Abstract
Purpose
Many studies have demonstrated that injection of various growth factors including platelet-derived growth factor could increase meniscal cell activity and stimulate repair. The purpose of this study was to augment repair and promote meniscal healing by the use of platelet-rich plasma (PRP) within horizontal cleavage meniscal tears repaired via an open approach. The hypothesis was that the clinical outcomes and healing process would be improved using this meniscal healing augmentation technique.
Methods
In this case–control study, 34 consecutive young patients underwent an open meniscal repair to treat symptomatic Grade 2 or Grade 3 horizontal meniscal tears [median age 28 years (13–40)]. The median time between the onset of symptoms and surgery was 11.5 months (6–50). In the first group (17 consecutive patients, Group 1), a standard open meniscal repair was performed. In the second group (17 consecutive patients, Group 2), the same surgical repair was performed, but platelet-rich plasma was introduced into the lesion at the end of the procedure. Clinical outcomes were evaluated using KOOS and IKDC 2000 scores. MRI was performed at 1 year after surgery for objective evaluation.
Results
At a minimum of 24 months postoperatively (mean 32.2 months, 24–40), three patients underwent subsequent meniscectomy (two in Group 1, one in Group 2). The mean KOOS distribution (pain, symptoms, daily activities, sports, quality of life) was 78.4, 86.1, 93.8, 74.4, 74.6 in Group 1, and 93.3, 90.7, 97.1, 88.8, 78.3 in Group 2 (p < 0.05 for pain and sports parameters). MRI revealed five cases with the complete disappearance of any hypersignal within the repaired meniscus in Group 2, and none in Group 1 (p < 0.01).
Conclusions
Open meniscal repair of horizontal tears extending into the avascular zone was effective at midterm follow-up in young patients. Clinical outcomes were slightly improved by the addition of PRP in this case–control study.
Level of evidence
III.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Meniscal healing occurs following two distinct patterns related to the location of the lesion. In lesions occurring in the vascular area, the blood supplies undifferentiated mesenchymal cells with nutrients thought to induce healing [5]. In lesions occurring in the avascular zone, the healing process is mainly based on the self-repair capacity of the meniscal tissue [2, 22].
Symptomatic horizontal meniscal lesions occurring in young patients are often extensive and located both in the vascular and avascular zone [7]. A meniscectomy of such lesions would be a subtotal meniscectomy. This is unacceptable in young patients, unless the lesion is irreparable, because of the risk of deterioration and flattening of the articular cartilage surfaces and subchondral bone sclerosis with time [31]. In a population of young patients with horizontal meniscal lesions, meniscal repair should be first considered even though potential healing of such lesions is questionable [30]. In these cases, biological factors may be needed to promote the biological response.
Platelet-rich plasma (PRP) has been widely used for treating tendinous, muscle, ligament and chondral problems, but its efficacy is a matter of controversy [14, 25]. Many in vitro or animal studies have demonstrated that injection of various growth factors including platelet-derived growth factor could increase meniscal cell activity and stimulate repair [6, 18, 49].
However, little is known about the clinical outcomes of repaired meniscal tissue with PRP augmentation. Literature review puts in evidence numerous publications discussing the theoretical benefit without clinical proof [9, 29, 37, 43]. So, there is need for clinical evidence of the healing enhancement effect of PRP on a repaired meniscus.
The purpose of this study was to augment repair and promote meniscal healing by the use of PRP within horizontal cleavage meniscal tears repaired via an open approach. The hypothesis was that the clinical outcomes and healing process would be improved using this meniscal healing augmentation technique.
Materials and methods
Thirty-seven consecutive patients underwent an open repair to treat a symptomatic horizontal cleavage of the meniscus between January 2009 and June 2012 at our hospital. The inclusion criteria for this study were patients younger than 40 years with a symptomatic horizontal cleavage (Grade II or III) of the meniscus [11] and persisting pain after complete medical treatment (rest, physiotherapy, intraarticular injections of corticosteroids) for at least 6 months.
The exclusion criteria were as follows: surgery of the knee for concurrent injuries, loss of cartilage (Outerbridge >2), ACL injury, PCL injury and collateral ligament injuries. Three patients were excluded due to severe concomitant chondral injuries, leaving thirty-four patients included in the study.
The first 17 patients (Group 1) had an isolated open meniscal repair. The last 17 patients (Group 2) had an open meniscal repair and an in situ injection of PRP. Preoperative data for the two groups are presented in Table 1. There were no patients insured through workers compensation. There were no differences between groups.
