Abstract
The effects of a variety of fibrates on the cell viability were examined in human embryonal rhabdomyosarcoma cells (HRMSC). Five fibrates, including fenofibrate, clofibrate, gemfibrozil, bezafibrate and ciprofibrate, all concentration-dependently reduced the cell viability determined by the mitochondrial enzyme activity. The cell injury occurred time-dependently and was marked at 24–48 h. The toxic action of fibrates was specific to HRMSC, since bezafibrate did not induce any marked changes in the viability of human microvascular endothelial cells or arterial smooth muscle cells. Synergistic cell injury was observed after a combined treatment with bezafibrate and simvastatin, although simvastatin alone reduced the cell viability. The cell injury was characterized by a typical nuclear damage, as evidenced by Hoechst 33342 staining and deoxynucleotidyl transferase dUTP nick-end label-positive staining. Similar cell-specific injury was induced by 8(S)-hydroxyeicosatetraenoic acid, a potent peroxisome proliferator-activated receptor α (PPARα) agonist. Consistent with these data, a marked expression for PPARα mRNA was observed in HRMSC but not in the endothelial or smooth muscle cells. Therefore, it is suggested that fibrates cause a cell-specific injury in HRMSC via activation of PPARα. Moreover, our present cell injury model using HRMSC may be useful for elucidating the mechanisms of clinical rhabdomyolysis induced by lipid-lowering agents.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Fibrates are potent and effective lipid-lowering agents showing the reduction of blood triglyceride and low-density lipoprotein cholesterol levels and elevation of high-density lipoprotein cholesterol, thus, widely used for the prevention of ischemic vascular diseases (Gotto 1998; Robins 2001). However, the clinical use of these agents is sometimes limited because of the incidence of serious side effects such as rhabdomyolysis. Rhabdomyolysis exhibits clinical signs of diffuse myalgia, muscle tenderness, and the elevation of blood creatinine phosphokinase. Cardiac arrest and acute renal failure are the major complications of the severe symptoms of this disease (Poels and Gabreels 1993). However, little is known about the mechanisms underlying the fibrate-induced muscular disease. Moreover, there have been few in vitro models of fibrates-induced rhabdomyolysis using human skeletal muscle-derived cells.
On the other hand, similar type of muscular injury is also induced by other lipid-lowering agents such as statins that inhibit the activity of 3-hydroxy-3-methylglutaryl- coenzyme A (HMG-CoA) reductase (Moghadasian et al. 2000; Omar et al. 2001). It has also been demonstrated that statins cause an apoptosis in a variety of cells, including skeletal muscle cells (Veerkamp et al. 1996), smooth muscle cells (Guijarro et al. 1998), macrophage-like cell line J774 (Coxon et al. 1998), HL-60 (Perez-Sala and Mollinedo 1993), prostate stromal cells (Padayatty et al. 1997), leukemia cells (Dimitroulakos et al. 1999) and lens epithelial cells (Maddala et al. 2001). In the clinical setting, the incidence of rhabdomyolysis has been reported to be greatly enhanced when statins are treated in combination with fibrates (Guyton 1999).
It has been shown that lipid-lowering effect of fibrates is largely dependent on the stimulation of nuclear receptor peroxisome proliferator-activated receptor α (PPARα) (Staels et al. 1998). However, species differences exist in the number of PPARα and moreover the response of this receptor to various ligands varies between human and experimental animals (Gonzalez et al. 1998; Brown et al. 1999; Holden and Tugwood 1999).
Therefore, the present study was designed to establish an in vitro model of fibrates-induced rhabdomyolysis using human embryonal rhabdomyosarcoma cells (HRMSC). The effect of the combined treatment with fibrate and statin on the viability of HRMSC was also examined. Moreover, the possible mechanisms underlying the fibrate-induced cell injury in HRMSC were subsequently investigated.
Materials and methods
Chemicals.
The following chemicals and reagents were obtained from commercial sources: bezafibrate and clofibrate (ICN Biomedicals Inc., Aurora, OH, USA), fenofibrate, ciprofibrate, gemfibrozil, mevalonolactone and 8(S)-hydroxyeicosatetraenoic acid [8(S)-HETE] (Sigma Chemical Co., St. Louis, MO, USA), simvastatin (Calbiochem, La Jolla, CA, USA), fetal bovine serum (FBS: JRH Biosciences, Lenexa, KS, USA), Hoechst 33342 (Molecular Probes, Eugene, OR, USA). Other chemicals and reagents used in the present study were all of specific grade. Mevalonolactone was converted to mevalonate by dissolving in 10 mM phosphate buffer (pH 4.5) and stored at −20°C until use. Bezafibrate, fenofibrate and gemfibrozil were dissolved in dimethyl sulfoxide, while clofibrate and ciprofibrate were dissolved in ethanol. The final concentration of the vehicle was 0.1 or 0.4% (v/v) for dimethyl sulfoxide, and 0.1% (v/v) for ethanol.
