Abstract
Background
Respiratory intensive care units (RICU) dedicated to weaning could be suitable facilities for clinical management of “post-ICU” patients.
Methods
We retrospectively analyzed the time course of patients’ characteristics, clinical outcomes and medical staff utilization in five Italian RICUs by comparing three periods of 5 consecutive years (from 1991 to 2005).
Results
A total of 3,106 patients (age 76 ± 4 years; 72% males) were analyzed. The number of co-morbidities per patient (from 1.8 to 3.0, p = 0.05) and the previous intensive care unit (ICU) stay (from 25 to 32 days, p = 0.002) increased over time. The doctor-to-patient ratio significantly decreased over time (from 1:3 to 1:5, p < 0.01), whereas the physiotherapist-to-patient ratio mildly increased (from 1:6 to 1:4.5, p < 0.05). The overall weaning success rate decreased (from 87 to 66%, p < 0.001), and the discharge destination changed (p < 0.001) over time; fewer patients were discharged to home (from 22 to 10%), and more patients to nursing home (from 3 to 6%), acute hospitals (from 6 to 10%) and rehabilitative units (from 70 to 75%). The mortality rate increased over time (from 9 to 15%). Significant correlations between the doctor-to-patient ratio and the rates of weaning success (r = 0.679, p = 0.005), home discharge (r = 0.722, p = 0.002) and the RICU length of stay (LOS) (r = −0.683, p = 0.005) were observed.
Conclusions
The clinical outcomes of our units worsened over 15 years, likely as consequence of admitting more severely ill patients. The potential further negative influence of reduced medical staff availability on weaning success, home discharge and LOS warrants future prospective investigations.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Severe chronic respiratory failure (CRF) patients may frequently require intensive care unit admission in order to overcome severe episodes of acute-on-chronic respiratory failure (ACRF) with ventilatory assistance [1]. However, ICUs are expensive resources [2]. Whereas only 40% of patients with ACRF in the ICU need invasive ventilation, they may be treated with non-invasive ventilation (NIV) [3] or need prolonged stay due to difficult weaning [4–6].
Furthermore, in the last years new technologies and improved levels of care have increased the number of “survivors of catastrophic illness” in the ICU, often requiring prolonged weaning [4].
Intermediate care units are expected to relieve congestion of ICUs, to maintain a high level of nursing assistance, to manage patients with ACRF needing NIV, to provide a multidisciplinary rehabilitative approach and to serve as bridge to home-care programs or long-term care facilities [7–9].
We therefore analyzed patients’ characteristics, main clinical outcomes and staff utilization in five respiratory intensive care units (RICU) of northern Italy over 15 years. We also analyzed whether changes in medical staff availability over time influenced major clinical outcomes.
Methods
We retrospectively reviewed medical records from five RICUs from northern Italy. Patients’ records were taken from electronic databases and hospital registers of the Salvatore Maugeri Foundation in Gussago-Lumezzane, Pavia, Veruno, and Montescano, and in Villa Pineta Hospital, Gaiato. Since individual patients’ data were not available, we analyzed mean annual rates of all variables.
Patients
Patients admitted between 1990 and 2005 with the following characteristics were recorded: (1) difficult weaning with tracheostomy after previous ventilation longer than 15 days in the ICU; (2) acute respiratory failure (ARF) needing NIV from our rehabilitative units, presenting with acute deterioration in neurological status, severe hypercapnia with respiratory acidosis and tachypnoa.
Mechanical ventilation (invasive or non-invasive) was adopted according to the previously described criteria [10, 11]. Patients admitted for difficult/prolonged weaning were managed according to previously described protocols [12–14].
Patients were grouped into three categories: chronic obstructive pulmonary disease (COPD) [15], cardiovascular diseases (CVD), including congestive heart failure, post-cardiac surgery sequelae, pulmonary edema and neurological and neuromuscular diseases (NNMD), including post-stroke, Guillain-Barrè syndrome, tetraplegia, Duchenne dystrophy and amyotrophic lateral sclerosis.
Setting
Our five RICUs belong to multidisciplinary respiratory rehabilitation units and receive patients from regional hospitals, with an overall number of beds ranging between 10 and 28. Respiratory assistance (including physiotherapy), speech and swallowing services were available. Intensivists or pneumologists trained in mechanical ventilation served as primary physicians.
