Abstract
Purpose
Historically, the results of posterior cruciate ligament (PCL) reconstructions are not as favourable as anterior cruciate ligament (ACL) reconstructions, and it is well recognized that nonoperative treatment and postoperative rehabilitation for PCL injuries must be altered compared to those for ACL injuries. The purpose of this article was to review current peer-reviewed PCL rehabilitation programmes and to recommend a nonoperative and postoperative programme based on basic science and published outcomes studies.
Methods
To discover the current practices being used to rehabilitate PCL injuries, we conducted a search of PubMed with the terms “posterior cruciate ligament” and “rehabilitation” from 1983 to 2011. All articles within the reference lists of these articles were also examined to determine their rehabilitation programmes.
Results
A review of peer-reviewed PCL rehabilitation protocols revealed that the treatment of PCL injuries depends on the timing and degree of the injury. Rehabilitation should focus on progressive weight bearing, preventing posterior tibial subluxation and strengthening of the quadriceps muscles. General principles of proper PCL rehabilitation, whether nonoperative or postoperative, should include early immobilization (when necessary), prone passive range of motion to prevent placing undue stress on grafts or healing tissue, and progression of rehabilitation based on biomechanical, clinical, and basic science research.
Conclusions
An optimal set of guidelines for the nonoperative or postoperative management of PCL injuries has not yet been defined or agreed upon. Based on the current review study, suggested guidelines are proposed.
Level of evidence
IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Unlike the anterior cruciate ligament (ACL), the posterior cruciate ligament (PCL) has an intrinsic ability to heal and may regain continuity following an injury; however, in a PCL-deficient knee, gravity and the forces on the joint from the hamstring muscles can potentially cause the tibia to be positioned in a posteriorly subluxed location relative to the femur [17, 25, 29, 44–47, 49]. Healing of the PCL in an elongated position can lead to chronic instability and disability [46]. The use of a cylindrical cast, which applies an anterior drawer force, has demonstrated that placing the PCL in a properly reduced position, with less posterior sag, allows for improved healing [26]. Patients who have undergone surgical reconstruction of the PCL commonly report residual posterior laxity, especially following treatment of chronic tears [2, 27, 43, 54].
Numerous studies have investigated rehabilitation protocols for patients following ACL reconstruction, but unfortunately the same cannot be said for patients with a PCL injury. This is likely due to the higher incidence of ACL versus PCL injuries each year and the fact that PCL tears are less frequently operated on compared to ACL tears, resulting in more research into ACL rehabilitation protocols [16, 18]. New investigations into PCL rehabilitation protocols could potentially help to improve outcomes following PCL reconstruction and nonoperative rehabilitation.
Materials and methods
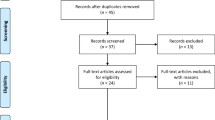
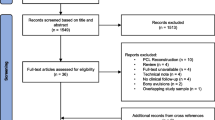
A systematic search of the literature was conducted utilizing a PubMed MEDLINE database (PubMed) keyword search with the keywords “posterior cruciate ligament” and “rehabilitation” (http://www.ncbi.nlm.nih.gov/pubmed). The articles were categorized by the degree of injury and the type of treatment employed: operative versus nonoperative. In addition, all of the articles within the reference lists of these articles were examined to determine their rehabilitation programmes and outcomes. The biomechanical properties of the PCL were also investigated through a literature search to determine the limits and characteristics that should be considered when developing an optimal PCL rehabilitation programme. The authors’ current practices and recommendations for treating and rehabilitating patients with PCL injuries were also reviewed.
Results
A search performed of the English literature in PubMed yielded 242 results when searching for “posterior cruciate ligament” and “rehabilitation”. Of the search results, 69 of the 242 articles mentioned or described aspects of rehabilitation protocols and exercises focused specifically on the treatment and rehabilitation of PCL injuries. Of these 69 articles, 33 were found to describe their PCL rehabilitation protocols and are described here. Of the 242 articles, none were outcome studies comparing different aspects of PCL rehabilitation.
