Abstract
Diesel exhaust particles contain redox-active quinones, such as 9,10-phenanthraquinone (9,10-PQ) and 1,2-naphthoquinone (1,2-NQ), which act as potent electron acceptors, thereby altering electron transfer on proteins. We have previously found that 9,10-PQ inhibits constitutive nitric oxide synthase (NOS) activity, by shunting electrons away from NADPH on the cytochrome P450 reductase domain of NOS, and thus suppresses acetylcholine (Ach)-induced vasorelaxation in the aortic ring. However, the effect of 1,2-NQ on endothelial NOS (eNOS) activity is still poorly understood. With the membrane fraction of cultured bovine aortic endothelial cells, we found that 1,2-NQ was a potent inhibitor of eNOS with an IC50 value of 1.4 μM, whereas trans-1,2-dihydroxy-1,2-dihydronaphthalene (1,2-DDN), a redox-negative naphthalene analog of 1,2-NQ, did not show such an inhibitory action. Although 1,2-DDN (5 μM) did not affect Ach-mediated vasorelaxation, 1,2-NQ caused a significant suppression of Ach-induced endothelium-dependent vasorelaxation in the aortic ring. However, 1,2-NQ did not affect sodium nitroprusside-induced endothelium-independent vasorelaxation. These results suggest that 1,2-NQ is an environmental quinone that inhibits eNOS activity, thereby disrupting NO-dependent vascular tone.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Endothelium-derived nitric oxide (NO), which is synthesized by NO synthase (NOS), is a critical regulator of cardiovascular homeostasis. In vascular physiology, NO regulates blood pressure (Calver et al. 1992; Moncada et al. 1991), maintains vasodilator tone (Palmer et al. 1987), prevents platelet aggregation (Radomski et al. 1987) and inhibits vascular smooth muscle cell proliferation (Stewart et al. 1994). In the vasculature, NO is synthesized from l-arginine, by the endothelial isoform of NOS (eNOS) (Ignarro 1989; Moncada and Higgs 1993), and NO production is regulated by eNOS activity and/or expression.
Diesel exhaust particles (DEP) contain numerous components such as aliphatic hydrocarbons, polycyclic aromatic hydrocarbons and their hydroxyl derivatives, quinones and various metals. It is well known that exposure to DEP components causes oxidative stress in experimental animal and in cultured mammalian cells (Sagai et al. 1993; Hiura et al. 1999; Li et al. 2000). Recently, polycyclic aromatic hydrocarbon quinones have been identified as a potential component of DEP in the oxidative stress-dependent deleterious action of DEP. We reported that a variety of quinones, with one-electron reduction potential (E 1 7) values ranging from −240 to −100 mV, are capable of inhibiting neuronal NOS (nNOS) activity (Kumagai et al. 1998). We also found that by shunting electrons away from NADPH as the electron donor, 9,10-phenanthraquinone (9,10-PQ), with an E 1 7 value of −124 mV, is the most potent inhibitor of nNOS with an IC50 value of 10 μM (Kumagai et al. 1998). Subsequent studies indicated that 9,10-PQ inhibits eNOS activity (IC50 value=0.6 μM) and, thus, diminished NO-dependent vasorelaxation in rat aortic ring (Kumagai et al. 2001). Since the exposure of DEP components to rat aorta results in the suppression of acetylcholine (Ach)-dependent vasorelaxation (Ikeda et al. 1995), these results suggest that quinones, such as 9,10-PQ, play a role in the impairment of NO-dependent vasorelaxation in the aortic ring.
We have recently developed a sensitive and reproducible assay for the simultaneous quantitation of quinones in DEP by gas chromatography–mass spectrometry. Using this assay, we reported that besides 9,10-PQ (24.19 μg/g DEP), 1,2-naphthoquinone, (1,2-NQ) is contained in DEP (13.69 μg/g DEP) (Cho et al. 2004). It was reported that 1,2-NQ affects the enzyme activity of nNOS with an IC50 value of 11.5 μM (Kumagai et al. 1998), but the effects of 1,2-NQ on eNOS activity and on NO-dependent vascular tone remain to be elucidated. This study shows that 1,2-NQ inhibits eNOS activity and suppresses NO-dependent vasorelaxation.
