Abstract
Objective
Many tests have been used to predict outcome following severe brain injury. We compared predictive powers of clinical examination (pupillary responses, motor responses and Glasgow Coma Scale, GCS), electroencephalography (EEG) and computed tomography (CT) to that of somatosensory evoked potentials (SEPs) in a systematic review.
Materials and methods
Medline (1976–2002) and Embase (1980–2002) were searched, manual review of article reference lists was conducted, and authors were contacted. We selected 25 studies addressing the prediction of outcome after severe brain injury using SEPs and either GCS, EEG, CT, pupillary or motor responses. Outcomes were determined for patients with normal or bilaterally absent SEPs and graded measures of GCS, EEG, CT, pupillary responses or motor responses. For favourable outcome prediction SEPs were superior in sensitivity, specificity and positive and negative predictive values, except for pupillary responses which had superior sensitivity and GCS which had higher specificity. SEPs had superior summary receiver operating characteristic curves, with the exception of motor responses, and superior ratio of odds ratios. For unfavourable outcome prediction SEPs were superior to the other tests in sensitivity, specificity and positive and negative predictive values, except for motor and pupillary responses, GCS and CTs which had superior sensitivity. All SEP summary receiver operating characteristic curves and pooled ratio of odds ratios were superior.
Conclusions
Although imperfect, SEPs appear to be the best single overall predictor of outcome. There is sufficient evidence for clinicians to use SEPs in the prediction of outcome after brain injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Many studies over the past 20 years have identified various clinical, electrophysiological and radiological tests that may be used as predictors of outcome. Zandbergen et al. [1] demonstrated the power of somatosensory evoked potentials (SEPs) compared indirectly to other tests to predict unfavourable outcome in a systematic review of anoxic coma. In addition, a recent systematic review [2] after all forms of brain injury showed the high predictive power and low false-positive rate of SEPs (specificity 98.7%, 97.7–99.3%) for unfavourable outcome but did not compare them to other tests. A proper, direct comparison of tests is required. The aim of the current study was to perform a systematic review summarising the published data for tests predicting outcome following acute, severe brain injury and to directly compare the predictive power of the common tests of motor responses, pupillary responses, the Glasgow Coma Scale (GCS), electroencephalography (EEG), and computed tomography (CT) to that of SEPs.
Methods
Studies were identified by two means. First, the databases Medline (1976–December 2002) and Embase (1980–March 2002) were searched using combinations of the terms somatosensory evoked potentials/response, electroencephalography, X-ray computed tomography, Glasgow Coma Scale, brain injury, head injury, coma, hypoxaemia, anoxia, heart arrest, outcome, health status, predictive value, sensitivity, specificity and related key words. Secondly, we conducted a manual review of articles’ bibliography and contacted the authors. The studies included had to include patients described as “severely” brain injured or “comatose” or have the majority of patients with a GCS less than 8 and allow the determination of outcomes in association with graded measures for at least one of either the GCS, EEG, CT or a clinical feature (pupillary response or motor response) and all patients with bilaterally absent SEPs in order to generate appropriate 2×2 tables. Case reports, studies using neonatal subjects, abstracts, studies that were duplicates of other studies and studies dealing only with brain dead subjects were excluded from the systematic review. Non-English-language studies were included if translation was possible.
Data analysis consisted of determining the relationship between dichotomised test and outcome data using standard 2×2 tables. Outcomes were defined as favourable or unfavourable: a favourable outcome consisted of the Glasgow Outcome Scale categories of normal and moderate while severe disability, vegetative state or death were considered unfavourable outcomes. For SEPs, outcomes were determined for patients with normal, abnormal and bilaterally absent SEPs. The cut-off points (thresholds) for the other predictors used are specified in the result tables. Separate 2×2 tables were generated for the prediction of favourable and unfavourable outcome. The number of true positives (test positive and outcome positive), false positives (test positive and outcome negative), true negatives (test negative and outcome negative) and false negatives (test negative and outcome positive) were determined for each test in each study in order to generate a standard 2×2 table for the use of SEPs and at least one other predictive measure. Data were excluded if an entire row of the 2×2 table consisted of cells with a value of 0. A number of specific methodological criteria were recorded from each study: whether the test was conducted and classified in a blinded manner, whether patient enrolment was prospective and consecutive, details of study entry criteria, patient characteristics and SEP methodology.
