Abstract
Purpose
Rapid shallow breathing may occur at any time during spontaneous breathing trials (SBT), questioning the utility of a single determination of the rapid shallow breathing index (RSBI). We hypothesize that change in RSBI during SBT may more accurately predict successful extubation than a single determination.
Methods
Prospective observational study. Seventy-two subjects were extubated. At 24 h, 63/72 remained extubated (Extubation Success), and 9 were re-intubated (Extubation Failure). Respiratory rate (RR), tidal volume (VT) and RSBI were measured every 30 min during 2-h T-piece SBT. Change in respiratory parameters was assessed as percent change from baseline.
Results
Initial RSBI was similar in Extubation Success and Extubation Failure groups (77.0 ± 4.8, 77.0 ± 4.8, p = ns). Nevertheless, RSBI tended to remain unchanged or decreased in the Extubation Success group; in contrast RSBI tended to increase in the Extubation Failure group because of either increased RR and/or decreased VT (p < 0.001 for mean percent change RSBI over time), indicating worsening of the respiratory pattern. Quantitatively, only 7/63 subjects of the Extubation Success group demonstrated increased RSBI ≥20% at any time during the SBT. In contrast, in the Extubation Failure group, RSBI increased in all subjects during the SBT, and eight of nine subjects demonstrated an increase greater than 20%. Thus, with a 2-h SBT the optimal threshold was a 20% increase (sensitivity = 89%, specificity = 89%). Similar results were obtained at 30 min (threshold = 5% increase). Percent change of RSBI predicted successful extubation even when initial values were ≥105.
Conclusion
Percent change of RSBI during an SBT is a better predictor of successful extubation than a single determination of RSBI.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Prolonged mechanical ventilation is a risk for morbidity and mortality in critical ill patients [1]. Weaning failure is frequently associated with development of a rapid shallow breathing pattern [2–4]. Measurement of the rapid shallow breathing index (RSBI) is a simple bedside determination that may be utilized to identify this respiratory pattern classically thought to predict respiratory failure. However, despite being widely used and extensively studied, RSBI has variable sensitivity and specificity for predicting outcome following extubation [5–9].
Use of RSBI during a weaning protocol has failed to reduce the incidence of extubation failure, weaning time, or days on mechanical ventilation. Furthermore, use of RSBI has not been demonstrated to result in a survival benefit [10]. There are multiple potential explanations for these findings. First, patients may fail extubation without developing a rapid shallow breathing pattern during the weaning trial. Second, the threshold value that predicts extubation outcome may differ among individuals. Finally, other studies have demonstrated that respiratory failure may develop in a progressive nature during spontaneous breathing trials (SBT) as indicated by changes in esophageal pressure swings and/or minute ventilation recovery time [11, 12]. Therefore, a rapid and shallow breathing pattern suggestive of respiratory failure may develop at any time, questioning the utility of a single RSBI determination. Serial RSBI measurements have been investigated but have shown minimal or no improvement in the ability to predict successful extubation [13–16]. Although these studies evaluated RSBI at multiple time points, the change of RSBI in individual patients has not been assessed as a predictor of extubation outcome.
The present study evaluates the change in breathing pattern (evaluated as percent change in RSBI) during a 2-h SBT in individual subjects. We hypothesize that the change of RSBI, regardless of its initial value, may be a more accurate predictor of the overall capacity to tolerate extubation than RSBI determination at one point in time.
Materials and methods
Ninety-four subjects were prospectively recruited from the medical/surgical intensive care unit and cardiac care unit. Subjects were included if they met the following criteria as described by the Evidence-Based Medicine Task Force of the American College of Chest Physicians [17]: evidence for reversal of the underlying cause for respiratory failure; adequate oxygenation (PaO2/FIO2 > 200 mmHg; PEEP < 8 cmH2O); pH ≥ 7.3; hemodynamic stability (absence of active myocardial ischemia, absence of vasopressor use or <5mcg/kg/min of dopamine or dobutamine, heart rate <140); absence of fever (T < 38°C); hemoglobin >8 or >10 g/dl in subjects with known coronary disease; and Glasgow coma scale >10. Exclusion criteria included: known upper airway obstruction, copious secretions with cough and “do not intubate/resuscitate” status. Subjects were 18 years of age or older, orally intubated (tube size ≥7.5 mm) and mechanically ventilated for more than 48 h. Assist-control ventilation (AC) was the preferred mode prior to initiation of the weaning trial. The decision to perform a weaning trial was made by the treating critical care physician.
