Abstract
Aims/hypothesis
Cellular cholesterol accumulation is an emerging mechanism for beta cell dysfunction in type 2 diabetes. Absence of the cholesterol transporter ATP-binding cassette transporter A1 (ABCA1) results in increased islet cholesterol and impaired insulin secretion, indicating that impaired cholesterol efflux leads to beta cell dysfunction. In this study, we aimed to determine the role of the LDL receptor (LDLr) in islet cholesterol uptake and to assess the contributions of cholesterol uptake compared with efflux to islet cholesterol levels.
Methods
Islet cholesterol and beta cell function were assessed in mice lacking LDLr (Ldlr −/−), or apolipoprotein E (Apoe −/−), as well as in mice with beta-cell-specific deficiency of Abca1 crossed to Ldlr −/− mice.
Results
Hypercholesterolaemia resulted in increased islet cholesterol levels and decreased beta cell function in Apoe −/− mice but not in Ldlr −/− mice, suggesting that the LDL receptor is required for cholesterol uptake leading to cholesterol-induced beta cell dysfunction. Interestingly, when wild-type islets with functional LDL receptors were transplanted into diabetic, hypercholesterolaemic mice, islet graft function was normal compared with Ldlr −/− islets, suggesting that compensatory mechanisms can maintain islet cholesterol homeostasis in a hypercholesterolaemic environment. Indeed, transplanted wild-type islets had increased Abca1 expression. However, lack of the Ldlr did not protect Abca1 −/− mice from islet cholesterol accumulation, suggesting that cholesterol efflux is the critical regulator of cholesterol levels in islets.
Conclusions/interpretation
Our data indicate that islet cholesterol levels and beta cell function are strongly influenced by LDLr-mediated uptake of cholesterol into beta cells. Cholesterol efflux mediated by ABCA1, however, can compensate in hypercholesterolaemia to regulate islet cholesterol levels in vivo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 2 diabetes is a significant risk factor for cardiovascular disease and occurs when beta cells are unable to secrete sufficient insulin to meet the increasing metabolic requirements associated with insulin resistance and obesity. Loss of first-phase glucose-stimulated insulin secretion has long been recognised as an invariant finding among individuals with type 2 diabetes [1], and the critical role of beta cell dysfunction in the pathogenesis of type 2 diabetes is well recognised. The reasons for beta cell dysfunction in type 2 diabetes are not completely understood. Data from several sources suggest that intracellular cholesterol levels may influence beta cell function [2–5].
We recently established a novel role for the ATP-binding cassette transporter A1 (ABCA1), a cellular cholesterol transporter, in beta cell cholesterol homeostasis and insulin secretion [2]. Mice with specific inactivation of Abca1 in beta cells showed marked impairment of glucose tolerance and defective insulin secretion. Mice lacking Abca1 globally, however, had more modest impairments in glucose tolerance and beta cell function. Analysis of islet cholesterol levels revealed that whereas islet cholesterol levels in total Abca1 −/− mice were normal, beta-cell-specific Abca1 knockout mice showed increased levels of islet cholesterol associated with beta cell dysfunction. One potential explanation for this difference is that mice with global Abca1 deficiency have a 90% reduction in plasma cholesterol levels, whereas mice with beta-cell-specific Abca1 deficiency have normal plasma cholesterol levels. Thus, beta cells lacking Abca1 appear to be susceptible to dysfunction in vivo only in the presence of sufficient levels of plasma cholesterol. These findings imply that cholesterol uptake into beta cells from plasma can contribute to cholesterol-induced beta cell dysfunction.
Uptake of cholesterol from the plasma is mediated through lipoprotein receptors and scavenger receptors. The mechanisms responsible for cholesterol uptake into beta cells are, however, not well defined. Several lipoprotein receptors, such as the VLDL receptor, LDL receptor (LDLr), LDL-related protein (LRP), scavenger receptor B1 (SRB1) and CD36 are produced in islets [6, 7]. In addition, VLDL, LDL and HDL are taken up in vitro and atherogenic lipoproteins such as LDL and VLDL induce apoptotic death in isolated islets and transformed beta cell lines [6, 8, 9]. Furthermore, addition of LDL to cultured islets at physiological concentrations decreases glucose-stimulated insulin secretion and beta cell proliferation [5]. Interestingly, this seems to be dependent on the presence of the LDLr [5], suggesting a major role for the LDLr in LDL uptake and cholesterol-induced beta cell dysfunction. The relevance of these studies in vivo, however, remains unclear.
The aim of this study was to determine the role of the LDL receptor in islet cholesterol homeostasis and to assess the relative contributions of cholesterol uptake compared with efflux in maintenance of intracellular cholesterol and function of beta cells in vivo.
Methods
Animals
Male wild-type C57Bl/6 mice, Ldlr −/− mice and Apoe −/− mice were obtained from the Jackson Laboratory (Bar Harbor, ME, USA). Mice received standard laboratory chow diet (LabDiet 5010 Autoclavable Rodent Diet: PMI Nutrition International, Richmond, IN, USA) or Western type diet (TD.88137, Harlan Teklad, WI, USA) for 1 month. Ldlr −/− mice were crossed to beta-cell-specific Abca1 knockout mice (Abca1 −P/−P) [2] to generate Abca1 −P/−P;Ldlr −/−, Abca1 fl/fl;Ldlr −/−. All studies were performed on 4-month-old male mice, except for mice used in the islet transplantation experiments described below. All mice were on a pure C57Bl6 background. All studies were approved by the University of British Columbia Animal Care Committee.
