Abstract
Vasoactive intestinal peptide (VIP) has been identified as one of major peptide transmitters in the central and peripheral nervous systems, being involved in a wide range of biological functions. The general physiologic effects of VIP include vasodilation, anti-inflammatory actions, cell proliferation, hormonal secretion, regulation of gastric motility, and smooth muscle relaxation; therefore, VIP has emerged as a promising drug candidate for the treatment of several diseases. A number of clinical applications of VIP or its derivatives have been developed; however, VIP-based drugs are not yet in clinical use, possibly because of mainly two serious problems: (1) poor metabolic stability and (2) poor penetration to the desired site of action. To overcome these shortcomings, the development of efficacious VIP analogues and several drug delivery systems has been attempted on the basis of numerous structure–activity relationships (SAR) studies and pharmacological experiments. Combination of the use of potent VIP analogues and an appropriate drug delivery system might be advantageous for the VIP-based therapy. We review in this paper SAR studies of VIP for the identification of potent therapeutic agents, describe the development of selective and/or metabolically stable VIP receptor agonists/antagonists, and discuss the potential application for clinical treatment using drug delivery systems.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vasoactive intestinal peptide (VIP), an octacosapeptide, was first isolated and characterized from porcine duodenum in the early 1970s by Said and Mutt (1970). Because of the high similarity of primary and secondary structures, VIP has been identified as a member of the glucagons–secretin family (Table 1), which includes pituitary adenylate cyclase-activating polypeptide (PACAP) 27 and 38 (Miyata et al. 1989; Miyata et al. 1990), glucagon (Unger et al. 1978), secretin (Jorpes 1968), glucagon-like peptide-1 (Mojsov et al. 1987), growth-hormone-releasing factor (GHRF)-(1–29) (Rivier et al. 1982) and helodermin (Hoshino et al. 1984). VIP is widely distributed in cholinergic presynaptic neurons of the central nervous system and peripheral peptidergic neurons innervating diverse tissues, such as the heart, lung, digestive and genitourinary tract, eye, skin, ovaries, and thyroid gland (Vaudry et al. 2000). It has been well identified that VIP acts as one of major peptide transmitters in the central and peripheral nervous systems, being involved in a wide range of biological functions in organisms (Abad et al. 2006), including metabolic processes, exocrine and endocrine secretions, cell differentiation, and relaxation of smooth muscle (Said 1991), secretion of regulatory hormones (Onoue et al. 2001a), and regulation of immune response (Delgado et al. 1999b). On the basis of its numerous biological actions, VIP has been considered a promising candidate for pharmaceutical agents for several diseases, including diabetes, asthma, impotence, and rheumatism (Pozo 2003; Gozes and Furman 2004; Abad et al. 2006).
A number of structure–activity relationship (SAR) studies of VIP were carried out with different techniques to identify the portions of peptides involved in interactions with VIP receptors (Stiuso et al. 2006). These SAR investigations enabled successful development of efficacious VIP-receptor agonists with high specificity and/or stability, clinical applications of which were also proposed. We will review various new developments of VIP derivatives in the context of previous findings, representing a glimpse of the increasing volume of literature. In addition, recent researches on a drug delivery system (DDS) for potential VIP-based therapy will also be discussed.
VIP/PACAP receptors
The effects of VIP are mediated through interaction with two receptor subclasses named VPAC1 and VPAC2 receptors, and the effects of PACAP are also mediated through interaction with the same receptors, as well as through a selective receptor named PAC1 (Table 2; Rawlings and Hezareh 1996). VIP/PACAP receptors are members of a large family of G protein-coupled receptors, often referred as the GPCR-B family, which includes the receptors of glucagons–secretin family peptides, calcitonin, and parathyroid hormone (Laburthe et al. 1996). These are widely distributed glycoproteins with a large hydrophilic extracellular domain followed by seven hydrophobic transmembrane helices (Vaudry et al. 2000). They share several specific properties, the most important of which is the presence of large N-terminal extracellular domains that contain ten highly conserved amino acids, including six cysteines, putative N-terminal leader sequences, and several potential N-glycosylation sites.
Several different splice variants of PAC1 receptor with different signaling properties were identified, which can be generated by alternative splicing of the exon encoding the third intracellular loop of the receptor. In contrast, no splice variants seem to exist for VPAC1 and 2 receptors. PACAP and VIP have approximately equal affinity for VPAC1 and VPAC2 receptors (which are 49% identical in amino acid sequence); however, PACAP has about 1,000 times higher binding activity than VIP toward PAC1 receptors. These VIP/PACAP receptors are encoded by different genes and expressed in different cell populations in both the central nervous system and peripheral tissues (Solano et al. 2001). PAC1 receptor is mainly localized in the central nervous system (CNS) and the anterior pituitary, whereas VPAC receptors are generally concentrated in peripheral tissues such as the intestine, adrenal gland, liver, and kidney (Shivers et al. 1991). Although the expression of PAC1 receptor messenger RNA (mRNA) in the CNS was found to be much higher than those of VPAC1 and VPAC2 receptor mRNA (Basille et al. 2000), the expression of VPAC2 receptor mRNA has been confirmed in brain tissues, including the hypothalamus and hippocampus (Hashimoto et al. 1993; Usdin et al. 1994). VPAC1 receptor mRNA has been found to be abundant in lung and T lymphocytes, and VPAC2 receptor is found predominantly in the smooth muscle layers and the basal part of the mucosal epithelium in the lung.
Signal transduction of VIP/PACAP receptors
VIP/PACAP receptors are preferentially coupled to Gαs proteins that stimulate adenylate cyclase activity. It has been shown that VIP induces the translocation and degradation of the α subunit of Gs protein (Yajima et al. 1998). PAC1 and VPAC1 receptors can stimulate, in addition, inositol triphosphate synthesis and calcium mobilization (Solano et al. 2001). Thus, VIP and PACAP exert their biological functions in the central and peripheral nervous systems via the stimulation of various protein kinases, including the phospholipase C/protein kinase C (PKC), the mitogen-activated protein (MAP) kinase, and the cGMP-dependent protein kinases pathways, as well as the adenylate cyclase/protein kinase A (PKA) pathway (Vaudry et al. 2000). There appears to be some differences in the activating signaling pathway among ligands, depending on which receptor has been activated. PAC1 receptor activation has been found to induce the above-mentioned signaling transduction mechanisms to various degrees (Filipsson et al. 2001). VPAC1 receptor seems to activate adenylate cyclase/PKA and phospholipase C/PKC signaling pathways, whereas ligand binding to VPAC2 receptor predominantly leads to stimulate adenylate cyclase/PKA. The main signal transduction pathway involved would depend on the cellular level of activation and/or differentiation, the predominant receptor subtype expressed, and the use of cell lines. By activation of these signaling pathways, VIP shows a variety of biological functions in many tissues (Said 1991; Delgado et al. 1999b; Onoue et al. 2001a; Abad et al. 2006; Onoue et al. 2007).
