Abstract
Objective
To assess acute cardiorespiratory effects of recruitment manoeuvres in experimental acute lung injury.
Design
Experimental study in animal models of acute lung injury.
Setting
Experimental laboratory at a University Medical Centre.
Animals
Ten pigs with bronchoalveolar lavage and eight pigs with endotoxin-induced ALI.
Interventions
Two kinds of recruitment manoeuvres during 1 min; a) vital capacity manoeuvres (ViCM) consisting in a sustained inflation at 30 cmH2O and 40 cmH2O; b) manoeuvres obtained during ongoing pressure-controlled ventilation (PCRM) with peak airway pressure 30 cmH2O, positive end-expiratory pressure (PEEP) 15 and peak airway pressure 40, PEEP 20. Recruitment manoeuvres were repeated after volume expansion (dextran 8 ml/kg). Oxygenation, mean arterial, and pulmonary artery pressures, aortic, mesenteric, and renal blood flow were monitored.
Measurements and results
Lower pressure recruitment manoeuvres (ViCM30 and PCRM30/15) did not significantly improve oxygenation. With ViCM and PCRM at peak airway pressure 40 cmH2O, PaO2 increased to similar levels in both lavage and endotoxin groups. Aortic blood flow was reduced from baseline during PCRM40/20 and ViCM40 by 57±3% and 61±6% in the lavage group and by 57±8% and 82±7% (P<0.05 vs PCRM40/20) in endotoxin group. The decrease in blood pressure was less pronounced. Prior volume expansion attenuated circulatory impairment. After cessation of recruitment hemodynamic parameters were restored within 3 min.
Conclusion
Effective recruitment resulted in systemic hypotension, pulmonary hypertension, and decrease in aortic blood flow especially in endotoxinemic animals. Circulatory depression may be attenuated using recruitment manoeuvres during ongoing pressure-controlled ventilation and by prior volume expansion.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acute lung injury (ALI) and the acute respiratory distress syndrome (ARDS) are accompanied by atelectasis formation, increasing venous admixture, and arterial hypoxemia [1, 2]. Different recruitment manoeuvres (RMs), as proposed by the “open lung concept”, have been used to expand lung volume and to improve gas exchange [3]. Application of a vital capacity manoeuvre, where the lungs are inflated to 40 cmH2O during 15 s in healthy anesthetised subjects [4] and for 40 s in ARDS patients [5] has been used. RMs have also been performed in pressure-controlled ventilation using PEEP levels of 15–25 cmH2O and increasing peak airway pressures (PAP) up to 45–60 cmH2O [6]. The optimal way of performing RMs is, however, still debated.
It is known that increased airway pressure and PEEP may have pronounced extrapulmonary effects [7]. The application of PEEP decreases cardiac output by reducing right ventricular preload and by increasing right ventricular afterload [8, 9]. The splanchnic organs are sensitive to the effects of increased PEEP due to decreased cardiac output, increased venous outflow pressure, pooling of blood, and organ compression [8, 10, 11, 12]. PEEP is known to influence renal function [13] by reduced renal blood flow, elevated renal venous pressure [14, 15], and hormonal responses [16, 17, 18]. In this study the acute effects of different RMs on arterial oxygenation, aortic, mesenteric and renal blood flow, and oxygen delivery were assessed in two experimental ALI models. In one group ALI was achieved by repeated bronchoalveolar lavage (BAL) with isotonic saline causing a lung injury with surfactant depletion [19, 20]. In the other group ALI was induced by infusion of endotoxin (ET) [21]. Two RMs were studied; a vital capacity manoeuvre (ViCM) with a sustained inflation and an RM during ongoing pressure-controlled ventilation (PCRM). Effects of RMs were studied in normovolemic animals and repeated after volume expansion.
Material and methods
The study was approved by the Committee for Ethical Review of Animal Experiments at Göteborg University and performed in accordance with NIH guidelines. Ten pigs (24–26 kg) were included in the BAL group and eight animals (28–33 kg) in the ET group.