SBT protocol
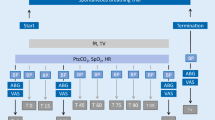
SBT was performed in a semi-seated position using a T-piece and supervised by a respiratory therapist. The T-piece was connected to a 200-ml reservoir of aerosol tubing on one port while the other port was connected via large-bore tubing to a high volume nebulizer (Airlife no. 002002, Cardinal Health Products). Oxygen flow was set at 15 l/min. The FIO2 was set to the same value used during mechanical ventilation. Criteria for SBT tolerance were defined as described by the ACCP: hemodynamic stability (pulse <140/min, systolic blood pressure <200 and >90 mmHg); absence of significant arrhythmia (increased premature ventricular beats of >4 beats/min or new onset of sustained supra-ventricular rhythm); respiratory rate <35/min; adequate gas exchange (SpO2 >88%; PO2 >55 mmHg; pH ≥7.3; increase in PaCO2 <10); no significant change in mental status; and absence of severe discomfort or signs of increased work of breathing [17]. Seventeen subjects failed at least one of the criteria during the SBT and were re-connected to the ventilator. The remaining subjects were maintained on T-piece for up to 2 h. If subjects tolerated the SBT, extubation was considered by the primary care team. Study investigators provided no input regarding the primary physician’s decision to start a weaning trial, reconnect the subjects to mechanical ventilation, or extubate/reintubate the subject. The primary physician decided to extubate 17 subjects before completing the 2-h SBT. The duration of SBT was similar in those subjects who were successfully extubated as compared with those who subsequently required re-intubation.
Data collection
Electrocardiogram, blood pressure and SpO2 were continuously monitored. Clinical and demographic characteristics, APACHE II score on admission, duration of mechanical ventilation and co-morbidities were recorded.
During the SBT, the respiratory pattern was measured by one investigator at 1, 30, 60, 90 and 120 min. Measurements were obtained for at least 60 s while the subjects breathed with a stable respiratory pattern. Minute ventilation was obtained using a calibrated Wright respirometer (Model Mark 20 Ferraris Respiratory, London, England) connected to the patient via an Adult Filtered Hygroscopic Condenser Humidifier (Airlife no. 003005, Cardinal Health). Respiratory rate was obtained by direct visualization, and tidal volume was derived allowing for calculation of RSBI. Measurements were not performed in subjects who were coughing, had copious secretions, were recently suctioned, or had a recent change in position. The primary care team was aware of the initial RSBI; however, the team was blinded to all subsequent values.
Change in respiratory pattern was assessed by the percent change of RSBI (relative to baseline) during the SBT. Two predefined parameters were evaluated: (1) maximum percent increase in RSBI at any time point during the 2-h SBT and (2) percent increase of RSBI assessed at 30 min.
Classification and analysis of outcomes
Subjects were classified into three groups based on ventilatory status 24 h after SBT. A 24-h period was used since all patients remained in the intensive care unit under the care of the critical care team for at least 24 h following extubation. The SBT-intolerant group included subjects who failed SBT before extubation and were reconnected to mechanical ventilation. The Extubation Failure group included subjects that required re-intubation within 24 h after extubation. The Extubation Success group included subjects that maintained spontaneous breathing >24 h after extubation.
Data are presented as mean ± SD unless otherwise indicated. Demographic and clinical variables were compared for the groups using analysis of variance with post hoc pairwise testing performed utilizing Tukey’s HSD. Sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), positive likelihood ratio (LR) and negative LR were calculated for the Extubation Success versus Extubation Failure subjects, and the receiver-operating characteristic (ROC) curves were plotted for RR, VT, RSBI, percent change in RSBI at 30 min and maximum percent change in RSBI over the 2-h SBT.
