Abstract
Introduction and hypothesis
We compared the prevalence of fecal incontinence between constipated and nonconstipated women and correlated its prevalence with the number of Rome III constipation symptoms.
Methods
We performed a cross-sectional survey to evaluate the prevalence of fecal incontinence and constipation among women who presented to two gynecologic clinics for routine care over a 24-month period. Fecal incontinence was defined as loss of well-formed and/or loose stool beyond the patient’s control that occurred at least once in the last 4 weeks, was bothersome, had been present for the past 3 or more months, and had affected the person’s activities, relationships, or feelings. Constipation was diagnosed using the Rome III criteria. Our study was exempt from institutional review board approval because it was a survey and did not ask for information that could be used to identify the participant.
Results
Mean age of the 2,319 participants was 50.1 ± 15 years and mean body mass index (BMI) was 28.7 ± 7. Seven hundred and twenty-five (31 %) women had constipation, and 233 (10 %) had fecal incontinence. One hundred and one (43 %) incontinent women had coexisting constipation. Logistic regression analysis identified white race (p = .013), menopause (p = .010), and constipation (p = .004) as risk factors for fecal incontinence. After controlling for these risk factors, constipated women were more likely to have fecal incontinence than nonconstipated women [relative risk (RR) 1.60, 95 % confidence interval (CI) 1.26–2.05]. In addition, the prevalence of fecal incontinence was strongly associated with the number of Rome III constipation symptoms (p < .001).
Conclusion
Constipation is an important risk factor for fecal incontinence.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Fecal incontinence (FI) is a physically and psychologically disabling condition with major social implications for the affected individual. It is present in about 2–17 % of all individuals, with a disproportionately higher prevalence among women, the elderly, and personal care facility residents [1, 2]. A major reason why FI can have such a debilitating effect is that its exact cause(s) is often unknown, which makes this condition less amenable to effective treatment. For example, anal sphincter tear and pelvic floor injury sustained during vaginal delivery are widely believed to be the major cause of FI in women [3]. However, neither surgical nor nonsurgical treatment designed to correct or compensate for these injuries have been very effective in alleviating this condition [4–8].
One approach to improving therapeutic outcome is to identify potential treatable conditions that either precipitate or exacerbate FI. One such condition is constipation, which has been cited as a risk factor for FI [9]. However, the relationship between constipation and FI among women is unclear. Studies associating these conditions often focus on high-risk groups, such as personal care home residents, whereas the few investigators that surveyed persons living in the community used study designs that overestimate the prevalence of FI by including individuals with transient gastrointestinal conditions, involuntary fecal loss that does not affect the person’s daily activity or quality of life (QoL), and other known causes of incontinence such as irritable bowel syndrome (IBS) [10–12]. We conducted this study to increase our understanding of the relationship between FI and constipation. Our first aim was to compare the prevalence of FI between constipated and nonconstipated women. Our second aim was to correlate the prevalence of FI with the number of constipation symptoms described in the Rome III criteria [13]. Identifying a frequently treatable risk factor that either precipitates or exacerbates FI is an important first step toward alleviating the adverse effects of this frequently devastating condition.
Materials and methods
This cross-sectional study was conducted at the outpatient gynecologic clinics of West Virginia University and East Carolina University Schools of Medicine. The Institutional Review Board at each site reviewed our study and concluded that the survey qualified for exempt status, as it was a questionnaire and did not ask for information that could be used to identify the participant. The study was performed to determine the prevalence of FI and constipation among women who presented to the study sites for routine gynecologic care over a 24-month period. Our clinic staff invited these women to complete our anonymous survey in the waiting room and deposit the completed form in a sealed box. Each was reminded not to fill out the form again if she had already completed the survey during a previous visit. Women unable to read English, were taking antidiarrheal medications, had delivered within the preceding 12 months, or were referred to urogynecologic clinic; who had pelvic radiation, IBS, celiac disease, or inflammatory bowel diseases; or who did not complete the survey were excluded. The 5-page questionnaire asked for demographic information, past obstetrical history, specific medical conditions, previous surgical procedures, prior pelvic radiation, current medications, menopausal status, and bowel symptoms.
