Abstract
Aims/hypothesis
Recent work has identified the important roles of M1 pro-inflammatory and M2 anti-inflammatory macrophages in the regulation of insulin sensitivity. Specifically, increased numbers of M2 macrophages and a decrease in M1 macrophages within the adipose tissue are associated with a state of enhanced insulin sensitivity. IL-10 is an anti-inflammatory cytokine and is a critical effector molecule of M2 macrophages.
Methods
In the present study, we examined the contribution of haematopoietic-cell-derived IL-10 to the development of obesity-induced inflammation and insulin resistance. We hypothesised that haematopoietic-cell-restricted deletion of IL-10 would exacerbate obesity-induced inflammation and insulin resistance. Lethally irradiated wild-type recipient mice receiving bone marrow from either wild-type or Il10-knockout mice were placed on either a chow or a high-fat diet for a period of 12 weeks and assessed for alterations in body composition, tissue inflammation and glucose and insulin tolerance.
Results
Contrary to our hypothesis, neither inflammation, as measured by the activation of pro-inflammatory stress kinases and gene expression of several pro-inflammatory cytokines in the adipose tissue and liver, nor diet-induced obesity and insulin resistance were exacerbated by the deletion of haematopoietic-cell-derived IL-10. Interestingly, however, Il10 mRNA expression and IL-10 protein production in liver and/or adipose tissue were markedly elevated in Il10-knockout bone-marrow-transplanted mice relative to wild-type bone marrow-transplanted mice.
Conclusions/interpretation
These data show that deletion of IL-10 from the haematopoietic system does not potentiate high-fat diet-induced inflammation or insulin resistance.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obesity, insulin resistance and type 2 diabetes are closely associated with a state of ‘low-grade’ chronic inflammation [1]. Specifically, elevated levels of pro-inflammatory cytokines such as TNFα, and infiltration of bone-marrow-derived macrophages (BMDMs) into adipose tissue appear to be key events mediating the deleterious effects of obesity on insulin sensitivity [2–4]. It is generally accepted that macrophages accumulate in the adipose tissue of obese humans and mice. Once resident within the adipose tissue, factors secreted by macrophages, such as TNFα, activate pro-inflammatory signalling molecules, such as c-Jun N-terminal kinase (JNK) and IκB kinase β (IKKβ), and initiate a state of local and, ultimately, systemic insulin resistance [5–8]. Underscoring the critical role of macrophages in the development of obesity-induced insulin resistance, the conditional deletion of CD11c+-expressing macrophages in obese mice results in a marked reduction in local and systemic inflammation and, importantly, normalisation of insulin sensitivity [9].
Resident tissue macrophages display considerable heterogeneity [10]. Lean chow-fed animals contain small amounts of resident adipose tissue macrophages (ATMs) and these ATMs stain positive for the surface markers F480, CD11b, and the anti-inflammatory marker macrophage galactose N-acetyl-galactosamine-specific lectin 1 (MGL1/CD301), but stain negative for CD11c. These MGL1+CD11c- ATM found in lean animals express many genes typical of the M2 alternatively activated state, including high expression of Il10, encoding the anti-inflammatory cytokine IL-10 [11–13]. In contrast, in high-fat-fed and genetically obese mice, macrophages show a characteristic triple-positive staining for F4/80, CD11b and CD11c and an absence of staining for MGL1/CD301 [11, 12, 14]. Thus, the progression from the lean to obese state results in a reduced expression of anti-inflammatory M2-macrophage-related genes, namely Arg1 and Il10, with a concomitant increase in the expression of pro-inflammatory M1-macrophage genes, including Tnf-α (also known as Tnf) and iNos (also known as Nos2), in ATM [11, 12]. While high-fat feeding does not alter the presence of the M2 MGL1+CD11c– cells, it induces the spatially restricted and more rapid accumulation of pro-inflammatory M1 MGL1– CD11c+ ATMs in ‘crown-like clusters’ surrounding dead adipocytes in the visceral region [12]. While the above studies support the idea that high-fat-feeding-induced obesity promotes an M2 to M1 polarisation shift, more recent data suggest that the M1–M2 ATM profile is relatively dynamic in nature and over the course of the high-fat-dietary period the M1 to M2 macrophage balance shifts, potentially reflecting periods of adipose tissue hypertrophy and re-modelling [15]. Underscoring the importance of macrophage polarisation state to the development of obesity-induced insulin resistance, the insulin-sensitising agent rosiglitazone dramatically increases the number of macrophages present in the adipose tissue depots of obese mice; however, these ATM are predominantly of the M2 anti-inflammatory state [16]. Recently, peroxisome proliferator-activated receptor γ (PPARγ) and δ (PPARδ) were identified as critical promoters of macrophage polarisation towards the M2 phenotype and, consequently, macrophage-specific deletion of PPARγ or PPARδ resulted in a reduced expression of M2-macrophage-specific genes in adipose tissue and liver, an increase in M1-macrophage-specific genes and, importantly, a worsening of glucose and insulin tolerance [17, 18].
While M2 macrophages express a wide range of anti-inflammatory genes, a critical effector of M2 macrophages is the anti-inflammatory cytokine IL-10 [19, 20]. Indeed, IL-10 or IL-10 receptor β-chain deficient mice develop chronic enterocolitis, an effect that can be substantially prevented with the treatment of IL-10 in Il10-knockout (KO) mice, demonstrating the importance of this cytokine in the regulation of host inflammatory responses [21–23]. Most [11, 24–28] but not all [29, 30] studies, support a protective role of IL-10 in the regulation of metabolic inflammation and insulin sensitivity both in vitro and in vivo. In addition, Il10 expression increases in adipose tissue following weight loss in obese patients, concomitant with a reduction in pro-inflammatory gene expression [31, 32]. To determine the contribution of haematopoietic-cell-derived IL-10 to the development of obesity-induced inflammation and insulin resistance we have used a bone marrow adoptive transfer model and hypothesised that haematopoietic-cell-restricted deletion of IL-10 would potentiate high-fat-diet-induced inflammation and insulin resistance.
