Abstract
Objective
This study assessed whether hyperglycemia and lipopolysaccharide (LPS) decrease the depression effect of interleukin (IL) 8 production by hypothermia in endothelial cells.
Design and setting
Laboratory study in a university laboratory.
Subjects
Human umbilical vein endothelial cells (HUVECs).
Interventions
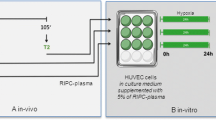
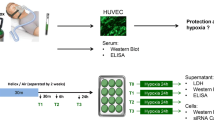
HUVECs were cultivated in various concentrations of glucose (5.5 or 16.5 mM = 100 or 300 mg/dl) with or without LPS stimulation for 5, 12, or 24 h at either 30° or 37 °C.
Results
After culturing, IL-8 mRNA expressions and IL-8 levels were measured. At 37 °C, hyperglycemia significantly increased basal IL-8 mRNA at 12 h and basal IL-8 at 24 h. At 37 °C hyperglycemia significantly increased LPS-stimulated IL-8 mRNA at 12 h and LPS-stimulated IL-8 at 12 and 24 h. At 30 °C basal IL-8mRNA, basal IL-8, and LPS-stimulated IL-8 were significantly decreased by hypothermia, but these hypothermic effects were not observed in LPS-stimulated IL-8 mRNA. Furthermore even at 30 °C hyperglycemia significantly increased LPS-stimulated IL-8 mRNA at all time points and LPS stimulated IL-8 at 24 h.
Conclusions
Hypothermia (30 °C) decreases the production of IL-8 in HUVECs but does not decrease the expression of IL-8 mRNA. When hypothermia is followed by hyperglycemia and LPS stimulation, such a combination may expose the patients to a high risk of secondary tissue damage during therapeutic hypothermia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hyperglycemia after a stress reaction is frequently observed after critical illness such as acute myocardial infarction [1]. Exposure to hyperglycemia is an important factor that contributes to endothelial cell damage [2, 3]. Endothelial cells play an important role in injury and inflammation by producing and regulating cytokines and adhesion molecules, free radicals, and chemoattractant mediators [4]. Interleukin (IL) 8 is generally recognized as a key mediator after an acute inflammatory response and plays an essential role in recruiting and activating neutrophil at the site of the inflammation. Recent studies have reported that therapeutic hypothermia can improve outcome in postresuscitative comatose patients after cardiogenic cardiopulmonary arrest (CPA) [5, 6]. Temperature-dependent cytokine release has been demonstrated for a variety of pro- and anti-inflammatory cytokines in vivo [7–11]. While monocytes and macrophages are major generators of cytokines, and cytokine production is clearly temperature dependent, with decreased production during hypothermia [12, 13], it remains unclear whether cytokine production in endothelial cells after lipopolysaccharide (LPS) stimulation is temperature dependent.
Depending on the degree and duration of organ ischemia during therapeutic hypothermia, cases such as postresuscitative comatose patients may develop pneumonia [14], systemic inflammation, which can cause medical complications such as hyperglycemia, or adult respiratory distress syndrome (ARDS) [14, 15]. These are the leading causes of late morbidity and mortality in comatose patients. ARDS, a component of postresuscitation disease, occurs frequently after CPA [15]. ARDS often accompanies bacteremia, sepsis and bacterial endotoxemia. LPS can stimulate vascular endothelial cells to produce IL-8 [16–18]. Moreover, therapeutic hypothermia for comatose patients is often associated with these medical complications [14].
We consider it very important to estimate LPS-induced cytokine production under a hyperglycemic condition during hypothermia. We hypothesized that hyperglycemia aggravates LPS induced IL-8 production from endothelial cells even in combination with hypothermia. The purpose of this investigation was to assess changes in the IL-8 mRNA expression and IL-8 production from endothelial cells stimulated by LPS in various concentrations of glucose during normotherimia or hypothermia.
Materials and methods
Cell culture
Human umbilical vascular endothelial cells (HUVECs; Cambrex Bio Science, Walkersville, Md., USA) were maintained as monolayers in EBM2 medium (Cambrex Bio Science) containing 10% fetal calf serum at 37 °C in a humidified atmosphere containing 5% carbon dioxide. Cells were passaged at 70–80% confluence and were maintained no longer than 4 weeks.
