Abstract
Purpose
To assess the impact of 6 % tetrastarch [hydroxyethyl starch (HES) 130/0.4 and 130/0.42] in severe sepsis patients. The primary outcome measure was 90-day mortality.
Methods
A structured literature search was undertaken to identify prospective randomised controlled trials (RCTs) in adult patients with severe sepsis receiving 6 % tetrastarch (of potato or waxy maize origin) as part of fluid resuscitation in comparison with other non-HES fluids after randomisation in the critical care setting. A systematic review and meta-analysis were performed.
Results
Six RCTs were included (n = 3,033): three from 2012 (n = 2,913) had low risk of bias. Median tetrastarch exposure was 37.4 ml/kg (range 30–43 ml/kg). Ninety-day mortality was associated with tetrastarch exposure [relative risk (RR) 1.13; 95 % confidence interval (CI) 1.02–1.25; p = 0.02] compared with crystalloid. The number needed to harm (NNH) was 28.8 (95 % CI 14.6–942.5). Publication bias and statistical heterogeneity (I 2 = 0 %) were not present. Tetrastarch exposure was also associated with renal replacement therapy (p = 0.01; NNH 15.7) and allogeneic transfusion support (p = 0.001; NNH 9.9). No difference between groups was observed for 28-day mortality, for comparison with colloid as control, or for waxy maize-derived tetrastarch, but power was lacking. Overall mortality was associated with tetrastarch exposure (RR 1.13; 95 % CI 1.02–1.25; p = 0.02).
Conclusions
In our analysis, 6 % tetrastarch as part of initial fluid resuscitation for severe sepsis was associated with harm and, as alternatives exist, in our view should be avoided.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hydroxyethyl starch (HES) solutions are in widespread use worldwide as a colloid to maintain or achieve volume expansion, with resuscitation of critically ill patients with severe sepsis a major indication [1, 2].
Specification of HES has evolved to 6 % tetrastarch, launched in Germany in 1999 and licenced in the USA in 2008. Tetrastarch (6 %) products have average molecular weight of 130 kDa (±20 kDa), and somewhat overlapping molar substitution [3] (the number of hydroxyethyl groups per glucose molecule) of 0.38–0.45 (hence the term “tetrastarch”), often abbreviated as 6 % HES 130/0.4 or 130/0.42. Starch preparations of waxy maize or potato origin are available in various crystalloid carrier solutions. They differ in terms of C2/C6 pattern of hydroxyethylation. It is currently unclear if these chemical differences are of clinical significance. Despite widespread clinical use, the safety and efficacy of HES are controversial [4–7].
Large critical care randomised controlled trials (RCTs) in severe sepsis reporting harm from HES [8, 9], concern over publication bias supporting HES [5, 6] and retraction of studies have raised safety and efficacy concerns [4, 10–12]. Tetrastarch (6 %) products were studied in eleven retracted papers [13]; however, severe sepsis patients were not the main study population in these. A meta-analysis of 6 % tetrastarch use in severe sepsis is lacking, and might address safety and efficacy.
Meta-analyses focussing on mortality associated with 6 % tetrastarch [5, 13] and other HES formulations [14, 15], in various clinical groups and settings, have failed to confirm adequate safety or efficacy. Most of the studies pooled were small, clinically and statistically heterogeneous and not designed to assess mortality. Their short follow-up (often hours to a few days) and low mortality rate mean that type II error from low power is a major concern [16]. Variable length of follow-up may partly explain the high heterogeneity in overall mortality. Studies comparing 6 % tetrastarch versus older higher-molecular-weight HES solutions are unsatisfactory for assessment of relative safety or efficacy [17–21] compared with non-HES solutions.
Patients with severe sepsis have high mortality of 24–39 % at 28 days, and 33–50 % at 90 days [22–24]. Ninety-day mortality was the primary outcome in the 2012 6S [25] and CHEST [3] trials that compared 6 % tetrastarch versus crystalloid control fluid. The 6S study [25] (n = 798) reported harm at 90 days (p = 0.03) [25], and CHEST [3] no difference overall (n = 7,000), or in the sepsis sub-group (n = 1,937), at 28 and 90 days. The CHEST mortality rate and power were lower than those of 6S, and the number of patients with severe sepsis or septic shock was not reported. However, persistent separation of Kaplan–Meier survival curves occurs between 5 and 15 days [3, 25, 26].
To assess safety and efficacy, international consensus recommends 90-day mortality as the primary outcome measure in all sepsis studies [27]. Hence, we conducted a systematic review and meta-analysis to examine whether administration of 6 % tetrastarch as compared with other non-HES fluids was associated with 90-day mortality in critically ill patients with severe sepsis. Other outcomes assessed were 28-day and overall mortality, requirement for renal replacement therapy, and allogeneic transfusion support.
Materials and methods
Objectives
Our objective is to use the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [28] statement methodology to conduct a systematic review and meta-analysis of randomised clinical trials to determine whether 6 % tetrastarch consistently differs from control non-HES fluid regimens in its effects upon mortality. The primary outcome measure was 90-day mortality [27]. The secondary outcome measure was overall mortality at final follow-up [27]. Post hoc sub-groups were explored for these outcome measures: by type of control fluid (colloid or crystalloid), tetrastarch origin (potato or waxy maize) and C2/C6 hydroxyethylation ratio (6:1 or 9:1). Tertiary outcome measures were 28-day mortality, renal support [renal replacement therapy (RRT)], acute kidney injury according to creatinine-based Risk, Injury, Failure, Loss, End-Stage (RIFLE) [29] categories, allogeneic transfusion support and adverse events.