Anaesthesia
Induction was performed using ketamine (Ketalar, Park-Davis, Sweden) 30 mg/kg and azaperon (Stresnil, Janssen-Cilag, Pharma, Austria) 80 mg intramuscularly. Anaesthesia was maintained by infusion of pentobarbitalnatrium (Apoteksbolaget, Sweden) 6 mg·kg·h and fentanyl (Fentanyl Pharmalink, Pharmalink, Sweden) 0.2 mg/h. Muscle relaxation was achieved by a bolus of pancuronium (Pavulon, Organon, Sweden) 0.1 mg/kg, followed by infusion 0.3 mg·kg·h. The pigs were tracheotomised and mechanically ventilated through an 8-mm endotracheal tube using a Servo 300 or 900C ventilator (Siemens-Elema, Sweden), volume-controlled ventilation (VC), tidal volume (TV) 8 ml/kg, respiratory rate (RR) 20/min, positive end-expiratory pressure (PEEP) 5 cmH2O, inspiration-to-expiration ratio (I:E) 1:2 and FiO2 0.5. Normovolemia was maintained by infusion of Ringer’s solution with 2.5% glucose, 10 ml·kg·h, increased to 20 ml·kg·h after laparotomy. Anticoagulation was achieved by 2500 IE heparin (Heparin Leo, Leo Pharma, Sweden) intravenously, repeated after 4 h.
Preparation
Arterial and central venous lines were surgically placed and a pulmonary artery catheter (CCOmbo/SVO2, Edwards Life Sciences, California, USA) inserted via the right internal jugular vein. Heart rate (HR), central venous pressure (CVP), mean arterial pressure (MAP), mean pulmonary artery pressure (MPAP), and mixed venous oxygen saturation (SvO2) were monitored. Oxygen saturation (SpO2) was recorded from the tail of the pig. A femoral artery and vein were cannulated and connected using silicon tubings. An on-line PaO2 monitor (Polytrode pO2 sensor, Polystan, Denmark, response time 20 s) was inserted in the circuit. Descending aortic blood flow (ABF) was determined using a transoesophageal echo-Doppler (Dynemo 3000, Sometec, France) positioned in the oesophagus. Ultrasonic flowmeter probes (Transsonic Systems, N.Y., USA) were placed around the portal vein and a renal artery to monitor mesenteric blood flow (QPV) and renal artery blood flow (QRA). The animals were placed in supine position. Respiratory rate, volumes, and pressures were measured using side stream spirometry. Inspiratory and expiratory fractions of oxygen and carbon dioxide (FiO2, FETO2, FiCO2, FETCO2) were measured with paramagnetic and infrared technology respectively (AS/3, Datex-Ohmeda, Finland).
Experimental procedure for BAL animals
After preparation the ventilator was set at VC 8 ml/kg, RR 20/min, I:E 1:2, PEEP 10 cmH2O, FiO2 1.0 and repeated BAL with saline (total amount 9–15 l) was performed to establish ALI [19, 20]. The procedure was finished when there were no visual signs of surfactant in the fluid exchange and PaO2 was less than 10 kPa at FiO2 1.0. The animals were allowed to stabilise for 1 h with PEEP set at 5–10 cmH2O to avoid severe hypoxemia. The experimental protocol started with an RM to expand the lungs initially followed by derecruitment with reduction of PEEP to 0 cmH2O and then resuming the initial ventilatory settings in each animal, PEEP kept at 5–10 cmH2O. Four RM, each preceded by derecruitment, were used in random order. Two ViCMs were performed with sustained inflation at 30 cmH2O and 40 cmH2O (ViCM30 and ViCM40) for 1 min using CPAP mode and two PCRMs performed in pressure-controlled mode, RR 40, I:E 1:1 and PAP 30 cmH2O and PEEP 15 (PCRM30/15) or PAP 40 and PEEP 20 (PCRM40/20) for 1 min.
MAP, MPAP, QPV, QRA, SvO2, SpO2, PaO2, and ABF were recorded every 15 s during the RMs. The animals were volume loaded using dextran 70 (Macrodex®, Pharmalink AB, Sweden), 8 ml/kg over 30 min followed by RMs repeated in the same order as before. Following cessation of RMs, hemodynamics were followed for 3 min. After the experiment the animal was killed during deepened anaesthesia.