Sensitivity, specificity, positive predictive value, negative predictive value and odds ratio (OR) were calculated for each test for the prediction of favourable and unfavourable outcome. Exact 95% confidence intervals were calculated using the binomial distribution for the proportions. If one or more of the fields of the 2×2 table were empty, 0.5 was added to all cells (Yates’ correction). All data analysis was performed using a computer software package (version 6.0, Stata, College Station, Tex., USA).
Comparisons were made between test results to identify which test has superior performance in regard to sensitivity, specificity, positive and negative predictive value and odds ratio. Formal meta-analysis was conducted using the technique of summary receiver operating characteristic curves (sROC) [3, 4]. The results were also summarised by dividing the odds ratio for SEPs by the odds ratio for the other test to determine the ratio of odds ratios (ROR) for each study. A ROR greater than 1 indicates superior performance of SEPs while a ROR less than 1 indicates inferior performance of SEPs compared to the other test. ORs and RORs were tested for homogeneity while individual study RORs were pooled for each comparison using a random effects model with weighting inversely proportional to the variance [5].
Results
We initially identified 151 publications, 126 of which were excluded for various reasons: could not generate 2×2 table (40%), study not prospective/retrospective (31%), SEPs compared to other test (17%), incorrect patient group (5%), long latency SEPs (3%), row of data consisting only of zeros (2%), not used to predict outcome (1%) and duplicate study (1%). Twenty-five English-language studies [6, 7, 8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30] and four non-English-language studies [27, 28, 29, 30] were identified that compared SEPs to other predictors (Table 1). Ten studies described their patients as “comatose” or “severely” injured while six consisted only of patients with a GCS less than 8, and nine studies also included some patients with GCS of 8 or higher. Only four studies focused specifically on children [8, 24, 25, 29] while nine included both children and adults [6, 12, 13, 15, 17, 20, 22, 28, 30].
SEP methods typically involved repeat median nerve stimulation at a level above the motor threshold at a rate of 3–6 Hz with recordings made from the neck and contralateral parietal cortex (C3/4 or 2 cm behind) in accordance with published recommendations [31, 32]. Some studies used filters outside the recommended ranges [6, 10, 11, 12, 13, 14, 15, 16, 17, 22, 26], a stimulus intensity below motor threshold [16, 19] or a high stimulation rate [23]. While 14 studies compared SEPs with only one other predictor, 10 compared two other predictors to SEPs, and one study compared SEPs to four predictors. Some of the studies provided details on the timing of SEPs and the other tests. SEPs and the other tests were typically performed at different times in different studies, generally within the first few days following injury with the initial test results commonly used. Only the tests in three studies [6, 18, 19] appear to have been performed simultaneously with SEPs. The results of the comparisons between SEPs and GCS, pupillary responses, motor responses, EEGs, and CT are presented, respectively, in Tables 2, 3, 4, 5, and 6.
In 61% of patients (range 14–90%) there was a unfavourable outcome, with 43% (range 17–80%) dying. For the prediction of unfavourable outcome SEPs were associated with far fewer false positives than the other tests. Only eight false positives were reported with the use of SEPs across all comparisons. Seven of these false positives, four in the study by Beca et al. [8] and one each in those by Pohlmann-Eden [20], Rumpl et al. [22] and Taylor and Farrell [24] failed to meet the criteria required for the proper determination of a bilaterally absent response [2]. The studies by Beca et al. [8] and Taylor and Farrell [24] included only children. By comparison, there were 77 false positives associated with the GCS, 17 with CT, 12 with pupillary responses, 8 with motor responses and 3 with the EEG. SEPs also tended to have higher numbers of true negatives than other tests. On the other hand, SEPs tended to be associated with higher numbers of false negatives and fewer true positives than the other tests. For favourable outcome prediction the only clear pattern is the tendency for SEPs to be associated with higher numbers of true positives and fewer false negatives than the other tests and their higher rate of false positives than the GCS.
Table 7 provides a comparison of the number of times that SEPs had higher, equal or lower values of sensitivity, specificity, positive predictive value and negative predictive value than each of the other tests. These comparisons showed that for unfavourable outcome prediction SEPs tended to display lower sensitivity, higher specificity, higher positive predictive value and lower negative predictive value. Motor responses, pupillary responses, GCS and CT tended to have higher sensitivity than SEPs. The specificity and positive predictive value of SEPs was consistently equal to or greater than that of all other tests. For favourable outcome prediction SEPs tended to display higher sensitivity, specificity, positive predictive value and negative predictive value. Exceptions were for pupillary response which had higher sensitivity and the GCS, which tended to have better specificity.
