Abstract
Summary
Participants with physical limitation and high degree of pain had poor mental and physical health-related quality of life. In addition, the more support and exercise that the participants had, the more likely theywere to report better health-related quality of life.
Introduction
Osteoporosis is a public health threat worldwide. The aim of this study is to examine the effects of individual demographics, disease characteristics, and social support on health-related quality of life (HrQoL) of adults with osteoporosis. Most psychosocial studies focused on the relationships but not the specific construct of social support on HrQoL.
Methods
In a correlational design, face-to-face, structured interviews were employed to collect information. Study questionnaires included a demographic sheet, the modified Social Support Inventory, and the Short-Form 36 scales on a convenience sample of 161 individuals recruited from four outpatient centers. Using the structural equation modeling approach, all relationships among factors, mediators, and HrQoL were analyzed.
Results
The mean duration of osteoporosis was longer than 5 years. Participants who exercised more than three times per week had greater HrQoL than individuals who exercised less frequently. Participants with physical limitation and high degree of pain had poor mental and physical HrQoL. The more support that the participants perceived, the more likely they were to report better HrQoL. The best fitted structural equation modeling (SEM) model included individual demographics and physical function, and social support as significant predictors on HrQoL, with informational support and physical function acting as mediators in those relationships. Moreover, this structural model explained 35, 42, and 40 % of the variance on activity of daily living (ADL), physical, and mental health-related quality of life.
Conclusions
The more informational support that individuals have, the more likely they were to report better HrQoL. Individuals with osteoporosis who have lower pain and more exercise are considered having better HrQoL. Further longitudinal research will help clarify the direction of these relationships.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoporosis is a serious worldwide health problem in most developed countries and will also impact many developing nations in the next few decades [1, 2]. It is estimated 5.3 million American older adults suffered from osteoporosis [3]. It is a systemic skeletal disease characterized by low bone mineral density and deterioration of bone structure with a consequent increase in bone fragility. Spinal or femur fracture is a common complication of osteoporosis and results in back pain and functional impairments of individuals, especially in older adults [4, 5]. Daily activities such as physical activities or work performance are affected, and negative consequences, such as falls, poor health-related quality of life (HrQoL), depression, or even financial drain to society are evident in individuals with osteoporosis [1, 4, 6].
The prevalence of osteoporosis is varied by gender and age [2, 3]. In China, the average prevalence was 15.1 % in men (ranged 0.5–35.3 %) and 29.9 % in women (ranged 2.5–57.3 %). The estrogen levels of women decrease after menopause; this has a direct effect on bone mineral density and may induce the condition of osteoporosis [7]. The prevalence of osteoporosis went up in those aged 50 years and above, and the average for men was 22.4 and 40.1 % for women [2]. In the USA, the prevalence of femur neck osteoporosis is 10 % in women aged 50 or more compared with the 2 % in men [3].
The 1-year incidence of any fracture in women with osteoporosis was 3.1 % in a 10-country, cohort study [8]. Among these fractures, 57 % were minor non-hip, non-vertebral; 26 % major non-hip, non-vertebral; 10 % spine; and 7 % hip, and the incident rate of fractures increased with age. Fractures cause pain, height loss, deformity, disability, and mortality, but spine and hip fractures have the most devastating prognosis and which consequently results into the loss of physical function, social interaction, and the need for a long-term care as well. In osteoporosis adults, psychosocial factors such as negative life events, lack of social support, and emotional problems may deteriorate their quality of life [9], and those may consequently result patients in depression, isolation, cognitive-behavioral problems, impairments of activity of daily living (ADL), and even suicide [10, 11].
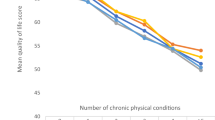
Studies have examined the impact of osteoporosis upon HrQoL. HrQoL in women with osteoporosis is lower than that in population norms or those without this condition [4, 12]. Furthermore, women with osteoporosis with fracture histories have worse HrQoL than those without such histories [6]. Study results showed that women with osteoporosis with fractures had lower HrQoL than those without fractures [4, 12]. Of different types of fractures, spine fractures had the strongest effect in decreasing HrQoL in women with osteoporosis [8]. Other chronic disease (i.e., cardiovascular diseases, diabetes, hypertension, cataract disease, etc.) and physical conditions (i.e., body mass index or comorbidities) are also associated with HrQoL in people with osteoporosis [4, 13]. Individual characteristics such as age, economic status, or living conditions are associated with HrQoL in those with osteoporosis [13].