The prevalence of FI was surveyed using four of the validated questions proposed by Barber and Vaizey [14, 15] (Table 1). FI was defined as loss of well-formed and/or loose stool beyond the individual’s control and had been present for the past 3 or more months, had occurred at least once in the last 4 weeks, was bothersome, and had affected activities, relationships, or feelings.
Constipation and IBS were diagnosed using the Rome III criteria [13]. The diagnosis of constipation required the presence of at least two of the following six symptoms in ≥25 % of bowel movements. These symptoms include straining, sensation of incomplete evacuation, and sensation of anorectal obstruction/blockage during bowel movements; using manual maneuvers to facilitate bowel movements; having lumpy or hard stools and fewer than three bowel movements per week. These symptoms must have been present for the past 3 months, with onset at least 6 months prior to diagnosis plus the absence of IBS. In addition, loose stools were rarely present without using a laxative. IBS was diagnosed by recurrent abdominal pain or discomfort, which occurred at least 3 days per month within the last 3 months, with onset ≥6 months prior to diagnosis. This pain or discomfort must be associated with at least two of the following three symptoms: Improvement in abdominal pain or discomfort with bowel movement, onset of pain or discomfort associated with a change in frequency of stool, and onset of pain or discomfort associated with a change in form (appearance) of stool.
A previous study found that approximately 26 % of women attending gynecologic clinics for routine care had FI and 25 % had constipation [12]. Assuming that the prevalence of FI is 10 % higher in constipated than nonconstipated women (31 % vs. 21 %), sample size analysis showed that 321 participants would be needed in each group to provide 80 % power to detect this difference with 0.05 significance. If we further assume that the prevalence of constipation among of our participants is also 25 %, then a sample size of 1,200 women would provide 325 constipated and 875 nonconstipated women.
Statistical analysis was performed using JMP statistical software, version 8 (SAS Institute, Cary, NC, USA). Categorical data were analyzed for significance using the chi-square test or Fischer’s exact test, as appropriate. Logistic regression was used to assess the significance of risk factors while controlling for other conditions.
Results
Two thousand five hundred and eighty-two women completed our survey. Approximately half of the participants came from each of the two sites. Two hundred and sixty-three (10 %) were excluded, comprising 15.6 % who did not complete the survey, 218 (8 %) with IBS, 6.2 % with inflammatory bowel disease, and 24 (1 %) who had given birth within the past year. The age of the remaining 2,319 women ranged from 16 to 94 years, with a mean of 50.1 ± 15. Their average BMI was 28.7 ± 7. Ethnicity comprised 89 % white, 9 % African American, and 2 % other. Median parity was two with a range of 0–14, and 10 % was nulliparous. Among the multiparas, 75 % had vaginal deliveries only.
Seven hundred and twenty-five (31 %) women had constipation. Within that group, 305 (42 %) had two of the six symptoms described in Rome III criteria, 210 (29 %) had three symptoms, 145 (20 %) had four, and 65 (9 %) had five or six. The most prevalent symptom was straining during bowel movement, which was present in 31 % of women surveyed. Two hundred and thirty-three (10 %) of the 2,319 women surveyed had FI. This involuntary loss occurred daily in 37 (16 %), weekly in 80 (34 %), sometimes in 72 (31 %), and rarely in 44 (19 %). One hundred and one (43 %) of these incontinent women had coexisting constipation.
Demographics and characteristics of incontinent and continent women are detailed in Table 2. The prevalence of FI was higher in constipated than in nonconstipated women [101/725 (14 %) vs. 132/1,594 (8 %), p <0.001], whereas the prevalence of constipation was higher in incontinent than continent women [101/233 (43 %) vs. 624/2086 (30 %), p <0.001].
