Abstract
Apigenin has a protective effect on d-galactosamine (d-GalN)/lipopolysaccharide (LPS)-induced mouse liver injury through the increments of hepatic nuclear factor erythroid 2-related factor 2 (Nrf-2) and peroxisome proliferator–activated receptor γ (PPARγ) expressions, but its exact mechanisms are still uncertain. This study aimed to further verify its protective effect on hepatocytes and to determine its target of action. The results showed that after treatment of D-GalN/LPS-stimulated hepatocytes with 2.5–20 μM apigenin, the supernatant alanine aminotransferase, aspartate aminotransferasein, tumor necrosis factor-α, and malondialdehyde levels and intracellular nuclear factor-κB protein expression were decreased, while the supernatant superoxide dismutase (SOD) and catalase (CAT) levels, intracellular PPARγ and inhibitor of kappa B-alpha protein expressions, and nucleus Nrf-2 protein expression were increased. After pretreatment with BML-111 or GW9662, the apigenin-induced nucleus Nrf-2 or intracellular PPARγ protein expressions were completely inhibited, respectively, but the both pretreatment differently affected the protective effect of apigenin on hepatocytes. The former completely canceled the protective effect, whereas the latter did not. These findings further demonstrate that apigenin can exert a protective effect on D-GalN/LPS-induced hepatocellular injury via the increment of Nrf-2 nucleus translocation, which may increase the SOD and CAT levels and PPARγ protein expression and subsequently inhibit the inflammatory response.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The pathogenesis of liver injury is very complicated and has not been completely elucidated yet. The virus infection (Oh and Park 2015), drug overdose (Stine and Chalasani 2017), idiosyncratic drug reaction (Mosedale and Watkins 2017), and heavy ethanol ingestion (Lee 2012; Wang et al. 2017) are main pathogenic factors and can cause the hepatic oxidative stress and inflammatory response, which is an important mechanism of liver injury (Jaeschke 2000). Nuclear factor erythroid 2-related factor 2 (Nrf-2), a redox-sensitive transcription factor, can control the expressions of anti-oxidative genes (Jaiswal 2004), while peroxisome proliferator-activated receptor γ (PPARγ) can also ameliorate the oxidative stress and inflammatory response by inhibiting nuclear factor-κB (NF-κB) activation and inflammatory cytokine production (Moraes et al. 2006). Recent study has revealed that Nrf-2 can positively regulate the PPARγ expression to protect against acute lung injury in mice (Cho et al. 2010), suggesting that the both may exert a synergic inhibitory effects on oxidative stress and inflammatory response.
Apigenin is a natural plant flavonoid that is abundant in plenty of vegetables (Tsanova-Savova and Ribarova 2013), fruits (Wang et al. 2018a), and medicinal plants (Vissiennon et al. 2017), some literature data have reported that apigenin has anti-oxidative and anti-inflammatory effects (Duarte et al. 2013; Han et al. 2012; Xu et al. 2016). Our previous study has shown that apigenin can inhibit the d-galactosamine (d-GalN)/lipopolysaccharide (LPS)-induced mouse liver injury through the increments of hepatic Nrf-2 and PPARγ expressions (Zhou et al. 2017). But, how apigenin affects the Nrf-2 and PPARγ remains unclear. In the present study, we examined the effects of apigenin in D-GalN/LPS-stimulated rat BRL cells to further understand its exact protective molecular mechanisms.
Materials and methods
Chemicals and reagents
Apigenin, with a purity of 98%, was kindly provided by Suzhou Baozetang Medical Technology Co., Ltd. (Suzhou, China), and solubilized in 1‰ dimethyl sulfoxide (DMSO) solution. d-GalN (purity > 99%) and LPS were the products of Sigma-Aldrich (St. Louis, MO, USA). GW9662 (purity > 98%) was purchased from Cayman Chemical Company (Michigan, USA) and dissolved in 1‰ DMSO solution. BML-111 (purity > 99%) was purchased from Abcam Company (Cambridge, UK) and dissolved in 1‰ DMSO solution. The assay kits for alanine aminotransferase (ALT), aspartate aminotransferase (AST), malondialdehyde (MDA), catalase (CAT), and superoxide dismutase (SOD) were purchased from Nanjing Jiancheng Bioengineering Institute (Nanjing, China). The ELISA kit for rat tumor necrosis factor-α (TNF-α) was provided by Shanghai Xitang Biotechnological Co., Ltd. (Shanghai, China). Anti-NF-κB p65, anti-IκB-α, and anti-β-actin antibodies were purchased from Cell Signaling Technology (Boston, MA, USA). Anti-Nrf-2 and anti-PPARγ antibodies were obtained from Proteintech Group Co., Ltd. (Wuhan, China). Anti-Lamin B1 antibody was a product of Abcam Company (Cambridge, UK).
