Abstract
This study characterizes the molecular neurotoxicity of diesel exhaust (DE) on the tachykinin substance P (SP) signaling system in the lungs. A total of 96 female Fischer 344/NH rats (~175 g, ~4 weeks old) were randomly assigned to eight groups in a 2×4 factorial design: capsaicin versus non-capsaicin (vehicle) pretreatment, and filtered room air versus two exposure levels of DE with diesel engine room control. The rats were exposed nose-only to room air or low (35.3 µg/m3) and high concentrations (669.3 µg/m3) particulates directly from a Cummins N14 research engine at 75% throttle for 4 h/day, 5 days/week, for 3 weeks. The findings showed that exposure to DE dose-dependently induced bronchopulmonary neurogenic inflammation, both in capsaicin- and vehicle-pretreated rats, as measured by plasma extravasation, edema, and inflammatory cells. DE inhalation affected the SP signaling processes, including stored SP depletion and the gene/protein overexpression for neurokinin-1 receptor. DE also significantly reduced the activity of neutral endopeptidase, a main degradation enzyme for SP. Consequently, these changes may be regarded as critical factors that switched neurogenic pulmonary responses from their protective functions to a detrimental role that perpetuates lung inflammation. These changes may possibly be associated with the mass concentration of DE particles due to their physico-chemical characteristics. Moreover, capsaicin-pretreated rats had more sensitivity to these levels of DE exposure due to stimulation of bronchopulmonary C-fibers. However, the effects of capsaicin treatment were not consistent and apparent in this study. Taken together, our findings suggest that neurokininergic mechanisms may possibly be involved in DE-induced lung inflammation, but that bronchopulmonary C-fibers did not dominate DE-induced inflammatory abnormalities.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Diesel exhaust (DE) is a mixture of gases, vapors, semivolatile organic compounds, and fine particles emitted by diesel-fueled compression-ignition engines. DE exposure has been a major issue for occupational and environmental health (Delfino 2002). Of specific concern are (1) oxides of nitrogen, which are ozone precursors, and (2) DE particles (DEP) because they all are respirable and have many chemicals adsorbed on their surfaces, including known or suspected mutagens and carcinogens (American Thoracic Society 1996). The daily average ambient concentrations of DEP have been documented to be 0.04–0.134 mg/m3 for truck drivers, 0.004–0.192 mg/m3 for railroad workers, and 8–42 µg/m3 for near road residency (WHO 1996). A huge body of cellular, animal, and human investigations of DE or its contents has been substantially conducted and critically reviewed (HEI 1995; 1999; California EPA 1998; Mauderly 1999; Sydbom et al. 2001; EPA 2002). Exposures to DE are associated with cough, sputum production, and lung function decrements. In addition to these symptoms, exposure studies in healthy humans demonstrated a number of profound inflammatory changes in the airways, notably before changes in pulmonary function could be detected (Salvi et al. 1999, 2000). Many adverse effects of diesel exhaust, both in vivo and in vitro, have been associated with asthma (Pandya et al. 2002), chronic obstructive pulmonary diseases (Mauderly et al., 1989), respiratory tract inflammation (Nikula et al. 1997), allergies (Hashimoto et al. 2001), and lung cancer (Iwai et al. 2000; Dawson and Alexeeff 2001). However, early action mechanisms of ambient DE toxicity, especially by generated particulates, are still unclear due to DE's complex nature and exposure conditions.
The tachykinin substance P (SP) has been demonstrated to play an important role, mediated through neurokinin-1 receptor (NK-1R) on effector cells, in initiating and regulating the severity of inflammatory processes (Killingsworth et al. 1996; Bozic et al. 1996). Subsequent to its release from afferent nerve endings, SP increases substantial responses, such as an increase of microvascular permeability, promotion of plasma extravasation, and priming of other inflammatory mediators. These effects are mostly modulated by neutral endopeptidase (NEP) through degradative cleavage of SP. In addition, there is recent evidence that immuno-inflammatory cells, such as macrophages (Killingsworth et al. 1997), lymphocytes (Lambrecht 2001), and leukocytes (Lambrecht 1987) also express the SP gene and protein. Although the basic function of SP is well documented, limited studies in vivo and in vitro have applied emerging molecular investigations of this tachykinin to explore the adverse effects of DE exposure. Experiments utilizing residual oil fly ash (Veronesi and Oortgiesen 2001) have demonstrated that afferent neural fibers play a crucial role in mediating a variety of inflammatory mechanisms following airborne pollutant exposure. Additional studies have indicated that these nerves are sensitive to many air pollutants, such as ozone (Jimba et al. 1995; Delaunois et al. 1997), SO2 (Long et al. 1999), NO2 (Lucchini et al. 1996; Joad et al. 1997), and cigarette smoke (Bonham et al. 1996). However, molecular tachykinergic mechanisms are relatively unknown in the pathogenesis of DE-induced inflammatory responses.
It seems reasonable to speculate that exposure to DE may result in neurogenic inflammation through bronchopulmonary C-fiber afferents. Due to its complexity, DE may have overlapping toxicity on tachykinin processing and its regulatory enzymes. To this end, we hypothesize that inhaled DE induces bronchopulmonary neurogenic inflammation that is mediated by the tachykinin substance P (SP), released from sensory C-fiber endings and others, acting via the NK-1R. In this study, we have demonstrated that inhalation of DE at the ambient pollution level for 4 h/day, 5 days/week during 3 weeks, induces neurogenic inflammation in the lungs involving overlapping tachykinergic mechanisms.
Materials and methods
Animals
A total of 96 specific-pathogen-free female Fischer 344/NH (F344/NH, weighing ~175 g, and 4±1 weeks old) were utilized for this study. All rats were housed in the American Association of Animal Laboratory and Care (AAALAC)-approved animal facility at the University of Wisconsin-Madison, School of Veterinary Medicine. In rats, SP-immunoreactive nerves have been demonstrated in the airways from the pharynx down to the terminal bronchioles and the alveolar septal level (Krause et al. 1993; Okamoto et al. 1993; Jimba et al. 1995; Szarek and Spurlock 1997). The rat has similar SP distribution in the lung to that of young children, but different from adults. Examination of autopsy specimens of children has revealed SP-containing nerves in the airways from bronchii to the alveolar ducts. Fischer 344 rats promise to offer insight into predisposing or acquired conditions that may contribute to the sensitive phenomenon of children exposed to DE. Female rats only were utilized to limit the gender-induced sample size. The rats, two per cage, were on a 12 h/12 h light/dark cycle and were given a standard rat chow diet /tap water ad libitum. The rats were randomly assigned to eight groups in a 2×4 factorial design: capsaicin versus non-capsaicin (vehicle) pretreatment, and filtered room air versus two concentrations of DEP and diesel engine room air.
