observed in this procedure. However, at doses active in alleviating pain in various tests, morphine did not increase the number of shocks received in the FPT (Boissier et al. 1968). Concerning AD drugs, serotonin reuptake inhibitors produce analgesic effects in the hot plate test (Fasmer et al. 1989; Ardid et al. 1992), but the effect was not stronger than those of norepinephrine reuptake inhibitors, like desipramine (Fasmer et al. 1989). Furthermore, antinociceptive activity was not observed in the hot plate reaction test with citalopram (Hyttel 1994) except at high doses (Fasmer et al. 1989), in addition the antinociceptive effect of paroxetine was found for higher doses than the one producing anxiolytic-like effect and was not affected by 5HT2 mechanism (Duman et al. 2004).
Although most SSRIs and SNRIs have both been found to have analgesic properties, they were not all found to be active in a previous study (Hascoët et al. 2000a). For example fluoxetine did not induce any anti-punishment effects in the FPT. Thus, one may conclude that the effects found for the active ADs in the FPT were indeed anxiolytic-like and not analgesic effects.
Clinical studies have demonstrated SSRI-induced anxiety and even occasional panic attacks at initiation of SSRI-treatment, a mechanism suggested to be mediated by stimulation of 5-HT2 receptors in the serotonin pathway that projects to the hippocampus and limbic cortex. Equally, the 5-HT2A receptor antagonist properties are believed to enhance antidepressant and anti-anxiety activities of many ADs (Szabo and Blier 2002). In contrast, in a previous study (Nic Dhonnchadha et al. 2003), we have observed an anxiolytic-like action of 5-HT2A/2B receptor agonists in the FPT. Different brain areas may be implicated in the anxiolytic-like responses detected, with 5-HT2 receptors in the peri-aqueductal gray area (PAG) involved in the anxiolytic response observed in the mouse EPM (unconditioned fear), whereas the same receptors in the amygdala may be involved in the response which was provoked in the FPT (conditioned fear), thus explaining different or opposing effects being observed with the same molecule, depending on the paradigm used. Thus the second part of this study involved the identification of the potential involvement of the 5-HT2 receptor subtypes in the anxiety effects of both paroxetine and venlafaxine.
Conflicting results as to the in vitro affinities of paroxetine and venlafaxine for the 5-HT2 receptor subtypes in the rat brain have been documented. The receptor binding affinity (IC50, nM) of paroxetine and venlafaxine is 18,000 and >10,000 for the 5-HT2A receptor and 20,000 and 40,000 for the 5-HT2C receptors, respectively (Hyttel 1994). Another study reported a Ki (nM) value of 6.320 for the 5-HT2A receptor for paroxetine and >100,000 for venlafaxine (Owens et al. 1997). The binding affinity for the 5-HT2B receptor was not determined. However, the in vivo binding profile of many compounds may differ substantially from the in vitro profile, complicating the interpretation of results.
The 5-HT2A receptor antagonist SR 46349B blocked the anti-punishment activity of paroxetine, while the 5-HT2B/2C receptor antagonist, SB 206553 and the 5-HT2C receptor antagonist, RS 10-2221 did not alter the effects of paroxetine. These results suggest that the 5-HT2A and not the 5-HT2B or 5-HT2C receptors are involved in the anxiolytic-like action of paroxetine in the mouse FPT. A similar study reported the participation of the 5-HT2A receptor in the ultrasonic vocalisation-reducing activity of paroxetine in rats, as only the selective 5-HT2A receptor antagonist (MDL 100,907) reversed the effects of paroxetine, whereas compounds with less selectivity, i.e. ritanserin and ketanserin, failed to alter the effects of paroxetine (Schreiber et al. 1998), possibly due to their affinity for the 5-HT2C receptor subtype.
This is one of the first studies to examine the potential role of the 5-HT2 receptors in the anxiolytic effects of venlafaxine. The anti-punishment action of venlafaxine was eliminated by both doses of SR 46349B and SB 206553 (0.1 mg/kg and 1 mg/kg), which when administered alone were without effect. The 5-HT2C receptor antagonist RS 10-2221 failed to alter the effects of venlafaxine, implicating both the 5-HT2A and 5-HT2B receptor subtypes but not the 5-HT2C receptors in the anxiolytic-like action of venlafaxine in the FPT.