Cell culture.
Human embryonal rhabdomyosarcoma cells (HRMSC) and human dermal microvascular endothelial cells (HMVEC) were obtained from American Type Culture Collection and BioWhittaker Inc. (Walkersville, MD, USA), respectively. Human umbilical artery smooth muscle cells (HUASMC) were isolated from the media of human umbilical arteries by explant. Cells were grown on 75 cm2 tissue culture flasks (Corning Costar, Corning, NY, USA) at 37°C in an air supplemented with 5% CO2 under humidified condition. HRMSC were grown in Eagle's minimum essential medium containing twice amounts of amino acids and vitamins in Hanks' BSS (ICN Biomedicals Inc.) supplemented with 10% FBS under antibiotic-free condition. HMVEC were grown in endothelial cell growth medium (Clonetics, Walkersville, MD, USA) supplemented with 5% FBS. HUASMC were grown in Dulbecco's modified Eagle's medium containing 1 g glucose/L (Sigma Chemical Co.) supplemented with 20% FBS. The culture media were changed every 2 days, and the cells were detached after addition of 0.25% trypsin-ethylenediaminetetraacetic acid (trypsin/EDTA; Gibco BRL, Rockville, MD, USA) when they reached subconfluence.
Evaluation of cell viability by mitochondrial activity to reduce WST-8.
The cell viability was estimated from the mitochondrial activity in reducing WST-8 [2-(2-methoxy-4- nitrophenyl)-3-(4-nitrophenyl)-5-(2,4-disulfophenyl)-2H-tetrazolium, monosodium salt] (Cell Counting Kit-8, Dojindo, Kumamoto, Japan) to the water-soluble formazan. HRMSC (2×104 cells/cm2), HMVEC (1×104 cells/cm2) or HUASMC (1×104 cells/cm2) were seeded on 24-well plates (Falcon, Becton Dickinson Labware, Lincoln Park, NJ, USA) and incubated for 48 h. Cells were exposed to fibrates including bezafibrate, clofibrate, fenofibrate, ciprofibrate and gemfibrozil (10–1,000 μM) for 24–48 h. After washing twice with phosphate-buffered saline, the cells were incubated with 200 μl of serum-free medium containing 20 μl of WST-8 assay solution (5 mM) and incubated at 37°C in humidified air supplemented with 5% CO2 for 90 min in case of HRMSC and HUASMC, or for 60 min in case of HMVEC. The incubation medium was carefully taken and transferred to 96-well flat-bottom plastic plates (Corning Costar). The amount of the formazan dye formed was measured at O.D. of 450 nm wavelength using a microplate reader (Immuno-mini NJ-2300, Inter Med, Tokyo).
Evaluation of cell viability by lactate dehydrogenase assay
Human embryonal rhabdomyosarcoma cells (2×104 cells/cm2), HMVEC (1×104 cells/cm2) or HUASMC (1×104 cells/cm2) were seeded on 24-well plates and incubated for 48 h. Cells were then exposed to bezafibrate (10–800 μM) for 24 h. At the end of the reaction, the incubation medium was transferred to plastic tubes to detect the extracellular lactate dehydrogenase (LDH) activity, and the remaining cells were lysed with 1% Triton-X for 30 min to determine the total LDH activity. The LDH activity was measured by the use of LDH assay kit (Takara Biomedicals, Osaka). The cell injury was expressed as the percentage of the LDH activity released into the medium to the total activity.
Hoechst 33342 staining.
Human embryonal rhabdomyosarcoma cells (4×104 cells/cm2) were incubated with 500 μM bezafibrate for 24 h, then the cells were washed and detached with 0.25% trypsin/EDTA. The cell suspension was centrifuged and fixed in 1% glutaraldehyde for 2 h. After staining of the nuclei of HRMSC with 5 mg/ml Hoechst 33342, fluorescence images were detected by using a fluorescence microscope (Eclipse E600; Nikon, ×100 magnification) at the excitation wavelength of 465 nm and the emission wavelength of 495 nm.
