Abstract
Aims/hypothesis
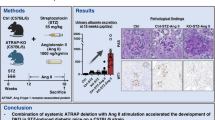
Diabetic nephropathy is one of the most common forms of chronic kidney disease. The role of adiponectin in the development of diabetic nephropathy has not been elucidated, and the aim of the present study was to investigate the hypothesis that deletion of the gene for adiponectin would accelerate diabetic nephropathy in the Akita mouse.
Methods
We followed four groups of mice from 4 weeks to 16 weeks of age (n ≥ 10 in each group): wild-type (WT) (Ins2 +/+ Adipoq +/+) mice; APN−/− (Ins2 +/+ Adipoq −/−) mice; Akita (Ins2 +/C96Y Adipoq +/+) mice and Akita/APN−/− (Ins2 +/C96Y Adipoq −/−) mice. The mice were then killed and diabetic kidney injury was assessed. In vitro experiments were performed in primary mesangial cells.
Results
Mice from both diabetic groups exhibited increased glomerular adiponectin receptor 1 (adipoR1) expression, kidney hypertrophy, glomerular enlargement, increased albuminuria and tissue oxidative stress compared with the WT control. Deletion of the adiponectin gene had no effect on glycaemia. However, Akita/APN−/− mice exhibited a greater extent of renal hypertrophy. In vitro, adiponectin attenuated high-glucose-induced phosphorylation of mammalian target of rapamycin (mTOR) and ribosomal protein S6 kinase (S6K). A higher level of fibrosis was observed in the tubulointerstitial and glomerular compartments of the Akita/APN−/− mice and adiponectin was found to inhibit TGFβ-induced Smad2 and Smad3 phosphorylation in vitro. There was an exaggerated inflammatory response in the Akita/APN−/− mice. Adiponectin also inhibited high-glucose-induced activation of nuclear factor κB (NFκB) in mesangial cells.
Conclusions/interpretation
Our data suggest that adiponectin is an important determinant of the kidney response to high glucose in vivo and in vitro.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetic nephropathy is a major form of chronic kidney disease leading to end-stage renal failure [1–3]. Much effort has gone into studying mechanisms by which hyperglycaemia causes chronic kidney injury [4, 5], but precise roles for factors involved in the pathogenesis of diabetic nephropathy are yet to be completely elucidated. Recent studies have shown that adiponectin may protect against mechanisms implicated in diabetic injury, including vascular injury [6, 7]. The goal of the current study was to define the role of adiponectin in the development of diabetic kidney injury.
Adiponectin is a 30 kDa hormone secreted predominantly by adipose tissue and has insulin-augmenting effects [8]. It has an impact on several signalling cascades, including the AMP-activated protein kinase (AMPK), peroxisome proliferator-activated receptor α, mitogen-activated protein kinase, Akt and cAMP pathways [9–11], after engagement of the two major receptors, adiponectin receptor 1 (adipoR1) and 2 (adipoR2) [12]. Adiponectin can also bind with T-cadherin to influence cellular responses, especially in cardiac tissue [13].
Previous studies have demonstrated that adiponectin may protect against diabetic injury by improving insulin sensitivity: replenishing adiponectin in obese mice attenuated insulin resistance and hyperglycaemia [14]. Additionally, mutant mice lacking adiponectin developed greater endothelial cell dysfunction in response to a high-fat diet, while the presence of adiponectin suppressed endothelial expression of adhesion molecules in response to TNFα stimulation [15, 16].
Adiponectin has also been found to influence kidney function. Sharma and colleagues identified a critical role of adiponectin in maintaining podocyte health that was dependent on inhibition of oxidative stress [17]. Pharmacological activation of AMPK, a major downstream signal mediator of adiponectin, was shown to suppress kidney H2O2 and monocyte chemotactic protein-1 (MCP-1) in mice on a high-fat diet [18]. However, the role of adiponectin in the development of mesangial expansion and glomerular hypertrophy has not been fully elucidated. We hypothesise that adiponectin attenuates hyperglycaemic kidney injury. To test this hypothesis, we crossed Ins2 +/+ Adipoq −/− (APN−/−) mice with the type 1 diabetic Ins2 +/C96Y Adipoq +/+ (Akita) mice to create a line of double-mutant Ins2 +/C96Y Adipoq −/− (Akita/APN−/−) mice and examined the pathological changes in the kidneys of these mice.
Methods
Animals
Ins2 +/+ Adipoq +/+ (wild-type [WT]) and Akita mice were purchased from The Jackson Laboratory (Bar Harbor, ME, USA). APN−/− mice were generously donated by S. Verma (Department of Surgery, University of Toronto, Toronto, ON, Canada) and were crossed with the Akita mice to generate the Akita/APN−/− mice. All mice were maintained on a C57BL/6 background, and were housed at the Division of Comparative Medicine at University of Toronto, with standard chow diet and free access to food and water. Male mice were followed from 4 to 16 weeks of age, with weekly blood glucose and body weight recordings. Twenty-four hour urine samples were obtained at 16 weeks of age and mice were then killed to extract plasma and kidney tissue. HbA1c levels were measured at the time of killing. See electronic supplementary material (ESM) Methods for further details. All experiments were conducted under the guidelines of the University of Toronto Animal Care Committee.
