Abstract
Aims/hypothesis
The aim of the study was to determine the loss of muscle volume in the lower leg and foot in long-term diabetic patients in relation to the presence of neuropathy.
Methods
We re-examined 26 type 1 diabetic patients who had participated in magnetic resonance imaging (MRI) studies on muscle volume in the lower leg and foot 9 to 12 years earlier. Re-examination involved MRI, isokinetic dynamometry, clinical examination, electrophysiological studies and quantitative sensory examinations.
Results
Annual loss of muscle volume of ankle dorsal and plantar flexors was 4.5 (5.5–3.9)% (median [range]) and 5.0 (7.0–4.2)% in neuropathic patients, 1.9 (3.2–1.0)% and 1.8 (2.6–1.3)% in non-neuropathic patients, and 1.7 (2.8–0.8)% and 1.8 (2.4–0.8)% in controls, respectively (p < 0.01). Annual change of volume and strength correlated for ankle dorsal flexors (r s = 0.73, p < 0.01) and for ankle plantar flexors (r s = 0.63, p < 0.05) in diabetic patients. In addition, annual change of muscle volume for dorsal and plantar flexors was related to the combined score of all measures of neuropathy (r s = −0.68, p < 0.02 and r s = −0.73, p < 0.01, respectively). Foot muscle volume declined annually by 3.0 (3.4–1.0)% in neuropathic patients and by 1.1 (4.0–0.2)% in non-neuropathic patients, both values being significantly different from controls (0.2 [−2.5 to 2.4]%). Loss of foot muscle volume was related to severity of neuropathy assessed at clinical evaluation (r s = −0.6, p < 0.05).
Conclusions/interpretation
Muscular atrophy in long-term diabetic neuropathy occurs early in the feet, progresses steadily in the lower legs, relates to severity of neuropathy and leads to weakness at the ankle.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Motor dysfunction is a late and severe manifestation of diabetic polyneuropathy (DPN). DPN can lead to impaired gait with foot drop, and poor balance and coordination, and could be involved in the pathogenesis of foot ulcers [1–4].
Previous studies have shown reduced strength in the lower extremities in neuropathic diabetic patients [5, 6]. Recently, a follow-up study found muscle weakness to be progressive in symptomatic neuropathic patients during a 7 year period [7]. Combining magnetic resonance imaging (MRI) with stereological principles for volume analysis, we have demonstrated atrophy of distal muscles of the leg and the foot in diabetic patients with polyneuropathy [8, 9]. These findings have been confirmed by other study groups in MRI studies evaluating diabetic feet [10, 11].
The underlying cause of muscular atrophy in DPN is thought to be a continuous loss of motor axons, which in combination with insufficient reinnervation [12] results in denervation of muscle fibres. As muscle strength deteriorates in patients with DPN, we hypothesised that muscular atrophy would also progress. The present report is a longitudinal MRI study of diabetic patients previously evaluated in two cross-sectional studies. In the first of those studies atrophy of dorsal and plantar flexors of the lower leg occurred in neuropathic patients [8]; in the second, reduced intrinsic foot muscle volume (FMV) was found in patients with DPN [9]. We now report the progression rate of atrophy of lower leg and foot muscles in the same group of patients studied 9 to 13 years previously, using the same methods as applied initially.
Methods
Patients and control participants
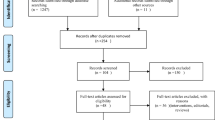
All 16 type 1 diabetic patients (eight non-neuropathic, eight symptomatic neuropathic patients) who participated in a cross-sectional MRI study of muscle volume of the leg from 1994 to 1995 (Leg study) and all 23 type 1 diabetic patients (15 non-neuropathic, eight with chronic neuropathy) who participated in a cross-sectional MRI study on FMV in 1997 (Foot study) were identified for follow-up [6, 8, 9]. Patient files were re-examined and patients were excluded if they had developed any disorder since the first examination that could interfere with motor performance apart from DPN. The remaining patients and their individually matched control participants received a written study invitation. If no answer was returned, a second and final invitation was sent.
Of the 16 patients in the Leg study, two had died, one had a metal object in the foot contradicting MRI and one did not wish to participate. These four patients were all neuropathic. In the Foot study, four of the initial 23 patients were excluded (stroke [one], inclusion body myositis [one], severe ischaemic heart disease [one], and metal object [one]. Three patients did not wish to participate and two patients had died. This left 12 patients (eight non-neuropathic, four neuropathic) for follow-up in the Leg study and 14 (seven non-neuropathic, seven neuropathic) for follow-up in the Foot study. The minimal criteria for diabetic neuropathy used in the initial studies were also applied for follow-up [6, 8, 13].
