Abstract
Objective
To determine whether ICU-acquired paresis (ICUAP) is an independent risk factor of prolonged weaning.
Design
Second study of a prospective cohort of 95 patients who were enrolled in an incidence and risk factor study of ICUAP.
Setting
Three medical and two surgical ICUs in four hospitals.
Patients and participants
Ninety-five patients without pre-existing neuromuscular disease recovering from the acute phase of critical illness after ≥7 days of mechanical ventilation.
Interventions
None.
Measurements and results
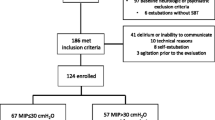
Duration of weaning from mechanical ventilation was defined as the duration of mechanical ventilation between awakening (day 1) and successful weaning. Muscle strength was evaluated at day 7 after awakening using the Medical Research Council (MRC) score. Patients with an MRC <48 were considered to have ICUAP. Among the 95 patients (mean age 62.0±15.3 years, SAPS 2 on admission 48.7±17.4) who regained satisfactory awakening after 7 or more days of mechanical ventilation, 67 (70.5%) were hospitalized in a medical ICU and 28 (29.5%) in a surgical ICU. Median duration (25th–75th percentiles) of weaning was longer in patients with ICUAP than in those without ICUAP: 6 days (1–22 days) vs 3 days (1–7 days); p=0.01; log-rank analysis. In multivariate analysis, the two independent predictors of prolonged weaning were ICUAP [hazard ratio (HR): 2.4; 95% confidence interval (CI): 1.4–4.2] and chronic obstructive pulmonary disease (HR: 2.7; 95% CI: 1.6–4.5)
Conclusions
ICU-acquired paresis is an independent predictor of prolonged weaning. Prevention of ICU-acquired neuromuscular abnormalities in patients recovering from severe acute illness should result in shorter weaning duration.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Paralysis acquired during the stay in the intensive care unit (ICU) has been progressively recognized as a major event which occurs during ICU management of patients with prolonged critical illness [1, 2]; however, the respective contribution of ICU-acquired neuromuscular involvement and other factors, such as preexisting pulmonary disease and severity of the acute illness on the duration of mechanical ventilation (MV), remains unclear.
The potential relationship between ICU-acquired neuromuscular involvement and duration of MV is complex. While mechanical ventilation may be prolonged by the occurrence of neuromuscular abnormalities, it is also conceivable that neuromuscular involvement may be facilitated by prolonged MV. Our first study in a cohort of 95 patients who recovered satisfactory consciousness after ≥7 days of MV showed that the duration of MV before awakening was an independent predictor of ICU-acquired paresis detected at awakening [3]. This finding suggested that, to determine whether ICU-acquired paresis is a cause of prolonged MV, it is necessary to investigate the period after awakening.
In this second study of our cohort of 95 patients, our aim was to determine whether ICU-acquired paresis (ICUAP) was an independent risk factor of prolonged weaning after awakening.
Materials and methods
Study population
We followed a prospective cohort of 95 patients without pre-existing neuromuscular disease recovering from the acute phase of critical illness after 7 or more days of mechanical ventilation in 5 ICUs. These patients were enrolled in an incidence and risk factor study of ICU-acquired paresis [3].
Patient management
All patients in the cohort had been on MV for ≥7 days and recovered satisfactory awakening (day 1). Muscle strength was evaluated at day 7 after awakening and patients were accordingly classified as ICUAP or controls. The decision to disconnect patients from the ventilator was made by the patient’s attending physician. Although no specific weaning procedure was used, weaning practices in all participating centres involved two steps. Firstly, all patients were screened daily after awakening for the absence of high-grade fever, use of catecholamines (except low doses of dopamine or dobutamine), high FiO2 level and PEEP >5 cm H2O. Secondly, as soon as patients had a positive screening test, they were switched to pressure support ventilation and underwent daily spontaneous breathing trials on a T-piece, regardless of the presence or absence of ICUAP. The decision to extubate was based on simple bedside tolerance parameters including respiratory rate, SpO2 and the use of accessory respiratory muscles during T-piece trials. Weaning was considered successful when reventilation was not required within the next 48 h.
Statistical analysis
We searched to determine whether ICUAP was an independent predictor of the duration of weaning from MV, defined as the duration of MV between awakening (day 1) and successful weaning. Firstly, we estimated the duration of weaning in patients with and without ICUAP using the Kaplan-Meier method [4], and compared the two groups using the log-rank test. Secondly, we analysed the association between the duration of weaning and a priori-selected covariates (Table 1) [5, 6] using log-rank test. Thirdly, variables (including ICUAP and the above covariates) with a p value <0.15 in log-rank analysis were entered in a multivariate Cox proportional-hazards model to identify the independent variables that influenced the duration of weaning from mechanical ventilation [7].