Islet isolation
Primary islets were isolated by collagenase (Sigma-Aldrich, Oakville, ON, Canada) digestion and filtration as previously described [10]. Islets used for cholesterol measurement, western blotting or real-time PCR were washed with PBS and frozen down immediately after isolation. Islets used for 1,1′-dioctadecyl-3,3,3′,3′-tetramethyl-indocarbocyanine perchlorate (DiI)-LDL uptake experiments, glucose-stimulated insulin secretion measurement and islet transplantation studies were incubated in RPMI with 10% FBS and 1% penicillin/streptomycin (Invitrogen Canada, Burlington, ON, Canada) overnight and experiments were performed the following day. Islets used for the mevastatin experiments were cultured for an additional 48 h in RPMI containing 200 µmol/l mevalonate, 10% delipidated FCS (Sigma-Aldrich) and 1% penicillin/streptomycin with or without 10 µmol/l mevastatin (Sigma-Aldrich).
Cell culture
Mouse insulinoma (MIN6) cells were cultured in DMEM containing 25 mmol/l glucose with 10% FBS and 1% penicillin/streptomycin. Cells were treated for 48 h with normal media, serum-free medium with 2% BSA, serum-free medium with 2% BSA and 50 µg/ml LDL (BTI, Stoughton, MA, USA) or serum-free medium with 2% BSA and 10 µmol/l mevastatin, after which cells were harvested for RNA isolation.
Islet transplantation study
Donor islets were isolated from 10-week-old C57Bl/6, Ldlr −/−, Abca1 +/+ and Abca1 +/−P mice and incubated in RPMI (11 mmol/l glucose) with 10% FBS and 1% penicillin/streptomycin overnight. The islets were washed, hand counted into aliquots of 200 islets and transplanted into the left renal subcapsular space of 10-week-old Ldlr −/− mice under isoflurane anaesthesia as previously described [11]. Recipient mice were previously rendered hyperglycaemic (blood glucose >25 mmol/l) by single intraperitoneal injection of streptozotocin (STZ) in citrate buffer. Recipient mice were transplanted 5 days after STZ injection. To obtain hypercholesterolaemia, mice were put on a Western type diet (WTD) as indicated. Glucose tolerance was performed after transplantation as described previously [2]. Fed glucose levels were measured daily for the first 14 days and twice a week thereafter. Nephrectomy of the graft-bearing kidney was performed after transplantation on all recipients to ensure that normoglycaemia was graft dependent. Islet grafts including kidney were embedded in Tissue-Tek OCT medium (VWR) and flash-frozen using isopentane and stored at −80°C. Before microdissection, 10 µm sections were cut, fixed in 100% ethanol for 30 s and stained with haematoxylin, followed by dehydration steps in 70, 95 and 100% ethanol. Once air-dried, islet grafts were microdissected using the Leica Laser Microdissection System.
Insulin secretion assay
Insulin secretion in vitro was performed on hand-picked islets. After isolation, islets were cultured overnight in RPMI containing 10% FBS and 1% penicillin/streptomycin, plated at 20 islets per well in KRB-BSA containing 1.67 mmol/l glucose for 2 h, then incubated with buffer containing 1.67 mmol/l glucose or 16.7 mmol/l glucose. After 1 h media was removed and islets lysed in 1 mol/l glacial acetic acid, and insulin levels were determined by ELISA (Mercodia Inc., Winston-Salem, NC, USA). Insulin secretion was expressed as a percentage of islet insulin content and is normalised to basal levels to allow comparison between multiple experiments.
Cholesterol measurements
Plasma cholesterol levels were determined using commercially available reagents (Wako Diagnostics, Richmond, VA, USA). For the islet cholesterol measurements, neutral sterols were isolated from 100 hand-picked islets according to Bligh and Dyer [12]. Cholesterol was then measured using the Amplex Red Cholesterol Assay Kit (Invitrogen Canada). Islet protein levels were measured by the Bradford method [13].
Lipoparticle uptake experiments
After overnight culture, islets were incubated with RPMI plus 0.5% BSA for 4 h, after which islets were incubated with DiI-LDL (10 µg/ml) (Invitrogen Canada) or DiI-VLDL (10 µg/ml; BTI) for 2 h. Islets were washed, fixed in 4% paraformaldehyde and embedded into 2% agarose, after which cryostat sections were cut. Sections were immunostained for insulin to identify beta cells as previously described [2].
Western analysis and real-time PCR
Western blotting was performed as previously described [2]. Briefly, tissues were homogenised in 20 mmol/l HEPES, 5 mmol/l KCl, 5 mmol/l MgCl2, 0.5% (vol./vol.) Triton X-100 and complete protease inhibitor (Roche Diagnostics, Laval, QC, Canada). Protein concentration was determined by the Bradford method [13]. Equivalent amounts of total protein (30 µg) were separated by SDS-PAGE, transferred to polyvinylidene difluoride membranes and probed with antibodies to ABCA1 [14], LDLr (R&D Systems, Minneapolis, MN, USA), or to actin (Millipore, Billerica, MA, USA). Protein bands were analysed by densitometry using Quantity One quantification analysis software.
