Abstract
Objective
We studied the relationship, and the effect of fluid loading on this, between the ratio of extravascular lung water (EVLW) to intrathoracic/pulmonary blood volumes (ITBV, PBV) and the radionuclide pulmonary leak index (PLI) to protein during sepsis-induced acute lung injury/acute respiratory distress syndrome (ALI/ARDS).
Design and setting
A prospective observational study, in the intensive care unit of a university hospital.
Patients
Twenty-two consecutive mechanically ventilated patients with sepsis-related ALI/ARDS from pneumonia (n = 12) or extrapulmonary sources (n = 10), without elevated cardiac filling pressures.
Intervention
Crystalloid (1700–1800 ml) or colloid (1000–1800 ml) fluid loading until target filling pressures.
Measurements and results
Protein permeability was assessed noninvasively over the lungs with help of 67Ga-labeled transferrin and 99mTc-labeled red blood cells (Pulmonary leak index, upper limit normal 14.1 × 10−3 /min) and EVLW and blood volumes by the thermal-dye transpulmonary dilution technique before and after fluid loading. Prior to fluids the pulmonary leak index related to the ratio of EVLW/ITBV and EVLW/PBV (r s = 0.46) particularly when the pulmonary leak index was below 100 × 10−3 /min and in extrapulmonary sepsis (PLI vs. EVLW/PBV r s = 0.71). Fluid loading did not alter EVLW, EVLW/ITBV, or EVLW/PBV or the relationship to PLI.
Conclusion
The data demonstrate that EVLW/ITBV or EVLW/PBV are imperfect measures of increased protein permeability in mechanically ventilated patients with sepsis-induced ALI/ARDS particularly when the PLI is severely increased and during pneumonia, independent of fluid status.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
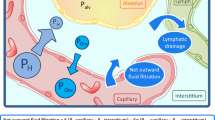
Acute lung injury (ALI) progressing to acute respiratory distress syndrome (ARDS) during sepsis is characterized by pulmonary radiographic, mechanical, and gas exchange abnormalities. These are thought to originate from increased permeability edema following a lung vascular injury, which may be aggravated by fluid loading, which is the first step in treating sepsis-induced hypotension [1, 2, 3]. The lung vascular injury is reflected by an elevated protein permeability, as measured by the noninvasive double-radionuclide 67Ga-labeled transferrin PLI (PLI) [4, 5, 6, 7, 8, 9]. The thermal(-dye) transpulmonary dilution technique allows estimating extravascular lung water (EVLW), but about one-third of ALI/ARDS patients have a normal EVLW [1, 3, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19]. It is unknown whether this can be attributed in part to inaccessibility of the thermal indicator in direct lung injury, thereby underestimating lung edema [1, 3, 12, 15, 16, 18, 19, 20, 21], or to Starling forces and lymph flow offsetting the effect of increased permeability on alveolar fluid volume [10]. Moreover, the ratio of EVLW to intrathoracic or pulmonary blood volume (ITBV, PBV), has been proposed as an index of permeability, but this remains unconfirmed [8, 13, 15, 17]. The ratio has also been suggested to increase by a low plasma colloid osmotic pressure, at least after cardiac surgery [7]. If confirmed, the ratio could help to assess pulmonary permeability at the bedside as a diagnostic tool when the cause of pulmonary edema is unclear and as a monitoring tool during treatment.
We evaluated the contribution of increased protein permeability (pulmonary leak index, PLI) to EVLW and its ratio to ITBV or PBV, and whether this relationship differs between direct and indirect lung injury and is affected by fluid loading by measuring the variables in 22 consecutive, mechanically ventilated patients with pneumonia or extrapulmonary sepsis-induced ALI/ARDS before and after fluid loading.