Methods
Animal procedures
Wild-type C57BL/6 and global Il10-KO mice bred onto a C57BL/6 background (Jackson Laboratory, Bar Harbor, ME, USA) were housed in pathogen-free barrier-protected environment (12:12 h light/dark cycle) at the Baker IDI Alfred Medical Research and Education Precinct (AMREP) animal facility. All procedures were approved by the AMREP Animal Ethics Committee. When the mice were 6 weeks of age, we performed the bone marrow transplant (BMT) experiment described in detail in the Electronic supplementary material (ESM).
Body composition and metabolic data analysis
Over the entire course of the dietary intervention, lean body mass (LBM) and fat mass were measured fortnightly in conscious mice using the four in one EcoMRI body composition analyser (Columbus Instruments, Columbus, OH, USA). Mouse metabolic data were also collected at week 12 using the Comprehensive Laboratory Animal Monitoring System (CLAMS, Columbus Instruments). Mice were placed inside the metabolism cages for a 26-h period, with the first 2 h of data not included to allow for acclimatisation of mice to the cages. Oxygen-consumption and food-intake data were normalised to total body mass (ml/h and kJ/day, respectively).
Glucose homeostasis data
Intraperitoneal glucose tolerance tests (IPGTT) and intraperitoneal insulin tolerance tests (IPITT) were performed at the end of the 12 week dietary intervention following a 6 h fast. Mice received an intraperitoneal injection of 1 g glucose/kg LBM and 0.6 U/kg LBM (chow) or 0.75 U/kg LBM (high-fat diet) human insulin (Humulin, Eli Lilly, IN, USA) during the IPGTT and IPITT, respectively. By using a lower dose (0.6 U/kg LBM) of insulin in the chow-fed animals, incidents of extreme hypoglycaemia were avoided. Tail blood was collected over the 120 min of the IPGTT and IPITT and glucose levels were measured with human Accu-Chek blood monitors and test strips (Roche, Basel, Switzerland). Fasting and fed plasma insulin concentrations were analysed using rat/mouse insulin ELISA kits (Millipore, Billerica, MA, USA).
Cell culture
RAW264.7 murine macrophages were cultured in Dulbecco’s modified Eagle’s medium (Invitrogen, Carlsbad, CA, USA) containing low glucose and supplemented with 10% FBS and 1% penicillin/streptomycin (Invitrogen). The cells were grown to ~70–80% confluence and then treated with 0.5 mmol/l palmitate (Sigma-Aldrich, St Louis, MO, USA) conjugated to 2% BSA (wt/vol.) for 4 h, either in the presence or absence of 20 ng/ml recombinant murine IL-10 (PeproTech, Rocky Hill, NJ, USA). The control medium was also supplemented with 2% BSA. Additionally, BMDMs from wild-type C57BL/6 control and global Il10-KO mice were also treated with 100 ng/ml lipopolysaccharide (LPS) (L8274, Sigma-Aldrich), 20 ng/ml recombinant murine IL-4 (R&D Systems, St Louis, MO, USA) and 0.5 and 0.75 mmol/l palmitate (Sigma-Aldrich) for the times indicated. Following treatment, medium supernatant fractions were collected, cells were washed twice with ice-cold PBS and scraped in ice-cold lysis buffer or TRIzol Reagent (Invitrogen) and stored at −79°C.
BMDM experiments
To obtain primary BMDMs, mice between 6 and 12 weeks of age were killed with CO2 asphyxiation. Hind leg bones were stripped of muscle and connective tissues, placed in ethanol for 1 min and then ice-cold PBS. Marrow was flushed out with RPMI 1640 medium and spun at 500 g for 10 min. Cells were seeded 1 × 106/ml in RPMI 1640 media (Invitrogen) supplemented with glutamine and Hepes, 20% (vol./vol.) conditioned media from L929 cells, 15% FBS (vol./vol.), 100 U/ml penicillin and 0.1 mg/ml streptomycin. Cells remaining in suspension 24 h later were divided into treatment plates with additional supplemented RPMI medium and differentiated into macrophages over 4–7 days.
Protein analyses
Proteins were analysed by immunohistochemistry and western blot analyses using standard techniques described in detail in the ESM.
Real-time PCR
To extract RNA, ~30–50 mg of either epididymal white adipose tissue or liver was homogenised in 800 μl of TRIzol Reagent according to the manufacturer’s instructions (Invitrogen). Total RNA quantity and quality was measured using the ND-1000 NanoDrop Spectrophotometer (Thermo Scientific, Waltham, MA, USA). For each sample, 1,500 ng RNA was reverse transcribed and converted to cDNA using TaqMan Reverse Transcription Reagents (Applied Biosystems, Foster City, CA, USA). All gene expression analysis was performed using TaqMan Gene Expression Assays (Applied Biosystems), including 18 S probe and primers for housekeeping gene measurement. In each RT-PCR reaction, 50 ng of total cDNA was used.
Statistical analysis
Data were analysed with either two-way ANOVA or three-way repeated-measures ANOVA (SigmaStat Version 3.5) where appropriate. All data are expressed as means ± SEM. A p value of less than <0.05 was used to denote statistical significance.
Results
Elevated levels of fatty acids, in particular long-chain saturated fatty acids, are postulated to be key drivers of inflammation. Therefore, we initially examined whether IL-10 could prevent palmitate-induced inflammation. Accordingly, we treated Raw264.7 macrophages with 0.5 mmol/l palmitate for 4 h, either in the presence or absence of IL-10. As shown previously by Shi et al. [33], palmitate increased both membrane-bound and secreted TNF-α (Fig. 1a, b), but co-treatment with IL-10 markedly reduced palmitate-induced increases in both membrane-bound and secreted TNF-α (Fig. 1a, b).