Capsaicin pretreatment
The rats were anesthetized with ketamine HCL intramuscularly (50 mg/kg; Research Biochemicals International, Natick, MA, USA), xylazine (8 mg/kg i.m.; Fort Dodge Laboratories, Fort Dodge, IA,USA), and acepromazine maleate (1 mg/kg i.m.; Fort Dodge Laboratories). Half of all rats in each group (n=24) were injected intraperitoneally with capsaicin, a pungent ingredient of hot pepper (40 mg/kg, 98% purity; Sigma, St. Louis, MO, USA) in six injections over 2 days according to a published protocol (Tjen-A-Looi et al. 1998). The rats were also treated with theophylline (2 mg/kg i.p.; American Regent Laboratories, Inc., Shirley, NY, USA) and terbutaline (0.2 mg/kg i.p.; Geigy) to counteract bronchoconstriction and excessive mucus secretion during capsaicin treatment. The remaining rats were treated with six injections of vehicle in place of capsaicin. The rats were examined by the webbing test 3–5 days later (day zero of the experiment) to confirm the efficacy of the capsaicin pretreatment. At the end of exhaust exposure, SP and its co-located neuropeptide, calcitonin gene-related peptide (CGRP), were quantitated in the lung tissues of the test and control rats using enzyme immunoassay (EIA).
Diesel exhaust exposure
The rats were exposed to filtered room air or low and high levels of DE for 4 h/day, 5 days/week during 3 weeks. DE dosage was derived not only from the WHO-documented practical ambient particulate pollution levels (WHO 1996), but also from the newly implemented 24-h EPA standard of particles smaller than 2.5 µm in aerodynamic diameter (PM2.5). The rats were exposed through a nose-only exposure chamber (InTox, Albuquerque, NM, USA). This route was chosen to model practical exposure patterns and prevent possible afferent responses due to intratracheal instillation itself. The engine-room rats were kept beside the DE animal-exposure chamber during exposure and were breathing room air, whereas the filtered-air controls were kept in the animal holding facility.
The protocols regarding engine bench setup, operation, sampling/measurement, and detailed particle characterization and chemical composition of the exposure system have been substantially described in previous publications (Kweon et al. 2002, 2003). Briefly, a research single-cylinder 4-cycle diesel engine, adapted from an in-line six-cylinder Cummins N14-series, was utilized in this study. This engine has a low swirl, turbo-charged, 4-valve, centrally located direct-injection combustion system. The properties of Mobil diesel fuel used in this study are shown in Table 1. Based on in-depth analyses on emissions of the California Air Resource Board (CARB) 8-Mode test matrix, we ran the engine at an operating mode 6, a 75% load condition at 1200 rpm. The mode 6 is characterized by a relative higher ratio of particles and lower level of organic compounds generated by diesel fuel and the lubricating oil among CARB 8 modes (Kweon et al. 2002; 2003). Our previous data indicated that the majority of the hopanes and steranes just contained in the lubricating oil were produced at light loads, especially at 25% and 50% loads at the engine speed of 1200 rpm (Kweon et al. 2003). We monitored quantitatively the engine operating conditions in real-time using a mass flow controller and a tapered element oscillating microbalance for particulate concentration. More precise filter-based measurements were used to fully characterize the exposures after the experiments had been completed (Schauer et al. 1999a; 1999b).
The augmented sampling systems allowed engine exhaust emissions to be diluted to near ambient temperature, pressure, and concentrations, such that sampling and chemical analysis techniques used for monitoring ambient particulate matter can be used for characterization of the exhaust emissions. The sampling system was made with electrically non-chargeable materials, such as 304, 316, and 316L stainless steels. In addition, the surface temperature of the residence time chamber was controlled to be approximately the same as the inside gas temperature by using four rows of heated bands and respective temperature controllers. A TSI 3936L10 Scanning Mobility Particle Sizer, including a TSI Model 3081 Electrostatic Classifier, a TSI Model 3077 Kr-85 Aerosol Neutralizer, and a TSI Model 3010 Condensation Particle Counter (TSI, Shoreview, MN, USA), were used for measurement of particle number concentrations and size distributions. Particle volume concentrations were obtained by assuming that the particle shape is spherical. Gaseous emissions, such as nitrogen oxides (NOx), carbon monoxide (CO), total hydrocarbon, and carbon dioxide (CO2), were measured using a Raw Engine Exhaust Emissions System (California Analytical Instruments, Orange, CA, USA). This gaseous emission system consists of a Model 300 heated flame ionization detector, total hydrocarbon analyzer, a Model 400 heated chemiluminescence detector, NO/NOx analyzer, and a Model 300 infrared gas analyzer for CO and CO2. The relative humidity of the diluted gases was measured with dry- and wet-bulb thermometers installed in one of the sampling ports.
Three Teflon membrane filters (47 mm diameter, 2 µm pore size, Gelman Teflo; Gelman Sciences, Ann Arbor, MI, USA) were used for gravimetric determination of PM2.5, measurement of sulfate ions by ion chromatography (IC; Mueller et al. 1978), and analysis of trace metals by inductively coupled plasma mass spectrometry (ICP-MS; Lough et al. 2000), respectively. One baked-quartz fiber filter (47 mm diameter, Pallflex Tissuequartz 2500 QAO) was used for determination of elemental and organic carbon, which were analyzed with a Sunset Laboratories Carbon Analyzer (Forest Grove, OR, USA), the operation of which was according to NIOSH method 5040. Another three baked-quartz fiber filters operated in parallel, which were then followed by a polyurethane foam (PUF) cartridge (Atlas Foam; density 0.022 g/cm3, ILD 30, 5.7 cm diameter, 7.6 cm long) in series. The particle-phase organic compounds were collected on the three quartz fiber filters and the PUF cartridges downstream of the filters collected semi-volatile organic compounds. The sampled filters and PUF cartridges were analyzed with a HP5973 gas chromatography/mass spectrometry (GC/MS) system with a 30-m HP-5MS GC column.
After leaving the tertiary dilution tunnel, the dilution ratio ranged between 170- and 290-fold, and 110- and 190-fold for the low and high levels of DE, respectively, and the emissions were routed to the animal exposure chamber. A flow-balancing system was established for the animal exposure chamber, which ensured that the chamber pressure was very slightly above atmospheric. This arrangement ensured that there would be no external dilution of the gases being breathed by the animals while not stressing the animals' respiratory systems through an abnormal pressure environment. The average ambient temperature inside the animal loading tubes was around 25°C.
Plasma extravasation
After DE exposure, the rats were anesthetized with our previously mentioned anesthetic mixture. Briefly, the right jugular vein of selected rats (n=6 per group) was cannulated and a bolus of 100 µCi/kg 99mTechnetium-labeled albumin (99mTc-albumin) was administered. A blood sample of 0.3 ml was taken 2 min later, for estimation of blood radioactivity and packed cell volume (PCV). After a further 10 min, abdominal and thoracic cavities were opened and a clamp was placed on the thoracic vena cava. The abdominal vena cava was severed and a blood sample collected for estimation of blood radioactivity and PCV. A total of 20 ml isotonic saline (5 ml/min) was infused to expel residual intravascular 99mTc-albumin. The trachea with extrapulmonary parts of bronchi and left lung lobes were dissected free, was gently blotted dry on filter paper and weighed, and the radioactivity was measured in a Ludlum gamma-counter (Model 44-62; Sweetwater, TX, USA). The specific plasma leakage in extra- and intra-pulmonary airways (microliters per gram wet weight tissue) were calculated by dividing the tissue radioactivity by the product of the 99mTc-albumin plasma radioactivity and the weight of each tissue sample to obtain the volume of extravascular plasma per gram of tissue.