Patients and methods
This prospective study was approved by the Ethics Committee of the Vrije Universiteit Medical Center, and the 22 consecutive mechanically ventilated patients with sepsis-induced ALI/ARDS in the ICU provided written informed consent (by relatives). The inclusion criteria were the presence of a pulmonary artery (n = 3) or central venous catheter (n = 19) within 24 h of meeting criteria for severe sepsis and ALI/ARDS. Table 1 describes the patients' characteristics. One pneumonia and two extrapulmonary sepsis patients were off vasopressors/inotropes, and the remaining patients had septic shock. Table 2 describes the hemodynamic and pulmonary data for pneumonia and extrapulmonary sepsis patients. ARDS occurred in five patients with pneumonia (42%) of and in two with extrapulmonary sepsis (20%). EVLW was higher than 7 ml/kg in 17 patients with pneumonia (83%) and in five with extrapulmonary sepsis (50%). PLI was above normal in all patients. Only 67% of ALI and 71% of ARDS patients had elevated EVLW. Patients with pneumonia had a higher cardiac index, lower oxygenation ratio and more radiographic densities than patients with extrapulmonary sepsis.
Severe sepsis/septic shock was defined by abnormal body temperature (> 38 °C, < 36 °C), abnormal white blood cell counts (< 4, > 12 × 109 /l or > 10% immature bands), hypotension and need for vasopressor/inotropic therapy (for septic shock), and a clinically evident and microbiologically confirmed source of infection. ICU-acquired sepsis was defined as sepsis developing after 2 days in the ICU. Pneumonia was defined by purulent sputum with a positive blood/tracheal aspirate culture, temperature above 38 °C or below 36 °C and recent-onset densities on chest radiography. Other origins of sepsis were defined on the basis of clinical signs and symptoms and positive local and/or blood cultures. ALI was defined by a lung injury score (LIS) higher than 0 and 2.5 or less, and ARDS by a LIS higher than 2.5 [22] in the absence of overt congestive heart failure or overhydration by virtue of inclusion criteria. The latter included presumed hypovolemia, defined by a systolic blood pressure below 110 mmHg and reduced filling pressures: a pulmonary capillary wedge pressure (PCWP) at or below 10 mmHg in the presence of a pulmonary artery catheter (n = 3) or a central venous pressure (CVP, n = 19) at or below 12 mmHg or 17 mmHg at positive end-expiratory pressure (PEEP) 15 cmH2O; this was done to compare effects of types of fluids in a randomized controlled clinical trial, to be reported later. Exclusion criteria were an age above 78 years, pregnancy, life expectancy less than 24 h, and known anaphylactoid reactions to colloids. After tracheal intubation the lungs were subjected to volume-controlled ventilation with a tidal volume (V t) of 6–8 ml/kg and adjusting respiratory rate to aim at normocarbia, using an O2-air mixture and positive end-expiratory pressure of 5 cmH2O or more, when needed, and an inspiratory to expiratory ratio of 1:2 (Dräger Evita 4, Lübeck, Germany). Patients were otherwise treated for hemodynamic optimization by vasopressor/inotropic support with norepinephrine or dopamine, infection control with antibiotics guided by sensitivities of causing micro-organisms, and continuous renal replacement techniques when indicated on clinical grounds.
PLI was measured as described previously [4, 5, 6, 7, 8, 9]. In brief, autologous red blood cells were labeled with 99mTc (11 MBq, physical half-life 6 h; Mallinckrodt Diagnostica, Petten, The Netherlands). Transferrin was labeled in vivo following intravenous injection of 67Ga-labeled citrate, 4.5 MBq (physical half-life 78 h; Mallinckrodt). Patients were in the supine position, and two scintillation detection probes (Eurorad CTT, Strasburg, France) were positioned over the right and left lung apices. Starting at the time of injection of 67Ga the radioactivity was detected every minute for 30 min. The count rates were corrected for background radioactivity, physical half-life, and spill-over and expressed as counts per minute (CPM) per lung field. During the 30 min after 67Ga injection eight blood samples (2 ml aliquots) were taken. Each blood sample was weighed and radioactivity was determined with a single well well-counter, corrected for background, spillover, and decay (LKB Wallac 1480 Wizard, Perkin Elmer, Life Science, Zaventem, Belgium). Results are expressed as CPM/g. For each blood sample a time-matched CPM over each lung was taken. A radioactivity ratio was calculated (67Ga-lung / 99mTc-lung) / (67Ga-blood / 99mTc-blood) and plotted against time. PLI was calculated by linear regression analysis from the slope of increase in radioactivity ratio divided by the intercept. The PLI represents the transport rate of 67Ga from the intravascular to the extravascular space of the lungs and is therefore a measure of pulmonary vascular protein permeability. The values from the two lung fields were averaged. The upper limit of normal for PLI is 14.1 × 10−3 /min, and measurement error is about 10% [4, 5, 6, 7, 8, 9]. PLI values typically exceed 40 × 10−3 /min in ARDS [4, 5, 6, 7, 8, 9].