Real-time PCR was performed as described [2]. Briefly, total RNA from isolated islets, islet grafts or MIN6 cells were extracted using the RNeasy Micro Kit (Qiagen, Mississauga, ON, Canada) and reverse-transcribed DNase-treated RNA using Superscript II (Invitrogen). RNase-treated cDNA was used for real-time PCR using SYBR Green PCR Master Mix (Applied Biosystems, Foster City, CA, USA). Gapdh and β-actin were used as invariant control.
Statistical analysis
Data are presented as means plus or minus standard error. Differences between groups were calculated by Student’s t test (for two groups) or one-way ANOVA with the Neuman–Keuls post test (for three or more groups) with a p value of 0.05 considered significant.
Results
Expression of the LDL receptor in islets is influenced by plasma LDL-cholesterol levels
Islets express high amounts of Ldlr mRNA (Fig. 1a) and protein (Fig. 1b), at levels similar to those in liver. To determine how LDLr is regulated in beta cells, we used the transformed beta cell line MIN6. Serum starvation for 48 h resulted in increased expression of Ldlr mRNA, whereas addition of LDL (50 µg/ml) resulted in a downregulation of Ldlr expression. Blockade of cholesterol synthesis using mevastatin further increased Ldlr expression (Fig. 1c), showing that beta cell Ldlr expression is regulated in a similar manner to Ldlr in the liver [15]. To determine whether these results can be extrapolated to islets in vivo, we examined Ldlr mRNA amounts in islets isolated from mice fed a chow or a WTD for 1 month. In agreement with the in vitro data, WTD feeding resulted in decreased Ldlr expression in islets (Fig. 1d). These results indicate specific and direct regulation of islet cell LDL receptor by LDL-cholesterol levels.
The LDLr is highly expressed in islet cells and regulated by serum LDL-cholesterol levels. a Relative Ldlr mRNA levels in liver and islet samples isolated from C57Bl/6 mice (n = 5). b Relative LDL receptor protein levels in liver and islet samples isolated from C57Bl/6 mice (n = 3). c Relative Ldlr mRNA levels in MIN6 cells cultured in medium containing 10% FBS and serum-free medium with 50 µg/ml LDL or 10 µmol/l mevastatin for 48 h (n = 3). d Relative Ldlr mRNA amounts in islets isolated from C57Bl6/J mice fed a chow or WTD for 1 month (n = 5–9 per group). All data were standardised for β-actin mRNA or protein levels. Values represent means ± SEM. *p < 0.05, **p < 0.01, ***p < 0.001 compared with 10% FBS (c) or chow islets (d). † p < 0.001 compared with serum-free medium
The relationship between plasma and islet cell cholesterol levels
To investigate whether LDLr mediates islet cholesterol uptake in vivo, we compared islet cholesterol levels in mice lacking the Ldlr (Ldlr −/− mice) to those in wild-type and hypercholesterolaemic Apoe −/− mice. Both Ldlr −/− mice and Apoe −/− mice had increased plasma cholesterol levels compared with C57Bl/6 control mice (Fig. 2a). The Apoe −/− mice, however, showed increased plasma cholesterol levels compared with Ldlr −/− mice (Fig. 2a). Lack of ApoE affects uptake of chylomicron remnants and VLDL, whereas LDL uptake is unaffected in liver cells [16, 17]. Lack of LDLr results in a marked impairment in uptake of LDL as well as partially impaired uptake of chylomicron remnants and VLDL in liver cells [18]. Islet cholesterol levels were increased only modestly in Apoe −/− mice and unchanged in Ldlr −/− mice (Fig. 2b). To increase plasma cholesterol levels, mice were fed a WTD for 1 month. As expected, plasma cholesterol was significantly increased in both Ldlr −/− and Apoe −/− mice, compared with C57Bl/6 control mice (Fig. 2c). Despite similar high plasma cholesterol levels in Ldlr −/− and Apoe −/− mice, islet cholesterol levels were increased only in Apoe −/− mice (11.2±2.8 µg/mg protein in control vs 19.2±4.4 µg/mg protein in Apoe −/− islets, p < 0.001; Fig. 2d).
Increased plasma cholesterol levels leads to increased islet cholesterol levels in Apoe −/− mice, but not in Ldlr −/− mice. Plasma cholesterol levels (a) and islet cholesterol levels (b) in chow-fed C57Bl6 control, Ldlr −/− and Apoe −/− mice (n = 7–10 per group). Plasma (c) and islet cholesterol (d) levels in C57Bl6 control, Ldlr −/− and Apoe −/− mice fed a Western type diet (WTD) for 1 month (n = 6–10 per group). Values represent means±SEM. *p < 0.05, **p < 0.01, ***p < 0.001 compared with control group. † p < 0.01 compared with the Ldlr −/− group
Ldlr −/− and Apoe −/− mice have increased levels of cholesterol in chylomicron, VLDL and LDL fractions, and decreased HDL [16–18]. As the LDLr is involved in uptake of VLDL and LDL, we hypothesised that the normal islet cholesterol levels seen in Ldlr −/− mice even in the presence of hypercholesterolaemia could be explained by decreased uptake of LDL and VLDL in the absence of the LDLr. Therefore, we analysed the uptake of DiI-LDL and DiI-VLDL in islets of control, Ldlr −/− and Apoe −/− mice. DiI-LDL was taken up by islets isolated from control and Apoe −/− mice (Fig. 3). By contrast, DiI-LDL uptake was nearly absent in islets isolated from Ldlr −/− mice (Fig. 3). Uptake of DiI-VLDL was also decreased in islets isolated from Ldlr −/− mice (data not shown).