Conformational analyses of VIP and related peptides
The study on the SAR of VIP is very important to characterize its interaction with the receptors and to modulate its stability and affinity. Moreover, to support SAR investigations, several efforts have been made to identify the preferred conformation of VIP and related peptides with various techniques such as nuclear magnetic resonance (NMR; Goossens et al. 1996) and circular dichroism (CD) spectral analyses (Haghjoo et al. 1996; Onoue et al. 2004d), and computational evaluation (Filizola et al. 1997). In general, after initial CD studies, a standard strategy was followed using homonuclear 2D 1H NMR techniques [correlation spectroscopy (COSY), total correlation spectroscopy (TOCSY), and nuclear overhauser enhancement spectroscopy (NOESY)], under various solution conditions, to identify amino acid spin systems and give sequence-specific assignments (Wuthrich 1989). Secondary structure regions were initially deduced from the difference in Hα chemical shifts from their random coil values and qualitative nuclear overhauser effect (NOE) data. Detailed structures at the atomic level were then calculated from qualitative NOE data, which were used as distance restraints in molecular dynamics and energy minimization calculations (Wuthrich 1998). Structural information has been used to guide the design of new analogues and mimetic versions of VIP. As shown in Table 1, all glucagons–secretin family peptides are short linear peptides consisting of approximately 30 amino acid residues, and they show significant sequence homology and even a secondary structure, featuring random coil structures at the N terminus and long α-helical structures at the C terminus (Clore et al. 1988; Wray et al. 1993; Thornton and Gorenstein 1994; Blankenfeldt et al. 1996; Wray et al. 1998; Onoue et al. 2004b). Of all glucagons–secretin family peptides, PACAP27, a PAC1 receptor agonist, has the highest sequence homology, as much as 68%, with VIP, and helodermin, a VPAC2 receptor agonist, also exhibit high structural similarities with VIP. Previous structural analyses, including circular dichroism (CD), nuclear magnetic resonance (NMR) and theoretical calculations, suggest remarkable similarities in secondary structures among the glucagon/secretin peptide family (Onoue et al. 2004b). With respect to the secondary structure of VIP, numerous conformational studies, including spectral and computational analyses, have characterized that VIP possesses two segments of secondary structures: a random coil structure in the N-terminal region containing approximately ten amino acid residues between positions 1 and 9, and a long α-helical structure in the C-terminal region stretching from position 10 to its C terminus (Bodanszky et al. 1974; Robinson et al. 1982; Bodanszky and Bodanszky 1986). As VIP acts through the interaction with two subclasses of G protein-coupled receptors, VPAC1 and VPAC2, it would be necessary to provide an artificial hydrophobic environment that mimics the vicinity of the peptide/receptor interface when performing conformational studies on VIP. The solvent system of water/alcohol, including methanol and trifluoroethanol, or micelle has often been used as a membrane-mimetic medium (Park et al. 1998; Kobayashi et al. 2000), and α-helical content of VIP dissolved in the water/alcohol system seemed to be much higher than that in water, possibly because of the enhanced intramolecular hydrogen bonding or other interactions (Bodanszky et al. 1974). Thus, α-helical contents estimated by spectroscopic analyses were variable, depending on solvent systems such as pH and polarity; however, N-terminal random coil and C-terminal helical structures were maintained under any conditions tested.
Structure–activity relationships of VIP
In past years, several chemical modification studies were carried out with different techniques, and valuable SAR information about receptor-binding pharmacophore and the stabilization of VIP have been reported (Table 3). Most SAR studies on VIP aimed to produce simplified VIP analogs having high affinity and selectivity for one VIP receptor subtype and enough metabolic stability for the following reasons: (1) VIP has high affinity for both VPAC1 and VPAC2 receptor subtypes and, therefore, does not discriminate between the two VIP receptor subtypes; (2) VIP undergoes rapid degradation in vivo with a half-life of less than 1 min (Hassan et al. 1994). In practice, outcomes from these SAR studies were not limited to a theoretical basis, as a number of VIP receptor agonists or antagonists have been identified and proposed as drug candidates (Tables 3 and 4).
Some groups attempted to identify the backbone and side-chain conformational requirements for interaction at the VIP receptor and to elicit high biological potency. These studies were accomplished by characterizing the in vitro and in vivo pharmacological effects of (1) analogues truncated sequentially at the N and C termini (O’Donnell et al. 1991; Onoue et al. 2004b), (2) analogues systematically modified with single Ala substitutions (O’Donnell et al. 1991; Nicole et al. 2000; Igarashi et al. 2002; Igarashi et al. 2005), and (3) analogues modified with d-amino acid substitutions (Bolin et al. 1995; Fig. 1). Site-directed modification through single-point Ala substitutions is a useful way to determine the potential binding and biological pharmacophores of peptides and small proteins. Once identified, it should be possible to enhance the biological potency of a specific compound by increasing binding energy at these positions. In SAR studies using Ala scanning to identify the VIP pharmacophore for hVPACs, analogues with Ala replacements in positions Asp3, Phe6, Thr7, Tyr10, Thr11, Tyr22, and Leu23 exhibited a significant loss in potency in the bioassay (O’Donnell et al. 1991). These results, taken together with previous findings about the crucial role of His1 (Bolin et al. 1989), the binding pharmacophore for VIP molecule was thought to be composed of three aromatic/hydrophobic moieties at residues 6, 10, and 22, a negatively charged site at residue 3, and a lone pair structure at residue 1. As shown in Fig. 1, functional analysis of the structure of VIP revealed that residues His1, Asp3, Phe6, Arg12, Arg14, and Leu23 interact with the VPAC1 receptor (Igarashi et al. 2002). Nicole et al. (2000) identified His1, Asp3, Val5, Phe6, Thr7, Asp8, Tyr10, Arg12, Arg14, Lys15, Lys20, Lys21, Leu23, and Ile26 as being important for binding to human VPAC1 receptor and subsequent stimulation of adenylate cyclase activity. In addition, Igarashi et al. (2005) also reported that a number of amino acids, particularly, Thr11, Tyr 22, Asn24, Leu27, and Asn28, were more important for VPAC2 than hVPAC1 affinity.
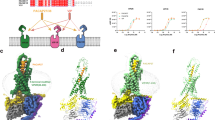
PACAP27 and VIP displayed similar binding activities toward VPAC1 and VPAC2, whereas the binding affinity of PACAP27 to PAC1 was much higher than that of VIP. To clarify the structural elements of VIP/PACAP for receptor selectivity, our group previously investigated the biological activities and structural/physicochemical properties of VIP/PACAP chimeric peptides (Onoue et al. 1999; Onoue et al. 2001b). Chemical modifications in the N-terminal random coil regions of both VIP and PACAP resulted in significant changes in their biological activities, including receptor-binding activity (Fig. 2) and activation of adenylate cyclase. In CHO cells stably expressing PAC1 short-form receptor, biological activities of [G4, I5]-VIP increased significantly in comparison with VIP, whereas that of [A4, V5]-PACAP27 was decreasing compared with PACAP27. Chemical modification of VIP/PACAP27 in the N-terminal region showed no significant influence on the C-terminal helical structure as determined by CD spectral analyses. In contrast, a high degree of similarity between N-terminal structures of PACAP and [G4, I5]-VIP, and between those of VIP and [A4, V5]-PACAP was observed (Fig. 2), suggesting that replacement of positions 4 and 5 between PACAP27 and VIP induced mutual conformational conversion. The results demonstrated the crucial role of the N-terminal structure of VIP/PACAP, especially residues 4 and 5, for receptor selectivity. These findings were consistent with other reports about the structural biology of PACAP (Sakiyama et al. 1991; Inooka et al. 2001). When replacing the N-terminal region of VIP with that of PACAP, the chimeric peptide, PACAP-(1–15)–VIP-(16–28), showed PACAP-like activity instead of VIP-like activity (Sakiyama et al. 1991). According to Inooka’s work, the presence of Gly4 was indispensable for the formation of the stable type II’ β-turn, possibly maintaining relative orientation between the hydrophobic cluster and N-terminal residues 1–3. Thus, the local main chain conformation of Gly4 and Ile5 is important for PACAP-receptor binding, and the weak binding of VIP to the PACAP receptor could be partly attributed to an inability to form a stable β-turn at this position. In addition to SAR investigation of the N-terminal region of VIP/PACAP, our group demonstrated that the binding activities of C-terminally truncated VIP analogues against lysates from rat lungs that express VPAC receptors were reduced in accordance with the decrease in α-helical contents (Onoue et al. 2004b). Gourlet et al. (1996b) also clarified that the presence of the C-terminal end of VIP is important for its interaction with the VPAC1 receptor. Hence, we conclude that N-terminal regions forming random coil structures in both VIP and PACAP may play a crucial role in the selective recognition of VPAC or PAC1 receptors and that the formation of the α-helical structure in the C terminus of VIP is critical to its binding to VPAC receptors.
