Abstract
Background
Low birth weight and preterm birth, and social disadvantage may negatively affect mental health of children, but findings have been inconsistent.
Objectives
To assess the influence of perinatal and social factors on mental health problems in children aged 7–9 years.
Methods
A random sample of 805 births in São Luís, Brazil was studied in 1997/1998 and again in 2005/2006. Perinatal, socioeconomic and demographic variables were assessed within 24 h after delivery. The Strengths and Difficulties Questionnaire (SDQ) was used to assess mental health problems in the children. Simple and multiple Poisson regressions were used for statistical analysis.
Results
The overall prevalence of mental health problems in the total sample was 47.7%. The prevalences of emotional and conduct problems were 58.2 and 48.8%, respectively. Only paternal age (<20 years) was associated with mental health problems as measured by the full SDQ scale (prevalence ratio PR = 1.27). Children born to single mothers (PR = 1.31) and those with birth weight from 1,500 to 2,499 g (PR = 1.18) and from 2,500 to 2,999 g (PR = 1.17) had a higher risk of emotional problems, but those from low income families had a lower risk (PR = 0.80). Children with a father of less than 20 years had a higher risk of having problems with their peers (PR = 1.75). A maternal education of 9 years or over was inversely associated with peer (PR = 0.70) and conduct problems (PR = 0.73). Girls had a lower risk of conduct (PR = 0.77) and hyperactivity problems (PR = 0.68). A maternal education of 4 years or less increased the risk of hyperactivity (PR = 1.48).
Conclusions
Socioeconomic and demographic conditions were better predictors of mental health problems in children than birth weight or preterm birth. However, since most effect sizes were small most mental health problems were, unexplained by the variables in the study.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Low birth weight (LBW) and preterm birth are related to neonatal mortality [30, 44]. Scientific and technological advances have increased the survival rate of newborns, but morbidity has increased [27] compromising the psychological development of children. This may have contributed to higher prevalence of long-term emotional (internalizing patterns) and behavioural problems (externalizing patterns) [32, 41]. Longitudinal studies assessing the effects of LBW and preterm birth on child development have showed a high risk of emotional and behavioural problems [42, 43] but findings have not been consistent [15, 22].
Socioeconomic factors can also have an effect on psychological problems in childhood [25, 38]. Low family income and unemployment result in difficulties in buying consumer goods and access to leisure and educational facilities, which influence the way families care for their children, and may be associated with psychosocial distress [11]. In Brazil, poverty, maternal psychiatric illness, and family violence were all strongly associated with higher rates of probable psychiatric disorders among 7–14-year-olds [13].
In developing countries, few investigations have been conducted on the relative influence of LBW, preterm birth, and socioeconomic factors on mental health problems during childhood [28]. In these countries, social disadvantage in terms of poverty and lack of opportunities are on a greater scale than in developed countries. In developing countries it is important to use scarce resources efficiently; thus advice to policy makers in government on the effects of material conditions on the psychological development of children is essential as this is an important feature of human capital [10]. In countries of intermediate development such as Brazil, LBW is common because of a high birth rate in young women and the liberal use of obstetric technologies (e.g. caesarian sections) [44].
In São Luís, a poor Brazilian region, we started a longitudinal study based on newborns in 1997/1998. In our second sweep in 2005/2006, we collected information on common psychological problems in 7–9-year-olds. The aims of this study were to assess the prevalence of emotional and behavioural problems, and to assess the possible contribution of perinatal factors, especially LBW and preterm birth, and socioeconomic and demographic factors to common mental health problems in childhood.