Cell culture
The rat BRL hepatocytes were obtained from Shanghai Institute of Biochemistry and Cell Biology, Chinese Academy of Sciences (Shanghai, China), and cultured in RPMI 1640 solution containing 10% fetal bovine serum at 37 °C in a humidified atmosphere with 5% CO2.
Treatment of d-GalN/LPS-stimulated hepatocytes with apigenin
The BRL cells were seeded into 6-well plates with a density of 5 × 105 cells/well and divided into 7 groups: control group, d-GalN/LPS group, d-GalN/LPS plus 1‰ DMSO group, and d-GalN/LPS plus apigenin 2.5, 5, 10, and 20 μM groups. After the cells of the latter five groups were respectively treated with 1‰ DMSO or 2.5, 5, 10, and 20 μM apigenin for 2 h, these cells, together with the D-GalN/LPS group, were stimulated with 8 mM D-GalN for 1 h and subsequently incubated with 1 μg/ml LPS for an additional 9 h. Finally, the cultured cells and supernatants were collected to measure the design parameters.
Pretreatment of apigenin-treated and d-GalN/LPS-stimulated hepatocytes with BML-111
The BRL cells were divided into 8 groups: control group, d-GalN/LPS group, d-GalN/LPS plus 1‰ DMSO group, d-GalN/LPS plus apigenin 20 μM group, d-GalN/LPS plus BML-111 group, d-GalN/LPS plus BML-111 plus apigenin 20 μM group, BML-111 group, and BML-111 plus apigenin 20 μM group. The cells of last four groups were firstly treated with 200 nM BML-111 for 2 h and the subsequent procedures of the cell treatment were the same as above apigenin-treated section.
Pretreatment of apigenin-treated and d-GalN/LPS-stimulated hepatocytes with GW9662
The BRL cells were divided into 8 groups: control group, d-GalN/LPS group, d-GalN/LPS plus 1‰ DMSO group, d-GalN/LPS plus apigenin 20 μM group, d-GalN/LPS plus GW9662 group, d-GalN/LPS plus GW9662 plus apigenin 20 μM group, GW9662 group, and GW9662 plus apigenin 20 μM group. The cells of last four groups were firstly treated with 10 μM GW9662 for 2 h and the subsequent procedures of the cell treatment were the same as above apigenin-treated section.
Measurements of supernatant ALT, AST, SOD, CAT, MDA, and TNF-α levels
The collected supernatants were used for measurements of ALT, AST, SOD, CAT, and MDA levels according to the colorimetric methods, respectively, and the supernatant TNF-α level was detected by the ELISA method.
Measurements of nucleus Nrf-2 protein expression and intracellular PPARγ, NF-κB, and IκB-α protein expressions
The nuclear and cytoplasmic proteins were extracted following the kit’s instructions (Nanjing KeyGen Biotech Co., Ltd., China) and the expression levels of intracellular PPARγ, NF-κB, and IκB-α and nucleus Nrf-2 proteins were detected by the Western blot method according to our previous description (Wang et al. 2018b; Zhao et al. 2018).
Statistical analysis
The data were expressed as the mean ± SD of samples from three independent experiments. The significance of difference between experimental groups was determined by using one-way ANOVA followed by a post hoc LSD test. The statistical analysis was performed by using SPSS 19.0 software (IBM, USA), and P < 0.05 was considered as different significance.
Results
Apigenin decreases the cultured supernatant ALT and AST levels
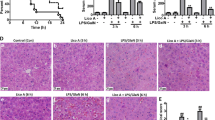
The results are presented in Fig. 1. Compared with the control group, the levels of supernatant ALT and AST in the d-GalN/LPS and 1‰ DMSO+d-GalN/LPS groups were higher (P < 0.01). After treatment of d-GalN/LPS-stimulated hepatocytes with 2.5–20 μM apigenin, the both indices were dose-dependently decreased (P < 0.05 or P < 0.01), indicating a protective effect of apigenin on hepatocellular injury induced by d-GalN/LPS.