Solution structures of VIP/PACAP N-terminal analogues determined by NMR spectral analysis and molecular simulation. a VIP, b PACAP, c [G4, I5]–VIP, and d [A4, V5]–PACAP. The 50 structures sampled during the last 100 ps of molecular dynamics at 313 K were superimposed so as to minimize root-mean-square deviation values of the backbone atoms N, C, C′, O and NH. IC50 values, shown in parentheses, were established from inhibition curves of tracer binding of [125I]–PACAP27 for PAC1 receptor by increasing concentrations of unlabelled peptides
Whereas the pharmacological potency of a peptide itself may be of general importance, chemical and physical stability is also a critical factor in the drug design of peptide for overall therapeutic success. In particular, enzymatic digestion, induced by neutral endopeptidase on bronchial epithelial cells, as well as tryptase and chymase derived from mast cells, could be significant. The blood half-life of VIP was found to be less than 1 min in rats (Hassan et al. 1994) and approximately 1 min in humans (Domschke et al. 1978). Herein, the rapid degradation of VIP after systemic administration is part of the reason for the limitation of its clinical applications. Therefore, for the clinical application of VIP as a therapeutic agent, a metabolically stable analogue of VIP needs to be developed, and many SAR studies focusing on VIP stabilization have been carried out (Table 3). According to comprehensive researches on the enzymatic cleavage and metabolism of VIP, VIP was found to be easily hydrolyzed by several enzymes, including neutral endopeptidase, mast cell chymase, and mast cell tryptase, and two primary cleavage sites on the VIP molecule were identified as amide bonds between Ser at 25 and Ile at 26, and Thr at 7 and Asp at 8 (Bolin et al. 1992; Lilly et al. 1993). After the identification of major cleavage sites, this information was used to synthesize cyclic peptides that incorporated disulfide and lactam ring structures (Bolin et al. 1993; Bolin et al. 1995). With respect to the stabilization of VIP against enzymatic cleavage, our group previously performed chemical modification studies by using a lot of synthetic VIP analogues. Based on the data obtained, the replacement of Lys residue at positions 15, 20, and 21 by Arg in VIP resulted in a significant improvement in metabolic stability (Kashimoto et al. 1996a; Kashimoto et al. 1996b; Onoue et al. 2004d). In addition to proteolytic degradation, Met at 17 is easily oxidized followed by conformational changes and disruption of the helical structure, and a significant decrease of biological activities was observed after oxidation of Met17 (Onoue et al. 2004b). Therefore, chemical modifications at Met17 have been proposed to improve the stability of VIP by (1) replacement of Met by Leu (Kashimoto et al. 1996b; Onoue et al. 2004b) and (2) Gln16-diaminopropane derivative (Stiuso et al. 2006).
Development of potent VIP receptor agonists
VIP has been considered a pharmaceutical agent candidate for several diseases, and clinical interest in developing novel VIP receptor agonists has recently been highlighted. Because of diverse actions of VIP on various receptor subtypes, considerable effort has been made to design peptide analogues that are selective for receptor subtypes. Whereas directed approaches to substitute or alter specific amino acids have been attempted, Ala and D-amino acid scanning has resulted in the design of stable and highly selective novel analogues.
So far, mainly three types of VIP receptor agonists have been proposed, including VPAC1 agonists, VPAC2 agonist, and nonselective agonists (Table 4). First, as VPAC1 selective agonists, [A11, 22, 28]-VIP (Nicole et al. 2000), [K15, R16, L27]-VIP(1–7)/GRF(8–27) (Robberecht et al. 1998), [DA2, Aib8,18, A9,15,16,22,24–26, Gab27]-hGRF(1–27) (GRF-6) (Ito et al. 2001), [R16]-chicken Secretin (Robberecht et al. 1998), [Y9, Dip18]-VIP (Tams et al. 2000), and [A2,8,9,11,19,22,24,25,27,28]-VIP (Igarashi et al. 2005) were designed on the basis of many SAR studies, and they, especially [K15, R16, L27]-VIP(1–7)/GRF(8–27), exhibited specific and high affinity for human or rat VPAC1 receptor. Second, two classes of VPAC2 receptor selective agonists have been reported: (1) cyclic derivatives of VIP with several mutations and extended basic C terminus, such as acetyl-[E8, K12,27,28, Nle17, A19, D25, L26, G29,30, T31]-VIP(cyclo 21–25) (Ro 25–1553) (Bolin et al. 1995) and acetyl-[E8,Ome-Y10, K12,27,28, Nle17, A19, D25, L26]-VIP(cyclo 21–25) (Ro 25–1392) (Xia et al. 1997), and (2) linear analogues including [V17, A19, Q24, K27,29, R30, Y31]-VIP (BAY 55–9837) (Tsutsumi et al. 2002), acetyl-[E8, K12,27,28, R16, Nle17,21, A19, N25, L26, G29,30, T31]-VIP (PG 96–277) (Moreno et al. 2000), and long-acting PEGylated derivative, [Q9,24,28, V17, A19, K27,29, R30, Y31]-VIP-C-PEG(43 kDa) (Pan et al. 2007). They displayed high selectivity for VPAC2 over VPAC1 and PAC1 in receptor-binding and functional assays; in particular, Ro 25–1553 was found to be a potent VPAC2 receptor agonist because of its highest selectivity (IC50 VPAC1/IC50 VPAC2 ratio, 800) and affinity (IC50, 1.0 nM) toward VPAC2 receptor. Third, nonselective VIP receptor agonists, stearyl-[Nle17]-VIP (Gourlet et al. 1998), [R15, 20, 21, L17]-VIP-GRR (IK312532) (Onoue et al. 2004a), and [R15, 20, 21, L17]-VIP(1–23) (Onoue et al. 2004d) have been proposed, and they displayed attractive biological functions.