Care was taken to include the same matched control participants as in the initial studies. In the Leg study four control participants initially matched with non-neuropathic patients could not be re-evaluated as three had developed disorders possibly interfering with motor performance (injury of the ankle ligaments [one], thrombophlebitis [one], breast cancer [one]) and one refused to participate. In the Foot study one control participant was excluded due to hip-replacement surgery, one had died, one had developed polyneuropathy and one could not be located. These control participants were replaced with other controls with similar anthropometric data from the same initial study. All participants gave informed consent to the study, which was approved by the local ethics committee.
MRI
All MRI scans were performed with a Philips Achieva 1.5 T (Best, the Netherlands). Conventional T1-weighted fast spin-echo (TSE) sequence using 5 mm cross-sectional magnetic resonance images was applied for MRI of the leg (echo time = 25 ms, repetition time = 550 ms, field of view 200 × 200 mm) and 4 mm cross-sectional magnetic resonance images were applied for MRI of the foot (echo time = 20 ms, repetition time = 540 ms, field of view 250 × 250 mm). A 256 × 256 matrix and two excitations were applied. All images were converted to digital pictures for analysis on a PC (Fig. 1).
Muscle volume estimation
Muscle anatomy of the leg and foot was defined using the same standards as in the initial studies [8, 14], with exactly the same stereological counting techniques being applied [15] using software designed for stereological analysis (NewCast, version 2.12.1.0; Visiopharm, Hoersholm, Denmark). The observer was blinded to the identity of all MRI images. The methods applied for volume estimation of the muscles of the leg and foot are described in detail elsewhere [8, 9].
Isokinetic dynamometry
Maximal isokinetic strength of knee extensors and flexors and of ankle dorsal and plantar flexors of the non-dominant leg was determined using the same isokinetic dynamometer and testing procedures as in the initial studies [5, 16].
Clinical examination
The patients were examined by a neurologist and evaluated according to the neuropathy impairment score (NIS; range 0–222) [17] and neuropathy symptom score (NSS; range 0–17) as applied in the initial studies. NIS is a combined score obtained from the neurological examination of muscle weakness, activity of tendon reflexes and sensation of the great toe and index finger. NSS includes motor, sensory and autonomic symptoms.
Studies of blood samples, sensory detection thresholds, nerve conduction and retinopathy
In all patients a blood sample was analysed for blood glucose, HbA1c, creatinine and carbamide levels using standard laboratory methods. To evaluate renal function, a sample of first-void urine was analysed for albumin and creatinine and the urinary albumin/creatinine ratio calculated.
Vibratory perception thresholds (VPT) were determined at the dominant index finger and the non-dominant great toe using the same equipment (CASE IV; WR Medical Electronics, Stillwater, MN, USA) and algorithm [18] as previously.
Nerve conduction studies were performed using standardised transcutaneous stimulation and recording techniques and an electromyograph (Keypoint; Medtronic, Copenhagen, Denmark) with standard filter settings [19, 20]. Motor nerve conduction velocity (MNCV) and response amplitudes of compound motor action potential (CMAP) were measured in the dominant forearm segment of the median (elbow to wrist) nerve and in the non-dominant leg segment of the peroneal (below capitulum to ankle) nerve in both studies. In addition, sensory nerve conduction velocity (SNCV) of the dominant median nerve (wrist to index finger) and of the non-dominant sural nerve was measured with anti-dromic activation in the Leg study. We calculated z scores for all MNCVs in both studies and for the amplitude of the CMAPs in the Foot study.
Retinopathy status was determined within 6 months of the MRI at the Department of Ophthalmology, Aarhus University Hospital and rated according to the International Clinical Diabetic Retinopathy Disease Severity Scale [21].
Definitions, calculations and statistical analyses
Change in muscle volume and muscle strength was calculated and expressed as a percentage of the initial value. As time between the two examinations was not identical for all participants, change of muscle volume was expressed as an annual rate.
To rank patients according to peripheral nerve function, a neuropathy rank-sum score (NRSS) was calculated for each patient in both follow-up studies, adding the rank scores for the NSS, NIS, VPTs and NCVs. The VPTs were ranked on the basis of the sum of the two percentiles obtained. In the Leg study, SNCVs of the median and sural nerves were included in the NRSS. In the Foot study amplitudes of the CMAPs were included in the NRSS and their z scores used for ranking. In both studies the z scores of the MNCVs of the median and peroneal nerves were included.
