Abstract
Ziram as a dithiocarbamate fungicide is widely used throughout the world in agriculture. We previously found that ziram significantly inhibited cytotoxic T lymphocyte activity in a dose-dependent manner. To explore the mechanism of this inhibition, we investigated ziram-induced apoptosis in human T lymphocytes. Jurkat T cells were treated with ziram at 0.031–1 μM for 2–24 h. Freshly isolated primary human T cells were treated with ziram at 0.0625–1 μM for 15 and 24 h. Apoptosis was determined by FITC-Annexin V/PI staining and the TUNEL assay. To explore the mechanism of apoptosis, intracellular levels of active caspases 3, 3/7, 8, and 9 and pan-caspase and mitochondrial cytochrome-c release were determined by flow cytometry. Disruption to mitochondrial transmembrane potential was determined with a MitoLight™ Apoptosis Detection Kit. We found that ziram induced apoptosis in a time- and dose-dependent manner in both Jurkat cells and primary human T cells. The primary human T cells were more sensitive to ziram than the Jurkat cell line. Ziram induced increases in active caspases 3, 3/7, 8, and 9 and pan-caspase in a dose-dependent manner, and a caspase-3 inhibitor, Z-DEVD-FMK, partially but significantly inhibited the apoptosis. Moreover, a general caspase inhibitor, Z-VAD-FMK, significantly and almost completely blocked the apoptosis. Ziram also disrupted mitochondrial transmembrane potential and caused mitochondrial cytochrome-c release. These findings indicate that ziram can induce apoptosis in human T cells, and the apoptosis is mediated by both the caspase-cascade and the mitochondria/cytochrome-c pathways.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ziram, a carbamate pesticide, is used throughout the world as a fungicide in agriculture and an accelerating agent in latex production (Richardson 1993). Several studies have found ziram to show immunotoxicity including inhibition of natural killer (NK) activity (Whalen et al. 2003; Wilson et al. 2004; Taylor et al. 2005; Taylor and Whalen 2009) and inhibition of TNF-alpha production in a human promyelocytic cell line, THP-1 (Corsini et al. 2006). We also found that ziram significantly inhibits NK, lymphokine-activated killer (LAK), and cytotoxic T lymphocyte (CTL) activity (Li et al. 2011a); however, the precise mechanism underlying its inhibition of CTL activity is still unclear. Having previously shown that organophosphorus pesticides induced apoptosis in immune cells and ultimately caused immunotoxicity (Nakadai et al. 2006; Li et al. 2007, 2009; Li 2007), we speculate that the ziram-induced inhibition of CTL activity may be partially mediated by apoptosis in T cells.
Thus, to explore the inhibiting mechanism, we investigated whether ziram induces apoptosis/necrosis in human T cells. The caspase family of cysteine proteases plays a key role in apoptosis. Caspase-3 is a key protease activated during the early stages of apoptosis and, like other members of the caspase family, is synthesized as an inactive proenzyme that is processed in cells undergoing apoptosis by self-proteolysis and/or cleavage by another protease such as caspase 8 or 9 (Patel et al. 1996). Caspase-7 is highly similar in structure (58%) and substrate-specificity to caspase-3, and caspases-3/7 are effector/executioner caspases (Lu and Chen 2011). Caspases 8 and 9 are also synthesized as inactive pro-caspases that are processed in cells undergoing apoptosis by self-proteolysis and/or cleavage by another protease (Patel et al. 1996). Caspase-8 is an initiator of apoptosis, and pro-caspase-3 is a major physiologic target of caspase-8 (Stennicke et al. 1998). Caspase-9 is also an initiator of apoptosis in the mitochondria/cytochrome-c pathway, and active caspase-9 directly cleaves and activates pro-caspase-3 (Cardone et al. 1998). Cytochrome-c initiates apoptosis through its release into the cytoplasm and binding of Apaf-1 which activates procaspase 9 (Okada et al. 2003). Goldstein et al. (2000) reported that the release of cytochrome-c from mitochondria was a very early event during apoptosis. Based on this background, we also investigated the effects of ziram on caspases and cytochrome-c release to explore the mechanism of ziram-induced apoptosis. Although we previously found that ziram induces apoptosis and necrosis in U937 cells, a monocytic cell line (Li et al. 2011b), there have been no reports on human T cells.
