Abstract
Primary Sjögren’s syndrome (pSS) is a chronic autoimmune exocrine disease associated with variable lymphocytic infiltration of the affected organs (primarily salivary and lachrymal glands). To investigate the potential implication of nerve growth factor-β (NGF-β) and its high affinity receptor tyrosine kinase receptor A (TrkA) in the regulation of pSS inflammatory responses, we studied their expression in the human salivary gland epithelial cells (SGEC) cultures from pSS minor salivary glands (MSG) biopsies and their relationship with histopathological disease parameters. Here, we demonstrated an increased expression of the NGF-β/TrkA system in pSS SGEC, correlated with the MSG inflammation grade. The results demonstrate that the pro-inflammatory cytokines TNF-α and IL-6 enhance NGF-β production; on the contrary, NGF-β production was reduced in the presence of both Raf-1 kinase and MEK inhibitors. Furthermore, TNF-α/IL-6 treatment increased ERK1/2 phosphorylation. Inhibition of the EGF/EGFR system also decreased NGF-β release by pSS SGEC, indicating that the chronic inflammatory condition characteristic of pSS enhances NGF-β production via EGFR/Raf-1/MEK/ERK pathway activation.
Key message
-
NGF-β and TrkA expression is elevated in salivary gland epithelial cells of primary Sjögren’s syndrome (pSS).
-
Overexpression of NGF-β/TrkA system in pSS occurs via EGFR/Raf-1/MEK/ERK pathway.
-
In pSS, NGF-β overexpression was prevented by EGFR/Raf-1/MEK/ERK pathway inhibition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The nerve growth factor-β (NGF-β), originally described as a neurotrophic factor required for cell survival and differentiation during development of the nervous system, is now recognized to have a much more extensive role and is considered to be a mediator of inflammation. NGF-β interacts with its high affinity receptor tyrosine kinase receptor A (TrkA) [1] to influence the inflammatory process, regulating immune cell functions and, indirectly, modulating inflammatory factors synthesis thus exacerbating the inflammatory reaction [2]. An altered expression of the NGF-β/TrkA system has been amply reported in diseases associated with inflammatory and/or autoimmune responses [2]. Numerous studies have shown that during the inflammatory process there is a localized increase of NGF-β at the sites of inflammation. Increased NGF-β concentrations, which closely reflect the course of disease, were initially found in the cerebrospinal fluid of multiple sclerosis patients [3], in the synovial fluids of rheumatoid arthritis patients [4] and in the sera of systemic lupus erythematosus (SLE) patients [5, 6]. NGF-β mRNA expression and protein levels are increased in animal models of inflammation such as Freund’s adjuvant-induced and carragenin-induced arthritis [7, 8] in NZB/W mice, a spontaneous model of human SLE [9], and in experimental autoimmune encephalomyelitis [10]. NGF-β enhancement seems to be a common feature of many other inflammatory diseases such as interstitial cystitis [11, 12], allergic asthma [13, 14], vernal keratoconjunctivitis [15], Crohn’s disease and colitis [16, 17], psoriasis [18, 19] and atopic dermatitis [20]. The data obtained from all these in vivo studies have clearly indicated that NGF-β synthesis is up-regulated during inflammatory processes, and that inflammation and tissue damage generate mediators that control the local concentration of NGF-β. Inflammatory cytokines such as IL-1, TNF-alpha and IL-6 are able to modify the basal production of NGF-β in the organism and induce the synthesis of NGF-β in a variety of cell types and tissues [10].
However, there have been few studies [21] on the correlation between the NGF-β/TrkA system and inflammation in patients with primary Sjögren’s syndrome (pSS), a chronic, systemic inflammatory autoimmune disorder primarily targeting the salivary and lachrymal glands [22]. Changes have been demonstrated in circulating levels of neuropeptides and neurotrophins, as well as the impairment of salivary gland innervation in patients with SS [23–25]. These changes are hypothesized to be a cause of a decreased salivary fluid flow during SS. One possible explanation is that this autoimmune disease and/or local inflammation may cause vasoneural dysregulation and injury to the peripheral nerves, leading to a decreased fluid flow and atrophy of the acinar cells [26–28]. Lee et al. recently showed an increase in NGF-β tear levels in patients with dry eye [29], in line with the well-known neural sensitizing role of this neuromediator and with the observations published by Lambiase et al. [30]. These observations suggested that NGF-β may be involved more in local tissue damage than in the disease pathogenesis [30].