Treatment/rehabilitation
The treatment of PCL injuries depends on the timing of the injury, degree of injury, the patient’s complaints, and the patient’s demands/level of activity [13, 29]. Isolated grade I and II tears (Table 1) and non-displaced PCL bony avulsions with a small fragment and grade I/II laxity should reportedly be initially treated nonoperatively [3, 17, 29]. Rehabilitation should focus on progressive weight bearing and emphasize quadriceps strengthening, while protecting the healing ligament or graft [8, 21]. The historical treatment for grade III isolated tears is an area of disagreement, but most reports note that the knee should be immobilized in extension for between 2 and 4 weeks to prevent posterior tibial subluxation and decrease tension on the anterolateral bundle of the PCL [6, 7, 14, 21, 33]. Further rehabilitation then progresses from that point, but not all patients recover and a large per cent have been reported to eventually require reconstruction of the PCL [5, 26, 47].
Rehabilitation protocols for both nonoperative and operative treatment of PCL injuries are generally divided into specific time-related and objective findings-related treatment phases. In general, phase I in both groups incorporated oedema/effusion control, knee motion within limits which have been reported to not stress the PCL, and reactivation of the quadriceps musculature, which was followed for the initial 4–6 weeks. Phase II, followed for the next 4–6 weeks, strove for regaining full knee range of motion, light low-impact strengthening activities, and avoidance of knee effusions. Further phases are progressed according to regaining strength, endurance, and agility with progressive advancement based on both functional testing and objective examination or stress radiographic outcomes.
There is a lack of quality studies investigating the effects that different rehabilitation protocols have on PCL treatment outcomes [29, 35, 55]. Rehabilitation of PCL injuries, whether following surgery or as part of a nonoperative protocol, focuses specifically on quadriceps strengthening and recovery of proprioception [21, 29, 35]. Studies have reported that patients with PCL injuries who regained greater quadriceps strength obtained better functional outcomes [40, 50]. The ultimate goal of rehabilitation protocols should be to re-establish a firm end point on the posterior drawer examination with minimal patient-reported instability. Patients should be allowed to return to sports-related activities once they have painless active range of motion and adequate return of quadriceps strength [29, 45]. Because PCL reconstructions typically do not yield as improved objective stability results compared to ACL reconstructions, it has been advocated that postoperative rehabilitation should be more conservative than ACL rehabilitation [15, 27].
Nonoperative treatment of PCL tears
An optimal set of guidelines for nonoperative management of PCL injuries has not yet been defined or agreed upon [19, 41]. However, all nonsurgical treatment modalities rely on physical therapy and temporary bracing or immobilization to restore normal tibiofemoral positioning [5, 6, 17, 21, 23, 25, 26, 47]. Knee range of motion exercises should be performed only in the prone position (Fig. 1) for the first week or weeks following injury/surgery to prevent hamstring activation and posterior sag of the tibia due to gravity, which would place increased stress on the healing ligament/graft [15]. Range of motion exercises during therapy should be limited to 90° for the first 2 weeks, with the least amount of stress placed on the injured PCL between 40° and 90° of knee flexion. Based on biomechanical studies, these motion limits should avoid placing increased sheer forces on the damaged PCL [18, 20, 30, 39]. Return to sporting activities is not typically allowed until near full quadriceps strength has been restored and a firm end point on clinical examination is achieved (typically several months, but for elite athletes the time frame could be as little as 6–8 weeks with the expected risk of increased residual joint laxity) [5].
Posterior cruciate ligament rehabilitation tends to follow slower rehabilitation protocols than those for ACL injuries. Nonsurgical treatment patients should meet the criteria for isolated PCL injury (Table 1). Additionally, a small, non-displaced PCL bony avulsion with grade I/II laxity can also reportedly be treated with progressive weight bearing and rehabilitation focused on quadriceps strengthening [53]. Nonoperative treatments are somewhat similar to the rehabilitation protocols for postoperative patients, but typically are shorter and allow for earlier range of motion and strengthening [34].
There are several reported nonsurgical treatment options for isolated grade I and II PCL injuries. A three-phase treatment course has been reported to successfully rehabilitate isolated PCL injuries regardless of the grade of injury [23]. During the first 4 weeks following the injury (phase I), patients had their knee placed in a brace locked between 0° and 60° of knee flexion. Rehabilitation during phase I focused on partial weight bearing, stretching of the hamstrings and gastrocnemius, and strengthening of the quadriceps. Phase II lasted until 12 weeks following the injury and allowed for resumption of full weight bearing and range of motion. Strengthening of the quadriceps and hamstrings using closed kinetic chain (CKC) and proprioceptive exercises was a key aspect of phase II. Phase III took place during the fifth and sixth months following the injury and was aimed at returning the patient to sports activities with a jogging programme, advanced proprioceptive exercises, and sport-specific exercises. The authors reported that patients with grade I and II injuries had good outcomes following this protocol, while grade III tears typically went on to require surgical reconstruction [23].