Materials and methods
Reagents
RPMI 1640 medium was purchased from Wako Pure Chemical Industries (Osaka, Japan). Fetal bovine serum (FBS) was purchased from JRH Biosciences (Lenexa, KS) and heat-inactivated at 56°C for 30 min prior to use. Glutamine, 2-mercaptoethanol (2-ME), and propidium iodide (PI) were obtained from Sigma (St. Louis, MO). Human CD3 MicroBeads were purchased from Miltenyi Biotec Inc. (Auburn, CA). Fluorescein isothiocynate (FITC)-anti-human Annexin V and FITC-anti-human active caspase-3, Z-DEVD-FMK (a caspase-3 inhibitor), Z-VAD-FMK (a general caspase inhibitor), Z-FA-FMK (a negative control for Z-DEVD-FMK and Z-VAD-FMK), Cytofix/cytoperm solution, PerCP-Cy5.5-CD3, and the APO-BRDU Apoptosis Detection Kit were purchased from BD Pharmingen (San Diego, CA). CaspaTag caspases 3/7, 8, 9 and pan-caspase in situ assay kits and the MitoLight™ Apoptosis Detection Kit were purchased from CHEMICON (Temecula, CA). Ziram was obtained from Wako Pure Chemical Industries (Osaka, Japan) and prepared as stock solutions in DMSO.
Cells
The human Jurkat T cell line was obtained from American Type Culture Collection (ATCC) (Manassas, VA) and maintained in RPMI 1640 medium containing 10% FBS. Human CD3+ T cells were freshly isolated from human peripheral blood with human CD3 MicroBeads by MACS® technology according to the manufacturer’s instructions (Auburn, CA). We confirmed that more than 96% of cells were CD3+ T cells after the separation using human CD3 MicroBeads. The Ethics Committee of the Nippon Medical School approved this study. Written informed consent was obtained from subjects who provided peripheral blood.
Ziram-induced apoptosis and necrosis in Jurkat T cells and freshly isolated human CD3+ T cells determined by FITC-Annexin V/PI staining
In Japan, the residual standards for ziram in rice and potato are 0.3 and 0.2 ppm calculated as carbon disulfide, respectively [http://ceis.sppd.ne.jp/fs2006/factsheet/pdf/1-249.pdf (in Japanese)]. Thus, 1 μM (approximately 0.3 ppm) of ziram as the highest concentration was applied in the present study.
The Jurkat T cells at 1 × 105/ml were treated with ziram at 0 (0.1% DMSO), 0.03125, 0.0625, 0.125, 0.25, 0.5, or 1 μM for 2, 4, 8, 15, or 24 h and freshly isolated human CD3+ T cells at 1 × 105/ml were treated with ziram at 0 (0.1% DMSO), 0.0625, 0.125, 0.25, 0.5, or 1 μM for 15 or 24 h at 37°C in a 5% CO2 incubator. The treated cells were stained with FITC-Annexin V/PI, and 10,000 cells were acquired and stored for analysis with a FACScan flow cytometer (Becton–Dickinson, San Jose, CA) as described previously (Nakadai et al. 2006; Li et al. 2007, 2009, 2011b).
Detection of DNA fragmentation by TUNEL assay
Jurkat T cells at 1 × 105/ml were treated with ziram at 0 (0.1% DMSO), 0.25, 0.5 or 1 μM for 15 and 24 h. The treated cells were harvested and washed with PBS. DNA fragmentation was detected by the TUNEL assay according to the manufacturer’s instructions. Flow cytometric analysis was performed with FACScan (10,000 cells per analysis).