Terminal deoxynucleotidyl transferase mediated dUTP nick end-labeling staining.
Cells were plated (2×104 cells/cm2) in poly-L-lysine-coated chamber slide glass (ASAHI TEHCNO GLASS Co., Tokyo, Japan) that had been washed and sterilized. Bezafibrate was added to the medium to the final concentration of 500 or 800 µM and cells were further incubated for 24 h. Then, the cells were washed with PBS and fixed for 15 min at room temperature with 4% (w/v) paraformaldehyde in PBS. Cells were permeabilized by incubating with 0.1% Triton X-100 and 0.1% sodium citrate. Terminal transferase-mediated labeling of the fragmented DNA with dUTP was carried out using in situ Cell Death Detection kit (Roche Applied Science, Tokyo), according to the manufacturer's instructions. The stained cells were visualized using a fluorescence microscope (×40 magnification).
Reverse-transcription polymerase chain reaction for PPARα mRNA.
Total cellular RNAs were extracted using Trizol reagent (Gibco BRL, Gaithersburg, MD, USA) from HRMSC, HMVEC and HUASMC. The reverse-transcription polymerase chain reaction (RT-PCR) was performed using Ready-To-Go RT-PCR Beads (Amersham Pharmacia Biotech, Uppsala, Sweden). Total cellular RNAs (1 μg) were used for the RT reaction and the products were amplified by PCR using PPARα primers (sense primer: 5'-GACGAATGCCAAGATCTGAGAAAGC-3'; antisense primer: 5'-CGTCTCCTTTGTAGTGCTGTCAGC-3') (fragment size: 948 bp), according to the method of Chinetti et al. (1998). Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) primers (sense primer: 5'-GGGAGCCAAAAGGGTCATCATC-3'; antisense primer: 5'-GAGTGGGTGTCGCTGTTGAAG-3') were used as the control (fragment size: 533 bp). The PCR products were visualized with ethidium bromide after 2% agarose gel electrophoresis.
Statistical analysis.
Data were shown as the mean ± S.E.M. Comparisons of data among multiple groups were performed by one-way analysis of variance, followed by Dunnett's test, or Student' t-test was used for comparison between the two groups (Stat View; Abacus Concepts, CA, USA). Statistical significance was defined as P<0.05.
Results
Comparative effects of various fibrates on the cell viability in human embryonal rhabdomyosarcoma cells
To determine whether fibrates have cytotoxic action on HRMSC, cells were treated with a variety of fibrates (10–1,000 μM) including bezafibrate, fenofibrate, clofibrate, gemfibrozil and ciprofibrate for 24 h, and the cell viability was assessed by the WST-8 assay. All of the fibrates tested produced a cytotoxic action in HRMSC in a concentration-dependent manner (Fig. 1).
Comparative effects of various fibrates on the viability of rhabdomyosarcoma cells (HRMSC). Cells were exposed to various concentrations of fibrates including A fenofibrate, B clofibrate, C gemfibrozil, D bezafibrate, and E ciprofibrate for 24 h, and the cell viability was determined by the WS-8 method. Each point represents the mean ± S.E.M. (n=3–4). For control (concentration = 0), cells were exposed to the vehicle (0.1% DMSO in case of bezafibrate and gemfibrozil, 0.4% DMSO in case of fenofibrate, or 0.1% ethanol in case of clofibrate and ciprofibrate)
Morphological changes and time-course of cytotoxic action of bezafibrate in HRMSC
The bezafibrate-induced cytotoxicity was time-dependent, which appeared at 24–48 h after exposure to 500 μM bezafibrate, as measured by the mitochondrial activity in reducing WST-8 to its formazan product (Fig. 2C). Marked changes in the morphology of HRMSC were observed after exposure to bezafibrate. The non-treated HRMSC was spindle-shaped (Fig. 2A), while the bezafibrate-treated cells showed a shrinkage and roundness (Fig. 2B).
A , B Representative photographs showing the morphology of HRMSC exposed to bezafibrate for 24 h and C the time course of the reduction in cell viability. Cells were exposed to 0.1% DMSO (A) or 500 μM bezafibrate for 24 h (B). Magnification ×40. In C, cells were exposed to 500 μM bezafibrate for 2–48 h, and the cell viability was determined by the WST-8 method. Each column represents the mean ± S.E.M. (n=7–8). For control group, cells were exposed to 0.1% DMSO in serum free medium. **P<0.01 as compared with the respective control group (Student's t-test)
Comparison of the cytotoxic effect of bezafibrate among HRMSC, human dermal microvascular endothelial cells (HMVEC) and human umbilical artery smooth muscle cells (HUASMC).