Apigenin decreases the supernatant MDA level and increases the nucleus Nrf-2 protein expression and supernatant SOD and CAT levels
As shown in Fig. 2, the supernatant MDA content and nucleus Nrf-2 protein expression were significantly higher, while the supernatant SOD and CAT contents were significantly lower in the d-GalN/LPS or 1‰ DMSO+d-GalN/LPS groups than in the control group (P < 0.05 or P < 0.01). In the apigenin-treated groups, the supernatant MDA content was lowered, the nucleus Nrf-2 protein expression and supernatant SOD and CAT contents were augmented (P < 0.05 or P < 0.01).
Hepatocellular nucleus Nrf-2 protein expression and cultured supernatant CAT, SOD, and MDA levels after pretreatment of D-GalN/LPS-stimulated rat BRL cells with apigenin for 2 h. Each value represents the mean ± SD, with n = 3 per group. #P < 0.05, ##P < 0.01 versus the control group; *P < 0.05, **P < 0.01 versus the 1‰ DMSO+D-GalN/LPS group
Apigenin increases the PPARγ and IκB-α protein expressions and decreases the NF-κB p65 protein expression and supernatant TNF-α levels
The results are shown in Fig. 3. In the d-GalN/LPS or 1‰ DMSO+d-GalN/LPS groups, the intracellular PPARγ and IκB-α protein expressions were significantly lower, whereas the intracellular NF-κB p65 protein expression and supernatant TNF-α content were significantly higher compared with the control group (P < 0.01). After treatment with apigenin, the expressions of intracellular PPARγ and IκB-α proteins were increased, while that of intracellular NF-κB p65 protein was decreased (P < 0.05 or P < 0.01). Also, apigenin treatment could decrease the supernatant TNF-α content (P < 0.05 or P < 0.01).
Hepatocellular PPARγ, NF-κB p65, and IκB-α protein expressions and cultured supernatant TNF-α level after pretreatment of D-GalN/LPS-stimulated rat BRL cells with apigenin for 2 h. Each value represents the mean ± SD, with n = 3 per group. ##P < 0.01 versus the control group; *P < 0.05, **P < 0.01 versus the 1‰ DMSO+D-GalN/LPS group
BML-111 completely reverses the protective effect of apigenin on hepatocellular injury
The results showed that the nucleus Nrf-2 protein expression was higher in the apigenin+d-GalN/LPS group than in the 1‰ DMSO+d-GalN/LPS group (Fig. 4a, P < 0.01). After pretreatment with 200 nM BML-111, the nucleus Nrf-2 protein expression in the apigenin+BML-111+d-GalN/LPS group was significantly decreased as compared with the apigenin+d-GalN/LPS group (Fig. 4a, P < 0.01), indicating that apigenin-induced nucleus Nrf-2 protein expression was completely canceled. The supernatant SOD level also exhibited similar changes (Fig. 4b). Accordingly, the significant variations in the intracellular PPARγ and NF-κB p65 protein expressions as well as supernatant ALT and AST contents were observed between the apigenin+d-GalN/LPS group and the apigenin+BML-111+d-GalN/LPS group (Figs. 5 and 6). These results suggested that the protective effect of apigenin on hepatocellular injury was completely reversed by BML-111.
