Abstract
Objective
To describe the use of volumetric capnography, a plot of expired CO2 concentration against expired volume, in monitoring fibrinolytic treatment of major pulmonary embolism.
Design and setting
Two case reports in the emergency department of a teaching hospital.
Patients
Two conscious and spontaneously breathing patients (69- and 31-year-old women) with major pulmonary embolism requiring thrombolysis. Decision for thrombolysis was based on the association of right ventricular afterload on echocardiography, with respiratory failure and hypotension in the first patient, and dyspnea and hemodynamically stable parameters in the second one.
Interventions
Successive capnographic measurements were performed before, during, and after thrombolysis. Curves of volumetric capnography were obtained from a sidestream gas monitor with flow sensor and an arterial blood gas analysis for CO2 partial pressure.
Measurements and results
We calculated late deadspace fraction, previously suggested as the most effective capnographic parameter in the diagnosis of pulmonary embolism. Late deadspace fraction decreased in the two patients, respectively, from 64.4% to 1.1% and from 25.6% to 5.7% after thrombolysis, with a concomitant disappearance of right heart dysfunction signs on echocardiography.
Conclusions
Volumetric capnography can monitor thrombolysis in major pulmonary embolism. Differences between volumetric capnography technology and the more traditional arterial to end-tidal CO2 gradient are important to take into account for clinical application.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Major pulmonary embolism (MPE), defined as pulmonary embolism (PE) with arterial hypotension, cardiogenic shock, or right ventricular afterload [1], is characterized primarily by increased alveolar deadspace from unperfused but well ventilated lung regions. The mortality rate of MPE ranges from 10% to 25%, justifying the potential recourse to thrombolysis for rapid clot dissolution [2]. Monitoring the thrombolytic efficacy is essential but may require serial echocardiograms or pulmonary catheterizations, the later being invasive, and inconvenient for conscious and spontaneously breathing patients.
Volumetric capnography (VCap), the plot of expired CO2 concentration against expired volume, is a bedside validated method for measuring airway and alveolar deadspace volumes, and appreciating the pulmonary ventilation-perfusion relationships [3, 4]. Because the performance of VCap in the diagnostic work-up for pulmonary embolism has been previously established [5, 6, 7], we hypothesized that it also applies in monitoring the clinical course during fibrinolytic treatment of MPE. The results of two first studied cases are presented here.
Material and methods
Volumetric capnography
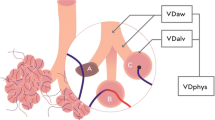
VCap analysis is illustrated in Fig. 1. VCap displays the expired CO2 as a function of the expired volume during one single breath, according to the work of Fletcher et al. [3] in 1981. The shape of the capnographic curve starts with a CO2-free phase continues with an ascending transition phase and ends with a plateau phase which slope depends on the ventilation-perfusion mismatches. The slope is determined by least squares linear regression analysis for the end-expiratory plateau phase using at least the last 15% of the expired tidal volume. The end of the curve corresponds to the end-tidal CO2 (EtCO2). A vertical line surrounding the curvature of the second phase determines the airway deadspace (VDaw). The arterial PaCO2 value delimitates an upper horizontal line, the surface between this line and the plateau phase corresponding to the alveolar deadspace volume (VDalv). The gradient between PaCO2 and EtCO2 traditionally represents the fraction of VDalv on the tidal volume. Eriksson et al. [7] found that the extrapolation of the capnographic curve should cross the PaCO2 horizontal line at a CO2 value corresponding to 15% of the predicted total lung capacity (ExpCO215% TLC) in healthy subjects, and in patients with obstructive lung diseases. He defined late deadspace fraction (Fdlate) as: Fdlate=(PaCO2−ExpCO215% TLC)/PaCO2, where TLC is estimated taking sex and height of the patient into consideration [8].
