Abstract
Primary human hepatocytes (PHH) are the “gold standard” for in vitro toxicity tests. However, 2D PHH cultures have limitations that are due to a time-dependent dedifferentiation process visible by morphological changes closely connected to a decline of albumin production and CYP450 activity. The 3D in vitro culture corresponds to in vivo-like tissue architecture, which preserves functional characteristics of hepatocytes, and therefore can at least partially overcome the restrictions of 2D cultures. Consequently, several drug toxicities observed in vivo cannot be reproduced in 2D in vitro models, for example, the toxic effects of acetaminophen. The objective of this study was to identify molecular differences between 2D and 3D cultivation which explain the observed toxicity response. Our data demonstrated an increase in cell death after treatment with acetaminophen in 3D, but not in 2D cultures. Additionally, an acetaminophen concentration-dependent increase in the CYP2E1 expression level in 3D cultures was detected. However, during the treatment with 10 mM acetaminophen, the expression level of SOD gradually decreased in 3D cultures and was undetectable after 24 h. In line with these findings, we observed higher import/export rates in the membrane transport protein, multidrug resistance-associated protein-1, which is known to be specific for acetaminophen transport. The presented data demonstrate that PHH cultured in 3D preserve certain metabolic functions. Therefore, they have closer resemblance to the in vivo situation than PHH in 2D cultures. In consequence, 3D cultures will allow for a more accurate hepatotoxicity prediction in in vitro models in the future.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Primary human hepatocytes (PHH) are considered to be the “gold standard” for in vitro toxicity tests (Hewitt et al. 2007; Gomez-Lechon et al. 2008). It has been proven that their functionality depends on their polarization. In contrast to other epithelial polarized cells which only dispose of one apical pole, hepatocytes possess several apical and basolateral membranes (Decaens et al. 2008). The apical membrane faces the bile canaliculi, while the basolateral membrane faces the endothelial cells of the blood vessels in the hepatic sinusoids. Culturing freshly isolated PHH in conventional 2D will cause morphological alterations that are provoked by an epithelial–mesenchymal transition (EMT) during which the PHH lose cell polarity and their specific liver functions (Godoy et al. 2009).
One of the most important functions of PHH is the metabolization of xenobiotic and endobiotic substances. This metabolization is composed of three different phases: Phase I reactions involve hydrolyses, reductions and oxidations (Lin et al. 2012). The latter are mainly performed by the cytochrome P450 enzyme family (Suzuki et al. 2002). Phase II reactions are based on conjugation reactions that are performed by transferases which introduce large water-soluble groups in order to facilitate excretion (Eckl and Bresgen 2003) via transporter proteins located at the apical and basolateral membranes of the hepatocytes (phase III). Moreover, transport proteins are responsible for the uptake of xenobiotic and endobiotic substances into the hepatocytes (Kock and Brouwer 2012). Some of the major membrane transporter proteins are gathered in the ATP-binding cassette (ABC) family, which is composed of different subfamilies such as ABCA, ABCB (ABCB1/MRD1/P-gp; ABCB4/MDR3; ABCB11/BSEP), ABCC (ABCC1/MRP1; ABCC2/MRP2; ABCC3/MRP3), ABCD, ABCE, ABDF and ABCG (white) (Glavinas et al. 2004; Hirano et al. 2005). One feature of the MRPs is their substance specificity: Multidrug resistance-associated protein-1 (MRP1), for example, is among other factors responsible for the transport of acetaminophen (Aleksunes et al. 2007).
Acetaminophen is a drug that is used all over the world and has analgesic and antipyretic properties. It has been shown that acetaminophen is safe when it is used at therapeutic doses (Espinosa Bosch et al. 2006; Hinson et al. 2010). But an overdosage can cause acute liver failure (Larson et al. 2005). In PHH, acetaminophen is mainly metabolized by the cytochromes P450 2E1 and 1A2 (phase I) to the highly toxic product N-acetyl-p-benzoquinone imine (NAPQI) (Zaher et al. 1998; Ullrich et al. 2006). This electrophilic metabolite can bind to several nucleophilic groups in proteins, RNA and DNA (Gonzalez 2005). Therefore, NAPQI is detoxified by binding to reduced glutathione (GSH) (phase II). The inactivated metabolite will be eliminated via the urine. However, at higher concentrations, glutathione, which impairs the inactivation of NAPQI, is depleted. NAPQI then binds to intracellular proteins causing hepatocyte necrosis (Fontana 2008).
In conventional in vitro toxicity tests (2D) for acetaminophen, PHH only display signs of intoxication at very high drug concentrations (5–20 mM) (Prot et al. 2011), while in in vivo, significantly lower concentrations (0.5–1 mM) already cause liver necrosis (Bruschi 2004). This discrepancy between in vivo and in vitro observations highlights the importance of understanding the involved intracellular mechanisms, in order to establish in vitro liver models that are able to reproduce the in vivo tissue situation.
