Abstract
The aim of the present work was to study the nephrotoxicity of aluminum lactate administered for 3 months (0.57 mg/100 g bodyweight aluminum, i.p., three times per week) to male Wistar rats. Renal function was studied after 6 weeks of treatment (urine was obtained from rats in metabolic cages) and at the end of the treatment using clearance techniques. Another group of rats was used as kidneys donors at the end of treatment. The renal cortex was separated and homogenized to determine glutathione (GSH) level, glutathione S-transferase (GST) activity and lipid peroxidation (LPO) level. Renal cortex slices were also used to study the p-aminohippuric acid (PAH) accumulation during steady-state conditions and the kinetics of uptake process. Clearance results, at the end of the treatment, indicated that renal functions in treated-rats were not different from those measured in control rats, although the renal concentration parameters differ when they were measured in treated rats after 24 h of food and water deprivation. Balances of water and sodium were also modified at both 1.5 and 3 months of treatment. The activity of alkaline phosphatase (AP) relative to inulin excreted in urine was significantly impaired: controls 2.2±0.6 IUI/mg, Al-treated 5.1±0.5 IU/mg, P<0.05. These data indicated that proximal tubular cells were loosing apical brush border membranes. Data obtained in cortex homogenates indicated that both GSH and GST activity were significantly decreased, and a significant increase of LPO was noted simultaneously in Al-treated rats. Renal accumulation of PAH, estimated as slice-to-medium ratio, decreased significantly in the Al-treated rats: control rats 3.06±0.02 (n=12), Al-treated rats 2.26±0.04 (n=12), P<0.0001. The maximal rate of uptake was also diminished in treated rats, while the apparent affinity remained unchanged. All these results indicate that aluminum accumulation in renal tissue affects cellular metabolism, promotes oxidative stress and induces alterations in renal tubular PAH transport, together with an impairment in sodium and water balance only detected under conditions of water deprivation, without other evident changes in glomerular filtration rate or other global functions measured by clearance techniques at least at this time of chronic toxicity.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The effect of renal failure on aluminum (Al) accumulation in different organs and the subsequent systemic toxicity is well known, but there are few reports about Al-induced nephrotoxicity. Various works reported that Al accumulates in mammalian tissues such as brain, bone, liver and kidney (Sahin et al. 1994; Wills et al. 1993; Gómez Alonso et al. 1990). This fact was observed simultaneously with renal failure (Alfrey 1980; Ecelbarger et al. 1994a) or associated with age (Ecelbarger et al. 1994a, 1994b). Aluminum is mainly excreted in urine. Different mechanisms of renal Al elimination, such as glomerular filtration (Yokel and McNamara 1985), tubular reabsorption of filtered Al (Burnatowska-Hledin et al. 1985) and excretion in the distal tubules (Monteagudo et al. 1988), have been suggested. Moreover, it has also been reported that aluminum accumulation in kidney promotes degeneration in renal tubular cells, and thus could induce nephrotoxicity (Ebina et al. 1984; Cacini and Yokel 1988; Berthold et al. 1989; Stein et al. 1987; Roy et al. 1991).
In a previous work we have reported that chronic administration of aluminum by parenteral exposure increased the renal tubular phosphate reabsorption, with an increase in the apparent maximal velocity without modifications in the apparent affinity (K m) (Mahieu and Calvo 1998).
The present study has been carried out to verify whether aluminum that accumulates in renal tissue due to chronic administration modifies other tubular transport mechanisms. Among them, carrier-mediated transport of xenobiotics and their metabolites system, known as organic anion transport (OAT) system, plays a critical role in protecting against the toxic effects of anionic substances and is target for the actions of many drugs and environmental toxicants (Sweet et al. 2001). A model drug for monitoring this transport system is p-aminohippuric acid (PAH); thus, we have studied the effects of aluminum on PAH accumulation in renal tissue. Furthermore, renal function was also studied by clearance techniques, and water and sodium balances in both normal and hydropenic conditions were also measured.
