Abstract
We present a case of meniscal cyst formation 1 year following a successful meniscal repair in a 30-year-old male using a hybrid suture–anchor meniscal repair system. Open excision of the cyst revealed it to be in continuity with the suture–anchor fragments. The patient made an uneventful recovery.
Level of evidence V.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Meniscal tears have an incidence of 60–70 per 100,000 people per year in the adult population [6]. While the incidence of tears suitable for repair is not known, meniscal preservation is important in the prevention of osteoarthritis [18]. Meniscal cysts following meniscal repair are uncommon. A case report of cyst formation 1 year following a successful meniscal repair using a non-absorbable PEAK-OPTIMA FastFix anchor system (Smith and Nephew, Andover, Massachusetts) is presented with a review of the literature.
Case report
A 30-year-old male manual worker felt his right knee ‘pop’ while deep squatting carrying a heavy load. Following this, he experienced a locked knee and medial knee pain. On examination, he had a moderate effusion, tenderness along the medial joint line and an extension loss of thirty degrees with full flexion.
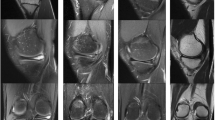
A magnetic resonance imaging (MRI) scan confirmed a large bucket handle tear of the medial meniscus (Fig. 1). At arthroscopy, the tear was reduced and repaired with four Ultra FastFix PEEK-OPTIMA suture anchors (Smith and Nephew, Andover, Massachusetts) using an ‘all-inside’ technique.
Post-operatively, he was allowed to partial weight bear with crutches in a hinged knee brace allowing movement from 0 to 90° for 6 weeks. He was referred to physiotherapy for quadriceps strengthening exercises and was told to avoid squatting for 3 months. The patient progressed well and at 6 months post-surgery had returned to normal duties and golf.
One year post-meniscal repair, he developed a lump on the posteromedial aspect of his knee which was slowly increasing in size. The lump was gradually increasing in size and mildly tender when knocked. Although not presently impeding the patient’s work or recreational activities, it was causing him concern and he was keen to have the lump removed.
Repeat MRI scan showed a healed meniscal tear, with a meniscal cyst, arising from the posterior body of the medical meniscus measuring 2.9 × 1.6 × 2.2 cm. Two FastFix fragments were protruding into the cyst on MRI scan (Figs. 2, 3). The patient had repeat arthroscopy that showed a healed medial meniscus. The cyst was removed via open excision and was found to be in continuity with three FastFix anchors, which were removed.
The patient made an uneventful recovery with no residual knee pain or clinical recurrence of the cyst.
Discussion
Many different techniques exist for meniscal repair. These consist of either suture repair using “inside-out” or “outside-in” techniques, or “all-inside” techniques utilizing implants such as meniscal arrows [10, 12] or hybrid suture–anchor combinations such as the FastFix [10].
Suture repair has been shown to have strong fixation of meniscal tears [9, 10]. All-inside techniques have the advantage of decreased risk to the neurovascular structures surrounding the knee [10]. However, implants such as meniscal arrows have the disadvantage of possible chondral irritation [1, 3, 10, 14]. Hybrid devices such as FastFix allow “all-inside fixation” with the benefits of suture repair.
The FastFix meniscal repair system consists of two suture anchors with high molecular weight polyethylene ultrabraid sutures with a preloaded sliding knot [2]. The suture anchors consist of either an absorbable poly-l-lactic acid (PLLA) [2] or non-absorbable PEEK-OPTIMA polymer. The previous generation of FastFix anchors has consisted of polyacetal plastic or PLLA anchors. It is not well known that two different types of anchors exist for this product.
This is the first published case of a cyst related to the FastFix system. There have been six case series reporting the clinical use of the FastFix system in the literature [2, 4, 5, 7, 8, 17]. A total of 283 meniscal repairs have been reported in these case series with no cyst formation complications following meniscal repair. Two series [4, 17] made clear that the absorbable polylactic acid (PLLA) anchors were used. The other reports made no differentiation between the use of absorbable and non-absorbable anchors.
We identified ten cases of cysts following meniscal repair in the literature [8, 10–12, 15, 20]. Seven of the cases were following fixation with a meniscal fixation device [8, 12, 13, 15, 20] and three related to non-absorbable sutures [8, 10, 11].
Five cysts related to a bioabsorbable meniscal arrow [12, 20] have been reported. These patients presented at 10–12 weeks, and all had spontaneous resolution without surgery.
Two other non-absorbable fixation devices have reported cyst formation at the tips of or incorporating the fixation device [8, 19]. These developed at 12 weeks and 5 months after meniscal repair. Three cysts have been reported following repair using a non-absorbable suture material (nylon). These occurred at 5 months, 3 years and 6 years after surgery. In two of these cases, it was noted that the cyst was in continuity with the nylon suture material.