Real-time polymerase chain reaction (PCR) assay
Lung tissue was stored in RNAlater (Ambion, Austin, TX, USA) at 20°C. From each sample (n=6), 75 mg was homogenized in the presence of guanidinium isothiocyanate, and total RNA was isolated using an RNAqueous-4PCR kit (Ambion). Residual DNA was digested by thorough treatment with 5 U deoxyribonuclease I at 37°C for 45 min, followed by inactivation with 1/10 volume of inactivation reagent. First strand cDNA was synthesized from 2 µg total RNA in a volume of 20 µl containing 1× reverse transcriptase (RT) buffer with 0.5 mM each dNTPs, 0.5 U/µl RNase inhibitor (Ambion), 5 µM oligo (deoxythymidine)15 primer, and 4 U Omniscript reverse transcriptase (Qiagen, Valencia, CA, USA). For no-template control samples, RNA was replaced by H2O. A negative control reaction omitting the reverse transcriptase (RT) was also performed for each DNase-treated RNA sample. All samples were reverse transcribed under the same conditions and from the same reverse transcription master mix in order to minimize differences in reverse transcription efficiency.
A series of standards were prepared by performing ten-fold serial dilutions of full-length β-preprotachykinin (PPT)-I and NK-1R cDNAs (a gift from Dr. Leeman, Boston University) in the range of 5 million copies to two copies per reaction. All plasmid samples were treated with RNase A before quantitation to minimize contamination with bacterial RNAs from the plasmid purification procedure and subsequently quantified using a combination of absorbance at 260 nm and gel electrophoresis. GAPDH mRNA levels were analyzed as a positive control for cDNA synthesis and a known amount of rat GAPDH and primers were custom-manufactured by Maxim Biotech, Inc (South San Francisco, CA, USA).
Real-time quantitative mRNA was determined with a SYBR Green real-time PCR assay using an ICycler PCR machine (Bio-Rad, Richmond, CA, USA). The potential benefits of using SYBR Green I dye to continuously monitor PCR product formation have been demonstrated (Wittwer et al. 1997; Morrison et al. 1998). Sense and antisense primers are designed using source from the Virtual Genome Center (http://alces.med.umn.edu) and listed in Table 2. Each sample was analyzed in triplicate along with standards and no-template controls. The reaction contained 100 ng cDNA, 0.3 µM primers, and 1× SYBR Green PCR Master Mix (Qiagen) in a final volume of 25 µl. After denaturation at 95°C for 15 min, the cDNA products were amplified for 45 cycles, each cycle consisting of a three-step procedure: denaturation at 94°C for 15 s, annealing at 60°C for 30 s, and extension at 72°C for 45 s. Acquisition of fluorescent signal from the samples was carried out at the end of the elongation step. Because SYBR Green I binds to any double-stranded DNA, the specific product from non-specific products and primer dimers were confirmed immediately after amplification by melting analysis. The PCR products were heated to 95°C for 1 min, annealed at 65°C (annealing temperature + 10°C), and then slowly heated from 65°C to 95°C at 0.3°C increments to obtain the melting curve. The PCR products were subjected to analysis by electrophoresis on a 2% agarose gel to confirm the efficiency of the melting curve analysis. A similar setup was used for negative controls except that the reverse transcriptase was omitted and no PCR products were detected under these conditions.
All SYBR Green PCR data were obtained using the ICycler PCR software (Bio-Rad). Direct detection of PCR products was monitored by measuring the increase in fluorescence caused by the binding of SYBR Green I dye to double-stranded DNA. These measurements resulted in an amplification plot of the fluorescence signal versus cycle number. The parameter threshold cycle (Ct) was defined as the fractional cycle number at which the fluorescence passes the fixed threshold. A plot of the log of initial target copy number for a set of standards versus the calculated Ct-value resulted in a straight line. Quantitation of the amount of target in unknown samples was accomplished by measuring Ct and using the standard curve to determine starting copy number. Standard curves were generated for each primer set and each PCR run using serial dilutions of rat NK-1R and β-PPT-I cDNA. All the samples were tested in duplicate with the reference gene GAPDH, a housekeeping gene, for normalization of data. A ratio of specific mRNA/GAPDH amplification was then calculated, to correct for any differences in efficiency at room temperature.
Enzyme immunoassay of substance P
SP was measured in the lung tissue (n=6) using a commercial EIA kit as directed by the kit supplier (Cayman Chemical, Ann Arbor, MI, USA), which is based on the competition between free SP, derived from the unknown sample, and a SP tracer (SP linked to an acetylcholinesterase molecule) for a limited number of SP-specific rabbit antiserum binding sites. Briefly, 0.2 mg lung tissue was homogenized in 1 ml EIA buffer with 4% acetic acid, and was centrifuged at 3,000 g for 15 min. The supernatant was then purified through an activated C-18 reverse phase cartridge and evaporated by vacuum. Test samples and the standards were run in triplicate in 96-well microplates. The absorbance was determined at 412 nm using a Bio-Tek Elx808 automated microplate reader (Bio-Tek Instruments Inc., Winooski, VT, USA). The sensitivity of the assay was determined by serial dilution and was found to be ~17 pg SP/ml. The amount of SP in the lung tissue was expressed in picograms per milligram protein, calculated following the manufacturer's instructions. Protein concentration in the lung tissue extract was determined by a dye binding method involving colloidal gold and bovine serum albumin was used as the standard (Pierce Chemical Company, Rockford, IL, USA).
Enzyme activity of neutral endopeptidase
Lung tissues (n=6) were washed with saline and stored at −70°C for later analysis. To obtain a cell-free extract, lung tissue was homogenized in 10 ml of T-PER tissue protein extraction reagent (Pierce Chemical Co.). The residue was removed from the extract by centrifuge at 12,000 g for 10 min at 4°C. Cell-free NEP activity in each tissue lysate was measured spectrophotometrically by a coupled assay as reported by Papandreou et al. (1998) and Van der Velden et al. (1999) with minor modifications. Briefly, 5 µl cell-free extract were incubated with 1 mM succinyl-Ala-Ala-Phe-p-nitroanilide (Suc-Ala-Ala-Phe-pNA) (Bachem Bioscience Inc., King of Prussia, PA, USA) as a substrate in 0.1 M Tris-HCl (pH 7.6) in the presence of 1 µl (0.14 units/µl) porcine kidney aminopeptidase N (Sigma). The reaction (total volume 200 µl) was measured in duplicate in a 96-well microtiter plate. In this coupled activity assay, NEP cleaves Suc-Ala-Ala-Phe-pNA between Ala and Phe, yielding Phe-pNA. Aminopeptidase N subsequently cleaves Phe-pNA, generating pNA as the final product. The increase in specific absorbance at 405 nm (as a result of the accumulation of free p-nitroaniline) was determined after 30 min incubated at 37°C using a plate reader (Bio-Tek Instruments). Cell-free (substrate alone or substrate with aminopeptidase N) and substrate-free blanks were run in parallel. Protein concentration was determined using a Coomassie Plus Protein Assay (Pierce Chemical Co.) using bovine serum albumin as a standard.