Categorical data are presented as number (%). Time-dependent quantitative data are presented as median (25th to 75th percentile). Other quantitative data are presented as mean±1SD. A p value of <0.05 was considered to indicate statistical significance.
Results
The study cohort was composed of 95 patients who regained satisfactory awakening after 7 or more days of mechanical ventilation [3]. The median (25th to 75th percentile) interval between onset of MV and awakening (day 1) was 9 days (7–17 days). The median duration of weaning from MV was 3 days (1–9 days). The median duration (25th to 75th percentile) of weaning in ICU centres 1, 2, 3, 4 and 5 was 4 (1–7), 3 (0–15), 2 (1–3), 4 (1–11) and 2 (0–25) days, respectively (p=0.77). The ICUAP was identified in 24 (25.3%) patients on day 7 after awakening.
The median (25th to 75th percentile) duration of weaning was significantly longer in patients with ICUAP compared with those without ICUAP [6 days (1–22 days), range 0–180 days vs 3 days (1–7 days), range 0–146 days; p=0.01]. Two patients had a duration of weaning >100 days due to prolonged severe tetraparesis and COPD in one ICUAP patient, and severe kyphoscoliosis in one control patient. Kaplan-Meier representation of duration of weaning in patients with and without ICUAP is shown in Fig. 1. Patients with COPD also had a significantly longer duration of weaning [9 days (1–22 days) vs 3 days (0–6 days); p=0.003], as did those with a SAPS II >26 on day 1 [5 days (1–15 days) vs 2 days (0–6 days); p=0.03; Table 1].
The ICUAP and COPD were both independent predictors of prolonged weaning in the Cox proportional analysis (Table 2). The probability of remaining on MV after awakening was 2.4 times greater for patients with ICUAP [95% confident interval (CI) 1.4–4.2] and 2.7 times greater for patients with COPD (95% CI 1.6–4.5). In patients with ICUAP but without COPD, the median duration of weaning was 3.5 days longer than in patients who did not have either ICUAP or COPD. In patients with COPD but without ICUAP, the median duration of weaning was 6 days longer than in patients who did not have either ICUAP or COPD.
Discussion
Our study showed that ICUAP was an independent factor of prolonged weaning from MV in patients who recovered satisfactory consciousness after 7 or more days of MV. Several conditions, including cardiac insufficiency, chronic pulmonary disease, persistent sepsis and neuromuscular disorders, may contribute to difficult weaning from the ventilator in critically ill patients [8]. Although respiratory neuromuscular involvement may occur in specific thoracic conditions, such as local mediastinal or cervical tumors and thoracic surgery [9], this is usually part of a general neuromuscular disorder which can be present on admission or acquired during the ICU stay. We showed that after adjusting for potential confounders such as the presence COPD, cardiopathy and severity of illness, the risk of prolonged weaning was more than doubled in patients with ICUAP.
Our finding is consistent with the only other study, to our knowledge, that also included ICU-acquired neuromuscular involvement in a multivariate analysis of MV duration [10]. It is also consistent with a recent large trial in surgical ICU patients who had been in ICU for 6 or more days and were treated with intensive insulin therapy [11]. Although this study did not analyse the specific contribution of the ICU-acquired neuromuscular abnormalities to reduced duration of mechanical ventilation, the positive outcomes included a lower incidence of electrophysiologically detected critical illness polyneuropathy and a shorter duration of MV.
Electrophysiological examination in selected patients with failure to wean has shown that peripheral and respiratory neuromuscular abnormalities are common [12]. Our finding in patients with prolonged severe illness also suggests that respiratory neuromuscular involvement coexists with limb involvement and might thus share the same risk factors; however, some pathways may be more specifically involved in respiratory muscle involvement, such as muscle inactivity resulting from controlled mechanical ventilation [13]. Furthermore, whether peripheral and respiratory muscles are involved to the same extent is another important question. Electrophysiological examination of limbs and the diaphragm revealed a significant positive correlation in a prospective study of 42 ICU patients with sepsis and multiple organ failure [14]; however, bedside measurement of respiratory muscle strength and endurance to detect a functional correlation with limb muscle strength is often volitional [15]. The use of phrenic nerve stimulation with twitch transdiaphragmatic pressure measurement may overcome this difficulty [16].
