Abstract
Magnolol, an active component extracted from Magnolia officinalis, has various pharmacological effects, including potent antioxidant activity. In the present study, we investigated the effect of magnolol on apoptosis in rat vascular smooth muscle cells (VSMCs), using terminal-deoxynucleotidyl-transferase-mediated deoxyuridine triphosphate nick end labelling (TUNEL) and flow cytometric analysis. Magnolol (5–20 µM) concentration-dependently induced significant VSMC apoptosis, this effect being blocked by the caspase inhibitor benzyloxycarbonyl-Val-Ala-Asp-fluoromethylketone (z-VAD-fmk, 50 µM). To study the molecular mechanism, the mitochondrial death pathway was examined. Magnolol increased caspase-3 and caspase-9 activities significantly and reduced the mitochondrial potential (Δψm). The levels of B-cell leukaemia/lymphoma-2 (Bcl-2), but not those of Bcl-2-associated X protein (Bax) or Bcl-xL, were down-regulated concentration dependently by magnolol. In an animal model, balloon angioplasty-induced neointima formation was inhibited significantly by magnolol and Bcl-2 protein levels were reduced. Taken together, these results show that magnolol induces apoptosis in VSMCs via the mitochondrial death pathway. This effect is mediated through down-regulation of Bcl-2 protein levels, both in vivo and in vitro. Magnolol thus shows potential as a novel therapeutic agent for the treatment of atherosclerosis and re-stenosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The increased potential for growth of vascular smooth muscle cells (VSMCs) is a key abnormality in the development of atherosclerosis and re-stenosis (Hanke et al. 1990; Pickering et al. 1993). Smooth muscle cells in normal vessels have a very low mitotic rate but start to proliferate and migrate when exposed to a variety of stimuli, including many growth factors (Deuel and Huang 1984). The proliferative potential can be regulated by various signals, e.g. signals blocking growth or inducing apoptosis (Libby et al. 1988).
Apoptosis (programmed cell death), which plays a critical role in both the normal development and pathology of a wide variety of tissues, is characterized by cytoplasmic shrinkage, nuclear condensation and DNA fragmentation (Jacobson et al. 1997; Nagata 1997). In recent years, the regulation of apoptosis has attracted much attention as a possible means of eliminating excessively proliferating cells (Mooberry et al. 1999; Kyprianou and Benning 2000). In particular, apoptotic death of vascular cells is a prominent feature of blood vessel remodelling, which occurs during normal development and fibroproliferative disorders of the vessel wall (Walsh and Isner 2000). Free radicals are thought to play an important role in apoptosis, and induction of apoptosis by reactive oxygen species (ROS) and ROS production by apoptotic cells have been described (Sandstrom et al. 1994; Zamzami et al. 1995; Li et al. 1997b). Antioxidants, however, also cause apoptosis in various cell types (Nobel et al. 1995; Chinery et al. 1997), including VSMCs (Tsai et al. 1996).
Magnolol, an active component purified from Magnolia officinalis, is a commonly used Chinese medicinal herb, and is reported to have various pharmacological activities, including anti-inflammatory (Wang et al. 1995) and antioxidant effects (Chiu et al. 1999) and inhibition of the expression of monocyte chemoattractant protein-1(MCP-1) (Chen et al. 2001) and vascular cell adhesion molecule (VCAM) (Chen et al. 2002). It can also induce apoptosis in cancer cells (Lin et al. 2001). The purpose of the present study was to evaluate the effect of magnolol on apoptosis in VSMC both in vitro and in vivo, and to study the molecular mechanism.