Methods
Study site and sample
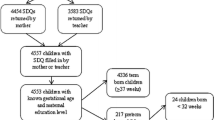
This study is based on data from the first birth cohort undertaken in São Luís (1997/1998) and a follow-up survey conducted in 2005/2006 [5]. São Luís is the capital of the State of Maranhão, in the Northeast of Brazil, one of the poorest regions in the country, with 957,515 inhabitants in 2007 [24]. Data in the first survey were collected from March 1997 to February 1998. Selection of newborns was carried out using systematic sampling, stratified according to the number of births at each of 10 public and private maternity hospitals in the city. In each hospital one out of seven children was randomly selected. 2,541 hospital births were sampled including live births, stillbirths, and single or multiple deliveries of mothers residing in São Luís [5]. The sample represents births in the city since hospital deliveries corresponded to 96.3% of total births; 5.8% of these refused to participate. After exclusion of multiple deliveries and stillbirths, the final sample consisted of 2,443 births (Fig. 1).
Five birth weight groups were considered for the follow-up study: very low birth weight (VLBW < 1,500 g), low birth weight (LBW 1,500–2,500 g), insufficient birth weight (2,500–2,999 g), normal birth weight (3,000–4,249 g), and children whose birth weight was at least two standard deviations above the population mean, who were classified as high birth weight (HBW ≥ 4,250 g). The children within the weight ranges with the smallest number of newborns (VLBW, LBW, HBW) were over-sampled in order to increase the power of study.
Excluding 65 deaths in the first year of life, 2,378 children were still alive at 1 year of age (Fig. 1). The intention was to follow-up all VLBW, LBW and HBW children and a one in three fraction of the normal and insufficient birth weight groups were selected for the follow-up study. Thus, all the parents or the person responsible for a child in the VLBW, LBW, or HBW groups and a fraction of those in the insufficient and normal birth weight groups were invited to participate in the study. Children were traced at schools, or using the addresses supplied by the mother at birth and by media advertising. Follow-up losses occurred due to migration, impossibility to locate the children, children not enrolled in school, and school or parental refusal. We were able to follow up 673 children, 81 of low birth weight, 19 high birth weight and 573 normal and insufficient birth weight, a follow up rate of 72.7%.
Since we anticipated that the final size of these groups would provide low statistical power to test some of the hypotheses because of attrition and high mortality of low birth weight children, a supplementary sample of 132 children who were 17 VLBW, 102 LBW, and 13 HBW was also included (Fig. 1). Children born at the time of the cohort studied, whose birth weight and gestational age were within the range as confirmed by hospital records, child’s medical record, or health card were invited to participate in the follow-up study.
The final sample consisted of 805 children, among them 22 VLBW, 178 LBW, and 32 HBW. This sample size has an 80% power to detect a prevalence ratio of 1:2 for exposures as common as 50%, with 5% significance level.
Data collection and instruments
The parents completed the Strength and Difficulties Questionnaire (SDQ) with the aid of trained psychologists responsible for psychological evaluation. When necessary, questions were read to the parents if they were illiterate and only those words/questions that were hard to understand were explained to them. The symptoms were not explained to the parents to avoid bias. The SDQ is an instrument developed by Goodman [19], which has been validated and adapted for Brazilian children [13]. The difficulties and skills of children/adolescents are ascertained from parental report of symptoms and problems. It consists of five subscales, each containing five items: (1) emotional symptoms, (2) conduct problems, (3) hyperactivity, (4) peer problems, and (5) prosocial behaviour. The scores for each subscale and the total score are classified as normal, borderline, or abnormal [19].
In the present study, we only considered the score of the questionnaire completed by the parents (SDQP4-16), and dichotomized the total score and the score for each subscale into absence (normal and borderline) or presence of mental health problems according to the proposed standardization [19, 27]. The prosocial behaviour subscale, which measures the sociability of the child, was not used in this study because it measures strength and not difficulty. The response variables were those referring to the mental health of the child as measured by the SDQ [19] on the basis of the total score of the questionnaire (a child with a score of 17 or over was considered to have psychological difficulties) and the threshold for the four subscales were: (1) emotional (>5), (2) peer problems (>4), (3) conduct problems (>4), and (4) hyperactivity (>7).