IL-10 suppresses lipid-induced TNF-α production in Raw264.7 macrophages. a,b Raw264.7 macrophages treated for 4 h with: BSA-containing control media (Con); recombinant mouse IL-10 (20 ng/ml) (IL-10); or 0.5 mmol/l palmitate (2% BSA; Pal); or co-treated with IL-10 and palmitate (IL-10 + Pal). a Western blot analysis of pro-TNF-α (membrane bound) with densitometry quantification from cell lysates. b Analysis of secreted TNF-α from cell culture media supernatant fractions as measured by ELISA. Representation of three and two independent experiments performed in triplicate, respectively. Data are means ± SEM; interaction effect, *p < 0.05
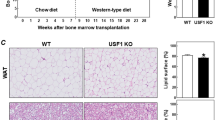
Given that IL-10 treatment prevented the palmitate-induced secretion of TNF-α in macrophages in vitro, we investigated the role of immune-cell-derived IL-10 in the development of high-fat-diet-induced obesity, inflammation and insulin resistance in vivo. To this end, we transplanted lethally irradiated mice as described above. Consistent with previously published reports [8, 34, 35], bone marrow was reconstituted with ~95% efficiency (Fig. 2). While a small amount of endogenous recipient-derived white blood cells remained in the circulation of the transplanted animals, no differences in reconstitution efficiency were observed between mice receiving wild-type or Il10-KO bone marrow (Fig. 2). Additionally, to confirm transplantation efficacy for each animal, whole blood was collected from each transplanted animal at the end of the study (18 weeks) and PCR genotyped for the wild-type or mutant Il10-KO allele. High levels of repopulation with donor white blood cells were observed in all animals (Fig. 2e). Wild-type and global Il10-KO mouse tissue serves here as the positive control (Fig. 2e). It is well established that the BMT technique results in very efficient repopulation of donor myeloid cells not only into the circulation, but into tissues such as the liver and adipose tissue after high-fat feeding [8]. Indeed, it has been demonstrated that most of the F4/80+ cells recruited to white adipose tissue in response to high-fat feeding are bone marrow derived [3]. Thus, the BMT technique is an efficient method to replace both circulating and tissue-resident bone-marrow-derived cells. Notwithstanding this, in the current study we did not determine tissue specific repopulation by donor bone marrow cells. Therefore, while it is likely that the majority of cells recruited to the white adipose tissue in response to high-fat feeding are donor bone marrow derived, we cannot categorically determine this in the current study.
BMT results in successful repopulation of WT and Il10-KO haematopoietic cells in lethally irradiated mice. a–d Male 6-week-old C57BL/6 mice were lethally irradiated, then tail-vein injected with bone marrow from donor wild-type (a, b) or global Il10-KO (c, d) mice. Following 6 weeks’ recovery, bone marrow reconstitution efficiency was measured using congenic donor and recipient mice that differed at the Ly5.1/Ly5.2 leucocyte locus. a, c Whole blood was collected and stained with anti-CD45.1-PE (Ly5.1) antibodies (grey) or isotype controls (black) and analysed by flow cytometry, revealing 5.75% (a) and 6.95% (c) of remnant endogenous leucocytes following transplantation with WT (a) and Il10-KO (c) bone marrow cells, respectively. b, d Whole blood stained with anti-CD45.2-FITC (Ly5.2) antibodies (grey) or isotype controls (black), showing 93.11% (b) and 93.73% (d) of leucocytes are of donor WT (b) or Il10-KO (d) origin, respectively. e Following the end of the dietary period (18 weeks following BMT) whole blood was collected from mice and DNA PCR genotyped for the presence or absence of the wild-type or mutant Il10 allele. Results from two representative mice from each genotype are shown. Wild-type and global Il10-KO tail DNA was used as a positive control. BM, bone marrow; KO, knockout; WT, wild type
Six weeks after recovery from the BMT procedure mice were randomised to chow- or high-fat-diet groups. As expected, mice placed on the high-fat diet accumulated more body fat than those on the chow diet (Fig. 3). No differences in body weight or fat mass were observed between animals receiving wild-type or IL-10 bone marrow (Fig. 3). There was a small but significant genotype–diet interaction for LBM (p < 0.05), with chow-fed Il10-KO BMT mice having less LBM than the chow-fed wild-type BMT mice at the end of the dietary period (Fig. 3). This effect likely reflects the lower lean mass in this group of mice at the commencement of the study. There were no differences in LBM between wild-type BMT and Il10-KO BMT mice on the high-fat diet (Fig. 3). These data demonstrate that deletion of IL-10 within the haematopoietic compartment does not affect fat mass accumulation with either the chow or the high-fat diet.
Il10-KO BMT mice on both chow and high-fat diets have no differences in body weight or fat mass compared with wild-type BMT controls. Mice were routinely weighed and body composition assessed using EcoMRI throughout the entire dietary period. a Change in body weight over time. Circles, chow-fed mice; squares, high-fat-fed mice; white symbols, wild-type BMT mice; black symbols, Il10-KO BMT mice. b Body composition data at the end of week 12. White bars, chow-fed wild-type BMT mice; black bars, chow-fed Il10-KO BMT mice; dark grey bars, high-fat-fed wild-type BMT mice; light grey bars, high-fat-fed Il10-KO BMT mice. Data are means ± SEM. Main effect for diet, *p < 0.05; diet–genotype interaction effect, † p < 0.05. Chow, n = 5–6 mice per genotype; high-fat diet, n = 11–16 per genotype. BW, body weight
In addition to measuring body composition, metabolic data were collected using the CLAMS apparatus (Table 1). There were no differences in food intake, respiratory exchange ratio (RER) or physical activity between Il10-KO BMT and wild-type BMT mice on either the chow or high-fat diet (Table 1). As expected there was a strong dietary effect for RER, in that mice on the high-fat diet had a markedly lower RER, indicating a shift in substrate utilisation that favours the oxidation of fatty acids in preference to carbohydrates. There was both a main effect for diet and genotype with whole-body oxygen uptake (\( \dot{V}{{\hbox{O}}_{{2}}} \)), in that \( \dot{V}{{\hbox{O}}_{{2}}} \) was elevated in response to the high-fat diet and Il10-KO BMT mice had slightly, although significantly, lower \( \dot{V}{{\hbox{O}}_{{2}}} \) compared with wild-type BMT controls (Table 1). The reason for this difference is not clear; however, it is unlikely to be of significant biological importance in the current context as levels of obesity were identical between genotypes.