Histopathological examination
One sagittal, 1-mm thick slice was collected from each of the diaphragmatic lung lobes and the right side upper lobes from all experimental rats and controls (n=4–6 rats per group). These slices were immersion-fixed in Bouin's fixative for 24 h and then placed on an automatic tissue processor followed by embedding together in pairs in paraffin (i.e., one pair per rat) using a short processing protocol and low melting point paraffin. Sections of 5 µm were dewaxed and processed histochemically with hematoxylin and eosin (H&E) for general pathology examination, and with Toluidine blue for selective evaluation of mast cells.
Immunohistochemical analyses
Sections of 5 µm from the same blocks used for histopathology were dewaxed, hydrated and treated as follows. Sections were first treated with normal, non-immune goat serum for 30 min (from the species of secondary antibody) to block any non-specific background. The sections were then treated lightly with Triton X-100 (0.2%, 5 min) to facilitate antibody access to the tissue antigen. Primary antiserum, raised in rabbit, was then applied overnight at 4°C (SP, 1:500; Peninsula, San Carlos, CA, USA) or for 4 h at room temperature (CGRP, 1:1000). After rinsing in phosphate-buffered saline, sections were treated with the Zymed Histostain kit (Zymed Laboratories, Inc., San Francisco, CA, USA). Briefly, this included secondary biotinylated goat anti-rabbit serum followed by horseradish peroxidase (HRP)-labeled streptavidin, and development in a diaminobenzidine substrate solution yielding a permanent reddish brown reaction product. Moreover, immunofluorescence was used for NK-1R to optimize detection of the minute immunoreactive sites. These sections were treated overnight with monoclonal (mouse) antibody (1:500, Chemicon) followed by Texas red-labeled goat anti-mouse antibody (1:50; Vector Labs, Inc., Burlingame, CA, USA), which yielded red fluorescence. All slides were coverslipped permanently with GVA-mount (SP and CGRP), or temporarily using polyvinyl alcohol mounting medium (NK1R; Fluka/Sigma-Aldrich, St. Louis, MO, USA). Slides were then observed with a Nikon Eclipse 600 microscope equipped with objectives for both brightfield (SP and CGRP) and fluorescence (NK1R). Images were captured using a Spot digital camera, imported to a Gateway computer, and printed on photograde paper.
Statistical analysis
Data distributions in (1) the groups of capsaicin versus vehicle-pretreatment, (2) the groups of air or DE exposure, and (3) the subgroups of capsaicin pretreatment and DE exposure were examined as frequency histograms and means ± SEM. Comparisons of means among groups were made using analysis of variance (ANOVA) in the log10 scale. Since the measures are independent variables, mean changes were evaluated when appropriate using post hoc linear contrasts, with adjustment for multiple comparisons being made using both Bonferroni and Fisher's PLSD correction of significance levels. Additional statistical analyses were performed to evaluate the strength of linear relationships among room air, the low and high DE exposures in NEP activity, plasma extravasation, and respiratory permeability. To determine whether these changes were induced dose-dependently by DE exposures, Pearson correlation coefficients were calculated following log10 transformation. All tests were two-tailed tests, and P<0.05 was considered to be significant. Data were collected and analyzed on a Macintosh computer with the Statview IV statistical program and were expressed as means ±SEM.
Results
Particle characterization of diesel exhaust exposure
Mass concentration
The mass concentration of DE particle at the low level of DE exposure (LDE) was 35.3±4.9 µg/m3 (mean ±SEM, n=14). For the high level of DE exposure (HDE), the mass concentration was controlled to 632.9±47.6 µg/m3 (mean ±SEM, n=11).
Size distributions
The measured particle size range was from 7.2 to 294.3 nm under the mode 6 in the CARB 8-mode test cycle. There was no difference in size distribution between LDE and HDE exposure due to the different dilution ratios. In Fig. 1, the particle number and volume concentrations are shown with respect to the particle diameter under these conditions for animal exposure.
Particle number (bell-shaped curves) and particle volume (linear curves) concentrations vs. size distributions for the low and high levels of diesel exhaust exposure (DEP). The engine was run at mode 6 of the California Air Resources Board (CARB) 8-mode test cycle: a 75% load condition at peak torque speed (1200 rpm)
Chemical composition
DE particles consist mainly of agglomerated solid carbonaceous material, volatile organics, sulfur compounds, and ash. Consequently, elemental carbon, organic carbon, and sulfates were analyzed in the samples collected over the entire test period for this operating condition (Table 3), and these indicated that there were significant differences between LDE and HDE exposure. Samples collected on a Teflon filter each day of LDE and HDE exposure were used for determination of 46 trace metal compounds, seven of which are shown in Table 3. Sodium (Na), magnesium (Mg), manganese (Mn), and lead (Pb) were not changed with the dilution ratio for LDE and HDE exposure. However, calcium (Ca), iron (Fe), and chromium (Cr) concentrations decreased approximately 50% with HDE exposure relative to LDE exposure.
Biomedical endpoints of tachykinin SP signaling in the lungs
Plasma extravasation
Pulmonary plasma extravasation was quantitated by the 99mTc-albumin technique. In vehicle-pretreated groups of rats, exposure to DE dose-dependently increased plasma extravasation in the extra- (Fig. 2) and intra-pulmonary airway (Fig. 3) compared with that of the air control. Using the same exposure protocol in the capsaicin-pretreated groups, plasma extravasation changes followed the same trend as those of the groups of the vehicle-treated rats. After data were adjusted by one factor of capsaicin treatment, significantly higher plasma extravasation was observed in rats treated with capsaicin than in those without capsaicin treatment. Interestingly, plasma extravasation increased significantly in the capsaicin-pretreated group exposed to room air at the Engine Research Center (EC).