Materials and methods
Acetaminophen was purchased from Sigma Aldrich (Munich, Germany). Fetal calf serum (FCS gold), cell culture medium, penicillin, streptomycin, HEPES, pyruvate and phosphate buffered saline (PBS) were obtained from PAA Laboratories GmbH (Pasching, Austria). Collagenase P from Clostridium histolyticum was purchased from Roche (Penzberg, Germany). Human insulin (r-DNS) was obtained from Novo Nordisk (Bagsværd, Denmark) and hydrocortisone from Pfizer (Berlin, Germany). Ethanol was obtained from Merck (Darmstadt, Germany) and DMSO was obtained from Carl Roth (Karlsruhe, Germany). All other chemicals were purchased from Sigma.
Isolation and 2D culture of primary human hepatocytes
Primary human hepatocytes were isolated from liver resections of tumor patients with their informed consent according to the ethical guidelines of the “Klinikum rechts der Isar” and the “Klinikum Neuperlach”, both located in Munich, Germany. A two-step collagenase P perfusion technique was used for the isolation of the PHH (Nussler et al. 2009). Isolated hepatocytes were cultured in Williams’ medium E (10 % FCS, 1 μM insulin, 15 mM HEPES, 0.8 μg/ml hydrocortisone, 100 U/ml penicillin and 100 μg/ml Streptomycin, 1 % l-glutamine, 1 % non-essential amino acids, 1 mM sodium pyruvate) over night on collagen-coated culture plates with a density of 1.5 × 105 cells/cm2. Afterwards, the cells were washed with PBS, the medium was replaced by starvation medium (Williams’ medium E supplemented with 500 μM insulin, 15 mM HEPES, 100 U/ml penicillin and 100 μg/ml streptomycin, 1 % l-glutamine) and the PHH were stimulated according to the experimental setup.
3D culture of primary human hepatocytes
Collagen for cell culture was isolated from rat tail tendons by breaking the skinned tails between every vertebra and pulling the tendons out. The fibers were air-dried and sterilized under UV radiation; 1 g of dried collagen fibers was stirred for 48 h in 300 ml of 1 % acetic acid solution in order to solubilize the collagen; 1:10 volume of 10× DMEM with phenol red (Biochrom, Berlin, Germany) was dissolved in collagen stock solution. The pH was neutralized to 7.2–7.3 with NaOH. Each step was conducted on ice under agitation in order to avoid collagen polymerization. The final collagen concentration was 2 mg/ml; 400 μl of collagen solution was spread into 10 cm2 wells (6-well plates). After the polymerization of the gel, the PHH were seeded onto 6-well plates that have been prepared as described above, with a density of 1.5 × 105 cells/cm2. Following the cell attachment, a second layer of collagen was added.
Dead/alive assay
Primary human hepatocytes in 2D or 3D culture were treated with acetaminophen for 72 h. Then, the cells were incubated for 30 min with 2 μM calcein acetoxymethyl ester (calcein AM) in order to detect living cells and with 4 μM ethidium homodimer in order to detect dead cells (both from Invitrogen, Paisley, UK). Calcein AM is a cell-permeable non-fluorescent dye which is converted into green fluorescent calcein by esterases in the cell cytoplasm (ex/em, 485/530). Ethidium homodimer-1 can only enter cells with damaged membranes. After having intercalated into DNA, it produces a bright red fluorescent signal (ex/em, 530/645 nm). Pictures were taken with an epifluorescence microscope Eclipse TE2000-5 from Nikon (Nikon, Germany). Additionally, the fluorescence was measured with a plate reader (FLUOstar Omega fluorometer, BMG Labtech—Offenburg, Germany).
LDH, AST and ALT assay
In order to evaluate cellular damage, culture supernatants were measured for lactate dehydrogenase (LDH), aspartate aminotransferase (AST) and alanine aminotransferase (ALT) leakage with a commercially available reaction kit (Analyticon Biotechnologies, Lichtenfels, Germany). For reference purposes, absorbance was measured at 570 and 690 nm with a FLUOstar Omega fluorometer, BMG Labtech (Offenburg, Germany).
Western blot
RNA was extracted by the Trifast reagent according to the manufacturer’s guidelines (peqlab, Erlangen, Germany). The cDNA synthesis was performed using the First Strand cDNA Synthesis kit (Thermo Scientific, Sankt Leon-Rot, Germany). The primer sequences were designed using the primer blast program (NM 000773—CYP2E1, and NM 000454.4—SOD1). The appropriate cDNA dilution and PCR cycling numbers were determined in order to ensure that the PCR did not reach saturation. Products were resolved by gel electrophoresis in a 1.5 % (w/v) agarose gel in Tris–borate EDTA and visualized with ethidium bromide. The quantification was carried out with the ImageJ 1.42q software (National Institute of Health, Maryland, USA).
