Abstract
Purpose
To describe long-term mortality and hospital readmissions of patients admitted to Brazilian intensive care units (ICU).
Methods
Retrospective cohort study of adult patients admitted to Brazilian hospitals affiliated to the Public Healthcare System from 10 state capitals. ICU patients were paired to non-ICU patients by frequency matching (ratio 1:2), according to postal code and admission semester. Hospitalization records were linked through deterministic linkage to national mortality data. Primary outcome was mortality up to 1 year. Other outcomes were mortality and readmissions at 30 and 90 days and 3 years. Multiple Cox regressions were used adjusting for age, sex, cancer diagnosis, type of hospital, and surgical status.
Results
We included 324,594 patients (108,302 ICU and 216,292 non-ICU). ICU patients had increased hospital length of stay [9 (5–17) vs. 3 (1–6) days, p < 0.001] and mortality (18.5 vs. 3.6%, p < 0.001) versus non-ICU patients. One year after discharge, ICU patients were more frequently readmitted to hospital (25.4 vs. 17.4%, p < 0.001) and to ICU (31.4 vs. 7.3%, p < 0.001) than controls. Mortality up to 1 year was also higher for ICU patients (14.3 vs. 3.9%, p < 0.001). A significant interaction between surgical status and mortality was found, with adjusted hazard ratios (HRs) up to 1 year of 2.7 [95% confidence interval (CI) 2.5–2.9] for surgical patients, and 3.4 (95%CI 3.3–3.5) for medical patients. The risk for death and readmission diminished over time up to 3 years.
Conclusions
In a public healthcare system of a developing country, ICU patients have excessive long-term mortality and frequent readmissions. The ICU burden tended to reduce over time after hospital discharge.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
In a national public healthcare system of an emerging country, long-term outcomes of patients admitted to ICUs are poor, with excessive mortality and frequent ICU and hospital readmissions. The burden of critical illness tended to diminish over time after hospital discharge. |
Introduction
Assessing long-term outcomes of critically ill patients has been a relevant subject worldwide as more patients are surviving intensive care [1]. Previous studies presented the huge impact of critical illness on the lives of the patients and their relatives, such as increased mortality after hospital discharge [2,3,4,5], hospital readmissions [6], continuous use of healthcare resources [7, 8], and poor quality of life [9, 10]. Post-ICU mortality seems to be increased during the first few months after ICU and hospital discharge, suggesting that hospital discharge is inaccurate for measuring the impact of critical illness on severe outcomes [7].
Although critical care represent a significant burden on healthcare economics [11], there is still an absence of large multicenter studies that allow national or international comparisons in order to adjust healthcare systems to support the increased demand for critical care and post-ICU care. This lack of data is even more pronounced for emerging countries, which account for more than 50% of the world’s population and face massive demographic and socioeconomic transformation, with increased urbanization, economic development, and population growth [12]. Very few studies have assessed long-term outcomes after ICU discharge in emerging countries. Most of them were single-center [7, 10, 13,14,15] and some were focused on a specific patient population [16]. Nationally representative information is needed to understand the patterns of mortality, morbidity, and healthcare resource use after critical illness to allow for better targeting of follow-up care, especially in the scenario of relative restrained resources of emerging countries. Given this knowledge gap, we developed a study aiming to describe long-term outcomes after ICU discharge, including mortality and hospital readmissions, in a large database of patients assisted by the Brazilian public healthcare system.
Methods
A more detailed description of the methods is available in the Electronic Supplementary Material (ESM).
We performed a retrospective multicenter cohort study aiming to compare the long-term outcomes of patients admitted to ICU or to regular wards of public and private hospitals affiliated to the public healthcare system in Brazil.
This study used two case-based administrative databases: the Hospitalization Information System (Sistema de Informações de Hospitalizações—SIH) database from 2005 to 2010 and the Mortality Information System (Sistema de Informações de Mortalidade—SIM) database from 2005 to 2010. The SIH database comprises about 75% of all hospitalizations in Brazil, as it contains only hospitalizations in hospitals that are vinculated to the National Public Health System (Sistema Único de Saúde—SUS). SIH data are primarily used for reimbursement purposes, so the likelihood of underreported records is small [17]. The SIM data comprise International Classification of Diseases, 10th Edition (ICD-10) codes for the underlying and associated causes of death variables. SIM data have national coverage and represent almost the totality of deaths occurring in Brazil [18, 19].