Measurements
Age, gender, admission diagnoses, Acute Physiology and Chronic Health Evaluation (APACHE-II) score, chronic co-morbidities (including peripheral vascular, cerebrovascular, coronary artery and chronic lung diseases, active cancer, acquired immunodeficiency syndrome, hepatic cirrhosis or diabetes) and previous length of stay (LOS) in the ICU of origin were collected.
We evaluated the medical staff availability through nurse, physiotherapist, and doctor-to-patient ratios. RICU bed availability for the regional population was also registered over the years.
Clinical outcomes were: (1) respiratory status (ventilator dependence, spontaneous breathing with or without tracheostomy), (2) RICU LOS, (3) location after discharge (home, nursing-home, rehabilitation hospital, acute-care hospital), (4) in-hospital and 3-month mortality and (5) need of home mechanical ventilation. Successful weaning was defined as the ability to breathe spontaneously for >7 consecutive days.
Statistics
Data are presented as mean ± SD or proportions of the mean annual rates of variables. Statistical significance was set at p < 0.05.
Comparisons were done among the three consecutive 5-year periods of time with one-way repeated analysis of variance (ANOVA) for quantitative variables and chi-square test for qualitative variables. The Bonferroni test was used for post hoc comparisons.
We correlated by Pearson’s test the major clinical outcomes (annual mean rates of in-hospital and 3-month mortality, home discharge and weaning success, LOS) with patients’ age, number of co-morbidities, APACHE-II score, previous ICU stay and medical staff resources (doctor, nurse and physiotherapist-to-patient ratios) in the 15 single-year periods of time.
Results
Patients
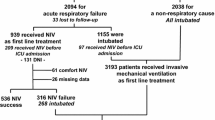
During the observational period, 3,106 consecutive adult patients were analyzed (Table 1); 2,016 (66%) underwent a weaning protocol for prolonged mechanical ventilation (PMV), and 1,090 patients (33%) needed monitoring or NIV treatment for severe ARF.
Demographic characteristics and all indices of functional status did not change over time except the number of co-morbidities and the previous ICU stay that increased over time (Table 1). The proportion of NNMD increased and the proportion of cardiovascular disease decreased over time (p < 0.001), while COPD remained constant.
Settings
The number of available beds increased over time, with a constant occupation rate of 97%. The doctor-to-patient ratio decreased over time, whereas the physiotherapist-to-patient ratio increased; the nurse-to-patient ratio remained stable (Table 1).
The RICU beds to the general population ratio increased over time (p = 0.001).
Clinical outcomes
The LOS (p = 0.004) and in-hospital mortality (p = 0.049) increased, and the weaning success rate (p < 0.001) decreased over time (Table 2). These outcomes in the three specific subgroups of patients showed trends similar to the overall population.
The discharge destination changed along time (p < 0.001), with fewer patients discharged home and an increasing trend of transfer to acute hospitals, rehabilitative units or nursing homes (Table 2). Among the patients discharged at home, we observed an increasing proportion of ventilator dependence by tracheostomy and NIV.
We found significant correlations between the doctor-to-patient ratio and the rates of weaning success (r = 0.679, p = 0.005), home discharge (r = 0.722, p = 0.002) and the RICU LOS (r = −0.683, p = 0.005), but not with mortality. The nurse and physiotherapist-to-patient ratios did not correlate with any outcome variable.
Discussion
Patients
The complexity of our patients increased over time, as demonstrated by the longer previous ICU stay, and higher number of co-morbidities and of proportion of NNMD subjects. The greater number of “chronically critical patients” surviving catastrophic illnesses and the transfer of more severe patients from nearby ICUs due to greater experience of our RICU staff may explain these changes in part. Moreover, the advances in respiratory and neurological physiotherapy, and the diffusion of home MV programs can justify the increased admission of NNMD patients to RICU facilities.
Settings
The RICU bed availability in Northern Italy has progressively increased over time. However, the ideal number of beds per population for a RICU dedicated to prolonged weaning, about 1/200,000 in Europe, is largely higher than in our regions (Table 1) [7]. Therefore, a further increase in RICU beds is needed to reduce ICU workload and reinforce cost-saving services such as home-care programs.
In addition, we found a progressive decrease in the doctor-to-patient ratio as a consequence of hospitals' fund-saving decisions because of the lack of a clear national reimbursement policy; however, its efficacy is unclear since prolonged stay in ICUs causes a considerable increase in costs.