Operative technique
The same surgical procedure was used for all patients.
Anteromedial and anterolateral portals were created, and a diagnostic arthroscopy was performed. The meniscal tear was identified in cases of Grade 3 lesions. In the case of Grade 2 lesions, no lesion was identified during arthroscopy. If present in Grade 3 lesions, unstable meniscal fragments and fibrous tissue were removed using a motorized shaver or basket forceps. To repair the medial meniscal tear, a posteromedial mini-arthrotomy was performed. To repair the lateral meniscal tear, a posterolateral mini-arthrotomy was performed. The capsule was open on the upper side of the meniscus, and the meniscosynovial junction was detached vertically in order to create access to the horizontal cleavage. The lesion was abraded with a rasp and a curette. Meniscal repair was performed by vertical sutures with type N°0 polydioxamone (PDS; Ethicon, Somerville, NJ, USA), in order to close the two layers (Fig. 1). The capsule was then closed. In Group 2 (PRP), 5 ml of PRP was obtained using the GPS®III system (Biomet, Warsaw, Indiana, USA) and injected directly into the repaired lesion before the closure of the wound (Fig. 2). No drainage was used.
All patients followed the same rehabilitation protocol. In the first week postoperatively, a passive range of motion from 0° to 90° was initiated, allowing partial weight-bearing for 4 weeks. For the first 4 weeks, a hinged knee brace locked in full extension was used. Jogging was not permitted until 3 months postoperatively. Return to pivoting sports was allowed 6–7 months after surgery.
Clinical assessment
Clinical outcome was assessed using the 2000 IKDC Knee Examination Score. The KOOS and the subjective IKDC scores were implemented to assess patient-oriented outcomes. Clinical evaluation using the IKDC and KOOS scores was performed at a minimum of 24 months after surgery. Clinical failure was defined by a reoperation on the same knee for a meniscectomy or an iterative repair of the same meniscus.
Follow-up MRI
MRI was performed 1 year after surgery. These conventional MRI scans were obtained on a 1.5-Tesla MRI scanner (Symphony, Siemens Medical Solutions, Erlangen, Germany). The signal intensity within the repaired meniscal area was evaluated (T2 fatsat). For MRI assessment, we described a new classification of the horizontal features of the repaired meniscus included the following: no hypersignal (Type I), low- or intermediate-intensity hypersignal in the white-white zone without hypersignal in the red-red zone (Type II), high-intensity hypersignal (red-red and white-white zones, Type III). The MRI was interpreted by an orthopaedic surgeon who did not participate in the surgery and who was blinded to the treatment received by the patient (PRP or no PRP). In type III, the hypersignal in the repaired meniscus was as high as the hypersignal in the preoperative lesion. In type II, there was a less intense remaining signal when compared to the preoperative lesion.
This study was approved by the institutional review board of the hospital and by the scientific committee of the A. Mignot Hospital in Versailles. This study was performed in accordance with the ethical standards outlined in the 1964 Declaration of Helsinki. All patients signed a written informed consent explaining the potential benefit of PRP, surgical procedure and follow-up. No patients declined to participate in this study.
Statistical analysis
The SSPS 13.0 Software was used for data processing. Pre- and postoperative quantitative variables were compared by the coefficient of correlation. Independent samples (t test and Mann–WhitneyU test) were used for group comparison. In all analyses, p values less than 0.05 were considered statistically significant. Post hoc power analysis was performed using G*Power version 3.1.9.2.
Results
The median follow-up period was 34 months (range 24–40 months) in Group 1 and 30 months (range 24–36 months) in Group 2.
In Group 1, the median active flexion was 130° (range 120–145). There were no extension lag signs. The objective IKDC score was grade A in nine patients, B in five, and C in two.
In Group 2, the median active flexion was 135° (range 120–145). There were no extension lag signs. The objective IKDC score was grade A in 10 patients, B in six, and C in one.
The median IKDC score was 87.9 (range 44–99) in Group 1 and 90.7 (range 48–100) in Group 2 (ns).
The mean KOOS distribution is shown in Fig. 3. The difference between groups was significant for pain and sports activities parameters (p = 0.046 and 0.03, respectively). There were no differences between the other subscales of the KOOS.
Topography, presence or absence of a cyst, and preoperative MRI grade were all shown to have no significant influence on the clinical outcome at final follow-up in either group.