In order to identify multiple hospitalization records pertaining to the same individuals and to link the hospitalization with the respective mortality records, a three-step process was applied. First, an in-house deterministic record linkage algorithm was done similarly as described to find SIH records of the same patient [20,21,22]. Then, consecutive records of the same patient with an interval of up to 2 days between discharge and readmission were considered as belonging to the same episode of disease. Repeated records of the same episode of disease were discarded. The third step was to link the hospitalization record of each patient with the corresponding mortality record.
We also merged the hospitalization database to the database of the National Registration of Healthcare Facilities (Cadastro Nacional de Estabelecimentos de Saude—CNES) to evaluate the type of hospital during admission (public/private and university/non-university).
Study population
We studied ICU patients aged 15 years or more and a sample of 2 patients from hospital wards (non-ICU) matched to each ICU patient. These patients were admitted to hospitals of nine state capitals and the Federal District in Brazil. Hospitalization records of women for delivery were excluded. ICU patients were considered those with a hospitalization in an ICU in 2006 or 2007 and no ICU admission in the preceding year. Non-ICU controls were those who had a non-ICU hospital admission in the same years and no ICU admission in the preceding year of the ward admission. This initial hospitalization that defined the start of the follow-up period for each patient is hereafter called the index hospitalization.
ICU patients were paired to non-ICU controls by frequency matching in a ratio of 1:2, according to postal code (first 3-digits of the ZIP code) and semester of admission. ZIP code was used as a proxy to socio-economic status [23, 24].
Outcomes
Primary outcome was death to all causes up to 1 year post-discharge. Secondary outcomes were: deaths due to all causes in 30 and 90 days and 3 years after discharge; hospitalizations due to all causes in 30 and 90 days and 1 and 3 years post-discharge. Subsequent hospitalizations after the index hospitalization were ascertained by assessing the several hospitalization records pertaining to the same patient. For patients who had multiple hospitalizations after the index hospitalization, only the first one was considered a study outcome.
Potential confounders and/or effect modifiers
We tested age, gender, cancer diagnosis, type of admission (medical/surgical), university/non-university hospital, and private/public hospital as potential confounders or effect modifiers. Diagnosis of cancer was defined as an ICD-10 code C00–C99 listed as the primary diagnosis of the index hospitalization.
Statistical analysis
Categorical variables were compared using Pearson Chi-square or Fisher exact texts. Continuous variables were compared using Student t tests or the Wilcoxon–Mann–Whitney tests, as appropriate.
Hazard ratios (HRs) were estimated for the outcomes studied using Cox models. Potential confounders and effect modifiers were tested in all models. We assessed confounding by comparing the adjusted and unadjusted HRs for each variable and likelihood ratio tests assessed the contribution of each variable and of interaction terms to the models. The proportional hazards assumption was tested statistically using Schoenfeld residuals and by checking for parallel curves in log–log plots [25]. Kaplan–Meier curves were used to analyze the differences in survival.
A sensitivity analysis was done to compare risks of death and readmission for patients with hospital length of stay (LOS) and ICU LOS divided in less than 2 days and 2 or more days. A significance level was set at 5% (p < 0.05). Statistical analyses were performed using STATA-13 software (Statacorp, College Station, TX, USA).
Ethical issues
Ethical approval for this study was obtained from the Ethical Committee of Hospital Sírio-Libanês, Sao Paulo, Brazil (CAAE: 01063212.1.0000.5461–3, January 2012).
Results
Baseline demographics and hospitalization characteristics
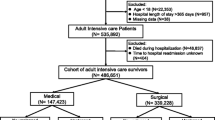
There were 3,259,008 records on SIH database referring to all hospitalization events, as shown on Fig. 1. After exclusion of patients for previous ICU admissions, admissions for deliveries and patients younger than 15 years of age, 1,912,704 records were left in the database from 1,544,780 unique patients, and of these, 108,302 were patients admitted to an ICU. Successful matches were found for 99.9% of the ICU group and the number of non-ICU patients in the study was 216,292.