For the Western blot analysis, cells were collected by centrifugation and lysed in 0.5 % Nonidet P40, 100 mM NaCl, 0.5 % Deoxycholic acid, 10 mM EDTA and 10 mM Tris–HCl (pH 7.5) with the Complete Protease Inhibitor Cocktail (Roche, Mannheim, Germany) for 30 min. Lysates were centrifuged at 10,000×g for 10 min at 4 °C. Protein concentration was determined by micro-Lowry as described above (Lowry et al. 1951). The proteins were separated by SDS-PAGE and transferred to nitrocellulose membranes (Carl Roth, Karlsruhe, Germany). Membranes were blocked for 1 h with 5 % semi-skimmed milk in 0.1 % Tween-20/PBS and incubated over night with a primary antibody against SOD-1 (mouse monoclonal antibody, Santa Cruz, Heidelberg, Germany), CYP2E1 and GAPDH (both rabbit polyclonal antibodies, Santa Cruz, Heidelberg, Germany). Proteins were visualized using secondary antibodies conjugated to horseradish peroxidase. Membranes were exposed to X-ray films and developed in a Curix 60 Developing processor (Agfa, Cologne, Germany). All primary antibodies were diluted at a ratio of 1:1,000, and all secondary antibodies at a ratio of 1:5,000 in 1 % semi-skimmed milk in 0.1 % Tween-20/PBS. Proteins were visualized using secondary antibodies conjugated to horseradish peroxidase. Membranes were exposed to X-ray films and developed in a Curix 60 Developing processor (Agfa, Cologne, Germany). The quantification was carried out with the ImageJ 1.42q software (National Institute of Health, Maryland, USA).
MRP1 gene expression and transport activity
RNA was extracted by the Trifast reagent according to the manufacturer’s guidelines (peqlab, Erlangen, Germany). The cDNA synthesis was performed using the First Strand cDNA Synthesis kit (Thermo Scientific, Sankt Leon-Rot, Germany). The primer sequence was designed using the primer blast program (NM 004996.3). The appropriate cDNA dilution and PCR cycling numbers were determined in order to ensure that the PCR did not reach saturation. Products were resolved by gel electrophoresis in a 1.5 % (w/v) agarose gel in Tris–borate EDTA and visualized with ethidium bromide. The quantification was carried out with the ImageJ 1.42q software (National Institute of Health, Maryland, USA).
Multidrug resistance-associated protein-1 transport activity was investigated by using a modified carboxyfluorescein (CF) efflux assay (Laupeze et al. 2001). Cells were seeded in 96-well plates; washed 3 times with PBS and incubated with 4 μM of 5(6)-carboxy-2′,7′-dichlorofluorescein diacetate (5-CFDA) for 30 min. The cells were washed 3 times with PBS and a fluorescence measurement was conducted in order to determine the amount of 5-CFDA that had been taken up and metabolized to 5-CFSE by the hepatocytes. The cells were re-incubated in PBS containing 11 mM glucose for 60 min. Supernatants were collected 5, 10, 20, 30 and 60 min after the incubation and transferred to a new 96-well plate in order to determine the amount of 5-CFSE that is eluted by the hepatocytes. The quantification was carried out by using a linear calibration curve of the linear standard curve.
Quantification of acetaminophen
Prior to the LC/MS analysis, the samples were precipitated with twice the volume of acetonitrile supplemented with the internal standard (1 μM griseofulvin). After vigorous shaking (10 min) and centrifugation (5,000×g), the particle-free supernatants were subjected to LC–MS/MS. The HPLC system consisted of an LC Plus pump and an auto sampler (both from Thermo Fisher Scientific, Dreieich, Germany). Mass spectrometry was performed on a TSQ Quantum Discovery Max triple quadrupole mass spectrometer equipped with an electrospray interface (Thermo Fisher Scientific) and connected to a PC with the Xcalibur 2.0.7 standard software. The flow rate of the HPLC pump was set to 600 μl/min and the compounds were separated on a Kinetex PFP, 2.6 μm, 50 × 2.1 mm analytical column (Phenomenex, Aschaffenburg, Germany) with Krudkatcher. The analytes were separated by gradient elution with acetonitrile/0.1 % formic acid as the organic phase (A) and 10 mM ammonium acetate/0.1 % formic acid as the aqueous phase (B) (% A (t (min), 0 (0–0.2)–97 (0.8–1.8)–0 (2.0–4.0)). The MS–MS identification of characteristic fragment ions was performed using the following set of parameters: ion source temperature: 350 °C, capillary voltage: 3.8 kV, collision gas: 0.8 mbar argon, spray and sheath gas: 20 and 8 (arbitrary units), respectively. The stable product ions with the highest S/N ratio were used to quantify the test item in the selected reaction monitoring mode (SRM). The transitions used for the analysis were m/z 152.1 to m/z 65.0 and m/z 93.0 (acetaminophen) and m/z 353.0 to m/z 215.0 (griseofulvin, internal standard).