Materials and methods
Materials
Chemicals were obtained as follows: 1,2-naphthoquinone (1,2-NQ), dithiothreitol (DTT) from Nacalai Tesque (Kyoto, Japan); dimethyl sulfoxide (DMSO), Ach, sodium nitroprusside (SNP) and l-arginine from Sigma Chemical (St Louis, MO); l-[2,3-3H]arginine from DuPont-NEN Research Products (Boston, MA) and AG50W-X8 resin from Bio-Rad Laboratories (Hercules, CA). Calmodulin (CaM) was purified from the bovine brain, as described by Gopalakrishna and Anderson (1982). trans-1,2-Dihydroxy-1,2-dihydronaphthalene (1,2-DDN) was synthesized as described by Platt and Oesch (1983). The synthetic chemical showed >95% purity. All other chemicals used were of the highest grade available.
Animals
A total of 11 male New Zealand rabbits (1–1.5 kg) were used in this study. They were obtained from the Experimental Animal Center of the University of Tsukuba. All of them were housed in standard cages and allowed free access to standard rabbit chow and water ad libitum. They were all handled and cared for according to institutional guidelines in compliance with the “Principles of Laboratory Animal Care” and the “Guide for the Care and Use of Laboratory Animals.”
Oxygen consumption by 1,2-NQ
Both 1,2-NQ and 1,2-DDN were dissolved in DMSO. Others were prepared with double distilled deionized water. The reaction mixture (2 ml) consisted of 1,2-NQ or 1,2-DDN (50 μM), 500 μM DTT and 100 mM HEPES (pH 7.6)–3 mM EDTA. After the reactions were initiated by the addition of 1,2-NQ or 1,2-DDN, oxygen consumption in the solution was measured by a DO meter B-505 (Iijima Electronics Corp., Aichi, Japan) every 30 s for 5 min at room temperature.
Enzyme preparation
Bovine aortic endothelial cells (BAECs) were obtained from Dainippon Pharmaceutical Industrial (Tokyo, Japan). The BAECs were maintained in a Dulbecco’s modified Eagle’s medium-nutrient F-12 (1:1, vol/vol) containing 15% heat-inactivated fetal bovine serum–penicillin (100 U/ml)–streptomycin (100 μg/ml) and fibroblast growth factor—acidic (5 ng/ml)–heparin (10 U/ml). The cells were incubated in a humidified atmosphere of 95% air–5% CO2. BAECs between passages 3 and 7 were used in the preparation of the enzyme. The enzyme was prepared and kept as described in Sun et al. (2005).
Enzyme activity
The incubation mixtures (0.1 ml) consisted of a suspension of the membrane fraction of the BAECs (0.08–0.10 mg of protein), 1,2-NQ (0.25–4 μM), a complete medium (20 nM 2,3-[3H]arginine, 50 μM l-arginine, 100 μM NADPH, 10 μM tetrahydrobiopterin, 2 mM CaCl2, 1 μg of CaM) and 20 mM HEPES (pH 7.4). 1,2-NQ was dissolved in DMSO; the maximal volume of the DMSO was maintained at 20 μl/ml of the assay mixture because DMSO slightly affected eNOS activity. The enzyme activity was measured according to the method described in Sun et al. (2005). To calculate the IC50 value, eNOS activities, in the presence of different concentrations of 1,2-NQ, were analyzed by a nonlinear regression program using the PRISM version 3.0 (Graph Pad Software, San Diego, CA).