In addition, we analyzed a possible effect of Al on metabolic systems present in renal tissue that could be involved in the proper maintenance of renal function, including the secretion of organic anions. Renal glutathione (GSH) levels, and the activity of glutathione S-transferase (GST) play an important role in detoxification of electrophilic metabolites of xenobiotics and in protection against oxidative damage to membrane proteins and lipids, avoiding the increment in level of lipid peroxidation (LPO) (Reed 1990). We studied these biochemical components to gain insight into the biochemical outcome of aluminum toxicity (Reed 1990). In this connection, renal GSH levels determine normal renal function (Torres et al. 1986) and the nephrotoxicity of mercuric chloride (Girardi et al. 1989).
Methods
Animals and treatments
Male Wistar rats weighing between 300 and 350 g were studied to evaluate the effects of aluminum on renal function, biochemical parameters in renal cortex homogenates and the uptake of PAH in renal cortical slices. Animals were allowed free access to a standard diet and tap water. Treated rats were injected intraperitoneally three times per week for 12 weeks with a solution of aluminum lactate containing 0.57 mg Al and 5.68 mg anion lactate (pH 7.0) per 100 g bodyweight. Control rats were injected with sodium lactate containing 5.68 mg anion lactate (pH 7.0) per 100 g bodyweight, i.p., during the same period and at the same frequency. In all the experiments described in this manuscript, rats treated with sodium lactate presented no differences from control rats without any treatment, and thus we decided to call them control rats. Animals of both groups were kept in an environment at a steady temperature of 22°C with a light:dark cycle of 12 h:12 h. No differences between control and treated rats were observed in food intake and body weight during the treatment.
Experiments were performed in accordance with the Guiding Principles in the Use of Animals in Toxicology, adopted by the Society of Toxicology in 1989, and were approved by the committees of each institution.
Renal function measurements
To study the evolution of renal function, all the animals were submitted to renal function studies both after 6 weeks of treatment and at the end of the third month. For this purpose rats were maintained for 24 h in metabolic cages, and urine was collected. Sodium and water balance were measured, and the creatinine and protein excretion during the 24-h period were analyzed. The urine concentration capacity was also assessed. This procedure was performed with normal-hydrated rats and then in animals without access to water and food during 24 h. At the end of these periods, spontaneously voided urine was collected over 4 h, and blood was obtained from the tail vein. The ratio of urine to plasma osmolality (Uosm/Posm), and the urine excretion rate (V, μl/min) were calculated.
At the end of the experiment (12 weeks) and a day after the studies described above, the animals were anesthetized by injection of pentobarbital (50 mg/kg bodyweight, i.p) and were prepared for renal clearances studies as previously reported (Torres et al. 1986; Mahieu and Calvo 1998). The femoral vein and the femoral artery were cannulated. The bladder was exposed through a small abdominal incision and cannulated with a catheter (internal diameter 3 mm) for urine collection. A solution containing inulin (1 g/100 ml), sodium p-aminohippurate (PAH, 0.3 g/100 ml) and isotonic saline was infused through the femoral vein catheter at a rate of 4.1 ml/h using a constant-rate infusion pump (Sage Instruments, model 341-B-syringe pump). After equilibration for 60 min, urine samples were obtained during two periods of 30 min. Blood samples from the femoral artery were also obtained at the midpoint of each collection period. At the end of the experiments, blood was collected by heart puncture, the kidneys were separated and the cortex excised and placed in ice-cold Krebs-Ringer bicarbonate buffer solution (pH 7.4). This tissue was used to measure the oxidative state of renal tissue.
Urinary volume was measured, glomerular filtration rate (GFR) was determined by inulin clearance, and renal plasma flow was estimated by PAH clearance. Creatinine, urea, protein, and sodium concentrations and osmolality were measured in serum and urine samples. The aluminum level in serum was also determined. Alkaline phosphatase (AP) activity was measured in urine samples.