Our results strongly suggest that activation of 5-HT2A receptors is critically involved in the anxiolytic activity of paroxetine, whereas the 5-HT2A and 5-HT2B receptors are involved in the anti-punishment action of venlafaxine in the FPT. A more complete profile of the exact mechanisms involved in the anxiolytic-like effects of both ADs requires more extensive interaction studies employing various receptor antagonists of other 5-HT receptor subtypes, e.g. 5-HT1B/1D, 5-HT3, 5-HT4 and monoamine transporter blockers, before definite conclusions can be drawn about the role of 5-HT receptor subtypes in the therapeutic effects of these two ADs.
The next part of the present study was undertaken to determine whether the association of 5-HT2 receptor agonists or antagonists with the ADs, paroxetine and venlafaxine could act in synergy, to induce anti-anxiety effects. The co-administration of 5-HT2 ligands with paroxetine or venlafaxine failed to alter the spontaneous motor activity of mice in the actimeter test (data not shown).
The co-administration of 5-HT2 agonists with paroxetine in the FPT demonstrated potentiation effects. DOI (a 5-HT2A receptor agonist), increased the effects of paroxetine in this model, however, in a non-significant manner, whereas RO 60-0175 (a 5-HT2C receptor agonist), only augmented the paroxetine response at one dose (1 mg/kg) and only at the weakest dose of paroxetine (0.25 mg/kg). However, BW 723C86 (a 5-HT2B receptor agonist) significantly potentiated the effects of paroxetine at both doses employed.
RO 60-0175 at 1 mg/kg may occupy 5-HT2B receptors, as it has been recently revealed to possess potent affinity for this receptor (pKi=9.3) and has now been suggested to act as a non-selective agonist for the 5-HT2C receptor (Damjanoska et al. 2003). This activation in conjunction with the lower dose of paroxetine may lead to an increase of synaptic 5-HT, resulting in the observed anti-punishment effects. At the higher dose of paroxetine the increase in 5-HT may lead to the activation of 5-HT auto-receptors, inducing the attenuation of 5-HT release and consequently decreasing 5-HT levels. Dopaminergic neurotransmission may equally be implicated as several studies have reported the opposing influence of 5-HT2C receptor ligands on dopamine firing (Di Matteo et al. 2002) depending on the brain region examined.
The mechanisms involved in the synergistic effects of BW 723C86 and RO 60-0175 with paroxetine are not the same as those of venlafaxine, as both RO 60-0175 and BW 723C86 failed to alter the response of venlafaxine after combination treatment, whereas DOI significantly increased the effects of venlafaxine. It may be that the doses used for venlafaxine were too weak to induce adequate 5-HT synaptic release in combination with BW 723C86 and RO 60-0175 to produce an anxiolytic-like effect or that the doses of the 5-HT2 receptor agonists employed resulted, in inhibitory effects via auto-receptor stimulation. Only co-treatment with DOI induced anti-punishment action; however the effects were greater at the lower doses of venlafaxine. Different neurotransmitter systems may be implicated at these doses, e.g. NA and 5-HT. Comprehensive receptor binding in conjunction with microdialysis studies would possibly enlighten us on this subject.
In conclusion, these results demonstrate that 5-HT2A and 5-HT2B receptor agonism can augment the anxiolytic-like properties of venlafaxine and paroxetine, respectively, in the FPT (Table 3). It can thus be suggested that 5-HT2 receptor agonists have the capacity to potentiate anxiolytic-like effects of these drugs and such association studies may lead to the development of novel combination therapies, e.g. SSRI or SNRI and 5-HT2A/2B receptor agonist.
