Abstract
Acute exposure to cadmium (Cd), a toxic heavy metal, causes systemic inflammation characterized by neutrophilia. To elucidate the mechanism of neutrophilia induced by Cd, we investigated the induction of granulocyte colony-stimulating factor (G-CSF), which regulates neutrophil production, in mice with acute Cd toxicity, and compared it with mice injected with lipopolysaccharide (LPS) as an inducer of general inflammatory responses. We injected BALB/c mice with Cd at 2.5 mg/kg i.p. or LPS at 0.5 mg/kg i.p. and sampled the peripheral blood and organs at time points up to 24 h. In Cd-treated mice, the peripheral neutrophil count increased steadily up to 24 h, whereas LPS-treated mice showed a more rapid increase with a peak at 12 h. The serum G-CSF level increased gradually to reach a plateau at 12–18 h in Cd-treated mice, but LPS-treated mice showed a marked increase, reaching a peak at 2–3 h. A gradual elevation of G-CSF mRNA expression up to 24 h was detected by real-time PCR in the livers of Cd-treated mice, but in LPS-treated mice its highest expression was observed in the liver with a rapid increase at 2 h. By in situ hybridization using G-CSF RNA probes, hepatic Kupffer cells were identified as G-CSF-producing cells in the liver. These results indicated that Cd has a characteristic effect of delayed induction of G-CSF in the liver, causing systemic inflammation accompanied by prolonged neutrophilia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cadmium (Cd) is a toxic heavy metal widely distributed in the environment. In addition to its natural origin, increasing emission of Cd into the environment is occurring because of industrial uses, which raises concerns over the hazardous effects on humans (Nordberg et al. 2015). Cd accumulates mainly in the liver and kidneys through Cd-contaminated food, and renal tubular dysfunction develops after chronic exposure. Therefore, people in Cd-polluted areas are at risk of renal injury and itai–itai disease, characterized by osteomalacia and renal anemia (Aoshima 1987; Horiguchi et al. 2010).
In addition, acute Cd toxicity has been observed in workers occupationally exposed to Cd via inhalation, who develop metal fume fever. Although many other metals cause transient and self-limiting metal fume fever, Cd induces relatively severe pulmonary injury consisting of three overlapping inflammatory phrases: edematous, proliferative, and fibrogenic, which can often be fatal (Dunphy 1967; Malaguarnera et al. 2013). Because inhaled Cd is effectively absorbed via the lungs and distributed systemically (Nordberg et al. 2015), the inflammation induced by Cd acute pulmonary exposure is not confined to the lungs. Indeed, leukocytosis accompanied by an elevated neutrophil count in peripheral blood, which is a representative sign of acute systemic inflammation, has often been observed in affected workers (Amdur and Caputi 1953; Beton et al. 1966; Johnson and Kilburn 1983). Animal experiments also showed systemic inflammation associated with neutrophilia after acute Cd exposure, which can be induced by both inhalation (Yamada et al. 1982) and injection (Kataranovski et al. 1999; Horiguchi et al. 2000, 2001) accompanied by lung and liver injury, respectively. These reports indicated that Cd has a strong effect on acute systemic inflammation involving neutrophilia. However, the mechanism of Cd-induced neutrophilia has not yet been well documented.
Many neutrophils exist in the bone marrow as a storage pool, but only a few percent of them are present in the peripheral blood as a circulating pool and in the vessel walls as a marginal pool (Dale 2011). In response to inflammation, neutrophils are mobilized from the pools, leading to neutrophilia. There are several factors that contribute to neutrophilia, such as granulocyte colony-stimulating factor (G-CSF), granulocyte macrophage colony-stimulating factor (GM-CSF), interleukin (IL)-1, IL-3, and tumor necrosis factor (TNF). Among these, G-CSF, which enhances the production, mobilization, and survival of neutrophils to regulate the number of circulating cells, plays a central role in the process of neutrophilia (Bugl et al. 2012; Bendall and Bradstock 2014). Diverse pro-inflammatory agents, including lipopolysaccharide (LPS), TNF, and IL-1, stimulate G-CSF production from monocytes or mesodermal cells to induce neutrophilia (Demetri and Griffin 1991). However, the involvement of G-CSF in Cd-induced neutrophilia has not yet been reported, although Cd is known to induce inflammatory cytokines, such as TNF and IL-8 (Horiguchi et al. 1993; Dong et al. 1998).