Biochemical studies in renal tissue
Renal tissue, prepared as stated above, was homogenized in order to determine the cytosolic activity of GST, non-protein sulfhydryl (NPSH) pool (principally GSH) and LPO. As each measurement requires different conditions, kidneys were excised, the cortex was separated and the tissue was divided as necessary. Determination of renal NPSH was carried out in homogenates prepared in cold 5% trichloroacetic acid in 0.01 M HCl as described by Ellman (1959). LPO was assayed as thiobarbituric acid (TBA)-reactive products, according to the method of Okhawa et al. (1979), in homogenates prepared in cold 1.15% KCl. To measure GST activity using 1-chloro2,4-dinitrobenzene (CDNB) as the substrate, renal tissue homogenates were prepared with sucrose 0.25 M containing 0.03 M buffer phosphate (pH 7.4) and Na2EDTA 1 mM, following the method of Habig et al. (1974). Aluminum concentration in renal tissue was also determined.
Renal cortical slices and medium preparation
Other groups of control rats and animals treated for 3 months were used as kidney donors. Renal cortical slices, approximately 0.5 mm, were prepared by freehand sectioning with a razor blade. Approximately 80–100 mg of sliced tissue (four to six slices randomly selected from the storage vessel) were placed in individual bakers containing 4 ml of the same buffer enriched with 10 mM glucose, 10 mM sodium lactate, 10 mM sodium acetate and 10 mM sodium pyruvate (pH 7.4)(Cross and Taggart 1950; Elías et al. 1982). All incubations were performed at 27°C in a Dubnoff metabolic shaker with a 95% O2/5% CO2 atmosphere. The tissue underwent a 20-min preincubation period in the buffer solution.
Measurement of accumulation of p-aminohippurate in kidney slices
After completion of the equilibration period, the slices were transferred to flasks containing 4 ml fresh Krebs-Ringer bicarbonate buffer with PAH (7×10−5 M) and inulin (4 mg/ml) for estimation of the extracellular water, and were then incubated for 60 min. Then the slices were removed quickly, gently blotted on filter paper, weighed and homogenized in 1 ml distilled water. A 1-ml aliquot of the respective incubation medium was also removed, and from this point both the homogenate and the incubation medium were treated identically. After addition of 1.5 ml 10% trichloroacetic acid and 2.5 ml distilled water, each sample was centrifuged. Both PAH and inulin concentrations were determined in the supernatants. Data were expressed as the slice-to-medium concentration ratio (S/M), where slice concentration is expressed as milligrams PAH per gram of wet tissue, and medium concentration is in milligram PAH per milliliter of medium.
Determination of kinetics of p-aminohippurate uptake
Following the equilibration period, the slices were transferred to flasks containing 4 ml fresh medium and PAH. The rate of PAH uptake by renal cortical slices was determined during a 15-min incubation at various PAH concentrations (50–1400 μM). At the end of the incubation the slices were treated as described above. Using duplicate flasks for each experimental point, slices were incubated for 60 min in a medium containing inulin (4 mg/ml) for the estimation of the extracellular water. The concentration of PAH in the cells was calculated by subtraction of the amount of extracellular PAH, as calculated from inulin space, from the total slice PAH content. The apparent kinetic parameters (V max and K m) were derived from nonlinear regression (Michaelis-Menten equation). Kinetics studies were also carried out under a gas phase of 100% N2 to determine PAH uptake in the absence of oxygen.
Determination of cellular functional parameters
The effect of Al on inulin space, total tissue water content, and intracellular sodium and potassium concentrations were studied. Slices were incubated for 60 min in 4 ml medium containing inulin (4 mg/ml). Following incubation the slices were blotted and weighed and then homogenized for determination of inulin space. To determine total water content of tissue, a duplicate series of slices were dried following incubation for 24 h at 100°C. The dried tissue was then extracted in 1 N HNO3 for 48 h and analyzed for electrolytes. Values were corrected for extracellular water content estimated for each experiment, and expressed as milli Eqivalents per liter of intracellular water.