Values for muscle volume, muscle strength, electrophysiological data, perception thresholds and clinical scores were not normally distributed and therefore the Wilcoxon–Mann–Whitney test was applied for all comparisons. The Kruskal–Wallis test was applied for comparisons of the non-neuropathic diabetic patients, the neuropathic diabetic patients and the control group. To estimate associations between various variables Spearman’s rank correlation was applied. Changes of various measures of neuropathy during follow-up were tested using a Wilcoxon signed rank-test. Demographic data were compared using an independent samples t test. For all statistical analyses a 5% limit of significance was applied. STATA software (version 9.2; Statacorp, College Station, TX, USA) was used for all analyses.
Results
Leg study
Demographic data, duration of diabetes and follow-up interval are presented in Table 1. The follow-up period was 12.6 (11.8–12.8) years (median [range]) for diabetic patients and 12.6 (12.6–12.9) years for control participants. Diabetes duration was 42.1 (32.6–45.8) years. Age, weight, height, follow-up interval and diabetes duration did not differ between study groups.
Clinical findings, nerve conduction, vibratory perception and muscle strength
NIS and NSS at the initial study were similar for participating and non-participating neuropathic patients. Both at the initial study and at follow-up, NIS and NSS differed between participating neuropathic and non-neuropathic diabetic patients (Table 2). Of the eight initially non-neuropathic patients, four had developed neuropathy during the follow-up period. Clinical signs of muscle weakness were observed in all neuropathic patients. Impairment of NIS during follow-up was more severe for neuropathic patients than for non-neuropathic patients (17 [15–19] vs 4 [−5 to 14], p < 0.019).
For the sural and peroneal nerves no response could be recorded in any of the neuropathic patients at follow-up. VPTs were abnormal (VPT ≥98th percentile) at both the index finger and the great toe in three neuropathic patients and in one non-neuropathic patient.
Annual loss of strength of knee extensors and flexors, and ankle dorsal and plantar flexors was more severe in neuropathic patients (−2.7 [−3.7 to −2.1]%, −2.7 [−3.9 to −2.1]%, −7.4 [−8.6 to −5.0]%, −4.4 [−5.9 to −3.5]%, respectively) than in non-neuropathic patients (−0.6 [−1.8 to −0.2]%, −0.9 [−2.3 to 2.2]%, −0.3 [−2.4 to 0.5]%, −0.4 [−1.5 to 0.8]%, respectively, all p < 0.05) and in controls (−0.8 [−2.0 to 0.7]%, 0.0 [−1.4 to 2.3]%, −0.7 [−3.3 to 0.5]%, −0.9 [−2.6 to 1.6]%, respectively, all p < 0.005). Annual change of muscle strength did not differ between non-neuropathic patients and controls.
Muscle volume
Muscle volume at the initial study was similar in diabetic patients with or without neuropathy, with a tendency for plantar flexor volume to be smaller in neuropathic patients than in controls (p = 0.056; Table 3). At follow-up, volume of both dorsal and plantar flexors was lower in neuropathic patients than in controls and non-neuropathic patients (Table 3). Correspondingly, atrophy of dorsal and plantar flexors was greater in patients with neuropathy than in patients without neuropathy and in controls (Fig. 2, Table 3).
During the total follow-up period neuropathic patients lost 57% of dorsal flexor volume and 66% of plantar flexor volume, whereas controls lost 21% and 20%, respectively, and non-neuropathic patients 24% of each (p < 0.01).
Annual loss of muscle mass was related to NRSS at follow-up for dorsal as well as for plantar flexors (Fig. 3a, b). Furthermore, the annual loss of muscle volume for dorsal and plantar flexors was related to NIS at the initial study (r s = −0.88, p < 0.001 and r s = −0.93, p < 1 × 10−5, respectively) and to NIS at follow-up (r s = −0.63, p < 0.05 and r s = −0.66, p < 0.05, respectively). No relationship could be established between annual change in muscle volume and change in NIS, duration of diabetes or MNCV and amplitude of the CMAP of the peroneal nerve.
A close relationship was found between annual loss of muscle volume and annual loss of strength for dorsal as well as for plantar flexors (Fig. 4a, b).