Statistics
All the experiments were performed at least twice. The results are expressed as mean ± SD. One-way analysis of variance (ANOVA) with Bonferroni’s multiple comparison test or unpaired t test was performed using the GraphPad Prism software (GraphPad Software, San Diego, CA). p < 0.05 was taken as minimum level of significance.
Results
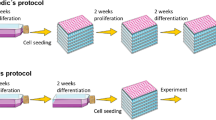
It is well known that PHH that are cultured with the 3D collagen sandwich technique maintain a compact hexagonal shape, whereas cells in 2D cultures rapidly gain a planar and fibroblast-like appearance after having been cultured for several days (Fig. 1).
Acetaminophen toxicity
Preliminary data had shown that the incubation of PHH with 10 mM acetaminophen for 72 h in standard 2D cultures had led to no or only low toxicity (data not shown). Furthermore, the solvent (DMSO or H2O) had no influence on fractional survival and LDH and AST release after the treatment with acetaminophen in 2D culture. However, following a recommendation that had been made in the literature (Arndt et al. 1989), acetaminophen was diluted in water or medium for all future experiments.
Primary human hepatocytes were plated in standard 2D or in 3D sandwich cultures and exposed to different concentrations of acetaminophen for 72 h. An increased number of dead cells were observed in 3D, but not in 2D cultures (Fig. 2a). The quantification of the fluorescence signal revealed that the drug sensitivity was concentration-dependent, as is shown in Fig. 2b. Treatment with 1 mM, 5 mM and 10 mM acetaminophen increased the fluorescence intensity significantly (up to 40, 40 and 50 %, respectively). This corresponded to an increase in dead cells in comparison with untreated cells. Even at 10 mM acetaminophen, no increase in the number of dead cells was detectable in the standard 2D culture.
Acetaminophen treatment in dependence of the culturing technique. Microscopic observation of PHH in standard 2D and in 3D sandwich cultures after the treatment with acetaminophen with varying concentrations for 72 h (a). Quantification of dead cells stained by fluorescent dye (b). The untreated control in each culture condition was set to 1. **p < 0.01; *p < 0.001, N = 3, n = 2
In line with these findings, a concentration-dependent release of LDH (Fig. 3a), AST (Fig. 3b) and ALT (Fig. 3c) was detected in 3D cultures treated with acetaminophen. Acetaminophen incubation in 3D cultures showed a dose-dependent but not statistically significant increase in LDH, AST and ALT levels at 72 h compared to 2D cultures. It is worth noting that the release of LDH, AST and ALT was lower in 2D cultures in the presence of acetaminophen, even after a prolonged cultivation time.
Primary human hepatocytes in 3D culture release more LDH, AST and ALT after the treatment with acetaminophen than cells in 2D culture. PHH in standard 2D or in 3D sandwich culture were treated for 24 and 72 h with different concentrations of acetaminophen. The release of LDH (a), AST (b) and ALT (c) was measured in a fluorescence reader. In each culture condition, the untreated control was set to 1
Acetaminophen influences CYP2E1 and SOD protein levels in 3D culture
CYP2E1 is involved in the formation of NAPQI, the reactive intermediate of acetaminophen. Therefore, the gene and protein expression of CYP2E1 in both culture models after the treatment with acetaminophen was compared. No difference in the gene expression of CYP2E1 between 2D and 3D cultures was detected (Fig. 4a, b). At protein level, only in the 3D culture, a concentration-dependent increase in CYP2E1 was observed (Fig. 4c). The quantification of the Western blot revealed a significant increase in the expression of CYP2E1 after 72 h of up to 230, 260 and 310 % in the presence of 1, 5 and 10 mM acetaminophen in 3D cultures; meanwhile, the protein expression was unaffected in 2D (Fig. 4d). Like CYP2E1, the antioxidant enzyme superoxide dismutase (SOD) showed no difference in the gene expression between 2D and 3D cultures (Fig. 4e, f). However, the SOD protein expression gradually decreased after the treatment with acetaminophen and was undetectable after 24 h of treatment with 10 mM acetaminophen in 3D cultures. SOD expression was unaffected in 2D cultures exposed to acetaminophen.