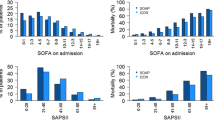
The demographic details of both groups are shown in Table 1. ICU patients were older (56.7 years ±18.4, p < 0.001) and more frequently male. Cardiovascular diseases were the main reported diagnosis for hospital admission in both groups, but more frequent for ICU patients (40.4 vs. 12.6%, p < 0.001). Admissions for medical reasons during the index hospitalization were more frequent than for surgical reasons for both ICU (66.0%) and non-ICU patients (88.9%). Median hospital LOS was higher for ICU patients and hospital mortality at index hospitalization was 18.5% for ICU patients vs. 3.6% for non-ICU patients (p < 0.001).
Long-term outcomes: mortality and readmissions
Up to 1 year after hospital discharge, readmissions were more frequent for ICU patients, considering both ICU and ward readmissions. Table 2 details data on patients readmitted. In the first year after discharge from the index hospitalization, 25.4% of all ICU patients and 17.4% of all non-ICU patients were readmitted in a median interval from first readmission of 81 (35–179) and 123 (49–225) days (p < 0.001), respectively. Patients were readmitted frequently up to 30 days in both groups (21.1 vs. 16.0%, p < 0.001) and patients readmitted to ICU beds represented 31.4% of all ICU patients and 7.3% of all non-ICU patients (Table 2).
Most of the first readmissions had the same diagnosis as the index hospitalization (52.5% for ICU vs. 61.1% for non-ICU patients, p < 0.001). Causes of first readmission are reported in E-table 1 of the ESM. Hospital mortality following the first readmission was 25.5% for ICU patients and 14.9% for non-ICU patients (p < 0.001).
The Kaplan–Meier survival curve of all patients discharged alive from their index hospitalization (88,285 ICU patients and 208,584 non-ICU patients) is shown on Fig. 2. Table 3 shows the overall mortality rate at 1 and 3 months and 1 and 3 years. Mortality rate at one year (primary outcome) was 14.3% for ICU patients and 3.9% for non-ICU patients (Table 3). In the non-adjusted analyses, ICU patients had an increased risk for mortality at all intervals evaluated. Risk of readmission was also higher for ICU patients on the same periods. In the adjusted analyses, a significant interaction was found between surgical status and mortality, so we reported the results stratified by this variable. Risk of mortality and readmission was higher for medical patients as compared to surgical ones in all periods analyzed (Table 3). E-table 2 of the ESM demonstrates the multivariate analysis adjusted for gender, age, cancer, and university/non-university hospital. There was no significant adjustment for the hospital according to public/private type.
The sensitivity analysis according to LOS is reported on E-table 3 of the ESM. In both subgroups (less than 2 days and 2 or more days), ICU patients had increased risk for mortality and readmission in all the periods of observation.
Throughout the study follow-up of 3 years, 60,617 patients died (37,321 ICU patients vs. 23,296 non-ICU patients), and the main causes of death for both groups were cardiovascular diseases (32.5% for ICU patients and 27.6% for non-ICU patients) and cancer (18.4% for ICU patients and 27.3% for non-ICU patients; ESM E-table 4).
Discussion
In this multicenter study, patients discharged from Brazilian ICUs affiliated to the public healthcare system had increased long-term mortality and more frequent ICU and hospital readmissions up to 3 years after discharge as compared to matched pairs admitted to the wards. The burden of ICU admission tends to reduce with time, and patients admitted for medical reasons have increased risk of death and readmission than surgical ones. This study has important implications regarding provision of critical care resources and establishing healthcare policies focusing on early rehabilitation for reducing post-discharge ICU burden.