Intrinsic muscle strength of dorsal flexors could not be calculated for two neuropathic patients due to paralysis of those flexors. Intrinsic muscle strength, calculated in N×m cm−3 of muscle tissue, did not differ between diabetic patients and control participants for dorsal (0.13 [0.06–0.16] vs 0.14 N×m cm−3 [0.1–0.17], p = 0.47) or plantar flexors (0.10 [0.07–0.52] vs 0.11 N×m cm−3 [0.09–0.15], p = 0.49). No difference was found for intrinsic muscle strength between neuropathic and non-neuropathic patients, or between patient subgroups and controls.
Foot study
Demographic data, duration of diabetes and follow-up interval are presented in Table 1. The follow-up period of 9.5 (9.3–9.6; median [range]) years for diabetic patients was slightly shorter than that for the control participants (9.7 [9.4–9.9] years; p < 0.05). Diabetes duration was 39.3 (25.6–47.6) years. No difference in age, weight, height or diabetes duration occurred between patient groups or patients and controls.
Clinical findings, nerve conduction, vibratory perception and muscle strength
The NSS at the initial study was better in diabetic patients who also participated (0 [0–4]) in follow-up than in those lost to follow-up (3 [0–7]; p < 0.01). NSS and NIS at the initial study and at follow-up are presented in Table 2. In the initial group with neuropathy, four patients experienced an increase in NSS, whereas NSS improved in one patient from 1 to 0. Three patients initially without neuropathy each developed one symptom of neuropathy. Two initially neuropathic patients complained of muscle weakness and unsteady gait. Clinical signs of muscle weakness were found in these two patients and in one other initially neuropathic patient. Change in NIS was not significantly different between neuropathic and non-neuropathic patients.
MNCV of the median nerve in neuropathic patients was slower in the initial study and at follow-up (p < 0.05). A decrease in CMAP of the peroneal nerve occurred in neuropathic patients (p < 0.05). VPTs were abnormal (VPT ≥98th percentile) at both the index finger and the great toe in four neuropathic patients.
Annual loss of strength for ankle dorsal flexion was −1.2% (−10.8 to 0.0) in all diabetic patients versus −0.2% (−2.7 to 1.6) in healthy controls (p < 0.05). No significant loss of strength occurred for ankle plantar flexors or for knee extensors and flexors. Only patients initially classified as neuropathic had a progressive loss of strength of ankle dorsal flexors compared with control participants (p < 0.05).
Muscle volume
In all diabetic patients annual change in FMV differed from that observed in controls (p < 0.001; Table 3). Annual decline of FMV in non-neuropathic and neuropathic patients exceeded that found in control participants (Fig. 5a). No significant difference was found between the two patient subgroups (p = 0.18). Total change of FMV during the follow-up period is presented in Table 3. Volume of the entire foot was similar in diabetic patients and controls (p = 0.8).
a Annual change of intrinsic FMW for neuropathic (Np) and non-neuropathic (Nnp) diabetic patients, and their matched controls (Cs). *p < 0.05 and ***p < 0.001 compared with control participants. b Relationship between annual change of intrinsic FMV and NIS in the initial study in all diabetic patients. r s = −0.60, p < 0.05
A relationship was found between the annual loss of FMV and NIS at time of the initial study (Fig. 5b). Annual loss of FMV was not related to initial NRSS, NRSS at follow-up, NIS at follow-up, annual change of NIS or diabetes duration. No correlation was established between annual loss of FMV and change in muscle strength at the knee or ankle. MNCV and amplitude of the CMAP of the peroneal nerve showed no relation to annual decline of FMV.
Discussion
Diabetic patients with polyneuropathy have reduced volume of leg and foot muscles closely related to the degree of neuropathy [8, 9]. The present follow-up studies provide new insights into the progression of muscle dysfunction in diabetes in relation to neuropathy. Nerve function declines with diabetes duration [22] leading to denervation and loss of muscle strength in patients with neuropathy [7]. In the present study we have shown that muscle volume in the lower leg was more than halved during an observational period of 13 years in type 1 diabetic patients with severe neuropathy and that in patients with a milder degree of neuropathy one fifth of the foot muscle volume was lost over a decade. Our findings support the hypothesis that the progressive loss of muscle strength seen in neuropathic patients is due to accelerated muscular atrophy.