Materials and methods
Materials
Magnolol was synthesized by Professor A.-R. Lee (Department of Pharmacy, National Defence Medical Centre, Taiwan). Leupeptin, phenylmethylsulphonyl fluoride, SDS and anti-β-actin antibody were purchased from Sigma-Aldrich (St. Louis, Mo., USA). Protein assay reagents were purchased from Bio-Rad (Hercules, Calif., USA). DMEM, fetal bovine serum (FBS), penicillin, and streptomycin were from Life Technologies (Gaithersburg, Md., USA). The enhanced chemiluminescence kit was obtained from Amersham Pharmacia Biotech (Arlington Heights, Il., USA). Propidium iodide was from Molecular Probes (Port Gebouw, The Netherlands). 3,3′-Dihexyloxacarbocyanine iodide (DiOC6) was from Calbiochem (San Diego, CA, USA). Benzyloxycarbonyl-Val-Ala-Asp-fluoromethylketone (z-VAD-fmk) was from BioVision (Mountain View, Calif., USA). The colourimetric assay kits for caspase-3 and caspase-9 were from Clontech (Palo Alto, Calif., USA) and R and D Systems (Minneapolis, Minn., USA). The terminal deoxynucleotidyl transferase-mediated dUTP nick end-labelling (TUNEL) kit was from Roche (Mannheim, Germany). The rabbit anti-Bcl-associated X protein (Bax) antibodies were from Santa Cruz Biotechnology (Santa Cruz, Calif., USA), and the mouse anti-B-cell leukaemia/lymphoma-2 (Bcl-2) and anti-Bcl-XL antibodies and horseradish peroxidase-conjugated anti-mouse and anti-rabbit IgG antibodies were from Transduction Laboratories (Lexington, Ky., USA). All other chemicals were from Sigma.
Cell culture
Rat aortic VSMCs were harvested from male Sprague-Dawley rats (200–250 g) by enzymatic digestion as described previously (Pauly et al. 1997) and cultured in DMEM supplemented with 10% FBS, 100 U/ml penicillin and 100 µg/ml streptomycin. The cells were passaged every 5 days and used up to the eighth passage.
Flow cytometry analysis
VSMCs were incubated for 18 h in serum-free DMEM with various concentrations of magnolol, then trypsinized. The trypsinized cells were washed with PBS and stained in subdued light (30 min at 4 °C) with 0.1% Triton X-100 and 0.1% sodium citrate (pH 7.0) containing 50 µg/ml propidium iodide. The stained cells were then analysed using a FACS Calibur flow cytometer (Becton Dickinson, Calif., USA). The percentage of hypodiploid cells was taken as the percentage of cells showing DNA fragmentation.
The TUNEL assay for apoptosis
Apoptotic cells were detected by the TUNEL method using an in situ cell death-detection kit (Roche, Germany). In brief, VSMCs in serum-free DMEM were incubated for 18 h with various concentrations of magnolol, and fixed for 15 min in 4% paraformaldehyde in PBS. The cells were blocked for 15 min with 0.3% H2O2 in methanol, washed, permeabilized for 2 min with 0.1% sodium citrate in PBS then exposed sequentially to the enzymatic reaction mixture (TdT enzyme plus Labeling Safe Buffer) for 60 min at 37 °C, fluorescein-conjugated dUTP for 30 min at 37 °C and 0.05% diaminobenzidine in 1% nickel sulphate and 0.01% H2O2 and analysed using a FACS Calibur flow cytometer.
Caspase-3 and -9 activity assays
Caspase activity was measured using colourimetric assay kits for caspase-3 or caspase-9. Briefly, 2×106 cells were collected and resuspended for 10 min on ice in lysis buffer and the lysate centrifuged at 10,000 g for 5 min to precipitate cellular debris. The supernatant was reacted for 2 h at 37°C with 5 µl of Asp-Glu-Val-Asp-p-nitroanaline (DEVD-pNA) or Leu-Glu-His-Asp-p-nitroaniline (LEHD-pNA) (final concentration 50 µM), substrates for caspase-3 and -9, respectively, and the absorbance at 405 nm read in a microplate reader.
Assessment of mitochondrial potential (Δψm)
To assess the mitochondrial potential, a fluorescent, cationic, cell-permeable, voltage-sensitive, lipophilic carbocyanine dye, DiOC6, was used. Its fluorescence is a measure of mitochondrial membrane potential (Srivastava et al. 1997). VSMCs (5×105 cells/ml; 2 ml) were incubated for 18 h at 37 °C with various concentrations of magnolol. During the last 15 min of incubation, the cells were labelled with DiOC6 (40 nM) at 37 °C. After washing, cells were analysed by flow cytometry.