Analytical methods
Determination of creatinine, protein and urea in serum were measured by use of an autoanalyzer. AP was measured with a commercial kit according to the manufacturer's directions (Wiener Laboratories, Rosario, Argentina). Inulin and PAH concentrations in the samples were determined by, respectively, Roe's procedure (Roe et al. 1949) and Brun's method as modified by Waugh and Beall (1974). Sodium and potassium levels were determined by flame photometry. Al content in serum and in the kidneys was measured by atomic absorption spectroscopy in graphite ovens.
Statistical analysis
Results are expressed as means ±SEM. Comparison between control and treated groups was carried out using Mann-Whitney U-test or Student's t-test as indicated. Regression lines were calculated by the method of least squares. Each point represents the average of triplicate determinations. The statistical analysis was performed with the SPSS program (Statistical Package for Social Sciences 1995).
Results
There were no consistent clinical signs observed among the aluminum-treated rats and controls. Neither body weight nor kidney weight were statistically different between groups, although rats treated with Al presented higher serum Al concentration and a higher amount of the metal in the renal tissue. The values are presented in Table 1.
Effect of aluminum on renal functions measured after 6-weeks and 3-months treatment with aluminum lactate
Table 2 shows systemic and urine parameters at the end of the experiment. Creatinine, urea and protein concentrations in plasma in treated rats were not different from those in controls, and neither was the 24-h excretion of creatinine. The urine excretion rate of proteins in treated rats was higher than that of controls.
Results of water and sodium balances are presented in Table 3. Data represent the values determined after 6 weeks and 3 months of treatment, and revealed that Al induced a failure in the balance of water and sodium, together with an increase in the excretion of sodium, after 6 weeks of treatment. After 3 months, the treated rats presented higher diuresis with less osmolality. These results indicated a development of tubular injury, at least from 6 weeks of treatment, without changes in the 24-h creatinine excretion, since at the end of the treatment the animals presented an increase in the urine volume with a diminution in urine concentration, while creatinine excretion rate maintained as controls.
The urine concentration ability was measured under normal hydration and hydropenic conditions. These values were measured after 3 months of treatment. This experimental group allowed us to describe a significant failure in the treated rats to concentrate the urine after being water-deprived (Table 4).
GFR estimated from the inulin clearance, and cortical renal flow estimated from PAH clearance were also assessed (Table 5). No differences were observed in these values but a significant increase in fractional sodium excretion in Al-treated rats was measured. AP values relative to inulin excreted in the urine increased (controls 2.2±0.6 IU/mg, Al-treated 5.1±0.5 IU/mg, P<0.05).
Biochemical studies in homogenates of renal cortex
The results are presented in Fig. 1. Data indicated that both GSH levels and GST activity, with CDNB as substrate, were significantly decreased by the treatment, and that a simultaneous and significant increase of LPO is noted in Al-treated rats.
Effects of aluminum on the activity of glutathion-S-transferase (GST), gluthathione (GSH) levels and the levels of lipid peroxidation (LPO) measured in renal cortical homogenates. Al-treated rats (n=9) received a solution containing aluminum lactate during 12 weeks (0.57 mg Al/100 g bodyweight, i.p., three times per week). Control rats (n=8) were injected with sodium lactate following the same schedule. Each result is the mean ±SEM. *P<0.05, compared with control
Effect of aluminum on the accumulation of p-aminohippurate in renal cortical slices
Tissue accumulation of PAH, estimated as S/M ratio, decreased significantly in the Al-treated rats. Values were: control rats 3.06±0.02 (n=12), Al-treated rats 2.26±0.04 (n=12), P<0.0001.