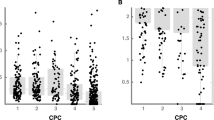
Figure 1 summarises the sensitivity and specificity data in sROC curves. These curves show that the SEP characteristics are superior to all but one of the other tests for both favourable and unfavourable outcome prediction. The exception is for the comparison with motor responses for favourable outcome prediction, where the two sROC curves intersect and show significant overlap. Examination of the results of paediatric studies and those consisting only of patients suffering traumatic brain injury (TBI) or hypoxic-ischemic encephalopathy (HIE) compared to the other studies failed to identify any differences. Individual points on the sROC curves show considerable variation, even amongst studies consisting of only children or patients suffering only TBI or HIE which are widely distributed amongst the other studies. There was a suggestion however of better sensitivity for SEPs for unfavourable outcome prediction amongst HIE patients.
Summary receiver operating characteristic curves comparing SEPs and other predictors: left for the prediction of favourable outcome; right for the prediction of unfavourable outcome. Filled circles, heavy line SEPs; empty circles, light line respective comparative predictor Glasgow Coma Scale (a), pupillary response (b), motor response (c), electroencephalography (d), computed tomography (e). TPR True positive rate (=sensitivity); FPR false positive rate (=1−specificity). Note that the data displayed are after Yates’ correction
Pooled RORs were all greater than 1 (Table 8). Statistical significance (p≤0.05) was reached only for the GCS (unfavourable) and CT (favourable) comparisons, due to wide confidence intervals for individual studies.
Discussion
Despite their availability for over 20 years it is alarming how few studies have directly compared the performance of SEPs to that of the more commonly used tests. Only studies that directly compared tests using a paired design were included in this systematic review in order to control for variation, as occurs within the design of randomised controlled trials, and because this is the most efficient and powerful means to perform such a comparison [3, 4, 33, 34, 35, 36]. The variation displayed amongst the individual results of studies, as shown by the spread of data in the sROCs, indicates how misleading comparisons can be if the results of individual tests obtained from different studies are simply compared.
The various results presented here suggest that SEPs are superior to pupillary responses, motor responses, GCS, EEG and CT for the prediction of outcome after acute, severe brain injury. We compared the tests in a number of ways to determine this. The formal meta-analysis with ORs was performed because the OR value is a good overall measure of a test’s statistical discriminatory power and a good way to contrast two tests and relates to the test’s sROC curves. Although significant in only two instances, pooled RORs were all greater than 1, with most individual studies reporting RORs greater than 1. The ROR confidence intervals also tended to extend further above 1 than below. A comparison of sensitivity, specificity and positive and negative predictive values was also performed because these values are clinically important (Table 7). sROC curves also summarise the relationship between sensitivity and specificity and portray its variation between studies while presenting the data visually. For two intersecting sROC curves, as for SEPs and motor responses for favourable outcome prediction, the question of which test is better depends on the circumstances of its use. The advantage of SEPs over motor responses is that it is common to be unable to assess motor function due to sedation or paralysis while SEPs are unaffected in these situations.
It is possible that other individual tests not compared here are superior to SEPs. This systematic review focussed on the most commonly used and available tests. Individual studies have compared SEPs to many tests, ranging from other evoked potential tests to biochemical markers. It is well documented that SEPs are the most powerful of the standard evoked potential modalities [6, 9, 20, 24, 37, 38, 39, 40, 41, 42, 43] although work by Madl et al. [18, 44] and Shermon et al. [45] suggest that long latency SEP components are superior to standard SEPs due to their higher sensitivity. Long latency components are reportedly more prone to technical artefacts and the effects of sedation than SEPs, however [45, 46, 47], which makes them potentially unsuitable in an ICU setting. Also, the use of SEPs recorded over the frontal cortex, rather than the standard parietal recordings, has shown promise as a more powerful predictor of outcome [13, 48, 49]. Two new biochemical markers, serum neuron-specific enolase [50, 51] and brain lactate measured by proton magnetic resonance spectroscopy [46], also appear to have good promise as predictors of outcome. These tests need further testing, including direct comparisons with suitable alternatives, such as SEPs, motor responses and pupillary responses.