Gene and protein levels of CYP2E1 and SOD after the treatment with acetaminophen in 2D and 3D cultures. The gene expression of CYP2E1 (a, b) and of SOD (e, f) was detected by semiquantitative PCR. Representative blots from two different experiments at 24 and 72 h are shown. Values are expressed as x-fold of control; one-way ANOVA, *p < 0.05; N = 2. Protein levels of CYP2E1 (c, d) and of (g, h) were detected by Western blot. Representative blots from two different experiments at 72 h are shown. Additionally, the relative gene expression and protein levels were quantified using the ImageJ software. Gene expression and protein levels were normalized to GAPDH. *p < 0.05, **p < 0.01; N = 2
MRP1 gene expression and transport activity
Gene expression of MRP1 in acetaminophen-treated hepatocytes showed significant statistical difference in comparison with the untreated control after 72 h. As we did not observe a statistical difference between 2D and 3D cultures (Fig. 5a, b), we investigated the activity of MRP1 with an elution assay. Hepatocytes were incubated for 30 min with 4 μM of 5-CFDA. 5-CFDA diffuses into the cells where it is cleaved by esterases into carboxyfluorescein succinimidyl ester (CFSE). In hepatocytes, CFSE is exported into the cell culture supernatant by the activity of hepatic transporters (Li et al. 2009). Finally, the elution of 5-CFSE was quantified by collecting the supernatants at different time points. Figure 5c shows the concentrations of diffused 5-CFDA and metabolized into 5-CFSE by hepatic esterases. Interestingly, the amount of 5-CFDA diffused and metabolized into 5-CFSE by hepatocytes in 3D was 260 % higher than in hepatocytes cultured in 2D (p < 0.0001) after 24 h. At 72 h, no statistically significant difference was observed, even though the amount of 5-CFDA diffused and metabolized by hepatocytes into 5-CFSE was higher in 3D cultures than in 2D cultures. As depicted in Fig. 5d, 2D and 3D cultures reached the peak of 5-CF efflux after 30 min. At 24 h, the efflux was 350 % higher in 3D cultures than in their 2D counterparts. However, at 72 h, no efflux was observed in 2D cultures. In 3D cultures, MRP1 showed a different behavior in comparison with 24 h reaching the peak of 5-CF efflux 20 min after incubation.
Transport activity of PHH in 2D and 3D cultures. The gene expression of MRP1 (a, b) was detected by semiquantitative PCR. Representative blots at 24 and 72 h are shown. The relative gene expression was quantified by the ImageJ software. Values are expressed as x-fold of control; one-way ANOVA, *p < 0.05; N = 2. (c) 5-CFDA taken up and metabolized into 5-CF by human primary hepatocytes in monolayer culture and in collagen gel after 24 and 72 h; unpaired t test, ****p < 0.0001. (d) 5-CF eluted by human primary hepatocytes in monolayer culture and in collagen gel through MRP1 after 24 and 72 h; one-way ANOVA, *p < 0.1, ***p < 0.001. Data are mean ± SD; N = 2, n = 4
Metabolism of acetaminophen
The formation rate of the toxic acetaminophen metabolite NAPQI was analyzed by LC/MS. However, as NAPQI is a highly unstable compound, it rapidly disintegrated into the measuring solution. In the hepatocyte samples, NAPQI not only disintegrated but it was also trapped by proteins and other structures, such as GSH (Madsen et al. 2007). However, NAPQI could not be measured by LC/MS. Therefore, although not a direct marker, the loss of acetaminophen was used as a marker for metabolite formation. A representative study on the kinetic metabolic turnover of acetaminophen in 2D and 3D was carried out (Fig. 6). PHH in culture were incubated with acetaminophen (0.25, 0.5, 1, 5 and 10 mM) for 24, 48 and 72 h. The metabolic turnover of acetaminophen at 10 mM was higher in 3D cultures until the end of the incubation. This resulted in lower concentrations of acetaminophen remaining in the cultures (51.79 vs. 73.48 nM after 24 h, 44.84 vs. 62.81 nM after 48 h and 39.46 vs. 50.31 nM after 72 h). At the lower concentrations of acetaminophen incubation (0.25–5 mM), the remaining acetaminophen concentrations were in the same range in 2D and 3D cultures after 48 h (5 mM) and 72 h (0.25–1 mM). Next, an independent experiment with 4 donors and incubation with acetaminophen for 72 h were performed. Differences between 2D and 3D cultures were only detected at high concentrations (10 mM). Although differences between the individual cultures became apparent, no statistically significant difference was observed (data not shown).