To determine whether decreased efflux could potentially contribute to increased islet cholesterol levels in Apoe −/− mice, we measured ABCA1 protein levels in isolated islets. Both Ldlr −/− and Apoe −/− mice showed decreased ABCA1 levels in islets (Fig. 4).
ABCA1 protein levels in islets isolated from WTD-fed C57Bl6 control, Ldlr −/− and Apoe −/− mice. Graph represents pooled densitometric measurements of ABCA1 signal intensity blots from three separate experiments. Actin was used as loading control. Values represent means ± SEM. *p < 0.05, **p < 0.01 compared with control mice
To examine the relationship between islet cholesterol levels and beta cell function, glucose-stimulated insulin secretion was measured in vitro in islets isolated from WTD-fed control, Ldlr −/− and Apoe −/− mice. Basal insulin secretion at low glucose (1.67 mmol/l) did not differ among genotypes. Insulin secretion in response to 16.7 mmol/l glucose, however, was significantly decreased in Apoe −/− islets (Fig. 5) compared with control islets. By contrast, glucose-stimulated insulin secretion from Ldlr −/− islets with normal islet cell cholesterol levels was not significantly different from that seen from control islets (Fig. 5). These findings suggest that elevated islet cholesterol in islets from Apoe −/− mice contributes to the observed reduction in glucose-stimulated insulin secretion.
Glucose-stimulated insulin secretion is reduced in islets isolated from Apoe −/− mice (black bars) compared with islets isolated from C57Bl6 control (white bars) and Ldlr −/− (grey bars) mice. C57Bl6 control, Ldlr −/− and Apoe −/− mice were fed a WTD for 1 month, after which islets were isolated. Islets were cultured overnight, cultured in low-glucose Krebs buffer for 2 h and then stimulated for 1 h in the conditions indicated. Values represent pooled data from three separate experiments, each consisting of pooled islets from two mice per genotype, and values are expressed as a percentage of islet content relative to basal secretion (which is arbitrarily set to 1). *p < 0.05 compared with control islets
Hypercholesterolaemia causes beta cell dysfunction in islets with decreased Abca1 function
Our findings suggest that hypercholesterolaemia causes beta cell dysfunction in mice as a result of LDL receptor-mediated uptake of cholesterol. To test this hypothesis, we transplanted 200 islets from Ldlr −/− and wild-type control mice into diabetic Ldlr −/− mice. To increase plasma cholesterol levels, mice were fed WTD after normalisation of glucose levels. We hypothesised that in a hypercholesterolaemic environment in vivo, wild-type islets that produce the LDLr would accumulate cholesterol and exhibit beta cell dysfunction. By contrast, islets lacking the LDLr would be less able to take up cholesterol from the blood and would therefore be protected from the deleterious effects of high circulating cholesterol.
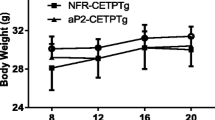
A WTD increased glucose levels temporarily in both groups, but glucose levels normalised within 4 days after the start of the diet to 7.6 ± 1.8 mmol/l in recipients of Ldlr −/− islet transplants vs 8.3 ± 1.6 mmol/l in C57Bl/6 islet transplant recipients. Interestingly, both Ldlr −/− and C57Bl/6 islets were able to maintain normoglycaemia for up to 124 days on a WTD (Fig. 6a). Furthermore, glucose tolerance was similar in mice transplanted with Ldlr −/− islets and mice transplanted with C57Bl/6 islets 120 days after the WTD (Fig. 6b). To determine how the transplanted C57Bl/6 islets handled the high plasma cholesterol levels without reduction in function, we dissected the donor islets from the graft with laser capture microscopy and measured expression levels of Abca1 and Gapdh. Relative Abca1 mRNA levels (normalised to Gapdh mRNA) were increased in C57Bl/6 islet grafts compared with Ldlr −/− islet grafts (Fig. 6c), suggesting increased cholesterol efflux as a response to maintain intracellular cholesterol homeostasis. Correction for insulin or Pdx1 mRNA amounts, to correct for non-islet tissue in the samples, gave similar results (data not shown).
Transplantation of islets expressing the LDL receptor in hypercholesterolaemic diabetic mice does not result in decreased beta cell function in vivo. Ldlr −/− mice were made diabetic using a single injection of STZ on day 0. STZ-treated diabetic Ldlr −/− mice received subcapsular transplants of C57Bl6 or Ldlr −/− islets on day 5, WTD on day 10 and nephrectomy on day 134 (n = 6–8 per group). a Blood glucose levels in transplant recipients (red line, Ldlr −/− islets; black line, C57B16 islets). b Blood glucose levels during intraperitoneal glucose tolerance test 120 days after transplantation. c Relative Abca1 mRNA amounts in islet grafts. Expression data were standardised for Gapdh expression. Values represent means ± SEM. *p < 0.05 compared with Ldlr −/− islet grafts. Red line or red bar, Ldlr −/− islets; black line or black bar, C57B16 islets
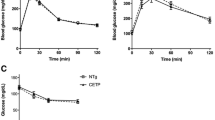
To determine whether increased ABCA1 protects against hypercholesterolaemia-induced beta cell dysfunction, a second transplant study was performed using diabetic Ldlr −/− mice as recipients of islets transplanted from Abca1 +/+ or Abca1 +/−P donors. We hypothesised that in a hypercholesterolaemic environment in vivo, Abca1 +/−P islets that have decreased ABCA1 activity would accumulate cholesterol and exhibit beta cell dysfunction. Indeed, mice transplanted with Abca1 +/−P islets tended to have increased blood glucose levels (p = 0.0675; Fig. 7a). One mouse transplanted with Abca1 +/−P islets failed to maintain normal blood glucose and became diabetic 64 days after STZ treatment. Furthermore, mice transplanted with Abca1 +/−P islets had more difficulty maintaining normal blood glucose levels, as indicated by an increased number of days with blood glucose levels above 11.0 mmol/l (Fig. 7b). Glucose tolerance testing 55 days (Fig. 7c, d) and 90 days (Fig. 7e, f) after STZ treatment showed impaired glucose tolerance in mice transplanted with Abca1 +/−P islets, indicating decreased beta cell function in Abca1 +/−P islets.
