Abstract
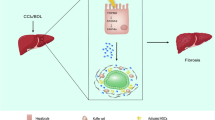
Liver fibrosis is the final common pathway for almost all causes of chronic liver injury. This chronic disease is characterized by excessive deposition of extracellular matrix components mainly due to transdifferentiation of quiescent hepatic stellate cell into myofibroblasts-like cells, which in turn is driven by cell death and inflammation. In the last few years, paracrine signaling through pannexin1 channels has emerged as a key player in the latter processes. The current study was set up to investigate the role of pannexin1 signaling in liver fibrosis. Wild-type and whole body pannexin1 knock-out mice were treated with carbon tetrachloride or subjected to bile duct ligation. Evaluation of the effects of pannexin1 deletion was based on a number of clinically relevant read-outs, including markers of liver damage, histopathological analysis, oxidative stress, inflammation and regenerative capacity. In parallel, to elucidate the molecular pathways affected by pannexin1 deletion as well as to mechanistically anchor the clinical observations, whole transcriptome analysis of liver tissue was performed. While pannexin1 knock-out mice treated with carbon tetrachloride displayed reduced collagen content, hepatic stellate cell activation, inflammation and hepatic regeneration, bile duct ligated counterparts showed increased hepatocellular injury and antioxidant enzyme activity with a predominant immune response. Gene expression profiling revealed a downregulation of fibrotic and immune responses in pannexin1 knock-out mice treated with carbon tetrachloride, whereas bile duct ligated pannexin1-deficient animals showed a pronounced inflammatory profile. This study shows for the first time an etiology-dependent role for pannexin1 signaling in experimental liver fibrosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Liver fibrosis is a wound healing response to chronic injury characterized by excessive extracellular matrix deposition. At the cellular level, the main contributors to the fibrotic response are activated hepatic stellate cells (HSCs) (Puche et al. 2013). This activation program is a complex cellular signaling process in which HSCs interact with hepatocytes, sinusoidal endothelial cells, Kupffer cells and infiltrating immune cells (Canbay et al. 2003; Karlmark et al. 2009; Pradere et al. 2013; Xie et al. 2012). In the past decade, the role of the immune response in both progression and regression of chronic liver diseases has gained increasing attention. Immune cells participate in the promotion of hepatocellular damage, the activation and survival of HSCs and fibrosis regression (Seki and Schwabe 2015). Indeed, blockage of macrophage infiltration inhibits HSC activation and attenuates fibrotic responses (Imamura et al. 2005; Pradere et al. 2013). The mechanisms driving cellular attraction mainly involve paracrine communication circuits, including adenosine-5′-triphosphate (ATP) signaling. Upon injury, apoptotic cells release ATP and uridine-5′-triphosphate into the extracellular milieu via pannexin1 (Panx1), which act as “find-me” signals to attract monocytes, macrophages and microglia to the area of the insult (Chekeni et al. 2010; Davalos et al. 2005). In addition, extracellular ATP potentiates HSC activation in a NACHT, LRR, and pyrin domain-containing protein 3 (Nalp3) inflammasome-dependent manner, in turn contributing to the generation of the pro-inflammatory cytokines interleukin 1 beta, 6 and 18 (IL1β/6/18) (Jiang et al. 2017). Panx channels have been recently identified as critical mediators in ATP release (Dahl 2015). The Panx family consists of 3 members, called Panx1-3, with the former being the most widespread isoform. In the liver, Panx1 was reported to be expressed by hepatocytes, Kupffer cells and HSCs (Kim et al. 2015; Willebrords et al. 2017b; Xiao et al. 2012). In addition to playing a role in physiological conditions, Panx1 channels underlie cell death and inflammatory processes. The latter involves the activation of the Nalp3 inflammasome complex and initiation of leukocyte migration (Crespo Yanguas et al. 2017). In fact, in cardiac fibrosis, cardiomyocytes release ATP through Panx1 channels leading to early fibroblast activation and subsequent expression of IL1β (Dolmatova et al. 2012). This supports the notion that extracellular ATP participates in myofibroblast activation pathways, which in turn trigger immune-related responses. In this study, it is tested whether a similar scenario takes place in liver fibrosis. For this purpose, liver fibrosis was experimentally induced through administration of carbon tetrachloride (CCl4) or application of bile duct ligation (BDL) to both wild-type (WT) and Panx1−/− mice.
Materials and methods
Animals and treatment
Male WT C57BL/6 mice were obtained from Jackson Laboratories (USA). The generation of the global Panx1−/− mice (CMV-Cre/Panx1) was previously described (Dvoriantchikova et al. 2012). Animals were housed in the animal facility of the School of Veterinary Medicine and Animal Science of the University of São Paulo-Brazil. Mice were kept in a room with ventilation (i.e., 16–18 air changes/hour), relative humidity (i.e., 45–65%), controlled temperature (i.e., 20–24 °C) and light/dark cycle 12:12 and were given water and balanced diet (NUVILAB-CR1, Nuvital Nutrientes LTDA, Brazil) ad libitum. This study has been approved by the Committee on Bioethics of the School of Veterinary Medicine and Animal Science of the University of São Paulo-Brazil (protocol number 9999100314) and all animals received humane care according to the criteria outlined in the “Guide for the Care and Use of Laboratory Animals”.
Eight-week old mice of each genotype were used and received 3 intraperitoneal (ip) injections of 20% v/v CCl4 (Sigma-Aldrich, Brazil) per week diluted in corn oil for 8 weeks. Specifically, 1 µl CCl4 per g body weight was administered for the first 2 weeks. Thereafter, a weekly increment of 0.25 µl CCl4 per g body weight to the utmost dose of 2 µl CCl4 per g body weight was given to the animals. Corresponding controls for both genotypes relied on the administration of corn oil ip (Oil). In parallel, a BDL mouse model was set up as described elsewhere (Tag et al. 2015). For this purpose, 8- to 12-weeks old mice from each genotype were used. All mice were weighed and sacrificed after 8 weeks of CCl4 treatment or 20 days after BDL by exsanguination during sampling under isoflurane-induced anesthesia. Blood collected by cardiac puncture was drawn into a heparinized syringe and centrifuged for 10 min at 1503×g, and serum was stored at − 20 °C. Livers were excised and fragments were fixed in 10% phosphate-buffered formalin or snap-frozen in liquid nitrogen with storage at − 80 °C.
Histopathological liver examination and collagen analysis
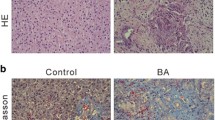
For microscopic evaluation, formalin-fixed liver fragments were embedded in paraffin and 5 µm sections were stained with hematoxylin-eosin (H&E) or Sirius red for blinded evaluation of the liver as previously described (Cogliati et al. 2011). Morphometric analysis of Sirius red staining was performed in 10 randomly selected fields per section from the left lobe (10× objective) using a Nikon Eclipse Ti microscope (Nikon, Japan). Semi-quantitative analysis of the fibrosis area was performed with ImageJ (National Institutes of Health, Bethesda, MD) (Schindelin et al. 2015) and calculated by the formula [area of fibrosis (%) = total fibrosis area/total area of the liver tissue].