Information on HrQoL in osteoporosis patients may give health-care professionals better insight into the perceptions of individuals’ health status. Individuals with osteoporosis are usually older than those with other musculoskeletal diseases [14], and those with osteoporosis and fractures were even older than those only with osteoporosis [5]. Osteoporosis patients who had fractures had worse HrQoL in terms of pain, physical function, social function, general health perception, and mental function than those who did not have a fracture [8, 15]. Having pain in osteoporosis patients would limit their social participations and HrQoL [16].
Having a social support from a friend who shared similar experience of osteoporosis is beneficial in psychosocial well-being [17]. Social support from families is important for improving knowledge in healthy lifestyle behaviors for the prevention of osteoporosis [18]. In the circumstance, social support also shows a better response in high level of quality of life of individuals with other chronic disease [19, 20]. The relationship between social support and HrQoL in Taiwanese patients with osteoporosis has not been explored. Therefore, direct/indirect support and the related quality of life in patients with osteoporosis were examined.
Conceptual framework
Reducing the chronic pain of osteoporosis is important since chronic pain is associated with depression, anxiety, frustration, and social withdrawal. These psychosocial consequences of osteoporosis may ultimately affect HrQoL. Osteoporosis is so extensive, and it causes mental and physical health problems [11]; social support may play a role to enhance an individual’s ability to cope with activities of daily life. The concept of social support is multidimensional; the definition of social support implies supportive ways, mediations or moderations, and behaviors that people apply to support a person in need [19]; different dimensions may have their own influences on positive health outcomes for adults with osteoporosis.
There are various concepts of social support from previous studies. Krause differentiated four types of social support including emotional support, informational support, tangible help, and integration support [21]. Emotional support focuses on the individual qualities or behaviors of a supporting person, including empathy, caring, and love. Informational support involves the provision of suggestions and information that a person may use to solve their problems. Tangible help comprises helping with transportation and/or providing financial support and integration support as providing support to others. Similarly, Barrera et al. [22] defined appraisal support as a part of social support, which affirms one’s actions or statements.
Social support has a direct substantial effect on health, when individuals with adequate social support may reduce psychological distress [23]. In our study, social support was hypothesized to have mediating effects on mental quality of life (MQoL) and physical quality of life (PQoL), including four dimensions: emotional support, appraisal support, tangible support, and informational support.
This study was designed to test a conceptual model of how pain, physical functioning, and social support contribute to HrQoL among women with osteoporosis. The specific aims were as follows: (1) to examine the relationships among osteoporosis patients with demographic and disease characteristics, disease factors, health-related quality of life, and social support dimensions (emotional, appraisal, informational, and tangible); (2) to investigate the predictors on PQoL and MQoL of osteoporosis patients and to explore which dimensions of social support are helpful to enhance QoL under specific manipulation over independent variables; (3) to estimate to what extent pain affects ADL, PQoL, and MQoL of osteoporosis patients; and (4) to verify which dimensions of social support are mediators to enhance PQoL and MQoL of patients with osteoporosis.
Methods
Participants
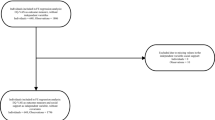
Participants, who met the inclusion criteria, were invited to participate in the study. One hundred and eighty patients were contacted, and 161 of them chose to enter the study with a response rate of 89.4 %. To be eligible for the study, participants had to meet the following criteria: (1) 18 years or above, (2) diagnosed with osteoporosis by a physician, (3) bone mineral density with T < −2.5, (4) no comorbid medical conditions influencing osteoporosis status, and (5) participants must be able to communicate in Chinese or Taiwanese. After receiving written informed consent from participants of four teaching hospitals, an investigator conducted individual face-to-face, structured interviews to collect data.