In this study, to elucidate the mechanism of Cd-induced neutrophilia, we observed the elevation of G-CSF mRNA expression levels in organs as well as serum G-CSF in mice after a single administration of Cd and their relationship with neutrophilia. We further compared their expression patterns of time course with those of mice treated with LPS, which is often used to induce general acute inflammation concomitant with neutrophilia (Zhang et al. 2005), as a positive control to characterize Cd-induced acute inflammation relevant to neutrophils.
Methods
Animals and treatments
These experiments were carried out under the supervision of the Animal Research Committee in accordance with the Guidelines on Animal Experiments of Jichi Medical University and the Animal Protection and Management Law (No. 105). Female BALB/c mice aged 8 weeks were used for experiments after a 1-week acclimation period. Mice were injected with Cd as CdCl2 (Wako Pure Chemical Industries, Osaka, Japan) at 2.5 mg/kg i.p., which was dissolved in Milli-Q water, filtered through a Millex-Millipore® 0.45-µm membrane filter (Merck Millipore, Billerica, MA) and then adjusted to 200 µL with sterile, pyrogen-free saline (Otsuka Pharmaceutical Co., Tokyo, Japan), or LPS from E. coli 0127:B8 (Sigma-Aldrich Co. LLC., Saint Louis, MO) at 0.5 mg/kg i.p., which was dissolved in saline of the same volume as the Cd solution. In some experiments, mice were injected with polymyxin B (PMB) sulfate (Sigma-Aldrich Co. LLC.) at 10 mg/kg i.p., dissolved in saline, and filtered through a Millex-Millipore® 0.45 µm membrane filter, 1 h before injection of Cd, LPS, or the equivalent volume of saline. After injection of Cd, LPS, or saline, mice were euthanized at the indicated time points within 24 h. Peripheral blood was collected from the heart under diethyl ether anesthesia; then, the liver, kidney, lungs, and spleen were removed. Peripheral blood was taken with heparin to obtain whole blood and plasma samples and without heparin followed by standing at 4 °C for more than 6 h and centrifugation to obtain serum.
Hematological analyses of peripheral blood
The whole blood sample had EDTA added to determine the white blood cell (WBC) count using a fully automatic blood cell counter, PCE-210 (ERMA, Tokyo, Japan). A smear specimen of whole blood on a glass slide was stained with May–Giemsa solution; then, differential leukocyte analysis was performed by counting 100 WBCs. Polymorphonuclear cell (PMN) count was calculated from the percentage of PMN and the total WBC count.
Measurements of serum G-CSF
We measured G-CSF levels in serum samples of mice using an enzyme-linked immunosorbent assay (ELISA) with a commercially available Quantikine kit (R&D Systems, Minneapolis, MN) in accordance with manufacturer’s instructions. Both samples and standards were tested in duplicate. Optical densities were determined using an iMark™ microplate absorbance reader (Bio-Rad Laboratories, Hercules, CA) at 450 nm with a correction wavelength at 540 nm. According to the manufacturer for the G-CSF ELISA, the intra-assay and inter-assay coefficients of variation were 3.6–6.2 % and 6.3–8.2 %, respectively, and the minimum detectable dose was less than 5 pg/mL.
Measurement of serum transaminases
Plasma levels of glutamic oxaloacetic transaminase (GOT) and glutamate pyruvate transaminase (GPT) in mice were measured using Japan Society of Clinical Chemistry (JSCC) transferable methods (Mitsubishi Chemical Medience Corporation, Tokyo, Japan).
Real-time PCR
Five-hundred nanograms of total RNA, purified from 100 mg tissue samples of liver, kidney, lung, and spleen using TRIzol reagent (Invitrogen, Carlsbad, CA) or from 750 µL whole blood samples using TRIzol LS reagent (Invitrogen), was reverse transcribed into complementary DNA using a PrimeScript RT reagent kit (TaKaRa, Tokyo, Japan). Then real-time PCR was carried out with the RT products using SYBR Premix Ex Taq (TaKaRa) and a primer pair specific for the mouse G-csf gene (GenBank accession no. NM_009971.1) or reference GAPDH (glyceraldehyde 3-phosphate dehydrogenase) gene (GenBank accession no. NM_001001303) using the TP800 Thermal Cycler Dice Real-Time System (TaKaRa). The sequences of the primers were as follows: forward G-csf, 5′-CCC ACC TTG GAC TTG CTT CAG-3′; reverse G-csf, 5′-AGG TAC GAA ATG GCC AGG ACA C-3′; forward GAPDH, 5′-AAA TGG TGA AGG TCG GTG TG-3′; reverse GAPDH, 5′-TGA AGG GGT CGT TGA TGG-3′. After the reaction, the initial amounts of DNA template of the target and reference genes were calculated from the standard curve from the CT (threshold cycle) values; then, the relative gene expression was obtained by dividing that of the target gene by the reference.