Magnetic resonance imaging was not performed with the same MRI scanner as used in the initial studies, but exactly the same scanning protocols were followed. Data from estimation of FMV in the initial study in 1997 were compared with the results of a re-analysis of the initial magnetic resonance images, revealing a difference of only 0.17% (p = 0.96; C. S. Andreassen, unpublished results). Since all stereological analyses of magnetic resonance images from the initial and present studies on muscle volume in the lower leg and the foot were performed by the same observer (C. S. Andreassen) at follow-up, an even smaller variability than the reported inter-observer variability can be expected.
As suggested by Greenman et al. [11], a difference in foot size might introduce bias. Thus if the diabetic patients have smaller feet, this will result in smaller muscle volume. We therefore calculated the total foot size, but no difference was found between healthy control participants and diabetic patients (Table 3). In this study, foot size had no influence, as change in muscle volume depends only on the relationship between the measured values in the initial study and at follow-up.
Reduced size of foot muscles using MRI has been reported by Greenman et al. [11] and Bus et al. [10], who calculated the ratio of muscle/total foot from one cross-sectional image. Their results are in accordance with the lower muscle volumes observed in patients with and without neuropathy in this study.
Volume estimations based on MRI can be affected by geometric distortions and thereby lead to errors in area measurements [23]. The degree of distortion is related partly to the performance of the imaging hardware (magnetic field homogeneity and gradient linearity) and partly to the magnetic properties of the imaged object. The 1.5 T MR system used was monitored regularly (periodical image quality test-data, Philips Achieva, 28 September 2007) to ensure that homogeneity was below 1 part per million. Also, we used a TSE sequence to reduce object-induced distortion. Furthermore, to attenuate system- and object-induced distortion, high read-out bandwidth was applied and the field of view was kept reasonably small.
The number of patients was small in both studies and a substantial proportion (25–35%) was lost to follow-up. In the Leg study, patients lost to follow-up had similar baseline data to those participating; therefore, the patients evaluated at follow-up would seem to be representative of the study population. However, the neuropathic group consisted of men only, so there could be a sex-related difference. In the Foot study, NSS and NIS were higher in the non-participating patients, of whom eight out of nine were neuropathic. Thus at follow-up patients with milder degrees of neuropathy were over-represented, probably leading to underestimation of loss of muscle volume in the feet of neuropathic patients.
The participants in our study were not examined for peripheral arterial disease (PAD) of the lower extremities. However, in the initial studies and at follow-up patients were excluded if they had symptoms or a history of PAD. PAD has been related to decreased muscular function in the lower extremities in non-diabetic [24, 25] and type 2 diabetic patients [26]. The impairments observed in PAD patients were much smaller than those found in diabetic patients [5, 8]; furthermore, the PAD patients studied were older, had a higher BMI and suffered severe comorbidities. In a study of type 2 diabetic patients with PAD [26] neuropathy was not sufficiently evaluated and might, therefore, explain the motor dysfunction observed, a finding supported by another study on muscle function in type 2 diabetes [27]. Though none of our participants had symptoms or a history of PAD, measurement of the ankle brachial index would have allowed us to exclude the influence of this potential confounder.
No correlations could be established between the rate of muscular atrophy and nerve conduction variables or VPT. Due to the design of the initial studies, only patients originally either with or without neuropathy were included at follow-up, resulting in a lack of data for the peroneal nerve, as no response could be obtained in three of the four neuropathic patients in the Leg study and in two neuropathic patients in the Foot study. These relationships might have been established if patients with lesser degrees of neuropathy had been included in the initial studies.
Several studies have demonstrated motor abnormalities during early stages of DPN using electromyography [28, 29], and also that loss of muscle strength is closely related to signs of reinnervation following axonal loss [12]. In diabetic patients without clinical signs of neuropathy, early motor neuropathy has been detected by invasive muscle fibre conduction velocity (MFCV) testing [30]. MFCV slowing due to muscle fibre atrophy is related to chronic and acute nerve lesions [31, 32]. The patients in our study were not examined using electromyography or MFCV testing, which would have added valuable information about the underlying cause of the observed muscular atrophy. However, an earlier electromyography study from our laboratory has indicated that insufficient collateral reinnervation is involved in loss of muscle strength [12].
The natural history of DPN has been described in large-scale long-term follow-up studies. Progressive deterioration of nerve conduction variables, autonomic tests, sensory detection thresholds and clinical examination scores can be slowed or prevented by tight glycaemic control [22, 33, 34]. To our knowledge, there is only one follow-up study on diabetic muscle mass and strength including older type 2 diabetic patients, but the participants were not characterised with respect to degree of neuropathy [27]. The present study and our previous study on muscle strength [7] are the only ones on motor function in diabetic patients in relation to neuropathy.