Another study reported improved PCL stability by placing patients in a cylindrical leg cast with a posterior support to prevent posterior displacement of the tibia [26]. Once the oedema had receded following the injury, patients had their leg casted in full extension for 6 weeks, and the cast was replaced if it became loose. While in the cast, straight leg raises and quadriceps strengthening exercises were recommended. After 6 weeks, the cast was removed and subjects were placed in a hinged knee brace with a posterior tibial spring support and started on a physical therapy programme, which included closed kinetic chain exercises. Flexion of up to 90° was allowed during the third week after cast removal and was progressed to 120° by 6–12 weeks after cast removal [26].
The results using a dynamic anterior drawer brace (PCL Jack brace [Albrecht GmbH, Stephanskirchen, Germany]) to nonoperatively treat patients with PCL injuries have also recently reported improved PCL stability [25]. The brace was worn by patients for 4 months. It applied an anteriorly directed force on the posterior proximal tibia while allowing full weight bearing through a range of motion from 0° to 110° (the brace reportedly only maintained an anterior translation force from 0° to 90°) of knee flexion. This restored the tibia to its normal position relative to the femur and reportedly allowed the intrinsic healing ability of the PCL to have a maximal effect by reducing tension on the anterolateral bundle. While patients were in the brace, they were only allowed to remove it to shower and when in the prone position. At the end of the 4 months, the brace was removed and physical therapy was initiated to help regain strength and mobility. Follow-up assessment showed improvement on radiological evaluation using bilateral Puddu views and bilateral lateral views in 70° of flexion and hamstring contraction (from 8.5 to 8.1 mm of posterior sag to 3.2 and 3.1 mm of posterior sag, respectively). Return to sport-related activities was allowed at 6 months [25].
A suggested nonoperative rehabilitation protocol for PCL injuries based on a compilation of these studies, with further stepwise details based on the authors’ clinical practice, is outlined in Table 2. Patients who fail conservative treatment should be reassessed and considered for surgical repair or reconstruction. Chronic isolated or combined PCL injuries may require serial PCL stress radiographs to objectively gauge injury progression and dictate treatment modifications [22, 24].
Postoperative rehabilitation of PCL reconstructions
Rehabilitation protocols following repairs and reconstruction of the PCL have not been clearly outlined [42]. Following surgery, patients are typically placed on a strict rehabilitation schedule that focuses on quadriceps strengthening and restoring full range of motion without stressing the graft [53]. It is very important that patients be advised that their compliance in the postoperative rehabilitation programme is essential to their ultimate outcome. Depending on the severity of the original injury and the structures that are concurrently reconstructed or repaired, rehabilitation protocols will vary somewhat; however, the approach to rehabilitation should be more conservative compared to techniques used following ACL reconstruction [15]. Rehabilitation exercises which cause posterior tibial translation (e.g. seated leg curls) should be discouraged [53]. Regardless of the postoperative treatment programme, the joint should be immobilized in extension immediately after surgery to keep the knee reduced and curtail posterior tibial sag due to gravity and the hamstring forces while the graft heals [21, 38].
One reported rehabilitation protocol, which has been widely accepted and implemented, recommended keeping the knee locked in a long leg brace in full extension for 3–6 weeks [15, 28]. Patients were kept non-weight bearing on crutches until the brace was unlocked between postoperative weeks 4–6. Progressive range of motion was started during week 4 and weight bearing with a 25% increase in body weight per week was initiated during postoperative week 7. Crutches were not discontinued until the patient had sufficient quadriceps strength and control for unassisted ambulation. Open kinetic chain (OKC) quadriceps exercises from 45° to 0° of knee flexion began at week 11, but OKC resisted knee flexion was not started until 6 months postoperatively. Return to athletics was allowed between 6 and 9 months following surgery, depending on return of strength, range of motion, and proprioceptive skills [15].