Discussion
Hepatic transporters are located in the apical and basolateral membranes of hepatocytes. They play a crucial role in the import of xenobiotic and endobiotic substances into the hepatocytes and in the efflux of the corresponding products after the metabolization by different hepatic enzymes (Eckl and Bresgen 2003). Here, we are describing the relevance of the 3D environment for the culture of PHH in vitro by comparing this technique to the conventional 2D culture method that is used for hepatotoxic prediction. Acetaminophen was used as a model drug for this comparison between both culture methods.
In contrast to 2D cultures, PHH were not transformed in 3D cultures before they were treated with acetaminophen. One possible explanation for this fact is the “artificial” environment to which PHH are exposed in conventional 2D cultures, resulting in an increment of cell stress, hepatic dedifferentiation and subsequent cell death (Hewitt et al. 2007). The most interesting fact was the observation that the exposure to acetaminophen leads to significant cell death in 3D cultures, but not in 2D cultures. This finding resembles results published by Schutte et al. (Schutte et al. 2011), which showed an increased cell death in 3D after acetaminophen incubation, which was not detected in 2D cultures. In the present study, we mainly focused on the establishment of a monoculture of hepatocytes in a 3D environment to better mimic in vivo acetaminophen toxicity. Such a simple system could be used for preliminary toxicity studies. However, we are aware that future culture models shall include non-parenchymal cells, too in order to reflect all participating cells in toxicity.
Acetaminophen is transported into PHH by SLC transporter proteins located at the basolateral membrane (Forster et al. 2012). In its unmetabolized form, acetaminophen is non-toxic to PHH (Espinosa Bosch et al. 2006; Hinson et al. 2010). However, NAPQI, its metabolite that is produced during phase I metabolism by CYP2E1, is highly toxic (Yamaura et al. 2011; Li et al. 2012). In this study, we have demonstrated that the increase in the level of the CYP2E1 protein only occurs if the acetaminophen treatment takes place a 3D environment, but not under 2D conditions, which means that acetaminophen-mediated CYP2E1 induction depends on the environmental conditions. The increase in the CYP2E1 protein could lead to higher concentrations of NAPQI accumulating in the PHH and binding intracellular proteins, which would result in cell necrosis (Zaher et al. 1998; Fontana 2008). Furthermore, SOD1, an antioxidant protein that protects PHH from oxidative stress, was investigated as a second protein. It catalyzes the cleavage of superoxide into molecular oxygen and hydrogen peroxide (Ramachandran et al. 2011). The level of the SOD1 protein gradually decreased after the treatment with acetaminophen in 3D, but not in 2D cultures. This decrease is attributed to nitration by reactive nitrogen species. The loss of SOD1 expression can be ascribed to the increment of toxicity by providing superoxide levels in mitochondria which react with nitric oxide (Agarwal et al. 2011). In contrast to PHH in 3D cultures, the PHH that were cultured in 2D featured a constant expression level of the CYP2E1 and SOD1 proteins during the whole treatment with acetaminophen. This finding was supported by the lower levels of acetaminophen remaining in the 3D cultures after 24–48 h of exposure. Overall, the metabolism of acetaminophen was more pronounced in 3D cultures. This fact leads to the hypothesis that, in 2D cultures, acetaminophen is metabolized to the active toxic metabolite NAPQI at lower initial formation rates. This would explain the higher concentrations of acetaminophen after 24 to at least 48 h of exposure. Due to the lower initial formation of NAPQI in the 2D cultures, metabolite-mediated toxic effects were less distinctive than in 3D cultures, which allow a higher metabolic turnover of acetaminophen and thus higher rates of metabolite formation.
As it has been mentioned above, hepatic polarization is a key factor for maintaining PHH in their functional state. Polarized PHH dispose of several transporter proteins located in the apical and basolateral membranes (Decaens et al. 2008).
Multidrug resistance-associated protein-1 is one of the major transporters for glutathione conjugates. The acetaminophen metabolite, NAPQI, is rapidly conjugated by glutathione for its elution out of the cell. In addition, MRP1 needs the presence of glutathione for its transport (Cole and Deeley 2006). Gene expression of different transporter channels (MRP1-4) of samples obtained after 24 and 72 h after acetaminophen stimulation was studied (data not shown). Only MRP1 showed a dose-dependent increase in expression. Therefore, in the present study, we analyzed the transport activity of MRP1, a transporter protein which belongs to the ABC transporter family, and is located at the basolateral membrane (Leslie et al. 2001; Aleksunes et al. 2007). For this transporter, we observed no differences between 2D and 3D cultures at mRNA level (Fig. 5a, b). However, both cell culture models affected the activity of MRP1 in a different way (Fig. 5c d). The 3D cultures demonstrated a higher import and efflux activity than the 2D cultures. These results confirm the lack of acetaminophen toxicity in 2D culture as the toxic metabolite NAPQI cannot be formed without the functional transporter.