The EVLW was measured with help of the transpulmonary thermal-dye dilution technique [1, 3, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19, 20, 21]. A 5-F introducing sheath (Arrow, Reading, Pa., USA) was inserted into the femoral artery. A 4-F fiberoptic thermodilution catheter was inserted in the femoral artery sheath. We injected 15 ml ice cold indocyanine green (1 mg/ml D5W) into a central vein and the thermal-dye dilution curve obtained at the femoral artery (COLD Z-021, Pulsion Medical Systems, Munich, Germany). This allowed calculation of the transpulmonary cardiac output, the global end-diastolic volume (GEDV), ITBV, PBV, and the extravascular thermal volume in the lungs as a measure of EVLW (normal < 7–10 ml/kg) [1, 3, 11, 12, 14, 20]. EVLW is typically above 10 ml/kg and elevated two- to threefold in cases of overt (radiographic) pulmonary edema [1, 3, 11, 12, 14, 20]. The normal ratio of EVLW/ITBV( is 0.2–0.3 and the normal EVLW/PBV ratio about 1 [7, 8, 13, 15, 17]. Measurements were carried out in duplicate and averaged. The cardiac output, GEDV, ITBV, and PBV were indexed to body surface area (cardiac index and blood volume indices, GEDVI, ITBVI, and PBVI) and EVLW to body weight (kg). Hemodynamics was included in the study since it may affect pulmonary variables.
LIS was calculated from the number of quadrants on the chest radiograph with densities, the PEEP level, the arterial PO2 (PaO2)/inspiratory O2 fraction (FIO2) and the total respiratory dynamic compliance [22]. The latter was calculated from tidal volume/(plateau pressure-PEEP), in ml/cmH2O. The chest radiograph was scored by a consultant radiologist blinded to the study who evaluated the number of quadrants with alveolar densities, ranging from 0 to 4. LIS values range between 0 (no injury) to 4, with those above 2.5 indicative of ARDS and those between 0 and 2.5 of ALI [22].
Demographics were recorded, including variables for calculation of Acute Physiology and Chronic Health Evaluation (APACHE) II score. EVLW, 67Ga-labeled transferrin PLI, and hemodynamics were measured, and an anteroposterior chest radiograph was made. Hemodynamic variables were measured after calibration and zeroing to atmospheric pressure at midchest level (Tramscope, Marquette, Wisc., USA). The central venous pressure was taken at end-expiration, with patients in the supine position. Arterial blood samples were obtained for determinations of partial O2/CO2 pressures (Rapidlab 865, Bayer Diagnostics, Tarrytown, NY, USA; at 37 °C). The plasma colloid osmotic pressure was measured by a membrane osmometer (Osmomat 050, Gonotex, Berlin, Germany; molecular cutoff at 20 kDa, normal about 24 mmHg). The FIO2, tidal volume, plateau inspiratory pressure, and PEEP (per cmH2O) were taken from the ventilator. Doses of vasoactive drugs were recorded. Variables were recorded and chest radiographs made before and after a 90-min fluid loading with crystalloid (n = 6) or colloid solution (n = 16) according to a pressure-guided fluid loading protocol published previously [9]. The fluid loading protocol is based on a change in the central venous pressure by a 100- to 200-ml bolus infusion per 10 min, aiming at a target central venous pressure of 13 or 18 mmHg if PEEP was 15 cmH2O or higher. The maximum amount to be infused is thus 1800 ml. Ventilatory settings and vasopressor/inotropic doses were unaltered during fluid loading. Patients were taken care of by intensive care physicians not involved in the study and followed until extubation and discharge/death in the ICU. Mortality as reported here is ICU mortality.