In situ hybridization
For in situ hybridization (ISH), whole mice were perfused with G-Fix (Genostaff Co., Ltd., Tokyo, Japan) under anesthesia, and then, the liver was removed and embedded in paraffin using G-Nox (Genostaff). Paraffin blocks of the liver were sectioned at 6 µm and placed onto glass slides. For ISH, a digoxigenin-labeled anti-sense RNA probe for G-csf (named G-Csf-1) was prepared using DIG RNA Labeling Mix (Roche Diagnostics, Nutley, NJ). The sequence of the probe was as follows: 5′-CCC AGA GGC GCA TGA AGC TAA TGG CCC TGC AGC TGC TGC TGT GGC AAA GTG CAC TAT GGT CAG GAC GAG AGG CCG TTC CCC TGG TCA CTG TCA GCG CTC TGC CAC CAT CCC TGC CTC TGC CCC GAA GCT TCC TGC TTA AGT CCC TGG AGC AAG TGA GGA AGA TCC AGG CCA GCG GCT CGG TGC TGC TGG AGC AGT TGT GTG CCA CCT ACA AGC TGT GTC ACC CCG AGG AGC TGG TGT TGC TGG GCC ACT CTC TGG GGA TCC CGA AGG CTT CCC TGA GTG GCT GCT CTA GCC AGG CCC TGC AGC AGA CAC AGT GCC TAA GCC AGC TCC ACA GTG GGC TCT GCC TCT ACC AAG GTC TCC TGC AGG CTC TAT CGG GTA TTT CCC CTG CCC TGG CCC CCA CCT TGG ACT TGC TTC AGC TGG ATG TTG CCA ACT TTG CCA CCA CCA TCT GGC AGC AGA TGG AAA ACC TAG GGG TGG CCC CTA CTG TGC AGC CCA CAC AGA GCG CCA TGC CAG CCT TCA CTT CT-3′. ISH was performed using an ISH Reagent Kit (Genostaff) in accordance with manufacturer’s instructions. After tissue sections were de-paraffinized and treated with Proteinase K (Wako Pure Chemical Industries), hybridization was performed with the probe at concentrations of 300 ng/mL in G-Hybo for 16 h at 60 °C. After hybridization, the sections were incubated with anti-DIG AP conjugate (Roche Diagnostics) with G-Block. Coloring reactions were performed with NBT/BCIP solution (Sigma-Aldrich Co. LLC.) overnight. The sections were counterstained with Kernechtrot stain solution (Muto Pure Chemicals Co., Ltd., Tokyo, Japan) and mounted with G-Mount.
Immunohistochemistry
Immunohistochemistry (IHC) was performed for the same sections as ISH as a second staining. After blocking endogenous peroxidase with G-Block and avidin/biotin blocking kit (Vector, Burlingame, CA), the sections were incubated with anti-ionized calcium binding adapter molecule 1 (Iba1) rabbit polyclonal antibody (Wako Pure Chemical Industries) or negative control rabbit immunoglobulin fraction (Dako, Carpinteria, CA) at 4 °C overnight. Next, they were incubated with biotin-conjugated anti-rabbit Ig (Dako), followed by the addition of peroxidase-conjugated streptavidin (Nichirei, Tokyo, Japan). Peroxidase activity was visualized using diaminobenzidine (Dojindo, Kumamoto, Japan). The sections were counterstained with Kernechtrot stain solution (Muto Pure Chemicals Co., Ltd.), and mounted with G-Mount.
Pathological examinations
Samples of liver were immediately washed by manual infusion of freshly prepared 4 % paraformaldehyde and subsequent agitation overnight at 4 °C. The samples were embedded in paraffin; then, the paraffin blocks were sliced, placed onto glass slides, and stained with hematoxylin and eosin after deparaffinization.
Measurement of Cd concentrations in blood and organs
The samples of whole blood, plasma, liver, and kidney were digested with an acid mixture (HNO3, HClO4, and H2SO4) on a hot plate at 130–200 °C. After resuspension of the residues in Milli-Q water, the Cd concentration was analyzed by flameless atomic absorption spectrometry, using a Z-9000 Polarized Zeeman Atomic Absorption Spectrophotometer (Hitachi, Tokyo, Japan).