Another report utilized a PCL Jack brace starting on day 3 and kept patients non-weight bearing on crutches for 6 weeks following surgery [48]. Range of motion exercises were initiated on postoperative day 1 and emphasized prone knee flexion from 0° to 90° and quadriceps strengthening. Patients were advised to avoid isolated hamstring exercises until at least 6 weeks postoperatively to prevent undue stress on the healing repair/graft due to potential posterior subluxation of the tibia [6]. Partial weight bearing and hamstring strengthening exercises were started at 6 weeks postoperatively in addition to leg presses to a maximum of 70° of knee flexion and riding a stationary bike. Strengthening exercises included both closed and open kinetic chain exercises accompanied by functional training and stability exercises. At 12 weeks postoperatively, patients were allowed to begin using low-impact knee exercises as well as a pool programme [48]. The authors evaluated the patients at 6 months postoperatively, both clinically and using posterior knee stress radiographs, to objectively determine the amount of PCL healing. If there had been adequate healing of the reconstruction/repair (<2 mm of increased posterior translation on PCL stress radiographs compared to the contralateral knee), the PCL Jack brace was discontinued. Patients were then allowed to begin a running progression programme, side-to-side exercises, and proprioceptive exercises. Between 9 and 12 months postoperatively, patients underwent functional testing, which included balance, strength, and endurance testing to gauge their ability to resume full activities and sports [48].
A study conducted on patients following a single-bundle PCL reconstruction used a “non-aggressive” rehabilitation protocol and reported significant improvements in subjective laxity at an average of 30 months postoperatively [42]. The protocol was based on bracing to temporarily reduce shear forces due to gravity and hamstring contraction, strength training in the quadriceps, and early and progressive increases in weight bearing. For 45 days following surgery, patients were kept immobilized in a brace locked in extension, which utilized a foam cushion behind the tibia to prevent strain on the graft. Minimal weight bearing on crutches was allowed on day 1, but progressive weight bearing was not allowed until day 10 and crutches were required until day 45. Passive flexion was limited to 60° for the first 2 weeks following surgery and was gradually progressed to 95° by day 45 and to 120° by day 90. Exercises to strengthen the gastrocnemius and quadriceps were initiated on day 15; on day 45, half-squats and horizontal leg presses were initiated within 0° to 60° of flexion. Strengthening of the hamstrings with open kinetic chain exercises was not allowed until the sixth postoperative month. Proprioceptive training was started around day 90, progressing from two-leg to one-leg exercises. An exercise bike without resistance was employed starting on day 45 and resistance was introduced on day 90. After day 90, light jogging was allowed, working up to unrestricted running at day 150. Athletes could begin sports-related training again 8 months after their surgery [42].
A five phase, early progressive rehabilitation protocol used following double bundle PCL reconstruction with allograft tissue was reported with improved stability on clinical laxity testing [37]. Subjects were advanced from one phase to the next every 4 weeks based on rehabilitation goals for each phase. Phase I (0–4 weeks postoperatively) had goals of reduced joint effusion, reestablished quadriceps contractility, and ambulation progression from crutches to using a locked long leg knee brace locked at 0° flexion. During phase I, knee flexion was not allowed past 90°. The goals of phase II (4–8 weeks postoperatively) were an active range of motion of 0° to 130° knee flexion, decreased suprapatellar girth measurements, independent performance of a 6-in. lateral step-down task and the ability to maintain balance during nonsagittal plane movement while standing on the involved side. Phase III (8–12 weeks postoperatively) goals included return to symmetrical active knee range of motion and suprapatellar girth, completing a coordinated single leg mini-squat and one-leg hop testing of at least 80 % of the contralateral normal side. Phase IV (weeks 12–16 postoperatively) aimed to return the subjects to running, and initiated agility and plyometric activities. One-leg hop testing was required to be at least 90 % of the contralateral normal side to progress to the final phase. Phase V (16–20 weeks postoperatively) was focused on improvement of the injured side on testing with an advanced functional manoeuvre simulating a sports movement [37].
A suggested postoperative rehabilitation protocol for PCL injuries based on the data in these studies, with further stepwise details based on the authors’ clinical practice, is outlined in Table 3. Similar to the nonoperative protocol, chronic isolated or combined PCL injuries may require PCL stress radiographs to objectively gauge injury progression and dictate treatment modifications [22, 24].
Discussion
This review demonstrates the importance of rehabilitation programmes following PCL injury or surgical repair/reconstruction as a key factor in influencing ligament or graft healing and improving patient outcomes. Current practices and reports of PCL rehabilitation programmes do not show continuity and typically do not address the majority of important aspects related to successful PCL rehabilitation. This is especially important because PCL injuries occur more often than initially thought, and surgical reconstructions of the PCL are increasing [32]. As such, rehabilitation programmes merit further attention and agreement in the medical community.