Analysis of serum biochemical parameters
Serum levels of alanine aminotransferase (ALT; IU/L), aspartate aminotransferase (AST; IU/L), alkaline phosphatase (ALP; IU/L), conjugated and total bilirubin (mg/dL) and albumin (g/dL) were measured with an automated spectrophotometric Labmax 240 analyzer (Labtest Diagnostica, Brazil) after appropriate dilution of samples.
Immunohistochemistry
Immunoreactivity for α-smooth muscle actin (α-SMA), CD68 or Ki-67 was performed as described elsewhere (Cogliati et al. 2011) with slight modifications. Briefly, 5-µm liver sections were subjected to antigen retrieval at 120 °C for 5 min in a Pascal Pressure Chamber (Dako Cytomation, Denmark) and blocked during 15 min. Then, slides were treated with low-fat milk for 60 min and incubated in a humidified chamber overnight at 4 °C with the appropriate antibodies (Abcam, UK). Subsequently, slides were incubated with a one-step polymer-HRP (EasyPath—Erviegas, Brazil) for 20 min, developed with 3 × 3-diaminobenzidine chromogen (Sigma-Aldrich, USA) and counterstained with Harris hematoxylin. Semi-quantitative analysis was performed using Image-Pro Plus 4.5 software (Media Cybernetics, USA) in 10 randomly selected fields (20× objective for α-SMA and 40× objective for CD68 and Ki-67) per section from the left lobe. Data analysis was based on the following calculations [α-SMA area (%) = α-SMA+ area/(total field area − vascular luminal area)], [CD68+ density = CD68+ cells/total field area (mm2)] and [Ki-67+ density = Ki-67+ cells/total field area (mm2)].
Immunofluorescence
The cellular distribution of T-lymphocytes, monocytes, granulocytes and neutrophils was determined by immunofluorescence as previously described (Maes et al. 2016), with slight modifications. Briefly, 10 µm liver sections from flash-frozen liver tissue were fixated with acetone (CD3, Ly6c and Ly6g) or methanol (CD11b) for 10 min at − 20 °C. Liver sections were incubated with primary antibodies directed against CD3 (Abcam, UK), CD11b (Abcam, UK), Ly6c (Abcam, UK) and Ly6g (Abcam, UK) diluted in blocking buffer based on 5% w/v donkey serum (Jackson Immunoresearch Inc., USA) and 1% w/v bovine serum albumin (Sigma-Aldrich, USA) dissolved in phosphate-buffered saline for 1 h at 37 °C. After intensive washing, liver sections were incubated for 1 h at room temperature against polyclonal donkey anti-rabbit Alexa Fluor® 488-conjugated secondary antibody (Jackson Immunoresearch Inc., USA) or polyclonal goat anti-rat Alexa Fluor® 488-conjugated secondary antibody (Abcam, UK) diluted in blocking buffer. Thereafter, Vectashield with DAPI (Vector laboratories, USA) was used to stain the nuclei and as a mounting medium. Detection was performed by fluorescence microscope Nikon Eclipse Ti (Nikon, Japan).
Analysis of hepatic antioxidant enzymes
The activity of superoxide dismutase (SOD), glutathione peroxidase (GPx), glutathione reductase (GR) and catalase was assayed as previously described (Cogliati et al. 2016). Enzymatic activity was expressed in U/mg protein.
Immunoblot analysis
Immunoblot analysis of liver tissue was performed as previously described (Maes et al. 2017) with slight modifications. After electrophoresis and blotting, blocking of the nitrocellulose membranes was performed with 5% w/v bovine serum albumin (Sigma-Aldrich, USA) in Tris-buffered saline solution containing 0.1% Tween 20. Membranes were incubated overnight at 4 °C with primary antibody directed against p-NF-κBp65 S536 (Cell signaling, USA) and β-actin (Abcam, UK) followed by incubation for 1 h at room temperature with appropriate secondary antibody. Detection of the proteins was carried out by means of an enhanced chemiluminescence. For semi-quantification purposes, a recently described normalization method based on the total protein loading was used to overcome the drawbacks exerted by the use of housekeeping proteins (Eaton et al. 2013; Rivero-Gutiérrez et al. 2014; Taylor et al. 2013; Taylor and Posch 2014), including (1) the lack of expression in a uniform manner within the experimental conditions (Eaton et al. 2013; Rivero-Gutiérrez et al. 2014). (2) The protein working range in which the linearity is maintained may differ between the housekeeping and the protein of interest (Chen and Xu 2015; Eaton et al. 2013; Taylor et al. 2013). (3) Data normalization with housekeeping proteins relies on a single data point, providing a poor reflection of inconsistencies. Consequently, p-NF-κBp65 S536 signals were normalized against total protein loading and expressed as relative alterations compared to BDL-subjected or CCl4-treated WT mice.
Analysis of liver inflammatory markers
Inflammatory markers were determined in hepatic homogenates using a mouse inflammation antibody array (Abcam, UK) following manufacturer’s instructions. Briefly, antibody-bound membranes were blocked during 30 min at room temperature. Thereafter, blocked membranes were exposed to 250 µg protein/ml blocking buffer overnight at 4 °C while shaking. Membranes were washed, incubated with biotin-conjugated anti-cytokines for 2 h at room temperature, washed and exposed to horseradish peroxidase-conjugated streptavidin for 2 h at room temperature. Following washing, proteins were detected by means of enhanced chemiluminescence and visualized by Chemidoc™ MP system (Bio-Rad, USA). Semi-quantitative results were obtained after densitometric analysis. Thereafter, background was subtracted from each data point and results were normalized against the positive controls provided by biotin-conjugated IgG. Final results were presented as relative signal intensity against sham-subjected or oil-treated WT mice.
Reverse transcription quantitative real-time polymerase chain reaction analysis
Reverse transcription quantitative real-time polymerase chain reaction (RT-qPCR) analysis of liver tissue was assayed as explained elsewhere (Maes et al. 2017). The Taqman probes and primers specific for the target and reference genes are represented in Table 1. Relative alterations (fold change) in RNA levels were calculated according to the 2(− ΔΔCq) formula (Livak and Schmittgen 2001).