For VIP-based clinical treatments, several early studies, focusing on the improvement of stability, have been attempted to create potent drug candidates (Bolin et al. 1995; Xia et al. 1997). Chemical modification studies clarify the best multiple-substitution sites with potent cyclic peptide. Cyclic compounds, Ro25-1553 and Ro25-1392, consisting of 31 and 28 amino acids, respectively, are highly selective for VPAC2 receptor, and they exhibited exceptionally high potency, metabolic stability, and a long duration of action (Bolin et al. 1995; Xia et al. 1997). Our group previously reported that polycationic VIP derivative, [R15, 20, 21, L17]-VIP, displayed a significant improvement in metabolic stability as compared to VIP (Kashimoto et al. 1996a). [R15, 20, 21, L17]-VIP showed a more sustained relaxation of rat isolated bronchial smooth muscles in vitro compared with VIP. In addition, Ito and Tachibana (1991) reported that C-terminally extended VIP derivative exhibited higher biological activity than natural VIP in vitro and in vivo. These findings led us to the successful development of a VIP analogue, IK312532; [R15, 20, 21, L17]-VIP-GRR, as a long-acting bronchodilator (Onoue et al. 2004a). Interestingly, IK312532 showed much higher stability against enzymatic digestion and even higher biological activities (Onoue et al. 2004a; Ohmori et al. 2006). In addition to IK312532, further investigation, together with our previous findings on the minimal sequence of VIP for receptor binding, also resulted in the successful development of a novel shortened and stable VIP analogue, [R15, 20, 21, L17]-VIP(1–23) (Onoue et al. 2004d).
Potential clinical application of VIP and analogues
Recent progress in our knowledge of the biological functions and mechanisms of action of VIP opened a new field of therapeutic possibilities for the treatment of multiple pathologies (Gozes and Furman 2003). In practice, the use of VIP and its derivatives as therapeutic agents has been suggested for erectile and female sexual dysfunction (Dinsmore et al. 1999), skin pathologies (Granoth et al. 2000), primary pulmonary hypertension (Petkov et al. 2003), heart failure (Saetrum Opgaard et al. 2001), acute lung injury (Said and Dickman 2000), type 2 diabetes (Tsutsumi et al. 2002), gastrointestinal motility disorders (Biancani et al. 1988), and nervous system pathologies of various nature (Abad et al. 2006). In addition, VIP and analogues have been believed to be effective in various inflammatory diseases because VIP acts as an endogenous anti-inflammatory mediator by altering the balance of Th1/Th2 cells and pro-/anti-inflammatory cytokines (Pozo 2003). In this context, VIP and analogues have recently arisen as promising candidates for the treatment of inflammatory pathologies such as septic shock (Delgado et al. 1999a), rheumatoid arthritis (Delgado et al. 2001), Crohn’s disease (Abad et al. 2003), and multiple sclerosis (Kato et al. 2004).
PAC1 and VPAC2 are expressed in pancreatic islets, and both PACAP and VIP have been shown to increase insulin secretion from the pancreas (Filipsson et al. 1998). Although the effect of PACAP on insulin secretion is much higher than VIP in vitro, glucagon secretion in vivo is also stimulated in mice, dogs, and humans (Filipsson et al. 2001). Furthermore, the administration of PACAP to either mice or humans has been reported to increase plasma insulin levels without affecting plasma glucose levels. The functional role of PACAP in the control of glucose homeostasis is complex because it also plays a role in increasing glucagon and catecholamine secretion, leading to the increase of glucose output from the liver. The expression pattern of VPAC1 suggests that activation of this receptor contributes to an increase in hepatic glucose production. Therefore, VPAC2-selective agonist has been believed to be a potential candidate for diabetic drugs and would enhance pancreatic β cell insulin release without causing increased glucose production by the liver. In practice, BAY 55-9837 and its PEGylated derivatives, BAY(Q9Q28C32)PEG22 and 43, were engineered as VPAC2 selective agonists through several rounds of site-directed mutagenesis (Tsutsumi et al. 2002; Pan et al. 2007), and they could stimulate glucose-dependent insulin secretion in vivo and in vitro. In particular, PEGylated BAY 55-9837 would have higher potential and developability as diabetic drugs because they retain significant VAPC2 activity and selectivity, as well as prolonged in vivo activity as compared to BAY 55-9837 (Pan et al. 2007). In addition to the VPAC2-selective agonist, a number of GLP-1 receptor agonists also promote glucose-dependent insulin secretion and have demonstrated glucose-lowering activity in clinical studies (Riddle and Drucker 2006). However, nausea and vomiting are common side effects associated with the inhibition of gastrointestinal motility by GLP-1. It is possible that VPAC2-selective agonists induce similar undesirable side effects because of VPAC2 localization in the gastrointestinal tract. This aspect of VPAC2-selective agonists has not yet been examined and, therefore, needs further study.
VIP is abundantly present in the normal human lung (Paul and Said 1987) and VIP-immunoreactive nerves are present in the smooth muscle layer and glands of the airway, and within the walls of pulmonary and bronchial vessels. Interestingly, VIP deficiency in the respiratory system is considered to be a pathogenetic factor in pulmonary disease (Said 1989). Because of its bronchodilating and anti-inflammatory effects, VIP may be a promising agent to treat pulmonary disease, including asthma (Said 1991) and chronic obstructive pulmonary disease (COPD; Onoue et al. 2004c; Groneberg et al. 2006). Interestingly, PACAP and its derivatives also exhibited potent bronchodilation and anti-inflammatory effects via interaction with VPAC receptors (Sergejeva et al. 2004; Yoshihara et al. 2004). However, the clinical application of VIP might be limited, as VIP is susceptible to rapid chemical and biochemical digestion after systemic administration, resulting in low potency and short duration of action in clinical application (Takubo et al. 1991). Hence, many chemical modification studies have been attempted to develop potent VIP derivatives with sufficient chemical and biochemical stability. So far, various stabilized VIP analogues, including Ro 25-1392, Ro 25-1553, and IK312532, have the potential to ameliorate asthmatic symptoms (Bolin et al. 1995; Xia et al. 1997; Onoue et al. 2004a). Ro 25-1553 is 24 to 89 times more potent than VIP as a relaxant of the guinea pig trachea, and pulmonary responses evoked by histamine, leukotriene D4, platelet-activating factor, and acetylcholine are inhibited dose-dependently by intratracheally instilled Ro 25-1553 (O’Donnell et al. 1994). IK312532 exhibits longer-lasting bronchodilation and suppression of the antigen-evoked infiltration of granulocytes in the bronchiolar mucosa as compared to VIP, possibly because of higher stability against enzymatic digestion (Ohmori et al. 2004). IK312532 also acts as protective agent against cigarette smoke-induced apoptosis of rat alveolar cells through the activation of PKA and MAP kinase signaling pathways and deactivation of caspase-3, an apoptotic enzyme (Onoue et al. 2004a). Therefore, these analogues have been proposed as candidates of asthma and/or COPD drugs, being in preclinical and clinical stages.