Experimental procedure for endotoxin animals
Anaesthesia and preparation was carried out as described above. E. coli lipopolysaccharide endotoxin, serotype 0111:B4, (Sigma, St. Louis, USA) was dissolved in saline and heated to 37 °C. The infusion was started at a rate of 2.5 g·kg·h and increased stepwise during 30 min to a rate of 20 g·kg·h kept for 2.5 h. During the last 30 min the animals were volume resuscitated using hetastarch solution (Heas-steril, Meda, Sweden) to baseline cardiac output. The study protocol then followed the BAL-animal protocol but using only the high airway pressure (PAP 40 cmH2O) RMs i.e., ViCM40 and PCRM40/20 in random order, each for 1 min before and after volume expansion with dextran solution 8 ml/kg.
Calculations and statistics
Respiratory, hemodynamic and shunt calculations were made using standard formulae. Global oxygen delivery (DO2global) was calculated from values for descending aortic blood flow and mesenteric (DO2mes) and renal (DO2ren) oxygen delivery from portal venous and renal artery blood flows respectively.
Values are presented as mean±SEM unless stated otherwise. Analysis of variance (ANOVA) for repeated measures were performed followed by Fisher’s PLSD and if significant, paired t-test was used to evaluate changes from baseline to 1 min. Comparisons of pulmonary shunt at baseline and 1 min were made using paired t-test. The change in ABF and shunt during RMs was calculated using linear regression analysis. A P-value <0.05 was considered statistically significant.
Results
BAL animals, low and high pressure RMs
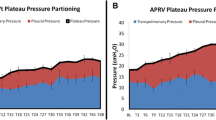
The hemodynamic and respiratory parameters for the BAL group during the low pressure RMs (PAP 30 cmH2O) at baseline and at 1 min of recruitment are presented in Table 1 and corresponding data for the high pressure RMs (PAP 40 cmH2O) in Table 2. Relative changes from baseline during high pressure RMs are shown in Fig. 1 and Fig. 2. Significantly greater improvement in oxygenation was achieved during recruitment with higher airway pressure levels (40 cmH2O vs 30 cmH2O, P<0.01) where PCRM40/20 was superior to ViCM40 (P<0.01). Recruitment with the higher pressure levels also caused significantly more negative circulatory effects with more pronounced decreases in MAP (P<0.01 both ViCM and PCRM) and ABF (P<0.01 and P<0.05 for ViCM and PCRM, respectively) than the lower airway pressure level. MPAP increased significantly during recruitment, especially during ViCM (P<0.01 vs PCRM, both pressure levels).
Improvement in arterial oxygenation (PaO2) and reductions in aortic blood flow (ABF), mesenteric blood flow (QPV), and renal artery blood flow (QRA) presented as relative changes from baseline at 15 s, 30 s, 45 s, and 60 s of recruitment using either vital capacity manoeuvre (ViCM40) or pressure-controlled recruitment manoeuvre (PCRM40/20) in bronchoalveolar lavage (BAL) and endotoxin-induced ALI. Bars grouped together indicate the same recruitment manoeuvre before and after volume expansion (VE).
The effect on global (DO2global), mesenteric (DO2mes), and renal (DO2ren) oxygen delivery as relative changes from baseline at 15 s, 30 s, 45 s, and 60 s of recruitment using either vital capacity manoeuvre (ViCM40) or pressure-controlled recruitment manoeuvre (PCRM40/20) in bronchoalveolar lavage (BAL) and endotoxin-induced ALI. Bars grouped together indicate the same recruitment manoeuvre before and after volume expansion (VE).
Volume expansion (dextran solution, 8 ml/kg) resulted in an increase in CVP from 5±1 mm Hg to 9±1 mm Hg (P<0.05), but had only minor effect on ABF at baseline (see Table 1 and Table 2). Volume expansion attenuated the decrease in ABF induced by the two RMs (P<0.01 both ViCM and PCRM, low- and high-pressure RMs). Despite a marked effect on arterial oxygenation, there was a significant decrease in the combined effect of recruitment on circulation and blood oxygenation, i.e., global DO2 during the recruitment procedures due to the negative effect on ABF. The decrease in global DO2 was greater during the ViCM compared to the PCRM (P<0.05, both pressure levels). Volume expansion prior to recruitment attenuated the decrease in global DO2, but the decrease was not statistically significant during PCRM40/20 or during lower pressure RMs.