Measurement of vascular relaxation
The rabbits were sacrificed after being anesthetized with pentobarbital sodium (120 mg/kg i.v.). Rabbit aortic rings were prepared as described by Furchgott and Zawadzki (1980). The thoracic aortas were carefully removed to protect the endothelial lining, cleared of adhering fat and connective tissue, and cut into 3-mm-wide transverse rings. The rings were mounted under 1 g of resting tension on stainless-steel hooks in 20-ml capacity muscle chambers and bathed in an oxygenated (95% O2–5% CO2) Krebs–Henseleit solution (115 mM NaCl, 4.7 mM KCl, 2.5 mM CaCl2, 1.2 mM MgSO4, 1.2 mM KH2PO4, 25 mM NaHCO3 and 10 mM glucose, pH 7.4) at 37°C. Tension was measured isometrically, using a force–displacement transducer (model DSA-603, Minebea, Tokyo, Japan). Experiments were conducted to determine the responsiveness of the endothelium-intact aortic rings to Ach, an endothelium-dependent vasodilator. After pre-incubation of the aortic rings with 1,2-NQ or 1,2-DDN for 60 min, the organ bath was washed three times in a Krebs–Henseleit solution. Then, 1 μM of phenylephrine was added to precontract the aortic ring and increasing concentrations of Ach were added in a cumulative manner (10−9–10−6.5 M). Concentration–response curves were then determined, with relaxation expressed as the percentage decrease in the contractile tone elicited by 1 μM phenylephrine. The responsiveness to the endothelium-independent vasodilator SNP (10−11–10−7 M) was also measured in the endothelium-denuded aortic rings.
Statistics
Each value was expressed as the mean ± SE with repeated measurements for each group. A t-test was carried out on a personal computer, using a biomedical program (HALBAU, Japan).
Results
Redox cycling
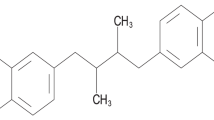
We reported that the inhibition potency of nNOS and eNOS activities by quinones is correlated with their E 1 7 values (Kumagai et al. 1998). Thus, it is postulated that redox-active quinones react readily with electron donors, such as thiol chemicals, resulting in the occurrence of redox cycling associated with the generation of reactive oxygen species (ROS) as previously reported (Kumagai et al. 2002). To investigate whether 1,2-NQ is a redox-active quinone like 9,10-PQ, we determined the redox cycling reaction of 1,2-NQ in the presence of DTT. Oxygen consumption in the incubation mixture of 1,2-NQ was monitored for ROS generation. As shown in Fig. 1, dissolved oxygen in the reaction mixture was rapidly consumed after the addition of DTT (500 μM) to 1,2-NQ (50 μM). Such oxygen consumption was also observed with 9,10-PQ (data not shown). However, when 1,2-DDN (see Fig. 2) was used instead of 1,2-NQ, no appreciable change in oxygen consumption in the presence of DTT was seen. For these reasons, 1,2-DDN was utilized as a redox-negative analog for 1,2-NQ in subsequent experiments.
Oxygen consumption by 1,2-NQ and 1,2-DDN. The reaction mixture (2 ml) consisted of 1,2-NQ or 1,2-DDN (50 μM), 500 μM DTT and 0.1 M HEPES (pH 7.6)–3 mM EDTA. Reactions were initiated by the addition of 1,2-NQ or 1,2-DDN. Dissolved oxygen in the solution was measured every 30 s for 5 min at room temperature. Each value is the mean ± SD of three determinations
eNOS activity
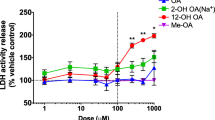
To determine whether 1,2-NQ affects eNOS enzyme activity, we incubated with 1,2-NQ and BAECs membrane fraction. As shown in Fig. 3a, 1,2-NQ inhibited eNOS enzyme activity in a concentration-dependent manner. The IC50 value of 1,2-NQ, estimated by a nonlinear regression analysis, was 1.4 μM. More than 90% of the eNOS activity was inhibited by 10 μM of 1,2-NQ. In contrast, 1,2-DDN showed a slight inhibition of eNOS activity even at 10 μM (Fig. 3b).