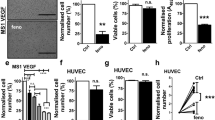
In HRMSC, bezafibrate (10–800 μM) caused a concentration-dependent reduction in the cell viability, as determined both by the WST-8 assay (Fig. 3A) or by the LDH leakage (Fig. 3B). To determine whether or not the cytotoxic action of bezafibrate is specific for HRMSC, the effect of this agent on the cell viability was examined in HMVEC and HUASMC. As shown in Fig. 3C–F, bezafibrate at concentrations up to 800 μM had no marked influence on the mitochondrial enzyme activity or the extracellular LDH leakage in HMVEC (Fig. 3C, D) or HUASMC (Fig. 3E, F). Therefore, it is likely that the fibrates-induced cell toxicity occurs specifically in HRMSC.
Comparative effects of bezafibrate on the cell viability among HRMSC, human dermal microvascular endothelial cells (HMVEC) cells and human umbilical arterial smooth muscle cells (HUASMC). Cells were exposed to 10–800 μM bezafibrate for 24 h, and the cell viability was determined by the WST-8 method (A, C, E) at 24 h and lactate dehydrogenase leakage (B, D, F) at 24 h. Each column represents the mean ± S.E.M. (n=9 in HRMSC, n=6 in HMVEC, n=4–6 in HUASMC). For control group, cells were exposed to 0.1% DMSO in serum free medium. **P<0.01 as compared with the respective control group (Dunnett's test)
Synergistic effect of simvastatin on bezafibrate-induced cell injury in HRMSC
In clinical setting, the incidence of rhabdomyolysis is enhanced when the fibrate is used in combination with statins (Guyton 1999). Therefore, we determined whether the fibrate-induced cell injury is augmented by a statin compound. As shown in Fig. 4, the toxic action of bezafibrate was enhanced by a sublethal concentration (3 μM) of simvastatin (Fig. 4B), although simvastatin alone significantly reduced the cell viability in HRMSC at high concentrations (10–30 μM) (Fig. 4A).
Concentration-dependent cell injury induced by A simvastatin and B synergistic effect of simvastatin on bezafibrate-induced reduction in cell viability in HRMSC. In B, cells were incubated with various concentrations of bezafibrate in the absence or presence of 3 μM simvastatin. The cell viability was determined by the WST-8 method. Each column represents the mean ± S.E.M. (n=4). For control group, cells were exposed to 0.1% DMSO in serum free medium. **P<0.01 (Dunnett's test), ††P<0.01 (Student's t-test)
Characteristics of the bezafibrate-induced cell injury in HRMSC
Nuclear staining with Hoechst 33342 or deoxynucleotidyl transferase dUTP nick-end labeling (TUNEL) staining was carried out in HRMSC after exposure to bezafibrate. Cells treated with 500 μM bezafibrate showed a chromatin condensation and small membrane-bound bodies, as assessed by Hoechst 33342 staining (Fig. 5A, B). In addition, TUNEL-positive cells were observed in bezafibrate-treated cells (Fig. 5D), while no positive cells were detected in non-treated HRMSC (Fig. 5C). Thus, it is likely that bezafibrate causes an apoptotic-like injury in HRMSC.
Representative photographs showing A, B nuclear fragmentation as stained with Hoechst 33342 and C, D TUNEL-positive HRMSC after exposure to bezafibrate. Cells were exposed to 500 μM bezafibrate for 24 h. The Hoechst 33342-stained nuclei were observed by a fluorescence microscopy. A, C control cells; B, D bezafibrate-treated cells. Magnification ×100 (A, B); ×40 (C, D)
Effect of mevalonate on the cell injury induced by simvastatin or bezafibrate in HRMSC
The simvastatin-induced cell injury was reversed by 25 μM mevalonic acid (Fig. 6). In contrast, the same concentration of mevalonic acid did not attenuate the cell injury induced by bezafibrate. Thus, it is unlikely that the inhibition in mevalonate cascade is involved in the fibrate-induced cell injury.