Determination of intracellular levels of active caspase-3 in Jurkat cells by flow cytometry
Jurkat T cells at 1 × 105/ml were incubated with ziram at 0 (0.1% DMSO), 0.125, 0.25, 0.5, or 1 μM for 15 h at 37°C in a 5% CO2 incubator, harvested, and washed twice with PBS. The cells were fixed/permeabilized with Cytofix/cytoperm solution for 20 min at 4°C, and active caspase-3 was stained with FITC-anti-human active caspase-3 for 30 min at room temperature according to the manufacturer’s instructions (BD PharMingen). Again, the flow cytometric analysis was performed with FACScan (10,000 cells per analysis) (Nakadai et al. 2006; Li et al. 2007, 2009, 2011b).
Determination of intracellular levels of active caspases 3/7, 8, and 9 and pan-caspase in Jurkat cells with CaspaTag caspase in situ assay kits
Jurkat T cells at 1 × 105/ml were incubated with ziram at 0 (0.1% DMSO), 0.0625, 0.125, 0.25, 0.5, or 1 μM for 15 h at 37°C in a 5% CO2 incubator, harvested, and washed twice with PBS. Then, the cells positive for caspases 3/7, 8, and 9 and pan-caspase were stained with fluorochrome inhibitors of caspases (FLICA) and subjected to flow cytometry (10,000 cells per analysis) according to the manufacturer’s instructions.
Protecting effects of caspase-3 and general caspase inhibitors on ziram-induced apoptosis in Jurkat T cells
Jurkat T cells at 1 × 105/ml were preincubated with Z-DEVE-FMK, an inhibitor of caspase-3, Z-VAD-FMK, a general caspase inhibitor, or Z-FA-FMK, a negative control for Z-DEVE-FMK and Z-VAD-FMK, at 20–30 μM for 30 min, treated with ziram at 0 (0.1% DMSO), 0.125, or 0.5 μM for 15 h, harvested, and washed twice with PBS. The treated cells were stained with FITC-Annexin V/PI. Flow cytometric analysis was performed with FACScan (10,000 cells for each analysis) (Nakadai et al. 2006; Li et al. 2007, 2009, 2011b).
Determination of the disruption of mitochondrial transmembrane potential with the MitoLight™ Apoptosis Detection Kit
Jurkat T cells at 1 × 105/ml were incubated with ziram at 0 (0.1% DMSO), 0.0625, 0.125, 0.25, 0.5, or 1 μM for 15 h at 37°C in a 5% CO2 incubator, harvested, and washed twice with PBS. The cells were stained with MitoLight™ solution and detected by flow cytometry (10,000 cells per analysis) according to the manufacturer’s instructions.
Analysis of cytochrome-c release
Jurkat cells at 1 × 105/ml were incubated with ziram at 0 (0.1% DMSO), 0.0625, 0.125, 0.25, 0.5, or 1 μM for 15 h at 37°C in a 5% CO2 incubator, harvested, and washed twice with PBS. The cells were fixed/permeabilized with Cytofix/cytoperm solution for 20 min at 4°C, and the intracellular cytochrome-c was stained with FITC-anti-human cytochrome-c (mouse IgG1) or FITC-mouse IgG1 as an isotypic control for 30 min at 4°C according to the manufacturer’s instructions (eBioscience, San Diego, CA). Flow cytometric analysis was performed with FACScan (10,000 cells per analysis) (Stahnke et al. 2004; Li et al. 2011b).
Statistical analyses
The numbers of apoptotic cells, active caspase-positive cells and cytochrome-c-negative cells were used for statistical analyses. Statistical analyses were performed using one-way ANOVAs followed by a post hoc test, Tukey’s test, with SPSS 16.0J software for Windows. A linear correlation analysis and paired t test were also conducted. The significance level for P-values was set at <0.05.
Results
Ziram-induced apoptosis and necrosis in Jurkat cells determined by FITC-Annexin V/PI staining
As shown in Fig. 1a, b, 52.5% of ziram-treated cells exhibited apoptosis (FITC-Annexin V+/PI−) and 7.9% of ziram-treated cells showed late apoptosis/necrosis (FITC-Annexin V+/PI+) (Fig. 1b), compared with only 5.6 and 4.5% of control cells, respectively (Fig. 1a). As shown in Fig. 1c, d, ziram induced apoptosis in a dose- and time-dependent manner. Similarly, as shown in Fig. 1e, f, ziram-induced late apoptosis/necrosis also exhibited a dose- and time-dependent profile.