Following 12 weeks of either the chow or the high-fat diet, plasma insulin and glucose levels were determined following a 6 h fast. As shown in Fig. 4a,b, animals fed a high-fat diet displayed significant hyperinsulinaemia and hyperglycaemia, compared with chow-fed animals. We observed no differences in either fasting basal insulin or glucose when comparing Il10-KO BMT with wild-type BMT animals (Fig. 4a, b). In addition, no differences were observed in 6 h fed and fasted plasma insulin levels (ESM Fig. 1). Animals fed the HF diet for 12 weeks displayed a marked intolerance to both glucose and insulin compared with chow-fed animals (Fig. 4c–e). However, we did not observe any differences when comparing Il10-KO BMT with wild-type BMT mice (Fig. 4c–e). Collectively, these data demonstrate that deletion of IL-10 within the haematopoietic compartment does not exacerbate high-fat-diet-induced insulin resistance.
Il10-KO BMT mice have no differences in glucose homeostasis compared with wild-type BMT controls on both chow and high-fat diets. Data were collected from Il10-KO BMT and wild-type BMT control mice after 12 weeks on chow and high-fat diets. All glucose homeostasis data were recorded after a 6 h fast. Levels of fasting blood glucose (a) and fasting plasma insulin (b); white bars, wild-type BMT mice; black bars, Il10-KO BMT mice. Results from IPGTT glucose 1 g/kg LBM (c) and IPITT insulin 0.6 U/kg LBM for chow-fed (d) and 0.75 U/kg LBM for high-fat-fed (e) animals. Circles, chow-fed mice; squares, high-fat-fed mice; white symbols, wild-type BMT mice; black symbols, Il10-KO BMT mice. Data are means ± SEM. Main effect for diet, *p < 0.05. Chow, n = 5–6 per genotype; high-fat diet, n = 11–16 per genotype
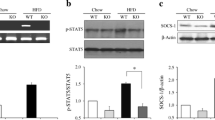
The adipose tissue is a key site of inflammation and macrophage recruitment in obesity and we hypothesised that a lack of the anti-inflammatory cytokine IL-10 within the haematopoietic compartment would exacerbate obesity-induced inflammation. Surprisingly, we did not observe an increase in the phosphorylation status of JNK (Fig. 5a), a key inflammatory kinase linked to the development of insulin resistance. However, we observed an increase in the phosphorylation status of IKKβ and an increase in the mRNA expression of the pro-inflammatory genes Tnf-α and iNos, in high-fat-diet- compared with chow-fed mice (Fig. 5b, c). Furthermore, F4/80 (also known as Emr1) mRNA expression, a marker of macrophage recruitment, and CD11c were elevated in the adipose tissue of high-fat-fed vs chow-fed mice (Fig. 5c). No significant genotype or dietary effects were observed for Il6, Il1β, Ifnγ (also known as Ifng) or Mgl1 (also known as Clec10a) mRNA expression (Fig. 5c). We observed no differences in any of these variables when comparing Il10-KO BMT mice with wild-type BMT mice (Fig. 5a–c). In addition to the adipose tissue, the liver is also an important site of pro-inflammatory events in obesity. However, in contrast with the adipose tissue, we were unable to detect any effect of the high-fat diet on JNK or IKKβ phosphorylation, or on any of the pro-inflammatory cytokine genes, compared with chow-fed mice (Fig. 5d–f). Furthermore, no genotype affect was observed on any of the variables we assessed (Fig. 5d–f). Taken together, these data indicate that while the high-fat diet promoted both an inflammatory response and the recruitment of macrophages to the adipose tissue, this response was not exacerbated by the deletion of immune-cell-derived IL-10.
Il10-KO BMT mice on both chow and high-fat diets have no differences in inflammatory markers in white adipose tissue (a–c) or liver (d–f) compared with wild-type BMT controls. Phosphorylation of JNK (a,d) and IKKβ (b,e) were measured using western blotting and values were expressed over the corresponding total protein values. White bars, wild-type BMT mice; black bars, Il10-KO BMT mice. c,f Cytokine gene expression as measured by RT-PCR. White bars, chow-fed wild-type BMT mice; black bars, chow-fed Il10-KO BMT mice; dark grey bars, high-fat-fed wild-type BMT mice; light grey bars, high-fat-fed Il10-KO BMT mice. Data are means ± SEM. Main effect for diet, *p < 0.05. Chow, n = 5–6 per genotype; high-fat diet, n = 11–16 per genotype. HFD, high-fat diet; P-, phosphorylated; T-, total; WT, wild type
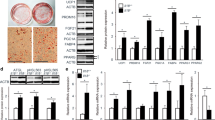
Given the unexpected nature of these results (i.e. we did not observe a potentiation in inflammation in the Il10-KO BMT mice compared with the wild-type BMT mice), we next sought to confirm that macrophages from wild-type and Il10-KO mice were equally able to stimulate pro-inflammatory responses following treatment with various inflammatory stimuli. Accordingly, we performed in vitro experiments using BMDMs harvested from Il10-KO and wild-type mice. LPS-induced increases in the gene expression of Tnf-α, Il6 and Il1β (Fig. 6a) as well as phosphorylation of IKKβ (Fig. 6c) and JNK (Fig. 6d) and the release of TNF-α (ESM Fig. 2a) were nearly identical between Il10-KO and wild-type BMDMs. As expected, LPS treatment increased Il10 mRNA expression and IL-10 release into the media in wild-type but not Il10-KO BMDMs (Fig. 6a, ESM Fig. 2b). Next we stimulated these cells with IL-4, which is known to polarise macrophages towards an ‘M2’ phenotype. IL-4 treatment increased Arg1 mRNA expression to similar levels in Il10-KO and wild-type BMDMs (Fig. 6b). Finally, in an attempt to mimic the action of the high-fat diet in vivo, we stimulated BMDMs with the long-chain saturated fatty acid palmitate. Palmitate treatment increased both the phosphorylation of JNK (Fig. 6e) and TNF-α release into the media (ESM Fig. 2c), but consistent with results observed for LPS stimulation, no differences were observed when comparing Il10-KO and wild-type BMDMs (Fig. 6e, ESM Fig. 2c).