In addition to the stability issue, there is a possible drawback that the systemic administration of VIP may cause moderate hypotension and/or other adverse effects, depending on the rate of infusion (Morice et al. 1983). It is, thus, also required to use an effective drug delivery system for specific delivery of VIP to the target tissue. The development of effective methods to use polypeptides to treat diseases is a significant challenge to the pharmaceutical industry. Serious problems associated with systemic treatment include: poor oral availability because of gastrointestinal peptidases, high intestinal and hepatic first pass metabolism, low stability in the blood, and poor penetration to the desired site of action. Against these challenging problems, the development of efficacious drug delivery systems for VIP has been attempted. Liposomal and PEG-phospholipid micellar formulation for intravenous use have been investigated and proposed to protect VIP from degradation (Suzuki et al. 1995; Ashok et al. 2004). The association of VIP with liposomes is believed to curtail enzyme-induced inactivation of VIP, and the association of VIP with sterically stabilized biocompatible liposome also circumvents peptide inactivation by catalytic VIP antibodies, leading to enhanced vasodilation (Rubinstein et al. 2001). To cross the BBB, several strategies, such as drug lipidization or conjugation to VIP in BBB-targeting molecules, have been proposed (Bickel et al. 1993; Dufes et al. 2004). Dufes and coworkers demonstrated that the administration of systemic glucose-bearing vesicles encapsulating VIP could deliver intact VIP to specific brain areas. Bickel and coworkers reported successful application of the drug transport vector avidin-OX26 for brain delivery of VIP, and systemic administration of a small dose of VIP resulted in an in vivo central nervous systemic pharmacologic effect. The intranasal route also offers a much simpler approach for brain drug delivery, as the olfactory receptor cells are in contact with both the nasal cavity and the CNS, the connection of which constitutes a direct pathway to the brain (Dufes et al. 2003). In practice, intact VIP could be delivered successfully to the brain using the intranasal route for administration, whereas no intact VIP was found either in the brain or blood by intravenous administration. For the treatment of asthma/COPD, our group previously suggested a dry powder inhalation system of IK312532, the use of which resulted in higher concentrations of the drug in the target organ, the lung, and minimized systemic adverse events (Ohmori et al. 2004; Onoue et al. 2007). Although VIP-based drugs have not yet been used for clinical purposes, these reported DDS, taken together with potent VIP derivatives, might provide efficacious medication in the clinical treatment of cardiovascular, CNS, and pulmonary diseases.
Concluding remarks
VIP receptors have been identified as promising drug targets for several diseases, and some VIP derivatives designed for clinical treatment of type II diabetes, asthma, and COPD are now in preclinical and clinical stages. So far, many SAR studies have been carried out to clarify the structural biology of VIP with several approaches, resulting in the production of many attractive agonists or antagonists of VIP receptors. Although therapy using developed VIP derivatives would offer potential benefits to patients, they are not yet in clinical use. For the clinical application of VIP, studies aimed at developing an appropriate delivery system of VIP will be a key direction of future research, and the combination use of potent VIP analogue and targeted DDS might provide novel insight into the therapeutic potential of VIP and its derivatives.
References
Abad C, Martinez C, Juarranz MG, Arranz A, Leceta J, Delgado M, Gomariz RP (2003) Therapeutic effects of vasoactive intestinal peptide in the trinitrobenzene sulfonic acid mice model of Crohn’s disease. Gastroenterology 124:961–971
Abad C, Gomariz RP, Waschek JA (2006) Neuropeptide mimetics and antagonists in the treatment of inflammatory disease: focus on VIP and PACAP. Curr Top Med Chem 6:151–163
Ashok B, Rubinstein I, Tsueshita T, Onyuksel H (2004) Effects of peptide molecular mass and PEG chain length on the vasoreactivity of VIP and PACAP(1–38) in pegylated phospholipid micelles. Peptides 25:1253–1258
Basille M, Vaudry D, Coulouarn Y, Jegou S, Lihrmann I, Fournier A, Vaudry H, Gonzalez B (2000) Comparative distribution of pituitary adenylate cyclase-activating polypeptide (PACAP) binding sites and PACAP receptor mRNAs in the rat brain during development. J Comp Neurol 425:495–509
Biancani P, Beinfeld MC, Coy DH, Hillemeier C, Walsh JH, Behar J (1988) Dysfunction of the gastrointestinal peptide in peristalsis and sphincter function. Ann N Y Acad Sci 527:545–567
Bickel U, Yoshikawa T, Landaw EM, Faull KF, Pardridge WM (1993) Pharmacologic effects in vivo in brain by vector-mediated peptide drug delivery. Proc Natl Acad Sci U S A 90:2618–2622
Blankenfeldt W, Nokihara K, Naruse S, Lessel U, Schomburg D, Wray V (1996) NMR spectroscopic evidence that helodermin, unlike other members of the secretin/VIP family of peptides, is substantially structured in water. Biochemistry 35:5955–5962
Bodanszky M, Bodanszky A (1986) Conformation of peptides of the secretin–VIP–glucagon family in solution. Peptides 7:43–48
Bodanszky M, Bodanszky A, Klausner YS, Said SI (1974) A preferred conformation in the vasoactive intestinal peptide (VIP). Molecular architecture of gastrointestinal hormones. Bioorg Chem 3:133–140
Bolin DR, Cottrell JM, O’Neill N, Garippa R, O’Donnell M (1989) N-terminal analogs of vasoactive intestinal peptide: Identification of a binding pharmacophore. In: Rivier JE, Marshall GR (eds) 11th American Peptide Symposium. ESCON Scientific, Leiden, The Netherlands, La Jolla, CA, pp 208–210
Bolin DR, Cottrell J, Michalewsky J, Garippa R, O’Neill N, Simko B, O’Donnell M (1992) Degradation of vasoactive intestinal peptide in bronchoalveolar lavage fluid. Biomed Res 13:25–30
Bolin DR, Cottrell J, Garippa R, O’Neill N, Simko B, O’Donnell M (1993) Structure-activity studies of vasoactive intestinal peptide (VIP): cyclic disulfide analogs. Int J Pept Protein Res 41:124–132
Bolin DR, Michalewsky J, Wasserman MA, O’Donnell M (1995) Design and development of a vasoactive intestinal peptide analog as a novel therapeutic for bronchial asthma. Biopolymers 37:57–66