There is increasing concern that the NGF-β/TrkA system may play an important functional role in mediating the activation of the EGFR/Raf-1/MEK/ERK signalling pathway [31], strengthening the hypothesis that NGF may be involved in the inflammatory response. The activation of the NGF-β/TrkA system is known to lead to a cascade of intracellular events that trigger the activation of Raf-1. Raf-1 phosphorylates and activates MEK. MEKs phosphorylate MAPKs/ERK1/2 that translocate into the nucleus regulating the expression of NGF-β-inducible genes and contributing to NGF-β activity [31].
The aim of this study was to evaluate the correlation between the NGF-β/TrkA system and the EGFR/Raf-1/MEK/ERK pathway in pSS minor salivary gland (MSG) biopsies using pSS salivary gland epithelial cells (SGEC) cultures as an experimental model of pSS.
Materials and methods
Patient population
pSS MSG biopsies were classified in four inflammation grades (SS-I, low; SS-II, mild; SS-III, intermediate; and SS-IV, advanced MSG lesions) and correlated with the histological focus score [32]. Grade I is characterized by a slight infiltrate, grade II by a moderate infiltrate or less than one focus, grade III by one focus and grade IV by more than one focus, where a focus is defined as an aggregate of 50 or more lymphocytes and histiocytes per 4 mm2 of salivary tissue. The same number of cases were assigned to each group (n = 8). Healthy subjects (n = 12), analysed for an abnormal salivary function and suspected Sjögren’s syndrome but whose biopsy and other diagnostic tests were normal, were enrolled as controls. Participants gave informed consent to the study that follows the tenets of the Declaration of Helsinki and was approved by the local Ethical Committee. Labial MSG were harvested according to the explant outgrowth technique [33]. Patients were confirmed to have definite disease according to the revised 2002 American-European criteria [32, 34]. pSS patients’ characteristics are summarized in Table 1. Biopsy samples were used to obtain primary cultures of SGEC, to extract RNA and proteins, and for immunohistochemical experiments.
SGEC culture
SGEC were isolated from the MSG by microdissection and collagenase (Millipore, Freehold, NJ, USA) digestion and re-suspended in McCoy’s 5a modified medium [10 % FBS, 1 % antibiotic solution, 2 mM l-glutamine, 50 ng/ml EGF (Promega, Madison, WI), 0.5 μg/ml insulin (Novo, Bagsvaerd, Denmark)] and incubated at 37 °C, 5 % CO2 in air. EDTA (0.02 %) was used to remove contaminating fibroblasts. The epithelial origin of cultured cells was confirmed by staining against epithelial-specific markers [35].
Cells treatment
To measure NGF-β release, 1 × 106 (cells/well) healthy SGEC were incubated with TNF-α [5–20 ng/ml] and with IL-6 [10–50 ng/ml] for 24–48 h in the presence or absence of cycloheximide [500 nM] (Sigma-Aldrich, St. Louis, MO, USA). To evaluate the effects of EGF on NGF-β release, healthy SGEC were incubated with or without TNF-α [5–20 ng/ml] or IL-6 [10–50 ng/ml] in the presence or absence of exogenously added EGF [50 ng/ml] for 48 h. To identify the transduction pathway involved in the NGF-β secretion, SGEC were treated with MAPK/ERK inhibitor PD98059 [1–4 μM] and Raf-1 inhibitor GW5074 [1–50 nM] (Sigma-Aldrich).
mRNA expression analysis
Total RNA was extracted from healthy and pSS SGEC, reverse transcribed and cDNA preparation was used for each semi-quantitative RT-PCR and real-time PCR as previously described [36]. Methods are described in detail in the Supplementary Materials and Methods. The primers and probes used are reported in Table 2.