Cells
Human renal mesangial cells were purchased from Lonza (Clonetics, Lonza, Walkersville, MD, USA) and cultured as previously described [19]. Cells were maintained at 37°C in 5% CO2–95% air and used at passages 4–7.
Histology and immunohistochemistry
Mesangial matrix expansion and glomerular volume were measured on periodic acid–Schiff (PAS)-stained sections. Primary antibodies against adipoR1, adipoR2, α smooth muscle actin (αSMA), collagen IV (ColIV), F4/80 and Wilm’s tumour-1 (WT-1) were used for immunohistochemistry. Positivity for adipoR1, ColIV and WT-1 staining was assessed in glomeruli, αSMA staining was assessed on whole-kidney sections excluding the large blood vessels and F4/80 staining was assessed on whole-kidney sections. Quantification of PAS-positive staining and immunohistochemistry was completed using the Aperio ImageScope software (Leica Microsystems, Concord, ON, Canada). See ESM Methods for further details.
ELISA and colorimetric assays
ELISA kits were used to measure urinary levels of albumin, nitric oxide (NO), malondialdehyde (MDA) and nephrin, as well as the tissue level of MCP-1 in the kidney. Urinary albumin levels were used to calculate the 24 h urinary albumin excretion (UAE) rate. Levels of NO and MDA in urine were normalised to urinary creatinine concentration, while the level of MCP-1 in the kidney was normalised to total protein concentrations. See ESM Methods for further details.
Western blot
Primary antibodies against the following proteins were used for immunoblot: phospho- and total mammalian target of rapamycin (mTOR); phospho- and total p70 ribosomal protein S6 kinase (S6K); phospho- and total Smad2; phospho- and total Smad3 and β-actin. Mesangial cells were stimulated with high glucose (30 mmol/l, 1 h) or TGF-β (2 ng/ml, 1 h) with or without adiponectin (100 ng/ml, 30 min pre-incubation), then collected and lysed. Mannitol was used as an osmotic control for high-glucose experiments. Protein concentrations were determined by the Bradford method. Scion Image software (Scion, release beta 4.0.2, Frederick, MD, USA) was used for densitometry calculation. See ESM Methods for further details.
NFκB activity assay
Mesangial cells were co-transfected with pNFκB-Luc plasmid and pRL-TK reporter vector, then treated with high glucose or TNFα (20 ng/ml), with or without adiponectin (100 ng/ml) or apocynin (100 μmol/l), for 24 h. Luciferase activity was determined with a spectrometer. Total protein measured with Bradford assay was used to normalise activity results. See ESM Methods for further details.
Dihydroethidium stain
Mesangial cells cultured on glass cover slips were incubated for 18 h in normal glucose or high glucose with or without adiponectin. Cells were then washed with PBS and stained with dihydroethidium (DHE; 2 μmol/l, 1 h at 37°C in the dark). After washing, cells were mounted onto glass slides and visualised under a confocal microscope. At least 12 high-power fields were captured for semiquantitative scoring of fluorescent intensity. See ESM Methods for further details.
Lucigenin enhanced chemiluminescence assay
NADPH oxidase activity was measured by lucigenin enhanced chemiluminescence assay as previously described [20]. Cultured mesangial cells were treated under the following conditions for 18 h before collection: normal glucose; high glucose with or without adiponectin (pretreatment for 1 h); specific antibodies against adipoR1 (10 μg/ml, pretreatment for 1 h) and adipoR2 (10 μg/ml, pretreatment for 1 h) and non-specific goat IgG. Mannitol was used as an osmotic control. Cell lysates were mixed with NADPH (100 μmol/l) and lucigenin (5 μmol/l). Peak light emission was recorded and normalised to the total protein concentration as determined by Bradford assay. See ESM Methods for further details.
Statistical analysis
Results are shown as mean ± SE. GraphPad Prism 5 (GraphPad Software, La Jolla, CA, USA) was used for statistical analyses. For multiple-group comparison, one-way ANOVA with Bonferroni’s post hoc test was performed and for two-group comparison, unpaired t test was performed. Statistical significance was set at p ≤ 0.05.
Results
Whole-animal data
All four groups of experimental mice exhibited an increase in body weight between 4 and 16 weeks of age (Fig. 1a). Beginning from 8 weeks of age, Akita and Akita/APN−/− mice became stably diabetic (Fig. 1b), with comparable rise in blood glucose levels (HbA1c: Akita 11.9% [107 mmol/mol] vs Akita/APN−/− 12.0% [108 mmol/mol], Fig. 1c). Blood chemistry measurements showed increased triacylglycerol levels in Akita/APN−/− mice compared with the Akita mice (Table 1).