Transplantation of islets with decreased beta cell ABCA1 expression in hypercholesterolaemic diabetic mice results in graft failure and impaired beta cell function. Ldlr −/− mice were made diabetic using a single injection of STZ on day 0. STZ-treated diabetic Ldlr −/− mice received subcapsular transplant of Abca1 +/+ or Abca1 +/−P islets on day 5, WTD on day 40 and nephrectomy on day 96 (n = 4 per group). a Blood glucose levels in transplant recipients (n = 4 per group). b Number of days with blood glucose levels above 11 mmol/l in transplant recipients. c Glucose tolerance testing 55 days post-STZ treatment (n = 4 per group). d Area under curve of c. e Glucose tolerance testing 90 days post-STZ treatment (n = 3–4 per group). f Area under curve of e. Values represent means±SEM. *p < 0.05 compared with Abca1 +/+ islet grafts. Red line or red bar, Abca1 +/−P islets; black line or black bar, Abca1 +/+
Lack of LDLr does not protect Abca1 −/− mice from islet cholesterol accumulation
To further dissect the relative importance of cholesterol uptake and efflux to islet cholesterol homeostasis in vivo, we created beta-cell-specific Abca1 knockout mice on a LDLr knockout background. Previously, we have shown that mice lacking the cholesterol efflux transporter Abca1 specifically in beta cells have increased islet cholesterol levels as a result of decreased efflux [2]. We hypothesised that intracellular levels of cholesterol in islets are determined by the homeostasis between cholesterol influx and efflux with either increased influx or decreased efflux leading to increased cholesterol levels in islets. To determine whether lack of the LDLr might protect beta cells lacking ABCA1 from cholesterol accumulation and islet dysfunction, we crossed Ldlr −/− mice with beta-cell-specific Abca1 knockout (Abca1 −P/−P) mice. As expected, mice lacking LDLr showed increased plasma cholesterol levels (7.29 ± 0.72 mmol/l in Abca1 fl/fl;Ldlr −/− and 5.48 ± 0.70 mmol/l in Abca1 −P/−P;Ldlr −/− mice) compared with LDLr +/+ mice (1.91 ± 0.51 mmol/l in Abca1 fl/fl and 2.12 ± 0.44 mmol/l in Abca1 −P/−P mice). As previously described, lack of Abca1 in beta cells resulted in cholesterol accumulation in islets (Fig. 8a). Lack of LDLr in Abca1 −P/−P mice, however, did not reduce islet cholesterol levels. Islet cholesterol levels in Abca1 −P/−P;LDLr −/− mice were comparable to Abca1 −P/−P mice (Fig. 8a). In addition, glucose-stimulated insulin secretion was impaired in Abca1 −P/−P;LDLr −/− islets to a similar extent to that in Abca1 −P/−P mice (Fig. 8b) with similar impairment in glucose tolerance (Fig. 8c, d).