References
Ables AZ, Baughman OL III (2003) Antidepressants: update on new agents and indications. Am Fam Phys 67:547–554
Ardid D, Marty H, Fialip J, Privat AM, Eschalier A, Lavarenne J (1992) Comparative effects of different uptake inhibitor antidepressants in two pain tests in mice. Fundam Clin Pharmacol 6:75–82
Beijamini V, Andreatini R (2003) Effects of Hypericum perforatum and paroxetine on rat performance in the elevated T-maze. Pharmacol Res 48:199–207
Besson A, Haddjeri N, Blier P, De Montigny C (2000) Effects of the co-administration of mirtazapine and paroxetine on serotonergic neurotransmission in the rat brain. Eur Neuropsychopharmacol 10:177–188
Beyer CE, Boikess S, Luo B, Dawson LA (2002) Comparison of the effects of antidepressants on norepinephrine and serotonin concentrations in the rat frontal cortex: an in-vivo microdialysis study. J Psychopharmacol 16:297–304
Boissier JR, Simon P (1965) Action of caffeine on the spontaneous motility of the mouse. Arch Int Pharmacodyn Ther 158:212–221
Boissier JR, Simon P, Aron C (1968) A new method for rapid screening of minor tranquillizers in mice. Eur J Pharmacol 4:145–151
Borsini F, Podhorna J, Marazziti D (2002) Do animal models of anxiety predict anxiety-like effects of antidepressants. Psychopharmacology 163:121–141
Bourin M, Lambert O (2002) Pharmacotherapy of anxious disorders. Hum Psychopharmacol 17:383–400
Bourin M, Chue P, Guillon Y (2001) Paroxetine: a review. CNS Drug Rev 7:25–47
Bourin M, David DJ, Jolliet P, Gardier A (2002) Mechanism of action of antidepressants and therapeutic perspectives. Therapie 57:385–396
Briley M (2003) New hope in the treatment of painful symptoms in depression. Curr Opin Invest Drugs 4:42–45
Cusack B, Nelson A, Richelson E (1994) Binding of antidepressants to human brain receptors: focus on newer generation compounds. Psychopharmacology 114:559–565
Damjanoska KJ, Muma NA, Zhang Y, D’Souza DN, Garcia F, Carrasco GA, Kindel GH, Haskins KA, Shankaran M, Petersen BR, Van de Kar LD (2003) Neuroendocrine evidence that (S)-2-(chloro-5-fluoro-indol- l-yl)-1-methylethylamine fumarate (Ro 60-0175) is not a selective 5-hydroxytryptamine(2C) receptor agonist. J Pharmacol Exp Ther 304:1209–1216
David DJ, Bourin M, Jego G, Przybylski C, Jolliet P, Gardier AM (2003) Effects of acute treatment with paroxetine, citalopram and venlafaxine in vivo on noradrenaline and serotonin outflow: a microdialysis study in Swiss mice. Br J Pharmacol 140:1128–1136
Davidson JR, Dupont RL, Hedges D, Haskins JT (1999) Efficacy, safety, and tolerability of venlafaxine extended release and buspirone in outpatients with generalized anxiety disorder. J Clin Psychiatry 60:528–535
Deakin JF, Graeff FG, Guimaraes FS (1993) Clinical implication of microdialysis findings. Trends Pharmacol Sci 14:263
Di Matteo V, Cacchio VM, Di Giulio C, Esposito E (2002) Role of serotonin 2C receptors in the control of brain dopaminergic function. Pharmacol Biochem Behav 71:727–734
Duman EN, Kesim M, Kadioglu M, Yaris E, Kalyoncu NI, Erciyes N (2004) Possible involvement of opioide and serotonergic mechanisms in antinociceptive effect of paroxetine in acute pain. J Pharmacol Sci 94:161–165
Duxon MS, Starr KR, Upton N (2000) Latency to paroxetine-induced anxiolysis in the rat is reduced by co-administration of the 5-HT1A receptor antagonist WAY100635. Br J Pharmacol 130:1713–1719
Fasmer OB, Hunskaar S, Hole K (1989) Antinociceptive effects of serotonergic reuptake inhibitors in mice. Neuropharmacology 28:1363–1366
Felton TM, Kang TB, Hjorth S, Auerbach SB (2003) Effects of selective serotonin and serotonin/noradrenaline reuptake inhibitors on extracellular serotonin in rat diencephalon and frontal cortex. Naunyn Schmiedebergs Arch Pharmacol 367:297–305