The association between ICU physician staffing and clinical outcomes has been studied. A systematic review showed lower mortality and LOS with high-intensity physician staffing [16]. Dara and Afessa [17] observed a longer stay during the periods with fewer intensivists in a medical ICU. Similarly, we found a correlation between fewer physicians and worse LOS, weaning success and home discharge, but not with mortality. However, it is worth noting that the statistical strength of our finding is low due to the inability to perform a deeper analysis with available data.
Clinical outcomes
There is great variability in the clinical outcomes of weaning centers in the literature [7]. Weaning success, ranging from 10 to 92% [7], seems strongly related to hospital organization such as the existence of dedicated ventilator units able to improve weaning success [18], patients’ autonomy and families’ preparation for home discharge with ventilation [19].
Similarly, hospital mortality [7] and LOS [20] are widely variable. Staff expertise and the learning effect could also explain this variability in clinical outcomes of weaning centres [21]. Improved methods of prevention and management of respiratory complications were shown to decrease mortality dramatically over time [22, 23]. By contrast, despite increasing expertise in weaning care, the main outcomes progressively worsened over time in our units. Potential reasons for this would include increased severity of patients as suggested by the higher number of comorbidities, longer stays in ICUs and RICUs and worse mortality rates. Consequently, the proportion of patients discharged without ventilatory support and, in general, discharged at home were lower than in other published series [21, 24]. However, the information on home discharge rate among RICUs is variable, mainly depending on the variability of local weaning procedures and home-care programs. The different diagnoses at admission, the increasing severity of patients, with reduced weaning success rates, and the encouragement/improvement of home-care programs for unweanable patients may all explain these findings [25, 26].
A lower doctor-to-patient ratio correlated with worsening in the weaning success rate, home discharge and LOS in this study. Unfortunately, the lack of individual patients’ information impeded a complete statisitcal analysis of other potential confounding factors such as changes in case mix and organization of the RICUs. Therefore, despite the fact that a lower availability of doctors in ICUs has been associated with increased LOS [17] and mortality [16], the reliability of the correlations observed in the present study warrants further prospective investigation.
Limitations
The study was conducted retrospectively, and clinical outcomes were taken from hospitals’ registers without individual patients’ data and long-term mortality. Therefore, the available information regarding pre-morbid functional status and complications during the previous ICU stay is limited. Moreover, changes in treatment patterns were not systematically registered over the 15-year study period. Finally, the present study was conducted in Northern Italy and may not be representative of other regions.
Conclusion
The clinical outcomes of our units has worsened over 15 years, likely as a consequence of admitting more severely ill patients. The potential further negative influence of reduced medical staff availability on weaning success rate, home discharge and LOS deserves future prospective investigations.
References
Esteban A, Anzueto A, Alia I, Gordo F, Apezteguia C, Palizas F, Cide D, Goldwaser R, Soto L, Bugedo G, Rodrigo C, Pimentel J, Raimondi G, Tobin MJ (2000) How is mechanical ventilation employed in the intensive care unit? An international utilization review. Am J Respir Crit Care Med 161:1450–1458
Wagner DP (1989) Economics of prolonged mechanical ventilation. Am Rev Respir Dis 140:S14–S18
Lightowler JV, Wedzicha JA, Elliott MW, Ram FS (2003) Non-invasive positive pressure ventilation to treat respiratory failure resulting from exacerbations of chronic obstructive pulmonary disease: cochrane systematic review and meta-analysis. BMJ 326:185–189
Esteban A, Alia I, Ibañez J, Benito S, Tobin MJ, the Spanish Lung Failure Collaborative Group (1994) Modes of mechanical ventilation and weaning. A national survey of Spanish hospitals. Chest 106:1188–1193
Seneff MG, Wagner DP, Wagner RP, Zimmerman JE, Knaus WA (1995) Hospital and 1-year survival of patients admitted to intensive care units with acute exacerbation of chronic obstructive pulmonary disease. JAMA 274:1852–1857
