Abstract
Fragility fractures are correlated to reduced bone size and/or reduced volumetric bone density (vBMD). These region-specific deficits may originate from reduced mineral accrual and/or reduced skeletal growth during the first 2 decades of life. Before pathological development can be defined, normal skeletal growth must be described. To evaluate growth of bone size, accrual of bone mineral content (BMC), areal bone mineral density (aBMD) and vBMD in a population-based cohort, 44 boys and 42 girls were followed by annual measurements from the age of 12 to 16 (attendance rates 90–100%). Segmental bone length, bone width, BMC, aBMD and vBMD were measured by dual-energy X-ray absorptiometry (DXA). Data were compared with predicted adult peak, as determined in 36 men aged 27.7±4.6 years and 44 women aged 26.8±4.9 years. Growth in width of the femoral neck precedes accrual of BMC in the femoral neck in both genders up to age 15. The girls were at all ages closer to their predicted adult peak in both bone width and BMC compared with the boys except in the femoral neck. As femoral neck vBMD had reached its predicted adult peak already at 12 years in both genders, the increase in femoral neck BMC and femoral neck aBMD from age 12 to 16 was most likely to be explained by the increase in bone size. In boys the peak velocity growth was recorded at ~14 years for BMC, height, width and lean mass. Growth from the age of 12 to 16 seems to build a bigger but not a denser skeleton in the femoral neck.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bone fragility which increases the fracture risk may be conferred by a reduction in bone size, bone mass and/or changes in the three-dimensional skeletal architecture [1, 2]. The measurement for bone density used in the clinical setting, namely areal bone mineral density, aBMD, g/cm2, may in fracture patients partly be artifactural, as fragility fractures are related to reduced bone size [2]. aBMD does not account for the third dimension, the skeletal depth, so that a smaller bone will be reported as having a lower aBMD than a larger bone even if it has the same volumetric BMD, vBMD, g/cm3. Skeletal size and vBMD are both independent risk factors for fragility fractures [2, 3]. Women and men who have had a spine fracture have both a smaller vertebral body and lower vBMD, but normal femoral neck size and femoral neck vBMD compared to controls [2, 3]. Women and men who have suffered a hip fracture have lower femoral neck vBMD but normal spine vBMD, while only the men with a hip fracture have a smaller femoral neck size compared to controls [2, 3]. The reduced skeletal size and/or reduced vBMD in fracture patients may be the result of failed bone growth and/or reduced bone accrual during the first 2 decades in life and/or excessive bone loss and/or failed periosteal expansion during adult life. Finding a reduced aBMD in children of patients with fragility fracture indicates that a low peak aBMD may at least partly account for the low aBMD found in the fracture patients [4, 5, 6]. Thus, illness or other factors disturbing the skeletal modeling during adolescence may interfere with skeletal growth and mineral accrual, perhaps irreversibly. Depending on age, different skeletal deficits will then occur. A region and trait further from the predicted adult peak will develop a more severe deficit than a region closer to the predicted adult peak if intervened by a disease [7]. In order to increase our knowledge of the pathogenesis of osteoporosis and the expected deficits that may develop if illness occurs during childhood, we must first define the normal growth pattern.
However, most published studies in growing children are non-population based, cross-sectional [8, 9] and the discrepancy between cross-sectional and longitudinal data are well described [10, 11]. Additionally, longitudinal studies in growing children with more than two measurements are scarce, although a few have been published [12, 13, 14, 15].
The purpose of this longitudinal, population-based study was to evaluate the skeletal growth from the age 12 to 16 years in both girls and boys. We postulated that a difference in peak growth rate occurs, between girls and boys and with respect to growth in size and accrual of mass. We proposed the questions: (i) whether growth in bone size precedes accrual of mass, (ii) whether growth in bone size and accrual of mass in girls precedes growth in bone size and accrual of mass in boys, and (iii) whether there is a time lag between peak velocity width/peak velocity height and BMC.