Effects of 1,2-NQ and 1,2-DDN on eNOS activity. a Concentration-dependent inhibition of eNOS activity by 1,2-NQ. After the enzyme solution was pre-incubated with 1,2-NQ from 0.25 to 4 μM at 37°C for 5 min, reactions were initiated by the addition of the complete medium and carried out at 37°C for 30 min. eNOS activity was determined as conversion from l-arginine to l-citrulline. Each point is the average of two determinations. b Alteration in eNOS enzyme activity during incubation with 10 μM 1,2-NQ or 1,2-DDN for 5 min. Under the same conditions in (a), the enzyme solution was pre-incubated with 1,2-NQ or 1,2-DDN by 10 μM, respectively, and then NO production was determined. Each bar is the average of two determinations
Vasorelaxation of the aortic ring
Although 1 μM of 1,2-NQ did not affect Ach-induced endothelium-dependent vasorelaxation, 5 μM of 1,2-NQ significantly suppressed endothelium-dependent relaxation (the percentage of maximal relaxation was 98.15±3.2, 96.3±6.4 and 13.74±1.1% in the control, the 1- and 5-μM concentrations of 1,2-NQ, respectively) (Fig. 4a). Under the same concentration, however, 1,2-DDN failed to diminish such a pharmacological action (the percentage of maximal relaxation was 98.15±3.2 and 99.35±1.1% in the control and the 5-μM concentration of 1,2-DDN) (Fig. 4b). In contrast, 1,2-NQ did not affect SNP-induced endothelium-independent vasorelaxation (Fig. 5).
Effects of 1,2-NQ and 1,2-DDN on Ach-induced endothelium-dependent relaxations in the aortic ring. a Effects of 1,2-NQ on endothelium-dependent relaxation. After the aortic rings with endothelium were treated with 1,2-NQ (1 and 5 μM) for 60 min, respectively, phenylephrine (1 μM) was added to precontract the aortic ring, and then increasing concentrations of Ach were added in a cumulative manner. Concentration–response curves were determined with relaxation expressed as the percentage decrease in contractile tone elicited by 1 μM phenylephrine, contrast to control. Each value is the mean ± SE of three animals. b Effects of 1,2-DDN on endothelium-dependent relaxation. After the aortic rings with endothelium were treated with 1,2-DDN (5 μM) for 60 min, the experiments were carried out as described in (a). Concentration–response curves were determined with relaxation expressed as the percentage decrease in the contractile tone elicited by 1 μM phenylephrine, in contrast with the control. Each value is the mean ± SE of three animals
Effects of 1,2-NQ on the SNP-induced endothelium-independent relaxation. After the endothelium-denuded aortic rings were treated with 1,2-NQ (5 μM) for 60 min, 1 μM phenylephrine was added to precontract the aortic rings and then increasing concentrations of SNP were added in a cumulative manner. Concentration–response curves were determined with relaxation expressed as the percentage decrease in the contractile tone elicited by 1 μM phenylephrine, in contrast with the control. Each value is the mean ± SE of three animals
Discussion
The present study indicates that 1,2-NQ is a component of DEP, which affects eNOS activity with the membrane fraction of endothelial cells; thus suppressing Ach-induced vasorelaxation of the aortic ring. Considering its structure, it is recognized that 1,2-NQ has at least two chemical properties. One is the covalent attachment to thiol functions, due to the existence of α,β-unsaturated carbonyl group, and the other is redox cycling, with electron donors such as dithiols, as indicated by a previous study (Kumagai et al. 2002). As shown in Fig. 1, a rapid oxygen consumption of dissolved oxygen occurs after the reaction of 1,2-NQ with DTT, but not after the reaction of 1,2-DDN with DTT; suggesting that 1,2-NQ is a potent redox-active chemical whereas 1,2-DDN is a poor substance for redox cycling. We found that quinones that interact with thiols, such as DTT, inhibit eNOS activity (Kumagai et al. 1998, 2001, 2002). Although the covalent binding of 1,2-NQ with eNOS, through reactive thiols, might be involved in 1,2-NQ-induced inhibition of eNOS activity, 1,2-NQ–4-mercaptoethanol, which has a negative covalent binding reactivity, caused marked oxygen consumption in the presence of DTT and also inhibited eNOS activity with 1,2-NQ (K. Taguchi et al., unpublished observation) with the same tendency. This suggests that 1,2-NQ-induced inhibition of eNOS activity is caused by its redox-active property rather than its covalent modification to eNOS. From these observations, we thought that unlike 1,2-DDN, 1,2-NQ could affect eNOS activity, thereby disrupting NO-dependent vasorelaxation. Consistent with this notion, 1,2-NQ suppressed Ach-induced endothelium-dependent vasorelaxation, whereas 1,2-NQ did not affect SNP-induced endothelium-independent vasorelaxation. In addition, 1,2-DDN had no effect on Ach-mediated vasorelaxation of rabbit aortic ring. Taken together, our findings suggest that 1,2-NQ-induced impairment of NO-dependent vascular tone is, at least, partially due to the inhibition of NO formation by eNOS, presumably through shunting electrons away from NADPH on the cytochrome P450 reductase domain of NOS, as reported previously (Kumagai et al. 1998, 2001).