The reduction in QPV and mesenteric DO2 paralleled the reduction in ABF and global DO2 during RM but were not significantly improved by volume expansion.
Renal blood flow and renal DO2 were not significantly changed during recruitment in normovolemic animals. Following volume expansion there was an increase in renal DO2 during a PCRM40/20 (P<0.05).
After cessation of RMs hemodynamic parameters gradually returned towards baseline, ABF being 86% (mean, range 27–124%) of baseline at 1 min and 96% (range 62–139%) of baseline at 3 min.
Endotoxin animals, high-pressure RMs
Data from six of the eight animals subjected to endotoxin infusion is presented in Table 1 and Fig. 1 and Fig. 2. Two pigs did not complete the protocol as they died in circulatory failure following endotoxin infusion. Endotoxin infusion lowered MAP and ABF with PaO2 at baseline being around 20 kPa at FiO2 1.0, corresponding to a shunt around 30%. During recruitment PaO2 increased to levels similar to that observed during recruitment in the BAL-group (see Table 2). RMs induced severe circulatory depression with marked decrease in ABF, QPV, and QRA as well as in global, mesenteric, and renal oxygen delivery. The reduction in QPV and DO2mes were significantly more pronounced during a ViCM compared to a PCRM (P<0.05 both).
Endotoxin animals responded to volume expansion (dextran solution, 8 ml/kg) with increase in CVP from 7±1 mmHg to 10±1 mmHg (P<0.05). Volume expansion also attenuated circulatory effects of RMs in the ET-group.
The relative changes in global and regional hemodynamics for the BAL- and ET-groups are shown in Fig. 1 and Fig. 2. Generally, greater decreases in ABF, QPV and QRA and in corresponding oxygen delivery were observed during RMs in the ET-group compared to the BAL-group and particularly during ViCMs.
After cessation of RMs in the ET-group ABF had returned to 81% (mean, range 40–119%) of baseline at 1 min and 103% (range 89–129%) at 3 min. Within 1–3 min after RMs, MAP, MPAP, QPV, and QRA all had returned to baseline levels.
Discussion
The main findings of this study were that: (1) RMs with high inspiratory pressure levels (40 cmH2O vs 30 cmH2O) were needed to achieve rapid and pronounced improvement in oxygenation in BAL-induced ALI in animals; (2) high-pressure RMs were associated with more negative hemodynamic effects which were generally more severe if performed as vital capacity manoeuvres compared to RMs performed by ongoing pressure-controlled ventilation; (3) despite improved oxygenation during RMs, a significant reduction in global oxygen delivery was observed; (4) in the BAL-induced ALI, RMs was associated with generally more pronounced reduction in mesenteric versus renal blood flow and oxygen delivery; (5) RMs performed in an endotoxin model of ALI was associated with greater negative circulatory effects than those performed in a BAL-model of ALI; and (6) prior volume expansion could partially attenuate circulatory depression induced by RMs.
Animal models of ALI
Recent clinical studies have pointed out subgroups of patients with ALI/ARDS based on the aetiology and duration of lung injury [22, 23, 24, 25]. It is logical that different experimental models of ALI should be used to mimic the heterogeneity of ALI/ARDS. In the present study we used a BAL-model in which repeated bronchoalveolar lavage was performed to achieve a reproducible and pronounced decrease in oxygenation and a model with endotoxin-induced lung injury where deterioration in gas exchange was more variable between animals and less pronounced than in the BAL-model.
In both models, however, RMs induced pronounced improvement in oxygenation to similar levels (although from different baselines). It has been suggested that the improvement in oxygenation in this situation could be due to several factors. In a study in ARDS-patients, Dantzker et al. observed that PEEP and high tidal volume ventilation resulted in parallel decrease in shunt and cardiac output together with an improvement in arterial oxygenation [26]. In the present study, RMs resulted in substantial decrease in aortic blood flow as well as shunt reduction and improvement in oxygenation. In contrast to the study by Dantzker et al we found no correlation (r=0.1) between the degree of reduction in ABF and the reduction in pulmonary shunt fraction. Furthermore, when the decrease in ABF during RMs was attenuated by prior volume expansion reduction in pulmonary shunt still occurred to a similar extent. This indicates that the decrease in ABF is not a prerequisite for the shunt reduction and improvement in oxygenation observed in this study during RMs.