(a, b) Changes in body weight (a) and blood glucose (b) levels were followed in the WT (circles), APN−/− (squares), Akita (triangles) and Akita/APN−/− (inverted triangles) mice weekly from 4 weeks to 16 weeks of age. (c) HbA1c levels in diabetic mice were measured at the time of death. At least six mice were used in each experimental group at any given age for body weight and blood glucose assessments. For HbA1c, n = 3 for Akita mice, n = 5 for Akita/APN−/− mice. To convert values for HbA1c in mmol/mol to %, use the equation: HbA1c (%) = (0.09148 × HbA1c [mmol/mol]) + 2.152
Immunohistochemistry for adipoR1 showed the most intense staining in glomeruli, with positive signals in both podocytes and mesangia (Fig. 2a–d, i). Staining was increased in the glomeruli of diabetic mice (Fig. 2k). Deletion of the gene for adiponectin did not alter baseline glomerular adipoR1, but caused a trend towards more glomerular adipoR1-positive areas in diabetic mice. Positive staining for adipoR1 could also be identified in the proximal tubules. No reliable staining for adipoR2 was detected in the kidney sections of our experimental mice (Fig. 2e–h, j).
Expression of adiponectin receptors in kidney. (a–h) Representative images for adipoR1 (a–d) and adipoR2 (e–h) immunohistochemical stainings are shown. (i, j) Sections incubated without primary antibodies were used as negative controls for adipoR1 (R1 Neg) and adipoR2 (R2 Neg). Magnification, ×200. (k) The percentage of adipoR1-positive area in glomeruli was computed using ImageScope software. Results are presented as mean ± SE, n ≥ 9 for each group. *p < 0.05 vs WT mice
Assessment of kidney hypertrophy
Kidney weight was increased in the Akita mice and further in the Akita/APN−/− mice (Fig. 3a, b). This was accompanied by even greater increases in kidney-to-body weight ratio (Fig. 3c). In agreement with increased kidney weight, mean glomerular volume was increased in the diabetic Akita and Akita/APN−/− mice compared with WT mice (Fig. 3d). The mean size of glomeruli was not significantly different between the two diabetic groups despite a higher mean glomerular volume in the Akita/APN−/− mice.
Body weight (a), kidney weight (b), kidney/body weight ratio (c) and glomerular volume (d) were assessed in 16-week-old mice. Glomerular volumes were calculated from mean glomerular areas in PAS-stained sections. Data are shown as mean ± SE. n ≥ 19 for body weight, kidney weight and kidney/body weight ratio in each experimental group; n ≥ 8 for glomerular volume in each experimental group. *p < 0.05 vs WT mice; † p < 0.05 vs Akita mice
To identify the mechanism(s) responsible for kidney hypertrophy we studied the effect of adiponectin on high-glucose-induced mTOR activation in mesangial cells. The dose of adiponectin was shown to be effective previously in cultured proximal tubular cells [20], and again verified in cultured mesangial cells (ESM Fig. 1). Phosphorylation of mTOR and S6K was increased by high glucose and suppressed by co-incubation with adiponectin (Fig. 4). The high-glucose-induced mTOR phosphorylation diminished to baseline after 24 h, while a non-significant increase in S6K phosphorylation was observed (ESM Fig. 2). Adiponectin was able to suppress the phosphorylation of S6K after incubation for 24 h. Increased osmotic pressure yielded no change in activation of mTOR signalling (ESM Fig. 3).
Adiponectin prevented high-glucose-induced activation of the mTOR signalling pathway in human mesangial cells. Cells were treated with the respective medium and collected for immunoblotting against phospho- and total mTOR (a, c) and S6K (b, d). NG, normal glucose (5.6 mmol/l); HG, high glucose (30 mmol/l); HA, high glucose with adiponectin (100 ng/ml). Results are presented as mean ± SE, n = 3 in each group. *p < 0.05 vs normal glucose; † p < 0.05 vs high glucose
Detection of renal fibrosis
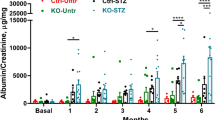
Kidney pathology was first examined at the microscopic structural level by PAS stain. The UAE rate was used for functional assessment (Fig. 5). Akita mice showed mesangial expansion (as quantified by PAS-positive area in glomerular profiles; Fig. 5a–d) that was exacerbated by the loss of the adiponectin gene (Fig. 5e). A similar pattern was seen for albuminuria (Fig. 5f). However the difference in UAE between the Akita and the Akita/APN−/− mice did not reach statistical significance by one-way ANOVA analysis of the four experimental groups, possibly due to the limited time of observation in the current study. Fibrosis within the tubulointerstitial and glomerular compartments was further assessed by immunohistochemical staining for αSMA (Fig. 6a–d) and ColIV (Fig. 6e–h), respectively. Similar trends emerged for quantification of both αSMA-positive and glomerular ColIV-positive areas, which were significantly increased in Akita/APN−/− mice compared with WT mice (Fig. 6i, j). Furthermore, for ColIV, the difference was significantly greater when comparing Akita/APN−/− mice with Akita mice.