Volumetric capnography and its different parameters, including alveolar deadspace (V D alv), airway deadspace (V D aw), and late deadspace fraction (Fd late ). Data are from patient 2 before starting thrombolysis. The arterial PaCO2 is 29 mmHg and the end-tidal CO2 is 21.9 mmHg; 15% of the predicted total lung capacity is 795 ml and the expired CO2 partial pressure corresponding to this 795 ml volume (E xp CO 2 15% TLC) is 22.1 mmHg; Fdlate is calculated as (29–22.1)/29=23.8%. Tidal volume (V T ) is 750 ml
A typical capnographic appearance of moderate to severe pulmonary embolism is characterized with a flat plateau phase and an elevated PaCO2−EtCO2 gradient, as shown in Fig. 1. In these conditions the extrapolation of the curve fails to reach the PaCO2 horizontal line. Since the VCap takes into consideration both the plateau phase curve pattern and the PaCO2−EtCO2 gradient, Fdlate has been found the most effective among the capnographic parameters for differentiating PE from other pulmonary illnesses [7]. Eriksson et al. [7] chose a cutoff value of 12% for Fdlate, patients with PE having higher values.
Time-based capnograms and respiratory flows were measured in this study by Datex-Ohmeda (GE Medical Systems, Information technology, Helsinki, Finland) CS/3 monitor, gas analyzer (M-COVX), and D-lite sensor (deadspace 9 cc) connected to the patient through a mouthpiece or a facial mask (deadspace 25 cc). Signals were synchronized at start of inspiration when CO2-free fresh gas enters gas-sampling point practically parallel with the flow turning. Arterial PaCO2 sample was collected slowly after 2 min stabilization period during capnographic registration. A breath of typical tidal volume, respiration rate, and EtCO2 collected during arterial sampling was selected for analysis.
Patients and measurements
The first patient was a 69-year-old woman with dyspnea for 1 day before admission. She fainted shortly after admission. At that time her blood pressure was 88/43 mmHg, pulse rate 145/min, and respiratory rate 50/min. Echocardiography showed a systolic pulmonary arterial pressure (sPAP) of 50 mmHg, a paradoxical septal wall motion, and a right-to-left ventricular size ratio of 1.67. A 10-mg bolus of alteplase was immediately started, followed by 90 mg over a 2-h period. A control echocardiogram 12 h later showed a sPAP of 19 mmHg and the disappearance of right heart dysfunction signs. Lung scintigraphy confirmed segmental defects in the upper right and middle lung lobes. Her VCap was recorded during thrombolysis and repeated 5 and 24 h later.
The second patient was a 31-year-old woman complaining of dyspnea for 3 days. On admission her blood pressure was 125/80 mmHg, pulse rate 120/min, and respiratory rate 26/min. Spiral computed tomography confirmed bilateral lobar and segmental pulmonary occlusions. Initial echocardiography showed a sPAP of 38 mmHg and the same right heart dysfunction signs as the previous patient. A 100-mg alteplase infusion was administered over a 2-h period. Echocardiography 12 h later was normal. VCap was measured seven times: twice before, twice during and three times after thrombolysis.
Neither of the two patients had bleeding complications.
Results
Patient 1
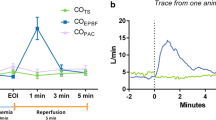
One hour after starting thrombolysis the patient’s PaCO2 was 37 mmHg and EtCO2 14.1 mmHg. The value for 15% of the predicted TLC was calculated as 765 ml, and ExpCO215% TLC was 13.3 mmHg. Fdlate corresponded to (37–13.3)/37 mmHg=64.4%. Fdlate was reduced to 21.9% 5 h after the end of thrombolysis and to 1.1%=(33–32.6)/33 mmHg the day thereafter. This Fdlate reduction parallels the decrease in the PaCO2−EtCO2 gradient related to VDalv fraction reduction: this gradient was 22.9 mmHg at the beginning of thrombolysis, 11.3 mmHg 5 h later, and 2.7 mmHg the day thereafter. Figure 2 shows the capnographic curves of patient 1 at the beginning and 24 h after thrombolysis.