In this as well as in previous studies [19, 20] we did observe that the BAL-model exhibited a prominent alveolar collapse and is responsive to different RMs if sufficient pressure is applied. This model is more responsive to RMs than other experimental models of ALI [22, 23] and could correspond to surfactant depletion in the early stage of ALI. In contrast, endotoxin infusion damaged pulmonary endothelial cells leading to increased permeability and interstitial oedema [21, 23]. Extrapulmonary effects of endotoxin infusion are more pronounced than in BAL-animals. Thus, hemodynamics were generally more unstable in the ET-group which also was reflected by two pigs dying from circulatory failure before the recruitment protocol was implemented.
Circulatory effects of RMs
The safety and efficacy of RMs are still not clear. In previous studies most investigators have used ViCMs using airway pressures of 30–60 cmH2O for 15–40 s [5, 22, 27, 28]. Fujino et al. [29] studied effects of RMs in a sheep model with lavage-induced ARDS where hemodynamic measurements were performed at the end of the RMs using bolus thermodilution. Only modest changes in cardiac output were observed. In the present animal study, and in a study performed in ARDS patients [5], more pronounced effects of RMs was observed using continuous Doppler monitoring of aortic blood flow. It is possible that in order to detect shortlasting but important effects during RMs on-line monitoring of central hemodynamics may be valuable [5, 22, 28, 29, 30].
In the present study, using a BAL-model of ALI/ARDS ViCM with pressure levels of 30 cmH2O was not sufficient to achieve more than a moderate (n.s.) increase in oxygenation during a 60-s manoeuvre. A more effective RM using a ViCM with a pressure level of 40 cmH2O was associated with pronounced circulatory side effects with a decrease in ABF of 61±6%. Generally, we observed using continuous monitoring that the relative reduction in ABF was much more pronounced than the decrease in MAP (34±5% during ViCM40 in BAL animals). Monitoring of changes in arterial pressure thus underestimates true effects of RMs which can be detected by continuous blood flow monitoring.
Circulatory effects using RMs during ongoing pressure control ventilation are less documented. In this study we observed less pronounced circulatory effects of this RM as compared to the ViCM especially in the ET-group although PCRMs produced a comparable improvement in oxygenation. This is probably a consequence of intermittent lowering of peak airway pressures from 40 cmH2O with each breath, resulting in a lower mean intrathoracic pressure and improved venous return compared to a sustained ViCM at 40 cmH2O. Performing RMs during ongoing ventilation may also be preferable to a ViCM to avoid further hypercapnia and decrease in pH which might increase pulmonary artery pressures and right ventricular afterload [31, 32].
A number of factors may determine the degree of hemodynamic effects of RMs. In this study we observed that RMs in endotoxin-induced ALI was associated with more marked circulatory effects than in BAL-induced ALI. This may mimic the clinical situation in patients with sepsis-induced ALI and unstable circulation which may then be especially vulnerable to recruitment with ViCM. Another factor is volume status. We observed that volume expansion by dextran solution only had minor effects on aortic blood flow at baseline in the BAL-group. Still, it did attenuate the hemodynamic effect induced by RMs indicating that volume expansion could be used to counteract circulatory side effects of RMs although maintenance of fluid balance in ALI/ARDS may limit this option. We also noted that volume expansion resulted in significant better improvement in oxygenation during ViCM40 in the BAL-group. This could be due to the high oxygen extraction during this manoeuvre as a consequence of pronounced circulatory depression. In endotoxin-induced ALI volume expansion was even more beneficial, improving ABF at baseline prior to recruitment as well as attenuating parts of the dramatic effects of RMs. Again, this emphasises the importance of individually evaluating volume status prior to RMs.