Effect of aluminum on the kinetics of p-aminohippurate uptake in renal cortical slices
The kinetics of PAH uptake as a function of PAH concentration in the incubation medium, under either O2 or N2 is presented in Fig. 2. The rate of uptake under the aerobic condition was nonlinear and higher than the linear PAH uptake under the anaerobic condition. As shown in the figure, the presence of aluminum in the tissue inhibited only the aerobic PAH uptake. Figure 2also shows the resulting points obtained when the linear component was subtracted from the nonlinear function. The points approached a stable value that was decreased by the presence of aluminum. The values calculated from these curves indicating the effect of aluminum on aerobic PAH uptake were: V max (μmol/15 min per g wet tissue)in control rats 0.25±0.01 (n=12), and in Al-treated rats 0.10±0.01 (n=12), P<0.001; and K m (μM) in control rats 97.2±13, and in Al-treated rats 89.8±17 (n indicating the number of rats used, with each point on the curve being the mean ±SEM of four to six values).
Effect of aluminum on the rate of p-aminohippurate (PAH) uptake by rat renal cortical slices. Al-treated rats (n=12) received a solution containing aluminum lactate during 3 months (0.57 mg Al/100 g bodyweight, i.p., three times per week). Control rats (n=12) were injected with sodium lactate following the same schedule. Solid circles represent the results from control slices incubated under 95% O2/5% CO2. Each point represent the mean ±SEM of 4–6 experiments, and the line is the regression fit to the Michaelis Menten equation. Solid squares represent the results from control slices incubated under 100% N2. Each point is the mean±SEM of 4–6 experiments, and the line is the linear regression. Subtraction of the values corresponding to the linear component from the nonlinear component at the same PAH concentration in control preparations is described with the solid line without symbols. Open circles represent the results from Al-treated slices incubated under 95% O2/5% CO2. Each point is the mean ±SEM of six experiments, and the line is the regression fit to the Michaelis-Menten equation. Open squares represent the results from Al-treated slices incubated under 100% N2. Each point is the mean ±SEM of six experiments, and the line is the linear regression. Subtraction of the values corresponding to the linear component from the nonlinear component at the same PAH concentration in Al-treated preparations is described with the dashed line without symbols
Effect of aluminum on cellular functional parameters
Table 6 indicates that the slices from Al-treated rats did not exhibit significant changes in the parameters representing general cell function compared with controls.
Discussion
Aluminum is a widely distributed metal to which all humans are continuously exposed. Although aluminum is present in only trace amounts in most biological systems, this cation accumulates in certain disease states such as end-stage renal disease (Quarles 1991; Cucarella et al. 1998). Such accumulation is implicated in the pathogenesis of suppressed parathyroid hormone secretion, bone disease, anemia, and of the central nervous system in end-stage renal failure (Quarles 1991; Lin et al. 1996). Aluminum is excreted by the kidneys (Sutherland and Greger 1998). It has also been reported that the renal cortex has the ability to accumulate aluminum against a concentration gradient and that the capacity for accumulation is high (Cacini and Yokel 1988).
Our work shows that several changes may occur in renal function after prolonged exposure of rats but without a marked renal failure, other than a higher excretion rate of proteins, in spite of the large amount of aluminum measured in renal tissue. Moreover, we could detect renal alterations by using balance-studies of sodium and water, and by the urine concentrating capacity, without changes in systemic parameters. It is remarkable that these failures were observed under stress conditions or during balance experiments, suggesting actual targets in different renal segments, and indicating that tubular transport systems could be affected in Al-induced nephrotoxicity. Furthermore, previous works from our laboratory demonstrated changes in renal handling of calcium and inorganic phosphate, without changes in GFR, and in fractional excretion of water. These results were observed together with a diminution in nephrogenic excretion of cAMP (Mahieu and Calvo 1998).
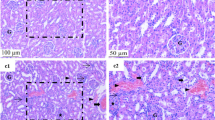
Our data indicated no differences in GFR nor in the renal blood flow. On the other hand, we described a higher excretion of proteins together with a higher alkaline phosphatase activity in urine, compared with control samples. The higher activity of alkaline phosphatase could be indicative that proximal tubular cells are loosing apical brush border membranes. It has been reported as a chronic cytotoxic renal effect of Al in kidney using light and electron microscopy. These results indicated atrophy of some tubules, interstitial fibrosis, and some glomerules that were undergoing partial sclerosis (Somova et al. 1997).