Statistics
Data that followed a normal or log-normal distribution are presented as arithmetic means or geometric means, respectively, and the latter were converted into base-10 logarithms before the following analyses. Student’s or Welch’s t test was applied for the comparison between two groups. For comparison among more than two mice groups, the significance of differences was examined by one-way ANOVA or the Kruskal–Wallis test, or multiple comparison methods such as the Tukey–Kramer, Games–Howell, or Dunnett test.
Results
WBC and PMN counts in peripheral blood
First, we observed time-dependent changes in WBC and PMN counts in peripheral blood of mice after injection of Cd or LPS over 24 h and compared them between these treatments. After injection of Cd, PMN counts increased steadily until 24 h, whereas WBC counts did not change at first followed by an increase in parallel with PMN counts (Fig. 1a). On the other hand, LPS injection induced a more rapid increase in WBC and PMN counts than Cd injection until 12 h, with decreasing PMN counts until 24 h (Fig. 1b).
White blood cell (WBC) and polymorphonuclear cell (PMN) counts in peripheral blood of mice injected with cadmium (Cd) at 2.5 mg/kg i.p. (a) or lipopolysaccharide (LPS) at 0.5 mg/kg i.p. (b) at the indicated time points. Data are presented as arithmetic mean values with SD bars. The number of mice in the groups was 13–17. “Asterisk” differs significantly from the group at 0 h without Cd or LPS injection (p < 0.05, Tukey–Kramer or Games–Howell test)
Serum G-CSF levels
We examined the serum levels of G-CSF in mice injected with Cd and compared with those injected with LPS. In Cd-treated mice, the serum G-CSF level increased gradually to reach a plateau at 12–18 h, which then decreased at 24 h (Fig. 2a), whereas LPS-treated mice showed a marked increase, reaching a peak at 2–3 h. The level was more than six times higher than that in Cd-treated mice and then decreased gradually, even to levels less than those of Cd-treated mice at 24 h (Fig. 2b). We also examined serum GM-CSF levels, another hematopoietic agent for neutrophils (Metcalf et al. 1987). The Cd-treated mice showed no detectable levels of GM-CSF for 24 h, whereas we detected an increase in GM-CSF in the serum from mice 2 h after the injection of LPS (geometric mean 19.3 pg/mL, N = 8).
Serum levels of granulocyte colony-stimulating factor (G-CSF) of mice injected with cadmium (Cd) at 2.5 mg/kg i.p. (a) or lipopolysaccharide (LPS) at 0.5 mg/kg i.p. (b) at the indicated time points. Data are presented as geometric mean values with 25th and 75th percentile bars. The number of mice in the groups was 7–9. “Asterisk” differs significantly from the group at 0 h without Cd or LPS injection (p < 0.05, Games–Howell test)
To confirm that the Cd solution used was not contaminated with endotoxin, we pretreated mice with PMB, a cationic antibiotic with high affinity to lipid A of the LPS molecule to neutralize its biological effects (Morrison and Jacobs 1976). Although PMB reduced the elevated serum levels of G-CSF in LPS-treated mice by half to 1/10, it did not counteract, but enhanced the increase in serum G-CSF levels of Cd-treated mice (Table 1), indicating no significant contamination of endotoxin in the Cd solution.
G-CSF mRNA expression in organs
To clarify the origin of the Cd-induced production of G-CSF in mice, we measured mRNA expression of G-CSF in the organs by real-time PCR, in comparison with that of LPS-treated mice. We detected a gradual elevation of G-CSF mRNA expression until 24 h in the liver of Cd-treated mice (Table 2). In contrast, LPS-treated mice showed a strong and rapid increase in hepatic G-CSF mRNA expression, reaching a peak at 2 h, followed by a gradual decrease. On the other hand, there were no significant elevations of G-CSF mRNA expression in the kidney, lung, or spleen of Cd-treated mice, whereas early elevations were detected in the organs of LPS-treated mice (Fig. 3). There were almost no changes in G-CSF mRNA expression in peripheral blood in mice after injection of Cd or LPS (data not shown).