A multivariate logistic regression model was used to identify factors that significantly predicted extubation success. In addition to RSBI, factors examined in the model included age, gender, days on ventilator, ventilator mode, endotracheal tube size, APACHE II score, hemoglobin concentration, fluid balance, Glasgow coma scale and past history of COPD, asthma, cardiac disease and diabetes. The backward elimination procedure was used to obtain the final model, and factors that showed no further significant improvement to the model fit were eliminated. Age and gender were forced into the final model.
The protocol was approved by the Institutional Review Board of Morristown Memorial Hospital where data were collected. Informed consent was waived due to the observational nature of this study.
Results
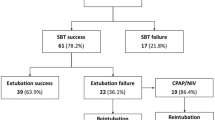
Ninety-four subjects were enrolled; three were excluded since RSBI could not be measured at the beginning of the SBT due to intractable cough, and two were excluded due to early intolerance precluding a second measurement of RSBI. Table 1 summarizes the clinical characteristics of the remaining 89 subjects. Seventeen of 89 did not tolerate spontaneous breathing and were not extubated (SBT Intolerant group). The remaining 72 subjects were extubated; 63 remained extubated for more than 24 h (Extubation Success group) and 9 required re-intubation (Extubation Failure group) after 9.1 ± 7.6 h. Of these nine subjects that failed extubation, seven developed respiratory failure that was attributed to the acute lung disease noted on presentation to the critical care unit, and two developed congestive heart failure. No subject was re-intubated due to upper airway obstruction, insufficient cough or impaired mental status, and none received continuous positive airway pressure or non-invasive ventilation. Demographic and clinical characteristics were similar between groups except for a lower prevalence of males in the SBT Intolerant group; there was no difference in gender between the Extubation Success and Extubation Failure group. There was a trend towards older age, higher APACHE II score, longer duration of mechanical ventilation and higher prevalence of COPD in the Extubation Failure as compared with the Extubation Success group. There were no significant differences between the groups in the indication for mechanical ventilation.
Respiratory data obtained at the onset of the SBT and at 30 min are presented in Table 1. At initiation of SBT, the SBT Intolerant group demonstrated higher RR and a trend towards higher RSBI compared to the other two groups. Mean values for RR, VT and RSBI at initiation of SBT were similar in the Extubation Success and Extubation Failure group. Of note, although mean values of RSBI were less than 105, rapid shallow breathing was present in 13/63 subjects (7 subjects with RSBI >125) in the Extubation Success group despite successful extubation. Furthermore, only 33% of subjects in the Extubation Failure group had rapid shallow breathing, but all failed extubation. Thus, the sensitivity and specificity of the initial RSBI to predict extubation outcome were 79 and 33%, respectively; sensitivity and specificity of RSBI were 76 and 33% when assessed at the last time point prior to extubation.
After 30 min of spontaneous breathing, the SBT Intolerant group showed a marked increase in the RSBI (mean 146.1 ± 88.6) associated with objective signs of respiratory distress, which prompted reinstitution of assisted ventilation. In contrast, there was no significant difference in the mean values for RR, VT or RSBI at 30 min between the Extubation Success and Extubation Failure groups.
Since the mean values for respiratory variables did not distinguish between the groups that tolerated the SBT, Fig. 1 analyzes the evolution of respiratory parameters in individual subjects during the SBT. The time course of RR and VT, expressed as percent change relative to baseline, during the 2-h SBT is plotted in the Extubation Success and Extubation Failure groups. While RR was highly variable in the Extubation Success group, an increase in RR was seen in the majority of subjects in the Extubation Failure group (p < 0.05 for mean values at each time point, data not shown). Similarly, while VT tended to remain either unchanged or increased in the Extubation Success group, VT rarely increased and frequently decreased in the Extubation Failure group (p = ns for mean values at each time point, data not shown). However, the individual data demonstrate significant overlap for the time course of both RR (top panel) and VT (bottom panel) in the Extubation Success compared with the Extubation Failure group, and ROC analysis demonstrated that neither parameter could be used to reliably predict extubation outcome (area under the curve 0.76 and 0.78, respectively).