Structural and functional changes in kidneys of experimental mice. (a–d) Representative images for PAS staining of kidney sections. Magnification, ×200. (e) Quantification of PAS-positive area in glomeruli. (f) Quantification of UAE rates in 16-week-old mice. Results are presented as mean ± SE. For PAS-positive area, n = 10 in each group; for UAE, n ≥ 6 for each experimental group. *p < 0.05 vs WT mice; † p < 0.05 vs Akita mice
(a–h) Immunohistochemical staining for αSMA (a–d) and ColIV (e–h) on renal sections. Magnification, ×200. (i, j) Quantification of αSMA-positive (i) and glomerular ColIV-positive areas (j). Results are presented as mean ± SE, n ≥ 6 for each experimental group. *p < 0.05 vs WT mice; † p < 0.05 vs Akita mice
To investigate the molecular mechanism(s) responsible for the role of adiponectin in fibrosis, mesangial cells were treated with TGF-β1 with or without adiponectin. Phosphorylation of Smad2 and Smad3 was strongly stimulated by TGF-β1 treatment, and adiponectin partially blocked this activation (Fig. 7). Treatment with adiponectin did not affect the baseline Smad2 and Smad3 activity (ESM Fig. 4).
Adiponectin partially inhibited phosphorylation of Smad2 and Smad3 following TGF-β1 stimulation in mesangial cells. Representative images of immunoblot (a) and the densitometry for Smad2 (b) and Smad3 (c) are shown. Results are presented as mean ± SE. n = 4 for Smad2 immunoblot; n = 3 for Smad3 immunoblot. *p < 0.05 vs control; † p < 0.05 vs TGF-β1 treatment
Pathological changes in inflammation
Infiltrating macrophages based on F4/80 staining (Fig. 8a–d) were significantly increased only in Akita/APN−/− mice compared with controls; Akita mice showed a trend towards increased macrophage infiltration when compared with WT mice (Fig. 8e). In agreement with F4/80 immunohistochemistry, tissue MCP-1 content was significantly higher only in the kidneys of Akita/APN−/− mice when compared with the WT mice, with a similar trend of increase in the Akita mice (Fig. 8f).
(a–d) Immunohistochemical staining for F4/80 on kidney sections (a–d) and the corresponding quantification (e) are shown. Magnification ×200. (f) Measurement of tissue MCP-1 concentration in kidney. Results are presented as mean ± SE. For F4/80, n ≥ 8 for each group; for MCP-1 measurement, n ≥ 4 for each group. *p < 0.05 vs WT
NFκB is a central mediator of inflammation and hence its activation was examined. Cultured mesangial cells were transfected with an NFκB-sensitive luciferase reporter construct and treated with high glucose with or without adiponectin. High glucose strongly activated NFκB in mesangial cells, and adiponectin reversed this effect (Fig. 9a). Reactive oxygen species (ROS) have been implicated in mediating many injurious effects of diabetes. In support of this, co-treatment with the antioxidant apocynin inhibited the high-glucose-induced NFκB activation (Fig. 9a). To test whether the inhibitory effect of adiponectin on NFκB activation was stimulus specific in cultured mesangial cells, the potential interaction between adiponectin and TNFα, a known activator of NFκB signalling, was investigated. Incubation with adiponectin caused a small, yet significant, reduction in TNFα-induced NFκB activation (Fig. 9b).
(a) High-glucose-induced NFκB activation in mesangial cells was inhibited by adiponectin. Co-incubation with apocynin also suppressed the NFκB activity after high-glucose treatment. (b) Adiponectin induced a modest reduction in NFκB activity after TNFα stimulation. Vector-transfected cells cultured in regular medium were used as controls. Results are shown as mean ± SE, n = 3 in each group. *p < 0.05 vs controls; † p < 0.05 vs high glucose (30 mmol/l) or TNFα treatment. RLU, relative light units
Evaluation of oxidative stress
To further study the role of adiponectin in oxidative stress in the kidney in response to high glucose, the excretion of MDA and NO was quantified in 24 h urine samples. Diabetic mice exhibited higher levels of urinary NO (Fig. 10a) and MDA (Fig. 10b). Despite a higher mean value, the levels of MDA and NO in Akita/APN−/− mice failed to reach statistical significance when compared with the levels in Akita mice.
The direct effect of adiponectin on cellular oxidative stress in response to high glucose was then studied in mesangial cells, with DHE stain as a marker for superoxide generation. High glucose raised ROS levels in mesangial cells, and co-incubation with adiponectin reduced this effect (Fig. 11a–d). In addition, adiponectin was able to inhibit the elevation in NADPH oxidase activity in mesangial cells exposed to high glucose (Fig. 11e). Stimulation of NADPH oxidase activity was not seen when mannitol was added as an osmotic control (ESM Fig. 5). As shown in vivo, adipoR1 appeared to be the dominant receptor for adiponectin in the kidney in our model (Fig. 2). Similarly in vitro, the suppression of high-glucose-induced NADPH oxidase activation by adiponectin was primarily mediated by adipoR1 in cultured mesangial cells, as demonstrated by the effect of blocking antibodies (ESM Fig. 6).