Research into context
Our study adds evidence to the literature that demonstrates increased mortality and healthcare resource utilization after hospital discharge of an ICU admission [8, 26]. Admission to the ICU resulted in elevated mortality rates during the entire study follow-up, starting with 18.5% at the index hospitalization, 9.7% up to 90 days, and 14.3% within 1 year for those that survived the index hospitalization. Population-based studies in developed countries found similar mortality rates of critically ill patients being 13–19% [2, 4, 11], while single-center studies from Brazil and Thailand demonstrated higher hospital mortalities of 33 and 44%. These discrepant numbers could be possibly explained by different case mix, since both studies were done in large regional tertiary hospitals [7, 13]. Regarding long-term mortality, our study identified an increased risk of death occurring up to 90 days after hospital discharge. This is in accordance with previous studies indicating that the effect of an acute illness reduces over time after discharge [7, 8, 27, 28]. In a single-center Brazilian study, Ranzani et al. identified that residual organ dysfunction at ICU discharge is related to increased healthcare resource use and predominant early mortality [7]. Accordingly, Garland et al. suggested that major determinants of mortality up to 90 days are related to acute illness, while late unfavorable outcomes are more associated with age and comorbidities [27]. Unfortunately, as neither organ dysfunction nor comorbidities were available in our secondary databases, we cannot clarify their impact on these results.
We reported that 25.4% of ICU patients were readmitted to a hospital facility in the first year after discharge and this readmission rate is lower than other studies. Data from previous studies identified readmission rates of 37% from Brazil [7], 41% from Canada [6], and 36.1% for a US Medicare-assisted population [2]. Since we could not obtain disease severity scores and comorbidities data, it is difficult to explain these discrepancies. Moreover, we found higher hospital mortality at the first readmission (25.5% for ICU patients and 14.9% for non-ICU patients) and a significant number (31.4%) of ICU patients that required again an ICU admission at rehospitalization. These numbers are in contrast with previous studies that identified 10.4% of ICU readmission in the subsequent year from ICU discharge [6]. Such events of readmission, critical care resource use, and high mortality after 1 year might be the result of premature discharges, limited access for post-hospitalization services, or both.
Strengths and limitations
A major strength of our study is its multicenter nature with a large number of patients included, which is not common in studies from a developing country. Moreover, our robust statistical methodology was able to adequately match ICU and non-ICU patients to evaluate their long-term mortality and resource use. ZIP code was used as a proxy for socio-economic status and semester of admission to allow for the groups to have a similar follow-up period. Linkage of national healthcare registries provided a more complete, national picture of longer-term outcomes for ICU survivors. Comparing ICU survivors to matched hospital cohorts also provides a method of exploring the magnitude of excess mortality and healthcare resources associated with ICU survivorship and identifying patients at greatest risk [8].
However, our study has several limitations. First, the hospitalization information system database is collected only for administrative and reimbursement purposes. While it provides a national representative picture from the public healthcare system, it does not have important information regarding functional status, comorbidities, or disease severity. Especially for comorbidities, the lack of data did not allow us to adjust our model for pre-illness potential trajectory. So, the long-term outcomes measured here may be more the result of severe chronic diseases than the impact of critical illness. Second, due to SIH characteristics, the cause of admission described in this study is related to hospital admission and not specifically ICU admission. This may be associated with coding issues, as demonstrated for instance by the low percentage of sepsis admissions in our subgroup of ICU patients.
Another limitation was that our matching strategy was only based on admission semester and ZIP code. Another possible matching approach would be to compare ICU and non-ICU patients according to the other variables like age, gender, and LOS. Even though this last strategy would allow more adequate group comparisons than the one used, in a context of few data characterization parameters available, such as in our database, using these clinical variables for matching would not allow us to study their effects on the outcomes and would reduce the number of patients for analysis, as not all ICU cases would have their correspondent controls. Also, as 25% of the non-ICU matched patients had only 1 day of hospital stay, our results may have been influenced towards uncomplicated patients in the non-ICU arm, since these short-stay patients add very little to the post-discharge burden. However, maintaining these patients in the cohort increases the generalizability of our findings, and our sensitivity analysis using a cutoff for LOS of 2 days corroborated the main results. As a retrospective study using an administrative database with limited patient data, our model is indeed not able to correct for unmeasured confounders even with the matching and model adjustments for the available confounders and interactions. The model only claims to provide an association, not a causal relationship.