Hepatocellular nucleus Nrf-2 protein expression and cultured supernatant SOD level after pretreatment of D-GalN/LPS-stimulated rat BRL cells with apigenin for 2 h in the presence or absence of BML-111. Each value represents the mean ± SD, with n = 3 per group. ##P < 0.01 versus the control group; **P < 0.01 versus the 1‰ DMSO+D-GalN/LPS group; △△P < 0.01 versus the apigenin+D-GalN/LPS group
Hepatocellular PPARγ and NF-κB p65 protein expressions after pretreatment of D-GalN/LPS-stimulated rat BRL cells with apigenin for 2 h in the presence or absence of BML-111. Each value represents the mean ± SD, with n = 3 per group. ##P < 0.01 versus the control group; *P < 0.05, **P < 0.01 versus the 1‰ DMSO+D-GalN/LPS group; △P < 0.05, △△P < 0.01 versus the apigenin+D-GalN/LPS group
Supernatan ALT and AST levels after pretreatment of D-GalN/LPS-stimulated rat BRL cells with apigenin for 2 h in the presence or absence of BML-111. Each value represents the mean ± SD, with n = 3 per group. ##P < 0.01 versus the control group; *P < 0.05, **P < 0.01versus the 1‰ DMSO+D-GalN/LPS group; △P < 0.05, △△P < 0.01 versus the apigenin+D-GalN/LPS group
GW9662 partially reverses the protective effect of apigenin on hepatocellular injury
The results showed that after pretreatment of apigenin-treated and d-GalN/LPS-stimulated hepatocytes with GW9662 for 2 h, the effects of apigenin-induced intracellular PPARγ protein expression and apigenin-reduced intracellular NF-κB p65 protein expression were completely canceled (Fig. 7), but the reduced effects of apigenin on supernatant ALT, AST, and TNF-α contents were not completely canceled and only attenuated in some degree (Fig. 8). The three indices were not significantly different between the apigenin+d-GalN/LPS group and the apigenin+GW9662+d-GalN/LPS group (Fig. 8, P > 0.05).
Hepatocellular PPARγ and NF-κB p65 protein expressions after pretreatment of D-GalN/LPS-stimulated rat BRL cells with apigenin for 2 h in the presence or absence of GW9662. Each value represents the mean ± SD, with n = 3 per group. ##P < 0.01 versus the control group; **P < 0.01 versus the 1‰ DMSO+D-GalN/LPS group; △△P < 0.01 versus the apigenin+D-GalN/LPS group
Discussion
In the present study, the results, in accordance with our previous animal research reports (Zhou et al. 2017), showed that the supernatant ALT and AST levels were decreased after treatment of d-GalN/LPS-stimulated hepatocytes with 2.5–20 μM apigenin, which further support that apigenin may exert a beneficial protective effect on hepatocellular injury induced by d-GalN/LPS.
Oxidative stress plays a vital role in d-GalN/LPS-induced liver injury (Lekic et al. 2011), and the production of excess reactive oxygen species can cause the lipid peroxidation, which can be observed by detecting a stable terminal metabolite of lipid peroxidation MDA. Nrf-2, a main regulator of anti-oxidative genes, can increase the levels of anti-oxidative enzymes SOD and CAT (Kwak et al. 2004). The present results showed that apigenin treatment could increase the nucleus Nrf-2 protein expression and cultured supernatant SOD and CAT levels, decrease the cultured supernatant MDA level. These findings are consistent with the results of in vitro cultured ARPE-19 cells (Xu et al. 2016) and suggest that apigenin can protect again oxidative stress-mediated hepatocellular injury via the increments of nucleus Nrf-2 protein and subsequent anti-oxidative enzymes SOD and CAT levels.
To further verify whether the protective effect of apigenin was related to the increment of nucleus Nrf-2 protein, the BML-111, an inhibitor of Nrf-2 nucleus translocation (Guo et al. 2016), was used in this study. In the present study, we observed that after pretreatment with BML-111 for 2 h, the apigenin-increased nucleus Nrf-2 protein was completely canceled, and the protective effect of apigenin on d-GalN/LPS-induced hepatocellular injury was simultaneously canceled. Also, the similar results have been observed in the Nrf2 siRNA-treated ARPE-19 cells (Xu et al. 2016). Therefore, we believed that Nrf-2 is a target of apigenin action, that is, apigenin increases the nucleus translocation of Nrf-2. It has been reported that apigenin can restore the silenced status of Nrf2 in skin epidermal JB6 P+ cells by CpG demethylation coupled with attenuated activities of DNA methyltransferase and histone deacetylase (Paredes-Gonzalez et al. 2014). Moreover, our previous studies have shown that apigenin can increase the levels of anti-oxidative enzymes glutathione reductase and glutathione peroxidase in cultured hepatocytes stimulated with ethanol (Wang et al. 2018b). Base on these data, we deduced that apigenin-induced these anti-oxidative enzymes are attributable to the increment of Nrf-2 nucleus translocation. On the other hand, we simultaneously observed that apigenin-induced PPARγ protein expression was also canceled following pretreatment with BML-111, suggesting that the increment of PPARγ expression by apigenin results from the induction of Nrf-2.