Adiponectin reversed the increase in high-glucose-induced oxidative stress in mesangial cells. (a–c) Representative images of DHE stains in cells treated with normal glucose (5.6 mmol/l, a), high glucose (30 mmol/l, b) and high glucose with adiponectin (c). Magnification, ×400. (d) Semiquantitative score for DHE intensity. (e) NADPH oxidase activity measurement in mesangial cells. Results are presented as mean ± SE. At least 12 images were used for DHE score; for NADPH oxidase activity assay, n ≥ 4 for each group. *p < 0.05 vs normal glucose; † p < 0.05 vs high glucose
Since it has been reported that the antioxidative effect of adiponectin could also contribute to a protective effect on podocytes [17], we evaluated podocyte numbers by quantifying WT-1-positive cells and urinary nephrin excretion (ESM Fig. 7). Neither the number of podocytes nor urinary nephrin excretion was significantly altered (ESM Fig. 7b, c), suggesting that pathological changes in podocytes were limited in our experimental mice at this stage of disease development.
Discussion
Adiponectin has been characterised as an insulin-sensitising adipokine that promotes glucose utilisation and lipid metabolism. In pancreatic beta cells, adiponectin prevents lipid-induced apoptosis by activating sphingosine-1-phosphate generation [21], as well as beta cell death from combined IL-1 and IFN-γ stimulation [22]. In the cardiovascular system, overexpression of adiponectin protects against atherosclerosis, while adiponectin deficiency exacerbates cardiac ischaemia–reperfusion injury [23, 24]. The administration of adiponectin as well as deletion of the gene for adiponectin have been reported to attenuate ischaemia–reperfusion-induced inflammation and apoptosis in the kidney [25, 26].
Sharma and colleagues were the first to establish a critical role for adiponectin in podocyte health [17]. These authors showed that adiponectin-null mice developed albuminuria and podocyte foot process effacement. Urinary measurements of oxidative stress and albuminuria were exacerbated by streptozotocin-induced diabetes mellitus. They demonstrated that adiponectin activated AMPK in cultured podocytes, maintained cell–cell contact and prevented high-glucose-induced changes in podocyte monolayer permeability. Adiponectin also prevented high-glucose-induced increases in NADPH oxidase 4 (Nox4) expression in cultured podocytes. Given these observations, we sought to more fully characterise the effect of deletion of the gene for adiponectin on the diabetic kidney. We also sought to extend our understanding of the impact of adiponectin on signal transduction in the mesangial cell. We selected the Akita mouse for our in vivo studies because it spontaneously develops profound but stable hyperglycaemia uncomplicated by the hormonal changes that accompany obesity. Our findings suggest that adiponectin plays a broad protective role in kidney responses to high glucose.
First we found that deletion of the adiponectin gene did not have a significant effect on weight gain or blood glucose in diabetic Akita mice. We next examined the effect of hyperglycaemia on adiponectin receptors. Based on our immunohistochemical analyses, adipoR1 appeared to be the dominant receptor. AdipoR1 was expressed in glomeruli, the primary target of diabetic injury, and its expression was increased in diabetic mice. In cultured mesangial cells, adipoR1 also predominantly mediated the inhibitory effect of adiponectin on high-glucose-induced NADPH oxidase activation. These results are consistent with previous findings of adiponectin receptor expression patterns in tissues and in kidney cell culture [12, 17, 20]. Interestingly, in studies using streptozotocin-induced diabetic rats and type 2 diabetic db/db mice, the expression of adipoR1 mRNA and protein was decreased in whole renal cortical tissue [27, 28]. These differences may be a consequence of the specific disease models but also suggest that adipoR1 expression may be regulated differentially in the glomerular and tubulointerstitial compartments of the kidney.
Although deletion of the adiponectin gene had no effect on blood glucose levels, we found that deletion led to exaggerated kidney hypertrophy in diabetic mice. Mesangial cells are important targets in diabetes [29], and we elected to study the effect of adiponectin on signal transduction pathways linked to cell hypertrophy, specifically the activation of mTOR by high glucose [30]. Previous studies in vascular smooth muscle cells [31] and in mesangial cells treated with platelet-derived growth factor [32] have demonstrated an interaction between adiponectin and this signalling pathway via AMPK. In accordance with these observations, our findings in mesangial cells showed that adiponectin attenuated high-glucose-induced mTOR and S6K activation, suggesting that mTOR pathway activation potentially mediates the exaggerated renal hypertrophic effect we observed in the diabetic Akita/APN−/− mice.
In addition to hypertrophy, long-standing hyperglycaemia is associated with fibrosis in the glomerular and tubulointerstitial compartments of the kidney. We found that glomerular matrix expansion was significantly increased in Akita/APN−/− mice compared with Akita mice, and there was a trend towards higher UAE. Consistent with the findings of renal hypertrophy and the structural and functional changes, the accumulation of αSMA and ColIV increased in the kidneys of Akita/APN−/− mice compared with WT mice. Our findings suggest that lack of adiponectin could accelerate fibrotic changes in the diabetic kidney. To better understand the effect of adiponectin on high-glucose-induced kidney fibrosis, we studied the effect of adiponectin on TGF-β signal transduction, because TGF-β has been linked to the expression of both αSMA and ColIV in the diabetic kidney [33, 34]. We observed that adiponectin reduced the phosphorylation of Smad2 and Smad3 in mesangial cells following TGF-β stimulation. Our results are in agreement with previous findings that adiponectin-null mice were susceptible to kidney fibrosis after subtotal nephrectomy and that administration of adiponectin ameliorated fibrosis in streptozotocin-induced diabetic rats [35, 36]. In contrast, Yang and colleagues discovered that adiponectin-null mice displayed less accumulation of matrix proteins in the kidney after both unilateral ureteral obstruction and renal ischaemia–reperfusion injury [37]. Adiponectin was able to stimulate monocyte–fibroblast differentiation in their model and thus promote renal fibrosis. Therefore, the mechanism by which adiponectin affects fibrotic changes in the kidney may be stimulus- and cell-type-specific.