Although this review shows that SEPs are excellent predictors of outcome when compared to a number of standard tests, they are not perfect. Some of the other tests perform better than SEPs in some regard. While SEPs are the best overall predictor of outcome, motor responses, pupillary responses, GCS and CT had better sensitivity for unfavourable outcome prediction while the pupillary responses had better sensitivity and GCS better specificity for favourable outcome prediction. Although specificity for predicting unfavourable outcome with SEPs approaches 100%, sensitivity and the specificity for favourable outcome prediction is not as good. While this could be improved with repeat testing and exclusion of patients who die of non-neurological disorders [2], the combined use of SEPs with other predictive tests is also likely to improve the accuracy of outcome predictions, although some compromises are likely. Various tests have been reported to improve the accuracy of favourable and unfavourable outcome when used in conjunction with SEPs. The additional measurement of frontal SEPs or motor SEPs [12, 13, 48, 49], EEG [21] or EEG reactivity [14] has improved the accuracy of outcome predictions when combined with SEPs. Schreiner and Pohlmann-Eden [51] and Sherman et al. [45] have also reported that the biochemical markers serum neuron-specific enolase and creatine kinase BB, respectively, improve the accuracy of unfavourable outcome prediction when combined with SEP results. Clinical features such as those investigated here, including the GCS, pupillary responses and motor responses, also improve the predictive powers of SEPs [7, 10, 23, 39, 52, 53, 54]. Kane et al. [55] reported that the combination of mismatch negativity and the GCS with SEPs was the best predictor of outcome while Ying et al. [26] also combined a number of tests, clinical and motor evoked potentials, with SEPs to obtain the best outcome prediction of mortality. Additional research is required to identify the most powerful combination of predictive tests.
The sROC curves show the variation in results that can exist between studies. One factor potentially causing this variation is the relative timing of the individual tests. Only three studies [6, 18, 19] appear deliberately to have performed the tests simultaneously with most studies conducting the tests independently, over wide time periods. This causes variation in the relative predictive power of tests within a study as well as introducing variation between studies. Clinical heterogeneity can also cause variations in results. Many factors, such as treatment strategies, SEP methodologies and patient characteristics, can influence between-study results but are largely controlled for when within-study results are examined. One limitation of all included studies, and common to other studies examining outcome prediction in general, is the lack or absence of details on the approach to the withdrawal of treatment. This is difficult to avoid, however. Ethical concerns prevent ongoing maximal treatment to patients thought to have a poor prognosis [56] and only two included studies [7, 10] reported the provision of maximal treatment for a predetermined minimal period (3 days). While many of the studies blinded clinicians to SEPs, other parameters were not blinded and were available to be used in the decision to withdraw or to continue treatment. This may bias the results but should add more weight to the findings on the relative performance of SEPs.
A comparison of the results of different studies using only paediatric patients and those using only patients suffering TBI compared to HIE failed to show any differences, although this was limited by small numbers and/or restricted variation between studies, except in the GCS comparison where SEPs had a better sensitivity for unfavourable outcome prediction amongst patients suffering HIE. This may be due to differences in the pathological changes or their changes over time between the two types of injury. There is also evidence [2] that false positives for unfavourable outcome prediction are more likely in children and after TBI.
The results presented here suggest that SEPs are the best single overall predictor of outcome, but that standard clinical tests—GCS, pupillary and motor responses—may improve overall predictive ability when combined with SEPs. SEPs must of course be performed following the correct technical procedures and interpreted with the appropriate expertise [2]. Although not as simple to perform as the clinical signs, SEPs can be determined in the presence of sedation and paralysis, are easily performed in an ICU and are easier to record and interpret than EEGs. Although no single predictor can predict outcome with certainty, and combinations are required [1, 44, 52, 57, 58, 59, 60, 61], we suggest that there is sufficient evidence for clinicians to incorporate SEPs into the prediction of outcome after brain injury.