Ziram induced apoptosis in Jurkat T cells. a Dot plot of FITC-Annexin V/PI in control cells, b dot plot of FITC-Annexin V/PI in ziram-treated cells, percentages in quadrants 2 and 3 show FITC-Annexin V+/PI+ (late apoptosis/necrosis) and FITC-Annexin V+/PI− (apoptosis) cells, respectively. c Dose-dependent increases in apoptotic cells in ziram-treated cultures (r = 0.777, P < 0.05 for 24 h), d time-dependent increases in apoptotic cells in ziram-treated cultures (r = 0.937, P < 0.05 for 0.5 μM), e dose-dependent increases in late apoptotic/necrotic cells in ziram-treated cultures (r = 0.906, P < 0.01 for 24 h), f time-dependent increases in late apoptotic/necrotic cells in ziram-treated cultures (r = 0.970, P < 0.01 for 1 μM). Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that both the concentration of ziram and incubation period significantly affected apoptosis and late apoptosis/necrosis (all P < 0.01). *P < 0.05, **P < 0.01, significantly different from 0 μM (c, e) or from 2 h (d, f) by Tukey’s test
Ziram-induced apoptosis and necrosis in primary human T cells determined by FITC-Annexin V/PI staining
To test whether ziram causes apoptosis in primary human T cells at similar concentrations and time points, freshly isolated primary human T cells were treated with ziram. As shown in Fig. 2a–c, ziram induced cell death (apoptosis and late apoptosis/necrosis) in a dose- and time-dependent manner with a similar pattern to Jurkat T cells. However, as shown in Fig. 2c, d, the primary human T cells were more sensitive to ziram than Jurkat T cells.
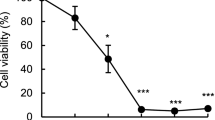
Ziram induced apoptosis in primary human T cells. a Dose-dependent increases in apoptotic cells among ziram-treated primary T cells, b dose-dependent increases in late apoptotic/necrotic cells among ziram-treated primary T cells, c dose-dependent increases in total cell death in ziram-treated primary T cells, d dose-dependent increases in total cell death in ziram-treated Jurkat T cells. Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that the concentration of ziram significantly affected apoptosis, late apoptosis/necrosis, and total cell death (all P < 0.01). *P < 0.05, **P < 0.01, significantly different from 0 μM by Tukey’s test
Ziram-induced apoptosis in Jurkat T cells determined by TUNEL assay
As shown in Fig. 3, ziram significantly induced DNA fragmentation in Jurkat T cells in a dose- and time-dependent manner.
Ziram induced DNA fragmentation in Jurkat T cells, as determined by TUNEL assay. a The shaded histogram shows the control cells (ziram at 0 μM) and the open histogram shows the cells treated with ziram at 0.5 μM for 15 h and stained with FITC-BrdU. b Dose-dependent increases in apoptotic cells in ziram-treated cultures. Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that the concentration of ziram significantly affected apoptosis in Jurkat T cells (P < 0.01). **P < 0.01, significantly different from 0 μM by Tukey’s test
Detection of intracellular levels of active caspase-3 in apoptotic Jurkat T cells by flow cytometry
As shown in Fig. 2, ziram-induced cell death in the primary human T cells showed a similar pattern to that in Jurkat T cells although the primary cells were more sensitive to ziram. Based on the results shown in Figs. 1 and 2, we used Jurkat T cells to explore the mechanism of ziram-induced apoptosis. Moreover, as shown in Fig. 1, because ziram induced a maximal response in apoptosis with 15 h treatment, based on the results shown in Fig. 1, we incubated the cells for 15 h to investigate the effect of ziram on caspases, cytochrome-c, and mitochondrial transmembrane potential in subsequent experiments.