To gain insight of further changes in transport systems in renal proximal cells we studied the effects of aluminum on PAH transport using renal cortical slices obtained from rats treated in vivo. This transport system is energetically uphill and is accomplished by tertiary active process. Substrate entry across the basolateral membrane is driven by indirect coupling to the sodium gradient maintained by Na–K-ATPase. Luminal exit across the brush border membrane is presumed to occur via anion exchange and/or facilitated diffusion (Sweet et al. 2001). It has been pointed out that tubular lumens are collapsed in slices of renal cortical tissue (Wedden and Vyas 1978), and thus transport events observed in this preparation would reflect preponderantly processes localized at the basolateral cell membrane (Foulkes 1971; Tune and Burg 1971). Therefore, accumulation of PAH in renal slices could reflect the rate of active transport from medium to cell and passive efflux from cell to medium at the basolateral cell membrane, and/or alterations in the metabolic machinery of the tubular cells that assures the active transport systems.
PAH transport as measured with the S/M ratio, an indicator of its steady-state accumulation, was diminished by the presence of aluminum in renal slices. The study of the kinetics data indicated a decrease in the aerobic and saturable transport of PAH without changes in the apparent affinity of PAH for the carrier system. Since no modification in total water content, inulin space, or ionic distribution could be observed, we can assume that the tubular cells' membrane permeability remained unaffected. This fact could explain why the anaerobic component is maintained in the presence of N2 atmosphere, and is not affected by aluminum. Thus, we might conclude that aluminum affected active PAH transport in basolateral membranes or the cellular regulation of the system. In this connection, we have found no changes in PAH clearance, which was used as a measure of cortical renal flow. Our interpretation of these contradictory results is that they could be due to the maintained affinity of the transport system as observed in vitro experiments stated above. The PAH concentration adjusted in plasma to assure a maximal arterio-venous PAH extraction (100 μM), and thus simplified the PAH clearance determination, could be low enough to maintain a proper uptake by renal tubules.
Certain work indicated that metabolism is an important intracellular event associated with the renal disposition of anionic xenobiotics. Both phase I and phase II reactions of biotransformations are present in kidneys (Lohr et al. 1998). Among these reactions the formation and degradation of glutathione S-conjugates is well developed in renal cells (Commandeur et al. 1995). Renal tissue obtained from aluminum-treated rats presented a diminution in GST activity using CDNB as subtrate, together with diminution in GSH, and an increase in LPO. Although aluminum has not been described as a metal that reacts with GSH and decreases free GSH in tissue, like mercury has (Girardi and Elías 1991), the increase of LPO could indicate an increase of oxidation reactions levels. This oxidative increment could promote the diminished GSH level, and also could modify the activity of the proteins in membrane (i.e., OTA) or cytosol (i.e., GST). It has been reported that acute intraperitoneal administration of aluminum induces a temporal diminution of GSH in liver, increases hemooxygenase activity with reduction of cytochrome P450 and, later, an increase in LPO (Jeffery et al. 1996). Other authors indicated that aluminum accumulation in liver was accompanied by a decreased GSH level and in a decrease in glutathione peroxidase (El-Maraghy et al. 2001), while, in adult mice, exposure to aluminum was proved to inhibit δ-aminolevulinate dehydratase activity of kidneys (Schetinger et al. 1999). Data described in this work do not allow us to determine the order of development of the events studied. The different results have indicated that aluminum could affect cellular metabolism by promoting oxidative stress and, thus, could promote alterations in renal proximal cells.
We conclude that chronic accumulation of aluminum might induce nephrotoxicity without important changes in global renal function but by modifying the cellular regulation of renal functions such as transport and metabolism. The identification of the actual target of aluminum in renal tissue is under study in our laboratory.