Identification of studies
A literature search of PubMed, PubMed Central, Web of Science (includes MEDLINE), OvidSP (includes EMBASE, Ovid MEDLINE), the Cochrane Library, clinicaltrials.gov and controlled-trials.com was undertaken on 1 November 2012. The terms used were “sepsis” with all of the following: “hydroxyethylstarch”, “HES”, “hydroxy ethyl starch”, “hydroxy ethylstarch”, “starch”, “130/0.4”, “tetrastarch”, “Tetraspan”, “Voluven”, “HES”. No language or date restrictions were applied. Reference lists of evaluable studies, systematic reviews, meta-analyses and reports were also hand-searched for additional studies eligible for inclusion. Grey literature was also sought [30] through supplementary material published online, including international drug data sheets. For included studies, if patients were in a pre-defined sub-group, we made efforts to contact the corresponding author for clarification and additional data.
Screening of studies
Two reviewers independently screened the initially identified studies from the search. Full-text articles of potentially eligible studies were independently assessed against the eligibility criteria. For each study, data extraction and appraisal of internal validity were undertaken independently. Disagreements between the two reviewers were resolved in meetings or referred to the third reviewer for resolution.
Eligibility criteria
All of the following criteria were met for inclusion of a study:
-
1.
Prospective randomised clinical trial;
-
2.
Reporting on adult human subjects (18 years or older);
-
3.
Critical/intensive care unit setting;
-
4.
Trial, or pre-defined sub-group, focussed on patients diagnosed with severe sepsis [31] present at randomisation;
-
5.
Fluid therapy was administered for volume expansion after randomisation;
-
6.
At least one exposure group that received 130 kDa 6 % tetrastarch (in any carrier or of any origin or of any molar substitution or hydroxyethylation) after randomisation;
-
7.
At least one control exposure group that received any non-HES fluid (crystalloid or colloid) after randomisation;
-
8.
Reporting of a mortality outcome at 90 days, and/or 28 days, and/or another follow-up time point;
-
9.
At least one death in each of the 6 % tetrastarch and control exposure groups (to facilitate meta-analysis).
Data extraction
Data from the longest complete follow-up was defined as overall mortality [27]. Data on the following study characteristics were collected: clinical setting, number of randomised patients, number of patients with severe sepsis, time of final follow-up, proportion of patients present at follow-up (data completeness) and primary end-point. When mortality was reported at different follow-up intervals, data from the longest complete follow-up was used along with 28- and 90-day values [27]. All-cause death in the control group was used as a measure of baseline mortality for each study. Sufficient data were collected to calculate observed study power [32–34] for the end-point of mortality at final follow-up.
The overall sepsis management protocol used was recorded. Details of baseline patient characteristics by group were also collected: age, sex, marker of disease severity [Acute Physiology and Chronic Health Evaluation (APACHE) II)] [35] or organ dysfunction [Sequential Organ Failure Assessment (SOFA)] [36], and an estimate of septic shock (and/or use of vasopressors or inotropes) [27, 31].
Data related to study fluid exposure were collected. This included days of trial fluid exposure, type of trial and control group fluid, prescribed fluid dose and actual dose administered (total and daily trial fluid). Details of RRT support, RIFLE criteria [29] components and allogeneic transfusion support by group were also collected. Information on reported adverse effects, such as pruritus, was also sought. Values were calculated if not stated, and means or medians were accepted if reported. Infused doses of intervention and control fluids were extracted and normalised for a 70-kg person in ml/kg or ml/kg/day to allow comparison between studies.
For studies with greater than one control exposure group, a single non-HES-containing comparator was selected, with preference given to crystalloid, then colloid. Remaining control groups were not included in the pooled analysis. Retracted studies were excluded [10, 11, 13].
Quality assessment
Study quality and bias risk of individual studies and across studies were assessed using the Cochrane Collaboration tool [37]. Studies at high risk of bias were included unless full evaluation was not possible for any reason, including lack of an English-translated version of a publication. A funnel plot was used to determine publication bias.
Statistical analysis
The primary outcome summary measure was relative risk (RR) of 90-day mortality. The secondary outcome measure was RR of overall mortality. Post hoc sub-groups were 6 % tetrastarch hydroxyethylation ratio/starch origin and type of control fluid for these two outcome measures. Tertiary outcome measures were RR of 28-day mortality, RR of RRT, RR of allogeneic transfusion and RR of pruritus.
The RR of death for 6 % tetrastarch compared with control fluid was calculated for each included study. Then, the pooled RR of studies and their 95 % confidence intervals (CI) were calculated. Statistical heterogeneity was assessed using the chi2 test (Cochran Q) and I 2 statistic [38]. I 2 values of 25, 50 and 75 % were considered as low, moderate and high [39]. A random-effects model was used in the presence of statistical heterogeneity (tau2 was reported as another measure of statistical heterogeneity; >1 suggests heterogeneity). Clinical heterogeneity (as judged by two reviewers) could not be excluded, so the more conservative random-effects model [40] (Mantel–Haenszel method) was used.
Sensitivity analysis was performed by excluding studies with high risk of bias, and also by using a fixed-effects model. Sensitivity analyses with or without CHEST data were performed where appropriate because it was unclear if the reported pre-defined sepsis group represented only patients with severe sepsis. Studies in forest plots are presented sorted by effect size. RevMan version 5.1.7 (Java 6), build 04/06/12 for Mac was used for analysis. Observed or post hoc power (at 95 % CI without continuity correction) calculations were performed with OpenEpi version 2.3, May 2009. Number needed to harm (NNH) or treat was calculated as the reciprocal of the absolute risk reduction with 95 % CIs, if it was statistically significant, with an online calculator (clinicalevidence.bmj.com). Simple calculations, including means and medians, were derived with Microsoft Excel for Mac version 14.2.4.
Results
Literature search and study selection
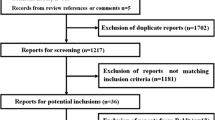
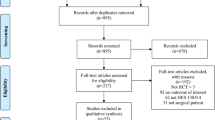
Figure 1 outlines a PRISMA [28] flow diagram illustrating the results of the literature search. Six RCTs [3, 25, 26, 41–43] published between July 2006 and October 2012 met the eligibility criteria and were included in this meta-analysis. They described adults suffering from severe sepsis in the critical care setting, and reported overall mortality in patients exposed to 6 % tetrastarch and a non-HES control fluid after randomisation for volume resuscitation. Four reports [44–47] were excluded because of inadequate information or because an English translation was not available for full appraisal. Their abstracts did not suggest that they reported our primary outcome measure of 90-day mortality. They were also not included by previous reviewers in their meta-analyses [5, 13].
A Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [28] flow diagram detailing the search, identification, screening and inclusion of RCTs assessed in this systematic review and meta-analysis
Study quality and bias
Assessment of within-study bias (internal validity) is summarised in Fig. 1 (online supplement). The three trials reporting 90-day mortality were of good quality and had low risk of bias. The 6S [25] and CHEST [3] trials were specifically designed to assess 90-day mortality (Table 1). The three [41–43] older, smaller trials reporting mortality at other time points had risk of performance and detection bias, two had risk of selection bias [42, 43], one had risk of attrition bias [41], while another had risk of reporting bias [42]. They were not designed to assess mortality, and the possibility of ascertainment bias could not be dismissed. Furthermore, information from other sources [14, 48] was required because of missing data.
The assessment of bias risk across studies (external validity) is shown in Fig. 2 (online supplement). Overall risk of bias for the studies reporting our primary endpoint was low. The risk of selection bias was a major concern in studies not reporting 90-day mortality, where performance, attrition and other risks of bias were also evident. Figure 3 (online supplement) shows a funnel plot assessment that does not yield very clear evidence of publication bias relating to the six included studies. Trial design and clinical heterogeneity were evident mainly for studies not reporting 90-day mortality.
Description of studies and patients
The study characteristics extracted from the RCTs included are outlined in Table 1. Four [3, 25, 26, 43] of the six were multicentre, and randomised 3,033 patients in critical/intensive care units across Europe, Australasia and South America. Five trials recruited patients with severe sepsis [25, 26, 41–43]. The largest trial [3] recruited sepsis patients in a pre-defined sub-group [49], but those with severe sepsis or septic shock were not reported separately. The median sepsis study sample size was 126 patients (range 24–1,937). Completeness of overall mortality outcome data was 99.3 % (n = 3,013). The median baseline mortality assessed in the control group was 31.9 % (range 13–54 %). The overall median observed study power for mortality was only 15.7 % (range 6.4–56.5 %).
Baseline patient characteristics are outlined in Table 1 (online supplement). The mean age of patients exposed to 6 % tetrastarch was 63.1 years (range 43–66 years), and 65 years (range 47–67 years) in the control groups. Male patients represented a median 64 % in the 6 % tetrastarch groups (range 60–85 %) compared with 60 % in the control groups (range 55–87 %). Only one [41] of the six studies reported a SOFA or APACHE II score in the 6 % tetrastarch group that was greater than that in the control group; it was equal in two studies [3, 25]. A summary measure was not possible because of varied reporting. The proportion of patients with septic shock or those who required vasopressors or inotropes (these were interchangeably reported, often as a composite and variably defined) in four RCTs [25, 26, 41, 43] was 86.0 % (range 46–100 %) in 6 % tetrastarch groups and 87.5 % in control groups, as shown in Table 1 (online supplement). CHEST trial [3] data for their sepsis group were not available.
Tetrastarch (6 %) exposure
Sepsis management protocols used in the RCTs and details of 6 % tetrastarch product and crystalloid or albumin control fluid are outlined in Table 2 (online supplement). Patients were exposed to study fluids for a median of 3.5 days (range 1–5 days). Four studies [3, 25, 26, 41] reported pre-defined 6 % tetrastarch dosing details. Five studies [3, 25, 26, 41, 43] reported a median total 6 % tetrastarch volume infusion of 2,615 ml (range 1,379–3,000 ml). The median actual 6 % tetrastarch dose exposure was 37.4 ml/kg (range 30–43 ml/kg) or 14 ml/kg/day (range 8–37 ml/kg/day).
Primary outcome: 90-day mortality
Three RCTs [3, 25, 50] reporting in 2012 (n = 2,913) presented follow-up data to 90 days, the primary outcome measure to assess safety and efficacy. Figure 2 shows the excess mortality found in patients exposed to 6 % tetrastarch (RR 1.13, 95 % CI 1.02–1.25; p = 0.02). The NNH was 28.8 (95 % CI 14.6–942.5). Statistical heterogeneity was not present (I 2 = 0 %; χ 2 0.81, p = 0.67; τ2 0.00). Sensitivity analysis performed by removing studies with risks of bias did not change this mortality difference (RR 1.13, 95 % CI 1.02– 1.25; p = 0.02), nor did the use of a fixed model (RR 1.12, 95 % CI 1.01–1.25; p = 0.03). Exclusion of data from CHEST did not alter the finding of 6 % tetrastarch-associated mortality (RR 1.18, 95 % CI 1.03–1.35; p = 0.02), as shown in Fig. 4a (online supplement). Post hoc sub-group analysis by control fluid type did not alter this association, as crystalloid was used for all three studies. Analysis by C2/6 hydroxyethylation ratio and starch origin is presented in Fig. 4b (online supplement).
Secondary outcome: overall mortality
Overall mortality was increased in patients exposed to 6 % tetrastarch (RR 1.13, 95 % CI 1.02–1.25; p = 0.02). The NNH was therefore 29.2 (95 % CI 14.9–896.7). Statistical heterogeneity was not present (I 2 = 0 %; χ 2 3.49, p = 0.62; τ2 0.00). Sensitivity analysis performed by removing studies with risk of bias from the analysis did not significantly change the finding of 6 % tetrastarch-associated mortality (RR 1.13, 95 % CI 1.02–1.25; p = 0.02). Also, use of a fixed model (RR 1.12, 95 % CI 1.01–1.24; p = 0.03) or exclusion of the CHEST data [3] yielded the same outcome (RR 1.17, 95 % CI 1.02–1.34; p = 0.02). Figure 3 shows the post hoc sub-group analyses of overall mortality by type of control fluid received, and Fig. 5 (online supplement) by 6 % tetrastarch origin/pattern of C2 to C6 hydroxyethylation.