Whole transcriptome analysis
Transcriptomic analysis was performed as previously described (Willebrords et al. 2017a, b) with slight modifications. After RNA extraction, integrity was assessed by microfluidic analysis using a Fragment Analyzer (Avanced Analytical Technologies, USA). A total of 100 ng RNA per sample was amplified with a Genechip 3′ IVT Express Kit, thereby following the manufacturer’s instructions (Affymetrix, Germany) and purified with magnetic beads. Subsequently, 12.5 µg fragmented amplified RNA was hybridized to Affymetrix Clariom™ D mouse arrays and placed in a Genechip Hybridization Oven-645 (Affymetrix, Germany) rotating at 60 rpm at 45 °C for 16 h. Thereafter, the arrays were washed and stained. The chips were scanned and quality control matrices were confirmed following the manufacturer’s guidelines. Background correction, summarization and normalization of all data were done with Expression Console and Affymetrix Transcriptome Analysis Console Software.
Statistical analysis
The number of repeats (n) for each type of analysis varied and is specified in the discussion of the results. All data were expressed as mean ± standard error of the mean (SEM) or median ± interquartile. Results were statistically processed by t tests with Welch’s correction, one-way analysis of variance (ANOVA) followed by post hoc tests with Bonferroni correction or Kruskal–Wallis tests followed by post hoc tests using Dunn’s correction depending on the distribution (D’Agostino-Pearson normality test for large n or Shapiro–Wilk normality test for low n) using GraphPad Prism7 software with probability (p) values of less than or equal to 0.05 considered as significant.
Results
Panx1 expression in liver fibrosis
A number of reports have described upregulated Panx1 expression levels as a consequence of liver disease (Csak et al. 2011; Kim et al. 2015; Maes et al. 2017). RT-qPCR analysis was used to assess Panx1 expression levels in experimental liver fibrosis in WT mice upon CCl4 or BDL. Panx1 RNA expression levels were increased in both the CCl4 mouse model (p ≤ 0.001) and the BDL mouse model (p ≤ 0.0001) in comparison with their untreated controls (Fig. 1).
Effects of genetic Panx1 deficiency on hepatocellular injury and liver fibrogenesis
CCl4-treated Panx1−/− animals displayed less collagen accumulation (p ≤ 0.01) as well as decreased amounts of α-SMA+ cells (p ≤ 0.05) in comparison with WT counterparts. In addition, RT-qPCR analysis revealed downregulated expression of collagen type 1 alpha 1 (Col1a1) and lysyl oxidase-like 2 (Loxl2) (p ≤ 0.001) (Fig. 2a). Furthermore, CCl4-treated Panx1−/− animals showed lowed serum ALT and AST levels (p ≤ 0.001), but no changes in albumin and total and conjugated bilirubin (Fig. 2b).
Effect of genetic Panx1 deficiency on hepatocellular injury and liver fibrogenesis in chemically-induced liver fibrosis. WT and Panx1−/− mice (n = 5–15) were administered 20% CCl4 ip at a gradually increased dose for 8 weeks. a Area of fibrosis, area of α-SMA-positive cells, and Col1a1 and Loxl2 RNA levels were evaluated. b Serum levels of ALT, AST, albumin, total and conjugated bilirubin were determined. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction. Data were expressed as means ± SEM (*p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.001; ****p ≤ 0.0001)
In the BDL group, no alterations in collagen accumulation or expression of HSC activation markers were noticed between Panx1−/− and WT mice (Fig. 3a). Nevertheless, hepatic damage was exacerbated in BDL-subjected Panx1−/− mice as evidenced by higher levels of serum ALT (p ≤ 0.001), yet with unchanged quantities of ALP, AST, albumin, conjugated and total bilirubin (Fig. 3b).
Effect of genetic Panx1 deficiency on hepatocellular injury and liver fibrogenesis in surgically-induced liver fibrosis. WT and Panx1−/− mice (n = 5–15) were subjected to BDL for 20 days. a Area of fibrosis, area of α-SMA-positive cells, and Col1a1 and Loxl2 RNA levels were evaluated. b Serum levels of ALP, ALT, AST, albumin, total and conjugated bilirubin were determined. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction. Data were expressed as means ± SEM (*p ≤ 0.05; ***p ≤ 0.001; ****p ≤ 0.0001)
Effect of genetic Panx1 deficiency on oxidative stress in liver fibrosis
Oxidative stress with generation of free radicals and lipid peroxidation constitutes an important hallmark in the pathophysiological mechanisms underlying fibrogenesis (Gandhi 2012). Accordingly, the activity of several oxidative stress scavengers was measured in liver tissue. CCl4-treated Panx1−/− mice showed an increase in SOD activity (p ≤ 0.01) and no changes in GPx, GR and catalase activities (Fig. 4a). Panx1−/− mice subjected to BDL displayed increased activity of GPx (p ≤ 0.05) with SOD, GR and catalase being unmodified (Fig. 4b).
Effect of genetic Panx1 deficiency on oxidative stress in liver fibrosis. WT and Panx1−/− mice (n = 8) were administered 20% CCl4 ip at a gradually increased dose for 8 weeks or subjected to BDL for 20 days. Activity of catalase, GPx, GR and SOD was evaluated in a the CCl4 model and b the BDL model. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction and with Kruskal–Wallis test followed by post hoc tests using Dunn’s correction in case of SOD in the CCl4 model as well as catalase and SOD in the BDL model. Data were expressed as means ± SEM or median ± interquartile (*p ≤ 0.05; **p ≤ 0.01)
Effect of genetic Panx1 deficiency on inflammation in liver fibrosis
Hepatic macrophages participate in the regulation of the severity of the fibrotic response mainly by promotion of hepatocellular damage and the initiation and survival of activated HSCs (Cai et al. 2017; Seki and Schwabe 2015; Woolbright and Jaeschke 2012). A key mechanism driving the survival of activated HSCs is the activation of nuclear factor kappa B (NF-κB) by tumor necrosis factor alpha (TNFα) and IL1β (Pradere et al. 2013). In this study, the number of macrophages was monitored through staining and counting of CD68+ cells in liver tissue. CD68+ cells were mainly located in the sinusoids of untreated animals, while in CCl4-treated or BDL-subjected mice, these cells were predominantly found in areas surrounding the scar tissue. In the CCl4 mouse model, the CD68+ cell population was not changed upon genetic Panx1 ablation (Fig. 5a). Furthermore, evaluation of NF-κB activation through semi-quantitative immunoblot analysis showed reduced protein levels of NF-κB p65 phosphorylated at the serine residue S536 (p-NF-κBp65 S536) in Panx1−/− mice (p ≤ 0.0001) (Fig. 5a; Supplementary Fig. 1a). In the BDL group, the number of CD68+ cells were increased in Panx1−/− mice (p ≤ 0.05) (Fig. 5b). However, these animals presented no differences of p-NF-κBp65 S536 protein levels (Fig. 5b; Supplementary Fig. 1b).