In Group 1, two symptomatic patients with an unhealed medial meniscus underwent partial meniscectomy 12 and 18 months after surgery. In Group 2, one patient underwent a subtotal medial meniscectomy 12 months after initial surgery. The failure rate was 11.8 and 5.8 % in Group 1 and Group 2, respectively.
One patient in Group 1 had a local haematoma requiring surgical drainage.
One patient in Group 2 had a septic arthritis 1 month after the procedure, requiring arthroscopic lavage of the joint and oral antibiotics for 45 days. When initially present, there was no recurrence of a cyst in either group (Fig. 4).
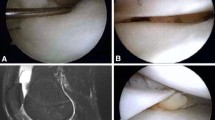
MRI interpretations of meniscal healing after surgery are shown in Table 2. The three types of MRI features of the repaired menisci are presented in Figs. 5a, b, 6a, b and 7a, b. There was a statistically significant difference in the healing appearance of repaired menisci by MRI evaluation between the two groups (p < 0.01). Nevertheless, there was no correlation between the postoperative signal in the repaired meniscus and the clinical outcomes (KOOS, IKDC).
Post hoc power analysis for pain, sports parameters of the KOOS and for MRI signal (effect size 0.88, 0.69, 0.91, respectively; α = 0.05) resulted in 0.81, 0.63, 0.83 (1−β err prob), respectively.
Discussion
The most important finding of this study is that PRP slightly improved clinical outcomes after open repair for horizontal cleavage.
The global failure rate (subsequent meniscectomy) was low in both groups, despite the extension of the lesion into the avascular zone. This is consistent with the results of meniscal repair for traumatic vertical lesions [26, 30, 36]. In systematic literature reviews, the mean rate of failure after meniscal repair of vertical lesions with all-inside repair devices was 15–19 % [15, 26]. There are few reports about the surgical treatment of horizontal meniscal cleavages [8, 20, 33]. Their incidence is relatively low, when compared to vertical lesions. Kurzweil et al. published recently a literature review about meniscal repair of horizontal meniscus tears. Among nine eligible articles (a total of 98 repairs), the overall success rate without subsequent surgery was 77.8 % [24].
These lesions should be differentiated from so-called degenerative horizontal lesions occurring typically after the age of 50 in patients with cartilage damage, meniscal extrusion or even advanced osteoarthritis [19, 21, 42]. In our cases, there was neither subchondral bone oedema, significant cartilage loss, nor meniscal extrusion on preoperative MRI, and all patients were under 40 with a failed medical treatment of at least 6 months.
Biedert was the first to describe four different treatments for such lesions (no operative treatment, partial meniscectomy, trephination, meniscal repair) [8]. We have previously reported a retrospective series of 30 cases operated on using the same surgical technique (open meniscal repair) and a mean follow-up of 4 years [33]. The clinical outcomes were good (median subjective IKDC score at 89 ± 14, 15 % reoperation rate). The functional results decreased significantly with age after 30. No postoperative imaging (MRI) was available.
The magnetic resonance imaging of the postoperative repaired meniscus is difficult to interpret [46]. A persisting hypersignal is frequent (>60 % of cases), even 10 years after open [28] or arthroscopic meniscal repair [34], even in the vascularised zones.
In our series, MRI at 2 years showed a persisting hypersignal in 84 % cases in the avascular zone. The intensity of the signal was lower than in preoperative imaging in all cases. Such a signal may reflect either immature fibrovascular granulation tissue or mature fibrocartilaginous scar tissue at the repair site. In the vascularised zone (outer third of the meniscus), the hypersignal was still present on MRI in 60 % of cases in Group 1 and in 25 % in Group 2. This difference was significant. These MRI features were not surprising, because the presented surgical technique allows the suture of the outer third of the meniscus, by an open approach. In the avascular zone, the cleavage was left in situ. Even when the signal was still present on postoperative MRI, it did not appear to have any clinical consequences. For example, Zanetti et al. [48] did bilateral MRI of the knees of 100 patients with clinical symptoms of unilateral meniscal lesion. He found a meniscal lesion in 36 % of the contralateral asymptomatic knees. Healing of the meniscocapsular junction with strong vertical sutures may be the most important factor in order to achieve durable pain relief in such horizontal meniscal lesions.
Tears extending into the avascular zone of the meniscus are generally complex and broad and are often associated with a poor prognosis following repair.
Once torn, the meniscus, because of its low cellularity and spontaneous healing response, is unable to fully repair itself in the avascular zone [35].