The sample size of 110 as suggested by Cohen [24] was for the analysis of correlation or regression in order to achieve a power of .80 with a medium effect size of .15 and an alpha level of .05. In addition, Pearson’s correlation and structural equation modeling (SEM) techniques were implemented to analyze the acquired dataset. Considering the possibility of participants dropping out during the study, the investigator had a sample size of 161 for the recruitment. Thus, the statistical analysis of this study bore at most 20 % of type II error and 5 % of type I error.
Measures
This study sought to investigate the relationships among demographic characteristics (age, marital status, school years, income, and exercise habits), disease characteristics (duration, pain level, number of chronic diseases, fracture experiences, and ADL), social support dimensions, and PQoL and MQoL of osteoporosis patients.
Demographic, disease characteristics, and ADL
Demographic variables and disease characteristics were measured with a demographic information form which was developed by one of the researchers. This form was used to record participants’ age; marital status as being married/co-living, widowed, divorced; education (years of schooling); monthly income (reported in Taiwan currency, NT dollar, <10,000, 10,000 to 20,000, and >20,000); exercise habits, dietary and/or calcium supplementation; and number of chronic diseases. Disease characteristics contained information about duration of osteoporosis, pain level, numbers of chronic diseases, fracture experiences, and ADL. Barthel’s scale is commonly used to measure ADL in neurological, muscular, or skeletal patients [25]. This questionnaire consists of ten items with total scores at 100. The overall score was the sum of all ratings, with higher scores indicating more independence of ADL. In this study, reliability was acceptable and Cronbach’s α was 0.91.
The social support questionnaire
Chang et al. [26] modified Barrera et al. [22] to develop the Inventory of Socially Supportive Behaviors (ISSB) to measure social support of participants. This questionnaire consists of 19 items in four dimensions: emotional support (ES; 1–4) focused on caring, listening, love, and trust; appraisal support (AS; 5–7), affirming individual’s actions and thoughts; informational support (IS; 8–13), providing the information of disease, suggestions of self-care; and tangible support (TS; 14–19) focused on providing assistance. Participants were asked to rate on a four-point scale (1 = none of the time, 2 = some or little of the time, 3 = occasionally or a moderate amount of time, 4 = most or all of the time) how frequently they had experienced certain symptoms or feelings during the previous week. The overall score was the sum of all ratings and ranged from 19 to 76, with higher scores reflecting a greater social support. This measurement has been used in a study of Huang et al. [19] to examine social support of stroke survivors by using the modified scale; Cronbach’s α was 0.90. In this study, reliabilities for these four constructs were acceptable, and values ranged from α = 0.71 to 0.91 for dimensions of social support.
Quality of life (Short-Form 36)
The 36-item Short Form (SF-36) of the Medical Outcomes Study (MOS) questionnaire was designed as a generic indicator of health [27]. The SF-36 had been shown to be a reliable and valid instrument and widely used to measure HrQoL in osteoporosis patients around the world [6]. The SF-36 serves as a measure of HrQoL, including eight subscales relevant to the general health of the individual: physical functioning, role limitations (problems with work or other daily activities as a result of physical health), bodily pain, social functioning, general mental health, role limitations (problems with work or other daily activities as a result of emotional problems), vitality, energy or fatigue, and general health perceptions. For easy interpretation, SF-36 is usually divided into two components, physical quality of life (PQoL) and mental quality of life (MQoL), and was employed in this manner for this study. The coefficients of Cronbach’s α were from 0.68 to 0.83 among these subscales in this analysis.
Data analysis
Except typical descriptive statistical approaches, the structural equation modeling (SEM) technique was implemented to analyze the acquired dataset. Prior to analysis, the dataset was evaluated in order to meet the assumptions of outliers, normality, and multicollinearity. Statistical tools, SPSS version 19.0, and AMOS version 19.0 were in use. Although Garver and Mentzer [28] and Hoelter [29] proposed a “critical sample size” of 200, the generally agreed-upon value is ten participants for every free parameter estimated [30]. The current sample (N = 161) was suitable for a model of nine exogenous variables.