Course of volumetric capnography measurement in patient 1, from beginning (curve A) to 24 h postthrombolysis (curve B). Arrow value for 15% of the predicted TLC (765 ml) used for Fdlate calculation. Note that the tidal volume of curve A (VT A ) is higher than 15% of the predicted TLC. The marked ranges (}) express Fdlate as the difference between PaCO2 and ExpCO215% TLC. Fdlate reduced from 64.4% at the beginning of thrombolysis to 1.1% on the day after, almost crossing the horizontal PaCO2 line at the 15% of predicted TLC vertical line
Patient 2
Considering a predicted TLC of 795 ml, Fdlate values were 25.6% and 23.8% 1 h before and at the beginning of thrombolysis, respectively, confirming stable baseline values. Fdlate was reduced to 1.4% after 50 min of thrombolytic treatment and to 1.8% at the end of the 2-h alteplase regimen. Fdlate stabilized to −1.3%, −3.6%, and 5.7%, respectively, 12, 36, and 60 h after thrombolysis. The PaCO2−EtCO2 gradient decreased as follows: 5.9 and 7.1 mmHg before thrombolysis, 2.4 and 2 mmHg during thrombolysis, 0.1, 1.2, and 2.4 mmHg after thrombolysis.
Discussion
This report shows that Fdlate measured by VCap can monitor the improvement in pulmonary vascular obstruction during thrombolysis for MPE. The normalization of echocardiographic signs of pulmonary dysfunction coupled with a significant decrease in the Fdlate ratio shows thrombolytic efficacy in two spontaneously breathing patients. The improvement in Fdlate during and after thrombolysis was markedly affected by the reduction in PaCO2−EtCO2 gradient.
One study and two case reports previously assessed the role of capnography in MPE requiring thrombolysis by using information from the PaCO2−EtCO2 gradient [9, 10, 11]. This gradient increases in the case of MPE, firstly because unperfused but well ventilated lung regions are unable to eliminate CO2, and secondly because right ventricular failure decreases the CO2 transport to the lungs [12, 13]. Wiegand et al. [11] showed a high intraindividual correlation (R2=0.77–0.98) between the changes in the PaCO2−EtCO2 gradient and the changes in pulmonary arterial pressure in 12 mechanically ventilated patients with MPE, demonstrating that capnography was a reliable noninvasive alternative to pulmonary catheterization in monitoring the efficacy of thrombolysis. The two other case reports shared the same encouraging results [9, 10], but only one patient in these three reports was breathing spontaneously, a clinical condition associated with less stable respiratory pattern and less extensive embolic burden.
VCap is based on solid physiological principles developed by Fletcher and associates [3, 14] in the early 1980s. The technique allows a breath-by-breath calculation of deadspace volumes and gives information on the ventilation-perfusion relationship thanks to the slope of the plateau phase. VCap is considered a gold standard for measuring deadspace [15], and several investigators have reported its role in the diagnostic work-up for a clinical suspicion of PE [5, 6, 16]. Fdlate is another VCap parameter that uses the extrapolation of the capnographic curve to differentiate patients with PE from those with obstructive lung diseases [7, 17]. Moreover, a recent study showed that the diagnostic performance of Fdlate was significantly better than the PaCO2−EtCO2 gradient in a group of 45 outpatients with a suspicion of PE, as assessed by a receiver operating characteristic curve analysis (87.6% vs. 75.9%, p=0.02) [16]. We therefore hypothesized that Fdlate is more appropriate in clinical conditions associated with potential false-positive PaCO2−EtCO2 gradients, such as in apprehensive and rapidly breathing patients or in cases of PE combined with chronic obstructive pulmonary disease [18, 19].
Physicians caring for patients with MPE currently use several methods to evaluate the effect of thrombolysis: (a) clinical signs of arterial hypotension, cardiogenic shock or right ventricular overload, (b) pulmonary catheterization, (c) serial echocardiography, and (d) lung scintigraphy or angiography. Fdlate provides advantages over these being a noninvasive, low-cost bedside measurement even for spontaneously breathing patients, which provides rapid information of the thrombolytic efficacy as shown in this study (Fig. 2). Fdlate may also complete or precede changes in the clinical vital signs assessment (e.g., blood pressure, heart rhythm, urinary output). Finally, VCap is a more easily repeatable technique than serial echocardiography.
VCap thus promises results in monitoring thrombolysis of spontaneously breathing patients with MPE. This validated noninvasive bedside technique can improve patient care by providing rapid information on the therapeutic efficacy and completing the clinical signs assessment.