Ferreri M, Lavergne F, Berlin I, Payan C, Puech AJ (2001) Benefits from mianserin augmentation of fluoxetine in patients with major depression non-responders to fluoxetine alone. Acta Psychiatr Scand 103:66–72
Fuller RW (1994) Uptake inhibitors increase extracellular serotonin concentration measured by brain microdialysis. Life Sci 55:163–167
Gelenberg AJ, Lydiard RB, Rudolph RL, Aguiar L, Haskins JT, Salinas E (2000) Efficacy of venlafaxine extended-release capsules in nondepressed outpatient with generalized anxiety disorder: a 6-month randomized controlled trial. JAMA 283:3082–3088
Hascoët M, Bourin M, Colombel MC, Fiocco AJ, Baker GB (2000a) Anxiolytic-like effects of antidepressants after acute administration in a four-plate test in mice. Pharmacol Biochem Behav 65:339–344
Hascoët M, Bourin M, Nic Dhonnchadha BÁ (2000b) The influence of buspirone, and its metabolite 1-PP, on the activity of paroxetine in the mouse light/dark paradigm and four plates test. Pharmacol Biochem Behav 67:45–53
Hashimoto S, Inoue T, Koyama T (1996) Serotonin reuptake inhibitors reduce conditioned fear stress-induced freezing behaviour in rats. Psychopharmacology 123:182–186
Hyttel J (1994) Pharmacological characterisation of selective serotonin reuptake inhibitors (SSRIs). Int Clin Psychopharmacol 9:19–26
Kent JM (2000) SNaRIs, NaSSAs and NaRIs: new agents for the treatment of depression. Lancet 355:911–918
Kõks S, Beljajev S, Koovit I, Abramov U, Bourin M, Vasar E (2001) 8-OH-DPAT, but not deramciclane, antagonizes the anxiogenic-like action of paroxetine in an elevated plus-maze. Psychopharmacology 153:365–372
Kreiss DS, Lucki I (1995) Effects of acute and repeated administration of antidepressant drugs on extracellular levels of 5-hydroxytryptamine measured in vivo. J Pharmacol Exp Ther 274:866–876
Lambert O, Bourin M (2002) SNRIs: mechanism of action and clinical features. Expert Rev Neurother 2:849–858
Lightowler S, Kennett GA, Williamson IJ, Blackburn TP, Tulloch IF (1994) Anxiolytic-like effect of paroxetine in a rat social interaction test. Pharmacol Biochem Behav 49:281–285
McDougle CJ, Epperson CN, Pelton GH, Wasylink S, Price LH (2000) A double-blind, placebo-controlled study of risperidone addition in serotonin reuptake inhibitor-refractory obsessive-compulsive disorder. Arch Gen Psychiatry 57:794–801
Millan MJ, Gobert A, Lejeune F, Newman-Tancredi A, Rivet JM, Auclair A, Peglion JL (2001a) S33005, a novel ligand at both serotonin and norepinephrine transporters: I. Receptor binding, electrophysiological, and neurochemical profile in comparison with venlafaxine, reboxetine, citalopram, and clomipramine. J Pharmacol Exp Ther 298:565–580
Millan MJ, Dekeyne A, Papp M, La Rochelle CD, MacSweeney C, Peglion JL, Brocco M (2001b) S33005, a novel ligand at both serotonin and norepinephrine transporters. II. Behavioral profile in comparison with venlafaxine, reboxetine, citalopram, and clomipramine. J Pharmacol Exp Ther 298:581–591
Mork A, Hogg S (2002) The 5-HT2C antagonist, irindalone has the potential as add-on therapy in combination with SSRIs: Microdialysis and light dark box studies. Int J Neuropsychopharmacol 5(Suppl 1):S69
Muth EA, Haskins JT, Moyer JA, Husbands GE, Nielsen ST, Sigg EB (1986) Antidepressant biochemical profile of the novel bicyclic compound Wy-45,030, an ethyl cyclohexanol derivative. Biochem Pharmacol 35:4493–4497
Nemeroff CB (2003) Anxiolytics: past, present, and future agents. J Clin Psychiatry 64:3–6
Nic Dhonnchadha BÁ, Hascoët M, Bourin M (2003) Anxiolytic-like effects of 5-HT2 ligands on three mouse models of anxiety. Behav Brain Res 140:203–214
Nierenberg AA (2001)Do some antidepressants work faster than others? J Clin Psychiatry 62:22–25
Ninan PT (2000) Use of venlafaxine in other psychiatric disorders. Depress Anxiety 12:90–94