For statistical analysis we compared pneumonia and extrapulmonary sepsis-induced ALI/ARDS groups, using the nonparametric Mann-Whitney U test for continuous and with help of Fisher's exact test for categorical data. The Wilcoxon signed rank test was used for paired data. Spearman's correlation coefficient was used to express the strength of relationships. Exact p values below 0.10 are given and values below 0.05 are considered to indicate statistical significance. All tests were two-tailed. Data are summarized as median and range.
Results
Effect of fluid loading
Table 2 describes the effect of 90 min fluid loading of a total of 1700–1800 ml crystalloid or 1000–1800 of colloid solution in the two groups. The cardiac index increased along with preload parameters, including the central venous pressure, GEDVI and ITBVI. During fluid loading in pneumonia PLI increased but not the EVLW and EVLW to blood volume ratios. Ventilatory plateau pressure increased, and therefore compliance decreased. Otherwise, the two groups did not differ in the response to fluids. The EVLW (ratios) and PLI did not differ according to fluid types before and after loading.
Correlations
Prior to fluid loading there was a direct relationship in the overall series between the PLI and the EVLW to ITBV or PBV ratio (Fig. 1). After fluid loading the EVLW/PBV ratio was also related to PLI (r s = 0.43, p = 0.045). In extrapulmonary sepsis before fluids PLI was related to EVLW/PBV (r s = 0.71, p = 0.022). In pneumonia alone no such significant correlations were observed either before or after fluid loading. At a PLI lower than 100 × 10−3 /min (n = 18) the EVLW/ITBV and EVLW/PBV were related even more closely to PLI: r s = 0.50, p = 0.035 and r s = 0.57, p = 0.014 before fluid loading and r s = 0.50–0.51, p = 0.034, after fluid loading. The highest correlation between PLI and EVLW/PBV was found in extrapulmonary sepsis, when PLI was lower than 100 × 10−3 /min and before fluid loading: r s = 0.83, p = 0.01.
Relationship between pulmonary leak index (PLI) and ratio of extravascular lung water (EVLW) to intrathoracic blood volume (ITBV), which is normally 0.2–0.3 (dashed lines) in patients with pneumonia or sepsis, before fluid loading (r s = 0.46, p = 0.032). A similar direct relationship was observed for PLI vs. EVLW/pulmonary blood volume. Logarithmic scale on the X-axis, for the purpose of clarity
PLI, EVLW, EVLW/ITBV, and EVLW/PBV values after fluid loading were related to those before (minimum r s = 0.77, p < 0.0001), indicating reproducibility of measurements after fluid loading. Furthermore there was no relationship with (changes in) the colloid osmotic pressure. Both before and after fluid loading ITBV was directly related to GEDV (r s = 0.95, p < 0.0001), with ITBV being 16–23% higher than GEDV, similarly in pneumonia and extrapulmonary sepsis. EVLW was not related to central venous pressure but to GEDVI and ITBVI after fluid loading (minimum r s = 0.47, p = 0.029).
Discussion
Our results demonstrate that lung vascular injury is associated with a rise in EVLW to ITBV or PBV ratio in mechanically ventilated patients with pneumonia or extrapulmonary sepsis-induced ALI/ARDS. These data nevertheless indicate that the ratios are imperfect measures of protein permeability (PLI), particularly when PLI is substantially increased and during pneumonia. The relationships are not affected by fluid loading augmenting preload or by cardiac index.