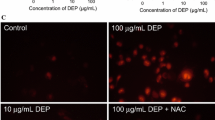
Epidemiological examinations have suggested that the exposure of humans to ambient particulate matter is associated with an increased risk of cardiopulmonary-related diseases and mortality (Dockery et al. 1993; Pope et al. 1995). Ikeda et al. (1995) previously reported that incubation of rat aortic ring with a suspension of DEP caused an impairment of Ach-induced endothelium-dependent vasorelaxation. These findings suggest that DEP chemicals in urban air participate in an impairment of vasorelaxation. Since DEP contains multiple quinones with high redox activity, other than 9,10-PQ and including 1,2-NQ (Cho et al. 2004), we speculate that such redox-positive quinones contaminated in DEP affect eNOS activity and, thus, alter NO-dependent vascular tones. It is reported that the exposure of 9,10-PQ to human pulmonary epithelial A549 cells resulted in marked oxidative protein modification and subsequent apoptosis (Sugimoto et al. 2005). These deleterious actions of 9,10-PQ result from the generation of ROS, through redox cycling, and account for the oxidative stress-dependent cellular toxicity caused by 1,2-NQ seen in the BAECs and A549 cells in our laboratory.
Abbreviations
- 1,2-NQ:
-
1,2-Naphthoquinone
- 1,2-DDN:
-
trans-1,2-Dihydroxy-1,2-dihydronaphthalene
- NO:
-
Nitric oxide
- eNOS:
-
Endothelial nitric oxide synthase
- Ach:
-
Acetylcholine
- SNP:
-
Sodium nitroprusside
References
Calver A, Collier J, Moncada S, Vallance P (1992) Effect of local intraarterial NG-monomethyl-l-arginine in patients with hypertension: the nitric oxide dilator mechanism appears abnormal. J Hypertens 10:1025–1031
Cho AK, Stefano ED, You Y, Rodriguez CE, Schmitz DA, Kumagai Y, Miguel AH, Eiguren-Fernandez A, Kobayashi T, Avol E, Froines JR (2004) Determination of four quinones in diesel exhaust particles, SRM 1649a and atmospheric PM2.5. Aerosol Sci Technol 38:1–14
Dockery DW, Pope AC III, Xu X, Spengler JD, Ware JH, Fay ME, Ferris BG Jr, Speizer FE (1993) An association between air pollution and mortality in six US cities. N Engl J Med 329:1753–1759
Furchgott RF, Zawadzki J (1980) The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature 89:288–373
Gopalakrishna R, Anderson WB (1982) Ca2+-induced hydrophobic site on calmodulin: application for purification of calmodulin by phenyl-sepharose affinity chromatography. Biochem Biophys Res Commun 104:830–836
Hiura TS, Kaszubowski MP, Li N, Nel AE (1999) Chemicals in diesel exhaust particles generate reactive oxygen radicals and induce apoptosis in macrophages. J Immunol 163:5582–5591
Ignarro LJ (1989) Endothelium-derived nitric oxide: actions and properties. FASEB J 3:31–36
Ikeda M, Suzuki M, Watarai K, Sagai M, Tomita T (1995) Impairment of endothelium-dependent relaxation by diesel exhaust particles in rat thoracic aorta. Jpn J Pharmacol 68:183–189
Kumagai Y, Nakajima H, Midorikawa K, Homma-Tkakeda S, Shimojo N (1998) Inhibition of nitric oxide formation by neuronal nitric oxide synthase by quinines: nitric oxide synthase as a quinine reductase. Chem Res Toxicol 11:608–613