Experimental groups
HUVECs (5 × 105 cells/well, n = 6 wells each) were maintained at 37 °C in EBM2 medium and incubated for 48 h. The cells were then cultured in various media to examine the effect of osmolalities, glucose or LPS stimulation on IL-8 production. EBM2 medium was replaced with Medium 199 (Invitrogen Corporation, Carlsbad, Calif., USA) containing 10% fetal calf serum, which were prepared in various glucose concentrations containing 5.5 mM (100 mg/dl) glucose, 16.5 mM (300 mg/dl) glucose, or 5.5 mM (100 mg/dl) glucose plus 11 mM (200 mg/dl) mannitol. Some of the media were prepared with 1 μg/ml LPS (Sigma-Aldrich, St. Louis Mo., USA).
To determine the effect of changes in glucose or osmolality on IL-8 production responses we used different concentrations of glucose or osmolality culture medium. Because the osmolality of the 16.5 mM glucose culture medium was higher than that of the 5.5 mM glucose culture medium, we prepared a hyperosmolality medium (5.5 mM of glucose plus 11 mM of mannitol) with a glucose concentration of 5.5 mM, which had the same osmolality as the medium of 16.5 mM of glucose plus mannitol. Medium osmolalities were assessed by freezing point depression. The HUVECs were then incubated for 5, 12, or 24 h at either 30 °C or 37 °C. The LPS doses and periods of exposure to the high glucose medium were determined by previous preliminary experiments (results not shown) [19].
Enzyme-linked immunoabsorbent assay
After incubation the supernatants were stored at minus 80 °C until the cytokine assay. IL-8 levels in the supernatants were quantified using a commercially available enzyme-linked immunosorbent assay (ELISA) kit (Quantikine Human IL-8 Immunoassay, R&D Systems, Minneapolis, Minn., USA) according to the manufacturer's instructions.
RNA isolation and reverse transcription
Total RNA was isolated from cells using a Micro-to-Midi Total RNA Purification System (Invitrogen) according to the manufacturer's instructions, which included a DNase process. Of the total RNA 500 ng was reverse-transcribed using a Takara RNA PCR kit (AMV, version 3.0; Takara, Shiga, Japan), according to the manufacturer's instructions, using random 9mers primers (Takara). After the reverse transcription (RT) reaction the cDNA was diluted with distilled water to 10 μl; 1 μl cDNA was used for each PCR reaction.
TaqMan real-time RT-PCR analysis
An Assay-on-Demand Gene Expression Assay (exon-overlapping primers and minor groove binder probes for real-time RT-PCR) was purchased from Applied Biosystems (Foster City, Calif., USA); housekeeping gene 18s [assay ID (Hs99999901_s1), IL-8 (Hs00174103_m1)]. These primers and minor groove binder probes were mixed in TaqMan PCR Master MIX (Applied Biosystems) according to the manufacturer's instructions. TaqMan real-time RT-PCR was performed using a 7500 Real Time PCR system (Applied Biosystems). Amplification was performed under the following cycling conditions: 2 min at 50 °C, 10 min at 95 °C, and 40 two-step cycles of 15 s at 95 °C and 1 min at 60 °C. According to the comparative Ct method described in the Applied Biosystems manual, gene expression was normalized to the expression of the housekeeping gene 18s, yielding the ΔCt value. The ΔCt value obtained from the control sample (incubated 5 h at 37.0 °C in Medium 199 with a glucose concentration of 5.5 mM and no LPS) was then subtracted from the ΔCt value of each sample that was subject to the experimental conditions described above, yielding the Δ ΔCt value. The gene expression level, normalized to the housekeeping gene and relative to the control sample, was calculated using 2-Δ Δ Ct. The mRNA levels were normalized to those of untreated control cells arbitrarily set to a value 1.