Effect of genetic Panx1 deficiency on inflammation in liver fibrosis. WT and Panx1−/− mice were administered 20% CCl4 ip at a gradually increased dose for 8 weeks or subjected to BDL for 20 days. Representative images for the calculation of hepatic CD68+ cell density (n = 5) and example of blot membranes for the determination of p-NF-κBp65 S536 protein levels (n = 9–15) in a the CCl4 model and b the BDL model. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction and with Kruskal–Wallis test followed by post hoc tests using Dunn’s correction in case of the p-NF-κBp65 S536. Data were expressed as means ± SEM or median ± interquartile (*p ≤ 0.05; ***p ≤ 0.001; ****p ≤ 0.0001). Scale bar represents 20 µm
Panx1 channels are known to modulate Nalp3 inflammasome activation in hepatic macrophages (Kim et al. 2015). In addition to the reduced protein levels of p-NF-κBp65 S536, the RNA levels of Nalp3 inflammasome components apoptosis-associated speck-like protein containing a C-terminal caspase-recruitment domain (ASC) (p ≤ 0.01) and caspase 1 (Casp1) (p ≤ 0.0001) were indeed downregulated in CCl4-treated Panx1−/− mice (Fig. 6). Thereafter, 40 proteins involved in inflammation were evaluated to determine the effect of Panx1−/− in liver fibrosis (Fig. 7). In the CCl4 model, lowed protein levels of IL1β (p ≤ 0.05), IL2 (p ≤ 0.05), lymphotactin (p ≤ 0.001), monocyte chemoattractant protein 1 (MCP-1) (p ≤ 0.05), T-cell activation protein 3 (TCA-3) (p ≤ 0.05), thymus-expressed chemokine (TECK) (p ≤ 0.05), TNFα (p ≤ 0.05), soluble TNF receptor 1 (sTNF-RI) (p ≤ 0.05) and sTNF-RII (p ≤ 0.01) were observed in the Panx1−/− mice (Fig. 8). In the BDL group, only the macrophage protein 1 gamma (MIP1γ) was increased due to Panx1−/− (Fig. 9). To further characterize the immune response, a series of stainings against typical immune cell markers were performed. In the CCl4 model, the immune cell population was mainly represented by the CD11b+ and Ly6c+ cells, usually expressed by the inflammatory monocyte subset considered as precursors of tissue macrophages. Both markers were observed in areas surrounding the scar tissue of WT and Panx1−/− mice treated with CCl4 (Fig. 10). In addition, only small amounts of neutrophils (Ly6g+ cells) and scarce T-lymphocytes (CD3+ cells) were observed in the fibrotic liver tissue of WT and Panx1−/− mice. In the BDL group, CD11b+, Ly6c+ and Ly6g+ cells were located in the portal and necrotic areas of liver from WT and Panx1−/− mice (Fig. 11). In addition, CD11b+ and Ly6c+ cell infiltration within the parenchyma of the BDL-subjected Panx1−/− cohort was observed (Fig. 11). T cells stained for CD3 were restricted to the liver portal areas of BDL-subjected WT and Panx1−/− animals.
Effect of genetic Panx1 deficiency on the Nalp3 inflammasome components in liver fibrosis. WT and Panx1−/− mice (n = 10) were administered 20% CCl4 ip at a gradually increased dose for 8 weeks. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction. Data were expressed as means ± SEM (**p ≤ 0.01; ****p ≤ 0.0001)
Antibody array map with the inflammatory proteins (BLC, B lymphocyte chemoattractant; CD30L, tumor necrosis factor ligand superfamily member 8; Eotx, eotaxin; Frck, fractalkine, GCSF, granulocyte colony-stimulating factor; GM-CSF, granulocyte–macrophage colony-stimulating factor; IFNγ, interferon gamma; IL1α/1β/2/7/4/6/9/10/12/13/17, interleukin 1 alpha/1 beta/2/7/4/6/9/10/12/13/17; ITAC, interferon-inducible T-cell alpha chemoattractant; KC, growth-regulated alpha protein; Lept, leptin; LIX, lipopolysaccharide-induced CXC chemokine; Lymp, lymphotactin; MCP-1, monocyte chemoattractant protein 1; MCSF, macrophage colony-stimulating factor; MIG, monokine induced by gamma interferon; MIP1α/γ, macrophage inflammatory protein 1 alpha/gamma; Neg, negative; Pos, positive; RNTS, rantes; SDF-1, stromal cell-derived factor 1; sTNF RI/II, soluble TNF receptor 1/2; TCA-3, T-cell activation protein 3; TECK, thymus-expressed chemokine; TIMP-1/-2, tissue inhibitor of metalloproteinase-1/-2; TNFα, tumor necrosis factor alpha)
Effect of genetic Panx1 deficiency on inflammatory proteins in chemically-induced liver fibrosis. WT and Panx1−/− mice (n = 4) were administered 20% CCl4 ip at a gradually increased dose for 8 weeks. Representative antibody array membranes from liver tissue extract corresponded to WT and Panx1−/− treated with oil or CCl4. Data were analyzed by densitometry analysis. Then, background was subtracted and results were normalized against the average of positive control. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction. Data were expressed as means ± SEM (*p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.001)
Effect of genetic Panx1 deficiency on inflammatory proteins in surgically-induced liver fibrosis. WT and Panx1−/− mice (n = 4) were subjected to BDL for 20 days. Representative antibody array membranes from liver tissue extract corresponded to WT and Panx1−/− subjected to sham or BDL. Data were analyzed by densitometry analysis. Then, background was subtracted and results were normalized against the average of positive control. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction. Data were expressed as means ± SEM (*p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.001; ****p ≤ 0.0001)
Effects of genetic Panx1 deficiency on regenerative capacity in liver fibrosis
Hepatocyte proliferation is critical to ensure the healing process after liver injury. Accordingly, the regenerative capacity was determined through staining and counting of Ki-67+ cells in liver tissue. Untreated WT and Panx1−/− mice seemed to rarely express Ki-67. In the CCl4 group, but not in the BDL cohort, Panx1−/− animals showed less Ki-67+ hepatocytes (p ≤ 0.05) (Fig. 12a, b). It is well-known that bile duct blockage leads to the proliferation of cholangiocytes, which triggers bile duct hyperplasia. In this respect, the number of Ki-67+ cholangiocytes upon BDL was equal among all experimental groups (Fig. 12b).