mRNA expression levels of granulocyte colony-stimulating factor (G-CSF) in the kidney (a), lung (b), and spleen (c) of mice injected with cadmium (Cd) at 2.5 mg/kg i.p. or lipopolysaccharide (LPS) at 0.5 mg/kg i.p. at the indicated time points. Data are presented as geometric mean values. The number of mice in all groups was 10. “Asterisk” differs significantly from the group at 0 h without Cd or LPS injection (p < 0.05, Dunnett test)
G-CSF-producing cells in the liver
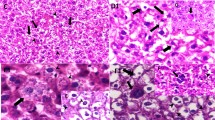
We further investigated which cells produced G-CSF in the liver of mice injected with Cd or LPS by ISH using G-CSF RNA probes, at 2 and 12 h (Fig. 4a, b). This corresponded to when the LPS- and Cd-induced hepatic expression of G-CSF mRNA peaked, respectively. The cells that existed in sinusoids showed expression of G-CSF mRNA, suggesting that hepatic Kupffer cells, resident macrophages, would produce G-CSF by Cd or LPS. To confirm that, we performed double staining with ISH and IHC using a specific antibody against macrophages, Iba1 (Imai et al. 1996), on the livers of mice (Fig. 5). G-CSF mRNA-expressing cells corresponded to cells that were stained with Iba1, indicating that they were Kupffer cells.
In situ hybridization using sense and anti-sense probes, G-Csf-1, for mRNA expression of granulocyte colony-stimulating factor (G-CSF) in the livers of mice injected with saline, cadmium (Cd) at 2.5 mg/kg i.p., or lipopolysaccharide (LPS) at 0.5 mg/kg i.p. at 2 h (a) and 12 h (b). The sites of G-CSF mRNA expression were colored blue by NBT/BCIP and counterstained with Kernechtrot stain. The magnification is ×400 (color figure online)
Double staining with in situ hybridization (ISH) and following immunohistochemistry (IHC) of the livers of mice injected with cadmium (Cd) at 2.5 mg/kg i.p. or lipopolysaccharide (LPS) at 0.5 mg/kg i.p. at 2 and 12 h. ISH was done with an anti-sense probe, G-Csf-1, for mRNA expression of granulocyte colony-stimulating factor (G-CSF), and IHC with a macrophage-specific anti-ionized calcium binding adapter molecule 1 (Iba1) rabbit polyclonal antibody. The former was colored blue by NBT/BCIP and the latter brown by DAB, counterstained with Kernechtrot stain. The arrowheads indicate Kupffer cells stained with ISH and IHC. The magnification is ×400 (color figure online)
Cd distribution in mice
We measured Cd levels in peripheral blood and organs of mice injected with Cd to observe the relationship between its distribution and G-CSF production in the liver. 1 h after Cd injection, Cd was detected in peripheral blood, and the plasma level was two times higher than the whole blood level, indicating almost all Cd existed in plasma since the volume of plasma was half of the whole blood (Fig. 6a). At 3 h after Cd injection, the plasma Cd level decreased to about one-twentieth, with the same level in whole blood. After that, Cd in whole blood remained at the same levels until 24 h, whereas plasma Cd decreased gradually. On the other hand, Cd levels in the liver and kidney, the former being three-times higher than the latter, did not show large changes after being detected as early as at 1 h after injection (Fig. 6b). These results suggested that Cd, after i.p. injection, appeared in plasma, and then promptly move to organs, mainly the liver, followed by reaching a steady state of distribution in the body.
Cadmium (Cd) concentrations in peripheral whole blood and plasma (a), and liver and kidney (b) of mice injected with Cd at 2.5 mg/kg i.p. at the indicated time points. Data are presented as arithmetic mean values with SD bars. The number of mice in the groups was 15–16. Cd concentrations in the blood and organs of mice at 0 h without Cd injection were all less than the detection limit. There were significant differences in Cd concentrations in blood and organs between time points (p < 0.05, Kruskal–Wallis test (a) or one-way ANOVA (b))
Liver injury by Cd
We examined liver injury in mice injected with Cd or LPS by measuring plasma GOT and GPT, and pathological examinations. In mice injected with Cd, plasma GOT and GPT levels increased time dependently in a two-phase pattern before and after 12 h (Fig. 7a). On the other hand, mice injected with LPS showed slight increases in plasma GOT and GPT levels at 12 h followed by decreases to the initial level at 24 h (Fig. 7b). Pathological examinations of the livers of Cd-treated mice at 24 h detected necrosis of hepatocytes along with infiltration of neutrophils, suggesting persistent injury, while the liver was not significantly affected by LPS (Fig. 8).