Forest plot assessing the RR of overall mortality, the secondary outcome measure, assessed at last follow-up. Observed power was 52.6 %. Post hoc sub-groups of control group fluid type are shown. The observed power in the crystalloid control sub-group was 46.6 %, and median baseline mortality was 38.4 % (range 23.7–53.8 %). In the colloid sub-group these were 18.6 % and 21.7 %, respectively (Table 1)
Tertiary outcome 1: 28-day mortality
In this group (n = 1,049), a mortality difference between 6 % tetrastarch and control was not detected in three trials [25, 26, 41], as shown in Fig. 4. Statistical heterogeneity was not present, and sensitivity analyses performed by removing studies with risk of bias (RR 1.10, 95 % CI 0.93–1.30; p = 0.28) or by using a fixed-effects model (1.11, 95 % CI 0.94–1.31; p = 0.21) did not alter the finding of possible harm or benefit. The CHEST trial [3] did not report 28-day mortality for their pre-defined sepsis group. For illustrative purposes, Fig. 6 (online supplement) shows inclusion of CHEST [3] data (n = 6,644) for enrolled patients in all sub-groups, but this did not alter the outcome.
Tertiary outcome 2a: renal replacement therapy (RRT) support
In two studies [25, 26] (n = 994), a median of 21.4 % of patients in the 6 % tetrastarch group (range 21.0–21.9 %) and 13.9 % in the control group (range 11.5–16.3 %) received RRT (Table 3, online supplement). Figure 5 demonstrates that the requirement for RRT with 6 % tetrastarch exposure was increased (RR 1.41, 95 % CI 1.08–1.84; p = 0.01) compared with control fluid. The NNH was 15.7 (95 % CI 8.9–64.4). Statistical heterogeneity was not present. Sensitivity analysis performed by removing studies with risk of bias did not alter this finding (RR 1.41, 95 % CI 1.08–1.84; p = 0.01), nor did the use of a fixed model (RR 1.42, 95 % CI 1.09–1,855; p = 0.01). The CHEST trial [3] reported this outcome as a composite of both sepsis and non-sepsis patients. For illustrative purposes, Fig. 7 (online supplement) shows that including the CHEST [3] data (n = 6,727) for enrolled patients in all sub-groups did not alter the overall finding.
Tertiary outcome 2b: acute kidney injury severity (RIFLE criteria)
Acute kidney injury severity defined by the RIFLE criteria for severe sepsis patients was reported in two studies [25, 26] using a creatinine-based score, which was thus used for analysis. Table 4a (online supplement) shows that no difference was detected between groups in each RIFLE category, hence one cannot rule out the possibility of harm or benefit with 6 % tetrastarch compared with control fluid, which was crystalloid. Sensitivity analyses by removing studies with risk of bias or by using a fixed model did not alter this overall finding or for any of the RIFLE components. Table 4b (online supplement) shows for illustrative purposes the inclusion of creatinine-based RIFLE data from the CHEST trial [3], including both sepsis and non-sepsis patients. Tetrastarch (6 %) exposure was associated with RIFLE-I and RIFLE-F, but not with RIFLE-R or the two clinical outcome components RIFLE-L and RIFLE-E. Sensitivity analyses performed by removing studies with risk of bias or by using a fixed model did not alter these findings.
Tertiary outcome 3: allogeneic transfusion
The median proportion of patients who received allogeneic transfusion in the 6 % tetrastarch group in three studies [25, 43, 50] (n = 972) was 29 % (range 22–65 %) compared with 21 % (range 18–54 %) in the control group (Table 3, online supplement). Figure 6 demonstrates the increased RR of allogeneic transfusion in patients exposed to 6 % tetrastarch (RR 1.21, 95 % CI 1.08–1.36; p = 0.001) compared with control fluid, which were crystalloid. The NNH was 9.9 (95 % CI 6.1–26.1). Statistical heterogeneity was not present. Sensitivity analysis performed by excluding the study with risk of bias [43] did not alter the conclusion (RR 1.21, 95 % CI 1.08–1.36; p = 0.001), nor did the use of a fixed-effects model (RR 1.22, 95 % CI 1.08–1.37; p = 0.0009). In three RCTs [25, 26, 42] this corresponded to a median transfusion volume of 1,340 ml (range 214–1,500 ml) in the 6 % tetrastarch group compared with 1055 ml (range 165–1400 ml) in the control group (Table 3, online supplement). The CHEST trial did not report these outcomes in their sepsis sub-group.
Tertiary outcome 4: pruritus
Pruritus was reported in two studies [3, 26] (CHEST reported this for all randomised patients) and was associated with 6 % tetrastarch exposure (RR 1.81, 95 % CI 1.37–2.38; p = < 0.00001). Observed power was 99.0 %, and NNH was 56.1 (95 % CI 38.6–102.9). Statistical heterogeneity was not present (I 2 = 0 %; χ 2 = 0.64, p = 0.42; τ2 = 0.00). Sensitivity analysis with a fixed model did not alter this conclusion or any of the statistical values. Other reported adverse events were reported in included studies, but these were not amenable to pooled summary.
Discussion
This meta-analysis has found that mortality in severe sepsis patients is associated with exposure to 6 % tetrastarch products in the critical care setting (Fig. 3; Fig. 5 online supplement). This excess mortality was identified at 90 days (Fig. 2), the primary outcome measure [27]. The point estimates are concordant and the 95 % CI is more precise than in the 6S trial [25]. The results are generalizable to critical/intensive care patients but may not apply to perioperative or trauma patients, in whom 6 % tetrastarch is used and has also been studied. In our analysis, 6 % tetrastarch is neither safe or efficacious: overall or at 90 days, one patient died for every 29 patients treated with 6 % tetrastarch products instead of control fluid.