Effect of genetic Panx1 deficiency on regenerative capacity in liver fibrosis. WT and Panx1−/− mice (n = 5) were administered 20% CCl4 ip at a gradually increased dose for 8 weeks or subjected to BDL for 20 days. Ki-67+ cell density in a the CCl4 model and b the BDL model. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction and with Kruskal–Wallis test followed by post hoc tests using Dunn’s correction in case of the Ki-67+ hepatocytes and cholangiocytes within the BDL model. Data were expressed as means ± SEM or median ± interquartile (*p ≤ 0.05; ****p ≤ 0.0001). Scale bar represents 20 µm
Effect of genetic Panx1 deficiency on the liver transcriptome in liver fibrosis
To shed more light onto the involvement of Panx1 signaling pathways in the fibrotic response, global gene expression profiles were studied in WT and Panx1−/− whether or not treated with CCl4 or subjected to BDL. CCl4 treatment in WT and Panx1−/− resulted in 223 and 192 differentially modulated genes, respectively, with at least twofold change and p < 0.05 compared to untreated WT animals. When compared, 3 clusters of genes were identified, including: (1) 103 genes specifically modulated due to CCl4 treatment in the WT genetic background (Supplementary Table 1), (2) 120 regulated genes resulting from the CCl4 treatment (Supplementary Table 2) and (3) 72 genes associated with the CCl4 treatment in the Panx1−/− genetic background (Table 2) (Fig. 13a). The most prominent reduction in the networks within the CCl4 treatment cluster due to Panx1−/− was centered on a plethora of genes related to cell cycle, fibrotic and immune responses, metabolism, and oxidation–reduction and epoxygenase activities. Among those, pro-fibrogenic genes required for pathological extracellular matrix formation as well as genes involved in muscle contraction were strongly downregulated. In addition, in the Panx1−/− genetic background cluster, suppressed expression of genes involved in the fibrotic response was observed, which reinforces the observed reduced collagen content and HSC activation in CCl4-treated Panx1−/− animals. Downregulated immune genes related to the Toll-like receptor (TLR) signaling, leukocyte migration and chemotaxis. Effects on the TLR signaling pathway were also confirmed by RT-qPCR analysis of the genes dectin-1 (Clec7a), lipopolysaccharide-binding protein (Lbp) and the lymphocyte antigen 96 (Ly96). Expression of Clec7a (p ≤ 0.0001) and Lbp (p ≤ 0.01) was significantly reduced, while no changes in Ly96 were found in the CCl4-treated Panx1−/− mice (Fig. 13b). This is in line with the observed reduced protein levels of p-NF-κBp65 S536. Several other genes encoding mediators of immunity, metabolism and transportation were also negatively affected (Table 2).
Panx1 deficiency effect in the liver transcriptome in liver fibrosis. WT and Panx1−/− mice (n = 5) administered 20% CCl4 ip at a gradually increased dose for 8 weeks. a Gene ontogeny of the different clusters of modulated genes expressed as the average of the fold change from genes with at least twofold difference and p < 0.05 and b RT-qPCR analysis from genes corresponded to the categories: CCl4 independent of genetic background or CCl4 in Panx1−/− genetic background. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction. Data were expressed as means ± SEM (**p ≤ 0.01; ****p ≤ 0.0001). N.M. not modulated
Likewise, 3 gene clusters could be identified following BDL, including: (1) 137 genes modulated due to the BDL procedure in the WT genetic background (Supplementary Table 3), (2) 341 genes altered through the BDL procedure (Supplementary Table 4), and (3) 39 genes associated with BDL procedure in Panx1−/− mice (Table 3) with at least twofold change and p < 0.05 (Fig. 14a). Although only minimum differences in the overall gene modulation ontogeny were observed within the BDL cluster, several genes related to the immune response were markedly downregulated as a consequence of genetic Panx1 ablation. Downregulated genes related to cell adhesion, activation, migration functions and TLR signaling. In contrast, genes critical for chemotaxis, TLR4 signaling, leukocyte migration, platelet activation and neutrophil degranulation were upregulated. Nevertheless, RT-qPCR analysis revealed no modification in S100 calcium-binding protein A9 (S100a9) levels in BDL-subjected Panx1−/− mice (Fig. 14b). The major upregulated pathways in BDL-subjected Panx1−/− mice were related to immune responses (Table 3). Out of them, chemokine ligand 14 (Cxcl14) was evaluated by RT-qPCR, resulting in a lack of modulation in BDL-subjected Panx1−/− mice (Fig. 14b). This supports the elevated numbers of macrophages observed in BDL-subjected Panx1−/− mice.
Panx1 deficiency effect in the liver transcriptome in liver fibrosis. WT and Panx1−/− mice (n = 5) subjected to BDL for 20 days. a Gene ontogeny of the different clusters of modulated genes expressed as the average of the fold change from genes with at least twofold difference and p < 0.05 and b RT-qPCR analysis from genes corresponded to the categories: BDL independent of genetic background or BDL in Panx1−/− genetic background. Results were analyzed by one-way ANOVA followed by post hoc tests using Bonferroni correction. Data were expressed as means ± SEM (***p ≤ 0.001). N.M. not modulated
Discussion
Transdifferentiation of quiescent into activated HSCs constitutes an important feature in the progression of liver fibrosis. Despite the wealth of knowledge regarding the involvement of signaling pathways to this process, the participation of communication mediated by Panx1 channels has been poorly documented thus far. In this regard, this study showed increased expression of Panx1 in mouse liver following CCl4 treatment or BDL surgery, which has also been found in experimental models of non-alcoholic steatohepatitis (Csak et al. 2011), acute liver failure (Maes et al. 2017) and ischemia/reperfusion injury (Kim et al. 2015). Accordingly, CCl4-treated Panx1−/− mice seem more protected as evidenced by the reduced fibrotic response, pro-inflammatory signaling and hepatic regeneration. By contrast, BDL-subjected Panx1−/− mice showed a marked hepatocellular injury and increased antioxidant enzyme activity with a predominant immune response.