Materials and methods
Subjects
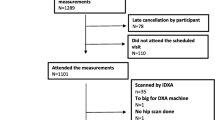
All pupils at a rural village in southern Sweden (Sösdala, population 2900), 45 girls and 48 boys, aged 12 and 13 years, were included in this longitudinal, population-based study. The children were all healthy and none was excluded. Bone mineral data from this population have previously been published with relation to physical activity [16, 17]. Bone size and bone mass were evaluated annually from age 12 or 13 to 16 years. Seven children moved during the study period, resulting in 86 children with at least two consecutive measurements available for inclusion in the final database. Twenty-three girls and 15 boys aged 12 years at baseline and 19 girls and 29 boys aged 13 years at baseline participated. Five measurements were offered to the 12-year-old pupils. Twenty-six of them attended all five measurements, nine for four, one for three, and two attended two measurements. Four measurements were offered to the 13-year-old pupils. Forty-five of them attended all four measurements and three attended three measurements. Only individuals with two consecutive measurements are included when longitudinal data are presented. (The attendance rate was between 90 and 100% at all measurements.) To compare growth data in the present population with predicted adult peak, a comparison was made with 36 men aged 27.7±4.6 years and 44 women aged 26.8±4.9 years from the same geographical region. They were measured by the same equipment and have previously been published as normative Swedish data [18].
Measurements
Bone size and bone mass were evaluated by dual-energy X-ray absorptiometry (DXA: Lunar DPX-L version 1.3z, Lunar, Madison, Wisc., USA). Bone mineral content, BMC, g, and aBMD were evaluated for the total body, spine and femoral neck, representing weight loaded skeletal regions, and of the head, representing an unloaded region. Femoral neck, FN bone size (width, cm) and FN vBMD were derived from the hip scan by the formula vBMD=BMC/estimated FN volume (π×r 2×FN length) where r=FN mid-diameter/2, assuming the FN to be cylindrical [2,19,20]. Total fat mass (kg) and total lean mass (kg) were derived from the total body scan. The precision, evaluated by duplicate measurements in 14 healthy adult individuals, was for aBMD total body 0.4%, spine 0.5%, FN 1.6% and head 1.7%. The precision for FN volume was 1.7% and for FN vBMD 1.5%, for total fat mass 4.1% and total lean mass 0.6%. Long-term precision was 0.6% over the study period, evaluated by scanning a Hologic spine phantom. The same equipment and software version was used in all measurements.
Bone mass in the forearm was evaluated by single-energy X-ray absorptiometry (SXA: Osteometer DTX-100, Osteometer, Denmark) in the non-dominant arm. BMC and aBMD were evaluated in the distal radius and ulna, DR, where the distance between radius and ulna is 8 mm (cortical bone), and in the ultradistal radius, UDR, adjacent to the radiocarpal joint (trabecular bone). The same equipment and software version was used in all measurements.
Height was measured by a standard height meter and weight with a non-electrical scale. Segmental lengths of the spine, arm and leg were measured by applying a software ruler on the total body scan. The spine was measured from the chin to the last lumbar vertebra, the arm from the superior border of the humeral head to the wrist joint and the leg from the superior border of the femoral head to the inferior border of the lateral malleolus.
Pubertal stage was determined according to Tanner and assessed by self-grading using photographs showing the different Tanner stages [21]. If individuals changed Tanner stage between two measurements, they were classified as the lower Tanner stage when the longitudinal changes in size and mass were evaluated in relation to pubertal development.
Statistical methods
The study was approved by the Ethical Committee of the University of Lund, Sweden. Data are presented in absolute terms, percentage terms and as rate of change (cm/year and g/year). To define the relative pattern of growth in bone size and accrual of mass, each measurement was expressed as a percentage of the predicted adult peak as derived from healthy individuals aged 20–40 years. Whole-year velocity values were calculated individually by dividing the difference between two following measurements with the age increment and expressed as relative change in percentages to control for size differences. To determine peak velocity from the whole-year velocity values a Lowess fitting curve procedure was used. Student's t-test between means was used when comparing boys and girls at different ages or Tanner stages. The statistical calculations were performed using Statistica version 6.1 (StatSoft, Inc).