Inflammation is a critical contributor to diabetic kidney injury [38]. We observed a marked increase in macrophage infiltration and MCP-1 levels in the kidneys of Akita/APN−/− mice. In support of the in vivo data, we found that adiponectin suppressed high-glucose-stimulated NFκB activation in mesangial cells, though this effect was not stimulus specific as adiponectin also inhibited the TNFα-induced NFκB activation. These findings are consistent with anti-inflammatory effects shown in previous studies using cultured human aortic endothelial cells [39] and in adiponectin-null mice with myocardial infarction [24]. In a study in humans, circulating levels of adiponectin also negatively correlated with various inflammatory markers, including C-reactive protein, IL-6 and phospholipase A2 [40]. Oxidative stress is another important pathogenic mechanism of diabetic kidney injury [41]. We measured urinary NO and MDA to assess kidney tissue oxidative stress and found that Akita/APN−/− mice tended to have a higher level of oxidative stress than Akita mice. Furthermore, adiponectin treatment of mesangial cells abrogated high-glucose-induced ROS generation and NADPH oxidase activation. Our data support the antioxidant role of adiponectin shown previously in endothelial cells [42] and podocytes [17]. Oxidative stress in our model was linked to mesangial cell injury and we found no measurable decline in podocyte number or increased urinary nephrin in the Akita mouse.
The current study has some important limitations. First, although several groups have used a 16 week time point for analyses of diabetic nephropathy, the changes in kidney structure and function are relatively modest on the C57BL/6 background [43–45]. This may have limited our ability to detect a significant difference in the UAE. Second, although WT-1 and nephrin excretion have been commonly used to assess podocyte injury [46–48], the lack of changes in these markers does not exclude a role for the podocyte in the phenotypical changes that we observed in our mice.
In summary, we found that deletion of the adiponectin gene exacerbated diabetes-induced kidney hypertrophy, fibrosis and inflammation. In vitro, adiponectin attenuated high-glucose-induced mTOR, TGF-β and NFκB signalling in glomerular mesangial cells. Together, this work supports the hypothesis that adiponectin is a protective factor in the kidney. Augmenting adiponectin signal transduction in the kidney may be an important treatment strategy in diabetic nephropathy.
Abbreviations
- adipoR1:
-
Adiponectin receptor 1
- adipoR2:
-
Adiponectin receptor 2
- AMPK:
-
AMP-activated protein kinase
- ColIV:
-
Collagen IV
- DHE:
-
Dihydroethidium
- MCP-1:
-
Monocyte chemotactic protein-1
- MDA:
-
Malondialdehyde
- mTOR:
-
Mammalian target of rapamycin
- NFκB:
-
Nuclear factor κB
- NO:
-
Nitric oxide
- PAS:
-
Periodic acid–Schiff
- ROS:
-
Reactive oxygen species
- αSMA:
-
α Smooth muscle actin
- S6K:
-
Ribosomal protein S6 kinase
- UAE:
-
Urinary albumin excretion
- WT:
-
Wild-type
- WT-1:
-
Wilm’s tumour-1
References
Tang SC (2010) Diabetic nephropathy: a global and growing threat. Hong Kong Med J 16:244–245
Packham DK, Alves TP, Dwyer JP et al (2012) Relative incidence of ESRD versus cardiovascular mortality in proteinuric type 2 diabetes and nephropathy: results from the DIAMETRIC (Diabetes Mellitus Treatment for Renal Insufficiency Consortium) database. Am J Kidney Dis 59:75–83
Eckardt KU, Coresh J, Devuyst O et al (2013) Evolving importance of kidney disease: from subspecialty to global health burden. Lancet 382:158–169
Brownlee M (2001) Biochemistry and molecular cell biology of diabetic complications. Nature 414:813–820
Sun YM, Su Y, Li J, Wang LF (2013) Recent advances in understanding the biochemical and molecular mechanism of diabetic nephropathy. Biochem Biophys Res Commun 433:359–361
Wiecek A, Adamczak M, Chudek J (2007) Adiponectin—an adipokine with unique metabolic properties. Nephrol Dial Transplant 22:981–988
Shetty S, Kusminski C, Scherer P (2009) Adiponectin in health and disease: evaluation of adiponectin-targeted drug development strategies. Trends Pharmacol Sci 30:234–239
Yamauchi T, Kamon J, Minokoshi Y et al (2002) Adiponectin stimulates glucose utilization and fatty-acid oxidation by activating AMP-activated protein kinase. Nat Med 8:1288–1295
Akingbemi BT (2013) Adiponectin receptors in energy homeostasis and obesity pathogenesis. Prog Mol Biol Transl Sci 114:317–342