References
Alfrey AC (1980) Metabolism and toxicity of aluminum in renal failure. Am J Clin Nutr 33:1509–1516
Berthold R, Herman M, Savory J, Carpenter R, Sturgill CB, Katsetos CD, Vandenberg SR, Wills M (1989) A long-term intravenous model of aluminum maltol toxicity in rabbits: tissue distribution, hepatic, renal and neuronal cytoskeletal changes associated with systemic exposure. Toxicol Appl Pharmacol 98:58–74
Burnatowska-Hledin MA, Mayor GH, Lau K (1985) Renal handling of aluminum in the rat: clearance and micropuncture studies. Am J Physiol 249:F192–F197
Cacini W, Yokel RA (1988) Accumulation of aluminum by rabbit renal cortex. Res Commun Chem Pathol Pharmacol 59:93–105
Commandeur JN, Stijntjes GJ, Vermeulen NP (1995) Enzymes and transport systems involved in the formation and disposition of glutathione S-conjugates. Role in bioactivation and detoxication mechanisms of xenobiotics. Pharmacol Rev 47:271–330
Cross RT, Taggart, JV (1950) Renal tubular transport: accumulation of p-aminohippurate by rabbit kidney slices. Am J Physiol 161:181–190
Cucarella C, Montoliu C, Hermenegildo C, Saez R, Manzo L, Minana MD, Felipo V (1998) Chronic exposure to aluminum impairs neuronal glutamate–nitric oxide–cyclic GMP pathway. J Neurochem 70:1609–1614
Ebina Y, Okada S, Hamazaki S, Midorikawa O (1984) Liver, kidney and central nervous system toxicity of aluminum given intraperitoneally to rats: a multiple dose subchronic study using aluminum nitriloacetate. Toxicol Appl Pharmacol 75:211–218
Ecelbarger CA, MacNeil GG, Greger JL (1994a) Importance of kidney function and duration of exposure on aluminum accumulation in mature rats. Nutr Res 14:577–586
Ecelbarger CA, MacNeil GG, Greger JL (1994b) Tissue aluminum accumulation and toxic consequences in rats chronically fed aluminum with and without citrate. J Agric Food Chem 42:2220–2224
Elías MM, Comin EJ, Grosman ME, Galeazzi SA, Rodriguez Garay EA (1982) Inhibitory effect of unconjugated bilirubin on p-aminohippurate transport in rat kidney cortex slices. Biochim Biophys Acta 693:265–272
Ellman GL (1959) Tissue sulphydryls groups. Arch Biochem Biophys 82:70–73
El-Maraghy SA, Gad MZ, Fahim AT, Hamdy MA, (2001) Effect of cadmium and aluminum intake on the antioxidant status and lipid peroxidation in rats tissues. J Biochem Mol Toxicol 15:207–214
Foulkes EC (1971) Effects of heavy metals on renal aspartate transport and the nature of solute movement in kidney cortex slices. Biochim Biophys Acta 241:815–822
Girardi G, Elías MM (1991) Effectiveness of N-acetylcysteine in protecting mercuric chloride-induced nephrotoxicity. Toxicology 67:155–164
Girardi G, Torres AM, Elías MM (1989) The implication of renal glutathione levels in mercuric chloride nephrotoxicity. Toxicology 58:187–195
Gómez Alonso C, Fernández Martín JL, Menéndez Rodríguez P, Fernández Soto Y, Virgos MJ, Cannata JB (1990) Aluminum body burden with normal renal function: risk of oral intoxication. Nefrología 10:386–392
Habig WH, Pabst MJ, Jakoby WB (1974) Glutathione S-transferases. The first enzymatic step in mercapturic acid formation. J Biol Chem 249:7130–7139
Jeffery EH, Abreo K, Burgess E, Cannata JB, Greger JL (1996) Systemic aluminum toxicity: effects on bone, hematopoietic tissue and kidney. J Toxicol Environ Health 48:649–665
Lin JL, Kou MT, Leu ML (1996) Effect of low-term low-dose aluminum-containing agents on hemoglobin synthesis in patients with chronic renal insufficiency. Nephron 74:33–38