Statistical analysis
Statistical analyses were performed using Stat-View 5.0 (SAS Institute, Cary, NC, USA). Duplicate or triplicate samples were obtained via parallel cultures throughout the entire experimental protocol. For the bioassays each sample was plated in triplicate and the results were averaged. Data were expressed as mean values ± SD. Comparisons of cytokine IL-8 data between the groups were conducted using one-way analysis of variance. The unpaired t-test was performed to determine differences between groups (glucose 5.5 mM vs. glucose 5.5 mM + mannitol 11 mM, glucose 5.5 mM + mannitol 11 mM vs. glucose 16.5 mM, glucose 5.5 mM vs. glucose 16.5 mM) adjusted using Bonferroni's method. Two-factor analysis of variance was performed to examine the between-group comparisons of IL-8 data after temperature manipulations. When there were no statistically significant interactions, the Tukey–Kramer post-hoc test was performed. When there were statistical interactions, a one-factor analysis of variance and the Tukey–Kramer post-hoc tests were performed. Differences were considered statistically significant if the p-value was less than 0.05.
Results
The real osmolality (mOsm/kgH2O) of the culture media with 5.5 mM glucose was 295.8 ± 0.4, that of the culture media with 16.5 mM glucose was 306.8 ± 0.8, and that of the culture media with 5.5 mM glucose plus 11 mM mannitol culture was 306.8 ± 0.4. There were no significant differences in the osmolality of the culture medium with 16.5 mM glucose and that with 5.5 mM glucose plus 11 mM mannitol, but the osmolalities of both were significantly greater (p < 0.01) than that of the culture medium with 5.5 mM glucose.
Sequential changes in constitutive IL-8 mRNA and IL-8 without LPS stimulation
Changes in the IL-8 mRNA expression of HUVECs at various time points (5, 12, 24 h) and glucose concentrations are illustrated in Fig. 1a. In the 16.5 mM glucose culture medium, significant (p < 0.05) increases in IL-8 mRNA expression were observed at 12 h vs. the 5.5 mM culture media. The groups showed no significant differences in IL-8 mRNA expression at 5 and 24 h. Changes in the IL-8 levels at various times are illustrated in Fig. 1b. In the 16.5 mM glucose culture medium significant increases in IL-8 were observed at 24 h vs. the 5.5 mM or 5.5 mM glucose plus 11 mM mannitol culture media. There was no significant difference in the IL-8 mRNA and IL-8 levels between the 5.5 mM glucose and 5.5 mM glucose plus 11 mM mannitol culture media during 5, 12, or 24 h of incubation.
Changes in IL-8 mRNA expression (a) and IL-8 (b) in HUVECs after 5, 12, 24 h of incubation at different glucose concentrations (without LPS stimulation). IL-8 mRNA expression at 12 h (a) and IL-8 at 24 h (b) in 16.5 mM glucose culture medium (glucose 16.5 mM) was significantly higher than in 5.5 mM glucose (glucose 5.5 mM; p < 0.05). Glucose 5.5 mM, 5.5 mM glucose culture medium without LPS; glucose 5.5 mM + mannitol 11 mM, 5.5 mM glucose plus 11 mM mannitol culture medium without LPS; glucose 16.5 mM, 16.5 mM glucose culture medium without LPS; N.S., not significant; bars, mean ± SD
Sequential changes in the levels of IL-8 mRNA and IL-8 with LPS stimulation
There were increased levels of IL-8 mRNA (e.g., in the 5.5 mM glucose culture medium at 5 h, from 1.0 ± 0.2 to 96.5 ± 21.2) and IL-8 (e.g., in the 5.5 mM glucose culture medium at 5 h, from 233.1 ± 70.0 to 8774.0 ± 643.0) after LPS stimulation when there was no LPS stimulation. The changes in the IL-8 mRNA (Fig. 2a) and IL-8 levels (Fig. 2b) stimulated by LPS at various times were observed. IL-8 mRNA was significantly higher (p < 0.05) in the high glucose medium (16.5 mM glucose medium) than in the 5.5 mM glucose medium at 12 h. IL-8 level was significantly higher (p < 0.05) in the high glucose medium (16.5 mM glucose medium) than in the 5.5 mM glucose medium at 12 and 24 h. There was no significant difference in the levels of IL-8 mRNA and IL-8 between the 5.5 mM glucose and 5.5 mM glucose plus 11 mM mannitol culture media during 5, 12, or 24 h of incubation.