Results
Growth in relation to chronological age
Bone size
Growth in length in the appendicular skeleton preceded growth in length in the axial skeleton by about 1 year in both girls and boys (Fig. 1). The girls seemed to reach their predicted adult peak in total body height, length of spine, length of arms and length of legs about 2 years earlier than the boys. The appendicular skeleton was at 12 years about 5% closer to the predicted adult peak than the axial skeleton in both genders, with a remaining leg growth of 7% in the girls and 15% in the boys and a remaining spine growth of 12% in the girls and 21% in the boys (Tables 1 and 2, Fig. 1).
Spine length and leg length in girls (●) and boys (∆) 12–16 years of age and Tanner stages 2–5 in relation to the expected adult peak value (=100%). Data are treated as cross-sectional and includes all measurements available at each age group. Data presented as mean±SEM. P-values represent t-test between boys and girls corrected for multiple comparisons (Bonferroni)
Growth of the FN width followed a similar pattern in both girls and boys from the age of 14. Both genders seemed to reach their predicted adult peak at about the age of 16. The width of the FN had at 12 years a remaining growth of 15% in the girls and 23% in the boys (Tables 1 and 2, Fig. 2). At all ages, length was closer to the predicted adult peak than width in both genders.
Bone mineral content (BMC), bone size (width), areal bone mineral density (aBMD) volumetric bone mineral density (vBMD) in the femoral neck for ages 12 to 16 in girls (●) and boys (∆) in relation to the expected adult peak value (=100%). Data are treated as cross-sectional and include all measurements available at each age group. Data presented as mean±SEM P-values represent t-test between boys and girls corrected for multiple comparisons (Bonferroni)
Bone mass
The accrual of BMC in the FN preceded the accrual of BMC in the spine by about 1 year in the girls and 1–2 years in the boys up to age 14 years (Fig. 3). FN BMC had virtually reached the predicted adult peak at 16 years in both genders. The FN BMC in the girls was at 12 years 10% closer to the predicted adult peak than the spine BMC, and the FN BMC in the boys was at 12 years 16% closer to the peak than the spine BMC. The remaining BMC to be accrued from 12 years was in the FN 26% for the girls and 36% for the boys, and in the spine 36% for the girls and 52% for the boys (Tables 1 and 2, Fig. 3). At all ages and for both genders, bone length and bone width were closer to the predicted adult peak than BMC (Tables 1 and 2).
Femoral neck (FN) bone mineral content (BMC) and spine BMC in girls (●) and boys (∆) of age 12–16 years, and Tanner stages 2–5 in relation to the expected adult peak value (=100%). Data are treated as cross-sectional and include all measurements available at each age group. Data are treated as cross-sectional and include all measurements available at each age group. Data presented as mean±SEM P-values represent t-test between boys and girls corrected for multiple comparisons (Bonferroni)
vBMD had reached the predicted adult peak already at 12 years or earlier in both genders (Tables 1 and 2, Fig. 2). At all ages, vBMD was closer to the predicted adult peak than BMC.
Peak velocity
For girls, fewer than ten individual peak velocity values could be identified. For all the others, the peak velocity values were declining already from the start of the study. The peak value for the girls most likely appeared before age 13.
Since the individual peak velocity value for the measured parameters could only be captured for about half of the boys (in the other half the highest peak velocity values were recorded between the last two measurements or occasionally between the first two), no true longitudinal mean peak value could be calculated. Instead, we plotted the relative changes in percentages between the measurements in Figs 4 and 5 for TB BMC, TB lean mass, height, FN BMC and FN width. The peak values, as estimated from the plots, were for all ~13.9 years.
Growth in relation to pubertal development
Bone size
Growth in length in the appendicular skeleton preceded growth in length in the axial skeleton at every Tanner stage (Tables 3 and 4, Fig. 1). The girls reached their predicted adult peak in total body height, length of spine, length of arms and length of legs at Tanner stage 4, whereas the boys reached their predicted adult peak in total body height and segmental lengths at Tanner stage 5. The appendicular skeleton at Tanner stage 2 was 5–8% closer to the predicted adult peak than the axial skeleton in both genders, with a remaining leg growth of 5% in the girls and 14% in the boys, and a remaining spine growth of 10% in the girls and 22% in the boys (Tables 3 and 4, Fig. 1).