BMDMs from wild-type and global Il10-KO mice have the same responses to inflammatory and immunomodulatory stimuli. a Cytokine gene expression as measured by RT-PCR from wild-type and Il10-KO BMDMs stimulated for 6 h with LPS (100 ng/ml). b Arg1 expression in wild-type and Il10-KO BMDMs stimulated for 6 h with IL-4 (20 ng/ml). a,b White bars, wild-type control; black bars, Il10-KO control; dark grey bars, wild-type LPS (a) or IL-4 (b); light grey bars, Il10-KO LPS (a) or IL-4 (b). c, d Phosphorylation of IKKβ and JNK in response to 30 min LPS (100 ng/ml) stimulation in BMDMs from wild-type and Il10-KO mice. e Phosphorylation of JNK in response to 4 h of 0.5 mmol/l palmitate treatment. Phosphorylation was measured by western blotting and values were expressed over the corresponding total protein values. Results are from three independent experiments performed in triplicate. Data are means ± SEM. Main effect for genotype, *p < 0.05. Con, control; P-, phosphorylated; Pal, palmitate treated; T-, total; WT, wild type
Unexpectedly, Il10 mRNA expression in the adipose tissue and liver of animals receiving Il10-KO bone marrow was significantly elevated compared with animals receiving wild-type bone marrow (Fig. 7a, b). However, plasma IL-10 levels were not different between wild-type BMT and Il10-KO BMT mice, and were unaffected by diet (Fig. 7c). To explore this unexpected finding in more detail we examined IL-10 protein production in adipose tissue by immunohistochemistry. IL-10 production (as indicated by brown staining) in the adipose tissue was markedly more abundant in the sections obtained from Il10-KO BMT adipose tissue compared with wild-type BMT adipose tissue (Fig. 8). The specificity of the IL-10 staining was confirmed using adipose tissue from global Il10-KO mice (ESM Fig. 3).
Il10-KO BMT mice have increased Il10 gene expression in white adipose tissue and liver compared with wild-type BMT controls, yet have unaltered plasma IL-10 levels. Il10 gene expression in white adipose tissue (a) and liver (b) as measured by RT-PCR. c Plasma IL-10 levels as measured by ELISA. Data are means ± SEM. Main effect for genotype, *p < 0.05; high-fat diet lower than chow-fed group, diet × genotype interaction effect, † p < 0.05. White, wild-type BMT mice; black, Il10-KO BMT mice. Chow, n = 5–6 per genotype; high-fat diet, n = 11–16 per genotype. HFD, high-fat diet
IL-10 protein production is higher in the white adipose tissue of Il10-KO BMT mice compared with wild-type BMT mice. Immunohistochemical staining for IL-10 in white adipose tissue sections from wild-type BMT and Il10-KO BMT mice from both chow-fed and high-fat-fed groups. Images shown are from three different animals from each genotype and dietary group (12 mice in total). The IL-10 protein is stained in brown. All images were taken with × 20 magnification. HFD, high-fat diet
Discussion
To address the role IL-10 derived from bone marrow cells (haematopoietic) plays in high-fat-diet-induced obesity, metabolic tissue inflammation and insulin resistance, we have used an adoptive transfer model whereby we transplanted bone marrow from global Il10-KO or wild-type control mice into lethally irradiated wild-type C57BL/6 recipient mice, thus creating chimeras that can produce IL-10 in all cells except those that are derived from the haematopoietic (immune cell) compartment. We hypothesised that deletion of IL-10 from the immune cell compartment would exacerbate high-fat-diet-induced inflammation in key metabolic tissues and, therefore, lead to a potentiation of high-fat-diet-induced insulin resistance. Unexpectedly, however, IL-10 deletion did not potentiate high-fat-diet-induced adipose tissue or liver inflammation, nor did it affect the severity of high-fat-diet-induced insulin resistance, suggesting endogenous immune-cell-derived IL-10 may not play a critical role in maintaining metabolic homeostasis in vivo.