Those structural path models were determined to examine the effects by risk factors and social support dimensions on health outcomes. Goodness of fit was evaluated by using the P value of the model minimum of discrepancy function (CMIN), goodness-of-fit index (GFI), average GFI (AGFI), and the root mean square error of approximation (RMSEA). Throughout the study, a path model was considered using the X 2/df ratio (<3), both the GFI and AGFI were greater than 0.90, and the RMSEA was below 0.08 [31–33]. A P value of 0.05 or less was set to indicate the statistical significance on effect weights.
Results
Participants’ characteristics
The characteristics of the sample and study variables are shown in Table 1. The majority of participants were married, and the average age was 70 years (SD = 11.2). Seventy (43.5 %) participants had been diagnosed with osteoporosis duration longer than 5 years. Seventy-four (46.0 %) participants were illiterate, and 49 (30.4 %) participants had at least an elementary school education. In addition, 76 (47.2 %) adults exercised at least three times per week. Only twelve (7.5 %) participants had no complaints of pain, 80 (49.7 %) participants had mild pain, and 69 (42.8 %) participants had moderate or serious pain. Regarding monthly income, 89 (55.3 %) participants had a monthly income of less than 10,000 NT dollars, approximately 330 USD. Sixty-six (41.0 %) of the participants had one chronic disease, 72 (44.8 %) had one fracture experience, and 78 (48.4 %) were independent in their activities of daily living.
Differences of HrQoL among participants
The differences of health-related quality of life among participants’ variables were shown in Table 2. Married participants had significantly better HrQoL than those of widowed ones. Participants who were illiterate had decreased HrQoL as compared with those with an elementary education or above. Household with monthly income greater than 20,000 NT dollars had better HrQoL compared to those with lower incomes. Participants who exercised more than three times per week had greater HrQoL than individuals who exercised less frequently. Participants with shorter duration of disease had decreased HrQoL than others, especially MQoL.
Relationships among variables
Bivariate correlations revealed that those who had higher pain scores and had less emotional and appraisal support (r = −0.261**, r = −0.226**) were more likely to have worse physical and mental QoL (r = −0.471***, r = −0.368***) (see Table 3). Moreover, the more emotional, appraisal, and informational support that the participants perceived, the more likely they were to report better physical and mental health-related QoL, but informational support was not significantly related to both PQoL and MQoL.
The age of participants negatively relate to ADL, PQoL, and MQoL (−.433***, −.287**, −.332***), and age also positively relate to the tangible support and fractures (.319*** and .274**); furthermore, age negatively relate to IS (−.187*). Participants’ ADL positively relate to both physical and mental QoL (.537*** and .482***), while it negatively relate to tangible support (−.321***) and informational support (.163*). Duration of osteoporosis for participants positively relate to fractures (.212**).
Development of a full path model
To investigate mediating effects, the full path model examined participant’s characteristics, disease factors, and social support on health-related quality of life by implementing structural equation model. After several model explorations and modifications, the standardized format was shown as Fig. 1. In this structural model, age, education, disease duration, and pain were regarded as independent variables. Both physical and mental QoL were regarded as dependent variables. In addition, four social support dimensions, such as emotional support (ES), appraisal support (AS), informational support (IS), and tangible support (TS), were determined as mediators between factors and physical/mental QoL. This optimal model included three path models toward endogenous measurements ADL, PQoL, and MQoL.
The direct/indirect effects on HrQoL
The overall goodness-of-fit statistics revealed that the employed model fits the dataset well with P = 0.87, χ 2/df = 0.67, GFI = 0.98, AGFI = 0.95, and RMSEA = 0.00. As shown in Fig. 1, this structural model consisted of nine independent variables (five individuals’ characteristics and four dimensions of social support) and two dependent variables (MQoL, PQoL). In addition, for integrated analysis concern, ordinal measurement such as education was used as a continuous variable. Furthermore, four dimensions of social support were arranged as mediators on HrQoL.