Western blot
Protein lysates were subjected to SDS-PAGE. Membranes were incubated with mouse anti-human NGF-β pAb, rabbit anti-human phospho-TrkA pAb (both from R&D systems, Minneapolis, MN, USA), mouse anti-human ERK1/ERK2 mAb or mouse anti-human phospho-ERK1/ERK2 mAb (both from R&D systems) as first antibodies. Tween-20-diluted secondary antibodies (anti-mouse and rabbit) were IRDye labelled (680/800CW) (LI-COR Biosciences, Lincoln, NE, USA). The Li-cor Odyssey infrared imaging system was used (LI-COR). Imaging densitometry was performed using Quantity One Software (Bio-Rad Laboratories) and compared with β-actin. The data are expressed as optical density × mm2.
FACS analysis
Healthy and SS SCEC (SS-I, low; SS-II, mild; SS-III, intermediate; and SS-IV, advanced MSG inflammatory lesions) were incubated with mouse anti-human NGF-β pAb, rabbit anti-human phospho-TrkA pAb (both from R&D systems) and with secondary antibodies conjugated with Alexa fluor 488 (Life Technologies, Carlsbad, CA, USA). For the NGF-β and TrkA expression analysis, cells were Fc-blocked by treatment with human IgG (R&D Systems) prior to staining. The protein expression was analysed by a Becton Dickinson (BD, Becton Dickinson, Germany) FACSCanto™ II flow cytometer and BD FACS Diva software. Values are given as percentages of positive cells and the MFI is reported.
Immunohistochemistry and immunofluorescence
Healthy and pSS formalin-fixed, paraffin-embedded tissue sections were submitted to immunohistochemistry and double immunofluorescence analysis for human NGF-β and human phospho-TrkA. Methods are described in detail in the Supplementary Materials and Methods.
Determination of NGF-β levels
NGF-β protein concentrations in the culture medium were quantified using the NGF-β Emax ImmunoAssay system kit (Promega, Madison, WI, USA), which typically exhibits less than 3 % cross-reactivity with other neurotrophic factors, following the manufacturer’s instructions. Absorbance was measured on a VERSAmax microplate reader (Molecular Devices Corp, Silicon Valley, CA, USA).
siRNA
The EGFR siRNA duplexes were chemically synthesized and purified by Ambion (Ambion, Austin, TX, USA). Treated healthy SGEC and pSS SGEC were transfected with siRNAs using the siPORT NeoFX transfection agent (Ambion) according to the manufacturer’s instructions. Scrambled siRNA (SCR-siRNA) were used as negative control groups.
Statistics
Analysis of variance (ANOVA) was performed and Mann–Whitney U test, Student’s t test and Spearman’s correlation were applied. Values of P < 0.05 were considered statistically significant.