Clore GM, Nilges M, Brunger A, Gronenborn AM (1988) Determination of the backbone conformation of secretin by restrained molecular dynamics on the basis of interproton distance data. Eur J Biochem 171:479–484
Delgado M, Martinez C, Pozo D, Calvo JR, Leceta J, Ganea D, Gomariz RP (1999a) Vasoactive intestinal peptide (VIP) and pituitary adenylate cyclase-activation polypeptide (PACAP) protect mice from lethal endotoxemia through the inhibition of TNF-alpha and IL-6. J Immunol 162:1200–1205
Delgado M, Munoz-Elias EJ, Gomariz RP, Ganea D (1999b) Vasoactive intestinal peptide and pituitary adenylate cyclase-activating polypeptide prevent inducible nitric oxide synthase transcription in macrophages by inhibiting NF-kappa B and IFN regulatory factor 1 activation. J Immunol 162:4685–4696
Delgado M, Abad C, Martinez C, Leceta J, Gomariz RP (2001) Vasoactive intestinal peptide prevents experimental arthritis by downregulating both autoimmune and inflammatory components of the disease. Nat Med 7:563–568
Dinsmore WW, Gingell C, Hackett G, Kell P, Savage D, Oakes R, Frentz GD (1999) Treating men with predominantly nonpsychogenic erectile dysfunction with intracavernosal vasoactive intestinal polypeptide and phentolamine mesylate in a novel auto-injector system: a multicentre double-blind placebo-controlled study. BJU Int 83:274–279
Domschke S, Domschke W, Bloom SR, Mitznegg P, Mitchell SJ, Lux G, Strunz U (1978) Vasoactive intestinal peptide in man: pharmacokinetics, metabolic and circulatory effects. Gut 19:1049–1053
Dufes C, Olivier JC, Gaillard F, Gaillard A, Couet W, Muller JM (2003) Brain delivery of vasoactive intestinal peptide (VIP) following nasal administration to rats. Int J Pharm 255:87–97
Dufes C, Gaillard F, Uchegbu IF, Schatzlein AG, Olivier JC, Muller JM (2004) Glucose-targeted niosomes deliver vasoactive intestinal peptide (VIP) to the brain. Int J Pharm 285:77–85
Filipsson K, Sundler F, Hannibal J, Ahren B (1998) PACAP and PACAP receptors in insulin producing tissues: localization and effects. Regul Pept 74:167–175
Filipsson K, Kvist-Reimer M, Ahren B (2001) The neuropeptide pituitary adenylate cyclase-activating polypeptide and islet function. Diabetes 50:1959–1969
Filizola M, Carteni-Farina M, Perez JJ (1997) Conformational study of vasoactive intestinal peptide by computational methods. J Pept Res 50:55–64
Goossens JF, Cotelle P, Chavatte P, Henichart JP (1996) NMR study of five N-terminal peptide fragments of the vasoactive intestinal peptide: crucial role of aromatic residues. Pept Res 9:322–326
Gourlet P, Vandermeers A, Vandermeers-Piret MC, De Neef P, Robberecht P (1996a) Addition of the (28–38) peptide sequence of PACAP to the VIP sequence modifies peptide selectivity and efficacy. Int J Pept Protein Res 48:391–396
Gourlet P, Vilardaga JP, De Neef P, Waelbroeck M, Vandermeers A, Robberecht P (1996b) The C-terminus ends of secretin and VIP interact with the N-terminal domains of their receptors. Peptides 17:825–829
Gourlet P, De Neef P, Cnudde J, Waelbroeck M, Robberecht P (1997a) In vitro properties of a high affinity selective antagonist of the VIP1 receptor. Peptides 18:1555–1560
Gourlet P, Vandermeers A, Vertongen P, Rathe J, De Neef P, Cnudde J, Waelbroeck M, Robberecht P (1997b) Development of high affinity selective VIP1 receptor agonists. Peptides 18:1539–1545
Gourlet P, Rathe J, De Neef P, Cnudde J, Vandermeers-Piret MC, Waelbroeck M, Robberecht P (1998) Interaction of lipophilic VIP derivatives with recombinant VIP1/PACAP and VIP2/PACAP receptors. Eur J Pharmacol 354:105–111
Gozes I, Furman S (2003) VIP and drug design. Curr Pharm Des 9:483–494
Gozes I, Furman S (2004) Clinical endocrinology and metabolism. Potential clinical applications of vasoactive intestinal peptide: a selected update. Best Pract Res Clin Endocrinol Metab 18:623–640
Gozes I, Meltzer E, Rubinrout S, Brenneman DE, Fridkin M (1989) Vasoactive intestinal peptide potentiates sexual behavior: inhibition by novel antagonist. Endocrinology 125:2945–2949
Gozes I, Perl O, Giladi E, Davidson A, Ashur-Fabian O, Rubinraut S, Fridkin M (1999) Mapping the active site in vasoactive intestinal peptide to a core of four amino acids: neuroprotective drug design. Proc Natl Acad Sci U S A 96:4143–4148
Granoth R, Fridkin M, Gozes I (2000) VIP and the potent analog, stearyl-Nle(17)-VIP, induce proliferation of keratinocytes. FEBS Lett 475:78–83
Groneberg DA, Rabe KF, Fischer A (2006) Novel concepts of neuropeptide-based drug therapy: vasoactive intestinal polypeptide and its receptors. Eur J Pharmacol 533:182–194
Haghjoo K, Cash PW, Farid RS, Komisaruk BR, Jordan F, Pochapsky SS (1996) Solution structure of vasoactive intestinal polypeptide (11–28)-NH2, a fragment with analgesic properties. Pept Res 9:327–331
Hashimoto H, Ishihara T, Shigemoto R, Mori K, Nagata S (1993) Molecular cloning and tissue distribution of a receptor for pituitary adenylate cyclase-activating polypeptide. Neuron 11:333–342
Hassan M, Refai E, Andersson M, Schnell PO, Jacobsson H (1994) In vivo dynamical distribution of 131I-VIP in the rat studied by gamma-camera. Nucl Med Biol 21:865–872
Hoshino M, Yanaihara C, Hong YM, Kishida S, Katsumaru Y, Vandermeers A, Vandermeers-Piret MC, Robberecht P, Christophe J, Yanaihara N (1984) Primary structure of helodermin, a VIP-secretin-like peptide isolated from Gila monster venom. FEBS Lett 178:233–239
Igarashi H, Ito T, Hou W, Mantey SA, Pradhan TK, Ulrich CD 2nd, Hocart SJ, Coy DH, Jensen RT (2002) Elucidation of vasoactive intestinal peptide pharmacophore for VPAC(1) receptors in human, rat, and guinea pig. J Pharmacol Exp Ther 301:37–50
Igarashi H, Ito T, Mantey SA, Pradhan TK, Hou W, Coy DH, Jensen RT (2005) Development of simplified vasoactive intestinal peptide analogs with receptor selectivity and stability for human vasoactive intestinal peptide/pituitary adenylate cyclase-activating polypeptide receptors. J Pharmacol Exp Ther 315:370–381
Inooka H, Ohtaki T, Kitahara O, Ikegami T, Endo S, Kitada C, Ogi K, Onda H, Fujino M, Shirakawa M (2001) Conformation of a peptide ligand bound to its G-protein coupled receptor. Nat Struct Biol 8:161–165
Ito O, Tachibana S (1991) Vasoactive intestinal polypeptide precursors have highly potent bronchodilatory activity. Peptides 12:131–137
Ito T, Igarashi H, Pradhan TK, Hou W, Mantey SA, Taylor JE, Murphy WA, Coy DH, Jensen RT (2001) GI side-effects of a possible therapeutic GRF analogue in monkeys are likely due to VIP receptor agonist activity. Peptides 22:1139–1151