Plasma levels of glutamic oxaloacetic transaminase (GOT) and glutamate pyruvate transaminase (GPT) in mice injected with cadmium (Cd) at 2.5 mg/kg i.p. (a) or lipopolysaccharide (LPS) at 0.5 mg/kg i.p. (b) at the indicated time points. Data are presented as geometric mean values with 25th and 75th percentile bars. The number of mice in the groups was 12–17. “Asterisk” differs significantly from the group at 0 h without Cd or LPS injection (p < 0.05, Tukey–Kramer or Games–Howell test)
Discussion
We first observed that a single injection of Cd into mice-induced neutrophilia that occurred slowly but continued to increase until 24 h, in contrast to LPS, which rapidly induced neutrophilia with a peak at 12 h followed by a decrease. Then, we demonstrated increases in serum G-CSF levels in mice after injection of Cd or LPS, the time-dependent patterns of which were consistent with those of neutrophilia. The peaks of serum G-CSF levels after Cd and LPS injections were at 12–18 and 2–3 h, respectively, followed by increases in neutrophil counts after similar time lags. In addition, the time-dependent patterns of hepatic expression of G-CSF mRNAs in Cd- and LPS-treated mice corresponded with those of serum G-CSF levels. These results indicated that Cd-induced acute systemic inflammation is characterized by prolonged neutrophilia, which is ascribed to the delayed production of G-CSF.
In this study, we focused on the acute effects of Cd on systemic inflammation and limited observations up to 24 h, which was enough to detect the characteristic G-CSF production in Cd-treated mice, reaching its maximum at 12–18 h. Cd-induced neutrophilia did not peak within 24 h, but it was estimated that the peripheral PMN count would decrease after 24 h, because serum G-CSF started to decrease at 24 h. Our previous study on the subacute effects of Cd to induce neutrophilia in rabbits showed a peak at 24 h, followed by a gradual decrease until 4 days (Horiguchi et al. 2001). On the other hand, hepatic G-CSF mRNA expression in Cd-treated mice continued to elevate until 24 h despite the serum G-CSF level peaking before, suggesting that a translational mechanism was involved. Further studies will be necessary.
The characteristic slow elevation of serum G-CSF by Cd indicates that a mechanism different from LPS might be involved in the Cd-induced production of G-CSF. Compared with a single, strong induction of G-CSF by LPS, there seemed to be two phases in Cd-induced G-CSF induction, being composed of an initial weaker induction and the subsequent stronger one (Fig. 2a, Table 2). The fast, strong induction of G-CSF by LPS may be derived from various effects on cells, such as interacting with the LPS binding protein (LBP), CD14, MD-2 and toll-like receptor 4 (TLR4), and activating nuclear factor-κB (NF-κB) (Lu et al. 2008; Chang et al. 2015), or increasing G-CSF mRNA stability (Demetri and Griffin 1991). Therefore, Cd may induce G-CSF in a similar, but weaker, manner to LPS in the early phase. Indeed, it has been reported that Cd activates NF-κB to induce various inflammatory mediators in monocytes (Freitas and Fernandes 2011), although the cellular effects involved in G-CSF induction by Cd are not yet known.
In contrast, the delayed production of G-CSF by Cd in the later phase suggests that Cd-induced G-CSF secondarily after direct cellular effects. One plausible explanation for its mechanism is the time-dependent toxic effect of Cd on hepatocytes, which also followed a biphasic pattern of moderate elevation of hepatic transaminases in the early phase and higher elevation in the later phase (Fig. 7a). Indeed, it was postulated that early apoptosis is followed by necrosis in the process of Cd-induced acute liver injury in mice in a previous report (Habeebu et al. 1998). In general, the debris released from necrotic cells can stimulate surrounding tissues to induce various inflammatory mediators, which activate hepatic Kupffer cells. These secondary inflammatory responses following the injury of hepatocytes induced by Cd toxicity may enhance induction of G-CSF additively in the later phase.
It has been noted that Cd-induced G-CSF production in mice was enhanced by PMB, although its mechanism is as yet unknown. PMB also increased G-CSF production in saline-treated mice, indicating that PMB itself can induce G-CSF. It was observed previously that PMB induced TNF-α in macrophages without any treatment (Turner et al. 2009), suggesting that PMB induces several inflammation-related cytokines. Therefore, Cd-induced G-CSF production might be synergistically increased by PMB treatment.