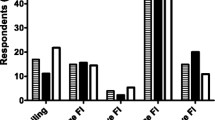
Logistic regression analysis identified race (p = .013) and menopause (p = .010) as risk factors for FI. After controlling for both risk factors, constipated women were more likely to have FI than were nonconstipated women [relative risk (RR) 1.60, 95 % confidence interval (CI) 1.26−2.05), and the prevalence of incontinence was strongly associated with the number of constipation symptoms described in the Rome III criteria (p < .001) (Fig. 1).
As the prevalence of FI in our study (10 %) was significantly lower than the estimation used in our sample-size calculation (26 %), we performed a retrospective analysis and found that 458 constipated and 458 nonconstipated women would provide an 80 % power to detect the 6 % (14 % vs. 8 %) difference in the prevalence of incontinence, with 0.05 significance.
Conclusion
Our study found that constipated women were more likely to have FI than their nonconstipated counterparts. In addition, FI was strongly correlated with the number of constipation symptoms described in the Rome III criteria. These findings suggest that constipation is an important risk factor for FI. Our study also found that FI and constipation were prevalent among women attending gynecologic clinics for routine care, and approximately half of the incontinent women were constipated.
Although they are widely believed to be mutually exclusive conditions, constipation may sometimes lead to FI. One possible mechanism is that constipation often produces small pieces of hard feces, which are more difficult for the individual to retain than large, bulky stool, especially if the person had a previous injury or age-related deterioration to the anal continence mechanisms. A second possible mechanism is that when a sufficient amount of stool accumulates in the rectum, it distends the intestinal lumen and relaxes the internal anal sphincter, resulting in intermittent incontinence while also allowing liquid stool from the upper intestine to seep past the fecal bolus, further increasing involuntary loss.
The generally accepted definition of FI does not include symptom duration. However, the Rome III criteria define functional (idiopathic) FI as uncontrolled passage of fecal material recurring for at least 3 months [16]. The reason for including this time frame is to avoid the inclusion of self-limited gastrointestinal conditions. Similarly, we included the 3-month duration in our definition since it is FI, which occurs episodically over a prolonged period of time that impairs daily function, places perpetual demands on the individual, and leads to social stigma and isolation. Also, with increased understanding of its pathophysiology and our diagnostic ability, functional FI is often difficult to distinguish from involuntary loss due to structural abnormalities in individual patients. This blurring in distinction is often caused by the unclear causal relation between structural abnormalities (such as anal sphincter tear) and incontinence, as these abnormalities may be present in both continent and incontinent individuals, as well as the heterogeneous nature of this disorder in that women often exhibit more than one structural and functional disturbance, each of which may contribute to but cannot solely explain the symptom.
Our data are consistent with findings from a previous report that surveyed 457 women from seven gynecologic clinics, which found that more constipated women had anal incontinence than did nonconstipated women and that both conditions were prevalent among the study population [12]. However, the prevalence of FI in the previous study was almost 2.5 times higher than found in this survey. Possible reasons for this difference are that our study included only individuals who had involuntary loss that had been present for at least 3 months and affected their activities, relationships, or feelings, while excluding women with IBS, which is known to cause FI.
Our study did not include women with flatal incontinence, as it has less impact on QoL than does involuntary loss of stool, and it is difficult to determine when passage of flatus is considered abnormal [12, 16]. Our survey also did not use a standardized scale to objectively measure the severity of FI. As FI is a symptom, we agreed with other investigators and used the person’s subjective perception as the foundation of our evaluation and the impact of incontinence. Similarly, we did not use a standardized scale to measure the severity of constipation. Although this study used the Rome III criteria to diagnose constipation, our literature search found no study that correlated the number of Rome III symptoms with constipation severity.