Plasma extravasation of the bronchi in Fischer 344/NH rats exposed to diesel exhaust with and without capsaicin pretreatment. AC Filtered room air exposure groups, LDE low level of diesel exhaust exposure, HDE high level of diesel exhaust exposure, EC exposure to room air at Engine Research Center. Data are expressed as means ±SEM. a P<0.05 compared with values of the vehicle-treated rats exposed to filtered room air; b P<0.05 compared with values of the capsaicin-treated rats exposed to filtered room air; c P<0.05 compared with values of the vehicle-pretreated rats in matched exposure group
Plasma extravasation of the lung parenchyma in Fischer 344/NH rats exposed to diesel exhaust with and without capsaicin pretreatment. AC Filtered room air exposure groups, LDE low level of diesel exhaust exposure, HDE high level of diesel exhaust exposure, EC exposure to room air at Engine Research Center. Data are expressed as means ±SEM. a P<0.05 compared with values of the vehicle-treated rats exposed to filtered room air; b P<0.05 compared with values of the capsaicin-treated rats exposed to filtered room air; c P<0.05 compared with values of the vehicle-pretreated rats in matched exposure group
Histopathological studies
Large numbers of activated alveolar macrophages were observed throughout the lungs of rats exposed to HDE compared with other groups (Fig. 4A–C). The rats exposed to LED had only occasional alveolar macrophages (Fig. 4B) as did air controls. These macrophages were easily identified by phagocytosed small, black DE particles within the cytoplasm of HDE rats (Fig. 4C), but not in air controls (Fig. 4A). Surprisingly, capsaicin pretreatment reduced the number of particle-laden alveolar macrophages to less than half the number observed in HDE rats (45.1±7.7 cells per 40× microscope field versus 18.9±1.2, P=0.011). There was no notable influx of polymorphonuclear leucocytes or eosinophils. Inflammatory cell margination was observed along the venular endothelium in the lungs of HDE rats, and diapedesis was evident by perivascular cuffing (Fig. 4D,E), with subsequent mononuclear cell migration and dispersal throughout the entire lung parenchyma and alveoli (Fig. 4F). This was not observed in other groups. These cells, which stained basophilic with Toluidine blue (Fig. 4E), were frequently in direct physical contact with individual nerve fibers. Moreover, these cells are most likely monocytes about to become activated macrophages. In addition, HDE rats had an increased number of mast cells that were oriented toward thin-walled vessels and airway smooth muscle (data not shown).
Representative micrographs of lungs of rats exposed to diesel exhaust. A Lung parenchyma from air control shows virtual absence of alveolar macrophages. B Very few alveolar macrophages (arrows) are seen after low level of diesel exhaust (LDE) exposure, whereas C shows a large number of macrophages (arrows) after high level of diesel exhaust (HDE) exposure. Note the accumulation of black particles in macrophages of lung after HDE exposure. D shows margination of inflammatory cells (arrowheads) along the lumenal surface of the vascular endothelium in H&E stained lung section of HDE rat. Note perivascular orientation (cuffing) of inflammatory cells. Activated alveolar macrophages are indicated with arrows. E A similar image is shown with Toluidine blue staining which renders inflammatory cells blue. F Lung parenchyma of rat after HDE exposure showing activated macrophages in alveolar spaces (arrows, H&E)
Substance P
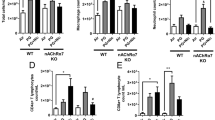
Exposure of the capsaicin- and vehicle-pretreated rats to DE did not induce any change in the expression of β-PPT-I mRNA encoding SP compared to their corresponding air controls (Fig. 5). Additionally, there was no statistically significant difference in β-PPT-I mRNA levels between the capsaicin- and vehicle-pretreated rats. In vehicle-treated groups, lung tissue levels of SP protein decreased significantly when exposed to HDE, but not to LDE, when compared with that of air control (Table 4). In capsaicin-treated groups, SP protein was just at or below the level of detection, confirming the efficiency of capsaicin treatment (Table 4). Immunohistochemistry also indicated a reduced density of SP in the capsaicin-pretreated HDE rats (Fig. 6B) compared with its corresponding vehicle-treated rats (Fig. 6A).
Expression of β-preprotachykinin-I (β-PPT-I) mRNA encoding substance P (SP) of the lung tissues in Fischer 344/NH rats exposed to diesel exhaust with and without capsaicin pretreatment. AC Filtered room air exposure groups, LDE low level of diesel exhaust exposure, HDE high level of diesel exhaust exposure, EC exposure to room air at Engine Research Center. Data are expressed as means ± SEM
Neurokinin-1 receptor
The NK-1R gene expression showed complicated response patterns following LDE and HDE exposure (Fig. 7). In vehicle-pretreated groups, NK-1R mRNA expression was significantly downregulated in the LDE group, whereas expression remained unchanged in the HDE-exposed rats relative to that in air controls. Conversely, NK-1R mRNA expression in the capsaicin-pretreated LDE group did not differ from the capsaicin-pretreated group exposed to filtered room air (AC), whereas there was a significant upregulation in the capsaicin-pretreated HDE group. Interestingly, capsaicin pretreatment induced a significant decrease in AC groups; conversely, there was a significant increase in the HDE or EC groups
Expression of neurokinin-1 receptor (NK-1R) mRNA in the lung tissue in Fischer 344/NH rats exposed to diesel exhaust with and without capsaicin pretreatment. AC Filtered room air exposure groups, LDE low level of diesel exhaust, HDE high level of diesel exhaust exposure, EC exposure to room air at Engine Research Center. Data are expressed as means ±SEM. aSignificantly different from vehicle-treated rats exposed to filtered room air; bSignificantly different from capsaicin-treated rats exposed to filtered room air; cSignificantly different from vehicle-pretreated rats in matched exposure group
NK-1R-like immunoreactivity appeared as discrete dots on the airway epithelium, resembling the pattern of synaptic varicosities (Fig. 8). Interestingly, there was a qualitative difference in the capsaicin-HDE rats in that immunoreacting "receptor sites" were larger and of higher intensity than in the other groups. The specific pattern of immunoreactivity allowed us to quantitate the number of such sites per unit basement membrane length. All four capsaicin- and vehicle-pretreated groups had approximately twice as many immunoreactive sites as the room air-exposed rats. There was not any difference of NK-1R pattern or density between AC and EC groups.
Immmunohistochemical location of neurokinin-1 receptor (NK-1R) in the lung tissue in Fischer 344/NH rats exposed to diesel exhaust with and without capsaicin pretreatment. NK-1R-like immunoreactivity appeared as discrete dots (arrows) on the airway epithelium and these sites resembled synaptic varicosities. There was a qualitative difference in the capsaicin- and vehicle-pretreated rats exposed to diesel exhaust (C–F) in that immunoreacting "receptor sites" were larger and of higher intensity than in the room air groups (A,B)
Neutral endopeptidase
NEP activity of the lungs in the vehicle-treated groups decreased significantly after exposure to LDE and HDE compared with that of the air control group (Fig. 9). In capsaicin-pretreated groups, the changes in NEP activity of DE-exposed rats followed the same trend as those of the vehicle control groups. No difference in NEP activity was observed between each pair of capsaicin- and vehicle-pretreated groups.
Neutral endopeptidase (NEP) activity of the lung tissue of Fischer 344/NH rats exposed to diesel exhaust with and without capsaicin pretreatment. AC Filtered room air exposure groups, LDE low level of diesel exhaust, HDE high level of diesel exhaust exposure, EC exposure to room air at Engine Research Center. aSignificantly different from vehicle-treated rats exposed to filtered room air; bSignificantly different from capsaicin-treated rats exposed to filtered room air
Discussion
This study reports the molecular neurotoxicity of DE on tachykinin SP signaling in lungs of F344/NH rats exposed nose-only, in an "on-line, real-time" inhalation system, to freshly generated diesel engine emissions at low and high ambient pollution levels. The findings indicate that exposure to DE can initiate "unconditional" neurogenic inflammatory responses that are involved in overlapping tachykinergic mechanisms, including stored-SP depletion, NK-1R gene/protein overexpression, and reduced NEP activity. Considering that NK-1R is a pathway in signaling transduction within a complex inflammatory network, and that NEP is a critical membrane degradation enzyme for tachykinins due to its co-location with NK-1R-expressed cells, this study may partially explain the role of the tachykinin SP signaling pathway in DE-induced lung inflammation and injury.