Panx1 channels have been described to play a role in inflammatory mechanisms in liver disease either by the recruitment of leukocytes or through the activation of the Nalp3 inflammasome (Csak et al. 2011; Kim et al. 2015; Maes et al. 2017; Xiao et al. 2015). Indeed, Nalp3 inflammasome activation in myeloid-derived cells triggers liver inflammation, leukocyte infiltration, pro-inflammatory macrophage recruitment and activation of fibrogenic pathways (Wree et al. 2014). In this respect, CCl4-treated WT and Panx1−/− showed an immune cell population mainly characterized by the presence of CD11b+ and Ly6c+ cells. In fact, unmodified CD68+ macrophage numbers, but decreased hepatic Nalp3 inflammasome component expression, lowed protein levels of p-NF-κBp65 S536 and reduced amounts of a number of inflammatory proteins were found. Among those, a lowed production of the inflammasome-dependent IL1β was observed as well as decreased protein levels of TNFα and its respective receptors, sTNF-RI and -RII. This suggests that genetic Panx1 deletion interferes with signaling pathways that contribute to IL1β and TNFα secretion, which in turn affects the survival of activated HSCs through NF-κB activation (Pradere et al. 2013). Consequently, pro-inflammatory proteins released by activated HSCs, macrophages or involved in HSC recruitment, such as MCP-1 or TECK, were negatively affected. In addition to the reduced survival of activated HSC, decreased cytokine secretion influences the occurrence of diminished hepatic injury (Seki and Schwabe 2015). Indeed, the lowed hepatic proliferation might constitute a compensatory effect. Other mechanisms involved in the apoptotic cell death of activated HSCs include excessive oxidative stress (Dunning et al. 2013). CCl4-treated Panx1−/− mice accumulate hydrogen peroxide because of SOD overactivation and the absence of modulation of the hydrogen peroxide-scavengers GPx and catalase. This may represent an alternative mechanism that could contribute to the decreased activated HSCs levels. In contrast, this effect may not apply to the BDL-subjected mice, since increased GPx activity was observed. Although no direct association between Panx1 and SOD or GPx has been reported thus far, hydrogen peroxide is known to transiently affect Panx1 channel function (Krick et al. 2016). This points to modulation of the oxidative stress scavengers as being a secondary effect to genetic Panx1 ablation. On the other hand, the Panx1−/− potentiates the number of macrophages and the protein levels of MIP1γ, but not NF-κB activation, upon BDL surgery. MIP1γ is mainly produced by macrophages and functions as a cell survival factor and plays a role in the recruitment of myeloid progenitor cells to mediate in a metastasis-promoting effect (Hara et al. 1995; Yan et al. 2015). It is uncertain whether these changes are induced by the accumulation of bile acids in macrophages. Recent data support that the farnesoid X receptor regulates bile acid-induced Nalp3 inflammasome activation in macrophages (Hao et al. 2017). Although ATP synergizes with bile acids to activate Nalp3 (Hao et al. 2017), selective inhibition of Panx1 does not alter extracellular ATP concentrations in pancreatic cells (Kowal et al. 2015), which could point to Panx1-independent activation of Nalp3 under these conditions. In fact, this was also evidenced by the lack of modification in the protein levels of IL1β. Alternatively, other immune cellular subsets clustered within the CD3+, CD11b+, Ly6c+ or Ly6g+ cell population were identified in the BDL-subjected WT and Panx1−/− cohorts. This substantiates that in addition to macrophages, T cells and neutrophils might contribute to the deterioration of the cholestatic liver. In experimental chronic cholestasis, however, neutrophils lack to participate in the wound healing response either in the promotion of hepatic damage (Moles et al. 2014; Saito et al. 2003) and are guided to the injured liver through a mechanism mediated by CXCL2 (Moles et al. 2014). This mechanism could explain why, in contrast to previous studies (Bao et al. 2013), Panx1 channels are not required for the fine-tuning of neutrophil migration in the BDL model. These changes indicate a shift towards an exacerbated immune reaction independently of Nalp3 inflammasome activation and neutrophil infiltration, but mainly governed by the action of macrophages, which may substantiate the maintenance of activated HSCs as well as the pronounced hepatic injury.
Global gene expression profiling was performed to investigate the molecular mechanisms driven by Panx1 signaling in CCl4-treated and BDL-subjected mice. Several genes associated with fibrotic and immune responses were downregulated or negatively modulated in the CCl4-treated Panx1−/− animals. Among those, the Clec7a, Lbp and Ly96 genes are involved in TLR4 activation. In fact, RT-qPCR analysis confirmed the downregulation of Clec7a and Lbp gene levels in the CCl4-treated Panx1−/− mice. In particular, Clec7a is mainly localized in dendritic cells and macrophages and counteracts the fibrotic response by suppressing TLR4 signaling (Seifert et al. 2015). This could suggest that interference of the NF-κB/Nalp3 signaling axis via Panx1 deletion reduces inflammatory responses and thus the fibrotic response, upon CCl4 treatment. In contrast, increased transcription of the S100a9 gene in BDL-subjected Panx1−/− mice was observed. S100a9 has recently been associated with inflammatory macrophages (Krenkel and Tacke 2017; Simard et al. 2013). In fact, several genes were identified in the BDL Panx1−/− genetic background cluster to be involved in chemotaxis and acute-phase reaction Cxcl14, Hp, Plscr1 and Saa2, NF-κB signaling pathway (S100a6), and adaptive immune response (Rnf125). Nevertheless, RT-qPCR analysis revealed an absence of significant modulation of S100a9 and Cxcl14.
In conclusion, this study shows for the first time an etiology-dependent role for Panx1 signaling in experimental liver fibrosis. Nevertheless, a more in-depth understanding of the mechanisms underlying the Panx1-dependent inflammatory response will require further investigation to assess the therapeutic potential of Panx1 channels as immunomodulators of the fibrotic response.
Abbreviations
- α-SMA:
-
Alpha smooth muscle actin
- ALT:
-
Alanine aminotransferase
- ALP:
-
Alkaline phosphatase
- ANOVA:
-
Analysis of variance
- ASC:
-