To explore the mechanism of the apoptosis, we investigated whether ziram affected the intracellular level of active caspase-3. As shown in Fig. 4a, b, ziram induced a significant increase in active caspase-3 in a dose-dependent manner. Moreover, an inhibitor of active caspase-3 significantly protected against the apoptosis (Fig. 4c). The findings strongly suggest that ziram induced apoptosis at least partially via the caspase-3 pathway.
Ziram induced an increase in active caspase-3-positive Jurkat T cells. a The shaded histogram shows the control cells (ziram at 0 μM) and the open histogram shows the cells treated with ziram at 0.5 μM for 15 h and stained with FITC-rabbit anti-human active caspase 3. b Dose-dependent increases in active caspase-3-positive cells in ziram-treated cultures. Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that the concentration of ziram significantly affected the active caspase-3-positive cells (P < 0.01). **P < 0.01, significantly different from 0 μM by Tukey’s test. c Caspase-3 inhibitor significantly inhibited ziram-induced apoptosis as determined with FITC-Annexin V staining by flow cytometry. Inhibitor (+): cells treated with Z-DEVD-FMK (a caspase-3 inhibitor). Inhibitor (−): cells treated with Z-FA-FMK (a negative control for Z-DEVD-FMK). Data are presented as the mean ± SD (n = 3). **P < 0.01, significantly different from the Inhibitor (−) by paired t test
Detection of caspases 3/7, 8, and 9 and pan-caspase in apoptotic Jurkat T cells with CaspaTag caspase in situ assay kits
To explore whether other caspases were also involved in the ziram-induced apoptosis, we investigated the intracellular levels of active caspases 3/7, 8, and 9 and pan-caspase in Jurkat T cells. As shown in Fig. 5, ziram induced significant increases in active caspases 3/7, 8, and 9 and pan-caspase in a dose-dependent manner. Moreover, a general inhibitor of caspases significantly and almost completely protected against the apoptosis (Fig. 6). The findings strongly suggest that ziram induced apoptosis via the caspase-cascade pathway.
Ziram induced an increase in active caspase-3/7-, caspase-8-, caspase-9-, and pan-caspase-positive Jurkat T cells. a, c, e, g The shaded histograms show the control cells (ziram at 0 μM) and the open histograms show the cells treated with ziram at 0.5 μM for 15 h and stained with FLICA. b, d, f, h dose-dependent increases in active caspase-3/7- (b), caspase-8- (d), caspase-9- (f), and pan-caspase (h)-positive cells in ziram-treated cultures. Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that the concentration of ziram significantly affected the active caspase-positive cells (all P < 0.01). *P < 0.05, **P < 0.01, significantly different from 0 μM by Tukey’s test
General caspase inhibitor significantly and almost completely blocked ziram-induced apoptosis as determined with FITC-Annexin V staining by flow cytometry. a Dot plot of FITC-Annexin V/PI in control cells (ziram at 0 μM), b dot plot of FITC-Annexin V/PI in cells treated with ziram at 0.5 μM in the presence of Z-FA-FMK (a negative control for Z-VAD-FMK) at 30 μM, c dot plot of FITC-Annexin V/PI in cells treated with ziram at 0.5 μM in the presence of Z-VAD-FMK (a general caspase inhibitor) at 30 μM; percentages in quadrants 2 and 3 show FITC-Annexin V+/PI+ (late apoptosis/necrosis) and FITC-Annexin V+/PI− (apoptosis) cells, respectively, d Inh (20 μM): cells pre-treated with Z-VAD-FMK at 20 μM, Inh (30 μM): cells pre-treated with Z-VAD-FMK at 30 μM, Inh (−): cells pre-treated with Z-FA-FMK at 30 μM. Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that the concentration of Z-VAD-FMK significantly affected apoptosis (P < 0.01). **P < 0.01, significantly different from Inh (−), ## P < 0.01, significantly different from Inh (20 μM) by Tukey’s test
Determination of the disruption of mitochondrial transmembrane potential with the MitoLight™ Apoptosis Detection Kit
To further investigate whether the mitochondrial pathway was also involved in the ziram-induced apoptosis of Jurkat T cells, we determined mitochondrial transmembrane potential with the MitoLight™ Apoptosis Detection Kit. We found that ziram disrupted the transmembrane potential in a dose-dependent manner (Fig. 7).