Muscle volume decreased by 1.6% per year in control participants in the Leg study, while FMV was unchanged in controls in the Foot study. It is well-known that sarcopenia occurs approximately from the age of 50 years [35] and preferentially affects fast-twitch fibres [36]. The plantar flexors consist mainly of slow-twitch fibres [37] and consequently it seems unlikely that a difference in muscle fibre distribution could explain our observations. As far as we know, no follow-up study has been performed on foot muscles. FMV remained stable throughout the follow-up period in controls, one explanation being that the size of foot muscles is relatively constant once they reach optimal functional size. We found no relationship between alterations in leg muscle volume or intrinsic muscle strength and age in controls such as those described by others [38], possibly due to the small number of participants examined in our study.
Disuse atrophy can contribute to accelerated loss of muscle volume [39]. This, however, probably plays a minor role in our study, as all patients were able to walk, managed normal activities of daily living and had stable body weight.
Intrinsic muscle strength (muscle quality) was similar in healthy control participants and diabetic patients in the present study. This is in contrast to the study by Park et al., who observed a small but significant difference in intrinsic muscle strength in a large group of older type 2 diabetic patients using dual-energy x-ray absorptiometry (DEXA) to evaluate muscle mass [40]. Overestimation of muscle mass by DEXA could account for the lower muscle quality observed [41], as could increased fat infiltration of the muscle, which is found more frequently in type 2 diabetic patients [42]. Analysis of magnetic resonance images allows exclusion of fat and fibrous tissue within muscle compartments. However, MRI is far more time-consuming and expensive than DEXA and therefore not suitable for large-scale studies.
The annual loss of muscle strength for ankle plantar and dorsal flexors is 3% in patients with symptomatic neuropathy [7]. In the present study, however, annual loss of strength was approximately 6%. This discrepancy can be explained by the more severe degree of neuropathy found in the neuropathic patients in the present study (NIS 55 vs 22, present vs previous study [7], respectively).
Finally, the reported values on muscular atrophy are an average based on two cross-sectional studies separated by a long follow-up period and may therefore simplify the pathological process observed.
In conclusion, long-term diabetic patients with severe neuropathy experience accelerated muscular atrophy of the lower leg and foot, leading to loss of muscle strength. In addition, an increased rate of muscular atrophy occurs in the foot in non-neuropathic patients, suggesting that motor dysfunction arises in subclinical neuropathy. Future prevention of muscular atrophy is important for helping avoid lower leg muscle weakness, poor walking performance [43, 44] and probably also development of foot ulcers [10, 45].
Abbreviations
- CMAP:
-
Compound motor action potential
- DEXA:
-
Dual-energy X-ray absorptiometry
- DPN:
-
Diabetic polyneuropathy
- FMV:
-
Intrinsic foot muscle volume
- MNCV:
-
Motor nerve conduction velocity
- MRI:
-
Magnetic resonance imaging
- NIS:
-
Neuropathy impairment score
- NRSS:
-
Neuropathy rank-sum score
- NSS:
-
Neuropathy symptom score
- PAD:
-
Peripheral arterial disease
- SNCV:
-
Sensory nerve conduction velocity
- TSE:
-
T1-weighted fast spin-echo
- VPT:
-
Vibratory perception thresholds
References
Menz HB, Lord SR, St George R, Fitzpatrick RC (2004) Walking stability and sensorimotor function in older people with diabetic peripheral neuropathy. Arch Phys Med Rehabil 85:245–252
Akashi PM, Sacco IC, Watari R, Hennig E (2008) The effect of diabetic neuropathy and previous foot ulceration in EMG and ground reaction forces during gait. Clin Biomech (Bristol, Avon) 23:584–592
Abboud RJ, Rowley DI, Newton RW (2000) Lower limb muscle dysfunction may contribute to foot ulceration in diabetic patients. Clin Biomech (Bristol, Avon) 15:37–45