G-CSF mRNA expression in Cd-treated mice was only detected in the liver, indicating that the liver is the main organ for G-CSF production in response to acute Cd exposure. In LPS-treated mice, hepatic G-CSF mRNA levels were much higher than in other organs, suggesting that the liver is the most effective organ for G-CSF production. In addition, injected Cd was rapidly distributed to the liver and accumulated there most among all organs examined, which was also reported in a previous study (Nordberg et al. 2015). These results indicated that the highest concentration of Cd was present in the liver, which has the highest capacity to produce G-CSF, and this may be why G-CSF mRNA expression was limited to the liver after Cd exposure.
In the liver, Kupffer cells not only eliminate endotoxin from the intestines as hepatic resident macrophages but also play a central role in inflammatory responses (Roberts et al. 2007). In this study, hepatic Kupffer cells in the sinusoid were identified as G-CSF-expressing cells in both Cd- and LPS-treated mice by double staining of ISH for G-CSF mRNA expression and IHC for macrophages. This is a reasonable result because monocytes and macrophages are well known to be prominent sources of G-CSF production in response to LPS and other stimulants, such as IL-1 and TNF (Demetri and Griffin 1991; Sallerfors 1994), and a number of inflammatory mediators, such as cytokines, adhesion molecules, and chemokines, are produced in macrophages in response to Cd (Rikans and Yamano 2000). However, endothelial cells and fibroblasts, which are reported to produce G-CSF in response to LPS, may also produce G-CSF in response to Cd exposure. Further studies will be necessary.
In conclusion, Cd-induced neutrophilia along with elevation of serum G-CSF and the expression of G-CSF mRNA in hepatic Kupffer cells in mice, which were slow and prolonged compared with LPS-induced elevation, indicating that Cd has a characteristic effect of delayed induction of G-CSF in the liver to cause systemic inflammation accompanied by prolonged neutrophilia. The results of this study will contribute to the further understanding of systemic inflammation caused by acute Cd toxicity that has been observed in workers as well as future investigations on the basic physiology of G-CSF.
References
Amdur ML, Caputi RA (1953) Cadmium intoxication: clinical report of an acute accidental group exposure. Ind Med Surg 22:561–566
Aoshima K (1987) Epidemiology of renal tubular dysfunction in the inhabitants of a cadmium-polluted area in the Jinzu River basin in Toyama Prefecture. Tohoku J Exp Med 152:151–172
Bendall LJ, Bradstock KF (2014) G-CSF: from granulopoietic stimulant to bone marrow stem cell mobilizing agent. Cytokine Growth Factor Rev 25:355–367
Beton DC, Andrews GS, Davies HJ, Howells L, Smith GF (1966) Acute cadmium fume poisoning. Five cases with one death from renal necrosis. Br J Ind Med 23:292–301
Bugl S, Wirths S, Müller MR, Radsak MP, Kopp HG (2012) Current insights into neutrophil homeostasis. Ann N Y Acad Sci 1266:171–178
Chang SF, Lin SS, Yang HC, Chou YY, Gao JI, Lu SC (2015) LPS-induced G-CSF expression in macrophages is mediated by ERK2, but not ERK1. PLoS ONE 10:e0129685
Dale DC (2011) Neutropenia and neutrophilia. In: Kaushansky K, Lichtman M, Beutler E, Kipps T, Prchal J, Seligsohn U (eds) Williams hematology, 8th edn. McGraw-Hill, New York, pp 939–950
Demetri GD, Griffin JD (1991) Granulocyte colony-stimulating factor and its receptor. Blood 78:2791–2808
Dong W, Simeonova PP, Gallucci R, Matheson J, Flood L, Wang S, Hubbs A, Luster MI (1998) Toxic metals stimulate inflammatory cytokines in hepatocytes through oxidative stress mechanisms. Toxicol Appl Pharmacol 151:359–366
Dunphy B (1967) Acute occupational cadmium poisoning. A critical review of the literature. J Occup Med 9:22–26
Freitas M, Fernandes E (2011) Zinc, cadmium and nickel increase the activation of NF-κB and the release of cytokines from THP-1 monocytic cells. Metallomics 3:1238–1243