Connors AF Jr, Dawson NV, Thomas C, Harrell FE Jr, Desbiens N, Fulkerson WJ, Kussin P, Bellamy P, Goldman L, Knaus WA (1996) Outcomes following acute exacerbation of severe chronic obstructive lung disease. The SUPPORT investigators (Study to Understand Prognoses and Preferences for Outcomes and Risks of Treatments). Am J Respir Crit Care Med 154:959–967
Nava S, Vitacca M (2006) Chronic ventilatory facilities. In: Tobin MJ (ed) Principles and practice of mechanical ventilation. McGraw-Hill, New York, pp 691–704
Rossi A, Ambrosino N (1994) The need for an intermediate cardiorespiratory unit. Monaldi Arch Chest Dis 49:463–465
Corrado A, Roussos C, Ambrosino N, Confalonieri M, Cuvelier A, Elliott M, Ferrer M, Gorini M, Gurkan O, Muir JF, Quareni L, Robert D, Rodenstein D, Rossi A, Schoenhofer B, Simonds AK, Strom K, Torres A, Zakynthinos S (2002) Respiratory intermediate care units: a European survey. Eur Respir J 20:1343–1350
Tobin MJ, Jubran A (2006) Discontinuation of mechanical ventilation. In: Tobin MJ (ed) Principles and practice of mechanical ventilation. McGraw-Hill, New York, pp 1185–1220
(2001) International Consensus Conferences in Intensive Care Medicine: noninvasive positive pressure ventilation in acute respiratory failure. Am J Respir Crit Care Med 163:283–291
Vitacca M, Vianello A, Colombo D, Clini E, Porta R, Bianchi L, Arcaro G, Vitale G, Guffanti E, Lo CA, Ambrosino N (2001) Comparison of two methods for weaning patients with chronic obstructive pulmonary disease requiring mechanical ventilation for more than 15 days. Am J Respir Crit Care Med 164:225–230
Boles JM, Bion J, Connors A, Herridge M, Marsh B, Melot C, Pearl R, Silverman H, Stanchina M, Vieillard-Baron A, Welte T (2007) Weaning from mechanical ventilation. Eur Respir J 29:1033–1056
Ely EW, Baker AM, Dunagan DP, Burke HL, Smith AC, Kelly PT, Johnson MM, Browder RW, Bowton DL, Haponik EF (1996) Effect on the duration of mechanical ventilation of identifying patients capable of breathing spontaneously. N Engl J Med 335:1864–1869
American Thoracic Society (1995) Standards for the diagnosis and care of patients with chronic obstructive pulmonary disease (COPD). Am J Respir Crit Care Med 152(Suppl):S77–S120
Pronovost PJ, Angus DC, Dorman T, Robinson KA, Dremsizov TT, Young TL (2002) Physician staffing patterns and clinical outcomes in critically ill patients: a systematic review. JAMA 288:2151–2162
Dara SI, Afessa B (2005) Intensivist-to-bed ratio: association with outcomes in the medical ICU. Chest 128:567–572
Gracey DR, Hardy DC, Naessens JM, Silverstein MD, Hubmayr RD (1997) The Mayo Ventilator-Dependent Rehabilitation Unit: a 5-year experience. Mayo Clin Proc 72:13–19
Bagley PH, Cooney E (1997) A community-based regional ventilator weaning unit: development and outcomes. Chest 111:1024–1029
Nasraway SA, Button GJ, Rand WM, Hudson-Jinks T, Gustafson M (2000) Survivors of catastrophic illness: outcome after direct transfer from intensive care to extended care facilities. Crit Care Med 28:19–25
Scheinhorn DJ, Chao DC, Stearn-Hassenpflug M, LaBree LD, Heltsley DJ (1997) Post-ICU mechanical ventilation: treatment of 1,123 patients at a regional weaning center. Chest 111:1654–1659
DeVivo MJ, Ivie CS III (1995) Life expectancy of ventilator-dependent persons with spinal cord injuries. Chest 108:226–232
Rogers RM, Weiler C, Ruppenthal B (1972) Impact of the respiratory intensive care unit on survival of patients with acute respiratory failure. Chest 62:94–97
Gracey DR, Viggiano RW, Naessens JM, Hubmayr RD, Silverstein MD, Koenig GE (1992) Outcomes of patients admitted to a chronic ventilator-dependent unit in an acute-care hospital. Mayo Clin Proc 67:131–136
Pilcher DV, Bailey MJ, Treacher DF, Hamid S, Williams AJ, Davidson AC (2005) Outcomes, cost and long term survival of patients referred to a regional weaning centre. Thorax 60:187–192
Schonhofer B, Euteneuer S, Nava S, Suchi S, Kohler D (2002) Survival of mechanically ventilated patients admitted to a specialised weaning centre. Intensive Care Med 28:908–916
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is discussed in the editorial available at: doi:10.1007/s00134-009-1672-4.
Rights and permissions
About this article
Cite this article
Polverino, E., Nava, S., Ferrer, M. et al. Patients’ characterization, hospital course and clinical outcomes in five Italian respiratory intensive care units. Intensive Care Med 36, 137–142 (2010). https://doi.org/10.1007/s00134-009-1658-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-009-1658-2