The remaining variables collected at birth were sex, duration of the gestation (term or preterm, the latter being <37 weeks assessed from mother’s information about the last normal menstrual period), birth weight in grams (500–1,499, 1,500–2,499, 2,500–2,999, 3,000–4,249, ≥4,250), paternal and maternal age in years (less than 20, 20–34, ≥35), maternal full time education in years (0–4, 5–8, ≥9), mother’s marital status (married, cohabiting, single), and family income divided into tertiles (high, middle, low, and unknown).
Statistical analysis
Due to the complex sampling design, as low and high birth weight children were oversampled, sampling weights were calculated based on information from birth records and accounted for different probabilities of selection from birth weight and preterm birth categories and allowing for non-response. Stratification by birth weight has also been taken into account.
In the univariable analysis, prevalence ratios (PRs) and their respective 95% confidence intervals were estimated in Poisson regression models because when the outcome is common, estimation of odds ratio in logistic regression analyses tend to produce false positive associations [2]. In multivariable analysis, all variables were entered in the model but the variables were removed from the adjusted model one by one (stepwise backward elimination) according to their statistical significance, with those with a p value < 0.10 being left in the final model [23], but only associations with p < 0.05 were considered statistically significant. Analyses were done for the full SDQ scale and for each of its four subscales, since previous reports suggest that factors associated with externalizing (peer and conduct problems and attention deficit/hyperactivity disorder) and internalizing problems (emotional symptoms) may differ [16, 33]. Effect sizes were considered small when PR was lower than 1.40 or higher than 0.7, and intermediate if between 1.40 and 2.30 or between 0.7 and 0.4. We used this lower PR because the prevalence of our outcomes was high and it has been shown that the relation between the differences in a pair of prevalences and the associated PR varies with the size of the prevalence, larger prevalences are associated with lower PR [12].
The project was approved by the Research Ethics Committees of the University Hospital/Federal University of Maranhão (No 3104-476/2005), and parents or carers gave written informed consent to participate.
Results
We compared characteristics between those who participated in the second survey and those who did not. There was a lower proportion of children born to families earning less than the minimum wage in the follow-up. There were no differences regarding the other independent variables in the analyses (Table 1).
The prevalence of mental health problems as measured by the SDQ score was 47.7%, with the highest levels being detected for the subscales emotional symptoms (58.2%) and conduct problems (48.8%), and the lowest for peer problems (27.2%) and hyperactivity (32.2%) (Table 2). Table 2 shows the median and interquartile range (IQR) for the full SDQ scale and its subscales.
Paternal age of less than 20 years and being born to a single mother at the time of birth increased the risk of mental health problems as measured by the total SDQ score. Birth weight and preterm birth were not associated with mental health problems. In the adjusted model for mental health problems only paternal age of less than 20 years was associated with the total SDQ score (PR = 1.27). The effect size was small (Table 3).
Being born to a single mother and having a birth weight of 1500–2,499 or 2,500–2,999 g were associated with emotional symptoms in the children, but the effect sizes were small (Table 4). Children whose family income was low were less likely to have emotional problems than the reference group, but the effect size was small. None of the other variables were associated with emotional symptoms in univariable or multivariable analysis (Table 4).
Children whose fathers were below 20 years at their birth were more likely to have peer problems and the effect size of the association was moderate (Table 4). Maternal education of 9 or more years was associated with fewer peer problems (Table 4). In the univariable analysis cohabitation and single motherhood were associated with more peer problems, but the associations disappeared after adjustment.
Girls were less likely to have conduct problems and attention deficit than boys, the effect size being small for conduct problems and intermediate for attention deficit. High maternal education protected the child from having conduct problems, whereas low maternal schooling was associated with higher prevalence of attention deficit (Table 5).