Regardless of the treatment modality selected for a PCL injury, specific rehabilitation exercises are shared among treatment protocols. Unlike ACL rehabilitation protocols, initially keeping a patient non-weight bearing immediately following PCL reconstruction is important to prevent strain on the graft, because the PCL is the primary static stabilizer of the knee [52].
Biomechanical studies have elucidated the sheer forces that act on the PCL during normal knee movements and following injury to the PCL [9, 17, 25, 29, 44–47, 49, 52]. During normal knee motion, the PCL is a primary static stabilizer preventing posterior translation of the femur over the tibia, and tension in the PCL changes with varying degrees of knee flexion [32, 52]. Sheer forces on the PCL have reported to increase at 30° of flexion and to be greatest at flexion angles higher than 50°–60° [9, 36]. Following PCL injury/reconstruction, isokinetic extension exercises at less than 70° of knee flexion have been reported to be safe and will not overstress the ligament/graft. Isokinetic flexion exercises and deep flexion squats, on the other hand, should not be attempted until sufficient time has passed to allow for healing of the injured ligament or reconstruction graft [9, 51].
In addition, further strain is placed on the PCL during active contraction of the hamstring muscles [49]. A proper rehabilitation programme should minimize these forces during PCL rehabilitation to allow for successful graft/ligament healing. This is readily accomplished by keeping the knee immobilized using an anterior directed drawer force and by not allowing active isolated hamstring exercises until an appropriate time during rehabilitation (12 weeks after starting a nonoperative rehabilitation programme and 24 weeks following surgery). Because graft healing in PCL reconstructions has been reported to take nearly twice as long compared to ACL reconstructions, it has been reported that keeping PCL reconstruction patients non-weight bearing for 6 weeks is necessary to allow for adequate graft healing and revascularization to occur [1, 4, 21].
Eccentric weakness of the quadriceps and hamstrings has been reported as major factors that need to be addressed following PCL injuries [31]. This suggests that eccentric strengthening, including open and closed kinetic chain exercises, should be a vital part of any therapy. Open and closed kinetic chain exercises are the foundation of PCL rehabilitation protocols; however, OKC exercises should only be used with limited flexion angles until the ligament/graft has had adequate time to heal [36].
Open kinetic chain exercises are able to isolate single muscle groups for strengthening, which makes them especially important in the early weeks following PCL injury or surgery [36]. However, OKC exercises that activate the hamstrings should be avoided in the initial phases of PCL rehabilitation, because studies have reported that they can stretch out grafts or cause further injury to the already damaged ligament [29, 30].
Closed kinetic chain exercises are unable to isolate a single muscle group because they activate antagonistic muscle groups across multiple joints [30]. They can also produce increased shear forces on the healing ligament. For these reasons, CKC exercises should be initially avoided while OKC exercises are used to strengthen the quadriceps during the early stages of rehabilitation [56].
Closed chain exercises, including squats and leg presses (Fig. 2), are ideal for strengthening the quadriceps and gluteal muscles [30]. It has been reported that the eccentric squat is an excellent exercise to increase quadriceps strength during any form of lower extremity rehabilitation [32]. Strengthening the quadriceps is especially important in PCL rehabilitation, because the quadriceps secondarily contribute to anteroposterior stability with the PCL, and, as previously stated, patients with improved quadriceps strength typically achieve significantly better outcomes following PCL injury [32]. Escamilla et al. [10] favoured leg presses with a narrow stance over squats during the initial phases of PCL rehabilitation. This is because squats generate greater PCL tensile forces than leg presses over varying knee flexion angles. Once the quadriceps strength of the injured side is great than or equal to 90 % compared to the uninjured side, the patient can begin a progression of running activities [53].
Single leg balance squat demonstrating the starting position (a) and finishing position (b); allow the toe of the uninvolved leg to touch the chair and squat with involved leg to 70° keeping the hips level and the knees behind the toes while avoiding full extension of the leg upon returning to start position
Single leg bridge demonstrating the starting position (a) and finishing position (b); lie supine with the knees bent and feet shoulder width apart, grasp the uninvolved knee to chest and contract the gluteal muscles of the involved side to raise the hips off the mat to form a straight line with the shoulders, hips, and knee
Reports have suggested that therapists and physicians should use caution when allowing patients to begin forward and side lunge exercises in the rehabilitation process, due to the high forces on the PCL that are generated by these exercises [11]. Lower knee flexion angles and a shorter stride lunge should be used when starting such exercises, because they have been reported to generate the least force on the PCL [12].