Caselli A, Pham H, Giurini JM, Armstrong DG, Veves A (2002) The forefoot-to-rearfoot plantar pressure ratio is increased in severe diabetic neuropathy and can predict foot ulceration. Diabetes Care 25:1066–1071
Andersen H, Poulsen PL, Mogensen CE, Jakobsen J (1996) Isokinetic muscle strength in long-term IDDM patients in relation to diabetic complications. Diabetes 45:440–445
Andersen H, Nielsen S, Mogensen CE, Jakobsen J (2004) Muscle strength in type 2 diabetes. Diabetes 53:1543–1548
Andreassen CS, Jakobsen J, Andersen H (2006) Muscle weakness: a progressive late complication in diabetic distal symmetric polyneuropathy. Diabetes 55:806–812
Andersen H, Gadeberg PC, Brock B, Jakobsen J (1997) Muscular atrophy in diabetic neuropathy: a stereological magnetic resonance imaging study. Diabetologia 40:1062–1069
Andersen H, Gjerstad MD, Jakobsen J (2004) Atrophy of foot muscles: a measure of diabetic neuropathy. Diabetes Care 27:2382–2385
Bus SA, Yang QX, Wang JH, Smith MB, Wunderlich R, Cavanagh PR (2002) Intrinsic muscle atrophy and toe deformity in the diabetic neuropathic foot: a magnetic resonance imaging study. Diabetes Care 25:1444–1450
Greenman RL, Khaodhiar L, Lima C, Dinh T, Giurini JM, Veves A (2005) Foot small muscle atrophy is present before the detection of clinical neuropathy. Diabetes Care 28:1425–1430
Andersen H, Stalberg E, Gjerstad MD, Jakobsen J (1998) Association of muscle strength and electrophysiological measures of reinnervation in diabetic neuropathy. Muscle Nerve 21:1647–1654
Dyck PJ, Kratz KM, Lehman KA et al (1991) The Rochester Diabetic Neuropathy Study: design, criteria for types of neuropathy, selection bias, and reproducibility of neuropathic tests. Neurology 41:799–807
Ferner H, Staubesand J (1982) Sobotta atlas of human anatomy 2. Urban and Schwarzenberg, Munich
Gundersen HJ, Jensen EB (1987) The efficiency of systematic sampling in stereology and its prediction. J Microsc 147:229–263
Andersen H (1996) Reliability of isokinetic measurements of ankle dorsal and plantar flexors in normal subjects and in patients with peripheral neuropathy. Arch Phys Med Rehabil 77:265–268
Dyck PJ (1993) Quantitating severity of neuropathy. In: Dyck PJ, Thomas PK, Griffin JW, Low PA, Poduslo JF (eds) Peripheral neuropathy. Saunders, Philadelphia, pp 686–697
Dyck PJ, O’Brien PC, Kosanke JL, Gillen DA, Karnes JL (1993) A 4, 2, and 1 stepping algorithm for quick and accurate estimation of cutaneous sensation threshold. Neurology 43:1508–1512
Stalberg E, Falck B (1993) Clinical motor nerve conduction studies. Methods Clin Neurophysiol 4:61–80
Falck B, Stalberg E, Bischoff C (1994) Sensory nerve conduction studies with surface electrodes. Methods Clin Neurophysiol 5:1–20
The Diabetic Retinopathy Study Research Group (1981) A modification of the Airlie House classification of diabetic retinopathy (DRS report no. 7). Invest Ophthalmol Vis Sci 21:210–226
Dyck PJ, Davies JL, Litchy WJ, O’Brien PC (1997) Longitudinal assessment of diabetic polyneuropathy using a composite score in the Rochester Diabetic Neuropathy Study cohort. Neurology 49:229–239
Fransson A, Andreo P, Potter R (2001) Aspects of MR image distortions in radiotherapy treatment planning. Strahlenther Onkol 177:59–73
McDermott MM, Hoff F, Ferrucci L et al (2007) Lower extremity ischemia, calf skeletal muscle characteristics, and functional impairment in peripheral arterial disease. J Am Geriatr Soc 55:400–406
McDermott MM, Tian L, Ferrucci L et al (2008) Associations between lower extremity ischemia, upper and lower extremity strength, and functional impairment with peripheral arterial disease. J Am Geriatr Soc 56:724–729
Dolan NC, Liu K, Criqui MH et al (2002) Peripheral artery disease, diabetes, and reduced lower extremity functioning. Diabetes Care 25:113–120
Park SW, Goodpaster BH, Strotmeyer ES et al (2007) Accelerated loss of skeletal muscle strength in older adults with type 2 diabetes: the health, aging, and body composition study. Diabetes Care 30:1507–1512