This analysis was performed promptly when new data were published in 2012 adding significant individual study power (Table 1), and therefore updates previous meta-analyses of 6 % tetrastarch for various indications, which were unable thus far to address long-term safety and efficacy concerns [5, 13, 14]. The addition of the 6S [25] and CHEST [3] trials add 90 % of the weight in this analysis that focusses on sepsis to address the clear knowledge gap of existing data identified by the ESICM Task Force committee [7].
The post hoc sub-group analysis of 6 % tetrastarch origin was unsurprisingly not statistically significant for C2/C6 9-ratio waxy maize products, given the low power of 20.7 % and the median baseline 90-day and overall mortality of 28.7 % and 30 %, respectively. However, generally concordant point estimates towards possible harm were found (Figs. 4b and 5, online supplement). The 6S trial [25] was the only 6-ratio potato-derived 6 % tetrastarch study associated with harm and has already been published [25]. The 9-ratio product is 98 % amylopectin, persists in the intravascular space for longer because of reduced susceptibility to plasma amylase degradation, has lower viscosity compared with the 6-ratio product, which is 75 % amylopectin and 25 % amylose, and is more prone to form inclusion complexes with several endogenous lipophilic molecules [51]. For both, storage in the reticulo-endothelial system and eventual conversion to water and CO2 occurs. Furthermore, the mean degree of molar substitution is 0.42 for the potato- and 0.4 for the waxy maize-derived products [51], but when the latter was measured in CHEST it was 0.44 (Table 2, online supplement) [3]. Thus, it is unclear if these chemical differences between 6 % tetrastarches, particularly with different plasma amylase levels [52], are clinically important. However, harm is associated with their exposure in severe sepsis (Figs. 2 and 3), perhaps predicted by similar degrees of tissue uptake compared with older, higher-molecular-weight HES preparations [53].
Risk of bias in the large, 2012 studies assessing 90-day mortality was low, and study quality was good. Most patients were from this group (97.6 % weight), the control fluid was crystalloid (Table 2, online supplement) and the robust pooled results were unaffected by sensitivity analyses (Fig. 4a, online supplement). The CHEST sepsis sub-group was not clearly described in the original report [3] and there were some missing data, but this did not affect the pooled mortality, RRT or allogeneic transfusion outcomes in our analysis. Pruritus was assessed in all CHEST patients, as this is not necessarily an adverse event specific to sepsis. A detailed sepsis analysis is awaited from the CHEST group (J Myburgh, personal communication), but patients with septic shock may have been underrepresented given the low baseline mortality (Table 1). Tetrastarch (6 %)-associated mortality was found in the pooled crystalloid sub-group (Fig. 3). Ambiguity remains about relative safety in the underpowered albumin sub-group, but the point estimates were also concordant with 6 % tetrastarch-associated harm. There were risks of bias in the three smaller, older trials (Figs. 1 and 2, online supplement). Their primary end-points were not focussed on mortality, data were missing and they had very short or unclear follow-up (Table 1).
Statistical heterogeneity ranged from not present to low (Figs. 2–6; Figs. 4–7 and Table 4, online supplement). Greater degrees of statistical heterogeneity have hampered the results of previous meta-analyses [5, 13, 14]. Clinical heterogeneity of 6 % tetrastarch dosing and frequency will remain within any meta-analysis (Table 2, online supplement). Therefore, the more conservative random-effects model was used, which assumes that individual studies are estimating different treatment effects.
Pooled data published in 2012 demonstrate that 6 % tetrastarch exposure increases the requirement of RRT support (Fig. 5). This was previously found for other HES formulations [8, 9, 12] and suspected for 6 % tetrastarch [54]. The point estimates are concordant and the pooled CI is narrower than already reported in trials [3, 25], improving precision. Sensitivity analysis did not alter this finding, suggesting it is robust. A meta-analysis of predominantly older, higher-molecular-weight HES formulations also found similar results [55]. The indication for initiating RRT might vary between centres and studies, introducing potential risk of bias. However, this effect would be expected to be the same across the blinded RCT cohorts, reducing potential bias affecting one particular group. The total 6 % tetrastarch dose exposures were below 50 ml/kg, and 3000 ml or less (Table 2, online supplement), thus incorrect use was not a major factor [54]. Some of the renal toxicity has been attributed to 43 % tissue uptake [53] and perhaps the effects of direct urinary ultrafiltration of less than 60 kDa molecules [51]. Overall, one patient with severe sepsis required RRT for every 16 patients treated with 6 % tetrastarch instead of (crystalloid) control fluid.
Comparison of RIFLE criteria components between 6 % tetrastarch and control fluid could not differentiate between safety and harm, partly because of low observed power (Table 4a, online supplement). With inclusion of septic and non-septic patients enrolled into CHEST, the more severe RIFLE-I and RIFLE-F acute kidney injury grades were associated with 6 % tetrastarch exposure (Table 4b, online supplement). However, no firm conclusions can be drawn from this.
Tetrastarch (6 %) exposure was associated with allogeneic transfusion (Fig. 6), and with larger volume (Table 3, online supplement). The point estimates are concordant across all studies, and the outcome withstands sensitivity analysis. This finding is consistent with non-significantly increased severe bleeding (p = 0.09) and significantly increased overall bleeding (p = 0.003) in the 6S study [25] but without major coagulation profile disturbance or blood loss in the smaller CRYSTMAS trial [26]. Anaemia from haemodilution [56], reduced platelet function and clot strength, effects on von Willebrand factor, and on factor XIII might explain a normal coagulation screen in the presence of bleeding with HES exposure [57–61]. Moreover, effects on erythropoiesis from tissue uptake [53, 62, 63] in bone marrow [64] of septic patients have not been adequately assessed, but lysosomal storage and toxicity might contribute. Hence, this observation requires further investigation. A transfusion protocol was not pre-defined, thus risk of bias is possible. However, the blinding of fluids and all personnel would likely reduce the effect of variations across the RCT groups, reducing the risk of imbalance. Patient characteristics were similar between groups, including those with septic shock (Table 1, online supplement).