Results
NGF-β and TrkA expression in pSS SGEC
The expression of NGF-β and TrkA genes in healthy and pSS SGEC primary cultures and the possible correlation with the different grades of pSS MSG inflammatory lesions (SS-I to SS-IV) were examined. Figure 1a, b shows that gene transcripts for NGF-β and TrkA were detected in healthy and pSS SGEC. As depicted, a clear up-regulation of NGF-β and TrkA genes expression was observed that was positively correlated with the pSS MSG inflammation grade. The NGF-β/GAPDH ratio ranged from about 0.98 ± 0.25-fold to about 3.2 ± 0.34-fold, proceeding from low to advanced inflammatory lesions. A similar correlation pattern of gene expression was observed for the TrkA gene (the TrkA/GAPDH ratio ranged from 0.89 ± 0.14-fold to about 3.07 ± 0.53-fold, proceeding from inflammation grades I to IV). At Spearman’s correlation analysis, the NGF-β gene expression increase was progressive, greater expression being correlated with a more advanced inflammatory activity grade in pSS (r = 0.728, P = 0.0087) and TrkA gene expression was found to be positively correlated with the MSG inflammatory status (r = 0.689, P = 0.0098). Real-time gene expression analysis of NGF-β (1.01 ± 0.12 for low grade inflammatory lesions to 3.32 ± 0.33 for high grade, P = 0.0045), and TrkA (0.98 ± 0.18 for low grade inflammatory lesions to 3.27 ± 0.48 for high grade, P = 0.0065), was markedly up-regulated in SGEC from pSS biopsies and this increase was correlated with the disease severity (Fig. 1c). At protein level, in SGEC from the pSS groups, the NGF-β and p-TrkA expression ranged from low to high according to the degree of chronic inflammation (Fig. 1d, e). Spearman’s correlation analysis showed a statistically significant association of NGF-β and p-Trk-A levels with the inflammation severity of the pSS disease (r = 0.698, P = 0.0057 and r = 0.623, P = 0.0061, respectively). Flow cytometry (Fig. 1f) confirmed these results; in fact, the percentage of NGF-β+ pSS SGEC was significantly higher in inflammation grade IV (99.6 % ± 1.7) than in grades III–I [III = 82.4 % ± 1.43, II = 75.3 % ± 1.52, I = 63.7 % ± 1.23, or in healthy SGEC (53.6 % ± 1.87); P = 0.027, P = 0.0073]. In addition, an increased expression of the p-TrkA receptor occurs in pSS SGEC that was found to be associated with an exacerbated inflammatory reaction (grade IV = 97.4 % ± 1.89, III = 85.5 % ± 2.23, II = 73.8 % ± 1.83, I = 66.3 % ± 1.52, and healthy SGEC = 48.7 % ± 1.98). A rapid increase in NGF-β MFI is evident (Fig. 1g), ranging between approximately 410 ± 25.6 and 3,187 ± 123.6, and for p-TrkA between 350 ± 43.8 and 3,015 ± 134.1, proceeding from low to high grade inflammation (r = 0.765, P = 0.0011 and r = 0.711, P = 0.0024).
Analysis of NGF-β/TrkA system expression in pSS SGEC. The NGF-β/TrkA system expression increases with the severity of MSG inflammatory lesions. a Levels of NGF-β and TrkA expression were analysed by RT-PCR on mRNA extracted from healthy and pSS SGEC (MSG inflammation grades I–IV). M = marker, C = healthy SGEC. GAPDH served as an internal control for amplification. Results presented are from one experiment but representative of three independent experiments. b NGF-β and TrkA gene expression levels were quantified by densitometric analysis (n = 3). c Real-time PCR analysis of NGF-β and TrkA gene expression in healthy and pSS SGEC (MSG inflammation grades I–IV) (n = 4). d Representative Western blot of proteins extracted from healthy and pSS SGEC (MSG inflammation grades I–IV) showing NGF-β and p-TrkA expression levels. β-Actin was used as loading control. C = healthy SGEC. All protein isolations and Western blots were repeated a minimum of three times. e NGF-β and p-TrkA protein levels were quantified by densitometry (n = 3). f Levels of NGF-β and p-TrkA expression on healthy and pSS SGEC (MSG inflammation grades I–IV) were measured by flow cytometry. Examples of flow cytometric images from one representative experiment. Negative controls represent cells stained only with secondary antibody g Percentage of healthy and pSS SGEC that resulted positive for NGF-β and p-TrkA, expressed as MFI (results represent mean ± S.E. of triplicate samples). *P < 0.05, ** P < 0.01
NGF-β/TrkA expression in pSS biopsies
As shown in Fig. 2, the patterns of staining were highly consistent within the same inflammation grade sections studied. Panels b–e show that the ductal structures of the pSS MSG showed cytoplasmic staining for NGF-β that resulted strongest in the SS-IV biopsies. In the pSS MSG, very few NGF-β-stained nuclei were seen in the ducts and cytoplasmic staining for NGF-β was very weak or absent in serous or mucous acini. For TrkA (panels g–j), basically, the serous or mucous acini in all the pSS MSG were unreactive, although occasionally a low or intermediate TrkA immunoreaction was observed. By contrast, the cells of the ductal system displayed a high TrkA positivity, with a variable intensity that increased with the inflammation grade. This was observed in the intercalated, striated and excretory ducts as well as in the serous demilunes. Immunostaining was both membranous and cytoplasmic, and was more intense at the basal pole of the cells. A striking feature observed in all sections was that several scattered, solitary cells in the connective tissue, with a morphology resembling that of leukocytes, fibroblasts and endothelial cells, expressed NGF-β. The staining intensity of solitary cells was far more pronounced for NGF-β than for TrkA. The immunofluorescence signal revealed that the pattern of distribution of NGF-β and TrkA was fairly homogeneous, although slight differences were noted between glands (Fig. 2o–r). NGF-β proteins (red staining) were widespread in the cytoplasm of both the intercalated and striated ducts but not in the serous or mucous acinar cells. The expression pattern of TrkA (green staining) was consistent with the immunohistochemistry results (Fig. 2o–r).