Njung’e K, Handley SL (1991) Effects of 5-HT uptake inhibitors, agonists and antagonists on the burying of harmless objects by mice; a putative test for anxiolytic agents. Br J Pharmacol 104:105–112
Owens MJ, Morgan WN, Plott SJ, Nemeroff CB (1997) Neurotransmitter receptor and transporter binding profile of antidepressants and their metabolites. J Pharmacol Exp Ther 283:1305–1322
Petersen EN, Lassen JB (1981) A water lick conflict paradigm using drug experienced rats. Psychopharmacology 75:236–239
Pollack MH, Zaninelli R, Goddard A (2001) Paroxetine in the treatment of generalised anxiety disorders: results of a placebo controlled, flexible-dosage trial. J Clin Psychiatry 62:350–357
Prut L, Belzung C (2003) The open field as a paradigm to measure the effects of drugs on anxiety-like behaviours: a review. Eur J Pharmacol 463:3–33
Rasmussen BB, Brosen K (2000) Is therapeutic drug monitoring a case for optimizing clinical outcome and avoiding interactions of the selective serotonin reuptake inhibitors? Ther Drug Monit 22:143–154
Rickels K, Pollack MH, Sheehan DV, Haskins JT (2000) Efficacy of extended-release venlafaxine in nondepressed outpatients with generalized anxiety disorder. Am J Psychiatry 157:968–974
Rosen RC, Lane RM, Menza M (1999) Effects of SSRIs on sexual function: a critical review. J Clin Psychopharmacol 19:67–85
Rupniak NM, Carlson EC, Harrison T, Oates B, Seward E, Owen S, De Felipe C, Hunt S, Wheeldon A (2000) Pharmacological blockade or genetic deletion of substance P (NK(1)) receptors attenuates neonatal vocalisation in guinea-pigs and mice. Neuropharmacology 39:1413–1421
Sanchez C (2003) Stress-induced vocalisation in adult animals. A valid model of anxiety? Eur J Pharmacol 463:133–143
Sanchez C, Meier E (1997) Behavioural profiles of SSRIs in animal models of depression, anxiety and aggression. Are they all alike? Psychopharmacology 129:197–205
Schreiber R, Melon C, De Vry J (1998) The role of 5-HT receptor subtypes in the anxiolytic effects of selective serotonin reuptake inhibitors in the rat ultrasonic vocalization test. Psychopharmacology 135:383–391
Stahl SM (1998) Mechanism of action of serotonin selective reuptake inhibitors. Serotonin receptors and pathways mediate therapeutic effects and side effects. J Affect Disord 51:215–235
Stahl SM, Entsuah R, Rudolph RL (2002) Comparative efficacy between venlafaxine and SSRIs: a pooled analysis of patients with depression. Biol Psychiatry 52:1166–1174
Szabo ST, Blier P (2002) Effects of serotonin (5-hydroxytryptamine, 5-HT) reuptake inhibition plus 5-HT2A receptor antagonism on the firing activity of norepinephrine neurons. J Pharmacol Exp Ther 302:983–991
Vaswani M, Linda FK, Ramesh S (2003) Role of selective serotonin reuptake inhibitors in psychiatric disorders: a comprehensive review. Prog Neuropsychopharmacol Biol Psychiatry 27:85–102
Winslow JT, Insel TR (1991) The infant rat separation paradigm: a novel test for novel anxiolytics. Trends Pharmacol Sci 12:402–404
Woods A, Smith C, Szewczak M, Dunn RW, Cornfeldt M, Corbett R (1993) Selective serotonin re-uptake inhibitors decrease schedule-induced polydipsia in rats: a potential model for obsessive compulsive disorder. Psychopharmacology 112:195–198
Zohar J, Westenberg HG (2000) Anxiety disorders: a review of tricyclic antidepressants and selective serotonin reuptake inhibitors. Acta Psychiatr Scand Suppl 403:39–49
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nic Dhonnchadha, B.Á., Ripoll, N., Clénet, F. et al. Implication of 5-HT2 receptor subtypes in the mechanism of action of antidepressants in the four plates test. Psychopharmacology 179, 418–429 (2005). https://doi.org/10.1007/s00213-004-2044-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-004-2044-y