"Neurogenic inflammation" in extra- and intra-pulmonary airways both in capsaicin- and vehicle-pretreated rats was concentration-dependently induced by exposure to DE, as determined by typical plasma protein extravasation and edema. The neurogenic plasma leakage, as a phenomenon known as neurogenic inflammation, has been well characterized in rat airways. Plasma extravasation correlated highly with DE exposure levels, and was noted especially in the lung parenchyma where respiratory airways and alveoli exist. We also found an increased number of macrophages and mast cells in the lungs of HDE-exposed rats. This could contribute to the proinflammatory effects of DE, and supports continued attention to macrophages and mast cells in DE-induced inflammation. Such changes as those described in this model may develop a pathophysiological microenvironment in the respiratory system that could lead to more absorption and metabolism of DE contents due to highly sustained respiratory permeability. As a potential consequence of this change, DE-exposed subjects could be rendered more susceptible to respirable environmental pollutants when they also have respiratory infection caused by viruses or bacteria. Such synergy may substantially compromise the afferent nerve defensive system that switches neurogenic pulmonary responses from their physiological and protective functions to a detrimental role that perpetuates and intensifies lung injury.
This study shows that mRNA and protein levels of SP and NK-1R in the lungs may be affected by DE exposure. In vehicle-pretreated rats, exposure to DE decreased lung tissue SP levels dose-dependently, without affecting expression of β-PPT-I mRNA encoding SP. It appears that repeated exposure to DE triggered SP release from stored tachykinin resources, such as afferent C-fiber nerve endings. This action would elicit potent bronchopulmonary effects, including contractile bronchoconstriction, hyperresponsiveness, and mucus secretion. Meanwhile, SP could be subjected to degradation or inactivation by NEP provided its activity remained at a physiologically relevant levels as suggested by approximately 80% activity. Therefore, at 3 weeks of exposure, SP content substantially decreased to a low level (89% in vehicle-treated HDE rats), which may result in loss or dysfunction of the afferent defensive mechanisms. Additionally, NK-1R mRNA transcription in the lungs was downregulated when exposed to LDE, whereas no change occurred on HDE exposure. It is likely that NK-1R gene expression is regulated with paracrine and/or autocrine signaling mechanisms, and the upregulation could be a compensatory measure triggered by reduced SP. However, immunohistochemical analysis indicated there was a qualitative difference in the DE-exposed rats in that immunoreacting "receptor sites" were larger and of higher intensity than in the other groups. It is well known that the NK-1R is an important pathway in signaling transduction within a complex network involving chemokines, cytokines, hormones, oxidative stress, and other inflammatory mediators. The changes of NK-1R gene and protein expression could be a key pathogenesis point in lung inflammatory responses following DE exposure (Bozic et al. 1996). However, we cannot determine from this study whether these changes are attributed to direct molecular toxicity of DE or an adaptive response to increase the efficacy of the respiratory system to SP signaling.
One of the most important findings of this study was that exposure of the rats to DE depressed NEP activity in the lungs. The main reason for this observation may be DE-induced membrane disruption, necrosis, and sloughing of epithelial cells in the airways. NEP is a membrane-bound enzyme, which is located mainly at the surface of airway epithelial cells, but is also present in airway smooth muscle cells, submucosal gland cells, and fibroblasts. It has been demonstrated that removal of the airway epithelium substantially increases the airway responses to SP (Lilly et al. 1993). In our previous studies, the airway epithelial lining showed conspicuous lesions, which were consistent in their severity, in the airways subjected to oil fly ash (Wang et al. 1999). Sloughing of epithelial cells was also apparent in the bronchioles of the DE-exposed animals. We speculate that the causes of depressed NEP activity may also include (1) inactivation of NEP by oxidants, (2) loss of NEP from cell surfaces through endocytosis and/or proteolytic clipping, and (3) decreased NEP transcription through protein kinase C activation. In addition, DE may directly and/or indirectly modulate the gene and protein expression of NEP in the lungs. It is not surprising that DE-induced loss of NEP activity led to an increase in plasma extravasation evoked by endogenous SP. Therefore, NEP is of critical importance in modulating the activity of endogenously released SP, and hence of neurogenic inflammation.
In order to confirm C-fiber involvement of neurogenic mechanisms underlying DE-induced inflammation, we utilized a model of capsaicin-pretreatment. In this protocol, capsaicin stimulated C-fibers, rather than obliterated them. It is documented that capsaicin induces the release of SP and other neurotransmitters from sensory endings, causing plasma leakage via the activation of tachykinin NK-1R on endothelial cells. In parallel measurements in vehicle-treated rats, capsaicin-pretreated rats followed the same trend and exacerbated responses as those measured in normal animals exposed to the identical level of DE. Moreover, those rats with capsaicin pretreatment had more predisposed neurogenic responses than those of the corresponding vehicle control exposed to the same level of DE. For example, exposure of the capsaicin-pretreated rats, but not the vehicle control, to LDE significantly increased plasma extravasation in extra-pulmonary airways. Similar to this pattern, the capsaicin-pretreated rats, but not the vehicle control, significantly increased NK-1R m RNA and protein expression in lung tissue when they were exposed to HDE. However, the effects of capsaicin treatment were not consistent and apparent in this study. It appears that DE exposure-induced inflammation could not be substantially attributed to SP from bronchopulmonary C-fiber endings at this time point. We speculate that the reasons for these findings may be as follows. (1) A significantly lower SP level was detected in lung tissue from HDE-exposed rats than in the controls at the end of 3-week exposure, which may reflect augmented release of SP, followed by degradation in the acute phase of exposure, whereas NEP activity retained its function at the same time. It is possible that the neurogenic inflammation included the role of other inflammatory mediators, such as cytokines. (2) The animals may have recovered their C-fiber function during the 3-week study, which is a possibility we cannot rule out completely. Although utilized frequently in our previous studies, this capsaicin protocol is to stimulate C-fibers, rather than to obliterate them permanently. Consequently, it is not surprising that rats with capsaicin pretreatment following DE exposure showed the same and greater responses of neurogenic inflammation, respectively, as those of intact animals. The immunohistochemistry study of SP supports this speculation. The density of SP-immunoreactive C-fibers was difficult to assess accurately due to inconsistencies in the intensity of the immunoreactivity compounds. In spite of an impressively reduced density in several capsaicin-treated rats compared with vehicle-treated rats when exposed to HDE, however, there was no consistent reduction due to individual variability following the 3-week DE exposure. Therefore, a time-course study with a state-of-the-art method, such as transgenic or knockout/down animal models, may be utilized to clarify this point in a future study.