Immunohistochemical and double immunofluorescence staining for NGF-β and TrkA of MSG sections from pSS patients. Healthy and pSS formalin-fixed, paraffin-embedded tissue sections (classified as SS-I to SS-IV inflammatory lesions) were used for immunohistochemical and double immunofluorescence confocal microscopy analysis and stained with the indicated antibodies. Scale bar, 20 μm. a, f, n Healthy controls for immunohistochemical and immunofluorescence analysis. b–e SS-I to SS-IV MSG, respectively (×200), anti-NGF-β, brown; counterstaining with hematoxylin. g–j SS-I to SS-IV MSG, respectively (×200), anti-p-TrkA, brown; counterstaining with hematoxylin. k Magnification (×400) of panel d, SS-III, anti-NGF-β, brown. l, m Magnifications (×400) of panels e and j, SS-IV, anti-NGF-β, and anti-TrkA, respectively, brown. o–r SS-I to SS-IV MSG, respectively (×400), anti-NGF-β, red; anti-p-TrkA, green; nuclear counterstaining was performed by TO-PRO-3 iodide, blue. s, t Magnifications (×600) of MSG from SS-IV, anti-NGF-β, red; anti-p-TrkA, green. u, v Negative controls without primary antibodies (anti-NGF-β and anti-TrkA, respectively). w, x Isotype controls with similarly labelled, non-specific primary antibodies
Inflammatory cytokines regulate NGF-β/TrkA signalling
Healthy SGEC constitutively secreted low amounts of NGF-β without any stimulation. The secretion was dose-dependently increased by TNF-α; the stimulatory effect of TNF-α manifested at 5 ng/ml and was maximal at 20 ng/ml, which is 3.3-fold the basal secretion level (Fig. 3a). Similar results were obtained with IL-6 addition that resulted dose-dependent from 10 to 50 ng/ml (Fig. 3b). The NGF-β levels produced by cultured pSS SGEC were comparable to those secreted by healthy SGEC treated with the maximum concentrations of TNF-α and IL-6 (Fig. 3a, b). When quantifying relative mRNA levels in TNF-α/IL-6-treated healthy SGEC (Fig. 3c), a remarkably increase of NGF-β mRNA levels (P = 0.0041) was detected that resulted correlated with the level observed in SGEC from pSS-IV. These results were in agreement with those obtained by flow cytometry (Fig. 3d). The increased TrkA expression after treatment with TNF-α or IL-6 in healthy SGEC was also visualized by flow cytometry, inducing similar levels of expression to those in pSS-IV SGEC (Fig. 3e). The protein biosynthesis inhibitor cycloheximide decreased the NGF-β secretion by TNF-α- or IL-6-treated healthy SGEC and pSS-IV SGEC, indicating that the enhanced secretion is accompanied by protein synthesis (Fig. 3f). We next treated the pSS SGEC cultures with TNF-α and IL-6 and evaluated the NGF-β release. As shown in Fig. 4a–e, an increased production of NGF-β was observed in all grades of pSS SGEC, resulting in exacerbation in the highest grades of inflammation.
