Abstract
The incontinence severity index (ISI) consists of two questions, regarding frequency and amount of leakage. It categorizes urinary incontinence (UI) into slight, moderate, severe, and very severe. The purpose of this study was to test its validity. The index was compared with the results of pad-weighing tests performed by 200 incontinent women referred to a hospital clinic and 103 at a primary care incontinence clinic. Inconvenience was scored by a six-level Likert scale. Mean pad-weighing results (grams per 24 hours, 95% confidence intervals) were 7 (4–10) for slight, 39 (26–51) for moderate, 102 (75–128) for severe, and 200 (131–268) for very severe UI. Spearman’s correlation coefficient for pad-weighing results and severity index was 0.58 (p<0.01), and inconvenience increased significantly with increasing severity. The ISI demonstrated good criterion validity against 24-h pad tests. Good construct validity was indicated by a clear link between ISI and inconvenience.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Many authors have investigated the prevalence of female urinary incontinence (UI), often with widely differing prevalence estimates, even when seemingly comparable settings and age groups have been studied [1]. Some studies have included large numbers of women with only slight leakage, who would probably object to being labeled incontinent. The 2nd International Consultation on Incontinence recommended development of standardized instruments for epidemiological research, including a screening question, frequency measure, quantity of urine loss, duration, type, and severity [1].
The incontinence severity index (ISI) was developed for use in epidemiological surveys to identify women with different severity of urinary leakage. It consists of two questions, regarding frequency (four levels) and amount (three levels) of leakage (Table 1). The ISI has been validated against pad tests in several studies [2–4]. Due to limited power, the first study was only able to validate a simplified three-level version of the ISI [2]. In a second study, more women were included, and we were able to show that the full four-level index was just as valid [3]. We recommend using the four-level index since it also gives a more balanced distribution in clinical materials.
The ISI has also been validated by a Scottish group who demonstrated that its reliability and responsiveness were also good [4]. Over the years, the ISI has been used in many different studies of UI, both epidemiological [5–10] and clinical [11–16], and it has received the highest recommendation from the 2nd and 3rd International Consultation on Incontinence [17, 18].
Maximum utility of the ISI requires that it can demonstrate validity in different countries and different clinical settings (primary and secondary care). The purpose of this study was to test its validity in a Spanish sample.
Materials and methods
The ISI was translated from English to Spanish and from Norwegian to Spanish by two independent translators who thereafter agreed upon the final version of the questionnaire.
The study was conducted in 2004 among 200 incontinent women referred to the urogynecology unit at the Hospital Clínic, University of Barcelona, and among 103 incontinent women referred to a primary care incontinence clinic. Patients with stage III and IV prolapse were excluded from the study.
All the women were asked to perform a pad test at home [19–21]. They were instructed to wear preweighed pads day and night during a 24-h period. Each pad was packed in a bag marked with the patient’s details and the dry weight of the pad. The women changed pads when required, putting used pads back into their bags. The pads were returned to the clinic for reweighing, and the weight gain was noted.
Before performing the pad test, all the women were categorized via the ISI. They were asked how often they experienced urinary leakage and how much urine they usually lost each time. Frequency (four levels) was multiplied by the amount of leakage (three levels). The resulting index values (1–12) were further categorized into slight, moderate, severe, and very severe (Table 1).
A patient was considered to have stress incontinence if she answered affirmatively to the question: “Do you have urine leakage when you cough, sneeze, make an effort or do physical exercise?” Likewise, she was considered to have urge incontinence if she answered affirmatively to the question: “Do you have urine leakage when you have a sudden feeling of wanting to pass water and you can’t hang on long enough?” If she answered affirmatively to both questions, she was considered to have mixed incontinence.
Patients attending the hospital clinic were also subjected to urodynamic evaluation, and they were asked how much they were inconvenienced by their incontinence symptoms: “In the past month (30 days), when you have experienced UI symptoms, how much did they inconvenience you?” They were made to choose among six answers, scored from 1 to 6 (not at all, slightly, somewhat, moderately, very much, and extremely).
Results of the pad tests (grams per 24 hours) are presented as means with 95% confidence interval (CI) and medians. t tests were used when comparing means, whereas chi-square tests were used when comparing proportions. Spearman’s correlation coefficients (R) were calculated when comparing pad tests with inconvenience score and severity index. Statistical significance was accepted at the 5% level (p<0.05).
Results
Mean age of the women was 58 years (median 58, range 27–85), with no difference between hospital and primary care. Also, the distribution of different types of incontinence did not differ between hospital and primary care, but severity was greater in hospital when measured by the severity index (p<0.05; Table 2). When measured by pad tests, however, the difference between hospital and primary care was not significant. The mean result of the pad tests was 78 g/24 h (95% CI 63–92, median 22, range 0–987). Five (2%) of the pad tests showed no weight gain.