Several different therapeutic approaches have been proposed, with a variety of reported results. The most notable of these approaches are the following: the use of parameniscal synovial tissue or collagen matrix [27, 32], trephination of the peripheral meniscus rim with suture of the meniscus tear [50], creation of vascular access channels, use of fibrin clot [3, 4, 16, 20, 39] and fibrin glue [38].
The use of PRP remains controversial in orthopaedics [40]. A number of randomised clinical trials have reported limited or no clinical efficacy for pathologies including patellar tendon healing [12], lateral epicondylitis [23], Achilles tendinopathy [13] and rotator cuff tears [10]. To our knowledge, there are no randomised or even comparative studies evaluating the use of PRP to augment meniscus repair [1].
Nevertheless, many in vitro studies have demonstrated that injection of various growth factors could stimulate repair of the meniscus tissue [37]. Platelet-derived growth factor (PDGF) has mostly been evaluated in sheep menisci. Following the use of PDGF, cell proliferation and migration and extracellular collagen matrix formation were increased in torn meniscus zones when compared to the control [17, 41, 44, 45], even in white-white zones [47]. The main difficulty when assessing the efficacy of PRP on meniscal healing after arthroscopic repair is accessed to the lesions located in the posterior segments of the meniscus and the risk of dilution of the PRP in the joint under arthroscopy. In this case–control series, the open approach allowed us to place the PRP precisely into the repaired lesion of the meniscus.
There are some limitations in this study. The number of cases is low; therefore, it involves a consecutive series of patients without randomisation. The observed differences between groups might have been statistically different with higher power. Patients were not blinded.
The strengths are the case–control design with two consecutive series of comparable patients. Finally, we did not lose any patients during follow-up. The clinical relevance of this could be that PRP might improve outcomes and enhance healing process when injected directly into the lesion (open approach) without any risk of dilution (arthroscopy).
Conclusion
Open meniscus repair of horizontal tears extending into the avascular zone was effective at midterm follow-up in young patients. Clinical outcomes were slightly improved by the addition of PRP in this case–control study. Although encouraging, no recommendation can be made. This technique should be further evaluated in larger studies with a longer follow-up.
References
Arnoczky SP, Sheibani-Rad S (2013) The basic science of platelet-rich plasma (PRP): what clinicians need to know. Sports Med Arthrosc 21:180–185
Arnoczky SP, Warren RF (1983) The microvasculature of the meniscus and its response to injury. An experimental study in the dog. Am J Sports Med 11:131–141
Arnoczky SP, Warren RF, Spivak JM (1988) Meniscal repair using an exogenous fibrin clot. An experimental study in dogs. J Bone Joint Surg Am 70:1209–1217
Barwad P, Ramakrishnan S, Kothari SS, Saxena A, Gupta SK, Juneja R, Gulati GS, Jagia P, Sharma S (2013) Amplatzer vascular plugs in congenital cardiovascular malformations. Ann Pediatr Cardiol 6:132–140
Becker R, Pufe T, Kulow S, Giessmann N, Neumann W, Mentlein R, Petersen W (2004) Expression of vascular endothelial growth factor during healing of the meniscus in a rabbit model. J Bone Joint Surg Br 86:1082–1087
Bhargava MM, Hidaka C, Hannafin JA, Doty S, Warren RF (2005) Effects of hepatocyte growth factor and platelet-derived growth factor on the repair of meniscal defects in vitro. In Vitro Cell Dev Biol Anim 41:305–310
Biedert RM (1993) Intrasubstance meniscal tears. Clinical aspects and the role of MRI. Arch Orthop Trauma Surg 112:142–147
Biedert RM (2000) Treatment of intrasubstance meniscal lesions: a randomized prospective study of four different methods. Knee Surg Sports Traumatol Arthrosc 8:104–108