Therefore, the transporter localization and functionality are affected by the cell culture conditions. The loss of transporter activity can be explained in several ways: Firstly, in the 2D culture, basolateral and canalicular transporters (Jemmitz et al. 2010) which might reduce the activity of the transporters are expressed on the cell surface. Secondly, this effect could be caused by an alteration of the location of the transporter protein. Under adverse stimulation, hepatic transporters migrate from the apical membrane to internal sites of the membrane reducing the activity of the export pump (Rost et al. 1999). The third reason might be the switch of the efflux activity between different transporter protein isoforms or different transporter proteins located at different membrane locations, when the PHH lose polarity (Roelofsen et al. 1999; Kullak-Ublick et al. 2000). In this case, the activity of the export pump will decrease as a consequence of a substrate-specific deficiency.
In summary, we have proven that there is a strong association between drug toxicity in PHH and the culture environment which correlates with an increase in the transporter activity in 3D cultures by using acetaminophen as a model drug. Furthermore, we have demonstrated that the increase in the metabolic activity of CYP2E1, the depletion of the antioxidative protein SOD, which acts as a protector against oxidative stress, and the increase in MRP1 activity were only maintained in 3D cultures. Therefore, we would like to emphasize the importance of 3D cultures for the achievement of a better comparability of the results that will be gathered in vitro during future hepatotoxicity prediction to the situation in vivo.
References
Agarwal R, MacMillan-Crow LA et al (2011) Acetaminophen-induced hepatotoxicity in mice occurs with inhibition of activity and nitration of mitochondrial manganese superoxide dismutase. J Pharmacol Exp Ther 337(1):110–116
Aleksunes LM, Augustine LM et al (2007) Influence of acetaminophen vehicle on regulation of transporter gene expression during hepatotoxicity. J Toxicol Environ Health A 70(21):1870–1872
Arndt K, Haschek WM et al (1989) Mechanism of dimethylsufoxide protection against acetaminophen hepatotoxicity. Drug Metab Rev 20:261–269
Bruschi SA (2004) Methods and approaches to study metabolism and toxicity of acetaminophen. In: Drug metabolism and transport. Totowa, NJ, pp 197–232
Cole SP, Deeley RG (2006) Transport of gluthathione and gluthathione conjugates by MRP1. Trends Pharmacol Sci 27(8):438–446
Decaens C, Durand M et al (2008) Which in vitro models could be best used to study hepatocyte polarity? Biol Cell 100(7):387–398
Eckl PM, Bresgen N (2003) The cultured primary hepatocyte and its application in toxicology. J Appl Biomed 1:117–126
Espinosa Bosch M, Ruiz Sanchez AJ et al (2006) Determination of paracetamol: historical evolution. J Pharm Biomed Anal 42(3):291–321
Fontana RJ (2008) Acute liver failure including acetaminophen overdose. Med Clin North Am 92(4):761–794, viii
Forster S, Thumser AE et al (2012) Characterization of rhodamine-123 as a tracer dye for use in in vitro drug transport assays. PLoS One 7(3):e33253
Glavinas H, Krajcsi P et al (2004) The role of ABC transporters in drug resistance, metabolism and toxicity. Curr Drug Deliv 1(1):27–42
Godoy P, Hengstler JG et al (2009) Extracellular matrix modulates sensitivity of hepatocytes to fibroblastoid dedifferentiation and transforming growth factor beta-induced apoptosis. Hepatology 49(6):2031–2043
Gomez-Lechon MJ, Castell JV et al (2008) An update on metabolism studies using human hepatocytes in primary culture. Expert Opin Drug Metab Toxicol 4(7):837–854
Gonzalez FJ (2005) Role of cytochromes P450 in chemical toxicity and oxidative stress: studies with CYP2E1. Mutat Res 569(1–2):101–110
Hewitt NJ, Lechon MJ et al (2007) Primary hepatocytes: current understanding of the regulation of metabolic enzymes and transporter proteins, and pharmaceutical practice for the use of hepatocytes in metabolism, enzyme induction, transporter, clearance, and hepatotoxicity studies. Drug Metab Rev 39(1):159–234
Hinson JA, Roberts DW, et al. (2010) Mechanisms of acetaminophen-induced liver necrosis. Handb Exp Pharmacol(196):369–405
Hirano M, Maeda K et al (2005) Bile salt export pump (BSEP/ABCB11) can transport a nonbile acid substrate, pravastatin. J Pharmacol Exp Ther 314:876–882