Discussion
Main findings
In spite of the high prevalence of difficulties in the four domains, especially emotional and conduct problems, the effect of birth weight and socioeconomic factors was only mildly associated with any of the outcomes. Birth weight of 1,500–2,499 or 2,500–2,999 g and being a single mother were associated with emotional symptoms, but not with conduct problems. Low paternal age at child’s birth was associated with increased risk of mental health problems as measured by the full SDQ scale and peer problems. Higher education of the mother protected the child from conduct problems, but low family income was associated with a lower risk of emotional problems. A maternal education of 9 years or more was a protective factor against peer and conduct problems whereas low maternal schooling increased the risk of attention deficit/hyperactivity disorder. Preterm birth was not associated with mental health problems. As expected, girls were less likely to have conduct problems and attention deficit/hyperactivity disorder than boys.
High prevalence of psychological problems
We were surprised by the very high prevalence of psychological problems in our study. A review study has shown a great heterogeneity in the prevalence of psychological problems among children, from as low as 5% to as high as 50% [14]. Results of the BELLA study show that 14.5% of those aged 7–17 years had an overall mental health problem based on SDQ scores [36]. The Copenhagen Child Cohort indicated a prevalence of mental health problems of 16–18% in children [45]. A population prevalence study of emotional and behavioural disorders among 6–12 year old children in Minia, Egypt using SDQ indicated 20.6% prevalence of total difficulties [9].
Previous Brazilian studies reported lower prevalences than those in the current study. Most other Brazilian studies reported prevalences between 19.0 and 24.6% [7, 31, 34], but a population-based study among all 848 mothers of children/adolescents (5–14-years-old) from Northeast Brazil, found a prevalence of 5.3% (using the SDQ impact supplement) [20]. We do not have an explanation for the large difference in prevalences between the two studies carried out in the same North eastern region of Brazil. We do not believe that reading the questions to mothers that were not able to read or explaining to them words/terms that were hard to understand may have somehow influenced the high prevalence reported.
Emotional symptoms and conduct problems were very common among children in our study. The lowest rates were those of peer problems and symptoms of attention deficit/hyperactivity disorder. An international study indicated a 4.1% prevalence of emotional problems, a 5.4% prevalence of emotional symptoms, a 5.4% prevalence of conduct and peer problems, and an 8.8% prevalence of attention deficit/hyperactivity disorder [41], much lower prevalences than those in our study.
Artifact as an explanation of the high prevalence of psychological problems
As the psychologists in our study were trained in the appropriate use of the instrument, and the SDQ has previously been validated and adapted for the Brazilian population [14, 18], it is unlikely that the administration of the test or the characteristics of the SDQ could explain the high prevalence of psychological problems. It is possible that the instrument is more difficult to administer in people with a higher level of poverty and lower education level, as they may have increased difficulty in understanding the questions. However, the participants in the study corresponded to a cross section of the social spectrum in São Luís and differences between social groups were small in our study. It is worth considering that the highest educational group in our study was 9 years or more, which is low in comparison to years of education in developed countries. Another possible explanation could be that parents who agreed to participate in the study were those who had a child with a psychological problem, but the comparison between participants and non-participants did not show large differences between these two groups. The parental or carer threshold of perception of a problem in a child might have been too low in São Luís. This explanation may have played a role in our study, as it has been shown in an international study of adults that the General Health Questionnaire, an instrument to assess psychological distress, has a large degree of heterogeneity in scores according to the country [17].