The limitations of this study are that it is a review article and does not have any outcome data to support the recommendations made. The studies which were reviewed all came from the English-based literature and reports published in other languages were not considered. This review clearly demonstrates that there is a paucity of peer-reviewed data comparing suggested forms of PCL rehabilitation and the impact they have on patient outcomes. Therefore, future research is needed to investigate and establish an accepted protocol for PCL rehabilitation. Based on these reports, the studies reviewed above, and the author’s clinical experience, recommended postoperative and nonoperative programme for patients following PCL injury are presented in Tables 2 and 3, respectively.
Conclusions
An optimal set of guidelines for nonoperative or postoperative management of PCL injuries has not yet been defined or agreed upon. There is a lack of peer-reviewed publications comparing the subjective and objective outcomes of both postoperative PCL rehabilitation and nonoperative treatment programmes. Future studies need to define outcomes for various PCL rehabilitation programmes to allow practitioners to agree on and implement the most effective protocols to improve patient outcomes.
References
Bellelli A, Adriani E, Margheritini F, Camillieri G, Della Rocca C, Mariani PP (1999) Synovial healing in reconstructed cruciate ligaments. Our personal experience compared in single interventions and combined reconstructions. Radiol Med 98:454–461
Bergfeld JA, Graham SM, Parker RD, Valdevit AD, Kambic HE (2005) A biomechanical comparison of posterior cruciate ligament reconstructions using single- and double-bundle tibial inlay techniques. Am J Sports Med 33:976–981
Miller RH, Azar FM (2007) Knee Injuries. In: Canale ST, Beaty JH (eds) Campbell’s operative orthopedics, 11th edn. Elsevier, Maryland Heights, pp 2552–2565
Clancy WG Jr, Narechania RG, Rosenberg TD, Gmeiner JG, Wisnefske DD, Lange TA (1981) Anterior and posterior cruciate ligament reconstruction in rhesus monkeys. J Bone Joint Surg Am 63:1270–1284
Colvin AC, Meislin RJ (2009) Posterior cruciate ligament injuries in the athlete: diagnosis and treatment. Bull NYU Hosp Jt Dis 67:45–51
Cosgarea AJ, Jay PR (2001) Posterior cruciate ligament injuries: evaluation and management. J Am Acad Orthop Surg 9:297–307
Dandy DJ, Pusey RJ (1982) The long-term results of unrepaired tears of the posterior cruciate ligament. J Bone Joint Surg Br 64:92–94
Edson CJ, Fanelli GC, Beck JD (2010) Postoperative rehabilitation of the posterior cruciate ligament. Sports Med Arthrosc 18:275–279
Escamilla RF (2001) Knee biomechanics of the dynamic squat exercise. Med Sci Sports Exerc 33:127–141
Escamilla RF, Fleisig GS, Zheng N, Lander JE, Barrentine SW, Andrews JR, Bergemann BW, Moorman CT (2001) Effects of technique variations on knee biomechanics during the squat and leg press. Med Sci Sports Exerc 33:1552–1566
Escamilla RF, Zheng N, MacLeod TD, Imamura R, Edwards WB, Hreljac A, Fleisig GS, Wilk KE, Moorman CT, Paulos L, Andrews JR (2010) Cruciate ligament tensile forces during the forward and side lunge. Clin Biomech 25:213–221
Escamilla RF, Zheng N, Macleod TD, Imamura R, Edwards WB, Hreljac A, Fleisig GS, Wilk KE, Moorman CT 3rd, Paulos L, Andrews JR (2010) Cruciate ligament forces between short-step and long-step forward lunge. Med Sci Sports Exerc 42:1932–1942
Fanelli GC (1993) Posterior cruciate ligament injuries in trauma patients. Arthroscopy 9:291–294
Fanelli GC, Boyd JL, Heckler MW (2009) How I manage posterior cruciate ligament injuries. Oper Tech Sports Med 17:175–193
Fanelli GC (2008) Posterior cruciate ligament rehabilitation: how slow should we go? Arthroscopy 24:234–235
Fanelli GC, Edson CJ (1995) Posterior cruciate ligament injuries in trauma patients: part II. Arthroscopy 11:526–529