Kumagai Y, Hayashi T, Miyauchi T, Endo A, Iguchi A, Sakai MK, Sakai S, Yuki K, Kikushima M, Shimojo N (2001) Phenanthraquinone inhibits eNOS activity and suppresses vasorelaxation. Am J Physiol Regul Integr Comp Physiol 281:R25–R30
Kumagai Y, Koide S, Taguchi K, Endo A, Nakai Y, Yoshikawa T, Shimojo N (2002) Oxidation of proximal protein sulfhydryls by phenanthraquinone, a component of diesel exhaust particles. Chem Res Toxicol 15:483–489
Li N, Venkatesan MI, Miguel A, Kaplan R, Gujuluva C, Alam J, Nel AE (2000) Induction of heme oxygenase-1 expression in macrophages by diesel exhaust particle chemicals and quinines via the antioxidant-responsive element. J Immunol 165:3393–3401
Moncada S, Higgs A (1993) The l-arginine-nitric oxide pathway. N Engl J Med 329:2002–2012
Moncada S, Palmer RMJ, Higgs EA (1991) Nitric oxide: physiology, pathophysiology, and pharmacology. Pharmacol Rev 43:109–142
Palmer RMJ, Ferrige AG, Moncada S (1987) Release of nitric oxide accounts for the biological activity of endothelium-derived relaxing factor. Nature 327:524–526
Platt KL, Oesch F (1983) Efficient synthesis of non-K-region trans-dihydro diols of polycyclic aromatic hydrocarbons from o-quinone and catachol. J Org Chem 48:265–268
Pope CA III, Thun MJ, Namboodiri MM, Dockery DW, Evans JS, Speizer FE, Heath CW Jr (1995) Particulate air pollution as a predictor of mortality in a prospective study of US adults. Am J Respir Crit Care Med 151:669–674
Radomski MW, Palmer RM, Moncada S (1987) The anti-aggregating prostacyclin and nitric oxide. Br J Pharmacol 92:639–646
Sagai M, Saito H, Ichinose T, Kodama M, Mori Y (1993) Biological effects of diesel exhaust particles I In vitro production of superoxide and in vivo toxicity. Free Radic Biol Med 14:37–47
Stewart AG, Phan LH, Grigoriadis G (1994) Physiological and pathophysiological roles of nitric oxide. Microsurgery 15:693–699
Sugimoto R, Kumagai Y, Nakai Y, Ishii T (2005) 9,10-Phenanthraquinone in diesel exhaust particles downregulates Cu, Zn-SOD and HO-1 in human pulmonary epithelial cells: intracellular iron scavenger 1,10-phenanthroline affords protection against apoptosis. Free Radic Biol Med 38:388–395
Sun Y, Iemitsu M, Shimojo N, Miyauchi T, Amamiya M, Sumi D, Hayashi T, Sun GF, Shimojo N, Kumagai Y (2005) 2,4,6-Trinitrotoluene inhibits endothelial nitric oxide synthase activity and elevates blood pressure in rats. Arch Toxicol (in press)
Acknowledgments
We are especially grateful to Ms. F. Miyamasu for grammatical corrections in the preparation of this manuscript. This research was supported in part by Grant-in-Aid #15390184 and #15659141 (YK) for scientific research from the Ministry of Education, Science, Culture and Sports of Japan.
Author information
Authors and Affiliations
Corresponding author
Additional information
An erratum to this article can be found at http://dx.doi.org/10.1007/s00204-006-0127-8
Rights and permissions
About this article
Cite this article
Sun, Y., Taguchi, K., Sumi, D. et al. Inhibition of endothelial nitric oxide synthase activity and suppression of endothelium-dependent vasorelaxation by 1,2-naphthoquinone, a component of diesel exhaust particles. Arch Toxicol 80, 280–285 (2006). https://doi.org/10.1007/s00204-005-0043-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-005-0043-3