The older half of the women (59 years and above) leaked more than the younger ones (100 vs 52 g/24 h, p<0.001). Nevertheless, older women were not more inconvenienced by their incontinence than the younger ones (inconvenience score 4.0 vs 4.4). Reported inconvenience increased significantly with increasing severity of leakage when measured by the severity index (Fig. 1). Inconvenience also correlated significantly with the pad tests (R=0.49, p<0.01).
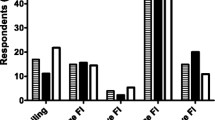
The severity index correlated significantly with the pad tests (R=0.58, p<0.01). Results of the pad tests according to reported amount and frequency of leakage as well as severity index are shown in Table 3. None of the differences between primary care and hospital was significant. Separate analyses of pad tests at different ISI levels were also carried out for stress, urge, and mixed incontinence (Fig. 2).
Discussion
In this Spanish sample, the ISI clearly demonstrated good criterion validity against 24-h pad tests, like previously shown in Norway and Scotland [2–4]. Given the simplicity of the ISI, it would have been surprising if a Spanish version would behave differently. However, health measurement scales should always be tested for validity after having been translated into a new language. An additional strength of the present study is the fact that the validity was equally good in primary care and hospital. Although impaired by wide CIs, validity was also demonstrated for different types of incontinence. In addition, good construct validity was indicated by the clear link between ISI and inconvenience, also in line with previous studies [2].
Although the ISI demonstrated good validity in defining groups with different severity, there was considerable overlap in the range of pad test results between the four severity groups. This means that although the ISI is valid for clinical and epidemiological research, it should not be regarded as a substitute for pad-weighing tests in individual cases.
A pad test is not, however, a perfect “gold standard” for measuring UI severity, but a 24-h test correlates well with symptoms of incontinence and has good reproducibility [20]. However, Lose et al. [22] found the reproducibility of the 24-h test insufficiently satisfactory to recommend its use in comparative scientific studies. Increasing test duration to 48 or 72 h slightly increases reliability but decreases patient compliance [19, 21]. The 24-h pad test is considered to be positive if the pad weight gain is ≥4 g/24 h [20].
Recently, the 1-h pad-test definitions for mild, moderate, and severe incontinence were used to categorize the 24-h test values in a similar way. This revealed that moderate incontinence ranged from 21 to 74 g/24 h, with mild and severe incontinence below and above this range, respectively [23]. These results correspond well with our findings.
In the present study, the women defined as slightly incontinent had a mean pad weight gain of 7 g/24 h, compared with 6 g/24 h in a similar Norwegian study [3]. However, the mean pad weight gain in the total sample was 78 g/24 h, as opposed to only 39 g/24 h in the Norwegian study. This can at least partly be explained by the fact that there were more women with severe and very severe incontinence in the Spanish sample. The Spanish women were older than the Norwegians, and it is well known that the severity of incontinence increases with advancing age [1, 2, 5].
This tendency toward more severe incontinence may also explain why the mean pad weight gain is higher in the ISI category very severe in the Spanish sample. However, it cannot explain why the pad weight gain in Spain is also higher in the ISI categories moderate and severe. Since differences between mean test results in large groups cannot be explained by low reproducibility of the test, there may have been systematic differences in how the pad tests have been performed in Norway and Spain. In the Norwegian sample, 48-h tests were used (although results were given per 24 hours), and it is known that increasing the length of test periods may decrease patient compliance [21]. There were more completely negative tests in the Norwegian sample (8%), possibly an indication of lower compliance [3].
So far, only one study has looked into the reliability and responsiveness of the ISI. Hanley et al. [4] found that 88% of the incontinent women recorded the same (three-level) ISI category 3 days apart (κ=0.78). Furthermore, 60% moved to a lower ISI category after treatment. In the future, it is important to repeat these analyses in different settings, and it is our intention to do so in this Spanish sample.