Fowler PJ, Messieh SS (1987) Isolated posterior cruciate ligament injuries in athletes. Am J Sports Med 15:553–557
Fox RJ, Harner CD, Sakane M, Carlin GJ, Woo SLY (1998) Determination of the in situ forces in the human posterior cruciate ligament using robotic technology a cadaveric study. Am J Sports Med 26:395–401
Grassmayr MJ, Parker DA, Coolican MR, Vanwanseele B (2008) Posterior cruciate ligament deficiency: biomechanical and biological consequences and the outcomes of conservative treatment. A systematic review. J Sci Med Sport 11:433–443
Grood ES, Stowers SF, Noyes FR (1988) Limits of movement in the human knee: effect of sectioning the posterior cruciate ligament and posterolateral structures. J Bone Joint Surg Am 70A:88–97
Harner CD, Hoher J (1998) Evaluation and treatment of posterior cruciate ligament injuries. Am J Sports Med 26:471–482
Hewett TE, Noyes FR, Lee MD (1997) Diagnosis of complete and partial posterior cruciate ligament ruptures. Stress radiography compared with KT-1000 arthrometer and posterior drawer testing. Am J Sports Med 25:648–655
Ittivej K, Prompaet S, Rojanasthien S (2005) Factors influencing the treatment of posterior cruciate ligament injury. J Med Assoc Thai 88(Supp 5):S84–S88
Jackman T, LaPrade RF, Pontinen T, Lender PA (2008) Intraobserver and interobserver reliability of the kneeling technique of stress radiography for the evaluation of posterior knee laxity. Am J Sports Med 36:1571–1576
Jacobi M, Reischl N, Wahl P, Gautier E, Jakob RP (2010) Acute isolated injury of the posterior cruciate ligament treated by a dynamic anterior drawer brace. J Bone Joint Surg Br 92:1381–1384
Jung YB, Tae SK, Lee YS, Jung HJ, Nam CH, Park SJ (2008) Active non-operative treatment of acute isolated posterior cruciate ligament injury with cylinder cast immobilization. Knee Surg Sports Traumatol Arthrosc 16:729–733
Lenschow S, Zantop T, Weimann A, Lemburg T, Raschke M, Strobel M, Petersen W (2006) Joint kinematics and in situ forces after single bundle PCL reconstruction: a graft placed at the center of the femoral attachment does not restore normal posterior laxity. Arch Orthop Trauma Surg 126:253–259
Levy BA, Boyd JL, Stuart MJ (2011) Surgical treatment of acute and chronic anterior and posterior cruciate ligament and lateral side injuries of the knee. Sports Med Arthrosc Rev 19:110–119
Lopez-Vidriero E, Simon DA, Johnson DH (2010) Initial evaluation of posterior cruciate ligament injuries: history, physical examination, imaging studies, surgical and nonsurgical indications. Sports Med Arthrosc 18:230–237
Lutz GE, Palmitier RA, An KN, Chao EY (1993) Comparison of tibiofemoral joint forces during open-kinetic-chain and closed kinetic-chain exercises. J Bone Joint Surg Am 75:732–739
MacLean CL, Taunton JE, Clement DB, Regan W (1999) Eccentric and concentric isokinetic moment characteristics in the quadriceps and hamstrings of the chronic isolated posterior cruciate ligament injured knee. Br J Sports Med 33:405–408
MacLean CL, Taunton JE, Clement DB, Regan WD, Stanish WD (1999) Eccentric kinetic chain exercise as a conservative means of functionally rehabilitating chronic isolated insufficiency of the posterior cruciate ligament. Clin J Sport Med 9:142–150
Margheritini F, Rihn J, Musahl V, Mariani PP, Harner C (2002) Posterior cruciate ligament injuries in the athlete: an anatomical, biomechanical and clinical review. Sports Med 32:393–408
Markey KL (1991) Functional rehabilitation of the cruciate-deficient knee. Sports Med 12:407–417
Matava MJ, Ellis E, Gruber B (2009) Surgical treatment of posterior cruciate ligament tears: an evolving technique. J Am Acad Orthop Surg 17:435–446
Mesfar W, Shirazi-Adl A (2008) Knee joint biomechanics in open-kinetic-chain flexion exercises. Clin Biomech 23:477–482
Nyland J, Hester P, Caborn DN (2002) Double-bundle posterior cruciate ligament reconstruction with allograft tissue: 2-year postoperative outcomes. Knee Surg Sports Traumatol Arthrosc 10:274–279