Changes in IL-8 mRNA expression (a) and IL-8 (b) in HUVECs after 5, 12, 24 h of incubation at different glucose concentrations (with LPS stimulation). LPS induced IL-8 mRNA expression (a) was significantly higher at the high glucose concentration (16.5 mM glucose, glucose 16.5 mM + LPS) at 12 h (p < 0.05). IL-8 (b) was significantly higher at the high glucose concentration after 12 h (p < 0.05). Glucose 5.5 mM + LPS, 5.5 mM glucose culture medium stimulated by LPS; glucose 5.5 mM + mannitol 11 mM + LPS, 5.5 mM glucose plus 11 mM mannitol culture medium stimulated by LPS; glucose 16.5 mM + LPS, 16.5 mM glucose culture medium stimulated by LPS; N.S., not significant; bars, mean ± SD
Effect of temperature manipulation
The levels of IL-8 mRNA expression (Fig. 3a) and IL-8 (Fig. 3b) under a hypothermic condition (30 °C) during 5, 12, or 24 h of incubation without LPS decreased significantly (p < 0.01) vs. those of IL-8 at 37 °C in the 5.5 and 16.5 mM glucose culture media. Temperature manipulation did not affect on IL-8 mRNA expression of the 12- or 24-h incubation groups stimulated by LPS except at 5-h, as shown in Fig. 4a. IL-8 levels under a hypothermic condition (30 °C) decreased significantly 5, 12, and 24 h after incubation with LPS (p < 0.01) vs. the group at 37 °C (37 °C vs. 30 °C, p < 0.01) at the same glucose concentration (5.5 or 16.5 mM), but differences in IL-8 levels of 16.5 mM glucose culture medium at 24 h were not significantly by temperature manipulation (Fig. 4b). IL-8 mRNA levels (12 and 24 h of incubation) and IL-8 levels (24 h of incubation) were significantly high (p < 0.05) in the hyperglycemic (16.5 mM glucose) hypothermic group (30 °C) vs. the normoglycemic (5.5 mM glucose) and hypothermic (30 °C) group.
Effect of hypothermia on IL-8 mRNA expression (a) and IL-8 (b; without LPS stimulation). IL-8 mRNA expression (a) and IL-8 (b) under hypothermic conditions (30 °C) during 5, 12, and 24 h of incubation without LPS was more significantly attenuated than the IL-8 levels at 37 °C in 5.5 (glucose 5.5 mM) or 16.5 mM glucose (glucose 16.5 mM) culture medium (p < 0.01); Glucose 5.5 mM, 5.5 mM glucose culture medium without LPS; glucose 16.5 mM, 16.5 mM glucose culture medium without LPS; bars, mean ± SD
Effect of hypothermia on IL-8 mRNA expression (a) and IL-8 (b; with LPS stimulation). Hypothermia did not affect IL-8 mRNA expression (a) in the groups incubated for 12 or 24 h and stimulated by LPS, but it significant decreased IL-8 mRNA expression in 5.5 mM glucose culture medium incubated for 5 h (p < 0.01). In hypothermic conditions (30 °C) IL-8 mRNA expression (12 and 24 h of incubation) in 16.5 mM glucose culture medium (glucose 16.5 mM + LPS) was significantly higher than the levels in 5.5 mM glucose culture medium (glucose 5.5 mM + LPS; p < 0.01). The IL-8 levels under hypothermic conditions (30 °C) during 5, 12, or 24 h incubation with LPS were significantly lower than the IL-8 levels at 37 °C in 5.5 mM (glucose 5.5 mM + LPS) or 16.5 mM glucose culture medium (glucose 16.5 mM + LPS; p < 0.01), but there was no significance in IL-8 level in 16.5 mM glucose culture medium incubated for 24 h. In hypothermic conditions (30 °C) IL-8 level at 24 h of incubation in 16.5 mM glucose culture medium (glucose 16.5 mM + LPS) was significantly higher than the level in 5.5 mM glucose culture medium (glucose 5.5 mM + LPS; p < 0.01)
Discussion
Prolonged exposure to hyperglycemia is an important factor in the pathogenesis of diabetic complications [20–22] that contribute to endothelial cell damage [2, 3, 23] in the clinical state. It is remains unclear, however, whether a hyperglycemic episode after postresuscitation from CPA or during therapeutic hypothermia can affect secondary endothelial cells damage. We demonstrated increases in both IL-8 mRNA expression and IL-8 level after incubation (12 or 24 h) in endothelial cells under high glucose conditions stimulated by LPS. Although IL-8 mRNA expression did not increase in the high-glucose medium (16.5 mM) after 5 h of incubation, it reached noticeably high levels after 12 h of incubation. In this study we concluded that the higher glucose concentrations in the presence of LPS enhance the expression of IL-8 mRNA from HUVECs cultured for 12 h since no significant changes were observed in the higher osmolality culture medium of mannitol without high glucose.