Also, some of our patients’ readmissions may have been missed because this database only comprises hospitalizations in hospitals that are public or private but associated with the National Public Health System. Some deaths may also have been missed because the linkage procedures used, despite previously demonstrated good performances when used in similar databases, do not have 100% sensitivity and specificity. In addition, although we collected data from major state capitals comprising all regions of the country, we do not know the outcomes of ICU patients admitted to countryside hospitals. Moreover, these administrative databases did not contain information on post-ICU quality of life and functional status, which would allow a more complete understanding of the long-term consequences of critical illness. Finally, we were not able to compare ICU and non-ICU patients with the general Brazilian population of similar age and gender.
Conclusions
In a national public healthcare system of a developing country, long-term outcomes of patients admitted to ICUs are poor, with excessive mortality and frequent ICU and hospital readmissions. The burden of critical illness tends to reduce over time after hospital discharge.
References
Angus DC, Carlet J, Brussels Roundtable P (2003) Surviving intensive care: a report from the 2002 Brussels Roundtable. Intensive Care Med 29:368–377
Wunsch H, Guerra C, Barnato AE, Angus DC, Li G, Linde-Zwirble WT (2010) Three-year outcomes for Medicare beneficiaries who survive intensive care. JAMA 303:849–856
Wright JC, Plenderleith L, Ridley SA (2003) Long-term survival following intensive care: subgroup analysis and comparison with the general population. Anaesthesia 58:637–642
Hill AD, Fowler RA, Pinto R, Herridge MS, Cuthbertson BH, Scales DC (2016) Long-term outcomes and healthcare utilization following critical illness–a population-based study. Crit Care 20:76
Niskanen M, Kari A, Halonen P (1996) Five-year survival after intensive care–comparison of 12,180 patients with the general population. Finnish ICU Study Group. Crit Care Med 24:1962–1967
Garland A, Olafson K, Ramsey CD, Yogendran M, Fransoo R (2015) A population-based observational study of intensive care unit-related outcomes. With emphasis on post-hospital outcomes. Ann Am Thorac Soc 12:202–208
Ranzani OT, Zampieri FG, Besen BA, Azevedo LC, Park M (2015) One-year survival and resource use after critical illness: impact of organ failure and residual organ dysfunction in a cohort study in Brazil. Crit Care 19:269
Lone NI, Gillies MA, Haddow C, Dobbie R, Rowan KM, Wild SH, Murray GD, Walsh TS (2016) Five-year mortality and hospital costs associated with surviving intensive care. Am J Respir Crit Care Med 194:198–208
Haas B, Wunsch H (2016) How does prior health status (age, comorbidities and frailty) determine critical illness and outcome? Curr Opin Crit Care 22:500–505
Haas JS, Teixeira C, Cabral CR, Fleig AH, Freitas AP, Treptow EC, Rizzotto MI, Machado AS, Balzano PC, Hetzel MP, Dallegrave DM, Oliveira RP, Savi A, Vieira SR (2013) Factors influencing physical functional status in intensive care unit survivors two years after discharge. BMC Anesthesiol 13:11
Wunsch H, Angus DC, Harrison DA, Linde-Zwirble WT, Rowan KM (2011) Comparison of medical admissions to intensive care units in the United States and United Kingdom. Am J Respir Crit Care Med 183:1666–1673
Soares M, Bozza FA, Angus DC, Japiassu AM, Viana WN, Costa R, Brauer L, Mazza BF, Correa TD, Nunes AL, Lisboa T, Colombari F, Maciel AT, Azevedo LC, Damasceno M, Fernandes HS, Cavalcanti AB, do Brasil PE, Kahn JM, Salluh JI (2015) Organizational characteristics, outcomes, and resource use in 78 Brazilian intensive care units: the ORCHESTRA study. Intensive Care Med 41:2149–2160