The growth of FN width in girls preceded the growth of the FN width in boys at Tanner stages 2–4. Both genders reached their predicted adult peak at Tanner stage 5. The FN width at Tanner stage 2 had a remaining growth of 15% in the girls and 25% in the boys (Tables 3 and 4, Fig. 2). At all Tanner stages, segmental lengths were closer to the predicted adult peak than the FN width in both genders.
Bone mass
The accrual of BMC in the FN preceded the accrual of BMC in the spine by about 0–1 Tanner stage in the girls and 1–2 Tanner stages in the boys (Tables 3 and 4, Fig. 3). Spine BMC in the girls and FN BMC in the boys had reached their predicted adult peak at Tanner stage 5. The FN BMC at Tanner stage 2 was 14% closer to the predicted adult peak than the spine BMC in the girls, and 16% closer to the predicted adult peak in the boys. The BMC remaining to be accrued at Tanner stage 2 was in the FN 26% for the girls and 41% for the boys, and in the spine 40% for the girls and 57% for the boys (Tables 3 and 4). At Tanner stages 2–4, bone length and bone width were closer to the predicted adult peak than BMC in both genders (Tables 3 and 4).
vBMD had reached the predicted adult peak already at Tanner stage 2 or earlier in both genders. At all ages, vBMD was closer to the predicted adult peak than the BMC.
Discussion
We report in this 4-year longitudinal, population-based study that (i) growth in bone size precedes the accrual of mass in both genders, (ii) growth in bone size and accrual of mass in girls precedes the growth in bone size and accrual of mass in boys, (iii) peak vBMD in the femoral neck was reached already at 12 years (or earlier) in both genders and (iv) no time lag between peak velocity width/peak velocity height and BMC accrual could be observed for boys.
The results regarding growth and bone mass as evaluated by DXA, have previously been described with more or less the same outcome in previous longitudinal or cross-sectional studies [9, 12, 14]. The contribution of our study is the high attendance rate, population-based longitudinal measurements. Furthermore, it is not clear if results from other parts of the world could be applied on other populations apart from Scandinavian, and this is the first prospective study from Scandinavia in this age group. In most longitudinal studies, the numbers of individual measurements exceeding two are scarce. This often means when analyzing data, there is a tendency to mix cross-sectional and longitudinal in the same presentation. This is also a problem in our study where the numbers differ at each measurement. The strength in our study is the high attendance rate (83%), which means that the analyses will be more longitudinal than cross-sectional.
Understanding bone fragility requires a knowledge of the development of the appendicular and the axial bone size and mineral accrual during growth, and a knowledge of bone loss during aging. Throughout the period of growth, bone size is closer to the expected adult peak than the mineral accrued within the periosteal envelope. Before puberty, the growth of the legs and arms is more rapid than the growth of the trunk, and during puberty, appendicular growth slows and axial growth accelerates [22, 23]. The growth pattern is also gender-specific, with girls closer to their predicted adult peak than boys at the same age and at the same pubertal stage [10, 22, 23, 24, 25]. The present study supports the studies cited, of a heterogeneous skeletal development during the period of growth [22, 23, 25, 26, 27], and also infers that growth in Scandinavian adolescents resembles growth in previous published cohorts.
We could not repeat the results of Bailey et al. [10] concerning peak velocity curves. For the girls, we would have needed further measurements prior to age 12–13 years. For the boys, the true longitudinal peak for each individual could not be calculated, because like in the girls we would have needed further measurements. We could not detect a time lag difference between the different traits like Bailey et al.; however, our data cannot rule out that this also exists in the Scandinavian cohort. The velocity curves for boys TB lean mass and BMC seems to be almost identical, which means that during this period of life the skeleton's response to load seems to be of minor importance. A previous report from our group supports this [17].