Hyperglycemia can cause vascular dysfunction in a variety of ways, including hyperosmolality, oxidant formation, and protein kinase C activation. Wilmer et al. [24] showed that high levels of extracellular glucose activate intracellular signal transduction (p38 mitogen-activated protein kinase; p38MAPK) and can be induced by oxidants, hyperosmolality, and proinflammatory cytokines, leading to apoptosis, cell growth, and gene regulation in human mesangial cells. Gosmanov et al. [25] showed that production of IL-8 from endothelial cells rises significantly due to hyperglycemia, but the glucose level in their experiment was 30 mM which was higher than the glucose level in our study. Igarashi et al. [26] also reported that the effect of hyperglycemia on p38MAPK activation and that glucose at 16.5 mM increased p38MAPK activity in a time-dependent manner vs. 5.5 mM glucose in rat aortic smooth muscle cells. However, hyperosmolality itself is the key factor that induces IL-8 production, through the signal transduction (p38MAPK) from the cell membrane to the nucleus [27].
In the present study we examined the effect of higher glucose medium and hyperosmolar mannitol stimulation on IL-8 production. Our results showed that hyperglycemia (16.5 mM) itself is the mediator of IL-8 production concomitant with IL-8 mRNA expression, regardless of hyperosmolar mannitol stimulation. Recent evidence [28] suggests that LPS-induced IL-8 synthesis in HUVECs depends on two parallel intracellular signaling pathways converging at the level of nuclear factor κB via p38MAPK or rho protein. The mechanism of LPS-induced IL-8 synthesis in HUVECs is still unclear, but we speculate that high glucose itself has an impact on the degree of activation of intracellular signaling molecules, and that the presence of LPS in a high glucose condition enhances the expression of IL-8 mRNA from HUVECs after 12 h of incubation. The increased levels of IL-8 after infection may work in combination with the hyperglycemia to aggravate endothelial cell damage and enhance the inflammatory process. If so, the process may subsequently lead to neutrophil infiltrating the injured tissue which in turn could worsen the outcome by enhancing secondary injury processes. These results suggest that it is important to strictly manage even short-term increases in blood glucose after acute stress.
Cardiac arrest with widespread cerebral ischemia frequently leads to severe neurological impairment. A recent study reported that for unconscious adult patients who have been successfully resuscitated after CPA, therapeutic mild hypothermia could increase the chance of a favorable neurological outcome and reduce mortality [5, 6]. An effect of reduction in the enzymatic reaction and certain reactions has been presented concerning cellular response under hypothermia in some cell lines [29]. However, little is known about the effects of temperature manipulation on the levels of IL-8 mRNA and IL-8 in HUVECs. The levels of constitutive IL-8 mRNA and IL-8 without stimulation by LPS from HUVECs decreased significantly during incubation at hypothermia (30 °C for 5 to 24 h) in various glucose concentrations. Although hypothermia attenuated LPS-induced IL-8 levels for 5–24 h, it failed to attenuate LPS induced IL-8 mRNA expression at any time for any glucose concentration except the glucose 5.5 mM medium at 5 h. Moreover, the levels of IL-8 mRNA in a 16.5 mM glucose concentration were significantly higher than that in a 5.5 mM glucose culture medium during hypothermia. Our study may indicate that hypothermia (30 °C) cannot attenuate expression of IL-8 mRNA in the presence of infection but can suppress the protein translation process after expression of IL-8 mRNA or other enzymatic activity for IL-8 protein synthetases.