Lohr JW, Willisky GR, Acara MA (1998) Renal drug metabolism. Pharmacol Rev 50:107–141
Mahieu S, Calvo ML (1998) Effect of the chronic poisoning with aluminum on the renal handling of phosphate in the rat. Toxicol Lett 94:47–56
Monteagudo FSE, Isaacson LC, Wilson G, Hickman R, Folb PI (1988) Aluminum excretion by the distal tubule of the pig kidney. Nephron 49:245–250
Ohkawa H, Ohishi N, Yagi K (1979) Assay of lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95:351–357
Quarles LD (1991) Paradoxical toxic and trophic osseous actions of aluminum: potential explanations. Miner Electrolyte Metab 17:233–239
Reed DJ (1990) Glutathione. Toxicological implications. Annu Rev Pharmacol Toxicol 30:603–631
Roe HH, Epstein JH, Goldstein NP (1949) A photometric method for determination of inulin in plasma and urine. J Biol Chem 178:839–845
Roy AK, Talukder G, Sharma A (1991) Similar effects in vivo of two aluminum salts on the liver, kidney, bone and brain of Rattus novergicus. Bull Environ Contam Toxicol 47:228–295
Sahin G, Varol I, Temizer A (1994) Determination of aluminum levels in the kidney, liver and brain of mice treated with aluminum hydroxide. Biol Trace Elem Res 41:129–135
Schetinger MR, Bonan CD, Morsch VM, Bohrer D, Valentim LM, Rodrigues SR (1999) Effects of aluminum sulfate on δ-aminolevulinate dehydratase from kidney, brain and liver of adult mice. Braz J Med Biol Res 32:761–766
Somova LI, Missankov A, Khan MS (1997) Chronic aluminum intoxication in rats: dose-dependent morphological changes. Methods Find Exp Clin Pharmacol 19:599–604
Stein G, Laske V, Muller A, Braunlich H, Lin BW, Fleck G (1987) Aluminum induced damage of the lysosomes in the liver, spleen, and kidney of rats. J Appl Toxicol 7:253–258
Sutherland JE, Greger JL (1998) Kinetics of aluminum disposition after ingestion of low moderate pharmacological doses of aluminum. Toxicology 126:115–125
Sweet D, Bush K, Nigam S (2001) The organic anion transporter family; from physiology to ontogeny and the clinic. Am J Physiol 281:F197–F205
Torres AM, Rodriguez JV, Ochoa JE, Elías MM (1986) Rat kidney function related to tissue glutathione levels. Biochem Pharmacol 35:3355–3358
Tune BM, Burg MB (1971) Glucose transport by proximal renal tubules. Am J Physiol 221:580–585
Waugh WH, Beall PT (1974) Simplified measurement of para-aminohippuric acid and other arylamines in plasma and urine. Kidney Int 5:429–436
Wedden RP, Vyas BT (1978) Phlorizin stimulation of p-aminohippurate uptake in rat kidney cortex slices. Kidney Int 14:158–168
Wills MR, Hewitt CD, Sturgill BC, Savory J, Herman MM (1993) Long term oral and intravenous aluminum administration in rabbits. 1. Renal and hepatic changes. Ann Clin Lab Sci 23:1–16
Yokel RA, McNamara PJ (1988)Aluminum bioavailability and disposition in adult and immature rabbits. Toxicol Appl Pharmacol 77:344–352
Acknowledgements
The authors express their appreciation for the technical assistance in statistical analyses to Lic Elena Carrera. This work was supported by grants from Universidad Nacional del Litoral, Argentina (Program C.A.I. + D).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mahieu, S.T., Gionotti, M., Millen, N. et al. Effect of chronic accumulation of aluminum on renal function, cortical renal oxidative stress and cortical renal organic anion transport in rats. Arch Toxicol 77, 605–612 (2003). https://doi.org/10.1007/s00204-003-0496-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-003-0496-1