Ziram caused a disruption of mitochondrial transmembrane potential in Jurkat T cells. a The shaded histogram shows the control cells (ziram at 0 μM) and the open histogram shows the cells treated with ziram at 0.5 μM for 15 h and stained with MitoLight™ solution. b Dose-dependent increases in apoptotic cells in ziram-treated cultures (r = 0.845, P < 0.05). Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that the concentration of ziram significantly affected apoptosis (P < 0.01). **P < 0.01, significantly different from 0 μM by Tukey’s test
Detection of mitochondrial cytochrome-c release in apoptotic Jurkat T cells by flow cytometry
To further explore the mechanism of ziram-induced apoptosis in Jurkat T cells, we investigated whether ziram induces mitochondrial cytochrome-c release. As shown in Fig. 8, ziram induced a significant increase of cytochrome-c-negative cells in a dose-dependent manner, indicating that it induced mitochondrial cytochrome-c release.
Detection of mitochondrial cytochrome-c release in apoptotic cells by flow cytometry. a The shaded histogram shows the control cells (ziram at 0 μM) and the open histogram shows the cells treated with ziram at 0.5 μM for 15 h and stained with FITC-cytochrome-c. b Dose-dependent increases in the percentage of cells without cytochrome-c in ziram-treated cultures (r = 0.918, P < 0.01). Data are presented as the mean ± SD (n = 3). One-way ANOVA indicated that the concentration of ziram significantly affected cytochrome-c release (P < 0.01). **P < 0.01, significantly different from 0 μM by Tukey’s test
Discussion
We previously found that ziram significantly inhibits CTL activity (Li et al. 2011a). To explore the mechanism of this inhibition, we investigated whether ziram induces apoptosis/necrosis in human T cells. In the present study, we found that ziram at a very low concentration (0.0625 μM) induced apoptosis in a dose- and time-dependent manner in both a human T cell line, the Jurkat cell line, and freshly isolated primary human T cells. The primary human T cells were more sensitive to ziram than the Jurkat cell line. Moreover, ziram significantly induced DNA fragmentation, a hallmark of apoptosis, supporting the findings made with Annexin V staining. In addition, it also induced necrosis in a dose- and time-dependent manner in human T cells. This is the first report on ziram-induced apoptosis in human T cells, although it has been reported that ziram induced apoptosis in U937, a monocytic cell line (Li et al. 2011b).
To explore the mechanism of ziram-induced apoptosis, we examined the active caspase-3 in ziram-treated Jurkat T cells and found a significant increase in its intracellular levels. Moreover, Z-DEVD-FMK, a caspase-3 inhibitor, significantly inhibited the apoptosis. These findings suggested that ziram induces apoptosis via the caspase-3 pathway. However, the caspase-3 inhibitor only partially prevented apoptosis, suggesting other pathways to be involved. Next, we investigated caspases 3/7, 8, and 9 and found that ziram significantly increased their intracellular levels in a dose-dependent manner. Moreover, we also found that ziram significantly increased the intracellular levels of active pan-caspase in a dose-dependent manner and that Z-VAD-FMK, a general caspase inhibitor, significantly and almost completely blocked the ziram-induced apoptosis indicating the involvement of all caspases (caspase cascade) in ziram-induced apoptosis in Jurkat T cells.
Disruption of mitochondrial transmembrane potential is one of the earliest intracellular events to occur following the induction of apoptosis (Okada et al. 2003). Ziram disrupted the transmembrane potential in Jurkat T cells in a dose-dependent manner as determined with a MitoLight™ Apoptosis Detection Kit, suggesting that ziram also affects the mitochondrial pathway.
