Abstract
Objective
To describe the various patterns of neurophysiological abnormalities which may complicate prolonged critical illness and identify possible aetiological factors.
Design
Prospective case series of neurophysiological studies, severity of illness scores, organ failures, drug therapy and hospital outcome. Some patients also had muscle biopsies.
Setting
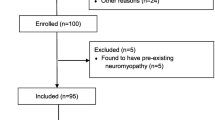
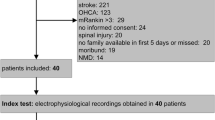
General intensive care unit (ICU) in a University Hospital. Patients: Forty-four patients requiring intensive care unit stay of more than 7 days. The median age was 60 (range 27–84 years), APACHE II score 19 (range 8–33), organ failures 3 (range 1–6), and mortality was 23%.
Results
Seven patients had normal neurophysiology (group I), 4 had a predominantly sensory axonal neuropathy (group II), 11 had motor syndromes characterised by markedly reduced compound muscle action potentials and sensory action potentials in the normal range (group III) and 19 had combinations of motor and sensory abnormalities (group IV). Three patients had abnormal studies but could not be classified into the above groups (group V). All patients had normal nerve conduction velocities. Electromyography revealed evidence of denervation in five patients in group III and five in group IV. There was no obvious relationship between the pattern of neurophysiological abnormality and the APACHE II score, organ failure score, the presence of sepsis or the administration of muscle relaxants and steroids. A wide range of histological abnormalities was seen in the 24 patients who had a muscle biopsy; there was no clear relationship between these changes and the neurophysiological abnormalities, although histologically normal muscle was only found in patients with normal neurophysiology. Only three of the eight patients from group III in whom muscle biopsy was performed had histological changes compatible with myopathy.
Conclusions
Neurophysiological abnormalities complicating critical illness can be broadly divided into three types — sensory abnormalities alone, a pure motor syndrome and a mixed motor and sensory disturbance. The motor syndrome could be explained by an abnormality in the most distal portion of the motor axon, at the neuromuscular junction or the motor end plate and, in some cases, by inexcitable muscle membranes or extreme loss of muscle bulk. The mixed motor and sensory disturbance which is characteristic of ‘critical illness polyneuropathy’ could be explained by a combination of the pure motor syndrome and the mild sensory neuropathy. More precise identification of the various neurophysiological abnormalities and aetiological factors may lead to further insights into the causes of neuromuscular weakness in the critically ill and ultimately to measures for their prevention and treatment.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Segredo V, Caldwell JE, Matthay MA, Sharma ML, Gruenke LD, Miller RD (1992) Persistent paralysis in critically ill patients after long term administration of vecuronium. N Engl J Med 327: 524–528
Coakley JH, Nagendran K, Honavar M, Hinds CJ (1993) Preliminary observations on the neuromuscular abnormalities in patients with organ failure and sepsis. Intensive Care Med 19: 323–328
Roelofs RI, Cerra F, Beilka N, Rosenberg L, Canton OH, Delaney J (1983) Prolonged respiratory insufficiency due to acute motor neuropathy; a new syndrome? Neurology 33 (Suppl 2): 240
Rivner MH, Kim S, Greenberg M, Swift TR (1983) Reversible generalised paresis following hypotension: a new neurological entity. Neurology 33 (Suppl 2): 164
Bolton CF, Gilbert JJ, Hahn AF, Sibbald WJ (1984) Polyneuropathy in critically ill patients. J Neurol Neurosurg Psychiatry 47: 1223–1231