Accumulating evidences have demonstrated that LPS can trigger the NF-κB activation to release inflammatory cytokines, such as TNF-α (Chen et al. 2017). NF-κB, a master transcription factor in regulating inflammatory response, can be activated by oxidative stress (Gloire and Piette 2009). IκB-α, an inhibitory protein of NF-κB, is combined with NF-κB for a cytoplasmic complex under normal conditions, while the free NF-κB can translocate to the nucleus to initiate the gene transcription of inflammatory cytokines under pathological conditions (Kanarek and Ben-Neriah 2012). PPARγ, an anti-inflammatory factor, can inhibit the generation of inflammatory cytokines through negative interference with NF-κB (Brun et al. 2013). Our present results showed that after treatment of d-GalN/LPS-stimulated hepatocytes with apigenin, the intracellular PPARγ and IκB-α protein expressions were increased, while the intracellular NF-κB p65 protein and cultured supernatant TNF-α level were decreased, suggesting that the protective effect of apigenin on hepatocytes may be, at least in part, due to the anti-inflammatory effect. To further understand the point of view, GW9662, an inhibitor of PPARγ (Collin et al. 2006), was used. The results showed that after pretreatment with GW9662, the apigenin-induced PPARγ protein expression was completely inhibited, but the protective effect of apigenin on hepatocellular injury was only attenuated, not completely canceled, indicating a decrease in the supernatant ALT, AST, and TNF-α levels yet. The results suggest that the Nrf-2-induced anti-oxidative enzymes still work after PPARγ inhibition.
In conclusion, our present results demonstrate that apigenin has a protective effect on d-GalN/LPS-induced hepatocellular injury, and its mechanisms may be related to the increment of Nrf-2 nucleus translocation, which may increase the anti-oxidative enzyme SOD and CAT levels and PPARγ protein expression, and subsequently inhibit the inflammatory cytokine TNF-α production. These findings may be helpful for understanding the exact hepatoprotective mechanisms of apigenin.
References
Brun P, Dean A, Di Marco V, Surajit P, Castagliuolo I, Carta D, Ferlin MG (2013) Peroxisome proliferator-activated receptor-gamma mediates the anti-inflammatory effect of 3-hydroxy-4-pyridinecarboxylic acid derivatives: synthesis and biological evaluation. Eur J Med Chem 62:486–497
Chen QL, Tang HL, Zha ZQ, Yin HP, Wang Y, Wang YF, Li HT, Yue L (2017) beta-D-glucan from Antrodia Camphorata ameliorates LPS-induced inflammation and ROS production in human hepatocytes. Int J Biol Macromol 104:768–777
Cho HY, Gladwell W, Wang X, Chorley B, Be D, Reddy SP, Kleeberger SR (2010) Nrf2-regulated PPARgamma expression is critical to protection against acute lung injury in mice. Am J Respir Crit Care Med 182:170–182
Collin M, Murch O, Thiemermann C (2006) Peroxisome proliferator-activated receptor-gamma antagonists GW9662 and T0070907 reduce the protective effects of lipopolysaccharide preconditioning against organ failure caused by endotoxemia. Crit Care Med 34:1131–1138
Duarte S, Arango D, Parihar A, Hamel P, Yasmeen R, Doseff AI (2013) Apigenin protects endothelial cells from lipopolysaccharide (LPS)-induced inflammation by decreasing caspase-3 activation and modulating mitochondrial function. Int J Mol Sci 14:17664–17679
Gloire G, Piette J (2009) Redox regulation of nuclear post-translational modifications during NF-kappaB activation. Antioxid Redox Signal 11:2209–2222
Guo S, Gong J, Yao SL (2016) Effects and mechanism of BML-111 on the hemorrhagic shock induced lung injury in rats. J Clin Emerg 17:442-446 (Chinese)
Han JY, Ahn SY, Kim CS, Yoo SK, Kim SK, Kim HC, Hong JT, Oh KW (2012) Protection of apigenin against kainate-induced excitotoxicity by anti-oxidative effects. Biol Pharm Bull 35:1440–1446
Jaeschke H (2000) Reactive oxygen and mechanisms of inflammatory liver injury. J Gastroenterol Hepatol 15:718–724