References
Zandbergen EGJ, de Haan RJ, Stoutenbeek CP, Koelman JHTM, Hijdra A (1998) Systematic review of early prediction of poor outcome in anoxic-ischaemic coma. Lancet 352:1808–1812
Carter BG, Butt W (2001) A review of the use of somatosensory evoked potentials (SEPs) in the prediction of outcome after severe brain injury. Crit Care Med 29:178–186
Irwig L, Macaskill P, Glasziou P, Fahey M (1995) Meta-analytic methods for diagnostic test accuracy. J Clin Epidemiol 45:119–130
Moses LE, Shapiro D, Littenberg B (1993) Combining independent studies of a diagnostic test into a summary ROC curve: data analytic approach and some additional considerations. Stat Med 12:1293–1316
DerSimonian R, Laird NM (1986) Meta-analysis in clinical trials. Control Clin Trial 7:177–188
Anderson DC, Bundlie S, Rockswold GL (1984) Multimodality evoked potentials in closed head trauma. Arch Neurol 41:369–374
Bassetti C, Bomio F, Mathis J, Hess CW (1996) Early prognosis in coma after cardiac arrest: a prospective clinical, electrophysiological, and biochemical study of 60 patients. J Neurol Neurosurg Psychiatry 61:610–615
Beca J, Cox PN, Taylor MJ, Bohn D, Butt W, Logan WJ, Rutka JT, Barker G (1995) Somatosensory evoked potentials for prediction of outcome in acute severe brain injury. J Pediatr 126:44–49
Cant BR, Hume AL, Judson JA, Shaw NA (1986) The assessment of severe head injury by short-latency somatosensory and brain-stem auditory evoked potentials. Electroencephalogr Clin Neurophysiol 65:188–195
Chen R, Bolton CF, Young GB (1996) Prediction of outcome in patients with anoxic coma: a clinical and electrophysiologic study. Crit Care Med 24:672–678
DeGiorgio CM, Rabinowicz AL, Gott PS (1993) Predictive value of P300 event-related potentials compared with EEG and somatosensory evoked potentials in non-traumatic coma. Acta Neurol Scand 87:423–427
Facco E, Baratto F, Munari M, Dona B, Liviero MC, Behr AU, Giron GP (1991) Sensorimotor central conduction time in comatose patients. Electroencephalogr Clin Neurophysiol 80:469–476
Facco E, Munari M, Dona B, Baratto F, Fiore D, Behr AU, Giron G (1991) Spatial mapping of SEP in comatose patients: improved outcome prediction by combined parietal N20 and frontal N30 analysis. Brain Topogr 3:447–455
Gutling E, Gonser A, Imhof H-G, Landis T (1995) EEG reactivity in the prognosis of severe head injury. Neurology 45:915–918
Judson JA, Cant BR, Shaw NA (1990) Early prediction of outcome from cerebral trauma by somatosensory evoked potentials. Crit Care Med 18:363–368
Hollerbach S, Kullmann F, Bartsch H, Lögl C, Geissler A, Zeuner M, Leser HG, Schölmerich J (1995) Prediction of outcome in resuscitated patients by clinical course and early somatosensory-evoked potentials. A comparison with the Glasgow coma scale (GCS) and cranial-computed tomography (CCT). Clin Intensive Care 6:219–227
Hutchinson DO, Frith RW, Shaw NA, Judson JA, Cant BR (1991) A comparison between electroencephalography and somatosensory evoked potentials for outcome prediction following severe head injury. Electroenceph Clin Neurophysiol 78:228–233
Madl C, Grimm G, Kramer L, Yeganehfar W, Sterz F, Schneider B, Kranz A, Schneeweiss B, Lenz K (1993) Early prediction of individual outcome after cardiopulmonary resuscitation. Lancet 341:855–858
Nakabayashi M, Kurokawa A, Yamamoto Y (2001) Immediate prediction of recovery of consciousness after cardiac arrest. Intensive Care Med 27:1210–1214
Pohlmann-Eden B, Dingethal K, Bender H-J, Koelfen W (1997) How reliable is the predictive value of SEP (somatosensory evoked potentials) patterns in severe brain damage with special regard to the bilateral loss of cortical responses. Intensive Care Med 23:301–308
Rothstein TL, Thomas EM, Sumi SM (1991) Predicting outcome in hypoxic-ischaemic coma. A prospective clinical and electrophysiological study. Electroenceph Clin Neurophysiol 79:101–107