The trait-, region- and gender-specific differences of growth in relation to chronological age and pubertal development indicates that the regulation of growth differs. Data in the literature support this; before puberty, periosteal expansion increases more than endosteal expansion, with increased cortical thickness as a result [22, 25]. During puberty, the periosteal expansion decreases in females, whereas it accelerates in males, resulting in a thicker cortical shell and a stronger skeleton in males [25, 28]. Endocortical contraction develops during puberty, more in girls than in boys, increasing the cortical thickness and bone strength in the girls [22]. The data in the current study contradict this. As vBMD was virtually constant in spite of an increasing FN width, it suggests that also en endocortical expansion occurred in both genders. Possibly, the periosteal and endocortical surface develops differently in different bones, but also different in different regions within the same bone [29]. However, differences in the growth pattern may result in similar cortical thickness in both genders at the end of puberty, but a wider and stronger bone as the end result in boys [30].
BMC and aBMD, the measures used clinically for bone mineral density, are good predictors of future fragility fractures [31, 32, 33, 34]. However, the failure of these measurements to distinguish between the contribution of bone size and bone mass, the two independent mechanisms for bone fragility (reduced bone size and reduced vBMD), will lead to an unsatisfactory understanding of the pathogenesis of osteoporosis. Reduced vBMD will occur if a deficit in size is relatively less than the deficit of mineral accrual within the periosteal envelope. vBMD will be a function of the relationship between size and mass, not just the absolute change in either.
From 12 years, FN size and FN BMC increase proportionally in healthy children, resulting in a virtually constant vBMD. As BMC is unadjusted for size and aBMD only partially adjusted, these traits will increase during growth [22, 35, 36, 37]. If only aBMD is applied, we would make erroneous inferences regarding the development of bone mass. We infer, supported by the present data and those of several other studies, that after 12 years, mainly size accounts for the increase in BMC and aBMD with age and not an increase in the vBMD [19, 20, 22, 23, 25, 37, 38]. Gilsanz et al. [38] reported constant vBMD in the lumbar spine and no difference in vBMD between boys and girls, but the size of the vertebra was bigger for boys than girls. Cowell et al. [19] and Lu et al. [20] reported that in contrast to FN aBMD, FN vBMD and midshaft femur vBMD were more or less constant from 5 to 27 years in a cross-sectional setting and not related to age in either boys or girls. Bradney et al. [23], and Bass et al. [22] reported a small but significant increase in midshaft femur vBMD in late puberty, but virtually no increase prepubertally. One weakness when evaluating vBMD with the DXA technique is that the estimation of vBMD is only a hypothetical estimation (an apparent volumetric BMD), since it calculates the skeletal volume from the measured skeletal area. Different methods to evaluate the vBMD may reach different outcomes. Also, the studies cited above evaluated skeletal regions different from those in the present study, regions that may be differently developed maturationally. Furthermore, when Bass et al. [22] predicted adult peak in the midshaft femoral vBMD 16-year-old girls were used, an age group in which a small remaining growth in bone size is expected to occur, as reported by the same author and by Bradney et al. [23] Bradney et al. [23] used only 14 men when calculating the predicted adult peak in the male study, a number in which a few outliners could confound the predicted adult peak value. In spite of this, most studies cited support the finding of a virtually constant vBMD from 12 years, with increased size conferring the main increases in BMC and aBMD.
We conclude that growth in bone size in the arms and legs precedes growth in bone size in the spine, and growth in size precedes accrual of mass in both genders. As FN vBMD did not change from 12 to 16 years, the increase in BMC (and aBMD) was most likely to be explained by an increase in bone size. Peak velocity growth was recorded at ~14 years with no time lag difference between height, skeletal width or BMC. We conclude that discrepancies in skeletal development may predispose to region-specific defects should illness intervene. A better knowledge of the pathogenesis of osteoporosis may be attained by evaluating whether bone fragility in old age may, at least partly, be the result of growth-related interference in skeletal size, mass or architecture during the first 2 decades in life.