In the present study we used a high-fat diet which contained 42% of energy from fat. This 12 week dietary intervention resulted in marked obesity, insulin resistance and inflammation as evidenced by the significant increases in Tnf-α, iNos, F4/80 and Cd11c (also known as Itgax) mRNA expression and IKKβ phosphorylation in adipose tissue. The degree of obesity (~40 g body weight on high-fat diet) and white adipose tissue inflammation (Tnf-α, iNos, F4/80, Cd11c gene induction) in this study was remarkably similar to that seen in other studies using BMT mice, even under conditions of longer-term high-fat-diet feeding (16–20 weeks) using the diet in which 60% of energy is from fat [8, 9, 36], thus demonstrating the effectiveness of the type of high-fat diet used and the duration of the feeding protocol. Despite the high-fat-diet-induced inflammation and insulin resistance, deletion of IL-10 from the immune cells did not exacerbate this pro-inflammatory phenotype. In contrast to many inflammatory diseases, the levels of inflammation observed in obesity are relatively low. It is possible that these relatively modest pro-inflammatory changes may not stimulate a potent counteractive anti-inflammatory response that requires the immune cells to upregulate IL-10 production. Consistent with this notion, Il10 mRNA expression was not altered in wild-type BMT mice following the high-fat diet compared with chow-fed animals. Indeed, previous studies have reported variable effects of obesity on Il10 expression [3, 4, 9, 37]. Furthermore, and in support of the idea that a high-fat diet may not upregulate a potent anti-inflammatory response, while classic pro-inflammatory stimuli such as LPS upregulate the production of both pro- and anti-inflammatory cytokines, macrophages treated with the saturated fatty acid palmitate do not secrete IL-10; however, they induce a strong pro-inflammatory response characterised by heightened TNF-α and IL-6 secretion [28]. Collectively, these data suggest that in conditions of obesity and lipid oversupply, IL-10 does not play an important anti-inflammatory role. If obesity does not stimulate an anti-inflammatory response, including the production of IL-10, then the deletion of IL-10 from the immune cell compartment would not be expected to exacerbate obesity-induced inflammation and insulin resistance, as we observed in the current study. However, in inflammatory diseases such as colitis, psoriasis, hepatitis C and rheumatoid arthritis, which induce both strong pro- and anti-inflammatory responses, IL-10 does play an important positive role in disease outcome [38].
Previous studies have demonstrated that the provision of IL-10, either via administration of recombinant IL-10 or via transgenic overexpression of Il10, ameliorates insulin resistance [11, 25]. Indeed, our own in vitro experiments demonstrate that the addition of IL-10 to palmitate-treated macrophages prevents TNF-α production and release. Thus, while experimentally increasing IL-10 levels improves insulin sensitivity, most likely via an attenuation of pro-inflammatory processes [25], because high-fat feeding in our hands does not change IL-10 production, then the deletion of endogenous IL-10 has little effect on the level of inflammation present in the tissues and, ultimately, whole-body insulin sensitivity.
An unexpected finding of the current study was the elevated Il10 mRNA expression and IL-10 protein production in key metabolic tissues (e.g. the adipose tissue and liver) in the Il10-KO BMT mice compared with the wild-type BMT mice. While the mechanism for this effect is not clear, the data suggest that the deletion of IL-10 within immune cells promotes a compensatory increase in IL-10 production. While we are unable to precisely determine the cellular origin of this increase, it was apparent from the immunohistochemical analyses that much of the staining appeared at the junctions between adipocytes, with a pattern of lower production within the adipocytes. Although speculative, these data suggest that the compensatory IL-10 production in the Il10-KO BMT mice may have originated from the vasculature and/or the adipocytes themselves. Importantly, however, any potential effect of this increase is likely to be constrained to the local tissue environment as plasma IL-10 levels were unaltered between Il10-KO BMT and wild-type BMT mice. It is possible that this compensatory increase in IL-10 production in the liver and adipose tissue may have suppressed pro-inflammatory responses within these tissues and, therefore, masked the effect of the deletion of IL-10 within the immune cell compartment. With regards to the cellular source contributing to the increased IL-10 production in the Il10-KO BMT mice, the BMT technique not only largely repopulates the recipient’s monocytes/macrophages with those of the donor, but also the resident liver Kupffer cells [8, 18], which are likely potential sources of liver-derived IL-10 production [29]. In addition, the BMT repopulates other bone-marrow-derived leucocytes, including lymphocytes, which are potent IL-10 producers and have also been shown to infiltrate adipose tissue and are implicated in adipose tissue inflammation and insulin resistance [39–47].
It is worth noting that, similarly to the global Il10-KO mice that develop chronic enterocolitis [21, 22], a proportion (7/18) of our Il10-KO BMT mice developed mild colitis-like symptoms including loss of total body weight, loss of LBM, a failure to put on total body and fat mass with a high-fat diet, loose stools and a generally dehydrated and poor appearance. These symptoms were not observed in any of the wild-type BMT mice. These observations are consistent with several previous studies that implicate IL-10 production by lymphoid or myeloid cells in the prevention of inflammation of the large intestine and, ultimately, the development of colitis [48–50]. Given that these mice (7/18 Il10-KO BMT mice) displayed a variety of colitis-like symptoms and did not increase their fat mass during the 12 week high-fat-diet period, we excluded these mice from the study.
In summary, the results of the present study demonstrate that the deletion of IL-10 within the immune cell compartment does not exacerbate obesity-induced inflammation and insulin resistance. We hypothesise that this is due to the lack of an effect of high-fat feeding in stimulating endogenous anti-inflammatory IL-10 production, and hence deletion of IL-10 has little effect. However, our in vitro data, and results from in vivo studies of others, suggest that increasing IL-10 levels through transgenic overexpression or administration of recombinant IL-10 decreases inflammation and improves insulin sensitivity.