Rumpl E, Prugger M, Gerstenbrand F, Hackl JM, Pallua A (1983) Central somatosensory conduction time and short latency somatosensory evoked potentials in post-traumatic coma. Electroencephalogr Clin Neurophysiol 56:583–596
Sandroni C, Barelli A, Piazza O, Proietti R, Mastria D, Boninsegna R (1995) What is the best test to predict outcome after prolonged cardiac arrest? Eur J Emerg Med 2:33–37
Taylor MJ, Farrell EJ (1989) Comparison of the prognostic utility of VEPs and SEPs in comatose children. Pediatr Neurol 5:145–150
Whittle IR, Johnston IH, Besser M (1987) Short latency somatosensory-evoked potentials in children. III. Findings following head injury. Surg Neurol 27:29–36
Ying Z, Schmid UD, Schmid J, Hess CW (1992) Motor and somatosensory evoked potentials in coma: analysis and relation to clinical status and outcome. J Neurol Neurosurg Psychiatry 55:470–474
Cheliout-Heraut F, Durand MC, Clair B, Gajdos P, Raphaël JC (1992) Prognosis value of evoked potentials in the postanoxic comas in adult. Neurophysiol Clin 22:269–280
Maurer E, Milewski P (1998) Usefulness and diagnostic value of evoked potentials in surgical ICU patients with neurological deficits. Anasthesiol Intensivmed Notfallmed Schmerzther 33:430–440
Parain D, Devaux AM, Proust B (1989) The contribution of EEG and evoked potentials in the post-anoxic prognosis of coma in children. Neurophysiol Clin 19:489–494
Riffel B, Stöhr M, Graser W, Trost E, Baumgärtner H (1989) Early outcome prediction in patients with severe head injury by Glasgow Coma Score and evoked potentials. Anaesthesist 38:51–58
Anonymous (1994) Guideline 9. Guidelines on evoked potentials. J Clin Neurophysiol 11:40–73
Mauguiere F, Allison T, Babiloni C, Buehner H, Eisen AA, Goodin DS, Jones SJ, Kakigi R, Matsuoka S, Nuwer M, Rossini PM, Shihasaki H (1999) Somatosensory evoked potentials. Electroencephalogr Clin Neurophysiol Suppl 52:79–90
Shapiro DE (1999) The interpretation of diagnostic tests. Stat Methods Med Res 8:113–134
Begg CB, McNeil BJ (1988) Assessment of radiologic tests: control of bias and other design considerations. Radiology 167:565–569
Zweig MH, Campbell G (1993) Receiver-operating characteristic (ROC) plots: a fundamental evaluation tool in medical research. Clin Chem 39:561–577
Irwig L, Tosteson ANA, Gatsonis C, Law J, Colditz G, Chalmers TC, Mosteller F (1994) Guidelines for meta-analyses evaluating diagnostic tests. Ann Intern Med 120:667–676
De Meirleir LJ, Taylor MJ (1987) Prognostic utility of SEPs in comatose children. Pediatr Neurol 3:78–82
Lindsay KW, Carlin J, Kennedy I, Fry J, McInnes A, Teasdale GM (1981) Evoked potentials in severe head injury—analysis and relation to outcome. J Neurol Neurosurg Psychiatry 44:796–802
Lindsay K, Pasaglou A, Hirst D, Allardyce G, Kennedy I, Teasdale G (1990) Somatosensory and auditory brain stem conduction after head injury: a comparison with clinical features in prediction of outcome. Neurosurgery 26:278–285
Greenberg RP, Becker DP, Miller JD, Mayer DJ (1977) Evaluation of brain function in severe head trauma with multimodality evoked potentials. II. Localization of brain dysfunction and correlation with post-traumatic neurological condition. J Neurosurg 47:163–177
Rappaport M, Hopkins HK, Hall K, Belleza T (1981) Evoked potentials and head injury. 2. Clinical applications. Clin Electroencephalogr 12:167–176
Cusumano S, Paolin A, Di Paolo F, Boccaletto F, Simini G, Palermo F, Carteri A (1992) Assessing brain function in post-traumatic coma by means of bit-mapped SEPs, BAEPs, CT, SPET and clinical scores. Prognostic implications. Electroencephalogr Clin Neurophysiol 84:499–514
De Weerd AW, Groenveld C (1985) The use of evoked potentials in the management of patients with severe cerebral trauma. Acta Neurol Scand 72:489–494
Madl C, Kramer L, Domanovitis H, Woolard RH, Gervais H, Gendo A, Eisenhuber E, Grimm G, Sterz F (2000) Improved outcome prediction in unconscious cardiac arrest survivors with sensory evoked potentials compared with clinical assessment. Crit Care Med 28:721–726