Reversal by mevalonic acid of simvastatin-induced but not bezafibrate-induced reduction in the cell viability in HRMSC. Cells were treated with 10 μM simvastatin or 500–800 μM bezafibrate for 24 h in the absence or presence of 25 μM mevalonic acid, and the viability was determined by WST-8 assay. Each column represents the mean ± S.E.M. (n=4)
Cell-specific toxic action induced by 8(S)-hydroxyeicosatetraenoic acid in HRMSC
The lipid-lowering action of fibrates is considered to be mediated by the activation of a nuclear receptor PPARα. Therefore, to determine whether the stimulation of PPARα induces a cell injury, the effect of 8(S)-hydroxyeicosatetraenoic acid (8(S)-HETE), an eicosanoid that stimulates PPARα (Yu et al. 1995; Muga et al. 2000), on the viability of HRMSC, HUASMC and HMVEC was investigated. As shown in Fig. 7, 8(S)-HETE (0.01–1 μM) produced a concentration-dependent injury in HRMSC (Fig. 7A), and the significant effect was observed at 1 μM, whereas 8(S)-HETE did not affect the viability of either HUASMC (Fig. 7B) or HMVEC (Fig. 7C).
Effect of 8(S)-hydroxyeicosatetraenoic acid [8(S)-HETE] on the cell viability in A HRMSC, B HUASMC and C HMVEC. Cells were exposed to 0.01–1 μM 8(S)-HETE for 24 h and the viability was determined by WST-8 assay. Each column represents the mean ± S.E.M. (n=4–6). **P<0.01 as compared with control group (Dunnett's test)
Expression for PPARα mRNA
To compare the expression for PPARα mRNA among HRMSC, HMVEC, and HUASMC, RT-PCR was carried out. As shown in Fig. 8, a highly amount of PPARα mRNA was observed in HRMSC, while only a small amount of the mRNA was detected in HMVEC. However, there was no detectable PPARα mRNA in HUASMC under the present experimental condition. On the other hand, there were no significant differences in the expression for GAPDH mRNA among these cells.
Discussion
The family of fibrates is in a widespread clinical use for lowering plasma triglyceride that is one of the risk factors of ischemic heart diseases (Gotto 1998). Among various fibrates, bezafibrate is most commonly prescribed for the prevention of coronary heart diseases in Japan because of the relative safety and effectiveness in lowering plasma triglyceride concentration while elevating that of high-density lipoprotein cholesterol (Goa et al. 1996). In spite of such beneficial effects, fibrates have been shown to cause a serious side effect, such as rhabdomyolysis, in various clinical practices (Sgro and Escousse 1991; Sharobeem et al. 2000). This myolytic syndrome is characterized by variable degree of striated muscular cramps and paralysis, and an excessive elevation of muscle-specific enzyme, such as CPK and LDH, in plasma. The incidence of rhabdomyolysis is enhanced, particularly when they are treated in combination with statins (Moghadasian 1999, 2000; Lau et al. 2001; Shek and Ferrill 2001). Rhabdomyolysis is also evoked as the adverse event of a variety of medicines or drugs such as alcohol, cocaine, diphenhydramine, haloperidol, propofol and vasopressin. To our knowledge, there have been few studies on the in vitro model of fibrates-induced rhabdomyolysis using human skeletal muscle-derived cells. In the present study, we determined whether a variety of fibrates alone cause a cell injury in HRMSC. Five different fibrates tested all produced a cell injury, as determined by the WST-8 method. This method is an improved assay of MTT method for the detection of cellular growth and survival. Like MTT, WST-8 is also reduced by mitochondrial reducing enzyme to the formazan compound which is highly water-soluble in contrast to MTT formazan. The cytotoxic action of fibrates was also confirmed by a marked LDH leakage observed at 24 h after exposure to bezafibrate, although the significant elevation of LDH leakage was observed only at the highest concentration of bezafibrate. A complete loss of mitochondrial enzymatic activity was observed by WST-8 assay at 24 h after exposure to 500 μM bezafibrate, thereby suggesting that the cells are functionally dead. However, the increase in the leakage of LDH, an intracellular marker, was less marked at 24 h. Therefore, it is suggested that the marked destruction of cell membranes appears later than 24 h after exposure to bezafibrate. It was noteworthy that the toxic action of fibrates was specific for HRMSC, since bezafibrate even at the highest concentration (800 μM) did not cause any influence on the cell viability in HUASMC or HMVEC. However, we cannot rule out the possibility that fibrates show the toxic actions preferentially to this transformed rhabdomyosarcoma cell line. The synergistic toxic action on HRMSC was observed after a combined treatment with bezafibrate (10–500 μM) and simvastatin (3 μM), although simvastatin alone reduced the cell viability at high concentrations (10–30 μM). Taken together, it is suggested that our present in vitro cell injury in HRMSC is a useful model of clinical rhabdomyolysis induced by fibrates, statins or their combination.