Douglass JA, Tuxen DV, Horne M, Sheinkestel C (1992) Myopathy in severe asthma. Am Rev Respir Dis 146: 517–519
Griffin D, Fairman N, Coursin D, Rawsthorne L, Grossman JE (1992) Acute myopathy during treatment of status asthmaticus with corticosteroids and steroidal muscle relaxants. Chest 102: 510–514
Barrett SA, Mourani S, Villareal CA, Gonzales JM, Zimmerman JI (1993) Rhabdomyolysis associated with status asthmaticus. Crit Care Med 21:151–153
Coakley JH, Edwards RHT, McClelland P, Bone JM, Helliwell TR (1990) Occult skeletal muscle necrosis associated with renal failure. BMJ 301: 370
Helliwell TR, Coakley JH, Wagenmakers AJ, Griffiths RD, Campbell IT, Green C, McClelland P, Williams PS, Bone JM (1991) Necrotising myopathy in critically ill patients. J Pathol 164: 307–314
Hirano M, Ott BR, Raps EC, Minetti C, Lennihan L, Libbey MP, Bonilla E, Hays AP (1992) Acute quadriplegic myopathy: a complication of treatment with steroids, nondepolarising blocking agents, or both. Neurology 42: 2082–2087
Rich MM, Teener JW, Raps EC, Schotland DL, Bird SJ (1996) Muscle is electrically inexcitable in acute quadriplegic myopathy. Neurology 46: 731–736
Coakley JH, Nagendran K, Ormerod IED, Ferguson CN, Hinds CJ (1992) Prolonged neurogenic weakness in patients receiving mechanical ventilation for acute airflow limitation. Chest 101: 1413–1416
Gorson KC, Ropper AH (1993) Acute respiratory failure neuropathy: A variant of critical illness polyneuropathy. Crit Care Med 21: 267–271
Hund E, Genzworker H, Bohrer J, Jacob H, Thiele R, Hacke W (1997) Predominant involvement of motor fibres in patients with critical illness neuropathy. Br J Anaesth 78: 274–278
Zochodne DW, Ramsay DA (1994) Acute quadriplegic myopathy. Neurology 44:988–989
Witt NJ, Zochodne DW, Bolton CF (1991) Peripheral nerve function in sepsis and multiple organ failure. Chest 99: 176–184
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: aseverity of disease classification system. Crit Care Med 13: 818–829
Berek K, Margreiter J, Willeit J, Berek A, Schmutzhard E, Mutz NJ (1996) Polyneuropathies in critically ill patients: a prospective evaluation. Intensive Care Med 22: 849–855
Op de Coul AAW, Lambregts PCLA, Koeman J, Van Puyenbroek MJE, Ter Laak HJ, Gabreels-Feston AAWM (1985) Neuromuscular complications in patients given Pavulon (pancuronium bromide) during artificial ventilation. Clin Neurol Neurosurg 87: 17–22
Tousignant EP, Bevan DR, Eisen AA, Fenwick JC, Tweedale MG (1995) Acute quadriparesis in an asthmatic treated with atracurium. Can J Anaesth 42: 224–227
Sladen RN (1995) Neuromuscular blocking agents in the intensive care unit: a two-edged sword. Crit Care Med 23: 423–428
Leijten FSS, Harinck-De Weerd JE, Poortvliet DCJ, De Weerd AW (1995) The role of polyneuropathy in motor convalescence after prolonged mechanical ventilation. JAMA 274:1221–1225
McKhann GM, Cornblath DR, Griffin JW, et al. (1993) Acute motor axonal neuropathy: a frequent cause of acute flaccid paralysis in China. Ann Neurol 33:333–342
Schwarz J, Planck J, Briegel J, Straube A (1997) Single fibre electromyography, nerve conduction velocities and conventional electromyography in patients with critical illness neuropathy: evidence for a lesion of terminal motor axons. Muscle Nerve 20: 696–701
Latronico N, Fenzi F, Recupero D, et al. (1996) Critical illness myopathy and neuropathy. Lancet 347:1579–1582
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Coakley, J.H., Nagendran, K., Yarwood, G.D. et al. Patterns of neurophysiological abnormality in prolonged critical illness. Intensive Care Med 24, 801–807 (1998). https://doi.org/10.1007/s001340050669
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s001340050669