Jorpes JE (1968) The isolation and chemistry of secretin and cholecystokinin. Gastroenterology 55:157–164
Kashimoto K, Nagano Y, Suitani Y, Hamanaka K, Mizumoto T, Tomizaki K, Takahata H, Nagamoto A, Ohata A, Yoshihara S, Ichimura T (1996a) Structure–activity relationship studies of PACAP-27 and VIP analogues. Ann N Y Acad Sci 805:505–510
Kashimoto K, Nagano Y, Suitani Y, Hamanaka K, Takahata H, Ohata A, Urauchi E, Watanabe S (1996b) The interaction studies of VIP and VIP analogue with glycosaminoglycan. In: Japanese Peptide Symposium, Tsukuba, Japan, pp 249–252
Kato H, Ito A, Kawanokuchi J, Jin S, Mizuno T, Ojika K, Ueda R, Suzumura A (2004) Pituitary adenylate cyclase-activating polypeptide (PACAP) ameliorates experimental autoimmune encephalomyelitis by suppressing the functions of antigen presenting cells. Mult Scler 10:651–659
Kobayashi S, Takeshima K, Park CB, Kim SC, Matsuzaki K (2000) Interactions of the novel antimicrobial peptide buforin 2 with lipid bilayers: proline as a translocation promoting factor. Biochemistry 39:8648–8654
Laburthe M, Couvineau A, Gaudin P, Maoret JJ, Rouyer-Fessard C, Nicole P (1996) Receptors for VIP, PACAP, secretin, GRF, glucagon, GLP-1, and other members of their new family of G protein-linked receptors: structure–function relationship with special reference to the human VIP-1 receptor. Ann N Y Acad Sci 805:94–109
Lilly CM, Drazen JM, Shore SA (1993) Peptidase modulation of airway effects of neuropeptides. Proc Soc Exp Biol Med 203:388–404
Miyata A, Arimura A, Dahl RR, Minamino N, Uehara A, Jiang L, Culler MD, Coy DH (1989) Isolation of a novel 38 residue-hypothalamic polypeptide which stimulates adenylate cyclase in pituitary cells. Biochem Biophys Res Commun 164:567–574
Miyata A, Jiang L, Dahl RD, Kitada C, Kubo K, Fujino M, Minamino N, Arimura A (1990) Isolation of a neuropeptide corresponding to the N-terminal 27 residues of the pituitary adenylate cyclase activating polypeptide with 38 residues (PACAP38). Biochem Biophys Res Commun 170:643–648
Mojsov S, Weir GC, Habener JF (1987) Insulinotropin: glucagon-like peptide I (7–37) co-encoded in the glucagon gene is a potent stimulator of insulin release in the perfused rat pancreas. J Clin Invest 79:616–619
Moreno D, Gourlet P, De Neef P, Cnudde J, Waelbroeck M, Robberecht P (2000) Development of selective agonists and antagonists for the human vasoactive intestinal polypeptide VPAC(2) receptor. Peptides 21:1543–1549
Morice A, Unwin RJ, Sever PS (1983) Vasoactive intestinal peptide causes bronchodilatation and protects against histamine-induced bronchoconstriction in asthmatic subjects. Lancet 2:1225–1227
Nicole P, Lins L, Rouyer-Fessard C, Drouot C, Fulcrand P, Thomas A, Couvineau A, Martinez J, Brasseur R, Laburthe M (2000) Identification of key residues for interaction of vasoactive intestinal peptide with human VPAC1 and VPAC2 receptors and development of a highly selective VPAC1 receptor agonist. Alanine scanning and molecular modeling of the peptide. J Biol Chem 275:24003–24012
O’Donnell M, Garippa RJ, O'Neill NC, Bolin DR, Cottrell JM (1991) Structure–activity studies of vasoactive intestinal polypeptide. J Biol Chem 266:6389–6392
O’Donnell M, Garippa RJ, Rinaldi N, Selig WM, Tocker JE, Tannu SA, Wasserman MA, Welton A, Bolin DR (1994) Ro 25-1553: a novel, long-acting vasoactive intestinal peptide agonist. Part II: Effect on in vitro and in vivo models of pulmonary anaphylaxis. J Pharmacol Exp Ther 270:1289–1294
Ohmori Y, Maruyama S, Kimura R, Onoue S, Matsumoto A, Endo K, Iwanaga T, Kashimoto K, Yamada S (2004) Pharmacological effects and lung-binding characteristics of a novel VIP analogue, [R15, 20, 21, L17]-VIP-GRR (IK312532). Regul Pept 123:201–207
Ohmori Y, Onoue S, Endo K, Matsumoto A, Uchida S, Yamada S (2006) Development of dry powder inhalation system of novel vasoactive intestinal peptide (VIP) analogue for pulmonary administration. Life Sci 79:138–143
Onoue S, Nagano Y, Tatsuno I, Uchida D, Kashimoto K (1999) Receptor-binding specificity depending on N-terminal structure of VIP/PACAP. Biomed Res 20:219–231
Onoue S, Waki Y, Hamanaka K, Takehiko Y, Kashimoto K (2001a) Vasoactive intestinal peptide regulates catecholamine secretion in rat PC12 cells through the pituitary adenylate cyclase activating polypeptide receptor. Biomed Res 22:77–82
Onoue S, Waki Y, Nagano Y, Satoh S, Kashimoto K (2001b) The neuromodulatory effects of VIP/PACAP on PC-12 cells are associated with their N-terminal structures. Peptides 22:867–872
Onoue S, Endo K, Ohmori Y, Yamada S, Kimura R, Yajima T, Kashimoto K (2004a) Long-acting analogue of vasoactive intestinal peptide, [R15, 20, 21, L17]-VIP-GRR (IK312532), protects rat alveolar L2 cells from the cytotoxicity of cigarette smoke. Regul Pept 123:193–199
Onoue S, Matsumoto A, Nagano Y, Ohshima K, Ohmori Y, Yamada S, Kimura R, Yajima T, Kashimoto K (2004b) Alpha-helical structure in the C-terminus of vasoactive intestinal peptide: functional and structural consequences. Eur J Pharmacol 485:307–316
Onoue S, Ohmori Y, Endo K, Yamada S, Kimura R, Yajima T (2004c) Vasoactive intestinal peptide and pituitary adenylate cyclase-activating polypeptide attenuate the cigarette smoke extract-induced apoptotic death of rat alveolar L2 cells. Eur J Biochem 271:1757–1767
Onoue S, Ohmori Y, Matsumoto A, Yamada S, Kimura R, Yajima T, Kashimoto K (2004d) Structure-activity relationship of synthetic truncated analogues of vasoactive intestinal peptide (VIP): an enhancement in the activity by a substitution with arginine. Life Sci 74:1465–1477
Onoue S, Yamada S, Yajima T (2007) Bioactive analogues and drug delivery systems of vasoactive intestinal peptide (VIP) for the treatment of asthma/COPD. Peptides 28(9):1640–1650
Pan CQ, Li F, Tom I, Wang W, Dumas M, Froland W, Yung SL, Li Y, Roczniak S, Claus TH, Wang YJ, Whelan JP (2007) Engineering novel VPAC2-selective agonists with improved stability and glucose-lowering activity in vivo. J Pharmacol Exp Ther 320:900–906
Pandol SJ, Dharmsathaphorn K, Schoeffield MS, Vale W, Rivier J (1986) Vasoactive intestinal peptide receptor antagonist [4Cl-D-Phe6, Leu17] VIP. Am J Physiol 250:G553–G557
Park IY, Park CB, Kim MS, Kim SC (1998) Parasin I, an antimicrobial peptide derived from histone H2A in the catfish, Parasilurus asotus. FEBS Lett 437:258–262
Paul S, Said SI (1987) Characterization of receptors for vasoactive intestinal peptide solubilized from the lung. J Biol Chem 262:158–162