ADL exerted a direct effect on PQoL (β = 0.34***). Poorer physical status for adults with osteoporosis contributed to a worsening PQoL. Pain had significantly negative direct effects on both MQol and PQoL, that is, higher levels of education, physical independence, and lower degree of pain contributed to the better PQoL or MQoL. Informational support had significant direct effects (β = 0.27**) on PQoL, whereby higher levels of informational support led to better physical-related quality of life for individuals with osteoporosis. As shown in Fig. 1, three main path models, ADL, PQoL, and MQoL, and their squared multiple correlations R 2 were up to .35, .42, and .40, respectively. Coefficients reported in Fig. 1 are standardized regression weights. Both age and pain of participants very negatively influenced their ADL (−.44*** and − .40***); and pain also influenced both PQoL and MQoL (−.34*** & − .26***). In addition, ADL enhanced substantially both PQoL and MQoL (.34*** and .24**). In summary, regarding four social support dimensions, results showed that only informational support was crucial to enhancing osteoporosis patients’ physical and mental health.
Overall, this structural model explained 40 % of the variance in MQoL and 42 % in PQoL. Two mediation effects of ADL occurred between “pain” and PQoL/MQoL, and two mediation effects of informational support existed between “education” and PQoL/MQoL (Fig. 2).
Discussion
This study focuses on the relationships among demographic variables and four dimensions of social support on HrQoL. The majority of participants were elderly, which might have put them at increased risk for fracture and consequently increased mortality. In addition, most participants reported at least having mild pain, which could also impair their HrQoL. ADL positively influenced HrQoL, but it reversely affected tangible support. The higher the ADL, the less the tangible support of participants. In addition, ADL played well as a mediator of pain in HQoL. Thus, in order to enhance HQoL, interventions and/or rehabilitation should focus on pain management to improve activities of daily living.
Regarding social support influences, the disability literature notes that satisfaction with both quality and quantity of social support can have an impact on psychological outcomes [19, 20]; in the four social support dimensions in this current study, the results showed that informational support was crucial to enhancing osteoporosis patients’ HrQoL. The other two dimensions, appraisal and tangible support, reversely reinforced the effect, although the effect was insignificant. We recognized that information is important to those participants; moreover, proper psycho-education toward improving their management of health could help them prevent the prevalence of osteoporosis or more consequently decreasing. Hip fractures are a common occurrence in those with osteoporosis and have a negative impact on mortality and morbidity. It also may result in added burdens for patients and/or caregivers. Health-care professionals and health policy stakeholders should take these issues into consideration.
In the studied full path model, both emotional and tangible support had no significant effect on PQoL. The fact that a majority of participants (78 %) were independent might be a reason. Moreover, the informational support was a positive mediator on both PQoL and MQoL. With the enhancement effect from informational support, individuals with osteoporosis had realized better HrQoL to some extent worsen by pain initially.
There are methodological and sampling limitations in this study. First, one limitation in this study may be that a convenient sample rather than randomizing sample was used. The participants with osteoporosis were located in Southern and Central Taiwan which might have restricted the population. Thus the generalizability was limited to these parts of Taiwan. The findings might possibly be limited to those with similar characteristic backgrounds. Second, the sample was voluntary and might become less representative of the population which is a threat to external validity [34]. Third, the cross-sectional nature of the present data was another limitation which possibly made it difficult to assess study variables overtime. We could not project the longitudinal influences of independent variables such as ADL or different dimensions of support on the outcomes of osteoporosis patients.
Health-care professionals may use these results to help clients receive needed support. For future study, we may conduct an intervention such as exercise for improving individuals’ physical functioning; moreover, social support may increase better HrQoL for those osteoporosis patients. We can also investigate QoL following multiple time points. Moreover, a prospective and experimental research design may apply for testing the effectiveness of intervention for osteoporosis adults and which may also promote the consequent HrQoL for osteoporosis patients. In regard to age, another demographic data, older adults had worse social support and worse QoL than the younger ones, which implies that health-care professionals may need to consider the relationship between age and outcome. Older patients with osteoporosis may need more specific care and attention.
Health-care professionals may design further research on mediating and moderating effects between social support and health outcome variables. In recent years, HrQoL studies have mentioned the comorbidity and mortality in osteoporosis fractures. Suitable methods are available to assess QoL in patients with osteoporosis fractures. Quality of life can be measured to compare the effect of different treatments in patients with osteoporosis. The assessment of QoL is also useful in community health studies to assess the burden of disease and to evaluate the cost-effectiveness of the society. Further studies are required to assess the influence of comorbidity in patients with vertebral and hip fractures and to evaluate cultural differences in HrQoL.