Causal explanations
The higher prevalence of mental health problems observed in the present study may have been associated with the socioeconomic and demographic conditions of the majority of the population. São Luís is located in one of the least developed regions of Brazil. Social inequalities in Brazil, one of the countries with the worse distribution of wealth in the world, may be one of the most important factors stopping children from reaching their full health and psychological development [6]. In our study there were several associations which would indicate that social factors may have played a role, especially, but not only, in terms of externalizing problems. Low maternal education, low paternal age and single status at the time of the birth of the child were significantly associated with the SDQ outcomes. Higher maternal education level has been shown to be a protective factor in developmental problems [1] by providing a more stimulating environment [10] promoting a more positive disposition towards education [47] and offering better emotional and material support [29]. It seems that families which function well are able to provide appropriate emotional support decreasing the risk of the child developing emotional and behavioural problems [8] probably by making the child more resilient and thus less vulnerable to stressful social events [21]. Although this paradigm was within our expectation, our results only partially support this explanation, as children from families with low income were protected against emotional symptoms. This is an unexpected finding in contrast to most studies which found that low family income is related to psychiatric disorders [11, 13]. It is possible that in our study other factors associated with poverty such as education level, paternal age, and marital status were more important contributors to psychological problems. Another reason for being cautious in interpreting our results as endorsing material conditions as the main explanation of psychological problems in the child is that the effect sizes of the socioeconomic variables were unexpectedly small and children from all social groups appeared to have a high prevalence of psychological problems.
The present results indicate that younger paternal age increases the risk of mental health problems (full SDQ scale) and of peer problems. This finding may be related to the low level of paternal emotional maturity and lower financial stability with consequent lower emotional support for the child, generating insecurity and difficulty in the development of social skills [10] possibly by decreasing cognitive development, social competence and comfort of the children [4]. In a previous study young maternal age was associated with externalizing problems among 2-year-old children [16] but other paper reported higher rates of mental health problems among children of older parents [40]. Maternal and paternal ages are usually highly correlated, but this high correlation does not explain the lack of effect of maternal age in our study because maternal age was not associated with any psychological problems in children in the unadjusted analyses.
In the present study, children born to a single mother had higher risk of emotional symptoms and this may be a contributing factor to the high rate of emotional symptoms in this population. Our study does not offer a chain of events which make children of single mothers more vulnerable to psychological problems, but the insecurities of single motherhood accompanied by low education, low income and frequently starting a family before the age of 20 years may all play a role.
Other factors associated with mental health problems
In our study birth weight between 1,500–2,499 and 2,500–2,999 g was associated with a higher risk of emotional symptoms only. Our results are consistent with those of several studies which have shown that LBW is associated with psychological problems [3, 27], especially emotional problems [26, 37] However, our study also showed that birth weight is not associated with other types of psychological problems, and preterm children did not have higher prevalence of psychological difficulties. Another study has shown that exposure only to biological birth risks does not cause adaptive difficulties during development [48]. A possible reason why birth weight may be associated with only one of the dimensions of the SDQ, and that slightly could be the high first-year mortality rate of the children in São Luís. 69% of VLBW and 7.5% of LBW children died in the first year of life. It is possible that the non-detection of an association between birth weight with most SDQ outcomes was due to selective survival.
In agreement with previous reports, our results showed that boys have a greater risk of developing problems [35] than girls, especially externalizing problems [39, 46].
Strengths and weaknesses
This study is one of the few population studies based on a longitudinal design in a developing country, assessing the magnitude and risk factors of psychological problems in childhood in a socially deprived area. The study was conceived as truly representative and personnel were especially trained for this study. This population cohort study used over-representation of some birth weight groups with higher mortality rates which increased its statistical power.
The rate of attrition in the follow up survey was satisfactory. Based on our initial survey, we were able to demonstrate that only differences between participants and non-participants at follow-up were in relation to family income. We doubt that these differences had more than a slight effect on the prevalence or risk factors found in the study, except that the 95% confidence intervals would have been wider. Although we accept that the attrition rate was higher among low income children, we do not believe that the prevalence of psychological problems would be higher in our study because the effect of family income on psychological problems was small and remained significant in multivariable analysis only for emotional symptoms.
Since questions other than birth weight and gestational age from the supplementary sample were collected retrospectively, recall bias may have affected some estimates. To reduce the chance of bias only objective perinatal questions, less susceptible to recall bias, were included in the analysis. However, models excluding the supplementary sample showed similar results (data not shown, available on request). The only important difference was that birth weight <1,500 g reached significance in univariable analysis in relation to hyperactivity.