Luangasanatip N, Hongsuwan M, Lubell Y, Limmathurotsakul D, Teparrukkul P, Chaowarat S, Day NP, Graves N, Cooper BS (2013) Long-term survival after intensive care unit discharge in Thailand: a retrospective study. Crit Care 17:R219
Fildissis G, Zidianakis V, Tsigou E, Koulenti D, Katostaras T, Economou A, Baltopoulos G (2007) Quality of life outcome of critical care survivors eighteen months after discharge from intensive care. Croat Med J 48:814–821
Miranda AF, Miranda S (1991) Quality of life and longterm survival after intensive care discharge. Med J Malaysia 46:66–71
Normilio-Silva K, de Figueiredo AC, Pedroso-de-Lima AC, Tunes-da-Silva G, da Silva AN, Levites ADD, de-Simone AT, Safra PL, Zancani R, Tonini PC, de Andrade ESUV, Silva TB, Giorgi JM, Eluf-Neto J, Costa A, Hajjar LA, Cavalcanti AB (2016) Long-term survival, quality of life, and quality-adjusted survival in critically ill patients with cancer. Crit Care Med 44:1327–1337
Bittencourt SA, Camacho LA, Leal Mdo C (2006) Hospital information systems and their application in public health. Cad Saude Publica 22:19–30
Jorge MH, Laurenti R, Di Nubila HB (2010) Death and its epidemiological investigation: considerations about some relevant aspects. Rev Bras Epidemiol 13:561–576
Taniguchi LU, Bierrenbach AL, Toscano CM, Schettino GP, Azevedo LC (2014) Sepsis-related deaths in Brazil: an analysis of the national mortality registry from 2002 to 2010. Crit Care 18:608
Pacheco AG, Saraceni V, Tuboi SH, Moulton LH, Chaisson RE, Cavalcante SC, Durovni B, Faulhaber JC, Golub JE, King B, Schechter M, Harrison LH (2008) Validation of a hierarchical deterministic record-linkage algorithm using data from 2 different cohorts of human immunodeficiency virus-infected persons and mortality databases in Brazil. Am J Epidemiol 168:1326–1332
Azevedo LC, Toscano CM, Bierrenbach AL (2013) Bacterial Meningitis in Brazil: baseline epidemiologic assessment of the decade prior to the introduction of pneumococcal and meningococcal vaccines. PLoS One 8:e64524
Oliveira GP, Bierrenbach AL, Camargo KRJ, Coeli CM, Pinheiro RS (2016) Accuracy of probabilistic and deterministic record linkage: the case of tuberculosis. Rev Saude Publica 50:49
Guiltinan AM, Kaidarova Z, Custer B, Orland J, Strollo A, Cyrus S, Busch MP, Murphy EL (2008) Increased all-cause, liver, and cardiac mortality among hepatitis C virus-seropositive blood donors. Am J Epidemiol 167:743–750
Fiscella K, Franks P (2001) Impact of patient socioeconomic status on physician profiles: a comparison of census-derived and individual measures. Med Care 39:8–14
Venables WN, Ripley BD (2002) Modern Applied Statistics With S. Springer, New York
Needham DM, Davidson J, Cohen H, Hopkins RO, Weinert C, Wunsch H, Zawistowski C, Bemis-Dougherty A, Berney SC, Bienvenu OJ, Brady SL, Brodsky MB, Denehy L, Elliott D, Flatley C, Harabin AL, Jones C, Louis D, Meltzer W, Muldoon SR, Palmer JB, Perme C, Robinson M, Schmidt DM, Scruth E, Spill GR, Storey CP, Render M, Votto J, Harvey MA (2012) Improving long-term outcomes after discharge from intensive care unit: report from a stakeholders’ conference. Crit Care Med 40:502–509
Garland A, Olafson K, Ramsey CD, Yogendran M, Fransoo R (2014) Distinct determinants of long-term and short-term survival in critical illness. Intensive Care Med 40:1097–1105
Prescott HC, Osterholzer JJ, Langa KM, Angus DC, Iwashyna TJ (2016) Late mortality after sepsis: propensity matched cohort study. BMJ 353:i2375
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
de Lima, V.C.B.F., Bierrenbach, A.L., Alencar, G.P. et al. Increased risk of death and readmission after hospital discharge of critically ill patients in a developing country: a retrospective multicenter cohort study. Intensive Care Med 44, 1090–1096 (2018). https://doi.org/10.1007/s00134-018-5252-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-018-5252-3