The theories proposed for the development of cysts following meniscal repair [8, 10] include the idea of cystic degeneration of the meniscus resulting from either trauma, degeneration or secondary to synovial cell migration into meniscal suture holes [8, 10, 11]. The placement of a fixation device external to the joint may allow the passage of synovial cells to the joint periphery via the pumping action of joint motion, with suture material acting as a tract for synovial fluid passage [11, 15], and a similar mechanism is found in synovial cyst formation in knees without any fixation devices [16]. Non-absorbable materials are at risk of late presentation of meniscal cysts, which appear directly related to the non-absorbable component.
The meniscal cysts associated with the use of absorbable meniscal arrows presented early and had spontaneous resolution of cysts. The cyst resolution is thus likely to have occurred when the arrows dissolved. There were no cases of meniscal cysts found after the use of absorbable suture material, or absorbable anchor/non-absorbable suture material combinations [11].
Although cyst formation post-meniscal repair is a rare complication, we suggest that meniscal fixation be carried out using an absorbable anchor component. It is important to be aware of the different combinations existing within the same fixation system.
References
Asik M, Atalar AC (2002) Failed resorption of bioabsorbable meniscus repair devices. Knee Surg Sports Traumatol Arthrosc 10:300–304
Barber A, Schroeder A, Barrera O, Beavis C (2008) Fast-fix meniscal repair: mid-term results. Arthroscopy 24:1342–1348
Bonshahi AY, Hopgood P, Shepard GJ (2004) Migration of a broken meniscal arrow: a case report and review of the literature. Knee Surg Sports Traumatol Arthrosc 12:50–51
Chiang CW, Chang CH, Cheng CY et al (2001) Clinical results of all-inside meniscal repair using the fast-fix meniscal repair system. Chang Gung Med J 34:298–305
Choi N, Sung-Jae K (2004) Meniscal cyst formation after inside-out meniscal repair. Arthroscopy 20:e1–e3
Greis PE, Bardana DD, Holmstrom MC, Burks RT (2002) Meniscal injury: I. basic science and evaluation. J Am Adac Orthop Surg 10:168–176
Haas AL, Schepsis AA, Hornstein J, Edgar CM (2005) Meniscal repair using the fast-fix all-inside meniscal repair device. Arthroscopy 21:167–175
Kimura M, Hagiwara A, Hasegawa A (1993) Cyst of the medial meniscus after arthroscopic meniscal repair. Am J Sports Med 21:755–757
Kocabey Y, Taser O, Hapa O et al (2011) Meniscal repair using large diameter horizontal sutures increases fixation strength: an in vitro study. Knee Surg Sports Traumatol Arthrosc 19:202–206
Kotsovolos ES, Hantes ME, Mastrokalos DS, Lorbach O, Paessler HH (2006) Results of all-inside meniscal repair with the fast-fix meniscal repair system. Arthroscopy 22:3–9
Lombardo S, Eberly V (1999) Meniscal cyst formation after all-inside meniscal repair. Am J Sports Med 27:666–667
Nagura I, Yagi M, Kokubu T, Yoshiya S, Kurosaka M (2004) Generation of meniscal cyst after arthroscopic meniscal repair. Arthroscopy 20:869–871
Nakamae A, Deie M, Yasumoto M, Kobayashi K, Ochi M (2004) Synovial cyst formation resulting from nonabsorbable meniscal repair devices for meniscal repair. Arthroscopy 20:16–19
Otte S, Klinger HM, Beyer J, Baums MH (2002) Complications after meniscal repair with bioabsorbable arrows: two cases and analysis of literature. Knee Surg Sports Traumatol Arthrosc 10:250–253
Popescu D, Sastre S, Caballero M et al (2010) Meniscal repair using the fast-fix device in patients with chronic meniscal lesions. Knee Surg Sports Traumatol Arthrosc 18:546–550
Shetty GM, Wang JH, Ahn JH, Lee YS, Kim BH, Kim JG (2008) Giant synovial cyst of knee treated arthroscopically through a cystic portal. Knee Surg Sports Traumatol Arthrosc 16:175–178
Tachibana Y, Sakaguchi K, Goto T, Oda H, Yamazaki K, Iida S (2010) Repair integrity evaluated by second-look arthroscopy after arthroscopic meniscal repair with the fast-fix during anterior cruciate ligament reconstruction. Am J Sports Med 38:965–971
Tengrootenhuysen M, Meermans G, Pittoors K, van Riet R, Victor J (2011) Long-term outcome after meniscal repair. Knee Surg Sports Traumatol Arthrosc 19:236–241
Tingstad EM, Teitz CC, Simonian PT (2001) Complications associated with the use of meniscal arrows: case reports. Am J Sports Med 29:96–98
Yoo JH, Yoon JR, Lee SJ (2008) Parameniscal cyst formation after arthroscopic meniscal repair with biodegradable meniscal arrow: a case report. Knee Surg Sports Traumatol Arthrosc 16:815–817
Conflict of interest
Neither author has any conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kulkarni, V., Mulford, J. Cyst following meniscal repair. Knee Surg Sports Traumatol Arthrosc 20, 2197–2199 (2012). https://doi.org/10.1007/s00167-011-1803-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-011-1803-7