Interestingly, we observed that the rats exposed to the room air had some greater responses in several measurements than animals kept in filtered air, as follows. First, plasma extravasation in intra-pulmonary airway and mRNA for IL-1β had significant increases in the capsaicin- but not the vehicle-pretreated rats. This suggests that capsaicin treatment made these rats more vulnerable to breathing normal air due to their loss of sensory protective responses. Second, although these exposure experiments were conducted in a well-closed laboratory, we could not rule out possibility that some pollutants exist. The NK-1R mRNA increase in the vehicle control may support this speculation. However, we did monitor any air quantities, including particulates, excepting air pressure and temperature in the diesel engine laboratory.
To identify what chemical/physical characteristics of DE are associated with the molecular and cellular neurotoxicity, efforts were made to determine the physical aspects and the chemical composition of particles that induce the deleterious effects in this animal species. We speculated that DE-induced neurogenic inflammation may be attributed to the particle number, volume, and mass concentration, including elemental/organic carbons and sulfates. In this exposure study to ambient levels of DE, there were no differences between LDE and HDE exposure in the sizes, several trace metals, and representative organic compounds of the particles. However, it is difficult to compare with previous studies of airborne particulates because of the variation of the particles' composition, different particle measurement methodology, and health endpoints.
In summary, Inhalation of DE could involve in lung inflammation through overlapping tachykinergic mechanisms. Based on these observations, either overexpression of NK-1R, or the reduction of SP, or NEP inactivity may be regarded as a key factor(s) that switches neurogenic pulmonary responses from their physiological and protective functions to a detrimental role that increases and perpetuates lung injury. These changes in afferent tachykinin SP signaling may present early patho-physiological responses during exposure to environmental DE. However, substantial future studies are needed to clarify the role(s) and mechanism of neurogenic inflammation in pathogenesis of DE exposure. First, data generated from this study demonstrated an SP-signaling profile of a cross-section examination at one time-point, but lacks a time-course study to clearly understand involvement of neurogenic inflammation parameters. Therefore, either time-course or intervention studies, such as antagonists and gene knockout/down models of NK-1R or inhibitors and antibody directed against NEP, are needed to confirm these data and examine the mechanism of neurogenic inflammation. Second, the study should be extended to additional neuropeptides in neurons and non-neuron lung cells, such as CGRP, neurokinin A, and neurokinin B, which may be involved in DE-induced pathogenesis. Therefore, only after extensive systematic studies to clarify the role(s) and mechanism of neurogenic inflammation in DE-induced known toxicity, could we develop appropriate therapeutic and preventive strategies that may help to mitigate a serious, widespread, and costly health problems associated with DE or other air pollution exposure.
References
American Thoracic Society, Committee of the Environmental and Occupational Health Assembly (1996) Health effects of outdoor air pollution. Am J Respir Crit Care Med 153:3–50
Bonham AC, Kott KS, Joad JP (1996) Sidestream smoke exposure enhances rapidly adapting receptor responses to substance P in young guinea pigs. J Appl Physiol 81:1715–1722
Bozic CR, Lu B, Hopken UE, Gerard C, Gerard NP (1996) Neurogenic amplification of immune complex inflammation. Science 273:1722–1725
California EPA (Environmental Protection Agency) (1998) Part B: health risk assessment for diesel exhaust, proposed identification of diesel exhaust as a toxic air contaminant. Office of Environmental Health Hazard Assessment, Air Resources Board, Sacramento
Dawson SV, Alexeeff GV (2001) Multi-stage model estimates of lung cancer risk from exposure to diesel exhaust, based on a U.S. railroad worker cohort. Risk Anal 21:1–18
Delaunois A, Segura P, Dessy-Doize C, Ansay M, Montano LM, Vargas MH, Gustin P (1997) Ozone-induced stimulation of pulmonary sympathetic fibers: a protective mechanism against edema. Toxicol Appl Pharmacol 147:71–82
Delfino RJ (2002) Epidemiologic evidence for asthma and exposure to air toxics: linkages between occupational, indoor, and community air pollution research. Environ Health Perspect 110 [Suppl 4]:573–589
EPA (US Environmental Protection Agency) (2002) Health assessment document for diesel engine exhaust. Document EPA/600/8-90/057F. US EPA, Office of Research and Development, National Center for Environmental Assessment, Washington DC
Hashimoto K, Ishii Y, Uchida Y, Kimura T, Masuyama K, Morishima Y, Hirano K, Nomura A, Sakamoto T, Takano H, Sagai M, Sekizawa K (2001) Exposure to diesel exhaust exacerbates allergen-induced airway responses in guinea pigs. Am J Respir Crit Care Med 164:1957–1963
HEI (Health Effects Institute) (1995) Diesel exhaust: a critical analysis of emissions, exposure, and health effects. A special report of the Institute's Diesel Working Group. Health Effects Institute, Cambridge MA
HEI (Health Effects Institute) (1999) Diesel emissions and lung cancer: epidemiology and quantitative risk assessment. A special report of the Institute's Diesel Working Group. Health Effects Institute, Cambridge MA
Iwai K, Adachi S, Takahashi M, Moller L, Udagawa T, Mizuno S, Sugawara I (2000) Early oxidative DNA damages and late development of lung cancer in diesel exhaust-exposed rats. Environ Res 84:255–264
Jimba M, Skornik WA, Killingsworth CR, Long NC, Brain JD, Shore SA (1995) Role of C fibers in physiological responses to ozone in rats. J Appl Physiol 78:1757–1763
Joad JP, Kott KS, Bonham AC (1997) Nitric oxide contributes to substance P-induced increases in lung rapidly adapting receptor activity in guinea pigs. J Physiol (Lond) 503:635–643
Killingsworth CR, Paulauskis JD, Shore SA (1996) Substance P content and preprotachykinin gene-I mRNA expression in a rat model of chronic bronchitis. Am J Respir Cell Mol Biol 14:334–340
Killingsworth CR, Shore SA, Alessandrini F, Dey RD, Paulauskis JD (1997) Rat alveolar macrophages express preprotachykinin gene-I mRNA-encoding tachykinins. Am J Physiol 273:L1073–L1081
Krause JE, Bu JY, Takeda Y, Blount P, Raddatz R, Sachais BS, Chou KB, Takeda J, McCarson K, DiMaggio D (1993) Structure expression and second messenger-mediated regulation of the human and rat substance P receptors and their genes. Regul Pept 46:59–66