The time course of the RR and VT for each individual expressed as percent change relative to baseline was plotted. Significant overlap is seen in the success compared with the failure group. Seventeen subjects (15 in the success group and 2 in the failure group) were extubated before completing the 2-h SBT, as decided by the primary physician. The duration of SBT was similar in the success and failure groups
Figure 2 illustrates the evolution of RSBI, expressed as percent change relative to baseline, over the 2-h SBT. The top panel plots data for each individual and illustrates that RSBI remained unchanged or decreased in the Extubation Success group. Only 7/63 subjects of this group (12%) demonstrated an increase in RSBI ≥20% (see ROC analysis below) at one time point during the SBT. In contrast, in the Extubation Failure group RSBI increased in all subjects during the SBT, and eight of nine subjects (89%) demonstrated an increase greater than 20% for at least one time point. The bottom panel illustrates the mean percent change in RSBI for the Extubation Success and Extubation Failure groups. At 30 min, the Extubation Success group demonstrated a reduction of RSBI that averaged −8.5 ± 2.2% (mean ± SE). In contrast, the Extubation Failure group demonstrated an increase in the RSBI at 30 min that averaged 21.8 ± 8.8% (p < 0.001). The divergence of the group means remained statistically different between the two groups throughout the SBT (p < 0.001).
The evolution of RSBI, expressed as percent change relative to baseline. The top panel plots data for each individual; RSBI remained unchanged or decreased in the success group, whereas it increased in the failure group. A reference line at 20% change in RSBI is plotted to highlight these differences. The bottom panel illustrates the mean percent change in RSBI (±SE) for the success (closed circle) and failure groups (open circle). *p < 0.001
Figure 3 plots the ROC curves that illustrate the ability of the initial RSBI and the maximum percent change in RSBI during the 2-h SBT to predict extubation outcome (area under the curve 0.41 and 0.93, respectively). The optimal threshold to predict successful extubation was a maximum increase in RSBI less than 20% at any time point during the SBT (sensitivity = 88.8%, specificity = 88.8%, PPV = 98%, NPV = 53%, positive LR = 8, negative LR = 0.125). Similar values for sensitivity and specificity were obtained for high-risk subgroups characterized by an initial RSBI >105 or ≥7 days of mechanical ventilation (Table 2). Multivariate logistic regression analysis confirmed that percent change in RSBI was an independent predictor of extubation outcome after accounting for demographic and clinical variables and after adjustment for initial RSBI (odds ratio for <20% change in RSBI as prediction of extubation success = 60, CI = 6–566, p < 0.001).
The percent change in RSBI obtained at 30 min was evaluated to determine if a shorter SBT would provide sufficient data to predict extubation outcome. The optimal threshold to predict extubation outcome was a 5% increase in RSBI at 30 min with sensitivity and specificity of 83% and 78% (PPV = 96%, NPV = 38%, positive LR = 3.71, negative LR = 0.22, area under the ROC curve = 0.83).
Discussion
This study evaluated the evolution of pattern of breathing in a heterogeneous group of subjects in a combined medical and surgical ICU. The data demonstrated that in subjects who tolerated a SBT, the percent change of RSBI (increase <20% over a 2-h period) predicted successful extubation. Percent change of RSBI predicted extubation outcome independent of respiratory rate, tidal volume and RSBI. In addition, percent change of RSBI predicted extubation outcome even in subjects with absolute values for initial RSBI greater than 105. Thus, evolution of respiratory pattern during spontaneous breathing may be an accurate, non-invasive and simple determination that can be used in the critical care setting to evaluate extubation readiness.
Respiratory failure may develop in a progressive manner and at a rate that may be difficult to predict [12, 18–20]. Jubran et al. [11] demonstrated that progressive change in esophageal pressure was predictive of weaning outcome; however, similar results were not obtained when variability of RSBI was analyzed. Using different methodologies, others have demonstrated that variability of respiratory parameters may be predictive of weaning outcome [21, 22]. However, the above studies analyzed breath-by-breath variability, which includes transient changes. In the present study, RSBI was measured during 1-min periods of stable breathing, avoiding times when subjects had copious secretions, cough, recent suctioning or changes in position. Thus, this protocol was designed to avoid transient changes that may obscure the overall trend.