Although the precise mechanisms of fibrates-induced damage of HRMSC remain to be clarified, apoptotic processes may contribute at least in part to the cell injury. This idea was supported by the findings that bezafibrate caused nuclear damage including chromatin condensation as evidenced by Hoechst 33342 staining. Moreover, TUNEL-positive cells were observed in bezafibrate-treated but not intact HRMSC.
A similar myolytic adverse effect is observed in patients who took statins that inhibit the activity of HMG-CoA reductase, a rate-limiting enzyme in cholesterol biosynthesis. It has also been demonstrated that the statins induce apoptosis in a variety of cells, including skeletal muscle cells (Veerkamp et al. 1996) by reducing the intermediate products, such as geranylgeranyl pyrophosphate, in the cholesterol biosynthesis from HMG-CoA (Guijarro et al. 1998; Eberlein et al. 2001). The decrease in geranylgeranyl pyrophosphate causes a reduction in the isoprenylation of small G proteins such as Rho, which, in turn, causes an induction of p53 followed by Bax, leading to apoptosis (Tanaka et al. 2000). In the present study, simvastatin reduced concentration-dependently the viability of HRMSC, an action that was significantly reversed by mevalonic acid. However, mevalonic acid did not affect the bezafibrate-induced cell injury, thereby indicating a lack of involvement of mevalonate cascade in the fibrate-induced cell injury.
It has been demonstrated that most of the actions of fibrates, including the reduction of plasma triglyceride level and the increase in HDL cholesterol, are mediated by the activation of the nuclear receptor PPARα (Staels et al. 1998). Winegar et al. (2001) have reported the potencies of various fibrate compounds in stimulating PPARα by the reporter assay in CV-1 cells transfected with rhesus monkey PPAR-GAL4 chimeric receptors. According to their data, the rank order of potencies was fenofibrate (EC50=42.5 μM) >gemfibrozil (184 μM) >bezafibrate (220 μM). Interestingly, this order of potencies of these three fibrates was similar to that in reducing the cell injury in HRMSC observed in the present study. In addition, 8(S)-HETE, which is shown to stimulate PPARα (Forman et al. 1997), reduced the viability of HRMSC in a concentration-dependent manner, but had no, if any, influence on HUASMC or HMVEC. The RT-PCR showed that the expression of PPARα mRNA was marked in HRMSC, whereas only a weak and little expression for PPARα mRNA was observed in HMVEC and HUASMC, respectively. Taken together, it is possible that fibrates induce an apoptotic cell death in HRMSC via activation of PPARα.
The synergistic effect of a combined treatment with bezafibrate and simvastatin observed in the present study may also be explained by the enhancement of the bezafibrate-induced transcriptional activity on PPARα by simvastatin. Inoue et al. (2002) have demonstrated that statins synergistically interact with fibrates in the transcriptional activation of PPARα/RXRα in a manner dependent on the inhibition of mevalonate cascade, although statins alone have no direct action on this receptor complex. The statin-induced activation of PPARα is also reported by Martin et al. (2001) who showed in human HepG2 hepatoma cells that statins increase the PPARα activation-mediated expression of apoA-I mRNA through inhibition of isoprenylation of Rho GTPase.
On the other hand, Diep et al. (2000) have shown that the stimulation of PPARα by docosahexaenoic acid causes phosphorylation of p38 mitogen-activated protein kinase, and enhances Bax expression and cytochrome c release, leading to apoptosis in rat vascular smooth muscle cells. The overexpression of Bax or its exogenous application causes an opening of mitochondrial permeability transient and induced cytochrome c release, which activates caspase 3 and results in DNA fragmentation and apoptosis (Pastorino et al. 1998, 1999).
In conclusion, a variety of fibrate compounds including fenofibrate, clofibrate, gemfibrozil, bezafibrate and ciprofibrate caused an apoptotic-like cell injury specifically in HRMSC without affecting the viability of HMVEC or HUASMC. The cell injury induced by bezafibrate was concentration- and time-dependent. A synergistic effect was observed, when bezafibrate was treated in combination with simvastatin, although the statin alone at high concentrations caused a cell injury. The fibrate-induced cell injury was characterized by nuclear damage such as chromatin condensation. A PPARα agonist 8(S)-HETE also caused a cell-specific injury in HRMSC. Moreover, the expression of PPARα mRNA was marked in HRMSC but not in HMVEC or HUASMC. Thus, it is possible that the cell-specific reduction in the viability of HRMSC induced by fibrates is associated with the activation of PPARα. Therefore, the present in vitro cell injury model using human rhabdomyosarcoma cells may be useful for studying the pathophysiology of rhabdomyolysis induced by lipid-lowering agents.