The strength of our study is that it surveyed a large number of women and included only women whose FI was chronic and affected her activities, relationships, or feelings. A used probable weakness is that this was not a population-based study, and the racial composition of participants did not reflect the general population of the United States. Despite this limitation, we believe our findings are important. The prevalence of FI and its relationship to constipation among women attending gynecologic clinics for routine care is important information for practicing gynecologists. A second probable weakness is that the higher prevalence of constipation in incontinent women may be caused by medication and/or treatment used to manage the involuntary loss of stool. Medication is a highly unlikely cause, as we excluded all women who were taking antidiarrheal medications. Similarly, behavioral changes, dietary modifications, and fiber therapy are unlikely causes, as our study included only women who had FI for at least 3 months, and they are thus unlikely to continue any unsuccessful therapy for such a length of time, especially if these treatments cause other uncomfortable gastrointestinal symptoms.
Constipation is rarely mentioned as a risk factor for FI, and there are few available data demonstrating a relation between these two conditions, which are widely believed to be mutually exclusive. Our study showed that constipation is a prominent risk factor for FI. This finding suggests that we need to investigate whether relieving constipation is an effective treatment for FI. In the mean time, we believe that healthcare providers should routinely screen all women with FI for constipation, as such screening may identify a potential etiology for this frequently devastating condition, which is often treatable with minimal morbidity and cost.
References
Nelson RL (2004) Epidemiology of fecal incontinence. Gastroenterology 126(Suppl 1):S3–S7
Whitehead WE, Norton NJ, Wald A (2004) Advancing the treatment of fecal and urinary incontinence through research. Gastroenterology 126(Suppl 1):S1–S2
Kamm MA (1994) Obstetric damage and faecal incontinence. Lancet 344:730–3
Karoui S, Leroi AM, Koning E, Menard JF, Michot F, Denis P (2000) Results of sphincteroplasty in 86 patients with anal incontinence. Dis Colon Rectum 43:813–20
Trowbridge ER, Morgan D, Trowbridge MJ, DeLancey JOL, Fenner DE (2006) Sexual function, quality of life, and severity of anal incontinence after anal sphincteroplasty. Am J Obstet Gynecol 195:1753–7
Malouf AJ, Chambers MG, Kamm MA (2001) Clinic and economic evaluation of surgical treatments for faecal incontinence. Br J Surg 88:1029–36
Halverson AL, Hull TL (2002) Long-term outcome of overlapping anal sphincter repair. Dis Colon Rectum 45:3451–8
Norton C, Chelvanayagam S, Wilson-Barnett J, Redfern S, Kamm MA (2003) Randomized controlled trial of biofeedback for fecal incontinence. Gastroenterology 125:1320–9
Scarlett Y (2004) Gastroenterology 126(Suppl 1):S55–63
Nelson R, Furner S, Jesudason V (1998) Fecal incontinence in Wisconsin nursing homes. Dis Colon Rectum 41:1226–9
Chassagne P, Landrin I, Neveu C, Czernichow P, Bouaniche M, Doucet J et al (1999) Fecal incontinence in the institutionalized elderly: Incidence, risk factors, and prognosis. Am J Med 196:185–90
Boreham MK, Richter HE, Kenton KS, Nager CW, Gregory WT, Aronson MP et al (2005) Anal incontinence in women presenting for gynecologic care: Prevalence, risk factors, and impact upon quality of life. Am J Obstet Gynecol 192:1637–42
Longstreth GF, Thompson WG, Chey WD, Houghton LA, Mearin F, Spiller RC (2006) Functional bowel disorders. Gastroenterology 130:1480–91
Vaizey CJ, Carapeti E, Cahill JA, Kamm MA (1999) Prospective comparison of fecal incontinence. Gut 44:77–80
Barber MD, Walters MD, Bump RC (2005) Short forms of two condition-specific quality-of-life questionnaire for women with pelvic floor disorders (PFDI-20 and PFIQ-7). Am J Obstet Gynecol 193:103–13
Bharucha A, Wald A, Enck P, Rao S (2006) Functional anorectal disorders. Gastroenterology 130:1510–8
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sze, E.H.M., Barker, C.D. & Hobbs, G. A cross-sectional survey of the relationship between fecal incontinence and constipation. Int Urogynecol J 24, 61–65 (2013). https://doi.org/10.1007/s00192-012-1851-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1851-7