Ogata K, McCarthy JA (1992) Measurements of length and tension patterns during reconstruction of the posterior cruciate ligament. Am J Sports Med 20:351–355
Pandy MG, Shelburne KB (1997) Dependence of cruciate-ligament loading on muscle forces and external load. J Biomech 30:1015–1024
Parolie JM, Bergfeld JA (1986) Long-term results of nonoperative treatment of isolated posterior cruciate ligament injuries in the athlete. Am J Sports Med 14:35–38
Petrigliano FA, McAllister DR (2006) Isolated posterior cruciate ligament injuries of the knee. Sports Med Arthrosc 14:206–212
Quelard B, Sonnery-Cottet B, Zayni R, Badet R, Fournier Y, Hager JP, Chambat P (2010) Isolated posterior cruciate ligament reconstruction: is non-aggressive rehabilitation the right protocol? Orthop Traumatol Surg Res 96:256–262
Sekiya JK, West RV, Ong BC, Irrgang JJ, Fu FH, Harner CD (2005) Clinical outcomes after isolated arthroscopic single-bundle posterior cruciate ligament reconstruction. Arthroscopy 21:1042–1050
Shelbourne KD, Davis TJ, Patel DV (1999) The natural history of acute, isolated, nonoperatively treated posterior cruciate ligament injuries: a prospective study. Am J Sports Med 27:276–283
Shelbourne KD, Gray T (2002) Natural history of acute posterior cruciate ligament tears. J Knee Surg 15:103–107
Shelbourne KD, Jennings RW, Vahey TN (1999) Magnetic resonance imaging of posterior cruciate ligament injuries: assessment of healing. Am J Knee Surg 12:209–213
Shelbourne KD, Muthukaruppan Y (2005) Subjective results of nonoperatively treated, acute, isolated posterior cruciate ligament injuries. Arthroscopy 21:457–461
Spiridonov SI, Slinkard NJ, LaPrade RF (2011) Isolated and combined grade III PCL tears treated with double bundle reconstructions using an endoscopic femoral graft placement: operative technique and clinical outcomes. J Bone Joint Surg Am 93:1773–1780
Strobel MJ, Weiler A, Schulz MS, Russe K, Eichhorn HJ (2002) Fixed posterior subluxation in posterior cruciate ligament-deficient knees: diagnosis and treatment of a new clinical sign. Am J Sports Med 30:32–38
Torg JS, Barton TM, Pavlov H, Stine R (1989) Natural history of the posterior cruciate ligament-deficient knee. Clin Orthop Relat Res 246:208–216
Toutoungi DE, Lu TW, Leardini A, Catani F, O’Connor JJ (2000) Cruciate ligament forces in the human knee during rehabilitation exercises. Clin Biomech 15:176–187
Van Dommelon BA, Fowler PJ (1989) Anatomy of the posterior cruciate ligament. A review. Am J Sports Med 17:24–29
Veltri DM, Warren RF (1993) Isolated and combined posterior cruciate ligament injuries. J Am Acad Orthop Surg 1:67–75
Veltri DM, Warren RF, Silver G (1993) Complications in posterior cruciate ligament surgery. Oper Techn Sport Med 1:154–158
Watsend AM, Oestad TM, Jakobsen RB, Engebretsen L (2009) Clinical studies on posterior cruciate ligament tears have weak design. Knee Surg Sports Traumatol Arthrosc 17:140–149
Wilk KE (1994) Rehabilitation of isolated and combined posterior cruciate ligament injuries. Clin Sports Med 13:649–677
Acknowledgments
This research was supported by the Steadman Philippon Research Institute, which is a 501(c)(3) non-profit institution supported financially by private donations and corporate support from the following entities: Smith & Nephew Endoscopy, Arthrex, Inc., Siemens Medical Solutions USA, Inc., OrthoRehab, ConMed Linvatec, Össur Americas, Small Bone Innovations, Inc., and Opedix. One of the authors is a paid consultant for Arthrex.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pierce, C.M., O’Brien, L., Griffin, L.W. et al. Posterior cruciate ligament tears: functional and postoperative rehabilitation. Knee Surg Sports Traumatol Arthrosc 21, 1071–1084 (2013). https://doi.org/10.1007/s00167-012-1970-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-012-1970-1