References
Brown P, Winegar D, Plunket K, Moore L, Lewis M, Wilson J, Sundseth S, Koble C, Wu Z, Chapman J, Lehmann J, Kliewer S, Willson T (1999) A ureido-thioisobutyric acid (GW9578) is a subtype-selective PPARalpha agonist with potent lipid-lowering activity. J Med Chem 42:3785–3788
Chinetti G, Griglio S, Antonucci M, Torra IP, Delerive P, Majd Z, Fruchart JC, Chapman J, Najb J, Staels B (1998) Activation of proliferator-activated receptors α and δ induces apoptosis of human monocyte-derived macrophages. J Biol Chem 273:255573–255580
Coxon FP, Benford HL, Russell RG, Rogers MJ (1998) Protein synthesis is required for caspase activation and induction of apoptosis by bisphosphonate drugs. Mol Pharmacol 54:631–638
Diep QN, Touyz RM, Schiffrin EL (2000) Docosahexaenoic acid, a peroxisome proliferator-activated receptor-alpha ligand, induces apoptosis in vascular smooth muscle cells by stimulation of p38 mitogen-activated protein kinase. Hypertension 36:851–855
Dimitroulakos J, Nohynek D, Backway KL, Hedley DW, Yeger H, Freedman MH, Minden MD, Penn LZ (1999) Increased sensitivity of acute myelogenous leukemias to lovastatin-induced apoptosis: a potential therapeutic approach. Blood 93:1308–1318
Eberlein M, Heusinger-Ribeiro J, Goppelt-Struebe M (2001) Rho-dependent inhibition of the induction of connective tissue growth factor (CTGF) by HMG CoA reductase inhibitors (statins). Br J Pharmacol 133:1172–1180
Forman BM, Chen J, Evans RM (1997) Hypolipidemic drugs, polyunsaturated fatty acids, and eicosanoids are ligands for peroxisome proliferator-activated receptors α and δ. Proc Natl Acad Sci USA 94:4312–4317
Goa KL, Barradell LB, Plosker GL (1996) Bezafibrate. An update of its pharmacology and use in the management of dyslipidaemia. Drugs 52:725–753
Gonzalez FJ, Peters JM, Cattley RC (1998) Mechanism of action of the nongenotoxic peroxisome proliferator-activator receptor alpha. J Natl Cancer Inst 90:1702–1709
Gotto AM Jr (1998) Triglyceride as a risk factor for coronary artery disease. Am J Cardiol 82:22Q–25Q
Guijarro C, Blanco-Colio LM, Ortego M, Alonso C, Ortiz A, Plaza JJ, Diaz C, Hernandez G, Egido J (1998) 3-Hydroxy-3-methylglutaryl coenzyme a reductase and isoprenylation inhibitors induce apoptosis of vascular smooth muscle cells in culture. Circ Res 83:490–500
Guyton JR (1999) Combination drug therapy for combined hyperlipidemia. Curr Cardiol Rep 1:244–250
Holden PR, Tugwood JD (1999) Peroxisome proliferation-activated receptor α: role in rodent liver cancer and species differences. J Mol Endocrinol 22:1–8
Inoue I, Itoh F, Aoyagi S, Tazawa S, Kusama H, Akahane M, Mastunaga T, Hayashi K, Awata T, Komoda T, Katayama S (2002) Fibrate and statin synergistically increase the transcriptional activities of PPARalpha/RXRalpha and decrease the transactivation of NFκB. Biochem Biophys Res Commun 290:131–139
Lau TK, Leachman DR, Lufschanowski R (2001) Severe rhabdomyolysis associated with the cerivastin-gemfibrozil combination therapy: report of a case. Tex Heart Inst J 28:142–145
Maddala RL, Reddy VN, Rao PV (2001) Lovastatin-induced cytoskeletal reorganization in lens epithelial cells: role of Rho GTPases. Invest Ophthalmol Vis Sci 42:2610–2615
Martin G, Duez H, Blanquart C, Berezowski V, Poulain P, Fruchart JC, Najib-Fruchart J, Glineur C, Staels B (2001) Statin-induced inhibition of the Rho-signaling pathway activates PPARalpha and induces HDL apoA-I. J Clin Invest 107:1423–1432