References
Karlsson M, Duan Y, Ahlborg H, Obrant K, Johnell O, Seeman E (2001) Age, gender, and fragility fractures are associated with differences in quantitative ultrasound independent of bone mineral density. Bone 28:118–122
Seeman E, Duan Y, Fong C, Edmonds J (2001) Fracture site-specific deficits in bone size and volumetric density in men with spine or hip fractures. J Bone Miner Res 16:120–127
Duan Y, Parfitt A, Seeman E (1999) Vertebral bone mass, size, and volumetric density in women with spinal fractures. J Bone Miner Res 14:1796–1802
Evans RA, Marel GM, Lancaster EK, Kos S, Evans M, Wong SY (1988) Bone mass is low in relatives of osteoporotic patients. Ann Int Med 109:870–873
Seeman E, Hopper JL, Bach LA et al. (1989) Reduced bone mass in daughters of women with osteoporosis. N Engl J Med 320:554–558
Ristevski S, Yeung S, Poon C, Wark JW, Ebeling P (1997) Ostepenia is common in young first-degree realtives of men with osteoporosis. Annual scientific meeting of Australian and New Zealand Bone Min Soc, Canberra, Australia
Seeman E, Karlsson MK, Duan Y (2000) On exposure to anorexia nervosa, the temporal variation in axial and appendicular skeletal development predisposes to site-specific deficits in bone size and density: a cross-sectional study. J Bone Miner Res 15:2259–2265
Bonjour JP, Theintz G, Buchs B, Slosman D, Rizzoli R (1991) Critical years and stages of puberty for spinal and femoral bone mass accumulation during adolescence. J Clin Endocrinol Metab 73:555–563
Lloyd T, Rollings N, Andon MB et al. (1992) Determinants of bone density in young women. I. Relationships among pubertal development, total body bone mass, and total body bone density in premenarchal females. J Clin Endocrinol Metab 75:383–387
Bailey DA, McKay HA, Mirwald RL, Crocker PR, Faulkner RA (1999) A six-year longitudinal study of the relationship of physical activity to bone mineral accrual in growing children: the University of Saskatchewan bone mineral accrual study. J Bone Miner Res 14:1672–1679
Karlsson MK, Obrant KJ, Nilsson BE, Johnell O (2000) Changes in bone mineral, lean body mass and fat content as measured by dual energy X-ray absorptiometry: a longitudinal study. Calcif Tissue Int 66:97–99
Bailey DA (1997) The Saskatchewan Pediatric Bone Mineral Accrual Study: bone mineral acquisition during the growing years. Int J Sports Med 18:S191–194
Maynard LM, Guo SS, Chumlea WC et al. (1998) Total-body and regional bone mineral content and areal bone mineral density in children aged 8–18 y: the Fels Longitudinal Study. Am J Clin Nutr 68:1111–1117
Bachrach LK, Hastie T, Wang MC, Narasimhan B, Marcus R (1999) Bone mineral acquisition in healthy Asian, Hispanic, black, and Caucasian youth: a longitudinal study. J Clin Endocrinol Metab 84:4702–4712
Nguyen TV, Maynard LM, Towne B et al. (2001) Sex differences in bone mass acquisition during growth: the Fels Longitudinal Study. J Clin Densitom 4:147–157
Sundberg M, Gardsell P, Johnell O et al. (2001) Peripubertal moderate exercise increases bone mass in boys but not in girls: a population-based intervention study. Osteoporos Int 12:230–238
Sundberg M, Gardsell P, Johnell O et al. (2002) Physical activity increases bone size in prepubertal boys and bone mass in prepubertal girls: a combined cross-sectional and 3-year longitudinal study. Calcif Tissue Int 71:406–415
Karlsson MK, Obrant KJ, Nilsson BE, Johnell O (1998) Bone mineral density assessed by quantitative ultrasound and dual energy X-ray absorptiometry. Normative data in Malmo, Sweden. Acta Orthop Scand 69:189–193
Cowell CT, Lu PW, Lloyd-Jones SA et al. (1995) Volumetric bone mineral density—a potential role in paediatrics. Acta Paediatr Suppl 411:12–6, 17
Lu PW, Cowell CT, LLoyd-Jones SA, Briody JN, Howman-Giles R (1996) Volumetric bone mineral density in normal subjects, aged 5–27 years. J Clin Endocrinol Metab 81:1586–1590