Cytochrome-c initiates apoptosis through its release into the cytoplasm and binding of Apaf-1 which activates procaspase 9 (Okada et al. 2003). Goldstein et al. (2000) reported that the release of cytochrome-c from mitochondria was a very early event during apoptosis. To explore whether this release mechanism was involved in the ziram-induced apoptosis, we determined intracellular cytochome-c levels in Jurkat T cells. Ziram produced a significantly higher proportion of cells without cytochome-c in a dose-dependent manner, indicating that it induced the release of cytochrome-c from mitochondria. This finding also suggested that cytochrome-c was involved in the apoptosis. Taken together, the findings suggested that ziram affects both the caspase-cascade and the mitochondria/cytochrome-c pathways.
Moreover, because the Fas/Fas ligand pathway is an important trigger for apoptosis and upstream of caspase 8 activation (Yang et al. 2011), the effect of ziram on Fas/FasL should also be considered. Therefore, a study to investigate the influence of ziram on the Fas/FasL pathway is necessary in the future.
The solubility of ziram in water is 65 mg/l (65 ppm) (Richardson 1993). The highest concentration of ziram used in the present study was 1 μM (0.312 ppm), suggesting that all ziram should be dissolved in the culture medium during the in vitro culture. Although ziram is rapidly metabolized in animals (Richardson 1993), it is difficult to account for its metabolism in vitro because ziram may bind to the membrane of cells or enter the cells during the incubation. In addition, there is little or no research available on the fate of the compound in water (Howard 1991).
Sook Han et al. (2003) reported that ziram induced apoptosis in neuronal-like pheochromocytoma (PC12) cells via Ca(2+) influx through non-selective cation channels. Wang et al. (2006) found that ziram-induced cell death in SK-N-MC neuroblastoma cells was closely correlated with proteasomal inhibition, but not correlated with the cellular production of reactive oxygen species, suggesting that cellular oxidative stress was not a mechanism of ziram-induced cell death. Moreover, Chou et al. (2008) also reported that ziram causes dopaminergic cell damage by inhibiting E1 ligase in the proteasome, suggesting that inhibition of the proteasome is a potential mechanism of ziram-induced cell death. However, they did not identify whether ziram-induced cell death consisted of apoptosis (Wang et al. 2006; Chou et al. 2008). We also previously found that ziram induced apoptosis in U937 cells partially mediated by the activation of intracellular caspase-3 and the release of cytochrome-c from mitochondria (Li et al. 2011b).
Taken together, the present findings indicate that ziram can induce apoptosis in human T cells, and the apoptosis is mediated by both the caspase-cascade and the mitochondria/cytochrome-c pathways.
References
Cardone MH, Roy N, Stennicke HR, Salvesen GS, Franke TF, Stanbridge E, Frisch S, Reed JC (1998) Regulation of cell death protease caspase-9 by phosphorylation. Science 282:1318–1321
Chou AP, Maidment N, Klintenberg R, Casida JE, Li S, Fitzmaurice AG, Fernagut PO, Mortazavi F, Chesselet MF, Bronstein JM (2008) Ziram causes dopaminergic cell damage by inhibiting E1 ligase of the proteasome. J Biol Chem 283:34696–34703
Corsini E, Viviani B, Birindelli S, Gilardi F, Torri A, Codecà I, Lucchi L, Bartesaghi S, Galli CL, Marinovich M, Colosio C (2006) Molecular mechanisms underlying mancozeb-induced inhibition of TNF-alpha production. Toxicol Appl Pharmacol 212:89–98
Goldstein JC, Waterhouse NJ, Juin P, Evan GI, Green DR (2000) The coordinate release of cytochrome C during apoptosis is rapid, complete and kinetically invariant. Nat Cell Biol 2:156–162