Moghadasian MH (1999) Clinical pharmacology of 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitors. Life Sci 65:1329–1337
Moghadasian MH, Mancini GB, Frohlich JJ (2000) Pharmacotherapy of hypercholesterolaemia: statins in clinical practice. Expert Opin Pharmacother 1:683–695
Muga SJ, Thuillier P, Pavone A, Rundhaug JE, Boeglin WE, Jisaka M, Brash AR, Fischer SM (2000) 8S-lipoxygenase products activate peroxisome proliferator-activated receptor alpha and induce differentiation in murine keratinocytes. Cell Growth Differ 11:447–454
Omar MA, Wilson JP, Cox TS (2001) Rhabdomyolysis and HMG-CoA reductase inhibitors. Ann Pharmacother 35:1096–1107
Padayatty SJ, Marcelli M, Shao TC, Cunningham GR (1997) Lovastatin-induced apoptosis in prostate stromal cells. J Clin Endocrinol Metab 82:1434–1439
Pastorino JG, Chen ST, Tafani M, Snyder JW, Farber JL (1998) The overexpression of Bax produces cell death upon induction of the mitochondrial permeability transition. J Biol Chem 273:7770–7775
Pastorino JG, Tafani M, Rothman RJ, Marcinkeviciute A, Hoek JB, Farber JL, Marcineviciute A (1999) Functional consequences of the sustained or transient activation by Bax of the mitochondrial permeability transition pore. J Biol Chem 274:31734–31739
Perez-Sala D, Mollinedo F (1993) Inhibition of isoprenoid biosynthesis induces apoptosis in human promyelocytic HL-60 cells. Biochem Biophys Res Commun 199:1209–1215
Poels PJ, Gabreels FJ (1993) Rhabdomyolysis: a review of the literature. Clin Neurol Neurosurg 95:175–192
Robins SJ (2001) PPARalpha ligands and clinical trials: cardiovascular risk reduction with fibrates. J Cardiovasc Risk 8:195–201
Sgro C, Escousse A (1991) Side effects of fibrates (except liver and muscle). Therapie 46:351–354
Sharobeem KM, Madden BP, Millner R, Rolfe LM, Seymour CA, Parker J (2000) Acute renal failure after cardiopulmonary bypass: a possible association with drugs of the fibrate group. J Cardiovasc Pharmacol Ther 5:33–39
Shek A, Ferrill MJ (2001) Statin-fibrate combination therapy. Ann Pharmacother 35:908–917
Staels B, Dallongeville J, Auwerx J, Schoonjans K, Leitersdorf E, Fruchart J-C (1998) Mechanism of action of fibrates on lipid and lipoprotein metabolism. Circulation 98:2088–2093
Tanaka T, Tatsuno I, Uchida D, Moroo I, Morio H, Nakamura S, Noguchi Y, Yasuda T, Kitagawa M, Saito Y, Hirai A (2000) Geranylgeranyl-pyrophosphate, an isoprenoid of mevalonate cascade, is a critical compound for rat primary cultured cortical neurons to protect the cell death induced by 3-hydroxy-3-methylglutaryl-CoA reductase inhibition. J Neurosci 20:2852–2859
Veerkamp JH, Smit JW, Benders AA, Oosterhof A (1996) Effects of HMG-CoA reductase inhibitors on growth and differentiation of cultured rat skeletal muscle cells. Biochim Biophys Acta 1315:217–222
Winegar DA, Brown PJ, Wilkison WO, Lewis MC, Ott RJ, Tong WQ, Brown HR, Lehmann JM, Kliewer SA, Plunket KD, Way JM, Bodkin NL, Hansen BC (2001) Effects of fenofibrate on lipid parameters in obese rhesus monkeys. J Lipid Res 42:1543–1551
Yu K, Bayona W, Kallen CB, Harding HP, Ravera CP, McMahon G, Brown M, Lazar MA (1995) Differential activation of peroxisome proliferator-activated receptors by eicosanoids. J Biol Chem 270:23975–23983
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maiguma, T., Fujisaki, K., Itoh, Y. et al. Cell-specific toxicity of fibrates in human embryonal rhabdomyosarcoma cells. Naunyn-Schmiedeberg's Arch Pharmacol 367, 289–296 (2003). https://doi.org/10.1007/s00210-002-0660-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-002-0660-9