Western blot analysis
Cells or homogenized rat aortas were lysed by incubation for 30 min at 4 °C in lysis buffer: 1% SDS, 100 mM NaCl, 62.5 mM TRIS, pH 7.6, 1 mM phenylmethylsulphonyl fluoride and 10 µg/ml leupeptin. Insoluble material was removed by centrifugation for 30 min at 10,000 g at 4 °C and the protein concentration of the supernatant determined using the Bio-Rad protein assay system (http://library.ndmctsgh.edu.tw/cgi-bin/ovidweb/-49). A sample of the material (40 µg protein) was then subjected to SDS-PAGE on a 10% polyacrylamide gel and electroblotted onto a polyvinylidene difluoride (PVDF) membrane (Millipore, Bedford, Mass., USA). After blocking non-specific binding by incubation for 1 h at room temperature with 5% non-fat milk in 20 mM TRIS-HCl, 137 mM NaCl, pH 7.4, containing 0.1% Tween 20 (TTBS), the membrane was incubated for 1 h at room temperature with primary antibodies (1:1,000), washed 3 times with TTBS, incubated for 10 min at room temperature with horseradish peroxidase-conjugated anti-mouse or anti-rabbit IgG antibodies (1:2,000 dilution) and washed 3 times with TTBS. Bound antibody was visualized using an enhanced chemiluminescence detection kit and exposure to X-ray film and the bands quantified by densitometry.
In vivo balloon angioplasty
All procedures complied with the standards for care and use of animal subjects as stated in the Guide for the Care and Use of Laboratory Animals (Department of Laboratory Animal Science of the National Defence Medical Centre). The study was approved by the local Institutional Review Board according to the Helsinki recommendations and internationally accepted principles for the care and use of experimental animals. Male Sprague-Dawley rats (350–400 g) were anaesthetized with chloralhydrate (0.35 g/kg i.p.) and a 2F embolectomy balloon catheter (Baxter Health Care, Irvine, Calif., USA) introduced into the right common carotid artery via the external artery. The balloon was inflated with sufficient saline to distend the common carotid artery and was then withdrawn to the external artery. This procedure was repeated 3 times, the catheter removed and the distal external artery segment ligated. The animals were then randomly allocated to one of three groups: (1) the no-magnolol treatment group, (2) the low-dose magnolol treatment group (0.5 mg/kg/day for 2 weeks) or (3) the high-dose magnolol treatment group (2 mg/kg/day for 2 weeks). A mini-osmotic pump (model 2001; Alza, Palo Alto, Calif., USA) with a pump rate of 1 µl/h containing sufficient solution for 7 days (replaced after 7 days) was filled with magnolol in alcohol or vehicle and implanted subcutaneously at the back of the neck. Fourteen days after balloon angioplasty, the rats were anaesthetized and perfused with saline through the ascending aorta. The right common carotid artery was isolated, then either homogenized in a homogenizer (PRO 200, PRO Scientific, Monroe, Conn., USA) for Western blotting, or fixed overnight with 4% paraformaldehyde, frozen, cut into 20-µm sections, stained with haematoxylin and eosin, photographed through a microscope and the neointimal areas measured.
Statistical analysis
Values are expressed as means±SEM for n samples. Data were analysed using one-way ANOVA followed by Dunnett's test. P<0.05 was regarded as significant.
Results
Magnolol induces cell apoptosis in VSMCs
The TUNEL procedure stains nuclei containing nicked DNA, a characteristic of cells in apoptosis. Flow cytometry showed that magnolol increased the percentage of TUNEL-positive cells concentration dependently (Fig. 1). In addition, flow cytometry of propidium iodide-stained VSMCs showed that magnolol increased the sub-G0/G1 ratio (DNA fragmentation) concentration dependently (Fig. 2). The EC50 for magnolol-induced VSMC apoptosis was about 6 µM.