Another limitation of the study was the absence of mental health assessment of the mother. Since mental health problems of mothers are related to mental health problems in children, confounding due to this variable may have affected the estimates.
Implications and conclusions
The current study demonstrates that psychological problems are not restricted to any socio-demographic group in São Luís, but maternal education, marital status and paternal age can explain in part some psychological problems in childhood. Our study also provides some clues on the specificity of some risk factors by SDQ domain such as birth weight and family income on emotional problems, paternal age in peer problems, and maternal schooling in externalizing problems. Policy makers should be aware that social disadvantage has a deleterious effect on the psychological health of children, mainly but not exclusively in relation to externalizing problems. These disadvantages may affect health, and have a social cost, which may explain the persistence of dysfunctional families in a cycle of social disadvantage. Birth weight played a role in the etiology of internalizing (emotional) problems, but not externalizing problems. It is worth noting that although some social factors explained in part the high prevalence of psychological problems, a major component remained unexplained.
References
Andrade SA, Santos DN, Bastos AC, Pedromonico MR, de Almeida-Filho N, Barreto ML (2005) Family environment and child’s cognitive development: an epidemiological approach. Rev Saude Publica 39:606–611
Barros AJ, Hirakata VN (2003) Alternatives for logistic regression in cross-sectional studies: an empirical comparison of models that directly estimate the prevalence ratio. BMC Med Res Methodol 3:21
Bhutta AT, Cleves MA, Casey PH, Cradock MM, Anand KJ (2002) Cognitive and behavioural outcomes of school-aged children who were born preterm: a meta-analysis. JAMA 288:728–737
Cabrera NJ, Tamis-LeMonda CS, Bradley RH, Hofferth S, Lamb ME (2000) Fatherhood in the twenty-first century. Child Dev 71:127–136
Cardoso VC, Simoes VM, Barbieri MA, Silva AA, Bettiol H, Alves MT, Goldani MZ (2007) Profile of three Brazilian birth cohort studies in Ribeirao Preto, SP and São Luís, MA. Braz J Med Biol Res 40:1165–1176
CNDSS (2008) Relatório Final da Comissão Nacional sobre Determinantes Sociais da Saúde: As Causas Sociais das Iniqüidades em Saúde no Brasil. In: Editora Fiocruz, p 216
Cury CR, Golfeto JH (2003) Strengths and Difficulties Questionnaire (SDQ): a study of school children in Ribeirao Preto. Rev Bras Psiquiatr 25:139–145
DeWolfe N, Byrne JM, Bawden HN (2000) ADHD in preschool children: parent-rated psychosocial correlates. Dev Med Child Neurol 42:825–830
Elhamid AA, Howe A, Reading R (2009) Prevalence of emotional and behavioural problems among 6–12 year old children in Egypt. Soc Psychiatry Psychiatr Epidemiol 44:8–14
Ferriolli SH, Marturano EM, Puntel LP (2007) Family context and child mental health problems in the family health program. Rev Saude Publica 41:251–259
Fitzgerald M, Jeffers A (1994) Psychosocial factors associated with psychological problems in Irish children and their mothers. Econ Soc Rev 25:285–301
Fleiss JL, Williams JB, Dubro AF (1986) The logistic regression analysis of psychiatric data. J Psychiatr Res 20:195–209
Fleitlich B, Goodman R (2001) Social factors associated with child mental health problems in Brazil: cross sectional survey. BMJ 323:599–600
Fleitlich BW, Goodman R (2000) Epidemiologia. Rev Bras Psiquiatr 22:02–06