Abbreviations
- AMREP:
-
Alfred Medical Research and Education Precinct
- ATM:
-
Adipose tissue macrophage
- BMDM:
-
Bone-marrow-derived macrophage
- BMT:
-
Bone marrow transplant
- CLAMS:
-
Comprehensive Laboratory Animal Monitoring System
- IKKβ:
-
Inhibitor of kappa kinase β
- IPGTT:
-
Intraperitoneal glucose tolerance test
- IPITT:
-
Intraperitoneal insulin tolerance test
- JNK:
-
c-Jun N-terminal kinase
- LBM:
-
Lean body mass
- LPS:
-
Lipopolysaccharide
- MGL1:
-
Macrophage galactose N-acetyl-galactosamine-specific lectin 1
- PPAR:
-
Peroxisome proliferator-activated receptor
- RER:
-
Respiratory exchange ratio
- \( \dot{V}{{\hbox{O}}_{{2}}} \) :
-
Whole-body oxygen uptake
References
Olefsky JM, Glass CK (2010) Macrophages, inflammation, and insulin resistance. Annu Rev Physiol 72:219–246
Hotamisligil GS, Shargill NS, Spiegelman BM (1993) Adipose expression of tumor necrosis factor-alpha: direct role in obesity-linked insulin resistance. Science 259:87–91
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante AW Jr (2003) Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest 112:1796–1808
Xu H, Barnes GT, Yang Q et al (2003) Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 112:1821–1830
Arkan MC, Hevener AL, Greten FR et al (2005) IKK-beta links inflammation to obesity-induced insulin resistance. Nat Med 11:191–198
Yuan M, Konstantopoulos N, Lee J et al (2001) Reversal of obesity- and diet-induced insulin resistance with salicylates or targeted disruption of Ikkbeta. Science 293:1673–1677
Hirosumi J, Tuncman G, Chang L et al (2002) A central role for JNK in obesity and insulin resistance. Nature 420:333–336
Solinas G, Vilcu C, Neels JG et al (2007) JNK1 in hematopoietically derived cells contributes to diet-induced inflammation and insulin resistance without affecting obesity. Cell Metab 6:386–397
Patsouris D, Li PP, Thapar D, Chapman J, Olefsky JM, Neels JG (2008) Ablation of CD11c-positive cells normalizes insulin sensitivity in obese insulin resistant animals. Cell Metab 8:301–309
Gordon S (2007) Macrophage heterogeneity and tissue lipids. J Clin Invest 117:89–93
Lumeng CN, Bodzin JL, Saltiel AR (2007) Obesity induces a phenotypic switch in adipose tissue macrophage polarization. J Clin Invest 117:175–184
Lumeng CN, DelProposto JB, Westcott DJ, Saltiel AR (2008) Phenotypic switching of adipose tissue macrophages with obesity is generated by spatiotemporal differences in macrophage subtypes. Diabetes 57:3239–3246
Lumeng CN, Deyoung SM, Bodzin JL, Saltiel AR (2007) Increased inflammatory properties of adipose tissue macrophages recruited during diet-induced obesity. Diabetes 56:16–23
Nguyen MT, Favelyukis S, Nguyen AK et al (2007) A subpopulation of macrophages infiltrates hypertrophic adipose tissue and is activated by free fatty acids via Toll-like receptors 2 and 4 and JNK-dependent pathways. J Biol Chem 282:35279–35292
Shaul ME, Bennett G, Strissel KJ, Greenberg AS, Obin MS (2010) Dynamic, M2-like remodeling phenotypes of CD11c + adipose tissue macrophages during high fat diet-induced obesity in mice. Diabetes 59:1171–1181
Stienstra R, Duval C, Keshtkar S, van der Laak J, Kersten S, Muller M (2008) Peroxisome proliferator-activated receptor gamma activation promotes infiltration of alternatively activated macrophages into adipose tissue. J Biol Chem 283:22620–22627
Odegaard JI, Ricardo-Gonzalez RR, Goforth MH et al (2007) Macrophage-specific PPARgamma controls alternative activation and improves insulin resistance. Nature 447:1116–1120
Odegaard JI, Ricardo-Gonzalez RR, Red Eagle A et al (2008) Alternative M2 activation of Kupffer cells by PPARdelta ameliorates obesity-induced insulin resistance. Cell Metab 7:496–507
Gordon S (2003) Alternative activation of macrophages. Nat Rev Immunol 3:23–35
Saraiva M, O'Garra A (2010) The regulation of IL-10 production by immune cells. Nat Rev Immunol 10:170–181
Kuhn R, Lohler J, Rennick D, Rajewsky K, Muller W (1993) Interleukin-10-deficient mice develop chronic enterocolitis. Cell 75:263–274
Rennick D, Davidson N, Berg D (1995) Interleukin-10 gene knock-out mice: a model of chronic inflammation. Clin Immunol Immunopathol 76:S174–S178
Spencer SD, Di Marco F, Hooley J et al (1998) The orphan receptor CRF2-4 is an essential subunit of the interleukin 10 receptor. J Exp Med 187:571–578
Cintra DE, Pauli JR, Araujo EP et al (2008) Interleukin-10 is a protective factor against diet-induced insulin resistance in liver. J Hepatol 48:628–637
Hong EG, Ko HJ, Cho YR et al (2009) Interleukin-10 prevents diet-induced insulin resistance by attenuating macrophage and cytokine response in skeletal muscle. Diabetes 58:2525–2535
Kim HJ, Higashimori T, Park SY et al (2004) Differential effects of interleukin-6 and -10 on skeletal muscle and liver insulin action in vivo. Diabetes 53:1060–1067
Morari J, Torsoni AS, Anhe GF et al (2009) The role of proliferator-activated receptor gamma coactivator-1alpha in the fatty-acid-dependent transcriptional control of interleukin-10 in hepatic cells of rodents. Metabolism 59:215–223
Samokhvalov V, Bilan PJ, Schertzer JD, Antonescu CN, Klip A (2009) Palmitate- and lipopolysaccharide-activated macrophages evoke contrasting insulin responses in muscle cells. Am J Physiol Endocrinol Metab 296:E37–E46
Clementi AH, Gaudy AM, van Rooijen N, Pierce RH, Mooney RA (2009) Loss of Kupffer cells in diet-induced obesity is associated with increased hepatic steatosis, STAT3 signaling, and further decreases in insulin signaling. Biochim Biophys Acta 1792:1062–1072
den Boer MA, Voshol PJ, Schroder-van der Elst JP et al (2006) Endogenous interleukin-10 protects against hepatic steatosis but does not improve insulin sensitivity during high-fat feeding in mice. Endocrinology 147:4553–4558