The open-label CRISTAL study (Colloids Compared to Crystalloids in Fluid Resuscitation of Critically Ill Patients: A Multinational Randomised Controlled Trial; ClinicalTrials.gov; NCT00318942) will report 28-day mortality as primary, and 90-day mortality as secondary endpoints. The results might be informative as a sufficiently powered large RCT is often recommended to confirm meta-analysis findings. The open-label Impact of Early Goal-directed Fluid Therapy in Septic Patients Undergoing Emergency Surgery trial (ClinicalTrials.gov; identifier: NCT01654003) will close in December 2013. It will report 28-day mortality in approximately 250 patients. The results of the BaSES trial (n = 240) (ClinicalTrials.gov; identifier: NCT00273728), which completed in May 2011, are awaited, but follow-up was only 5 days and mortality was not a primary end-point. Therefore these two latter studies will not affect our 90-day mortality findings.
The major strength of this study has been to improve power sufficiently to investigate the safety and efficacy of 6 % tetrastarch products in a defined severe sepsis population using the recommended outcome measure of 90-day mortality [27]. A major limitation has been the inability to assess definitively some tertiary outcomes, partly due to inadequate power, and partly because of inconsistent or inadequate reporting of data. Studies at high risk of bias were included, but their impact on the primary outcome was minimal, as confirmed by subsequent sensitivity analysis with these studies removed. We tested the impact of the available CHEST data, but this did not affect our primary or secondary mortality outcomes.
Summary
Studies reporting 90-day mortality were of good quality. Overall and 90-day mortality were significantly higher in severe sepsis patients receiving 6 % tetrastarch 130 kDa solutions as part of initial fluid resuscitation. On the basis of our meta-analysis of currently available data, in our view the use of 6 % tetrastarch for volume resuscitation in severe sepsis cannot be recommended because of an association with harm, particularly as alternative fluids are available.
References
Finfer S, Liu B, Taylor C, Bellomo R, Billot L, Cook D, Du B, McArthur C, Myburgh J (2010) Resuscitation fluid use in critically ill adults: an international cross-sectional study in 391 intensive care units. Crit Care 14:R185
Investigators FS, Trials SCC (2008) Preferences for colloid use in Scandinavian intensive care units. Acta Anaesthesiol Scand 52:750–758
Myburgh JA, Finfer S, Bellomo R, Billot L, Cass A, Gattas D, Glass P, Lipman J, Liu B, McArthur C, McGuinness S, Rajbhandari D, Taylor CB, Webb SA (2012) Hydroxyethyl starch or saline for fluid resuscitation in intensive care. N Engl J Med 367:1901–1911
Hartog CS, Kohl M, Reinhart K (2011) A systematic review of third-generation hydroxyethyl starch (HES 130/0.4) in resuscitation: safety not adequately addressed. Anesth Analg 112:635–645
Wiedermann CJ, Joannidis M (2012) Mortality after hydroxyethyl starch 130/0.4 infusion: an updated meta-analysis of randomized trials. Swiss Med Wkly 142:w13656
Hartog CS, Skupin H, Natanson C, Sun J, Reinhart K (2012) Systematic analysis of hydroxyethyl starch (HES) reviews: proliferation of low-quality reviews overwhelms the results of well-performed meta-analyses. Intensive Care Med 38:1258–1271
Reinhart K, Perner A, Sprung CL, Jaeschke R, Schortgen F, Johan Groeneveld AB, Beale R, Hartog CS, European Society of Intensive Care M (2012) Consensus statement of the ESICM task force on colloid volume therapy in critically ill patients. Intensive Care Med 38:368–383
Brunkhorst FM, Engel C, Bloos F, Meier-Hellmann A, Ragaller M, Weiler N, Moerer O, Gruendling M, Oppert M, Grond S, Olthoff D, Jaschinski U, John S, Rossaint R, Welte T, Schaefer M, Kern P, Kuhnt E, Kiehntopf M, Hartog C, Natanson C, Loeffler M, Reinhart K (2008) Intensive insulin therapy and pentastarch resuscitation in severe sepsis. N Engl J Med 358:125–139
Schortgen F, Lacherade JC, Bruneel F, Cattaneo I, Hemery F, Lemaire F, Brochard L (2001) Effects of hydroxyethylstarch and gelatin on renal function in severe sepsis: a multicentre randomised study. Lancet 357:911–916
Shafer SL (2011) Shadow of doubt. Anesth Analg 112:498–500
Reinhart K, Takala J (2011) Hydroxyethyl starches: what do we still know? Anesth Analg 112:507–511
Wiedermann CJ (2008) Systematic review of randomized clinical trials on the use of hydroxyethyl starch for fluid management in sepsis. BMC Emerg Med 8:1
Gattas DJ, Dan A, Myburgh J, Billot L, Lo S, Finfer S (2012) Fluid resuscitation with 6% hydroxyethyl starch (130/0.4) in acutely ill patients: an updated systematic review and meta-analysis. Anesth Analg 114:159–169
Bunn F, Trivedi D (2012) Colloid solutions for fluid resuscitation. Cochrane Database Syst Rev 6:CD001319
Perel P, Roberts I (2012) Colloids versus crystalloids for fluid resuscitation in critically ill patients. Cochrane Database Syst Rev 6:CD000567
Freiman JA, Chalmers TC, Smith H Jr, Kuebler RR (1978) The importance of beta, the type II error and sample size in the design and interpretation of the randomized control trial. Survey of 71 “negative” trials. N Engl J Med 299:690–694