Habeebu SS, Liu J, Klaassen CD (1998) Cadmium-induced apoptosis in mouse liver. Toxicol Appl Pharmacol 149:203–209
Horiguchi H, Mukaida N, Okamoto S, Teranishi H, Kasuya M, Matsushima K (1993) Cadmium induces interleukin-8 production in human peripheral blood mononuclear cells with the concomitant generation of superoxide radicals. Lymphokine Cytokine Res 12:421–428
Horiguchi H, Harada A, Oguma E, Sato M, Homma Y, Kayama F, Fukushima M, Matsushima K (2000) Cadmium-induced hepatic injury is exacerbated in human interleukin-8 transgenic mice. Toxicol Appl Pharmacol 163:231–239
Horiguchi H, Oguma E, Kayama F, Satoh M, Fukushima M (2001) Dexamethasone prevents acute cadmium-induced hepatic injury but exacerbates kidney dysfunction in rabbits. Toxicol Appl Pharmacol 174:225–234
Horiguchi H, Aoshima K, Oguma E, Sasaki S, Miyamoto K, Hosoi Y, Katoh T, Kayama F (2010) Latest status of cadmium accumulation and its effects on kidneys, bone, and erythropoiesis in inhabitants of the formerly cadmium-polluted Jinzu River Basin in Toyama, Japan, after restoration of rice paddies. Int Arch Occup Environ Health 83:953–970
Imai Y, Ibata I, Ito D, Ohsawa K, Kohsaka S (1996) A novel gene iba1 in the major histocompatibility complex class III region encoding an EF hand protein expressed in a monocytic lineage. Biochem Biophys Res Commun 224:855–862
Johnson JS, Kilburn KH (1983) Cadmium induced metal fume fever: results of inhalation challenge. Am J Ind Med 4:533–540
Kataranovski M, Popovic S, Kataranovski D (1999) Differential effects of in vivo cadmium administration on lymphocytes and granulocytes in rats. Vet Hum Toxicol 41:200–204
Lu YC, Yeh WC, Ohashi PS (2008) LPS/TLR4 signal transduction pathway. Cytokine 42:145–151
Malaguarnera M, Drago F, Malaguarnera G, Li Volti G, Salomone S, Caraci F, Galvano F, Vacante M, Bucolo C, Malaguarnera M (2013) Metal fume fever. Lancet 381(9885):2298
Metcalf D, Begley CG, Williamson DJ, Nice EC, De Lamarter J, Mermod JJ, Thatcher D, Schmidt A (1987) Hemopoietic responses in mice injected with purified recombinant murine GM-CSF. Exp Hematol 15:1–9
Morrison DC, Jacobs DM (1976) Binding of polymyxin B to the lipid A portion of bacterial lipopolysaccharides. Immunochemistry 13:813–818
Nordberg GF, Nogawa K, Nordberg M (2015) Cadmium. In: Nordberg GF, Fowler BA, Nordberg M (eds) Handbook on the Toxicology of Metals, 4th edn. Academic Press, Burlington, pp 667–716
Rikans LE, Yamano T (2000) Mechanisms of cadmium-mediated acute hepatotoxicity. J Biochem Mol Toxicol 14:110–117
Roberts RA, Ganey PE, Ju C, Kamendulis LM, Rusyn I, Klaunig JE (2007) Role of the Kupffer cell in mediating hepatic toxicity and carcinogenesis. Toxicol Sci 96:2–15
Sallerfors B (1994) Endogenous production and peripheral blood levels of granulocyte-macrophage (GM-) and granulocyte (G-) colony-stimulating factors. Leuk Lymphoma 13:235–247
Turner JJ, Smolinska MJ, Sacre SM, Foxwell BM (2009) Induction of TLR tolerance in human macrophages by adiponectin: Does LPS play a role? Scand J Immunol 69:329–336
Yamada H, Damiano VV, Tsang AL, Meranze DR, Glasgow J, Abrams WR, Weinbaum G (1982) Neurtrophil degranulation in cadmium-chloride-induced acute lung inflammation. Am J Pathol 109:145–156
Zhang P, Quinton LJ, Gamble L, Bagby GJ, Summer WR, Nelson S (2005) The granulopoietic cytokine response and enhancement of granulopoiesis in mice during endotoxemia. Shock 23:344–352
Acknowledgments
This work was supported by a Grant-in-Aid for Scientific Research (C) (No. 15590519) from the Ministry of Education, Science, and Culture of Japan. This publication was subsidized by JKA through its promotion funds from KEIRIN RACE. We thank Prof. Fujio Kayama of Jichi Medical University for financial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Horiguchi, H., Oguma, E. Acute exposure to cadmium induces prolonged neutrophilia along with delayed induction of granulocyte colony-stimulating factor in the livers of mice. Arch Toxicol 90, 3005–3015 (2016). https://doi.org/10.1007/s00204-016-1661-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-016-1661-7