The EVLW to ITBV or PBV ratios have been suggested to reflect increased permeability edema, but this has not yet been confirmed [3, 7, 8, 13, 15, 17], although we have previously noted high ratios concomitant with an elevated PLI after major vascular surgery [8]. In contrast, a high ratio may also result from a low plasma colloid osmotic (to hydrostatic) pressure (gradient) promoting fluid filtration into the lungs, rather than increased permeability, at least after cardiac surgery [7]. Our findings indicate for the first time that there is a moderate and direct relationship between independently measured pulmonary protein permeability and EVLW ratios during extrapulmonary sepsis, independently of fluid loading and the plasma colloid osmotic pressure. Moreover, we observed a tendency to a closer relationship of PLI to EVLW/PBV than to EVLW/ITBV, while both have been used in the literature [3, 7, 8, 13, 15, 17]. A better relationship has been noted between EVLW and filling volumes than pressures in sepsis [14]. That increased permeability was only loosely linked to edema (Fig. 1), may be due in part, to the concomitant effect of other Starling factors affecting edema formation in the lungs, including lymph flow [10], as well to sampling error by the radionuclide probes compared to thermal distribution volume measurements or to combinations. In any case EVLW was normal in about 30% of patients, in agreement with the literature [3, 18, 21]. Conversely, our data suggest that PLI is a greater determinant of the manifestations of sepsis-induced lung injury than EVLW since, in contrast to EVLW, it was elevated in all patients.
Fluid loading increased cardiac preload and thereby the cardiac index and lowered total respiratory dynamic compliance without elevating EVLW. The fall in compliance can thus be attributed to increased intrathoracic and intrapulmonary intravascular filling rather than augmentation of edema fluid. Although the EVLW (and ratios) was not related to the colloid osmotic pressure, we cannot exclude that an increase in colloid osmotic pressure prevented a rise in EVLW during fluid loading and increased filling, although pulmonary microvascular permeability was increased and may have decreased the effective transvascular colloid osmotic pressure gradient ameliorating fluid filtration. Nevertheless, the high PLI during pneumonia was further increased by fluid loading, probably as a consequence of augmented microvascular protein filtration during increased fluid filtration. That the EVLW remained unchanged may have been caused by poor accessibility to the thermal indicator, by increased lymph flow, or both. Together, the data may explain the poor relationship between PLI and EVLW/ITBV or PBV during pneumonia before and after fluid loading. Experimental literature suggests that, compared to the gravimetric methods, the double indicator dilution method may somewhat underestimate pulmonary edema in direct, as opposed to indirect, ALI/ARDS [16, 20].
We obtained our EVLW (indices) with help of a thermal-dye transpulmonary dilution technique, while in the currently advocated and validated single thermodilution technique [3, 19, 23] EVLW is assessed from intrathoracic thermal distribution volume and ITBV, which is calculated from GEDV assuming a constant relationship. The constant relationship was confirmed in our study as well as the roughly 20% higher ITBV than GEDV, apparently independently of fluid loading increasing preload. The single thermodilution technique to assess EVLW is fully comparable to the double indicator dilution method, according to the literature [19], so that we may speculate that our current results also apply to those obtained after single thermal dilution.
In conclusion, our study in mechanically ventilated patients with sepsis-induced ALI/ARDS suggests that EVLW/ITBV and EVLW/PBV are imperfect measures of increased protein permeability, particularly if severely increased and during pneumonia, independently of fluid status and the colloid osmotic pressure.