Duke PM, Litt IF, Gross RT (1980) Adolescents' self-assessment of sexual maturation. Pediatrics 66:918–920
Bass S, Delmas PD, Pearce G, Hendrich E, Tabensky A, Seeman E (1999) The differing tempo of growth in bone size, mass, and density in girls is region-specific. J Clin Invest 104:795–804
Bradney M, Karlsson MK, Duan Y, Stuckey S, Bass S, Seeman E (2000) Heterogeneity in the growth of the axial and appendicular skeleton in boys: implications for the pathogenesis of bone fragility in men. J Bone Miner Res 15:1871–1878
Fournier PE, Rizzoli R, Slosman DO, Theintz G, Bonjour JP (1997) Asynchrony between the rates of standing height gain and bone mass accumulation during puberty. Osteoporos Int 7:525–532
Bradney M, Pearce G, Naughton G et al. (1998) Moderate exercise during growth in prepubertal boys: changes in bone mass, size, volumetric density, and bone strength: a controlled prospective study. J Bone Miner Res 13:1814–1821
Theintz G, Buchs B, Rizzoli R et al. (1992) Longitudinal monitoring of bone mass accumulation in healthy adolescents: evidence for a marked reduction after 16 years of age at the levels of lumbar spine and femoral neck in female subjects. J Clin Endocrinol Metab 75:1060–1065
Matkovic V, Jelic T, Wardlaw GM et al. (1994) Timing of peak bone mass in Caucasian females and its implication for the prevention of osteoporosis. Inference from a cross-sectional model. J Clin Invest 93:799–808
Garn SM (1970) The earlier gain and later loss of cortical bone. Nutritional perspectives. C.C. Thomas Publishers, Springfield, Illinois, pp 3−120
Bass SL, Saxon L, Daly RM et al. (2002) The effect of mechanical loading on the size and shape of bone in pre-, peri-, and postpubertal girls: a study in tennis players. J Bone Miner Res 17:2274–2280
Ruff CB, Hayes WC (1988) Sex differences in age-related remodeling of the femur and tibia. J Orthop Res 6:886–896
Gärdsell P, Johnell O, Nilsson BE (1989) Predicting fractures in women by using forearm bone densitometry. Calcif Tissue Int 44:235–242
Hui SL, Slemenda CW, Johnston Jr CC (1989) Baseline measurement of bone mass predicts fracture in white women. Ann Int Med 111:355–361
Melton LJ 3, Atkinson EJ, O'Fallon WM, Wahner HW, Riggs BL (1993) Long-term fracture prediction by bone mineral assessed at different skeletal sites. J Bone Miner Res 8:1227–1233
Düppe H, Gärdsell P, Nilsson B, Johnell O (1997) A single bone density measurement can predict fractures over 25 years. Calcif Tissue Int 60:171–174
Düppe H (1997) Bone mass in young adults. Determinants and fracture prediction. Thesis, Malmö, Lund University
Sundberg M, Gärdsell P, Johnell O, Ornstein E, Sernbo I (1998) Comparison of quantitative ultrasound measurements in calcaneus with DXA and SXA at other skeletal sites: a population-based study on 280 children aged 11–16 years. Osteoporos Int 8:410–417
Bass S, Pearce G, Bradney M et al. (1998) Exercise before puberty may confer residual benefits in bone density in adulthood: studies in active prepubertal and retired female gymnasts. J Bone Miner Res 13:500–507
Gilsanz V, Boechat MI, Roe TF, Loro ML, Sayre JW, Goodman WG (1994) Gender differences in vertebral body sizes in children and adolescents. Radiology 190:673–677
Acknowledgements
Financial support was obtained from Kristianstad Higher Educational School, Region Skåne, Lund University and Malmö University Hospital Foundations.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sundberg, M., Gärdsell, P., Johnell, O. et al. Pubertal bone growth in the femoral neck is predominantly characterized by increased bone size and not by increased bone density—a 4-year longitudinal study. Osteoporos Int 14, 548–558 (2003). https://doi.org/10.1007/s00198-003-1406-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-003-1406-3