Howard PH (1991) Handbook of fate and exposure data for organic chemicals, vol III. Lewis Publishers, Chelsea
Li Q (2007) New mechanism of organophosphorus pesticide-induced immunotoxicity. J Nippon Med Sch 74:92–105
Li Q, Kobayashi M, Kawada T (2007) Organophosphorus pesticides induce apoptosis in human NK cells. Toxicology 239:89–95
Li Q, Kobayashi M, Kawada T (2009) Chlorpyrifos induces apoptosis in human T cells. Toxicology 255:53–57
Li Q, Kobayashi M, Kawada T (2011a) Effect of ziram on natural killer, lymphokine-activated killer, and cytotoxic T lymphocyte activity. Arch Toxicol 29 Oct [Epub ahead of print]
Li Q, Kobayashi M, Kawada T (2011b) Ziram induces apoptosis and necrosis in human immune cells. Arch Toxicol 85:355–361
Lu Y, Chen GQ (2011) Effector caspases and leukemia. Int J Cell Biol 2011:738301, 14 Apr [Epub]
Nakadai A, Li Q, Kawada T (2006) Chlorpyrifos induces apoptosis in human monocyte cell line U937. Toxicology 224:202–209
Okada S, Li Q, Whitin JC, Clayberger C, Krensky AM (2003) Intracellular mediators of granulysin-induced cell death. J Immunol 171:2556–2562
Patel T, Gores GJ, Kaufmann SH (1996) The role of proteases during apoptosis. FASEB J 10:587–597
Richardson ML (1993) Z19: Ziram. In: Richardson ML (ed) The dictionary of substances and their effects, vol 7. The Royal Society of Chemistry, Cambridge, pp 908–911
Sook Han M, Shin KJ, Kim YH, Kim SH, Lee T, Kim E, Ho Ryu S, Suh PG (2003) Thiram and ziram stimulate non-selective cation channel and induce apoptosis in PC12 cells. Neurotoxicology 24:425–434
Stahnke K, Mohr A, Liu J, Meyer LH, Karawajew L, Debatin KM (2004) Identification of deficient mitochondrial signaling in apoptosis resistant leukemia cells by flow cytometric analysis of intracellular cytochrome c, caspase-3 and apoptosis. Apoptosis 9:457–465
Stennicke HR, Jürgensmeier JM, Shin H, Deveraux Q, Wolf BB, Yang X, Zhou Q, Ellerby HM, Ellerby LM, Bredesen D, Green DR, Reed JC, Froelich CJ, Salvesen GS (1998) Pro-caspase-3 is a major physiologic target of caspase-8. J Biol Chem 273:27084–27090
Taylor TR, Whalen MM (2009) Effects of ziram on tumor-cell-binding capacity, cell-surface marker expression, and ATP levels of human natural killer cells. Cell Biol Toxicol 25:447–455
Taylor TR, Tucker T, Whalen MM (2005) Persistent inhibition of human natural killer cell function by ziram and pentachlorophenol. Environ Toxicol 20:418–424
Wang XF, Li S, Chou AP, Bronstein JM (2006) Inhibitory effects of pesticides on proteasome activity: implication in Parkinson’s disease. Neurobiol Dis 23:198–205
Whalen MM, Loganathan BG, Yamashita N, Saito T (2003) Immunomodulation of human natural killer cell cytotoxic function by triazine and carbamate pesticides. Chem Biol Interact 145:311–319
Wilson S, Dzon L, Reed A, Pruitt M, Whalen MM (2004) Effects of in vitro exposure to low levels of organotin and carbamate pesticides on human natural killer cell cytotoxic function. Environ Toxicol 19:554–563
Yang C, Liu HZ, Fu ZX (2011) PEG-liposomal oxaliplatin induces apoptosis in hunman colorectal cancer cells via Fas/FasL and caspase-8. Cell Biol Int 2 Sep [Epub ahead of print]
Acknowledgments
This work was supported by a grant from the Ministry of Education, Culture, Sports, Science and Technology. We are grateful to the staff at the Department of Hygiene and Public Health, Nippon Medical School for their assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, Q., Kobayashi, M. & Kawada, T. Mechanism of ziram-induced apoptosis in human T lymphocytes. Arch Toxicol 86, 615–623 (2012). https://doi.org/10.1007/s00204-011-0791-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-011-0791-1