In this study, data obtained during the first 30 min of SBT indicated that an increase in RSBI of <5% from the initial value predicted extubation success. When the data were analyzed over the full 2 h, increased variability of RSBI was detected, and the optimal threshold for predicting extubation outcome was a 20% increase in RSBI. This higher threshold may reflect either progressive development of rapid shallow breathing or increased detection of variability when multiple measurements are performed. However, the high positive predictive value for data obtained at 30 min (96%) suggests that a 30-min SBT may be sufficient to predict successful extubation.
Conflicting results regarding the usefulness of a single determination of RSBI during the weaning process have been reported. In the present study, RSBI at any time point was not predictive of successful extubation. Prior studies have reported a wide range of predictive values for RSBI, which may reflect differences in methodology, classification of outcomes and patient populations [23–27]. Prior studies have measured RSBI during partially supported ventilation and/or with uncalibrated equipment (e.g., mechanical ventilator) [28–33]. In the present study a precise protocol to measure the RSBI was utilized; data were obtained using a calibrated Wright spirometer during a 1-min period of stable breathing. Prior studies have variably defined the term “failure” to indicate either failure to tolerate a trial of spontaneous breathing and/or failure to tolerate a trial of extubation. In the present study, failure to tolerate a trial of spontaneous breathing (SBT Intolerant group) was associated with development of rapid shallow breathing; in this group RSBI at 30 min was generally greater than 105. In contrast, the rapid shallow breathing index measured at any given time point did not predict the primary outcome of this study: prediction of extubation success versus subsequent requirement for re-intubation.
Several factors may have influenced the results of this study. Although the results suggest that the change in RSBI is capturing a physiological phenomenon associated with extubation failure, it is possible that the results were in part due to a selection bias. This selection bias might have occurred since the initial RSBI was not blinded, and the treating physician may not have performed an SBT if the RSBI was elevated. However, the percent of subjects with elevated RSBI was similar in all three groups, and 16 subjects with elevated initial RSBI were included because they were clinically stable, completed the SBT and were subsequently extubated. A further selection bias may be present since the SBT Intolerant group was reconnected to the ventilator and therefore was not included in the analysis of factors predicting extubation outcome. As a result, the number of patients that failed extubation was small compared with the group that was successfully extubated. However, the observed extubation failure rate of 12.5% is in accord with prior published data [34, 35]. These considerations suggest that the impact of a selection bias on the observed data was minimal.
This study had few subjects with characteristics associated with higher rates of extubation failure (e.g., prolonged intubation or prior failed weaning trials), which may limit applicability of the results to these high risk patients. Furthermore, the change in RSBI would not predict extubation outcome when changes in respiratory status occur following extubation due to mucus plugging, upper airway obstruction, aspiration and/or alteration of mental status. Finally, the exploratory nature of the present results requires prospective validation in a larger and more heterogeneous population.
Whereas prior studies have evaluated individual values for RSBI as a predictor of weaning outcome, the present study extends prior observations by evaluating the dynamic changes of the breathing pattern as an index for the subsequent requirement for re-intubation. Respiratory failure occurs when there is an imbalance between mechanical work load and ventilatory output capacity, and may develop because of multiple different pathophysiologic derangements. Change in breathing pattern may be an expression of the increased effort needed to overcome different elements of respiratory mechanics (e.g., expiratory flow limitation, dynamic hyperinflation, dynamic lung compliance and/or respiratory muscle dysfunction), or it may occur as an end product of load-capacity imbalance [18, 36]. Thus, the evolution of respiratory pattern, as assessed by change in RSBI, is a marker of the dynamic changes that occur during weaning that may improve the ability to predict extubation outcome. In addition, the change in RSBI can identify subjects who might be successfully extubated despite elevated initial values for RSBI.