Sherman AL, Tirschwell DL, Micklesen PJ, Longstreth WT, Robinson LR (2000) Somatosensory potentials, CSF creatine kinase BB activity, and awakening after cardiac arrest. Neurology 54:889–894
Berek K, Lechleitner P, Luef G, Felber S, Saltuari L, Schinnerl A, Traweger C, Dienstl F, Aichner F (1995) Early determination of neurological outcome after prehospital cardiopulmonary resuscitation. Stroke 26:543–549
Pfurtscheller G, Schwarz G, Gravenstein N (1985) Clinical relevance of long-latency SEPs and VEPs during coma and emergence from coma. Electroencephalogr Clin Neurophysiol 62:88–98
Gutling E, Gonser A, Imhof H-G, Landis T (1994) Prognostic value of frontal and parietal somatosensory evoked potentials in severe head injury: a long-term follow-up study. Electroencephalogr Clin Neurophysiol 92:568–570
Gutling E, Gonser A, Regard M, Glinz W, Landis T (1993) Dissociation of frontal and parietal components of somatosensory evoked potentials in severe head injury. Electroencephalogr Clin Neurophysiol 88:369–376
Stelzl T, von Bose MJ, Hogl B, Fuchs H-H, Flugel KA (1995) A comparison of the prognostic value of neuron-specific enolase serum levels and somatosensory evoked potentials in 13 reanimated patients. Eur J Emerg Med 2:24–27
Schreiner A, Pohlmann-Eden B (1999) Cerebral hypoxia after cardiopulmonary resuscitation. Lancet 353:750–751
Narayan RK, Greenberg RP, Miller JD, Enas GG, Choi SC, Kishore PRS, Selhorst JB, Cutz HA, Becker DP (1981) Improved confidence of outcome prediction in severe head injury. A comparative analysis of the clinical examination, multimodality evoked potentials, CT scanning and intracranial pressure. J Neurosurg 54:751–762
Greenberg RP, Newlon PG, Becker DP (1982) The somatosensory evoked potential in patients with severe head injury: outcome prediction and monitoring of brain function. Ann NY Acad Sci 388:683–688
Sleigh JW, Havill JH, Frith R, Kersei D, Marsh N, Ulyatt D (1999) Somatosensory evoked potentials in severe traumatic brain injury: a blinded study. J Neurosurg 91:577–580
Kane NM, Curry SH, Rowlands CA, Manara AR, Lewis T, Moss T, Cummins BH, Butler SR (1996) Event-related potentials-neurophysiological tools for predicting emergence and early outcome from traumatic coma. Intensive Care Med 22:39–46
Shewmon DA, DeGiorgio CM (1989) Early prognosis in anoxic coma. Reliability and rationale. Neurol Clin 7:823–843
Adams E, Kane N, Boyd S, Kerr S (1996) Somatosensory evoked potentials: predictors of outcome in children with severe brain injury. J Pediatr 128:438–439
Attia J, Cook DJ (1998) Prognosis in anoxia and traumatic coma. Crit Care Clin 14:497–511
Bohn D (1993) Tools for predicting outcome in the neurologically injured child. Crit Care Med 21 [Suppl]:S332–S333
Diringer MN (1992) Early prediction of outcome from coma. Curr Opin Neurol Neurosurg 5:826–830
Facco E, Zuccarello M, Pittoni G, Zanardi L, Chiarnadra M, Davia G, Giron GP (1986) Early outcome prediction in severe head injury: comparison between children and adults. Childs Nerv Syst 2:67–71
Acknowledgements
We thank Professor John Carlin and Professor Frank Shann for their advice and Cathy Gatt and Poh Chua for their assistance with the Embase database search and for obtaining studies. We are also indebted to the group of persons who helped translate the non-English-language papers required for the review: Dr. Andreas Schibler, Associate Professor Jim Tibballs, Jo Murphy, Dr. Alvaro Brilla, Dr. Doris Doberenz, Dr. Petra Schäffler, and Dr. Georg Staubli.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Carter, B.G., Butt, W. Are somatosensory evoked potentials the best predictor of outcome after severe brain injury? A systematic review. Intensive Care Med 31, 765–775 (2005). https://doi.org/10.1007/s00134-005-2633-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-005-2633-1