Magnolol induces apoptosis in vascular smooth muscle cells (VSMCs). VSMCs were treated for 18 h with magnolol (5–20 µM), fixed, stained with terminal-deoxynucleotidyl-transferase-mediated deoxyuridine triphosphate nick end labelling (TUNEL) reagents, analysed flow cytometrically or photographed by fluorescent microscopy (upper panel) and the percentage of TUNEL-positive cells calculated (lower panel). Means±SEM, n=6, *P<0.05 vs. untreated (0 µM)
Magnolol activates caspase-3 and -9
The caspase inhibitor, z-VAD-fmk (50 µM) completely blocked the DNA fragmentation induced by magnolol (5–20 µM), but only partially blocked that induced by 30 µM magnolol (Fig. 3). Colorimetric assays of caspase-3 and caspase-9 activity showed both to be increased concentration dependently by magnolol (Fig. 4a, b).
Magnolol-induced cell death is caspase dependent. VSMCs were incubated for 30 min with the caspase inhibitor benzyloxycarbonyl-Val-Ala-Asp-fluoromethylketone (z-VAD-fmk, 50 µM), and then treated with magnolol (5–30 µM) for 18 h. After fixing, staining with propidium iodide and flow cytometric analysis the percentage of hypodiploid cells calculated. Means±SEM, n=4, *P<0.05 vs. no magnolol
Magnolol activates caspase-3/caspase-9 and reduces the mitochondrial membrane potential (ΨΔm). VSMCs were incubated for 18 h with magnolol (5–20 µM) caspase-3 (a) and -9 (b) activity assayed colourimetrically. c The mitochondrial membrane potential was also assessed using 3,3′-dihexyloxacarbocyanine iodide (DiOC6). Left: representative fluorescent images; right: summary. Means±SEM, n=4, *P<0.05 vs. untreated
Magnolol reduces mitochondrial membrane potential (Δψm)
Dissipation of the mitochondrial potential is a characteristic of apoptosis. Staining VSMCs with DiOC6 showed that magnolol reduced the mitochondrial membrane potential concentration dependently (Fig. 4c).
Effects of magnolol on Bcl-2, Bcl-XL, and Bax protein expression
The Bcl family of mitochondrial-associated proteins plays an important role in cell apoptosis. Immunoblotting studies showed that magnolol treatment decreased the expression of Bcl-2 concentration dependently, while having no effect on Bcl-xL and Bax expression (Fig. 5).
Effect of magnolol on B-cell leukaemia/lymphoma-2 (Bcl-2), Bcl-xL and Bcl-2-assocaited X protein (Bax) expression in VSMCs. VSMCs were incubated for 18 h with or without magnolol (5–20 µM) and the expression of Bcl-2, Bcl-xL and Bax determined by Western blotting. a Representative blots. b–d Densitometric results for Bcl-2 (b), Bcl-XL (c) and Bax (d). Means±SEM, n=4. Equal loading in each lane was demonstrated by the amounts of β-actin. *P<0.05 vs. control
Beneficial effects of magnolol in animals with re-stenosis
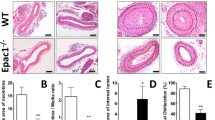
Two weeks after balloon angioplasty, vehicle-treated operated animals showed marked neointimal formation with extracellular matrix deposition (Fig. 6b) compared with sham-operated animals (Fig. 6a). In contrast, the injured right common carotid arteries in the low-dose magnolol (0.5 mg/kg per day) group showed significant suppression of neointimal formation (Fig. 6c), while those in the group treated with high-dose magnolol (2 mg/kg per day) were almost indistinguishable from controls (Fig. 6d). Bcl-2 protein expression in the carotid arteries was reduced concentration dependently by magnolol (Fig. 7), as in the in vitro studies.