References
Sakka SG, Klein M, Reinhart K, Meier-Hellman A (2002) Prognostic value of extravascular lung water in critically ill patients. Chest 122:2080–2086
Piantadosi CA, Schwartz DA (2004) The acute respiratory distresss syndrome. Ann Intern Med 141:460–470
Martin GS, Eaton S, Mealer M, Moss M (2005) Extravascular lung water in patients with severe sepsis: a prospective cohort study. Crit Care 9:R74–R82
Groeneveld ABJ (1997) Radionuclide assessment of pulmonary microvascular permeability. Eur J Nucl Med 34:449–461
Groeneveld ABJ, Raijmakers PGHM (1997) The 67Ga transferrin pulmonary leak index in pneumonia and associated adult respiratory distress syndrome. Clin Sci 92:463–470
Groeneveld ABJ, Raijmakers PGHM (1998) The 67gallium-transferrin pulmonary leak index in patients at risk for the acute respiratory distress syndrome. Crit Care Med 26:685–691
Verheij J, Van Lingen A, Raijmakers RGHM, Spijkstra JJ, Girbes ARJ, Jansen EK, Van den Berg FG, Groeneveld ABJ (2005) Pulmonary abnormalities after cardiac surgery are better explained by atelectasis than by increased permeability oedema. Acta Anaesthesiol Scand 49:1302–1310
Groeneveld ABJ, Verheij J, Van den Berg FG, Wisselink W, Rauwerda JA (2006) Increased pulmonary capillary permeability and extravascular lung water after major vascular surgery: effect on radiography and ventilatory variables. Eur J Anaesthesiol 23:36–41
Verheij J, van Lingen A, Raijmakers PGHM, Rijnsburger ER, Veerman DP, Wisselink W, Girbes ARJ, Groeneveld ABJ (2006) Effect of fluid loading with saline or colloids on pulmonary permeability, oedema and lung injury score after cardiac and major vascular surgery. Br J Anaesth 96:21–30
Schuster DP, Haller J (1990) A quantitative correlation of extravascular lung water accumulation with vascular permeability and hydrostatic pressure measurements: a positron emission tomographic study. J Crit Care 5:161–168
Goedje O, Peyerl M, Seebauer T, Dewald O, Reichart B (1998) Reproducibility of double indicator dilution measurements of intrathoracic blood volume compartments, extravascular lung water, and liver function. Chest 113:1070–1077
Davey-Quinn A, Gedney JA, Whiteley SM, Bellamy MC (1999) Extravascular lung water and acute respiratory distress syndrome-oxygenation and outcome. Anaesth Intensive Care 27:357–362
Honoré PM, Jacquet LM, Beale RJ, Renauld J-C, Valadi D, Noirhomme P, Goenen M (2001) Effects of normothermia versus hypothermia on extravascular lung water and serum cytokines during cardiopulmonary bypass: a randomized, controlled trial. Crit Care Med 29:1903–1906
Holm C, Tegeler J, Mayr M, Pfeiffer U, Henckel von Donnersmarck G, Mühlbauer W (2002) Effect of crystalloid resuscitation and inhalation injury on extravascular lung water. Chest 121:1956–1962
Boussat S, Jacques T, Levy B, Laurent E, Gache A, Capellier G, Neldhardt A (2002) Intravascular volume monitoring and extravascular lung water in septic patients with pulmonary edema. Intensive Care Med 28:712–718
Groeneveld AB, Verheij J (2004) Is pulmonary edema associated with a high extravascular thermal volume? Crit Care Med 32:899–901
Matejovic M, Krouzecky A, Rokyha R, Novak I (2004) Fluid challenge in patients at risk for fluid loading-induced pulmonary edema. Acta Anaesthesiol Scand 48:690–673
Michard F, Zarka V, Alaya S (2004) Better characterization of acute lung injury/ARDS using lung water. Chest 125:1166
Michard F, Schachtrupp A, Toens C (2005) Factors influencing the estimation of extravascular lung water by transpulmonary thermodilution in critically ill patients. Crit Care Med 33:1243–1247
Roch A, Michelet P, Lambert D, Delliaux S, Saby C, Perrin G, Ghez O, Bregeon F, Thomas P, Carpentier J-P, Papazian L, Auffray J-P (2004) Accuracy of the double indicator method for measurement of extravascular lung water depends on the type of acute lung injury. Crit Care Med 32:811–817
Groeneveld AB, Polderman KH (2005) Acute lung injury, overhydration or both? Crit Care 9:136–137
Murray JF, Matthay MA, Luce JM, Flick MR (1988) An expanded definition of the adult respiratory distress syndrome. Am Rev Respir Dis 138:720–723
Kirov MY, Kuzkov VV, Kuklin VN, Waerhaug K, Bjertnaes LJ (2004) Extravascular lung water assessed by transpulmonary single thermodilution and postmortem gravimetry in sheep. Crit Care 8:R451–R458
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Groeneveld, A.B.J., Verheij, J. Extravascular lung water to blood volume ratios as measures of permeability in sepsis-induced ALI/ARDS. Intensive Care Med 32, 1315–1321 (2006). https://doi.org/10.1007/s00134-006-0212-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-006-0212-8