Apoptosis-associated speck-like protein containing a C-terminal caspase-recruitment domain
- AST:
-
Aspartate aminotransferase
- ATP:
-
Adenosine-5′-triphosphate
- BDL:
-
Bile duct ligation
- Casp1:
-
Caspase 1
- CCl4 :
-
Carbon tetrachloride
- Clec7a:
-
Dectin-1
- Col1a1:
-
Collagen type 1 alpha 1
- Cxcl14:
-
Chemokine ligand 14
- GPx:
-
Glutathione peroxidase
- GR:
-
Glutathione reductase
- HSCs:
-
Hepatic stellate cells
- IL:
-
Interleukin
- ip:
-
Intraperitoneally
- Lbp:
-
Lipopolysaccharide-binding protein
- Loxl2:
-
Lysyl oxidase-like 2
- Ly96:
-
Lymphocyte antigen 96
- MCP-1:
-
Monocyte chemoattractant protein 1
- MIP1γ:
-
Macrophage protein 1 gamma
- Nalp3:
-
NACHT, LRR, and pyrin domain-containing protein 3
- n :
-
Number or repeats
- NF-κB:
-
Nuclear factor kappa B
- Panx:
-
Pannexin
- p :
-
Probability
- RT-qPCR:
-
Reverse transcription quantitative real-time polymerase chain reaction
- S100a9:
-
S100 calcium-binding protein A9
- SEM:
-
Standard error of mean
- SOD:
-
Superoxide dismutase
- sTNF-RI/-RII:
-
Soluble TNF receptor 1/2
- TCA-3:
-
T-cell activation protein 3
- TECK:
-
Thymus-expressed chemokine
- TLR:
-
Toll-like receptor
- TNFα:
-
Tumor necrosis factor alpha
- WT:
-
Wild-type
References
Bao Y, Chen Y, Ledderose C, Li L, Junger WG (2013) Pannexin 1 channels link chemoattractant receptor signaling to local excitation and global inhibition responses at the front and back of polarized neutrophils. J Biol Chem 288:22650–22657. https://doi.org/10.1074/jbc.M113.476283
Cai SY, Ouyang X, Chen Y et al (2017) Bile acids initiate cholestatic liver injury by triggering a hepatocyte-specific inflammatory response. JCI Insight 2:e90780. https://doi.org/10.1172/jci.insight.90780
Canbay A, Taimr P, Torok N, Higuchi H, Friedman S, Gores GJ (2003) Apoptotic body engulfment by a human stellate cell line is profibrogenic. Lab Invest 83:655–663
Chekeni FB, Elliott MR, Sandilos JK et al (2010) Pannexin 1 channels mediate ‘find-me’ signal release and membrane permeability during apoptosis. Nature 467:863–867. https://doi.org/10.1038/nature09413
Chen W, Xu WH (2015) β-Actin as a loading control: less than 2 µg of total protein should be loaded. Electrophoresis 36:2046–2049. https://doi.org/10.1002/elps.201500138
Cogliati B, Da Silva TC, Aloia TP et al (2011) Morphological and molecular pathology of CCL4-induced hepatic fibrosis in connexin43-deficient mice. Microsc Res Tech 74:421–429. https://doi.org/10.1002/jemt.20926
Cogliati B, Crespo Yanguas S, Da Silva TC et al (2016) Connexin32 deficiency exacerbates carbon tetrachloride-induced hepatocellular injury and liver fibrosis in mice. Toxicol Mech Methods 26:362–370. https://doi.org/10.1080/15376516.2016.1190991
Crespo Yanguas S, Willebrords J, Johnstone SR et al (2017) Pannexin1 as mediator of inflammation and cell death. Biochim Biophys Acta 1864:51–61. https://doi.org/10.1016/j.bbamcr.2016.10.006
Csak T, Ganz M, Pespisa J, Kodys K, Dolganiuc A, Szabo G (2011) Fatty acid and endotoxin activate inflammasomes in mouse hepatocytes that release danger signals to stimulate immune cells. Hepatology 54:133–144. https://doi.org/10.1002/hep.24341
Dahl G (2015) ATP release through pannexon channels. Philos Trans R Soc Lond B Biol Sci 370:20140191. https://doi.org/10.1098/rstb.2014.0191
Davalos D, Grutzendler J, Yang G et al (2005) ATP mediates rapid microglial response to local brain injury in vivo. Nat Neurosci 8:752–758
Dolmatova E, Spagnol G, Boassa D et al (2012) Cardiomyocyte ATP release through pannexin 1 aids in early fibroblast activation. Am J Physiol Heart Circ Physiol 303:H1208–H1218. https://doi.org/10.1152/ajpheart.00251.2012
Dunning S, Ur Rehman A, Tiebosch MH et al (2013) Glutathione and antioxidant enzymes serve complementary roles in protecting activated hepatic stellate cells against hydrogen peroxide-induced cell death. Biochim Biophys Acta 1832:2027–2034. https://doi.org/10.1016/j.bbadis.2013.07.008
Dvoriantchikova G, Ivanov D, Barakat D et al (2012) Genetic ablation of Pannexin1 protects retinal neurons from ischemic injury. PLoS One 7:e31991. https://doi.org/10.1371/journal.pone.0031991
Eaton SL, Roche SL, Llavero Hurtado M et al (2013) Total protein analysis as a reliable loading control for quantitative fluorescent Western blotting. PLoS One 8:e72457. https://doi.org/10.1371/journal.pone.0072457
Gandhi CR (2012) Oxidative stress and hepatic stellate cells: a paradoxical relationship. Trends Cell Mol Biol 7:1–10
Hao H, Cao L, Jiang C et al (2017) Farnesoid X receptor regulation of the NLRP3 inflammasome underlies cholestasis-associated sepsis. Cell Metab 25:856–867. https://doi.org/10.1016/j.cmet.2017.03.007
Hara T, Bacon KB, Cho LC et al (1995) Molecular cloning and functional characterization of a novel member of the C-C chemokine family. J Immunol 155:5352–5358
Imamura M, Ogawa T, Sasaguri Y, Chayama K, Ueno H (2005) Suppression of macrophage infiltration inhibits activation of hepatic stellate cells and liver fibrogenesis in rats. Gastroenterology 128:138–146. https://doi.org/10.1053/j.gastro.2004.10.005
Jiang S, Zhang Y, Zheng JH et al (2017) Potentiation of hepatic stellate cell activation by extracellular ATP is dependent on P2 × 7R-mediated NLRP3 inflammasome activation. Pharmacol Res 117:82–93. https://doi.org/10.1016/j.phrs.2016.11.040
Karlmark KR, Weiskirchen R, Zimmermann HW et al (2009) Hepatic recruitment of the inflammatory Gr1 + monocyte subset upon liver injury promotes hepatic fibrosis. Hepatology 50:261–274. https://doi.org/10.1002/hep.22950
Kim HY, Kim SJ, Lee SM (2015) Activation of NLRP3 and AIM2 inflammasomes in Kupffer cells in hepatic ischemia/reperfusion. FEBS J 282:259–270. https://doi.org/10.1111/febs.13123
Kowal JM, Haanes KA, Christensen NM, Novak I (2015) Bile acid effects are mediated by ATP release and purinergic signalling in exocrine pancreatic cells. Cell Commun Signal 13:28. https://doi.org/10.1186/s12964-015-0107-9
Krenkel O, Tacke F (2017) Liver macrophages in tissue homeostasis and disease. Nat Rev Immunol 17:306–321. https://doi.org/10.1038/nri.2017.11
Krick S, Wang J, St-Pierre M, Gonzalez C, Dahl G, Salathe M (2016) Dual oxidase 2 (Duox2) regulates pannexin 1-mediated ATP release in primary human airway epithelial cells via changes in intracellular pH and not H2O2 production. J Biol Chem 291:6423–6432. https://doi.org/10.1074/jbc.M115.664854