Braun HJ, Wasterlain AS, Dragoo JL (2013) The use of PRP in ligament and meniscal healing. Sports Med Arthrosc 21:206–212
Cheung EV, Silverio L, Sperling JW (2010) Strategies in biologic augmentation of rotator cuff repair: a review. Clin Orthop Relat Res 468:1476–1484
Crues JV 3rd, Mink J, Levy TL, Lotysch M, Stoller DW (1987) Meniscal tears of the knee: accuracy of MR imaging. Radiology 164:445–448
de Almeida AM, Demange MK, Sobrado MF, Rodrigues MB, Pedrinelli A, Hernandez AJ (2012) Patellar tendon healing with platelet-rich plasma: a prospective randomized controlled trial. Am J Sports Med 40:1282–1288
de Vos RJ, Weir A, van Schie HT, Bierma-Zeinstra SM, Verhaar JA, Weinans H, Tol JL (2010) Platelet-rich plasma injection for chronic Achilles tendinopathy: a randomized controlled trial. JAMA 303:144–149
Foster TE, Puskas BL, Mandelbaum BR, Gerhardt MB, Rodeo SA (2009) Platelet-rich plasma: from basic science to clinical applications. Am J Sports Med 37:2259–2272
Grant JA, Wilde J, Miller BS, Bedi A (2012) Comparison of inside-out and all-inside techniques for the repair of isolated meniscal tears: a systematic review. Am J Sports Med 40:459–468
Henning CE, Yearout KM, Vequist SW, Stallbaumer RJ, Decker KA (1991) Use of the fascia sheath coverage and exogenous fibrin clot in the treatment of complex meniscal tears. Am J Sports Med 19:626–631
Ionescu LC, Lee GC, Huang KL, Mauck RL (2012) Growth factor supplementation improves native and engineered meniscus repair in vitro. Acta Biomater 8:3687–3694
Ishida K, Kuroda R, Miwa M, Tabata Y, Hokugo A, Kawamoto T, Sasaki K, Doita M, Kurosaka M (2007) The regenerative effects of platelet-rich plasma on meniscal cells in vitro and its in vivo application with biodegradable gelatin hydrogel. Tissue Eng 13:1103–1112
Jarvinen TL, Sihvonen R, Malmivaara A (2014) Arthroscopic partial meniscectomy for degenerative meniscal tear. N Engl J Med 370:1260–1261
Kamimura T, Kimura M (2011) Repair of horizontal meniscal cleavage tears with exogenous fibrin clots. Knee Surg Sports Traumatol Arthrosc 19:1154–1157
Kijowski R, Woods MA, McGuine TA, Wilson JJ, Graf BK, De Smet AA (2011) Arthroscopic partial meniscectomy: MR imaging for prediction of outcome in middle-aged and elderly patients. Radiology 259:203–212
Kobayashi K, Fujimoto E, Deie M, Sumen Y, Ikuta Y, Ochi M (2004) Regional differences in the healing potential of the meniscus-an organ culture model to eliminate the influence of microvasculature and the synovium. Knee 11:271–278
Krogh TP, Fredberg U, Stengaard-Pedersen K, Christensen R, Jensen P, Ellingsen T (2013) Treatment of lateral epicondylitis with platelet-rich plasma, glucocorticoid, or saline: a randomized, double-blind, placebo-controlled trial. Am J Sports Med 41:625–635
Kurzweil PR, Lynch NM, Coleman S, Kearney B (2014) Repair of horizontal meniscus tears: a systematic review. Arthroscopy. doi:10.1016/j.arthro.2014.05.038
Lopez-Vidriero E, Goulding KA, Simon DA, Sanchez M, Johnson DH (2010) The use of platelet-rich plasma in arthroscopy and sports medicine: optimizing the healing environment. Arthroscopy 26:269–278
Lozano J, Ma CB, Cannon WD (2007) All-inside meniscus repair: a systematic review. Clin Orthop Relat Res 455:134–141
Moriguchi Y, Tateishi K, Ando W, Shimomura K, Yonetani Y, Tanaka Y, Kita K, Hart DA, Gobbi A, Shino K, Yoshikawa H, Nakamura N (2013) Repair of meniscal lesions using a scaffold-free tissue-engineered construct derived from allogenic synovial MSCs in a miniature swine model. Biomaterials 34:2185–2193
Muellner T, Egkher A, Nikolic A, Funovics M, Metz V (1999) Open meniscal repair: clinical and magnetic resonance imaging findings after twelve years. Am J Sports Med 27:16–20
Nourissat G, Mainard D, Kelberine F, French Arthroscopic Society (SFA) (2013) Current concept for the use of PRP in arthroscopic surgery. Orthop Traumatol Surg Res 99(8 Suppl):S407–S410