Lack of the LDL receptor does not prevent cholesterol accumulation and, subsequently, beta cell dysfunction in islets lacking beta cell ABCA1. a Islet cholesterol levels of islets isolated from Abca1 fl/fl, Abca1 fl/fl ;Ldlr −/−, Abca1 −P/−P and Abca1 −P/−P ;Ldlr −/− mice (n = 6–11 per group). b Isolated islets from Abca1 fl/fl, Abca1 fl/fl ;Ldlr −/−, Abca1 −P/−P and Abca1 −P/−P ;Ldlr −/− mice were cultured overnight, after which glucose-stimulated insulin secretion was measured. Values represent pooled data from two separate experiments; each consisting of pooled islets from three mice per genotype and values are expressed as a percentage of islet content relative to basal secretion (which is arbitrarily set to 1). c Glucose tolerance testing in 4-month-old Abca1 fl/fl (black dotted line with triangle), Abca1 fl/fl;Ldlr −/− (red dotted line with square), Abca1 −P/−P ( black line with diamond) and Abca1 −P/−P ;Ldlr −/− (red line with triangle) mice (n = 4–6 per group). d Area under the curve of the glucose tolerance test as depicted in c. ***p < 0.001 compared with Abca1 fl/fl mice. e Islet cholesterol levels of isolated islets from Abca1 fl/fl, Abca1 fl/fl;Ldlr −/−, Abca1 −P/−P and Abca1 −P/−P;Ldlr −/− mice treated with or without 10 µmol/l mevastatin for 48 h (n = 3–4 per group). f Isolated islets from Abca1 fl/fl, Abca1 fl/fl;Ldlr −/−, Abca1 −P/−P and Abca1 −P/−P;Ldlr −/− mice were treated with or without 10 µmol/l mevastatin for 48 h (n = 3–4 per group), after which glucose-stimulated insulin secretion was measured. Values represent pooled data from two separate experiments, each consisting of pooled islets from two mice per genotype, and values are expressed as a percentage of islet content relative to basal secretion (which is arbitrarily set to 1). *p < 0.05, ***p < 0.001, † p = 0.065 compared with control group. White bar, Abca1 fl/fl islets; light grey bar, Abca1 fl/fl ;Ldlr −/− islets; black bar, Abca1 −P/−P islets; dark grey bar, Abca1 −P/−P ;Ldlr −/− islets
The accumulation of cholesterol in islets isolated from Abca1 −P/−P;Ldlr −/− mice indicates that cholesterol biosynthesis or cholesterol uptake via other receptors contributes to islet cholesterol levels. To determine whether cholesterol synthesis contributes to the islet cholesterol content in these mice, we treated islets isolated from Abca1 fl/fl, Abca1 −P/−P, Abca1 fl/fl ;Ldlr −/− and Abca1 −P/−P /Ldlr −/− mice with 10 µmol/l mevastatin in RPMI media containing 200 µmol/l mevalonate and 10% delipidated FCS for 48 h. Mevastatin, which inhibits cholesterol synthesis, has previously been shown to decrease islet cholesterol content by approximately 40% [4]. Although mevastatin treatment did result in decreased islet cholesterol levels in Abca1 fl/fl and Abca1 fl/fl;Ldlr −/− islets, no change was noted in the Abca1 −P/−P and Abca1 −P/−P;Ldlr −/− islets (Fig. 8e). We next determined how this treatment and its effect on cholesterol content influenced glucose-stimulated insulin secretion. Mevastatin treatment increased glucose-stimulated insulin secretion in Abca1 fl/fl and Abca1 fl/fl;Ldlr −/− islets, in accordance with previous findings in C57Bl6/J islets [4], but had no impact on insulin secretion in islets isolated from Abca1 −P/−P and Abca1 −P/−P;Ldlr −/− mice (Fig. 8f).
Discussion
The results of this study point to an important role for the beta cell LDLr in regulating islet cholesterol uptake and beta cell function. High circulating cholesterol levels, as seen in Apoe −/− mice, increase islet cholesterol and decrease beta cell function. Lack of the LDLr leads to increased circulating cholesterol levels without affecting islet cholesterol levels or beta cell function (Table 1). Thus, lack of the LDLr protects beta cells from accumulation of cholesterol and cholesterol-induced beta cell dysfunction in a hypercholesterolaemic environment. These findings suggest an important role for the LDL receptor in the uptake of cholesterol by islets. In addition, our findings point to a crucial role for beta cell ABCA1 in regulating islet cholesterol homeostasis in vivo. Lack of the LDL receptor did not prevent cholesterol accumulation in beta cells lacking ABCA1, indicating that cholesterol efflux is rate limiting in maintaining cellular cholesterol levels in beta cells.
Islets are known to express several lipoprotein receptors, including the VLDL receptor, LDL receptor, LRP, SRB1 and CD36 [6, 7]. In vitro studies have shown that the LDLr is involved in islet LDL uptake [6] and in the LDL-induced reduction in glucose-stimulated insulin secretion [5]. In this study, we show that the LDLr is essential for uptake of circulating cholesterol by the islet in vivo. Protection against hypercholesterolaemia-induced cholesterol accumulation in islets lacking the LDLr indicates that lipoprotein receptors such as VLDLr or LRP or scavenger receptors such as SRB1 or CD36 do not play a major role in cholesterol uptake in islets with functional ABCA1.
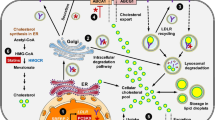
Our results support previous in vitro studies that found that dysregulation of beta cell cholesterol homeostasis may result in impaired beta cell function [3, 4, 19]. Both depletion of islet cholesterol [3, 4] or islet cholesterol loading using water-soluble cholesterol lead to decreased insulin secretion in vitro [4]. Interestingly, inhibition of cholesterol synthesis in islets also leads to decreased insulin secretion [19], suggesting that either too much or too little cholesterol can result in impaired beta cell function. Although the precise mechanisms by which decreased ABCA1 function influences this process remain to be elucidated, a model has emerged in which impaired ABCA1 function leads to elevated islet cholesterol levels, disordered beta cell membrane cholesterol composition and inhibition of fusion of insulin granules from the readily releasable pool, leading to the observed impairment in first-phase insulin secretion [2].
Beta cell cholesterol homeostasis in vivo appears to be tightly regulated. Feeding of a WTD to control animals decreases Ldlr expression and does not result in increased islet cholesterol levels. Furthermore, transplantation of wild-type islets with functional LDL receptors into diabetic, hypercholesterolaemic Ldlr −/− mice did not result in impaired beta cell function. Transplantation of islets with decreased levels of beta cell Abca1 (Abca1 +/−P) into diabetic, hypercholesterolaemic Ldlr −/− mice, however, did result in impaired beta cell function and beta cell failure, suggesting that sufficient Abca1 expression is necessary for islets to adapt to a hypercholesterolaemic environment. Interestingly, hypercholesterolaemic Apoe −/− mice showed decreased islet ABCA1 production, which makes it interesting to speculate that this contributed to the increased islet cholesterol levels observed in these mice. Total lack of beta cell Abca1 leads to increased islet cholesterol levels, even in the absence of the LDLr. These findings highlight the importance of ABCA1 in regulating islet cholesterol levels in vivo.