Petkov V, Mosgoeller W, Ziesche R, Raderer M, Stiebellehner L, Vonbank K, Funk GC, Hamilton G, Novotny C, Burian B, Block LH (2003) Vasoactive intestinal peptide as a new drug for treatment of primary pulmonary hypertension. J Clin Invest 111:1339–1346
Pozo D (2003) VIP- and PACAP-mediated immunomodulation as prospective therapeutic tools. Trends Mol Med 9:211–217
Rawlings SR, Hezareh M (1996) Pituitary adenylate cyclase-activating polypeptide (PACAP) and PACAP/vasoactive intestinal polypeptide receptors: actions on the anterior pituitary gland. Endocr Rev 17:4–29
Riddle MC, Drucker DJ (2006) Emerging therapies mimicking the effects of amylin and glucagon-like peptide 1. Diabetes Care 29:435–449
Rivier J, Spiess J, Thorner M, Vale W (1982) Characterization of a growth hormone-releasing factor from a human pancreatic islet tumour. Nature 300:276–278
Robberecht P, De Neef P, Lefebvre RA (1998) Influence of selective VIP receptor agonists in the rat gastric fundus. Eur J Pharmacol 359:77–80
Robinson RM, Blakeney EW Jr., Mattice WL (1982) Lipid-induced conformational changes in glucagon, secretin, and vasoactive intestinal peptide. Biopolymers 21:1271–1228
Rubinstein I, Dagar S, Sethi V, Krishnadas A, Onyuksel H (2001) Liposomal VIP potentiates DNA synthesis in cultured oral keratinocytes. Peptides 22:671–675
Saetrum Opgaard O, Knutsson M, de Vries R, Tom B, Saxena PR, Edvinsson L (2001) Vasoactive intestinal peptide has a direct positive inotropic effect on isolated human myocardial trabeculae. Clin Sci (Lond) 101:637–643
Said SI (1989) Vasoactive intestinal polypeptide and asthma [editorial]. N Engl J Med 320:1271–1273
Said SI (1991) Vasoactive intestinal polypeptide (VIP) in asthma. Ann N Y Acad Sci 629:305–318
Said SI, Mutt V (1970) Polypeptide with broad biological activity: isolation from the small intestine. Science 169:1217–1218
Said SI, Dickman KG (2000) Pathways of inflammation and cell death in the lung: modulation by vasoactive intestinal peptide. Regul Pept 93:21–29
Sakiyama A, Kitada C, Watanabe T, Masuda Y, Fujino M (1991) Structure–activity relationship of pituitary adenylate cyclase activating polypeptide (PACAP). In: Suzuki A (ed) Japanese Peptide Symposium. Protein Research Foundation, Osaka, pp 215–220
Sergejeva S, Hoshino H, Yoshihara S, Kashimoto K, Lotvall J, Linden A (2004) A synthetic VIP peptide analogue inhibits neutrophil recruitment in rat airways in vivo. Regul Pept 117:149–154
Shivers BD, Gorcs TJ, Gottschall PE, Arimura A (1991) Two high affinity binding sites for pituitary adenylate cyclase-activating polypeptide have different tissue distributions. Endocrinology 128:3055–3065
Solano RM, Langer I, Perret J, Vertongen P, Juarranz MG, Robberecht P, Waelbroeck M (2001) Two basic residues of the h-VPAC1 receptor second transmembrane helix are essential for ligand binding and signal transduction. J Biol Chem 276:1084–1088
Stiuso P, Marabotti A, Facchiano A, Lepretti M, Dicitore A, Ferranti P, Carteni M (2006) Assessment of the conformational features of vasoactive intestinal peptide in solution by limited proteolysis experiments. Biopolymers 81:110–119
Suzuki H, Noda Y, Paul S, Gao XP, Rubinstein I (1995) Encapsulation of vasoactive intestinal peptide into liposomes: effects on vasodilation in vivo. Life Sci 57:1451–1457
Takubo T, Banks K, Martin JG (1991) Epithelium modulates the potency of vasoactive intestinal peptide in the guinea pig. J Appl Physiol 71:2146–2151
Tams JW, Jorgensen RM, Holm A, Fahrenkrug J (2000) Creation of a selective antagonist and agonist of the rat VPAC(1) receptor using a combinatorial approach with vasoactive intestinal peptide 6–23 as template. Mol Pharmacol 58:1035–1041
Taylor DP, Pert CB (1979) Vasoactive intestinal polypeptide: specific binding to rat brain membranes. Proc Natl Acad Sci U S A 76:660–664
Thornton K, Gorenstein DG (1994) Structure of glucagon-like peptide (7–36) amide in a dodecylphosphocholine micelle as determined by 2D NMR. Biochemistry 33:3532–3539
Tsutsumi M, Claus TH, Liang Y, Li Y, Yang L, Zhu J, Dela Cruz F, Peng X, Chen H, Yung SL, Hamren S, Livingston JN, Pan CQ (2002) A potent and highly selective VPAC2 agonist enhances glucose-induced insulin release and glucose disposal: a potential therapy for type 2 diabetes. Diabetes 51:1453–1460
Unger RH, Dobbs RE, Orci L (1978) Insulin, glucagon, and somatostatin secretion in the regulation of metabolism. Annu Rev Physiol 40:307–343
Usdin TB, Bonner TI, Mezey E (1994) Two receptors for vasoactive intestinal polypeptide with similar specificity and complementary distributions. Endocrinology 135:2662–2680
Vaudry D, Gonzalez BJ, Basille M, Yon L, Fournier A, Vaudry H (2000) Pituitary adenylate cyclase-activating polypeptide and its receptors: from structure to functions. Pharmacol Rev 52:269–324
Waelbroeck M, Robberecht P, Coy DH, Camus JC, De Neef P, Christophe J (1985) Interaction of growth hormone-releasing factor (GRF) and 14 GRF analogs with vasoactive intestinal peptide (VIP) receptors of rat pancreas. Discovery of (N-Ac-Tyr1,D-Phe2)-GRF(1–29)-NH2 as a VIP antagonist. Endocrinology 116:2643–2649
Wray V, Kakoschke C, Nokihara K, Naruse S (1993) Solution structure of pituitary adenylate cyclase activating polypeptide by nuclear magnetic resonance spectroscopy. Biochemistry 32:5832–5841
Wray V, Nokihara K, Naruse S (1998) Solution structure comparison of the VIP/PACAP family of peptides by NMR spectroscopy. Ann N Y Acad Sci 865:37–44
Wuthrich K (1989) Protein structure determination in solution by nuclear magnetic resonance spectroscopy. Science 243:45–50
Wuthrich K (1998) The second decade—into the third millenium. Nat Struct Biol 5(Suppl):492–495
Xia M, Sreedharan SP, Bolin DR, Gaufo GO, Goetzl EJ (1997) Novel cyclic peptide agonist of high potency and selectivity for the type II vasoactive intestinal peptide receptor. J Pharmacol Exp Ther 281:629–633
Yajima Y, Akita Y, Saito T, Kawashima S (1998) VIP induces the translocation and degradation of the alpha subunit of Gs protein in rat pituitary GH4C1 cells. J Biochem (Tokyo) 123:1024–1030
Yoshihara S, Yamada Y, Abe T, Kashimoto K, Linden A, Arisaka O (2004) Long-lasting smooth-muscle relaxation by a novel PACAP analogue in human bronchi. Regul Pept 123:161–165
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Onoue, S., Misaka, S. & Yamada, S. Structure-activity relationship of vasoactive intestinal peptide (VIP): potent agonists and potential clinical applications. Naunyn-Schmied Arch Pharmacol 377, 579–590 (2008). https://doi.org/10.1007/s00210-007-0232-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-007-0232-0