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Maes M, McGill MR, da Silva TC et al (2016) Involvement of connexin43 in acetaminophen-induced liver injury. Biochim Biophys Acta 1862:1111–1121. https://doi.org/10.1016/j.bbadis.2016.02.007
Maes M, McGill MR, da Silva TC et al (2017) Inhibition of pannexin1 channels alleviates acetaminophen-induced hepatotoxicity. Arch Toxicol 91:2245–2261. https://doi.org/10.1007/s00204-016-1885-6
Moles A, Murphy L, Wilson CL et al (2014) A TLR2/S100A9/CXCL-2 siganling for neutrophil recruitment in acute and chronic liver injury in the mouse. J Hepatol 60:782–791. https://doi.org/10.1016/j.jhep.2013.12.005
Pradere JP, Kluwe J, De Minicis S et al (2013) Hepatic macrophages but not dendritic cells contribute to liver fibrosis by promoting the survival of activated hepatic stellate cells in mice. Hepatology 58:1461–1473. https://doi.org/10.1002/hep.26429
Puche JE, Lee YA, Jiao J et al (2013) A novel murine model to deplete hepatic stellate cells uncovers their role in amplifying liver damage in mice. Hepatology 57:339–350. https://doi.org/10.1002/hep.26053
Rivero-Gutiérrez B, Anzola A, Martínez-Augustin O, de Medina FS (2014) Stain-free detection as loading control alternative to Ponceau and housekeeping protein immunodetection in Western blotting. Anal Biochem 467:1–3. https://doi.org/10.1016/j.ab.2014.08.027
Saito JM, Bostick MK, Campe CB, XU J, Maher JJ (2003) Infiltrating neutrophils in bile duct-ligated livers do not promote hepatic fibrosis. Hepatol Res 25:180–191. https://doi.org/10.1016/S1386-6346(02)00247-4
Schindelin J, Rueden CT, Hiner MC, Eliceiri KW (2015) The ImageJ ecosystem: an open platform for biomedical image analysis. Mol Reprod Dev 82:518–529. https://doi.org/10.1002/mrd.22489
Seifert L, Deutsch M, Alothman S et al (2015) Dectin-1 regulates hepatic fibrosis and hepatocarcinogenesis by suppressing TLR4 signaling pathways. Cell Rep 13:1909–1921. https://doi.org/10.1016/j.celrep.2015.10.058
Seki E, Schwabe RF (2015) Hepatic inflammation and fibrosis: functional links and key pathways. Hepatology 61:1066–1079. https://doi.org/10.1002/hep.27332
Simard JC, Cesaro A, Chapeton-Montes J et al (2013) S100A8 and S100A9 induce cytokine expression and regulate the NLRP3 inflammasome via ROS-dependent activation of NF-κB. PLoS One 8:e72138. https://doi.org/10.1371/journal.pone.0072138
Tag CG, Sauer-Lehnen S, Weiskirchen S et al (2015) Bile duct ligation in mice: induction of inflammatory liver injury and fibrosis by obstructive cholestasis. J Vis Exp 96:52438. https://doi.org/10.3791/52438
Taylor SC, Posch A (2014) The design of a quantitative western blot experiment. Biomed Res Int 2014:361590. https://doi.org/10.1155/2014/361590
Taylor SC, Berkelman T, Yadav G, Hammond M (2013) A defined methodology for reliable quantification of Western blot data. Mol Biotechnol 55:217–226. https://doi.org/10.1007/s12033-013-9672-6
Willebrords J, Cogliati B, Pereira IVA et al (2017a) Inhibition of connexin hemichannels alleviates non-alcoholic steatohepatitis in mice. Sci Rep 7:8268. https://doi.org/10.1038/s41598-017-08583-w
Willebrords J, Maes M, Pereira IVA et al (2017b) Protective effect of genetic deletion of pannexin1 in experimental mouse models of acute and chronic liver disease. Biochim Biophys Acta 1864:819–830. https://doi.org/10.1016/j.bbadis.2017.12.013
Woolbright BL, Jaeschke H (2012) Novel insight into mechanisms of cholestatic liver injury. World J Gastroenterol 18:4985–4993. https://doi.org/10.3748/wjg.v18.i36.4985
Wree A, Eguchi A, McGeough MD et al (2014) NLRP3 inflammasome activation results in hepatocyte pyroptosis, liver inflammation, and fibrosis in mice. Hepatology 59:898–910. https://doi.org/10.1002/hep.26592
Xiao F, Waldrop SL, Khimji AK, Kilic G (2012) Pannexin1 contributes to pathophysiological ATP release in lipoapoptosis induced by saturated free fatty acids in liver cells. Am J Physiol Cell Physiol 303:C1034–C1044. https://doi.org/10.1152/ajpcell.00175.2012
Xiao F, Waldrop SL, Bronk SF, Gores GJ, Davis LS, Kilic G (2015) Lipoapoptosis induced by saturated free fatty acids stimulates monocyte migration: a novel role for Pannexin1 in liver cells. Purinergic Signal 11:347–359. https://doi.org/10.1007/s11302-015-9456-5
Xie G, Wang X, Wang L et al (2012) Role of differentiation of liver sinusoidal endothelial cells in progression and regression of hepatic fibrosis in rats. Gastroenterology 142:918–927.e6. https://doi.org/10.1053/j.gastro.2011.12.017
Yan HH, Jiang J, Pang Y et al (2015) CCL9 induced by TGF-β signaling in myeloid cells enhances tumor cell survival in the premetastatic organ. Cancer Res 75:5283–5298. https://doi.org/10.1158/0008-5472.CAN-15-2282-T
Acknowledgements
This work was supported by the grants of the “Fundação de Auxílio à Pesquisa do Estado de São Paulo” (FAPESP Grants 14/23890-4; 14/23887-3 and SPEC 13/50420-6), the European Research Council (ERC Starting Grant 335476), the Fund for Scientific Research-Flanders (FWO Grants G009514N and G010214N) and the University Hospital of the Vrije Universiteit Brussel-Belgium (“Willy Gepts Fonds” UZ-VUB). The authors thank Miss Tineke Vanhalewyn, Miss Dinja De Win and Mr Steven Branson for their dedicated technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Electronic supplementary material
Below is the link to the electronic supplementary material.
204_2018_2255_MOESM1_ESM.pdf
Western blots from p-NF-κBp65 S536 protein expression in liver fibrosis. WT and Panx1-/- mice (n = 10-15) were administered 20% CCl4 ip at a gradually increased dose for 8 weeks or subjected to BDL for 20 days. Representative blot membranes expressing p-NF-κBp65 S536 proteins, total protein loading and β-actin proteins from a the CCl4 model and b the BDL model (PDF 230 KB)
204_2018_2255_MOESM3_ESM.docx
Gene modulation by the CCl4 treatment independent of background: comparison between WT CCl4 vs WT-oil and Panx1-/- CCl4 vs WT-oil (DOCX 25 KB)
204_2018_2255_MOESM5_ESM.docx
Gene modulation by the BDL procedure independent of background: comparison between WT BDL vs WT-sham and Panx1-/- BDL vs WT-sham (DOCX 45 KB)
Rights and permissions
About this article
Cite this article
Crespo Yanguas, S., da Silva, T.C., Pereira, I.V.A. et al. Genetic ablation of pannexin1 counteracts liver fibrosis in a chemical, but not in a surgical mouse model. Arch Toxicol 92, 2607–2627 (2018). https://doi.org/10.1007/s00204-018-2255-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-018-2255-3