Kasper SM, Meinert P, Kampe S, Gorg C, Geisen C, Mehlhorn U, Diefenbach C (2003) Large-dose hydroxyethyl starch 130/0.4 does not increase blood loss and transfusion requirements in coronary artery bypass surgery compared with hydroxyethyl starch 200/0.5 at recommended doses. Anesthesiology 99:42–47
Kozek-Langenecker SA, Jungheinrich C, Sauermann W, Van der Linden P (2008) The effects of hydroxyethyl starch 130/0.4 (6%) on blood loss and use of blood products in major surgery: a pooled analysis of randomized clinical trials. Anesth Analg 107:382–390
Neff TA, Doelberg M, Jungheinrich C, Sauerland A, Spahn DR, Stocker R (2003) Repetitive large-dose infusion of the novel hydroxyethyl starch 130/0.4 in patients with severe head injury. Anesth Analg 96:1453–1459 table of contents
Niemi T, Schramko A, Kuitunen A, Kukkonen S, Suojaranta-Ylinen R (2008) Haemodynamics and acid-base equilibrium after cardiac surgery: comparison of rapidly degradable hydroxyethyl starch solutions and albumin. Scand J Surg 97:259–265
Schramko AA, Suojaranta-Ylinen RT, Kuitunen AH, Kukkonen SI, Niemi TT (2009) Rapidly degradable hydroxyethyl starch solutions impair blood coagulation after cardiac surgery: a prospective randomized trial. Anesth Analg 108:30–36
Ranieri VM, Thompson BT, Barie PS, Dhainaut JF, Douglas IS, Finfer S, Gardlund B, Marshall JC, Rhodes A, Artigas A, Payen D, Tenhunen J, Al-Khalidi HR, Thompson V, Janes J, Macias WL, Vangerow B, Williams MD (2012) Drotrecogin alfa (activated) in adults with septic shock. N Engl J Med 366:2055–2064
Russell JA, Walley KR, Singer J, Gordon AC, Hebert PC, Cooper DJ, Holmes CL, Mehta S, Granton JT, Storms MM, Cook DJ, Presneill JJ, Ayers D (2008) Vasopressin versus norepinephrine infusion in patients with septic shock. N Engl J Med 358:877–887
Sprung CL, Annane D, Keh D, Moreno R, Singer M, Freivogel K, Weiss YG, Benbenishty J, Kalenka A, Forst H, Laterre PF, Reinhart K, Cuthbertson BH, Payen D, Briegel J (2008) Hydrocortisone therapy for patients with septic shock. N Engl J Med 358:111–124
Perner A, Haase N, Guttormsen AB, Tenhunen J, Klemenzson G, Aneman A, Madsen KR, Moller MH, Elkjaer JM, Poulsen LM, Bendtsen A, Winding R, Steensen M, Berezowicz P, Soe-Jensen P, Bestle M, Strand K, Wiis J, White JO, Thornberg KJ, Quist L, Nielsen J, Andersen LH, Holst LB, Thormar K, Kjaeldgaard AL, Fabritius ML, Mondrup F, Pott FC, Moller TP, Winkel P, Wetterslev J (2012) Hydroxyethyl starch 130/0.42 versus Ringer’s acetate in severe sepsis. N Engl J Med 367:124–134
Guidet B, Martinet O, Boulain T, Philippart F, Poussel JF, Maizel J, Forceville X, Feissel M, Hasselmann M, Heininger A, Van Aken H (2012) Assessment of hemodynamic efficacy and safety of 6% hydroxyethylstarch 130/0.4 vs. 0.9% NaCl fluid replacement in patients with severe sepsis: the CRYSTMAS study. Crit Care 16:R94
Cohen J, Guyatt G, Bernard GR, Calandra T, Cook D, Elbourne D, Marshall J, Nunn A, Opal S (2001) New strategies for clinical trials in patients with sepsis and septic shock. Crit Care Med 29:880–886
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535
Bellomo R, Ronco C, Kellum JA, Mehta RL, Palevsky P, Workgroup A (2004) Acute renal failure - definition, outcome measures, animal models, fluid therapy and information technology needs: the Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group. Crit Care 8:R204–R212
Cook DJ, Guyatt GH, Ryan G, Clifton J, Buckingham L, Willan A, McIlroy W, Oxman AD (1993) Should unpublished data be included in meta-analyses? Current convictions and controversies. JAMA 269:2749–2753
Dellinger RP, Levy MM, Carlet JM, Bion J, Parker MM, Jaeschke R, Reinhart K, Angus DC, Brun-Buisson C, Beale R, Calandra T, Dhainaut JF, Gerlach H, Harvey M, Marini JJ, Marshall J, Ranieri M, Ramsay G, Sevransky J, Thompson BT, Townsend S, Vender JS, Zimmerman JL, Vincent JL (2008) Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock: 2008. Intensive Care Med 34:17–60
Sawyer AG, Ball AD (1981) Statistical power and effect size in marketing-research. J Marketing Res 18:275–290
Sahai H, Khurshid A (1996) Formulae and tables for the determination of sample sizes and power in clinical trials for testing differences in proportions for the two-sample design: a review. Stat Med 15:1–21
Onwuegbuzie AJ, Leech NL (2004) Post hoc power: a concept whose time has come. Underst Stat 3:201–230
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: a severity of disease classification system. Crit Care Med 13:818–829
Vincent JL, Moreno R, Takala J, Willatts S, De Mendonca A, Bruining H, Reinhart CK, Suter PM, Thijs LG (1996) The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the working group on sepsis-related problems of the European society of intensive care medicine. Intensive Care Med 22:707–710
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Dolecek M, Svoboda P, Kantorova I, Scheer P, Sas I, Bibrova J, Radvanova J, Radvan M (2009) Therapeutic influence of 20% albumin versus 6% hydroxyethylstarch on extravascular lung water in septic patients: a randomized controlled trial. Hepatogastroenterology 56:1622–1628
Palumbo D, Servillo G, D’Amato L, Volpe ML, Capogrosso G, De Robertis E, Piazza O, Tufano R (2006) The effects of hydroxyethyl starch solution in critically ill patients. Minerva Anestesiol 72:655–664