Following cessation of the RMs, ABF and MAP returned to baseline levels during the first 3 min in agreement with previous observations [5]. It may be argued that these shortlasting hemodynamic alterations can be acceptable in terms of patient safety. One problem is, however, that the degree of hemodynamic impairment with a combination of pulmonary hypertension, systemic hypotension, and decrease in aortic blood flow/cardiac output may be variable in animals/humans and possibly life-threatening in a hypovolemic patient with sepsis as suggested by the profound hemodynamic alterations observed in the endotoxin group in our study.
During the last decade the open lung concept and the use of RMs has been advocated with the use of airway pressure up to 60 cmH2O to fully open up the lungs [3, 6]. This, and other studies, indicates that these recommendations may need to be modified and that before RM are advocated as routine procedures their safety and efficacy should be evaluated in controlled clinical trials.
References
Ashbaugh DG, Bigelow DB, Petty TL, Levine BE (1967) Acute respiratory distress in adults. Lancet 2:319–323
Russell J, Walley K (1999) Overwiew, clinical evaluation and chest radiology of ARDS. Cambridge University, New York, p 6–27
Lachmann B (1992) Open up the lung and keep the lung open. Intensive Care Med 18:319–321
Rothen HU, Sporre B, Engberg G, Wegenius G, Hedenstierna G (1993) Re-expansion of atelectasis during general anaesthesia: a computed tomography study. Br J Anaesth 71:788–795
Grasso S, Mascia L, Del Turco M, Malacarne P, Giunta F, Brochard L, Slutsky AS, Marco Ranieri V (2002) Effects of recruiting maneuvers in patients with acute respiratory distress syndrome ventilated with protective ventilatory strategy. Anesthesiology 96:795–802
Böhm S, Vazques de Anda G, Lachmann B (1998) The open lung concept. In: Vincent J (ed), Yearbook of intensive care and emergency medicine. Springer, Berlin Heidelberg New York, pp 430–440
Pinsky MR (1997) The hemodynamic consequences of mechanical ventilation: an evolving story. Intensive Care Med 23:493–503
De Backer D (2000) The effects of positive end-expiratory pressure on the splanchnic circulation. Intensive Care Med 26:361–363
Vieillard-Baron A, Loubieres Y, Schmitt JM, Page B, Dubourg O, Jardin F (1999) Cyclic changes in right ventricular output impedance during mechanical ventilation. J Appl Physiol 87:1644–1650
Brienza N, Revelly JP, Ayuse T, Robotham JL (1995) Effects of PEEP on liver arterial and venous blood flows. Am J Respir Crit Care Med 152:504–510
Aneman A, Eisenhofer G, Fandriks L, Olbe L, Dalenback J, Nitescu P, Friberg P (1999) Splanchnic circulation and regional sympathetic outflow during peroperative PEEP ventilation in humans. Br J Anaesth 82:838–842
Winso O, Biber B, Gustavsson B, Holm C, Milsom I, Niemand D (1986) Portal blood flow in man during graded positive end-expiratory pressure ventilation. Intensive Care Med 12:80–85
Priebe HJ, Heimann JC, Hedley-Whyte J (1981) Mechanisms of renal dysfunction during positive end-expiratory pressure ventilation. J Appl Physiol 50:643–649
Shinozaki M, Muteki T, Kaku N, Tsuda H (1988) Hemodynamic relationship between renal venous pressure and blood flow regulation during positive end-expiratory pressure. Crit Care Med 16:144–147
Mullins RJ, Dawe EJ, Lucas CE, Ledgerwood AM, Banks SM (1984) Mechanisms of impaired renal function with PEEP. J Surg Res 37:189–196
Farge D, De la Coussaye JE, Beloucif S, Fratacci MD, Payen DM (1995) Interactions between hemodynamic and hormonal modifications during PEEP- induced antidiuresis and antinatriuresis. Chest 107:1095–1100
Venus B, Mathru M, Smith RA, Pham CG, Shirakawa Y, Sugiura A (1985) Renal function during application of positive end-expiratory pressure in swine: effects of hydration. Anesthesiology 62:765–769