Conclusion and relevance to clinical practice
Social support played as mediators between pain and HrQoL of individuals with osteoporosis. The results might help health-care professionals to better understand the relationships among ADL, different dimensions of social support, and HrQoL of patients with osteoporosis. Either improving ADL by exercising an intervention to enhance muscle strength or widening accesses to various dimensions of social support, osteoporosis patients may achieve a better HrQoL. Moreover, individuals were provided with adequate informational support which might prompt better health-related outcomes for osteoporosis patients.
The impact of osteoporosis is long lasting, and it is not limited to the individuals’ concerns, but it also may extend to their family caregivers. Once impairments of individuals with osteoporosis occurred, health-care professionals should implement exercise intervention and psycho-education intervention as well, in order to strengthen osteoporosis HrQoL. In addition, it is helpful to seek various dimensions of social support, for example, a support group in helping osteoporosis patients to strengthen their physical function or informational support to encourage knowledge of self-care.
References
Harvey N, Dennison E, Cooper C (2010) Osteoporosis: impact on health and economics. Nat Rev Urol 6(2):99–105
Wang Y, Tao Y, Hyman ME, Li J, Chen Y (2009) Osteoporosis in China. Osteoporosis Int 20(10):1651–1662
Looker AC, Melton LJ, Harris TB, Borrud LG, Shepherd JA (2010) Prevalence and trends in low femur bone density among older US adults: NHANES 2005–2006 compared with NHANES III. J Bone Miner Res 25(1):64–71
Guillemin F, Martinez L, Calvert M, Cooper C, Ganiats T, Gitlin M, Horne R, Marciniak A, Pfeilschifter J, Shepherd S, Tosteson A, Wade S, Macarios D, Freemantle N (2013) Fear of falling, fracture history, and comorbidities are associated with health-related quality of life among European and US women with osteoporosis in a large international study. Osteoporos Int 24(12):3001–3010
Looker AC (2013) Femur neck bone mineral density and fracture risk by age, sex, and race or Hispanic origin in older US adults from NHANES III. Arch Osteoporos 8(1–2):141
Wilson S, Sharp CA, Davie MW (2012) Health-related quality of life in patients with osteoporosis in the absence of vertebral fracture: a systematic review. Osteoporos Int 23(12):2749–2768
Krum SA, Brown M (2008) Unraveling estrogen action in osteoporosis. Cell Cycle 7(10):1348–1352
Roux C, Wyman A, Hooven FH, Gehlbach SH, Adachi JD, Chapurlat RD, Compston JE, Cooper C, Diez-Perez A, Greenspan SL, Lacroix AZ, Netelenbos JC, Pfeilschifter J, Rossini M, Saag KG, Sambrook PN, Silverman S, Siris ES, Watts NB, Boonen S (2012) Burden of non-hip, non-vertebral fractures on quality of life in postmenopausal women: the Global Longitudinal study of Osteoporosis in Women (GLOW). Osteoporos Int 23(12):2863–2871
Petronijevic M, Petronijevic N, Ivkovic M, Stefanovic D, Radonjic N, Glisic B, Ristic G, Damjanovic A, Paunovic V (2008) Low bone mineral density and high bone metabolism turnover in premenopausal women with unipolar depression. Bone 42(3):582–590
Chan HL, Liu CY, Chau YL, Chang CM (2011) Prevalence and association of suicide ideation among Taiwanese elderly—a population-based cross-sectional study. Chang Gung Med J 34(2):197–204
Wu Q, Magnus JH, Liu J, Bencaz AF, Hentz JG (2009) Depression and low bone mineral density: a meta-analysis of epidemiologic studies. Osteoporosis Int 20(8):1309–1320
de Oliveira FN, Arthuso M, da Silva R, Pedro AO, Neto AMP, Costa-Paiva L (2009) Quality of life in women with postmenopausal osteoporosis: correlation between QUALEFFO 41 and SF-36. Maturitas 62(1):85–90