References
Epstein SK, Ciubotaru RL, Wong JB (1997) Effect of failed extubation on the outcome of mechanical ventilation. Chest 112:186–192
Tobin MJ, Perez W, Guenther SM, Semmes BJ, Mador MJ, Allen SJ, Lodato RF, Dantzker DR (1986) The pattern of breathing during successful and unsuccessful trials of weaning from mechanical ventilation. Am Rev Respir Dis 134:1111–1118
Yang KL, Tobin MJ (1991) A prospective study of indexes predicting the outcome of trials of weaning from mechanical ventilation. N Engl J Med 324:1445–1450
Berger KI, Sorkin IB, Norman RG, Rapoport DM, Goldring RM (1996) Mechanism of relief of tachypnea during pressure support ventilation. Chest 109:1320–1327
Afessa B, Hogans L, Murphy R (1999) Predicting 3-day and 7-day outcomes of weaning from mechanical ventilation. Chest 116:456–461
Lee KH, Hui KP, Chan TB, Tan WC, Lim TK (1994) Rapid shallow breathing (frequency-tidal volume ratio) did not predict extubation outcome. Chest 105:540–543
Meade M, Guyatt G, Cook D, Griffith L, Sinuff T, Kergl C, Mancebo J, Esteban A, Epstein S (2001) Predicting success in weaning from mechanical ventilation. Chest 120:400S–424S
Epstein SK (1995) Etiology of extubation failure and the predictive value of the rapid shallow breathing index. Am J Respir Crit Care Med 152:545–549
Conti G, Montini L, Pennisi MA, Cavaliere F, Arcangeli A, Bocci MG, Proietti R, Antonelli M (2004) A prospective, blinded evaluation of indexes proposed to predict weaning from mechanical ventilation. Intensive Care Med 30:830–836
Tanios MA, Nevins ML, Hendra KP, Cardinal P, Allan JE, Naumova EN, Epstein SK (2006) A randomized, controlled trial of the role of weaning predictors in clinical decision making. Crit Care Med 34:2530–2535
Jubran A, Grant BJB, Laghi F, Parthasarathy S, Tobin MJ (2005) Weaning prediction: esophageal pressure monitoring complements readiness testing. Am J Respir Crit Care Med 171:1252–1259
Martinez A, Seymour C, Nam M (2003) Minute ventilation recovery time: a predictor of extubation outcome. Chest 123:1214–1221
Kuo P-H, Wu H-D, Lu B-Y, Chen M-T, Kuo S-H, Yang P-C (2006) Predictive value of rapid shallow breathing index measured at initiation and termination of a 2-hour spontaneous breathing trial for weaning outcome in ICU patients. J Formos Med Assoc 105:390–398
Chatila W, Jacob B, Guaglionone D, Manthous CA (1996) The unassisted respiratory rate-tidal volume ratio accurately predicts weaning outcome. Am J Med 101:61–67
Krieger BP, Isber J, Breitenbucher A, Throop G, Ershowsky P (1997) Serial measurements of the rapid-shallow-breathing index as a predictor of weaning outcome in elderly medical patients. Chest 112:1029–1034
Teixeira C, Zimermann Teixeira PJ, Hoher JA, de Leon PP, Brodt SF, da Siva Moreira J (2008) Serial measurements of f/VT can predict extubation failure in patients with f/VT < or = 105? J Crit Care 23:572–576
MacIntyre NR, Cook DJ, Ely EW Jr, Epstein SK, Fink JB, Heffner JE, Hess D, Hubmayer RD, Scheinhorn DJ (2001) Evidence-based guidelines for weaning and discontinuing ventilatory support: a collective task force facilitated by the American College of Chest Physicians; the American Association for Respiratory Care; and the American College of Critical Care Medicine. Chest 120:375S–395S
Jubran A, Tobin MJ (1997) Pathophysiologic basis of acute respiratory distress in patients who fail a trial of weaning from mechanical ventilation. Am J Respir Crit Care Med 155:906–915
Tobin MJ (2006) Remembrance of weaning past: the seminal papers. Intensive Care Med 32:1485–1493