Chou IP, Lin YY, Ding ST, Chen CY (2014) Adiponectin receptor 1 enhances fatty acid metabolism and cell survival in palmitate-treated HepG2 cells through the PI3 K/AKT pathway. Eur J Nutr 53:907–917
Kim JE, Song SE, Kim YW et al (2010) Adiponectin inhibits palmitate-induced apoptosis through suppression of reactive oxygen species in endothelial cells: involvement of cAMP/protein kinase A and AMP-activated protein kinase. J Endocrinol 207:35–44
Yamauchi T, Nio Y, Maki T et al (2007) Targeted disruption of AdipoR1 and AdipoR2 causes abrogation of adiponectin binding and metabolic actions. Nat Med 13:332–339
Denzel MS, Scimia MC, Zumstein PM, Walsh K, Ruiz-Lozano P, Ranscht B (2010) T-cadherin is critical for adiponectin-mediated cardioprotection in mice. J Clin Invest 120:4342–4352
Yamauchi T, Kamon J, Waki H et al (2001) The fat-derived hormone adiponectin reverses insulin resistance associated with both lipoatrophy and obesity. Nat Med 7:941–946
Ouchi N, Kihara S, Arita Y et al (2000) Adiponectin, an adipocyte-derived plasma protein, inhibits endothelial NF-κB signaling through a cAMP-dependent pathway. Circulation 102:1296–1301
Ouchi N, Ohishi M, Kihara S et al (2003) Association of hypoadiponectinemia with impaired vasoreactivity. Hypertension 42:231–234
Sharma K, Ramachandrarao S, Qiu G et al (2008) Adiponectin regulates albuminuria and podocyte function in mice. J Clin Invest 118:1645–1656
Decleves AE, Mathew AV, Cunard R, Sharma K (2011) AMPK mediates the initiation of kidney disease induced by a high-fat diet. J Am Soc Nephrol 22:1846–1855
Liu GC, Oudit GY, Fang F, Zhou J, Scholey JW (2012) Angiotensin-(1-7)-induced activation of ERK1/2 is cAMP/protein kinase A-dependent in glomerular mesangial cells. Am J Physiol Ren Physiol 302:F784–F790
Fang F, Liu GC, Kim C, Yassa R, Zhou J, Scholey JW (2013) Adiponectin attenuates angiotensin II-induced oxidative stress in renal tubular cells through AMPK and cAMP-Epac signal transduction pathways. Am J Physiol Ren Physiol 304:F1366–F1374
Holland WL, Miller RA, Wang ZV et al (2011) Receptor-mediated activation of ceramidase activity initiates the pleiotropic actions of adiponectin. Nat Med 17:55–63
Rakatzi I, Mueller H, Ritzeler O, Tennagels N, Eckel J (2004) Adiponectin counteracts cytokine- and fatty acid-induced apoptosis in the pancreatic beta-cell line INS-1. Diabetologia 47:249–258
Okamoto Y, Kihara S, Ouchi N et al (2002) Adiponectin reduces atherosclerosis in apolipoprotein E-deficient mice. Circulation 106:2767–2770
Shibata R, Sato K, Pimentel DR et al (2005) Adiponectin protects against myocardial ischemia-reperfusion injury through AMPK- and COX-2-dependent mechanisms. Nat Med 11:1096–1103
Cheng CF, Lian WS, Chen SH et al (2012) Protective effects of adiponectin against renal ischemia-reperfusion injury via prostacyclin-PPARα-heme oxygenase-1 signaling pathway. J Cell Physiol 227:239–249
Jin X, Chen J, Hu Z, Chan L, Wang Y (2013) Genetic deficiency of adiponectin protects against acute kidney injury. Kidney Int 83:604–614
Guo Z, Zhao Z (2007) Effect of N-acetylcysteine on plasma adiponectin and renal adiponectin receptors in streptozotocin-induced diabetic rats. Eur J Pharmacol 558:208–213
Tamura Y, Murayama T, Minami M, Matsubara T, Yokode M, Arai H (2012) Ezetimibe ameliorates early diabetic nephropathy in db/db mice. J Atheroscler Thromb 19:608–618
Qian Y, Feldman E, Pennathur S, Kretzler M, Brosius FC 3rd (2008) From fibrosis to sclerosis: mechanisms of glomerulosclerosis in diabetic nephropathy. Diabetes 57:1439–1445
Lieberthal W, Levine JS (2009) The role of the mammalian target of rapamycin (mTOR) in renal disease. J Am Soc Nephrol 20:2493–2502
Zhan JK, Wang YJ, Wang Y et al (2014) Adiponectin attenuates the osteoblastic differentiation of vascular smooth muscle cells through the AMPK/mTOR pathway. Exp Cell Res 323:352–358
Su YX, Deng HC, Zhang MX, Long J, Peng ZG (2012) Adiponectin inhibits PDGF-induced mesangial cell proliferation: regulation of mammalian target of rapamycin-mediated survival pathway by adenosine 5-monophosphate-activated protein kinase. Horm Metab Res 44:21–27
Liu X, Hubchak SC, Browne JA, Schnaper HW (2014) Epidermal growth factor inhibits transforming growth factor-β-induced fibrogenic differentiation marker expression through ERK activation. Cell Signal 26:2276–2283
Sharma K, Ziyadeh FN (1994) The emerging role of transforming growth factor-beta in kidney diseases. Am J Physiol 266:F829–F842