Liu N, Zeng LX, Li Z, Wang JE (2013) Health-related quality of life and long-term care needs among elderly individuals living alone: a cross-sectional study in rural areas of Shaanxi Province. BMC Public Health, China, 13
Yilmaz F, Sahin F, Ergoz E, Deniz E, Ercalik C, Yucel S, Kuran B (2008) Quality of life assessments with SF 36 in different musculoskeletal diseases. Clin Rheumatol 27(3):327–332
Tadic I, Vujasinovic Stupar N, Tasic L, Stevanovic D, Dimic A, Stamenkovic B, Stojanovic S, Milenkovic S (2012) Validation of the osteoporosis quality of life questionnaire QUALEFFO-41 for the Serbian population. Health Qual Life Out 10:74
Ekstrom H, Ivanoff SD, Elmstahl S (2008) Restriction in social participation and lower life satisfaction among fractured in pain. Arch Gerontol Geriat 46(3):409–424
Qvist N, Bergstrom I, Kronhed ACG, Karlesson S, Forss A (2011) Empowering the fragile body: experiences of a back muscle group training program in postmenopausal women with vertebral fractures. A qualitative interview study. Adv Physiother 13(2):63–70
Ievers-Landis CE, Burant C, Drotar D, Morgan L, Trapl ES, Kwoh CK (2003) Social support, knowledge, and self-efficacy as correlates of osteoporosis preventive behaviors among preadolescent females. J Pediat Psychol 28(5):335–345
Huang CY, Hsu MC, Hsu SP, Cheng PC, Lin SF, Chuang CH (2010) Mediating roles of social support on poststroke depression and quality of life in patients with ischemic stroke. J Clin Nurs 19(19–20):2752–2762
Muller R, Peter C, Cieza A, Geyh S (2012) The role of social support and social skills in people with spinal cord injury—a systematic review of the literature. Spinal Cord 50(2):94–106
Krause N (1986) Social support, stress, and well-being among older adults. J Gerontol 41(4):512–519
Barrera M Jr, Sandler I, Ramsay T (1981) Preliminary development of a scale of social support: studies on college students. Am J Commun Psychol 9(4):435–447
Huang CY, Sousa VD, Tsai CC, Hwang MY (2008) Social support and adaptation of Taiwanese adults with mental illness. J Clin Nurs 17(13):1795–1802
Cohen J (1988) Statistical power analysis for the behavioral sciences. Lawrence Erlbaum Association, New Jersey
Shah S, Vanclay F, Cooper B (1989) Improving the sensitivity of the Barthel Index for stroke rehabilitation. J Clin Epidemiol 42(8):703–709
Chang CP, Tsai YF, Chen YC, Hwang SL (2001) Factors related to depression among burns patients. J Nurs 48(2):37–48. doi:10.6224/JN.48.2.37
Ware JE Jr, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30(6):473–483
Garver MS, Mentzer JT (1999) Logistics research methods: employing structural equation modeling to test for construct validity. J Bus Logist 20:33–57
Hoelter JW (1983) The analysis of covariance structures: goodness-of-fit indices. Sociol Method Res 11:325–344
Hoe SL (2008) Issues and procedures in adopting structural equation modeling techniques. J Appl Quant Method 3:76–83
Byrne BM (2001) Structural equation modeling with AMOS: basic concepts, applications, and programming. Lawrence Erlbaum Associates Publishers, Mahwah
Hu LZ, Bentler PM (1999) Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Modeling 6(1):1–55
Kline RB (2005) Principles and practice of structural equation modeling, 2nd edn. Guilford Press, New York
Cook DC, Campell DT (1979) Quasi-experimentation: design and analysis issues for field settings. Houghton Mifflin, Boston
Acknowledgments
There is no funding for this study. We would like to thank the patients from the four medical centers who participated in this study.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Huang, CY., Liao, LC., Tong, KM. et al. Mediating effects on health-related quality of life in adults with osteoporosis: a structural equation modeling. Osteoporos Int 26, 875–883 (2015). https://doi.org/10.1007/s00198-014-2963-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-014-2963-3