Dubin A, Pozo MO, Casabella CA, Murias G, Palizas F Jr, Moseinco MC, Kanoore Edul VS, Palizas F, Estenssoro E, Ince C (2010) Comparison of 6% hydroxyethyl starch 130/0.4 and saline solution for resuscitation of the microcirculation during the early goal-directed therapy of septic patients. J Crit Care 25:659 e1–659 e8
Lv J, Zhao HY, Liu F, An YZ (2012) [The influence of lactate Ringer solution versus hydroxyethyl starch on coagulation and fibrinolytic system in patients with septic shock]. Zhongguo Wei Zhong Bing Ji Jiu Yi Xue 24:38–41
Zhu GC, Quan ZY, Shao YS, Zhao JG, Zhang YT (2011) [The study of hypertonic saline and hydroxyethyl starch treating severe sepsis]. Zhongguo Wei Zhong Bing Ji Jiu Yi Xue 23:150–153
Li F, Sun H, Han XD (2008) [The effect of different fluids on early fluid resuscitation in septic shock]. Zhongguo Wei Zhong Bing Ji Jiu Yi Xue 20:472–475
Protsenko DN, Leiderman IN, Grigor’ev EV, Kokarev EA, Levit AL, Gel’fand BR (2009) [Evaluation of the effectiveness and safety of synthetic colloid solutions in the treatment of severe abdominal sepsis: a randomized comparative study]. Anesteziologiia i reanimatologiia: 9–13
Jacob M, Chappell D, Conzen P, Wilkes MM, Becker BF, Rehm M (2008) Small-volume resuscitation with hyperoncotic albumin: a systematic review of randomized clinical trials. Crit Care 12:R34
Committee TCvHSTCM (2011) The crystalloid versus hydroxyethyl starch trial: protocol for a multi-centre randomised controlled trial of fluid resuscitation with 6% hydroxyethyl starch (130/0.4) compared to 0.9% sodium chloride (saline) in intensive care patients on mortality. Intensive Care Med 37:816–823
Hartog CS, Reinhart K (2012) CRYSTMAS study adds to concerns about renal safety and increased mortality in sepsis patients. Crit Care 16:454
Ertmer C, Rehberg S, Van Aken H, Westphal M (2009) Relevance of non-albumin colloids in intensive care medicine. Best Pract Res Clin Anaesthesiol 23:193–212
Sahin SH, Memis D, Sut N (2009) High C-Reactive protein and amylase levels as prognostic markers in non-pancreatic severe sepsis patients. Trak Univ Tip Fak De 26:9–17
Bellmann R, Feistritzer C, Wiedermann CJ (2012) Effect of molecular weight and substitution on tissue uptake of hydroxyethyl starch. Clin Pharmacokinet 51:225–236
Hartog CS, Brunkhorst FM, Engel C, Meier-Hellmann A, Ragaller M, Welte T, Kuhnt E, Reinhart K (2011) Are renal adverse effects of hydroxyethyl starches merely a consequence of their incorrect use? Wien Klin Wochenschr 123:145–155
Dart AB, Mutter TC, Ruth CA, Taback SP (2010) Hydroxyethyl starch (HES) versus other fluid therapies: effects on kidney function. Cochrane Db Syst Rev
Vincent JL, Sakr Y, Sprung C, Harboe S, Damas P (2008) Are blood transfusions associated with greater mortality rates? Results of the sepsis occurrence in acutely ill patients study. Anesthesiology 108:31–39
Matsota P, Politou M, Kalimeris K, Apostolaki S, Merkouri E, Gialeraki A, Travlou A, Kostopanagiotou G (2010) Do different substitution patterns or plant origin in hydroxyethyl starches affect blood coagulation in vitro? Blood Coagul Fibrin 21:448–451
von Roten I, Madjdpour C, Frascarolo P, Burmeister MA, Fisch A, Schramm S, Bombeli T, Spahn DR (2006) Molar substitution and C2/C6 ratio of hydroxyethyl starch: influence on blood coagulation. Br J Anaesth 96:455–463
Nielsen VG (2005) Colloids decrease clot propagation and strength: role of factor XIII-fibrin polymer and thrombin-fibrinogen interactions. Acta Anaesthesiol Scand 49:1163–1171
Sossdorf M, Marx S, Schaarschmidt B, Otto GP, Claus RA, Reinhart K, Hartog CS, Losche W (2009) HES 130/0.4 impairs haemostasis and stimulates pro-inflammatory blood platelet function. Crit Care 13:R208
Godier A, Durand M, Smadja D, Jeandel T, Emmerich J, Samama CM (2010) Maize- or potato-derived hydroxyethyl starches: is there any thromboelastometric difference? Acta Anaesthesiol Scand 54:1241–1247
Sirtl C, Laubenthal H, Zumtobel V, Kraft D, Jurecka W (1999) Tissue deposits of hydroxyethyl starch (HES): dose-dependent and time-related. Br J Anaesth 82:510–515
Stander S, Szepfalusi Z, Bohle B, Stander H, Kraft D, Luger TA, Metze D (2001) Differential storage of hydroxyethyl starch (HES) in the skin: an immunoelectron-microscopical long-term study. Cell Tissue Res 304:261–269
Schmidt-Hieber M, Loddenkemper C, Schwartz S, Arntz G, Thiel E, Notter M (2006) Hydrops lysosomalis generalisatus–an underestimated side effect of hydroxyethyl starch therapy? Eur J Haematol 77:83–85
Acknowledgments
We acknowledge the Medical Research Council (MRC) Chain–Florey Fellowship scheme based at the Clinical Sciences Centre, Imperial College London. The research was supported by the National Institute for Health Research (NIHR) Biomedical Research Centre based at Imperial College Healthcare NHS Trust and Imperial College London. The views expressed are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Patel, A., Waheed, U. & Brett, S.J. Randomised trials of 6 % tetrastarch (hydroxyethyl starch 130/0.4 or 0.42) for severe sepsis reporting mortality: systematic review and meta-analysis. Intensive Care Med 39, 811–822 (2013). https://doi.org/10.1007/s00134-013-2863-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-013-2863-6