Vassilakopoulos T, Routsi C, Sotiropoulou C, Bitsakou C, Stanopoulos I, Roussos C, Zakynthinos S (2006) The combination of the load/force balance and the frequency/tidal volume can predict weaning outcome. Intensive Care Med 32:684–691
Wysocki M, Cracco C, Teixeira A, Mercat A, Diehl J-L, Lefort Y, Derenne J-P, Similowski T (2006) Reduced breathing variability as a predictor of unsuccessful patient separation from mechanical ventilation. Crit Care Med 34:2076–2083
Engoren M (1998) Approximate entropy of respiratory rate and tidal volume during weaning from mechanical ventilation. Crit Care Med 26:1817–1823
Vallverdu I, Calaf N, Subirana M, Net A, Benito S, Mancebo J (1998) Clinical characteristics, respiratory functional parameters, and outcome of a two-hour T-piece trial in patients weaning from mechanical ventilation. Am J Respir Crit Care Med 158:1855–1862
Tobin MJ, Jubran A (2008) Meta-analysis under the spotlight: focused on a meta-analysis of ventilator weaning. Crit Care Med 36:1–7
Nava S, Rubini F, Zanotti E, Ambrosino N, Bruschi C, Vitacca M, Fracchia C, Rampulla C (1994) Survival and prediction of successful ventilator weaning in COPD patients requiring mechanical ventilation for more than 21 days. Eur Respir J 7:1645–1652
Alvisi R, Volta CA, Righini ER, Capuzzo M, Ragazzi R, Verri M, Candini G, Gritti G, Milic-Emili J (2000) Predictors of weaning outcome in chronic obstructive pulmonary disease patients. Eur Respir J 15:656–662
Jacob B, Chatila W, Manthous CA (1997) The unassisted respiratory rate/tidal volume ratio accurately predicts weaning outcome in postoperative patients. Crit Care Med 25:253–257
Sassoon CS, Mahutte CK (1993) Airway occlusion pressure and breathing pattern as predictors of weaning outcome. Am Rev Respir Dis 148:860–866
El-Khatib MF, Jamaleddine GW, Khoury AR, Obeid MY (2002) Effect of continuous positive airway pressure on the rapid shallow breathing index in patients following cardiac surgery. Chest 121:475–479
Namen AM, Ely EW, Tatter SB, Case LD, Lucia MA, Smith A, Landry S, Wilson JA, Glazier SS, Branch CL, Kelly DL, Bowton DL, Haponik EF (2001) Predictors of successful extubation in neurosurgical patients. Am J Respir Crit Care Med 163:658–664
Krieger BP, Campos M (2002) Weaning parameters: read the methodology before proceeding. Chest 122:1873–1874
Manthous CA (2002) The anarchy of weaning techniques. Chest 121:1738–1740
Rose L, Presneill JJ, Johnston L, Cade JF (2008) A randomised, controlled trial of conventional versus automated weaning from mechanical ventilation using SmartCare/PS. Intensive Care Med 34:1788–1795
Frutos-Vivar F, Ferguson ND, Esteban A, Epstein SK, Arabi Y, Apezteguia C, Gonzalez M, Hill NS, Nava S, D’Empaire G, Anzueto A (2006) Risk factors for extubation failure in patients following a successful spontaneous breathing trial. Chest 130:1664–1671
Epstein SK, Ciubotaru RL (1998) Independent effects of etiology of failure and time to reintubation on outcome for patients failing extubation. Am J Respir Crit Care Med 158:489–493
Tobin MJ, Laghi F, Brochard L (2009) Role of the respiratory muscles in acute respiratory failure of COPD: lessons from weaning failure. J Appl Physiol 107:962–970
Acknowledgments
This study was not supported by any funding.
Conflict of interest statement
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Segal, L.N., Oei, E., Oppenheimer, B.W. et al. Evolution of pattern of breathing during a spontaneous breathing trial predicts successful extubation. Intensive Care Med 36, 487–495 (2010). https://doi.org/10.1007/s00134-009-1735-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-009-1735-6