Cancello R, Henegar C, Viguerie N et al (2005) Reduction of macrophage infiltration and chemoattractant gene expression changes in white adipose tissue of morbidly obese subjects after surgery-induced weight loss. Diabetes 54:2277–2286
Clement K, Viguerie N, Poitou C et al (2004) Weight loss regulates inflammation-related genes in white adipose tissue of obese subjects. FASEB J 18:1657–1669
Shi H, Kokoeva MV, Inouye K, Tzameli I, Yin H, Flier JS (2006) TLR4 links innate immunity and fatty acid-induced insulin resistance. J Clin Invest 116:3015–3025
Janowska-Wieczorek A, Majka M, Kijowski J et al (2001) Platelet-derived microparticles bind to hematopoietic stem/progenitor cells and enhance their engraftment. Blood 98:3143–3149
Senftleben U, Li ZW, Baud V, Karin M (2001) IKKbeta is essential for protecting T cells from TNFalpha-induced apoptosis. Immunity 14:217–230
Saberi M, Woods NB, de Luca C et al (2009) Hematopoietic cell-specific deletion of toll-like receptor 4 ameliorates hepatic and adipose tissue insulin resistance in high-fat-fed mice. Cell Metab 10:419–429
Li P, Lu M, Nguyen MT et al (2010) Functional heterogeneity of CD11C positive adipose tissue macrophages in diet-induced obese mice. J Biol Chem 285(20):15333–15345
Mocellin S, Panelli MC, Wang E, Nagorsen D, Marincola FM (2003) The dual role of IL-10. Trends Immunol 24:36–43
Wu H, Ghosh S, Perrard XD et al (2007) T cell accumulation and regulated on activation, normal T cell expressed and secreted upregulation in adipose tissue in obesity. Circulation 115:1029–1038
Kintscher U, Hartge M, Hess K et al (2008) T-lymphocyte infiltration in visceral adipose tissue: a primary event in adipose tissue inflammation and the development of obesity-mediated insulin resistance. Arterioscler Thromb Vasc Biol 28:1304–1310
Rausch ME, Weisberg S, Vardhana P, Tortoriello DV (2008) Obesity in C57BL/6 J mice is characterized by adipose tissue hypoxia and cytotoxic T cell infiltration. Int J Obes (Lond) 32:451–463
Duffaut C, Galitzky J, Lafontan M, Bouloumie A (2009) Unexpected trafficking of immune cells within the adipose tissue during the onset of obesity. Biochem Biophys Res Commun 384:482–485
Rocha VZ, Folco EJ, Sukhova G et al (2008) Interferon-gamma, a Th1 cytokine, regulates fat inflammation: a role for adaptive immunity in obesity. Circ Res 103:467–476
Feuerer M, Herrero L, Cipolletta D et al (2009) Lean, but not obese, fat is enriched for a unique population of regulatory T cells that affect metabolic parameters. Nat Med 15:930–939
Liu J, Divoux A, Sun J et al (2009) Genetic deficiency and pharmacological stabilization of mast cells reduce diet-induced obesity and diabetes in mice. Nat Med 15:940–945
Nishimura S, Manabe I, Nagasaki M et al (2009) CD8+ effector T cells contribute to macrophage recruitment and adipose tissue inflammation in obesity. Nat Med 15:914–920
Winer S, Chan Y, Paltser G et al (2009) Normalization of obesity-associated insulin resistance through immunotherapy. Nat Med 15:921–929
Murai M, Turovskaya O, Kim G et al (2009) Interleukin 10 acts on regulatory T cells to maintain expression of the transcription factor Foxp3 and suppressive function in mice with colitis. Nat Immunol 10:1178–1184
Roers A, Siewe L, Strittmatter E et al (2004) T cell-specific inactivation of the interleukin 10 gene in mice results in enhanced T cell responses but normal innate responses to lipopolysaccharide or skin irritation. J Exp Med 200:1289–1297
Rubtsov YP, Rasmussen JP, Chi EY et al (2008) Regulatory T cell-derived interleukin-10 limits inflammation at environmental interfaces. Immunity 28:546–558
Acknowledgements
We acknowledge the technical support provided by A. Selathurai and T. Soe Kyaw. This study was supported by grants from the Diabetes Australia Research Trust (to G. I. Lancaster) and the National Health and Research Council of Australia (NHMRC Project Grant No. 526619; to M. A. Febbraio and G. I. Lancaster). C. R. Bruce is an NHMRC Career Development Fellow. A. Bobik and M. A. Febbraio are NHMRC Principal Research Fellows.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
Test (PDF 104 kb)
ESM Fig. 1
Il10-KO BMT and wild-type BMT mice on a high-fat diet have comparable fed and 6 h fasting plasma insulin concentrations. Plasma insulin levels as measured by ELISA after 4 weeks on the high-fat diet. n = 9–12 per genotype. White bars, fed state; black bars, fasted state (PDF 16 kb)
ESM Fig. 2
BMDMs from wild-type and Il10-KO mice secrete similar amounts of TNF-α protein in response to LPS and palmitate treatment. a–cBMDMs from wild-type and Il10-KO mice stimulated with LPS (100 ng/ml) for 24 h (a, b) or 0.75 mmol/l palmitate for 6 h (c). a, bSecretion of TNF-α (a) and IL-10 (b) into the media supernatant fraction; IL-10 secretion was not detected in Il10-KO BMDMs under basal and stimulated conditions. cTNF-α secretion in response to palmitate; control media contained 2% BSA (vehicle). Data are means ± SEM. Main effect for genotype, *p < 0.05 (PDF 53 kb)
ESM Fig. 3
IL-10 immunohistochemistry negative control section images.Immunohistochemistry performed on white adipose tissue sections from global Il10-KO and Il10-KO BMT chow-fed mice. No brown IL-10 protein staining is visible in the global Il10-KO section. Negative staining (no IL-10 antibody treatment) in the Il10-KO BMT section also reveals no non-specific staining, indicating the hydrogen peroxide blocking protocol was successful (PDF 81 kb)
Rights and permissions
About this article
Cite this article
Kowalski, G.M., Nicholls, H.T., Risis, S. et al. Deficiency of haematopoietic-cell-derived IL-10 does not exacerbate high-fat-diet-induced inflammation or insulin resistance in mice. Diabetologia 54, 888–899 (2011). https://doi.org/10.1007/s00125-010-2020-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-010-2020-5