It is surprising that islet cholesterol levels are increased in islets lacking both the LDLr and ABCA1. The cholesterol that accumulated in the Abca1 −P/−P;Ldlr −/− islets could originate from cholesterol uptake via other receptors such as LRP or VLDLr facilitated by the increased plasma cholesterol levels. Importantly, despite increased plasma cholesterol levels in Abca1 −P/−P;Ldlr −/− compared with Abca1 −P/−P mice, islet cholesterol levels were similar, indicating that the absence of LDLr-mediated cholesterol uptake may help ameliorate the effect of increased plasma cholesterol on islet cholesterol levels.
Besides cholesterol uptake and efflux, cholesterol synthesis contributes to islet cholesterol content. Inhibition of cholesterol synthesis by mevastatin treatment in lipid-poor media leads to decreased islet cholesterol content and improved glucose-stimulated insulin in Abca1 fl/fl and Abca1 fl/fl; Ldlr −/− islets, in accordance with previous data [4]. The contribution of cholesterol synthesis to islet cholesterol content could explain the observation that islets from hypercholesterolaemic Ldlr −/− mice have normal cholesterol levels and that the islet cholesterol content in hypercholesterolaemic Apoe −/− mice is only increased 1.7-fold compared with controls. Interestingly, mevastatin treatment failed to decrease islet cholesterol content in both Abca1 −P/−P and Abca1 −P/−P;Ldlr −/− islets, indicating a crucial role of ABCA1 in cellular cholesterol homeostasis. We have previously shown that mRNA levels of HmgCoA-reductase, a key enzyme in the cholesterol synthesis pathway, are decreased in islets of Abca1 −P/−P mice [2]. In addition, we found that mRNA levels of HmgCoA-reductase are decreased to a similar extent in Abca1 −P/−P; Ldlr −/− islets (data not shown). This could in part explain the failure of statin treatment to decrease islet cholesterol levels in these mice.
In agreement with our finding that Ldlr −/− islets are protected against hypercholesterolaemia-induced beta cell dysfunction, patients with familial hypercholesterolaemia (FH), which is either caused by mutations in the LDL receptor or in the ApoB100 (also known as Apob) gene, are not reported to develop type 2 diabetes more frequently or at an earlier age than controls, despite markedly increased plasma cholesterol levels. Some studies even report a decreased incidence of type 2 diabetes in FH [20, 21]. Based on our results, we speculate that this is due to the impaired uptake of LDL by islets of FH patients. Carriers of loss-of-function mutations in ABCA1, however, do display pancreatic beta cell dysfunction [22], indicating the importance of functional ABCA1 in beta cell function. In addition, several SNPs in ABCA1 have been reported to be associated with diabetes as well as decreased HDL levels [23–27].
In conclusion, these findings indicate that hypercholesterolaemia causes increased islet cholesterol levels and decreased beta cell function via LDL receptor-mediated uptake of cholesterol into beta cells. In addition, cholesterol efflux in islet cells via ABCA1 is crucial for regulating islet cell cholesterol homeostasis in vivo. These data add to the growing body of literature that suggests that hypercholesterolaemia may contribute to beta cell dysfunction in type 2 diabetes.
Abbreviations
- ABAC1:
-
ATP-binding cassette transporter A1
- ApoE:
-
Apolipoprotein E
- DiI:
-
1,1′-Dioctadecyl-3,3,3′,3′-tetramethyl-indocarbocyanine perchlorate
- FH:
-
Familial hypercholesterolaemia
- LDLr:
-
LDL receptor
- LRP:
-
LDL-related protein
- MIN6:
-
Mouse insulinoma
- SNP:
-
Single-nucleotide polymorphism
- SRB1:
-
Scavenger receptor B1
- STZ:
-
Streptozotocin
- WTD:
-
Western type diet
References
Perley MJ, Kipnis DM (1967) Plasma insulin responses to oral and intravenous glucose: studies in normal and diabetic subjects. J Clin Invest 46:1954–1962
Brunham LR, Kruit JK, Pape TD et al (2007) Beta-cell ABCA1 influences insulin secretion, glucose homeostasis and response to thiazolidinedione treatment. Nat Med 13:340–347
Xia F, Gao X, Kwan E et al (2004) Disruption of pancreatic beta-cell lipid rafts modifies Kv2.1 channel gating and insulin exocytosis. J Biol Chem 279:24685–24691
Hao M, Head WS, Gunawardana SC, Hasty AH, Piston DW (2007) Direct effect of cholesterol on insulin secretion: a novel mechanism for pancreatic beta-cell dysfunction. Diabetes 56:2328–2338
Rütti S, Ehses JA, Sibler RA et al (2009) Low and high-density lipoproteins modulate function, apoptosis and proliferation of primary human and murine pancreatic beta cells. Endocrinology 150:4521–4530
Roehrich ME, Mooser V, Lenain V et al (2003) Insulin-secreting beta-cell dysfunction induced by human lipoproteins. J Biol Chem 278:18368–18375