Effects of inflammatory cytokines on NGF-β secretion from healthy SGEC. Exposure to pro-inflammatory cytokines activates TrkA receptors and determines NGF-β secretion by healthy SGEC. a, b Healthy SGEC were incubated with the indicated concentrations of TNF-α and IL-6, respectively. The culture medium was assayed for NGF-β secretion. The results shown are the mean ± S.E. of triplicate cultures of three separate experiments. c Real-time PCR analysis of NGF-β gene expression in healthy SGEC treated with TNF-α [20 ng/ml] and IL-6 [50 ng/ml] compared with pSS SGEC, inflammation grade IV (SS-IV). C = healthy SGEC. d Levels of NGF-β expression on healthy SGEC treated with TNF-α [20 ng/ml] and IL-6 [50 ng/ml], measured by flow cytometry. Examples of flow cytometric images from one representative experiment. e Flow cytometry of p-TrkA expression on healthy SGEC treated with TNF-α [20 ng/ml] and IL-6 [50 ng/ml]. Examples of flow cytometric images from one representative experiment. Negative controls represent cells stained only with secondary antibody f Healthy and pSS (IV) SGEC were pre-incubated with cycloheximide (500 nM), subsequently TNF-α [20 ng/ml] and IL-6 [50 ng/ml] were added to the cultures and ELISA for NGF-β secretion was performed. Values are each the mean ± S.E. of triplicate cultures of four independent experiments. *P < 0.05, **P < 0.01
Effects of TNF-α and IL-6 treatment on NGF-β secretion from pSS SGEC. a, b pSS (inflammation grades I–IV) SGEC were incubated with TNF-α [20 ng/ml] and IL-6 [50 ng/ml] and the culture medium was assayed for NGF-β secretion. The results shown are the mean ± S.E. of triplicate cultures of three separate experiments. c, d Levels of NGF-β expression on pSS SGEC I–IV treated with TNF-α [20 ng/ml] and IL-6 [50 ng/ml], measured by flow cytometry. Examples of flow cytometric images from one representative experiment. Negative represents cells stained only with secondary antibody e Real-time PCR analysis of NGF-β gene expression in pSS SGEC I–IV treated as described above. Values are the mean ± S.E. of triplicate cultures of four independent experiments. **P < 0.01
Involvement of the MEK/ERK pathway in NGF-β secretion
We explored whether the release of NGF-β following pro-inflammatory cytokines treatment can be modulated by interrupting signalling of the MEK/ERK pathway. As shown in Fig. 5a, b, when healthy SGEC, stimulated with TNF-α and IL-6, were treated with the MAPK inhibitor PD98059, which selectively blocks ERK activity via inhibiting ERK1/2 phosphorylation by MEK1/2, the NGF-β secretion was reduced to basal levels at the inhibitory concentration of 2.0 μM, and completely inhibited at 4.0 μM. As shown in Fig. 5c, the NGF-β secretion by pSS-IV SGEC was likewise susceptible to inhibition by PD98059 treatment (P = 0.0056). As shown in Fig. 5d, ERK1/2 phosphorylation was significantly enhanced by TNF-α/IL-6 treatment and ERK1/2 activation also occurred in pSS-IV SGEC. We next examined whether Raf-1 kinase, involved in the upstream portion of the MEK/ERK pathway, is a regulatory step in the TNF-α/IL-6-activation of the MEK/ERK pathway that leads to NGF-β secretion by SGEC. We determined the effects of GW5074, a known inhibitor of Raf-1 kinase, on the cytokines-induced NGF-β secretion. Pretreatment of healthy SGEC with increasing doses of GW5074 [1–50 nM] inhibited the TNF-α/IL-6-determined NGF-β secretion, in a dose-dependent manner (Fig. 5e, f). On pSS-IV SGEC, we observed similar inhibitory effects of GW5074 on NGF-β secretion (Fig. 5g).