Gale CR, Martyn CN (2004) Birth weight and later risk of depression in a national birth cohort. Br J Psychiatry 184:28–33
Gilliom M, Shaw DS (2004) Codevelopment of externalizing and internalizing problems in early childhood. Dev Psychopathol 16:313–333
Goldberg DP, Gater R, Sartorius N, Ustun TB, Piccinelli M, Gureje O, Rutter C (1997) The validity of two versions of the GHQ in the WHO study of mental illness in general health care. Psychol Med 27:191–197
Goodman R (2001) Psychometric properties of the Strengths and Difficulties Questionnaire. J Am Acad Child Adolesc Psychiatry 40:1337–1345
Goodman R (1997) The Strengths and Difficulties Questionnaire: a research note. J Child Psychol Psychiatry 38:581–586
Goodman R, Neves dos Santos D, Robatto Nunes AP, Pereira de Miranda D, Fleitlich-Bilyk B, Almeida Filho N (2005) The Ilha de Mare study: a survey of child mental health problems in a predominantly African-Brazilian rural community. Soc Psychiatry Psychiatr Epidemiol 40:11–17
Halpern R, Figueiras AC (2004) Environmental influences on child mental health. J Pediatr (Rio J) 80:S104–S110
Hille ET, den Ouden AL, Saigal S, Wolke D, Lambert M, Whitaker A, Pinto-Martin JA, Hoult L, Meyer R, Feldman JF, Verloove-Vanhorick SP, Paneth N (2001) Behavioural problems in children who weigh 1,000 g or less at birth in four countries. Lancet 357:1641–1643
Hosmer DW, Lemeshow S (2000) Applied logistic regression. Wiley, New York
GE IB (2004) Resultados da Amostra do Censo Demográfico 2000—Malha municipal digital do Brasil: situação em 2001. IBGE, Rio de Janeiro
Jansen PW, Raat H, Mackenbach JP, Jaddoe VW, Hofman A, Verhulst FC, Tiemeier H (2009) Socioeconomic inequalities in infant temperament: the generation R study. Soc Psychiatry Psychiatr Epidemiol 44:87–95
Johnson S (2007) Cognitive and behavioural outcomes following very preterm birth. Semin Fetal Neonatal Med 12:363–373
Kelly YJ, Nazroo JY, McMunn A, Boreham R, Marmot M (2001) Birthweight and behavioural problems in children: a modifiable effect? Int J Epidemiol 30:88–94
Kramer MS, Seguin L, Lydon J, Goulet L (2000) Socio-economic disparities in pregnancy outcome: why do the poor fare so poorly? Paediatr Perinat Epidemiol 14:194–210
Martins Mde F, da Costa JS, Saforcada ET, Cunha MD (2004) Quality of the environment and associated factors: a pediatric study in Pelotas, Rio Grande do Sul, Brazil. Cad Saude Publica 20:710–718
Mathews TJ, MacDorman MF (2008) Infant mortality statistics from the 2005 period linked birth/infant death data set. Natl Vital Stat Rep 57:1–32
Mello M, Mello A, Kohn R (2007) Epidemiologia da saúde mental no Brasil. Artmed, Porto Alegre
Nomura Y, Rajendran K, Brooks-Gunn J, Newcorn JH (2008) Roles of perinatal problems on adolescent antisocial behaviours among children born after 33 completed weeks: a prospective investigation. J Child Psychol Psychiatry 49:1108–1117
Orlebeke JF, Knol DL, Verhulst FC (1999) Child behaviour problems increased by maternal smoking during pregnancy. Arch Environ Health 54:15–19
Paula CS, Duarte CS, Bordin IA (2007) Prevalence of mental health problems in children and adolescents from the outskirts of Sao Paulo city: treatment needs and service capacity evaluation. Rev Bras Psiquiatr 29:11–17
Prior M, Virasinghe S, Smart D (2005) Behavioural problems in Sri Lankan schoolchildren: associations with socio-economic status, age, gender, academic progress, ethnicity and religion. Soc Psychiatry Psychiatr Epidemiol 40:654–662