Jemmitz K, Veres Z et al (2010) Contribution of high basolateral bile salt efflux to the lack of hepatotoxicity in rat in response to drugs inducing cholestasis in human. Toxicol Sci 115(1):80–88
Kock K, Brouwer KL (2012) A perspective on efflux transport proteins in the liver. Clin Pharmacol Ther 92(5):599–612
Kullak-Ublick GA, Stieger B et al (2000) Hepatic transport of bile salts. Semin Liver Dis 20(3):273–292
Larson AM, Polson J et al (2005) Acetaminophen-induced acute liver failure: results of a United States multicenter, prospective study. Hepatology 42(6):1364–1372
Laupeze B, Amiot L et al (2001) Multidrug resistance protein (MRP) activity in normal mature leukocytes and CD34-positive hematopoietic cells from peripheral blood. Life Sci 68(11):1323–1331
Leslie EM, Deeley RG et al (2001) Toxicological relevance of the multidrug resistance protein 1, MRP1 (ABCC1) and related transporters. Toxicology 167(1):3–23
Li FC, Liu Y et al (2009) In vivo dynamic metabolic imaging of obstructive cholestasis in mice. Am J Physiol Gastrointest Liver Physiol 296(5):G1091–G1097
Li J, Wei DQ et al (2012) Molecular dynamics simulations of CYP2E1. Med Chem 8(2):208–221
Lin J, Schyschka L et al (2012) Comparative analysis of phase I and II enzyme activities in 5 hepatic cell lines identifies Huh-7 and HCC-T cells with the highest potential to study drug metabolism. Arch Toxicol 86(1):87–95
Lowry OH, Rosebrough NJ et al (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193(1):265–275
Madsen KG, Olsen J et al (2007) Development and evaluation of an electrochemical method for studying reactive phase-I metabolites: correlation to in vitro drug metabolism. Chem Res Toxicol 20(5):821–831
Nussler AK, Nussler NC et al (2009) The Holy grail of hepatocyte culturing and therapeutic use. In: Santin M (ed) Strategies in regenerative medicine. Springer International, Germany
Prot JM, Briffaut AS et al (2011) Integrated proteomic and transcriptomic investigation of the acetaminophen toxicity in liver microfluidic biochip. PLoS One 6(8):e21268
Ramachandran A, Lebofsky M et al (2011) The impact of partial manganese superoxide dismutase (SOD2)-deficiency on mitochondrial oxidant stress, DNA fragmentation and liver injury during acetaminophen hepatotoxicity. Toxicol Appl Pharmacol 251(3):226–233
Roelofsen H, Hooiveld GJ et al (1999) Glutathione S-conjugate transport in hepatocytes entering the cell cycle is preserved by a switch in expression from the apical MRP2 to the basolateral MRP1 transporting protein. J Cell Sci 112(Pt 9):1395–1404
Rost D, Kartenbeck J et al (1999) Changes in the localization of the rat canalicular conjugate export pump Mrp2 in phalloidin-induced cholestasis. Hepatology 29(3):814–821
Schutte M, Fox B et al (2011) Rat primary hepatocytes show enhanced performance and sensitivity to acetaminophen during three-dimensional culture on a polystyrene scaffold designed for routine use. Assay Drug Dev Technol 9(5):475–486
Suzuki N, Higuchi T et al (2002) Multiple active intermediates in oxidation reaction catalyzed by synthetic heme-thiolate complex relevant to cytochrome p450. J Am Chem Soc 124(32):9622–9628
Ullrich A, Berg C et al (2006) Use of a novel; standardized and validated human hepatocyte culture system for repetitive analyses of drugs: repeated administrations of acetaminophen reduces albumin and urea secretion. Faseb Journal 20(4):A630–A630
Yamaura K, Shimada M et al (2011) Protective effects of goldenseal (Hydrastis canadensis L.) on acetaminophen-induced hepatotoxicity through inhibition of CYP2E1 in rats. Pharmacognosy Res 3(4):250–255
Zaher H, Buters JT et al (1998) Protection against acetaminophen toxicity in CYP1A2 and CYP2E1 double-null mice. Toxicol Appl Pharmacol 152(1):193–199
Acknowledgments
This work was supported by the Federal Ministry of Research project “EmbryoTox” (BMBF 0315208E) and by the SET Foundation. We would like to thank Luc Koster for his help with the editing of this paper.
Author information
Authors and Affiliations
Corresponding author
Additional information
L. Schyschka, J. J. Martínez Sánchez, G. Damm and A. K. Nussler have equally contributed to this work.
Rights and permissions
About this article
Cite this article
Schyschka, L., Sánchez, J.J.M., Wang, Z. et al. Hepatic 3D cultures but not 2D cultures preserve specific transporter activity for acetaminophen-induced hepatotoxicity. Arch Toxicol 87, 1581–1593 (2013). https://doi.org/10.1007/s00204-013-1080-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-013-1080-y