Nakamaki S, Satoh H, Kudoh A, Hayashi Y, Hirai H, Watanabe T (2011) Adiponectin reduces proteinuria in streptozotocin-induced diabetic Wistar rats. Exp Biol Med (Maywood) 236:614–620
Ohashi K, Iwatani H, Kihara S et al (2007) Exacerbation of albuminuria and renal fibrosis in subtotal renal ablation model of adiponectin-knockout mice. Arterioscler Thromb Vasc Biol 27:1910–1917
Yang J, Lin SC, Chen G et al (2013) Adiponectin promotes monocyte-to-fibroblast transition in renal fibrosis. J Am Soc Nephrol 24:1644–1659
Duran-Salgado MB, Rubio-Guerra AF (2014) Diabetic nephropathy and inflammation. World J Diabetes 5:393–398
Kobashi C, Urakaze M, Kishida M et al (2005) Adiponectin inhibits endothelial synthesis of interleukin-8. Circ Res 97:1245–1252
Krakoff J, Funahashi T, Stehouwer CD et al (2003) Inflammatory markers, adiponectin, and risk of type 2 diabetes in the Pima Indian. Diabetes Care 26:1745–1751
Badal SS, Danesh FR (2014) New insights into molecular mechanisms of diabetic kidney disease. Am J Kidney Dis 63:S63–S83
Essick EE, Ouchi N, Wilson RM et al (2011) Adiponectin mediates cardioprotection in oxidative stress-induced cardiac myocyte remodeling. Am J Physiol Heart Circ Physiol 301:H984–H993
Oudit GY, Liu GC, Zhong J et al (2010) Human recombinant ACE2 reduces the progression of diabetic nephropathy. Diabetes 59:529–538
Liu GC, Fang F, Zhou J et al (2012) Deletion of p47phox attenuates the progression of diabetic nephropathy and reduces the severity of diabetes in the Akita mouse. Diabetologia 55:2522–2532
Lo CS, Liu F, Shi Y et al (2012) Dual RAS blockade normalizes angiotensin-converting enzyme-2 expression and prevents hypertension and tubular apoptosis in Akita angiotensinogen-transgenic mice. Am J Physiol Ren Physiol 302:F840–F852
Schiffer M, Mundel P, Shaw AS, Bottinger EP (2004) A novel role for the adaptor molecule CD2-associated protein in transforming growth factor-beta-induced apoptosis. J Biol Chem 279:37004–37012
Chodavarapu H, Grobe N, Somineni HK, Salem ES, Madhu M, Elased KM (2013) Rosiglitazone treatment of type 2 diabetic db/db mice attenuates urinary albumin and angiotensin converting enzyme 2 excretion. PLoS One 8:e62833
Alter ML, Kretschmer A, von Websky K et al (2012) Early urinary and plasma biomarkers for experimental diabetic nephropathy. Clin Lab 58:659–671
Acknowledgements
The authors would like to acknowledge the expert technical assistance of the PRP Laboratory of the Pathology Department at University Health Network (Toronto, ON, Canada) and the Centre for Modeling Human Disease at Toronto Centre for Phenogenomics (Toronto, ON, Canada).
Funding
This work was supported by grants from the Heart and Stroke Foundation and the Canadian Institutes of Health Research (CIHR) to JWS and RJ. JWS was supported by a CIHR-Amgen Canada Inc. Chair in Kidney Research. FF is supported by CIHR-Banting Scholarship and Queen Elizabeth II-Graduate Scholarship in Science and Technology award. AK was supported by a Kidney Foundation of Canada Research Fellowship and the University of Toronto Clinician Scientist Training Program. GCL is supported by a Queen Elizabeth II-Graduate Scholarship in Science and Technology award. CL was supported by a Banting and Best Summer Studentship Award.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Contribution statement
All persons listed as authors contributed substantially to the experimental conception and design, acquisition of data or analysis and interpretation of data; all authors participated in the drafting of the article or revising it critically for important intellectual content and all gave final approval to the version to be published. JWS is the guarantor of this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Rohan John and James W. Scholey contributed equally to this manuscript.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM Methods
(PDF 367 kb)
ESM Fig. 1
(PDF 100 kb)
ESM Fig. 2
(PDF 471 kb)
ESM Fig. 3
(PDF 603 kb)
ESM Fig. 4
(PDF 631 kb)
ESM Fig. 5
(PDF 375 kb)
ESM Fig. 6
(PDF 406 kb)
ESM Fig. 7
(PDF 1,542 kb)
Rights and permissions
About this article
Cite this article
Fang, F., Bae, EH., Hu, A. et al. Deletion of the gene for adiponectin accelerates diabetic nephropathy in the Ins2 +/C96Y mouse. Diabetologia 58, 1668–1678 (2015). https://doi.org/10.1007/s00125-015-3605-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-015-3605-9