We frequently see hyperglycemia and pneumonia as medical complications during therapeutic hypothermia [14]. Endogenous IL-8 has been shown to be a key mediator of chemotactic activity for neutrophils, participating in this process by recruiting neutrophils [16, 18]. Neutrophil activation and adhesion to the endothelium play important roles in inflammation and sepsis. Therefore while there is still a significant rise in IL-8 mRNA levels in a hypothermic condition with these medical complications, endothelial cells may be at risk of subsequently developing adverse affects in the secondary inflammatory process during therapeutic hypothermia. Thus taken together our data suggest that tight glucose control and management of infectious complications is necessary to prevent the secondary inflammatory process during therapeutic hypothermia.
Conclusion
We conclude that high glucose concentration is an important factor of IL-8 production in HUVECs. Constitutive expression of IL-8 mRNA is usually low but can be greatly stimulated in response to infection. Hyperglycemia may have a deleterious effect because the exaggerated inflammatory response cannot efficiently control infection, which may predispose the patients to secondary tissue injury. Enhanced LPS induced IL-8 production may contribute to the immunomodulatory effects of hyperglycemia in various clinical settings. Hypothermia (30 °C) could not attenuate expression of IL-8 mRNA in the presence of LPS. Theses processes may be further aggravated by hyperglycemia, and leading to medical complications in critically ill patients. In cases of combined hyperglycemia and infection such a process would leave postresuscitation patients at high risk of secondary tissue damage. Strict management of plasma glucose and infectious complications may be key strategies during therapeutic hypothermia.
References
Capes SE, Hunt D, Malmberg K, Gerstein HC (2000) Stress hyperglycemia and increased risk of death after myocardial infarction in patients with and without diabetes: a systematic overview. Lancet 55:773–778
Nishikawa T, Edelstein D, Du XL, Yamagishi S, Matsumura T, Kaneda Y, Yorek MA, Beebe D, Oates PJ, Hammes HP, Giardino I, Brownle M (2000) Normalizing mitochondrial superoxide production blocks three pathways of hyperglycaemic damage. Nature 404:787–790
Aronson D, Rayfield EJ (2002) How hyperglycemia promotes atherosclerosis: molecular mechanisms. Cardiovasc Diabetol 1:1
Shrotri MS, Peyton JC, Cheadle WG (2000) Leukocyte-endothelial cell interactions: review of adhesion molecules and their role in organ injury. In: Baue AE, Faist E, Fry DE (eds) Multiple organ failure pathophysiology, prevention, and therapy. Springer, Berlin Heidelberg New York pp 224–240
Bernard SA, Gray TW, Buist MD, Jones BM, Silvester W, Gutteridge G, Smith K (2002) Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. N Engl J Med 346:557–563
The Hypothermia after Cardiac Arrest Study Group (2002) Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. N Engl J Med 346:549–556
Puttick MI, Scott-Coombes DM, Dye J, Nduka CC, Menzies-Gow NM, Mansfield AO, Darzi A (1999) Comparison of immunologic and physiologic effects of CO2 pneumoperitoneum at room and body temperatures. Surg Endosc 13:572–575
Aibiki M, Maekawa S, Nishiyama T, Seki K, Yokono S (1999) Activated cytokine production in patients with accidental hypothermia. Resuscitation 41:263–268
Aibiki M, Maekawa S, Ogura S, Kinoshita Y, Kawai N, Yokono S (1999) Effect of moderate hypothermia on systemic and internal jugular plasma IL-6 levels after traumatic brain injury in humans. J Neurotrauma 16:225–232
Kinoshita K, Chatzipanteli K, Vitarbo E, Truettner JS, Alonso OF, Dietrich WD (2002) Interleukin-1beta messenger ribonucleic acid and protein levels after fluid-percussion brain injury in rats: importance of injury severity and brain temperature. Neurosurgery 51:195–203