Shields RW Jr (1987) Single-fiber electromyography is a sensitive indicator of axonal degeneration in diabetes. Neurology 37:1394–1397
Bril V, Werb MR, Greene DA, Sima AA (1996) Single-fiber electromyography in diabetic peripheral polyneuropathy. Muscle Nerve 19:2–9
Meijer JW, Lange F, Links TP, van der Hoeven JH (2008) Muscle fiber conduction abnormalities in early diabetic polyneuropathy. Clin Neurophysiol 119:1379–1384
van der Hoeven JH, Zwarts MJ, van Weerden TW (1993) Muscle fiber conduction velocity in amyotrophic lateral sclerosis and traumatic lesions of the plexus brachialis. Electroencephalogr Clin Neurophysiol 89:304–310
Blijham PJ, ter Laak HJ, Schelhaas HJ, van Engelen BG, Stegeman DF, Zwarts MJ (2006) Relation between muscle fiber conduction velocity and fiber size in neuromuscular disorders. J Appl Physiol 100:1837–1841
The Diabetes Control and Complications Trial Research Group (1995) The effect of intensive diabetes therapy on the development and progression of neuropathy. Ann Intern Med 122:561–568
Martin CL, Albers J, Herman WH et al (2006) Neuropathy among the diabetes control and complications trial cohort 8 years after trial completion. Diabetes Care 29:340–344
Hughes VA, Frontera WR, Roubenoff R, Evans WJ, Singh MA (2002) Longitudinal changes in body composition in older men and women: role of body weight change and physical activity. Am J Clin Nutr 76:473–481
Thompson LV (2009) Age-related muscle dysfunction. Exp Gerontol 44:106–111
Saltin B, Gollnick PD (1983) Skeletal muscle adaptability: significance for metabolism and performance. In: Peachey LD, Adrian PH, Geiger SR (eds) Handbook of physiology—skeletal muscle. American Physiological Society, Washington, DC, pp 555–631
Faulkner JA, Larkin LM, Claflin DR, Brooks SV (2007) Age-related changes in the structure and function of skeletal muscles. Clin Exp Pharmacol Physiol 34:1091–1096
Berg HE, Eiken O, Miklavcic L, Mekjavic IB (2007) Hip, thigh and calf muscle atrophy and bone loss after 5-week bedrest inactivity. Eur J Appl Physiol 99:283–289
Park SW, Goodpaster BH, Strotmeyer ES et al (2006) Decreased muscle strength and quality in older adults with type 2 diabetes: the health, aging, and body composition study. Diabetes 55:1813–1818
Delmonico MJ, Kostek MC, Johns J, Hurley BF, Conway JM (2007) Can dual energy X-ray absorptiometry provide a valid assessment of changes in thigh muscle mass with strength training in older adults? Eur J Clin Nutr 62:1372–1378
Dube MC, Joanisse DR, Prud’homme D et al (2006) Muscle adiposity and body fat distribution in type 1 and type 2 diabetes: varying relationships according to diabetes type. Int J Obes (Lond) 30:1721–1728
Mueller MJ, Minor SD, Sahrmann SA, Schaaf JA, Strube MJ (1994) Differences in the gait characteristics of patients with diabetes and peripheral neuropathy compared with age-matched controls. Phys Ther 74:299–308
Kwon OY, Minor SD, Maluf KS, Mueller MJ (2003) Comparison of muscle activity during walking in subjects with and without diabetic neuropathy. Gait Posture 18:105–113
van Schie CH (2005) A review of the biomechanics of the diabetic foot. Int J Low Extrem Wounds 4:160–170
Acknowledgements
The study was presented in a shortened form at the 18th Annual Meeting of the Diabetic Neuropathy Study Group of the EASD, held in Orvieto, Italy, 4–7 September 2008. Special thanks to J. Andersen and J. Nyengaard at the Stereology and Electron Microscopy Research Laboratory and MIND Centre, University of Aarhus, Aarhus, Denmark. This study was supported by the Danish Diabetes Association and the Danish Medical Society’s Research fund.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
An erratum to this article can be found at http://dx.doi.org/10.1007/s00125-009-1372-1
Rights and permissions
About this article
Cite this article
Andreassen, C.S., Jakobsen, J., Ringgaard, S. et al. Accelerated atrophy of lower leg and foot muscles—a follow-up study of long-term diabetic polyneuropathy using magnetic resonance imaging (MRI). Diabetologia 52, 1182–1191 (2009). https://doi.org/10.1007/s00125-009-1320-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-009-1320-0