Kweon CB, Foster DE, Schauer JJ, Okada S (2002) Detailed chemical composition and particle size assessment of diesel engine exhaust. Society of Automotive Engineers (SAE) 2002 Powertrain and Fluid Systems Conference, 21–24 October 2002, San Diego. SAE Technical Papers, Document No. 2002-01-2670. Available via http://www.sae.org
Kweon C, Okada S, Bae M, Mieritz M, Schauer JJ, Foster DE (2003) Effect of engine operating conditions on organic compounds in engine exhaust of a heavy-duty (HD) direct-injection (DI) diesel engine. Society of Automotive Engineers (SAE) 2003 World Congress. MArch2003, Detroit. SAE Technical Papers, Document No. 2003-01-0342. Available via http://www.sae.org
Lambrecht BN (1987) Substance P receptor-dependent responses of leukocytes in pulmonary inflammation. Am Rev Respir Dis 136:S39–S43
Lambrecht BN (2001) Immunologists getting nervous: neuropeptides, dendritic cells and T cell activation. Respir Res 2:133–138
Lilly CM, Drazen JM, Shore SA (1993) Peptidase modulation of airway effects of neuropeptides. Proc Soc Exp Biol Med 203:388–404
Long NC, Abraham J, Kobzik L, Weller EA, Krishna Murthy GG, Shore SA (1999) Respiratory tract inflammation during the induction of chronic bronchitis in rats: role of C-fibres. Eur Respir J 14:46–56
Lough GC, Shafer MM, Schauer JJ (2000) ICP-MS analysis of ultra-trace metals present in fine particulate matter. In: Proceedings of 93rd A&WMA (Air and Waste Management Association) National Meeting, Salt Lake City. Available via http://www.awma.org
Lucchini RE, Springall DR, Chitano P, Fabbri LM, Polak JM, Mapp CE (1996) In vivo exposure to nitrogen dioxide (NO2) induces a decrease in calcitonin gene-related peptide (CGRP) and tachykinin immunoreactivity in guinea pig peripheral airways. Eur Respir J 9:1847–1851
Mauderly JL (1999) Diesel exhaust. In: Lippmann M (ed) Environmental toxicants: human exposures and their health effects, 2nd edn. Wiley, New York, pp 193–241
Mauderly JL, Bice DE, Cheng YS, Gillett NA, Henderson RF, Pickrell JA, Wolff RK (1989) Influence of experimental pulmonary emphysema on the toxicological effects from inhaled nitrogen dioxide and diesel exhaust. Res Rep Health Eff Inst 30:1–47
Morrison TB, Weis JJ, Wittwer CT (1998) Quantification of low-copy transcripts by continuous SYBR Green I monitoring during amplification. Biotechniques 6:954–962
Mueller PK, Mendoza BV, Collins JC, Wilgus EA (1978) Application of Ion Chromatography to the Analysis of Anions Extracted from Airborne Particulate Matter. In: Sawicki E, Mulik JD, Wittgenstein E (eds) Ion chromatographic analysis of environmental pollutants. Ann Arbor Science, Ann Arbor MI, pp 77–86
Nikula KJ, Avila KJ, Griffith WC, Mauderly JL (1997) Lung tissue responses and sites of particle retention differ between rats and cynomolgus monkeys exposed chronically to diesel exhaust and coal dust. Fundam Appl Toxicol 37:37–53
Okamoto Y, Shirotori K, Kudo K, Ishikawa K, Ito E, Togawa K, Saito I (1993) Cytokine expression after the topical administration of substance P to human nasal mucosa: the role of substance P in nasal allergy. J Immunol 151:4391–4398
Pandya RJ, Solomon G, Kinner A, Balmes JR (2002) Diesel exhaust and asthma: hypotheses and molecular mechanisms of action. Environ Health Perspect 110 [Suppl 1]:103–112
Papandreou CN, Usmani B, Geng Y, Bogenrieder T, Freeman R, Wilk S, Finstad CL, Reuter VE, Powell CT, Scheinberg D, Magill C, Scher HI, Albino AP, Nanus DM (1998) Neutral endopeptidase 24.11 loss in metastatic human prostate cancer contributes to androgen-independent progression. Nat Med 4:50–57
Salvi S, Blomberg A, Rudell B, Kelly F, Sandström T, Holgate ST, Frew A (1999) Acute inflammatory responses in the airways and peripheral blood after short-term exposure to diesel exhaust in healthy human volunteers. Am J Respir Crit Care Med 159:702–709
Salvi S, Nordenhall C, Blomberg A, Rudell B, Pourazar J, Kelly FJ, Wilson S, Sandström T, Holgate ST, Frew AJ (2000) Acute exposure to diesel exhaust increases IL-8 and GRO-a production in healthy human airways. Am J Respir Crit Care Med 161:550–557
Schauer JJ, Kleeman MJ, Cass GR, Simoneit BT (1999a) Measurement of emissions from air pollution sources. 1. C1 through C29 organic compounds from meat charbroiling. Environ Sci Technol 33:1566–1577
Schauer JJ, Kleeman MJ, Cass GR, Simoneit BT (1999b) Measurement of emissions from air pollution sources. 2. C1 through C30 organic compounds from medium duty diesel trucks. Environ Sci Technol 33:1578–1587
Sydbom A, Blomberg A, Parnia S, Stenfors N, Sandstrom T, Dahlen SE (2001) Health effects of diesel exhaust emissions. Eur Respir J 17:733–746
Szarek JL, Spurlock B (1997) Sensory nerve-mediated inhibited response in airways of F344 rats. Toxicology 122:101–110
Tjen-A-Looi S, Kraiczi H, Ekman R, Keith IM (1998) Sensory CGRP depletion by capsaicin exacerbates hypoxia-induced pulmonary hypertension in rats. Regul Pept 74:1–10
Van der Velden VHJ, Naber BAE, van Hal PTHW, Overbeek SE, Hoogsteden HC, Versnel MA (1999) Peptidase activity in serum and bronchoalveolar lavage fluid from allergic asthmatics-comparison with healthy non-smokers and smokers and effects of inhaled glucocorticoids. Clin Exp Allergy 29:813–823
Veronesi B, Oortgiesen M (2001) Neurogenic inflammation and particulate matter (PM) air pollutants. Neurotoxicology 22:795-810
Wang S, Lantz RC, Robledo RF, Breceda V, Chen GJ, Hays AM, Witten ML (1999) Early alterations of lung injury following acute smoke exposure and 21-aminosteroid treatment. Toxicol Pathol 27:334–341
WHO (World Health Organisation) (1996) Diesel fuel and exhaust emissions. Environmental Health Criteria 171. WHO, Geneva
Wittwer CT, Ririe KM, Andrew RV, David DA, Gundry RA, Balis UJ (1997) The LightCycler: a microvolume multisample fluorimeter with rapid temperature control. Biotechniques 22:176–181
Author information
Authors and Affiliations
Corresponding author
Additional information
Research described in this article was conducted under contract to Health Effects Institute (HEI), an organization jointly funded by the United States Environmental Protection Agency (EPA) (Assistance Agreement R82811201) and automotive manufacturers. The contents of this article do not necessarily reflect the views of HEI, nor do they necessarily reflect the views and policies of EPA, or motor vehicle and engine manufacturers.
Rights and permissions
About this article
Cite this article
Wong, S.S., Sun, N.N., Keith, I. et al. Tachykinin substance P signaling involved in diesel exhaust-induced bronchopulmonary neurogenic inflammation in rats. Arch Toxicol 77, 638–650 (2003). https://doi.org/10.1007/s00204-003-0485-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-003-0485-4