Jaiswal AK (2004) Nrf2 signaling in coordinated activation of antioxidant gene expression. Free Radic Biol Med 36:1199–1207
Kanarek N, Ben-Neriah Y (2012) Regulation of NF-kappaB by ubiquitination and degradation of the IkappaBs. Immunol Rev 246:77–94
Kwak MK, Wakabayashi N, Kensler TW (2004) Chemoprevention through the Keap1-Nrf2 signaling pathway by phase 2 enzyme inducers. Mutat Res 555:133–148
Lee WM (2012) Acute liver failure. Semin Respir Crit Care Med 33:36–45
Lekic N, Cerny D, Horinek A, Provaznik Z, Martinek J, Farghali H (2011) Differential oxidative stress responses to D-galactosamine-lipopolysaccharide hepatotoxicity based on real time PCR analysis of selected oxidant/antioxidant and apoptotic gene expressions in rat. Physiol Res 60:549–558
Moraes LA, Piqueras L, Bishop-Bailey D (2006) Peroxisome proliferator-activated receptors and inflammation. Pharmacol Ther 110:371–385
Mosedale M, Watkins PB (2017) Drug-induced liver injury: advances in mechanistic understanding that will inform risk management. Clin Pharmacol Ther 101:469–480
Oh IS, Park SH (2015) Immune-mediated liver injury in hepatitis B virus infection. Immune Netw 15:191–198
Paredes-Gonzalez X, Fuentes F, Su ZY, Kong ANT (2014) Apigenin reactivates Nrf2 anti-oxidative stress signaling in mouse skin epidermal JB6 P+ cells through epigenetics modifications. AAPS J 16:727–735
Stine JG, Chalasani NP (2017) Drug hepatotoxicity: environmental factors. Clin Liver Dis 21:103–113
Tsanova-Savova S, Ribarova F (2013) Flavonols and flavones in some Bulgarian plant foods. Pol J Food Nutr Sci 63:173–177
Vissiennon C, Hammoud D, Rodewald S, Fester K, Goos KH, Nieber K, Arnhold J (2017) Chamomile flower, myrrh, and coffee charcoal, components of a traditional herbal medicinal product, diminish proinflammatory activation in human macrophages. Planta Med 83:846–854
Wang F, Liu JC, Zhou RJ, Zhao X, Liu M, Ye H, Xie ML (2017) Apigenin protects against alcohol-induced liver injury in mice by regulating hepatic CYP2E1-mediated oxidative stress and PPARalpha-mediated lipogenic gene expression. Chem Biol Interact 275:171–177
Wang BY, Goldsmith CD, Zhao JH, Zhao SS, Sheng ZL, Yu WH (2018a) Optimization of ultrasound-assisted extraction of quercetin, luteolin, apigenin, pinocembrin and chrysin from Flos populi by Plackett-Burman design combined with taguchi method. Chiang Mai J Sci 45:427–439
Wang F, Zhou RJ, Zhao X, Ye H, Xie ML (2018b) Apigenin inhibits ethanol-induced oxidative stress and LPS-induced inflammatory cytokine production in cultured rat hepatocytes. J Appl Biomed 16:75–80
Xu XR, Li M, Chen WW, Yu HT, Yang Y, Hang L (2016) Apigenin attenuates oxidative injury in ARPE-19 cells thorough activation of Nrf2 pathway. Oxid Med Cell Longev 2016:4378461
Zhao X, Wang F, Zhou RJ, Zhu ZY, Xie ML (2018) PPARα/γ antagonists reverse the ameliorative effects of osthole on hepatic lipid metabolism and inflammatory response in steatohepatitic rats. Inflammopharmacol 26:425–433
Zhou RJ, Ye H, Wang F, Wang JL, Xie ML (2017) Apigenin inhibits D-galactosamine/LPS-induced liver injury through upregulation of hepatic Nrf-2 and PPARγ expressions in mice. Biochem Biophys Res Commun 493:625–630
Funding
This work was supported by the Priority Academic Program Development of the Jiangsu Higher Education Institutes (PAPD), China.
Author information
Authors and Affiliations
Contributions
ZRJ performed the cell culture and measurements of inflammatory cytokine TNF-α and protein expressions, and drafted the manuscript. ZY and FK performed the measurements of biochemistry indexes. ZY analyzed the data. XML designed the research and reviewed the whole manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhou, RJ., Zhao, Y., Fan, K. et al. Protective effect of apigenin on d-galactosamine/LPS-induced hepatocellular injury by increment of Nrf-2 nucleus translocation. Naunyn-Schmiedeberg's Arch Pharmacol 393, 929–936 (2020). https://doi.org/10.1007/s00210-019-01760-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-019-01760-w