References
Hunskaar S, Burgio K, Diokno A, Herzog AR, Hjalmas K, Lapitan MC (2002) Epidemiology and natural history of urinary incontinence. In: Abrams P, Cardozo L, Khoury S, Wein A (eds) Incontinence: 2nd International Consultation on Incontinence. Health Publication Ltd., Plymouth, UK, pp 165–201
Sandvik H, Hunskaar S, Seim A, Hermstad R, Vanvik A, Bratt H (1993) Validation of a severity index in female urinary incontinence and its implementation in an epidemiological survey. J Epidemiol Community Health 47:497–499
Sandvik H, Seim A, Vanvik A, Hunskaar S (2000) A severity index for epidemiological surveys of female urinary incontinence: comparison with 48-hour pad-weighing tests. Neurourol Urodyn 19:137–145
Hanley J, Capewell A, Hagen S (2001) Validity study of the severity index, a simple measure of urinary incontinence in women. BMJ 322:1096–1097
Hannestad YS, Rortveit G, Sandvik H, Hunskaar S (2000) A community-based epidemiological survey of female urinary incontinence: the Norwegian EPINCONT study. Epidemiology of incontinence in the county of Nord-Trondelag. J Clin Epidemiol 53:1150–1157
Yu HJ, Wong WY, Chen J, Chie WC (2003) Quality of life impact and treatment seeking of Chinese women with urinary incontinence. Qual Life Res 12:327–333
Rortveit G, Daltveit AK, Hannestad YS, Hunskaar S (2003) Urinary incontinence after vaginal delivery or cesarean section. N Engl J Med 348:900–907
Hannestad YS, Lie RT, Rortveit G, Hunskaar S (2004) Familial risk of urinary incontinence in women: population based cross sectional study. BMJ 329:889–891
Hägglund D, Walker-Engström ML, Larsson G, Leppert J (2003) Reasons why women with long-term urinary incontinence do not seek professional help: a cross-sectional population-based cohort study. Int Urogynecol J 14:296–304
Iglesias FJG, Ocerin JMCY, Martin JPDM, Gama EV, Perez ML, Lopez MR, Aranguren MVP, Munoz JBG (2000) Prevalence and psychosocial impact of urinary incontinence in older people of a Spanish rural population. J Gerontol 55A:M207–214
Seim A, Sivertsen B, Eriksen BC, Hunskaar S (1996) Treatment of urinary incontinence in women in general practice: observational study. BMJ 312:1459–1462
Indrekvam S, Sandvik H, Hunskaar S (2001) A Norwegian national cohort of 3198 women treated with home-managed electrical stimulation for urinary incontinence—effectiveness and treatment results. Scand J Urol Nephrol 35:32–39
Arya LA, Jackson ND, Myers DL, Verma A (2001) Risk of new-onset urinary incontinence after forceps and vacuum delivery in primiparous women. Am J Obstet Gynecol 185:1318–1323
Kerschan-Schindl K, Uher E, Wiesinger G, Kaider A, Ebenbichler G, Nicolakis P, Kollmitzer J, Preisinger E, Fialka-Moser V (2002) Reliability of pelvic floor muscle strength measurement in elderly incontinent women. Neurourol Urodyn 21:42–47
Chiarelli P, Cockburn J (2002) Promoting urinary continence in women after delivery: randomised controlled trial. BMJ 324:1241
Melville JL, Miller EA, Fialkow MF, Lentz GM, Miller JL, Fenner DE (2003) Relationship between patient report and physician assessment of urinary incontinence severity. Am J Obstet Gynecol 189:76–80
Donovan JL, Badia X, Corcos J, Gotoh M, Kelleher C, Naughton M, Shaw C, Lukacs B (2002) Symptom and quality of life assessment. In: Abrams P, Cardozo L, Khoury S, Wein A (eds) Incontinence: 2nd International Consultation on Incontinence. Health Publication Ltd., Plymouth, UK, pp 267–316
Donovan JL, Ruud Bosch JLH, Gotoh M, Jackson S, Naughton M, Radley S, Valiquette L (2005) Symptom and quality of life assessment. In: Abrams P, Cardozo L, Khoury S, Wein A (eds) Incontinence: 3rd International Consultation on Incontinence. Health Publication Ltd., Plymouth, UK, pp 519–584
Versi E, Orrego G, Hardy E, Seddon G, Smith P, Anand D (1996) Evaluation of the home pad test in the investigation of female urinary incontinence. Br J Obstet Gynaecol 103:162–167
Artibani W, Andersen JT, Gajewski JB, Ostergard DR, Raz S, Tubaro A, Khullar V, Klarskov P, Rodriguez L (2002) Imaging and other investigations. In: Abrams P, Cardozo L, Khoury S, Wein A (eds) Incontinence: 2nd International Consultation on Incontinence. Health Publication Ltd., Plymouth, UK, pp 425–477
Groutz A, Blaivas JG, Chaikin DC, Resnick NM, Engleman K, Anzalone D, Bryzinski B, Wein AJ (2000) Noninvasive outcome measures of urinary incontinence and lower urinary tract symptoms: a multicenter study of micturition diary and pad tests. J Urol 164:698–701
Lose G, Jorgensen L, Thunedborg P (1989) 24-hour home pad weighing test versus 1-hour ward test in the assessment of mild stress incontinence. Acta Obstet Gynecol Scand 68:211–215
O’Sullivan R, Karantanis E, Stevermuer TL, Allen W, Moore KH (2004) Definition of mild, moderate and severe incontinence on the 24-hour pad test. Br J Obstet Gynaecol 111:859–862
Acknowledgement
The study was supported by a research grant from Eli Lilly Spain to the Fundacion Clinic for Biomedical Research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sandvik, H., Espuna, M. & Hunskaar, S. Validity of the incontinence severity index: comparison with pad-weighing tests. Int Urogynecol J 17, 520–524 (2006). https://doi.org/10.1007/s00192-005-0060-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-005-0060-z