Magnolol reduces angioplasty-induced neointima formation. a–d Haematoxylin and eosin-stained cross-sections of rat carotid arteries (×200). a Untreated control, no angioplasty, b balloon angioplasty, no magnolol, c balloon angioplasty, low-dose magnolol (0.5 mg/kg per day), d balloon angioplasty, high-dose magnolol (2 mg/kg per day. e Quantification of the neointimal area. Means±SEM, n=4, *P<0.05 vs. balloon angioplasty/no magnolol
Magnolol reduces Bcl-2 expression in vivo. After balloon angioplasty, the rats were treated with vehicle or magnolol (0–2 mg/kg per day) for 14 days. a Western blot analysis of Bcl-2 protein expression in the carotid arteries. Equal loading of each lane is shown by the amount of β-actin. b Densitometric results. Means±SEM, n=4, *P<0.05 vs. balloon angioplasty/no magnolol
Discussion
Atherosclerosis and post-angioplasty re-stenosis are characterized by the abnormal accumulation of VSMCs, inflammatory cells and extracellular matrix proteins (Hanke et al. 1990; Pickering et al. 1993). Neointimal thickening is mainly due to smooth muscle cells, which proliferate and migrate from the media. Excessive proliferative potential can be regulated by apoptosis (Perlman et al. 2000). Since our results demonstrated that magnolol induced apoptosis of VSMCs (Figs. 1 and 2), it is possible that magnolol could reduce the proliferative potential of VSMCs.
To clarify the involvement of caspases in magnolol-induced apoptosis in VSMCs, the effect of the caspase inhibitor z-VAD-fmk was examined. z-VAD-fmk blocked the cell death induced by 5–20 µM magnolol completely, indicating that the magnolol-induced cell death is caspase dependent (Fig. 3). The cell death induced by a higher concentration of magnolol (30 µM) was only partly blocked by z-VAD-fmk, suggesting that high concentrations may induce caspase-independent cell death or non-specific cytotoxicity. However, since the aim of this study was to examine apoptosis, these other possible effects of high-dose magnolol were not studied in detail.
Induction of apoptosis often involves activation of the caspase family of cysteine proteases. One principal mechanism of caspase activation requires the release of cytochrome c from mitochondria; this then associates with apoptotic protease activating factor-1 (Apaf-1) to form a complex termed the apoptosome (Li et al. 1997a), which recruits and activates caspase-9, which, in turn, activates other caspases, such as caspase-3 (Loeffler and Kroemer 2000). Colourimetric assays showed that magnolol increased both caspase-3 and caspase-9 activities (Fig. 4a, b), suggesting that caspase-3 and caspase-9 mediate magnolol-induced VSMC apoptosis.
Since the above results suggested the involvement of the mitochondrial death pathway in magnolol-induced VSMCs apoptosis, we examined the effect of magnolol on the mitochondrial membrane potential using DiOC6. Magnolol reduced the mitochondrial membrane potential concentration dependently (Fig. 4c), thus implying that magnolol-induced apoptosis results from activation of the mitochondrial death pathway, with subsequent activation of the downstream caspases 3 and 9.
The expression of the mitochondrion-associated proteins, Bcl-2, Bcl-XL, and Bax, was examined by Western blotting. Magnolol treatment of cells resulted in down-regulation of Bcl-2 expression, but had no effect on Bcl-XL and Bax levels. This suggests that the magnolol-induced apoptosis is mediated by down-regulation of Bcl-2 protein expression.
Interestingly, several studies have shown that antioxidants can rescue various types of cell from programmed cell death and magnolol is reported to have a high antioxidant potential (Chiu et al. 1999). However, in contrast, other antioxidants, pyrrolidinedithiocarbamate (Tsai et al. 1996, Erl et al. 2000), N-acetylcysteine (Tsai et al. 1996) and catalase (Brown et al. 1999), reportedly induce cell apoptosis in VSMCs, but the intracellular mechanism is not clear. Thus, the association between antioxidant activity and apoptosis is not clearly defined in VSMCs. It is possible that magnolol causes apoptosis by a mechanism independent of its antioxidant activity; however this requires further study.