One limitation of our study might be that according to our a priori definition, ICUAP was diagnosed 7 days after awakening, and thus precluded the use of this parameter to predict the need for prolonged MV at the time of awakening. Nevertheless, our results suggest that the presence of ICUAP seven days after awakening can in fact explain the need for MV ventilation in patients recovering from severe acute illness. Another limitation might be that, despite the systematic performance of daily T-piece trials once prerequisite criteria for weaning were present, the weaning procedure was not more formally standardized; however, there was no difference in the duration of MV after day 1 between participating centres. Furthermore, the fact that MV had already been discontinued in more than half of the patients at the time ICUAP was confirmed suggests that the decision to extubate was not influenced by peripheral neuromuscular function.
Conclusion
In conclusion, our study showed that ICUAP was an independent contributor to MV duration after awakening from the acute phase of critical illness. We suggest that clinical research on weaning duration as an outcome should include ICUAP as a potential confounder. Our results also suggest that interventions to prevent ICUAP in patients recovering from severe acute illness might have a direct impact on weaning duration.
References
Bolton CF, Gilbert JJ, Fhahn A, Sibbald WJ (1984) Polyneuropathy in critically ill patients. J Neurol Neurosurg Psychiatr 47:1223–1231
De Jonghe B, Cook D, Sharshar T, Lefaucheur J, Carlet J, Outin H (1998) Acquired neuromuscular disorders in critically ill patients: a systematic review. Intensive Care Med 24:1242–1250
De Jonghe B, Sharshar T, Lefaucheur JP, Authier FJ, Durand-Zaleski I, Boussarsar M, Cerf C, Renaud E, Mesrati F, Carlet J, Raphael JC, Outin H, Bastuji-Garin S (2002) Paresis acquired in the intensive care unit: a prospective multicenter study. J Am Med Assoc 288:2859–2867
Kaplan EL, Meier P (1958) Nonparametric estimation from incomplete observations. J Am Stat Assoc 53:457–481
LeGall JR, Lemeshow S, Saulnier F (1993) A new simplified acute physiologic score (SAPS II) based on a European/North American multicenter study. J Am Med Assoc 270:2957–2963
Fagon JY, Chastre J, Novara A, Medioni P, Gibert C (1993) Characterization of intensive care unit patients using a model based on the presence or absence of organ dysfunctions and/or infection: the ODIN model. Intensive Care Med 19:137–144
Cox DR (1972) Regression models and life-tables. J R Stat Soc 34:187–220
Lemaire F (1993) Difficult weaning. Intensive Care Med 19: S69–S73
Sander HW, Saadeh PB, Chandswang N, Greenbaum D, Chokroverty S (1999) Diaphragmatic denervation in intensive care unit patients. Electromyogr Clin Neurophysiol 39:3–5
Garnacho-Montero J, Madrazo-Osuna J, Garcia-Garmendia JL, Ortiz-Leyba C, Jimenez-Jimenez FJ, Barrero-Almodovar A, Garnacho-Montero MC, Moyano-Del-Estad MR (2001) Critical illness polyneuropathy: risk factors and clinical consequences. A cohort study in septic patients. Intensive Care Med 27:1288–1296
Van den Berghe G, Wouters P, Weekers F, Verwaest C, Bruyninckx F, Schetz M, Vlasselaers D, Ferdinande P, Lauwers P, Bouillon R (2001) Intensive insulin therapy in the critically ill patients. N Engl J Med 345:1359–1367
Maher J, Rutledge F, Remtulla H, Parkes A, Bernardi L, Bolton CF (1995) Neuromuscular disorders associated with failure to wean from the ventilator. Intensive Care Med 21:737–743
Sassoon CS, Caiozzo VJ, Manka A, Sieck GC (2002) Altered diaphragm contractile properties with controlled mechanical ventilation. J Appl Physiol 92:2585–2595
Witt NJ, Zochodne DW, Bolton CF, Grand’Maison F, Wells G, Young GB, Sibbald WJ (1991) Peripheral nerve function in sepsis and multiple organ failure. Chest 99:176–184
Multz AS, Aldrich TK, Prezant DJ, Karpel JP, Hendler JM (1990) Maximal inspiratory pressure is not a reliable test of inspiratory muscle strength in mechanically ventilated patients. Am Rev Respir Dis 142:529–532
Polkey MI, Duguet A, Luo Y, Hughes PD, Hart N, Hamnegard CH, Green M, Similowski T, Moxham J (2000) Anterior magnetic phrenic nerve stimulation: laboratory and clinical evaluation. Intensive Care Med 26:1065–1075
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
De Jonghe, B., Bastuji-Garin, S., Sharshar, T. et al. Does ICU-acquired paresis lengthen weaning from mechanical ventilation?. Intensive Care Med 30, 1117–1121 (2004). https://doi.org/10.1007/s00134-004-2174-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-004-2174-z