Ravens-Sieberer U, Wille N, Erhart M, Bettge S, Wittchen HU, Rothenberger A, Herpertz-Dahlmann B, Resch F, Holling H, Bullinger M, Barkmann C, Schulte-Markwort M, Dopfner M (2008) Prevalence of mental health problems among children and adolescents in Germany: results of the BELLA study within the National Health Interview and Examination Survey. Eur Child Adolesc Psychiatry 17(Suppl 1):22–33
Reijneveld SA, de Kleine MJ, van Baar AL, Kollee LA, Verhaak CM, Verhulst FC, Verloove-Vanhorick SP (2006) Behavioural and emotional problems in very preterm and very low birthweight infants at age 5 years. Arch Dis Child Fetal Neonatal Ed 91:F423–F428
Roberts G, Howard K, Spittle AJ, Brown NC, Anderson PJ, Doyle LW (2008) Rates of early intervention services in very preterm children with developmental disabilities at age 2 years. J Paediatr Child Health 44:276–280
Rothenberger A, Becker A, Erhart M, Wille N, Ravens-Sieberer U (2008) Psychometric properties of the parent Strengths and Difficulties Questionnaire in the general population of German children and adolescents: results of the BELLA study. Eur Child Adolesc Psychiatry 17(Suppl 1):99–105
Saha S, Barnett AG, Buka SL, McGrath JJ (2009) Maternal age and paternal age are associated with distinct childhood behavioural outcomes in a general population birth cohort. Schizophr Res 115(2–3):130–135
Samara M, Marlow N, Wolke D (2008) Pervasive behaviour problems at 6 years of age in a total-population sample of children born at </= 25 weeks of gestation. Pediatrics 122:562–573
Schmidt LA, Miskovic V, Boyle MH, Saigal S (2008) Shyness and timidity in young adults who were born at extremely low birth weight. Pediatrics 122:e181–e187
Schothorst PF, Swaab-Barneveld H, van Engeland H (2007) Psychiatric disorders and MND in non-handicapped preterm children. Prevalence and stability from school age into adolescence. Eur Child Adolesc Psychiatry 16:439–448
Silva AA, Bettiol H, Barbieri MA, Brito LG, Pereira MM, Aragao VM, Ribeiro VS (2006) Which factors could explain the low birth weight paradox? Rev Saude Publica 40:648–655
Skovgaard AM, Olsen EM, Christiansen E, Houmann T, Landorph SL, Jorgensen T (2008) Predictors (0–10 months) of psychopathology at age 11/2 years—a general population study in The Copenhagen Child Cohort CCC 2000. J Child Psychol Psychiatry 49:553–562
Syed EU, Hussein SA, Mahmud S (2007) Screening for emotional and behavioural problems amongst 5–11-year-old school children in Karachi, Pakistan. Soc Psychiatry Psychiatr Epidemiol 42:421–427
Wang WL, Sung YT, Sung FC, Lu TH, Kuo SC, Li CY (2008) Low birth weight, prematurity, and paternal social status: impact on the basic competence test in Taiwanese adolescents. J Pediatr 153:333–338
Werner EE (1997) Vulnerable but invincible: high-risk children from birth to adulthood. Acta Paediatr Suppl 422:103–105
Acknowledgments
We are indebted to all the participants and schools which helped us to identify the children for our follow-up survey. The present study was financed by Fundação de Amparo a Pesquisa do Estado de São Paulo (FAPESP) and Conselho Nacional para o Desenvolvimento Científico e Tecnológico (CNPQ).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rodriguez, J.D.M., da Silva, A.A.M., Bettiol, H. et al. The impact of perinatal and socioeconomic factors on mental health problems of children from a poor Brazilian city: a longitudinal study. Soc Psychiatry Psychiatr Epidemiol 46, 381–391 (2011). https://doi.org/10.1007/s00127-010-0202-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-010-0202-6