References
Konstantinides S, Geibel A, Heusel G, Heinrich F, Kasper W (2002) Heparin plus alteplase compared with heparin alone in patients with submassive pulmonary embolism. N Engl J Med 347:1143–1150
Konstantinides S, Geibel A, Olschewski M, Heinrich F, Grosser K, Rauber K, Iversen S, Redecker M, Kienast J, Just H, Kasper W (1997) Association between thrombolytic treatment and the prognosis of hemodynamically stable patients with major pulmonary embolism: results of a multicenter registry. Circulation 96:882–888
Fletcher R, Jonson B, Cumming G, Brew J (1981) The concept of deadspace with special reference to the single breath test for carbon dioxide. Br J Anaesth 53:77–78
Lucangelo U, Blanch L (2004) Dead space. Intensive Care Med 30:576–579
Kline JA, Israel EG, Michelson EA, O’Neil BJ, Plewa MC, Portelli DC (2001) Diagnostic accuracy of a bedside D-dimer assay and alveolar dead-space measurement for rapid exclusion of pulmonary embolism: a multicenter study. JAMA 285:761–768
Rodger MA, Jones G, Rasuli P, Raymond F, Djunaedi H, Bredeson CN, Wells PS (2001) Steady-state end-tidal alveolar dead space fraction and D-dimer: bedside tests to exclude pulmonary embolism. Chest 120:115–119
Eriksson L, Wollmer P, Olsson CG, Albrechtsson U, Larusdottir H, Nilsson R, Sjogren A, Jonson B (1989) Diagnosis of pulmonary embolism based upon alveolar dead space analysis. Chest 96:357–362
Anonymous (1983) Standardized lung function testing. Report working party. Bull Eur Physiopathol Respir [Suppl 5]:1–95
Rodger MA, Jones G, Raymond F, Lalonde D, Proulx M, Huebsch L, Bredeson C (1998) Dead space ventilation parallels changes in scintigraphic vascular obstruction at recurrence of pulmonary embolism and after thrombolytic therapy: a case report. Can Respir J 5:215–218
Thys F, Elamly A, Marion E, Roeseler J, Janssens P, El Gariani A, Meert P, Verschuren F, Reynaert M (2001) PaCO2/ETCO2 gradient: early indicator of thrombolysis efficacy in a massive pulmonary embolism. Resuscitation 49:105–108
Wiegand UK, Kurowski V, Giannitsis E, Katus HA, Djonlagic H (2000) Effectiveness of end-tidal carbon dioxide tension for monitoring thrombolytic therapy in acute pulmonary embolism. Crit Care Med 28:3588–3892
Robin ED, Julian DG, Travis DM, Crump CH (1959) A physiological approach to the diagnosis of acute pulmonary embolism. N Engl J Med 260:586–591
Chopin C, Fesard P, Mangalaboyi J et al (1990) Use of capnography in diagnosis of pulmonary embolism during acute respiratory failure of chronic obstructive pulmonary disease. Crit Care Med 18:353–357
Fletcher R (1985) Deadspace, invasive and non-invasive. Br J Anaesth 57:245–249
Astrom E, Niklason L, Drefeldt B, Bajc M, Jonson B (2000) Partitioning of dead space-a method and reference values in the awake human. Eur Respir J 16:659–664
Verschuren F, Liistro G, Coffeng R, Thys F, Roeseler J, Zech F, Reynaert M (2004) Volumetric capnography as a screening test for pulmonary embolism in the emergency department. Chest 125:841–850
Olsson K, Jonson B, Olsson CG, Wollmer P (1998) Diagnosis of pulmonary embolism by measurement of alveolar dead space. J Intern Med 244:199–207
Nutter DO, Massumi RA (1966) The arterial-alveolar carbon dioxide tension gradient in diagnosis of pulmonary embolus. Dis Chest 50:380–387
Colp C, Stein M (2001) Re-emergence of an “orphan” test for pulmonary embolism. Chest 120:115–119
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Verschuren, F., Heinonen, E., Clause, D. et al. Volumetric capnography as a bedside monitoring of thrombolysis in major pulmonary embolism. Intensive Care Med 30, 2129–2132 (2004). https://doi.org/10.1007/s00134-004-2444-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-004-2444-9