Noushmehr H, D'Amico E, Farilla L et al (2005) Fatty acid translocase (FAT/CD36) is localized on insulin-containing granules in human pancreatic beta-cells and mediates fatty acid effects on insulin secretion. Diabetes 54:472–481
Cnop M, Grupping A, Hoorens A, Bouwens L, Pipeleers-Marichal M, Pipeleers D (2000) Endocytosis of low-density lipoprotein by human pancreatic beta cells and uptake in lipid-storing vesicles, which increase with age. Am J Pathol 156:237–244
Grupping AY, Cnop M, van Schravendijk CF, Hannaert JC, van Berkel TJ, Pipeleers DG (1997) Low density lipoprotein binding and uptake by human and rat islet beta cells. Endocrinology 138:4064–4068
Salvalaggio PR, Deng S, Ariyan CE et al (2002) Islet filtration: a simple and rapid new purification procedure that avoids ficoll and improves islet mass and function. Transplantation 74:877–879
Plesner A, Liston P, Tan R, Korneluk RG, Verchere CB (2005) The X-linked inhibitor of apoptosis protein enhances survival of murine islet allografts. Diabetes 54:2533–2540
Bligh EG, Dyer WJ (1959) A rapid method of total lipid extraction and purification. Can J Biochem Physiol 37:911–917
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72:248–254
Wellington CL, Walker EK, Suarez A et al (2002) ABCA1 mRNA and protein distribution patterns predict multiple different roles and levels of regulation. Lab Invest 82:273–283
Goldstein JL, Brown MS (2009) The LDL receptor. Arterioscler Thromb Vasc Biol 29:431–438
Plump AS, Smith JD, Hayek T et al (1992) Severe hypercholesterolemia and atherosclerosis in apolipoprotein E-deficient mice created by homologous recombination in ES cells. Cell 71:343–353
Zhang SH, Reddick RL, Piedrahita JA, Maeda N (1992) Spontaneous hypercholesterolemia and arterial lesions in mice lacking apolipoprotein E. Science 258:468–471
Ishibashi S, Brown MS, Goldstein JL, Gerard RD, Hammer RE, Herz J (1993) Hypercholesterolemia in low density lipoprotein receptor knockout mice and its reversal by adenovirus-mediated gene delivery. J Clin Invest 92:883–893
Xia F, Xie L, Mihic A et al (2008) Inhibition of cholesterol biosynthesis impairs insulin secretion and voltage-gated calcium channel function in pancreatic beta-cells. Endocrinology 149:5136–5145
Skoumas I, Masoura C, Pitsavos C et al (2007) Evidence that non-lipid cardiovascular risk factors are associated with high prevalence of coronary artery disease in patients with heterozygous familial hypercholesterolemia or familial combined hyperlipidemia. Int J Cardiol 121:178–183
Vohl MC, Gaudet D, Moorjani S et al (1997) Comparison of the effect of two low-density lipoprotein receptor class mutations on coronary heart disease among French-Canadian patients heterozygous for familial hypercholesterolaemia. Eur J Clin Invest 27:366–373
Vergeer M, Brunham LR, Koetsveld J et al. (2010) Carriers of loss-of-function mutations in ABCA1 display pancreatic beta cell dysfunction. Diabetes Care doi:10.2337/dc09-1562
Daimon M, Ji G, Saitoh T et al (2003) Large-scale search of SNPs for type 2 DM susceptibility genes in a Japanese population. Biochem Biophys Res Commun 302:751–758
Daimon M, Kido T, Baba M et al (2005) Association of the ABCA1 gene polymorphisms with type 2 DM in a Japanese population. Biochem Biophys Res Commun 329:205–210
Frikke-Schmidt R, Nordestgaard BG, Schnohr P, Steffensen R, Tybjaerg-Hansen A (2005) Mutation in ABCA1 predicted risk of ischemic heart disease in the Copenhagen City Heart Study population. J Am Coll Cardiol 46:1516–1520
Saleheen D, Nazir A, Khanum S, Haider SR, Frossard PM (2006) R1615P: a novel mutation in ABCA1 associated with low levels of HDL and type II diabetes mellitus. Int J Cardiol 110:259–260
Villarreal-Molina MT, Flores-Dorantes MT, Arellano-Campos O et al (2008) Association of the ATP-binding cassette transporter A1 R230C variant with early-onset type 2 diabetes in a Mexican population. Diabetes 57:509–513
Acknowledgements
Special thanks to E. Abbott for technical assistance with the microdissection experiments and J. Bohlmann for the use of the LCM system. J. K. Kruit is supported by post-doctoral fellowship awards from the Canadian Institutes of Health Research (CIHR) and the Michael Smith Foundation for Health Research (MSFHR). C. B. Verchere is a MSFHR Senior Scholar. M. R. Hayden holds a Canada Research Chair in Human Genetics and is a University of British Columbia Killam Professor. This work was supported by CIHR grants to M.R. Hayden and C.B. Verchere.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kruit, J.K., Kremer, P.H.C., Dai, L. et al. Cholesterol efflux via ATP-binding cassette transporter A1 (ABCA1) and cholesterol uptake via the LDL receptor influences cholesterol-induced impairment of beta cell function in mice. Diabetologia 53, 1110–1119 (2010). https://doi.org/10.1007/s00125-010-1691-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-010-1691-2