Noyes FR, Barber-Westin SD (2002) Arthroscopic repair of meniscal tears extending into the avascular zone in patients younger than twenty years of age. Am J Sports Med 30:589–600
Noyes FR, Barber-Westin SD (2012) Management of meniscus tears that extend into the avascular region. Clin Sports Med 31:65–90
Piontek T, Ciemniewska-Gorzela K, Szulc A, Slomczykowski M, Jakob R (2012) All-arthroscopic technique of biological meniscal tear therapy with collagen matrix. Pol Orthop Traumatol 77:39–45
Pujol N, Bohu Y, Boisrenoult P, Macdes A, Beaufils P (2013) Clinical outcomes of open meniscal repair of horizontal meniscal tears in young patients. Knee Surg Sports Traumatol Arthrosc 21:1530–1533
Pujol N, Tardy N, Boisrenoult P, Beaufils P (2013) Magnetic resonance imaging is not suitable for interpretation of meniscal status ten years after arthroscopic repair. Int Orthop 37:2371–2376
Rodkey WG (2000) Basic biology of the meniscus and response to injury. Instr Course Lect 49:189–193
Rubman MH, Noyes FR, Barber-Westin SD (1998) Arthroscopic repair of meniscal tears that extend into the avascular zone. A review of 198 single and complex tears. Am J Sports Med 26:87–95
Scotti C, Hirschmann MT, Antinolfi P, Martin I, Peretti GM (2013) Meniscus repair and regeneration: review on current methods and research potential. Eur Cell Mater 26:150–170
Scotti C, Pozzi A, Mangiavini L, Vitari F, Boschetti F, Domeneghini C, Fraschini G, Peretti GM (2009) Healing of meniscal tissue by cellular fibrin glue: an in vivo study. Knee Surg Sports Traumatol Arthrosc 17:645–651
Sethi PM, Cooper A, Jokl P (2003) Technical tips in orthopaedics: meniscal repair with use of an in situ fibrin clot. Arthroscopy 19:E44
Sheth U, Simunovic N, Klein G, Fu F, Einhorn TA, Schemitsch E, Ayeni OR, Bhandari M (2012) Efficacy of autologous platelet-rich plasma use for orthopaedic indications: a meta-analysis. J Bone Joint Surg Am 94:298–307
Spindler KP, Mayes CE, Miller RR, Imro AK, Davidson JM (1995) Regional mitogenic response of the meniscus to platelet-derived growth factor (PDGF-AB). J Orthop Res 13:201–207
Suter LG, Fraenkel L, Losina E, Katz JN, Gomoll AH, Paltiel AD (2009) Medical decision making in patients with knee pain, meniscal tear, and osteoarthritis. Arthritis Rheum 61:1531–1538
Taylor SA, Rodeo SA (2013) Augmentation techniques for isolated meniscal tears. Curr Rev Musculoskelet Med 6:95–101
Tumia NS, Johnstone AJ (2004) Promoting the proliferative and synthetic activity of knee meniscal fibrochondrocytes using basic fibroblast growth factor in vitro. Am J Sports Med 32:915–920
Tumia NS, Johnstone AJ (2009) Platelet derived growth factor-AB enhances knee meniscal cell activity in vitro. Knee 16:73–76
Vance K, Meredick R, Schweitzer ME, Lubowitz JH (2009) Magnetic resonance imaging of the postoperative meniscus. Arthroscopy 25:522–530
Wei LC, Gao SG, Xu M, Jiang W, Tian J, Lei GH (2012) A novel hypothesis: the application of platelet-rich plasma can promote the clinical healing of white-white meniscal tears. Med Sci Monit 18:HY47–HY50
Zanetti M, Pfirrmann CW, Schmid MR, Romero J, Seifert B, Hodler J (2003) Patients with suspected meniscal tears: prevalence of abnormalities seen on MRI of 100 symptomatic and 100 contralateral asymptomatic knees. AJR Am J Roentgenol 181:635–641
Zellner J, Mueller M, Berner A, Dienstknecht T, Kujat R, Nerlich M, Hennemann B, Koller M, Prantl L, Angele M, Angele P (2010) Role of mesenchymal stem cells in tissue engineering of meniscus. J Biomed Mater Res A 94:1150–1161
Zhang Z, Arnold JA (1996) Trephination and suturing of avascular meniscal tears: a clinical study of the trephination procedure. Arthroscopy 12:726–731
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pujol, N., Salle De Chou, E., Boisrenoult, P. et al. Platelet-rich plasma for open meniscal repair in young patients: Any benefit?. Knee Surg Sports Traumatol Arthrosc 23, 51–58 (2015). https://doi.org/10.1007/s00167-014-3417-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-014-3417-3