Aneman A, Ponten J, Fandriks L, Eisenhofer G, Friberg P, Biber B (1997) Hemodynamic, sympathetic and angiotensin II responses to PEEP ventilation before and during administration of isoflurane. Acta Anaesthesiol Scand 41:41–48
Lachmann B, Robertson B, Vogel J (1980) In vivo lung lavage as an experimental model of the respiratory distress syndrome. Acta Anaesthesiol Scand 24:231–236
Nielsen JB, Sjostrand UH, Edgren EL, Lichtwarck-Aschoff M, Svensson BA (1991) An experimental study of different ventilatory modes in piglets in severe respiratory distress induced by surfactant depletion. Intensive Care Med 17:225–233
Borg T, Alvfors A, Gerdin B, Modig J (1985) A porcine model of early adult respiratory distress syndrome induced by endotoxaemia. Acta Anaesthesiol Scand 29:814–830
Kloot TE, Blanch L, Melynne Youngblood A, Weinert C, Adams AB, Marini JJ, Shapiro RS, Nahum A (2000) Recruitment maneuvers in three experimental models of acute lung injury. Effect on lung volume and gas exchange. Am J Respir Crit Care Med 161:1485–1494
Neumann P, Berglund JE, Mondejar EF, Magnusson A, Hedenstierna G (1998) Dynamics of lung collapse and recruitment during prolonged breathing in porcine lung injury. J Appl Physiol 85:1533–1543
Gattinoni L, Pelosi P, Suter PM, Pedoto A, Vercesi P, Lissoni A (1998) Acute respiratory distress syndrome caused by pulmonary and extrapulmonary disease. Different syndromes? Am J Respir Crit Care Med 158:3–11
Ranieri VM, Brienza N, Santostasi S, Puntillo F, Mascia L, Vitale N, Giuliani R, Memeo V, Bruno F, Fiore T, Brienza A, Slutsky AS (1997) Impairment of lung and chest wall mechanics in patients with acute respiratory distress syndrome: role of abdominal distension. Am J Respir Crit Care Med 156:1082–1091
Dantzker DR, Lynch JP, Weg JG (1980) Depression of cardiac output is a mechanism of shunt reduction in the therapy of acute respiratory failure. Chest 77:636–642
Rothen HU, Sporre B, Engberg G, Wegenius G, Hedenstierna G (1995) Reexpansion of atelectasis during general anaesthesia may have a prolonged effect. Acta Anaesthesiol Scand 39:118–125
Lapinsky SE, Aubin M, Mehta S, Boiteau P, Slutsky AS (1999) Safety and efficacy of a sustained inflation for alveolar recruitment in adults with respiratory failure. Intensive Care Med 25:1297–1301
Fujino Y, Goddon S, Dolhnikoff M, Hess D, Amato MB, Kacmarek RM (2001) Repetitive high-pressure recruitment maneuvers required to maximally recruit lung in a sheep model of acute respiratory distress syndrome. Crit Care Med 29:1579–1586
Villagra A, Ochagavia A, Vatua S, Murias G, Del Mar Fernandez M, Lopez Aguilar J, Fernandez R, Blanch L (2002) Recruitment maneuvers during lung protective ventilation in acute respiratory distress syndrome. Am J Respir Crit Care Med 165:165–170
Carvalho CR, Barbas CS, Medeiros DM, Magaldi RB, Lorenzi Filho G, Kairalla RA, Deheinzelin D, Munhoz C, Kaufmann M, Ferreira M, Takagaki TY, Amato MB (1997) Temporal hemodynamic effects of permissive hypercapnia associated with ideal PEEP in ARDS. Am J Respir Crit Care Med 156:1458–1466
Thorens JB, Jolliet P, Ritz M, Chevrolet JC (1996) Effects of rapid permissive hypercapnia on hemodynamics, gas exchange, and oxygen transport and consumption during mechanical ventilation for the acute respiratory distress syndrome. Intensive Care Med 22:182–191
Acknowledgements
Valuable assistance was provided by laboratory assistant Marita Ahlqvist. The study was supported by grants from the Medical Faculty of Göteborg University, the Swedish Research Council (K2003–04X-14032-03A), and the Göteborg Medical Society.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Odenstedt, H., Åneman, A., Kárason, S. et al. Acute hemodynamic changes during lung recruitment in lavage and endotoxin-induced ALI. Intensive Care Med 31, 112–120 (2005). https://doi.org/10.1007/s00134-004-2496-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-004-2496-x