Magnolol inhibits the expression of VCAM (Chen et al. 2002) and MCP-1 (Chen et al. 2001) and, as shown above, also induces cell apoptosis in VSMCs, effects which could be useful in the treatment of atherosclerosis and re-stenosis. We examined the in vivo therapeutic effect of magnolol in a balloon angioplasty model. Neointima formation was inhibited dose dependently by magnolol. Induction of VSMC apoptosis in vivo, either by forced over-expression of p53 (Yonemitsu et al. 1998) or down-regulation of Bcl-2 protein levels (Perlman et al. 2000), inhibits neointima formation. Other authors have shown that magnolol can reduce neointima formation (Chen et al. 2001) and concluded that the therapeutic effect is mediated by inhibition of MCP-1 expression. Our results showed that magnolol down-regulated Bcl-2 expression in vivo (Fig. 7). Although antioxidant activity or inhibition of MCP-1 or VACM expression may explain the reduction of neointima formation by magnolol, induction of apoptosis (or down-regulation of Bcl-2 expression) may also play an important role in prevention of intimal thickening. However, the detailed mechanism by which magnolol down-regulates Bcl-2 requires further study.
In summary, we have shown that magnolol induces cell apoptosis in rat aortic smooth muscle cells. The apoptotic effect of magnolol on VSMCs may be due to down-regulation of Bcl-2 protein expression. In addition, magnolol had a therapeutic effect in animals in which a balloon angioplasty had been established, suggesting its potential as a therapeutic agent for the treatment of atherosclerosis or re-stenosis.
References
Brown MR, Miller FJ Jr, Li WG, Ellingson AN, Mozena JD, Chatterjee P, Engelhardt JF, Zwacka RM, Oberley LW, Fang X, Spector AA, Weintraub NL (1999) Overexpression of human catalase inhibits proliferation and promotes apoptosis in vascular smooth muscle cells. Circ Res 85:524–533
Chen YL, Lin KF, Shiao MS, Chen YT, Hong CY, Lin SJ (2001) Magnolol, a potent antioxidant from Magnolia officinalis, attenuates intimal thickening and MCP-1 expression after balloon injury of the aorta in cholesterol-fed rabbit. Basic Res Cardiol 96:353–363
Chen YH, Lin SJ, Chen JW, Ku HH, Chen YL (2002) Magnolol attenuates VCAM-1 expression in vitro in TNF-α-treated human aortic endothelial cells and in vivo in the aorta of cholesterol-fed rabbits. Br J Pharmacol 135:37–47
Chinery R, Brockman JA, Peeler MO, Shyr Y, Beauchamp RD, Coffey RJ (1997) Antioxidants enhance the cytotoxicity of chemotherapeutic agents in colorectal cancer: a p53-independent induction of p21 WAF1/CIP1 via C/EBPβ. Nat Med 3:1233–1241
Chiu JH, Wang JC, Lui WY, Wu CW, Hong CY (1999) Effect of magnolol on in vitro mitochondrial lipid peroxidation and isolated cold-preserved warm-reperfused rat livers. J Surg Res 82:11–16
Deuel TF, Huang JS (1984) Platelet-derived growth factor: structure, function and roles in normal and transformed cells. J Clin Invest 74:669–676
Erl W, Weber C, Hansson GK (2000) Pyrrolidine dithiocarbamate-induced apoptosis depends on cell type, density, and the presence of Cu++ and Zn++. Am J Physiol 278:C1116–C1125
Hanke H, Strohschneider T, Oberhoff M, Betz E, Karsch KR (1990) Time course of smooth muscle cell proliferation in the intima and media of arteries following experimental angioplasty. Circ Res 67:651–659
Jacobson MD, Weil M, Raff MC (1997) Programmed cell death in animal development. Cell 88:85–89
Kyprianou N, Benning CM (2000) Suppression of human prostate cancer cell growth by alpha1-adrenoceptor antagonists doxazosin and terazosin via induction of apoptosis. Cancer Res 60:4550–4555
Li P, Nijhawan D, Budihardjo I, Srinivasula SM, Ahmad M, Alnemri ES, Wang X (1997a) Cytochrome c and dATP-dependent formation of Apaf-1/caspase-9 complex initiates an apoptotic protease cascade. Cell 91:479–489