Vitarbo EA, Chatzipanteli K, Kinoshita K, Truettner JS, Alonso OF, Dietrich WD (2004) Tumor necrosis factor alpha expression and protein levels after fluid percussion injury in rats: the effect of injury severity and brain temperature. Neurosurgery 55:416–425
Russwurm S, Stonans I, Schwerter K, Stonane E, Meissner W, Reinhart K (2002) Direct influence of mild hypothermia on cytokine expression and release in cultures of human peripheral blood mononuclear cells. J Interferon Cytokine Res 22:215–221
Fairchild KD, Viscardi RM, Hester L, Singh IS, Hasday JD (2000) Effects of hypothermia and hyperthermia on cytokine production by cultured human mononuclear phagocytes from adults and newborns. J Interferon Cytokine Res 20:1049–1055
Polderman KH (2004) Application of therapeutic hypothermia in the ICU: opportunities and pitfalls of a promising treatment modality. I. Indications and evidence. Intensive Care Med 30:556–575
Negovsky VA (1998) Postresuscitation disease. Crit Care Med 10:942–946
Mantovani A, Dejana E (1989) Cytokines as communication signals between leukocytes and endothelial cells. Immunol Today 10:370–375
Strieter RM, Kunkel SL, Showell HJ, Remick DG, Phan SH, Ward PA, Marks RM (1989) Endothelial cell gene expression of a neutrophil chemotatic factor by TNF-alpha, LPS, and IL1 beta. Science 243:1467–1469
Baggiolini M, Dewald B, Moser B (1994) Interleukin-8 and related chemotactic cytokines-CXC and CC chemokines. Adv Immunol 55:97–179
Kinoshita K, Furukawa M, Ebihara T, Sakurai A, Noda A, Kitahata Y, Utagawa A, Tanjoh K (2006) Acceleration of chemokine production from endothelial cells in response to lipopolysaccharide in hyperglycemic condition. Acta Neurochir Suppl (Wien) 96:419–421
Laakso M (1999) Hyperglycemia and cardiovascular disease in type 2 diabetes. Diabetes 48:937–942
Grundy SM, Benjamin IJ, Burke GL, Chait A, Eckel RH, Howard BV, Mitch W, Smith SC Jr, Sowers JR (1999) Diabetes and cardiovascular disease: a statement for healthcare professionals from the American Heart Association. Circulation 100:1134–1146
Diabetes Control and Complications Trial Research Group (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329:977–986
Ruderman NB, Haudenschild C (1984) Diabetes as an atherogenic factor. Prog Cardiovasc Dis 26:373–412
Wilmer WA, Dixon CL, Hebert C (2001) Chronic exposure of human mesangial cells to high glucose environments activates the p38 MAPK pathway. Kidney Int 60:858–871
Gosmanov AR, Stentz AB, Kitabchi AE (2006) De novo emergence of insulin-stimulated glucose uptake in human aortic endothelial cells incubated with high glucose. Am J Physiol Endocrinol Metab 290:516–522
Igarashi M, Wakasaki H, Takahara N, Ishii H, Jiang ZY, Yamauchi T, Kuboki K, Meier M, Rhodes CJ, King GL (1999) Glucose or diabetes activates p38 mitogen-activated protein kinase via different pathways. J Clin Invest 103:185–195
Hashimoto S, Matsumoto K, Gon Y, Nakayama T, Takeshita I, Horie T (1999) Hyperosmolarity-induced interleukin-8 expression in human bronchial epithelial cells through p38 mitogen-activated protein kinase. Am J Respir Crit Care Med 159:634–640
Hippenstiel S, Soeth S, Kellas B, Fuhrmann O, Seybold J, Krull M, Eichel-Streiber C, Goebeler M, Ludwig S, Suttorp N (2000) Rho proteins and the p38-MAPK pathway are important mediators for LPS-induced interleukin-8 expression in human endothelial cells. Blood 95:3044–3051
Sonna LA, Fujita J, Gaffin SL, Lilly CM (2002) Invited review: effects of heat and cold stress on mammalian gene expression. J Appl Physiol 92:1725–1742
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Noda, A., Kinoshita, K., Sakurai, A. et al. Hyperglycemia and lipopolysaccharide decrease depression effect of interleukin 8 production by hypothermia: an experimental study with endothelial cells. Intensive Care Med 34, 109–115 (2008). https://doi.org/10.1007/s00134-007-0861-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-007-0861-2