Li PF, Dietz R, Von Harsdorf R (1997b) Differential effect of hydrogen peroxide and superoxide anion on apoptosis and proliferation of vascular smooth muscle cells. Circulation 96:3602–3609
Libby P, Warner SJC, Friedman GB (1988) Interleukin 1: a mitogen for human vascular smooth muscle cells that induces the release of growth-inhibitory prostanoids. J Clin Invest 81:487–498
Lin SY, Liu JD, Chang HC, Yeh SD, Lin CH, Lee WS (2001) Magnolol suppresses proliferation of cultured human colon and liver cancer cells by inhibiting DNA synthesis and activating apoptosis. J Cell Biochem 84:532–544
Loeffler M, Kroemer G (2000) The mitochondrion in cell death control: certainties and incognita. Exp Cell Res 256:19–26
Mooberry S, Tien G, Hernandez AH, Plubrukarn A, Davidson BS (1999) Laulimalide and isolaulimalide, new paclitaxel-like microtubule-stabilizing agents. Cancer Res 59:653–660
Nagata S (1997) Apoptosis by death factor. Cell 88:355–365
Nobel CI, Kinland M, Lind B, Orrenius S, Slater AF (1995) Dithiocarbamates induce apoptosis in thymocytes by raising the intracellular level of redox-active copper. J Biol Chem 270:26202–26208
Pauly RR, Bilato C, Cheng L, Monticone R, Crow MT (1997) Vascular smooth muscle cell cultures. Methods Cell Biol 52:133–152
Perlman H, Sata M, Krasinski K, Dorai T, Buttyan R, Walsh K (2000) Adenovirus-encoded hammerhead ribozyme to Bcl-2 inhibits neointimal hyperplasia and induces smooth muscle cell apoptosis. Cardiovasc Res 45:570–578
Pickering JG, Weir L, Jekanowski J, Kearney MA, Isner JM (1993) Proliferative activity in peripheral and coronary atherosclerotic plaque among patients undergoing percutaneous revascularisation. J Clin Invest 91:1469–1480
Sandstrom PA, Mannie MD, Buttke TM (1994) Inhibition of activation-induced death in T cell hybridomas by thiol antioxidants: oxidative stress as a mediator of apoptosis. J Leukoc Biol 55:221–226
Srivastava IK, Rottenberg H, Vaidya AB (1997) Atovaquone, a broad spectrum antiparasitic drug, collapses mitochondrial membrane potential in a malarial parasite. J Biol Chem 272:3967–3962
Tsai JC, Jain M, Hsieh CM, Lee WS, Yoshizumi M, Patterson C, Perrella MA, Cooke C, Wang H, Haber E, Schlegel R, Lee ME (1996) Induction of apoptosis by pyrrolidinedithiocarbamate and N-acetylcysteine in vascular smooth muscle cells. J Biol Chem 271:3667–3670
Walsh K, Isner JM (2000) Apoptosis in inflammatory-fibroproliferative disorders of the vessel wall. Cardiovasc Res 45:756–765
Wang JP, Ho TF, Chang LC, Chen CC (1995) Anti-inflammatory effect of magnolol, isolated from Magnolia officinalis, on A23187-induced pleurisy in mice. J Pharm Pharmacol 47:857–860
Yonemitsu Y, Kaneda Y, Tanaka S, Nakashima Y, Komori K, Sugimachi K, Sueishi K (1998) Transfer of wild-type p53 gene effectively inhibits vascular smooth muscle cell proliferation in vitro and in vivo. Circ Res 82:147–156
Zamzami N, Marchetti P, Castedo M, Decaudin D, Macho A, Hirsch T, Susin SA, Petit PX, Mignotte B, Kroemer G (1995) Sequential reduction of mitochondrial transmembrane potential and generation of reactive oxygen species in early programmed cell death. J Exp Med 182:367–377
Acknowledgements
We are grateful to Professor A-R Lee (Department of Pharmacy, National Defence Medical Centre, Taiwan) for providing synthetic magnolol. This study was supported by a grant from the Foundation of Biomedical Sciences and grant NSC90-2315-B-016-002 (to M-H. Y.) from the National Science council, Taipei, Taiwan, ROC.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, JH., Wu, CC., Hsiao, G. et al. Magnolol induces apoptosis in vascular smooth muscle. Naunyn-Schmiedeberg's Arch Pharmacol 368, 127–133 (2003). https://doi.org/10.1007/s00210-003-0779-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-003-0779-3