Effects of typical MEK inhibitor (PD98059) and Raf-1 inhibitor (GW5074) on NGF-β secretion. Specific inhibitors of the Raf-1/MEK/ERK pathway block NGF-β secretion by TNF-α/IL-6-treated healthy SGEC and pSS SGEC. a, b Healthy SGEC were pre-incubated with the indicated concentrations of PD98059 and then cultured with TNF-α [20 ng/ml] or IL-6 [50 ng/ml] for 24 h in the presence of the inhibitor. The culture medium was assayed for NGF-β secretion and protein lysates were used to perform the corresponding Western blot analysis. Values are the mean ± S.E. of triplicate cultures of three independent experiments. c pSS SGEC (SS-IV) were pre-incubated with the indicated concentrations of PD98059 for 24 h. The culture medium was assayed for NGF-β secretion. Values are the mean ± S.E. of triplicate cultures of three independent experiments. d The effects of TNF-α and IL-6 treatment on ERK1/2 phosphorylation visualized by Western blot. The levels of phosphorylated ERK1/2 (upper panel) and total ERK1/2 (lower panel) were analysed in healthy SGEC, treated with 20 ng/ml TNF-α and 50 ng/ml IL-6, and in pSS SGEC (SS-IV). Similar results were obtained in two independent experiments. Quantification of ERK1/2 phosphorylation was done by Quantity One Software and compared with β-actin. e, f Healthy SGEC were pre-incubated with the indicated concentrations of GW5074 and then cultured with TNF-α [20 ng/ml] or IL-6 [50 ng/ml] in the presence of the inhibitor. The culture medium was assayed for NGF-β secretion and protein lysates were used to perform the corresponding Western blot. Values are the mean ± S.E. of triplicate cultures of three independent experiments. g pSS SGEC (SS-IV) were pre-incubated with the indicated concentrations of GW5074 for 24 h. NGF-β secretion was evaluated by ELISA. Values are the mean ± S.E. of triplicate cultures of three independent experiments. *P < 0.05, **P < 0.01
EGF/EGFR system is necessary for the TNF-α/IL-6-enhanced NGF-β secretion in SGEC
Healthy SGEC were incubated with or without TNF-α or IL-6, in the presence or not of EGF, to examine whether EGF directly regulated the TNF-α/IL-6-dependent NGF-β release. As shown in Fig. 6a, b, EGF dose-dependently induced NGF-β secretion by healthy SGEC and the secretion was enhanced by the addition of TNF-α or IL-6. As shown in Fig. 6c, d, pretreatment with PD98059 and GW5074 significantly inhibited the NGF-β secretion induced by TNF-α or IL-6 + EGF (P = 0.0081; P = 0.0071). We next examined the effects of EGFR gene knockdown on ERK1/2 phosphorylation in TNF-α- or IL-6-treated healthy SGEC and pSS-IV SGEC under full serum growth conditions. The knockdown ratios for the TNF-α- or IL-6-treated healthy SGEC and pSS-IV SGEC were in the same range: 86, 88 and 88 %, respectively, and highly statistically significant (P = 0.0058). EGFR expression in the cells transfected with EGFR-specific siRNAs was strongly reduced as compared to the negative control scrambled siRNAs that had no effect (Fig. 6e). The levels of phospho-ERK1/2 in TNF-α- or IL-6-treated healthy SGEC and pSS-IV SGEC transfected with EGFR siRNAs were analysed by immunoblotting (Fig. 6f). As shown, a decreased phosphorylation of ERK1/2 was observed. Then, we assessed whether the depletion of EGFR determined changes in the NGF-β levels in TNF-α- or IL-6-treated healthy SGEC and pSS-IV SGEC. As shown in Fig. 6g, e, g, r, f, gene knockdown dramatically reduced NGF-β release as compared with scrambled siRNAs-transfected control cells.
EGF/EGFR system activation is necessary for NGF-β secretion. EGF-induced NGF-β expression is mediated through the EGFR/Raf-1MEK/ERK pathway in SGEC. a, b Healthy SGEC were pre-incubated for 12 h in EGF-free medium and then treated with TNF-α [20 ng/ml] or IL-6 [50 ng/ml] in the presence of EGF [0–50 ng/ml] for 24 h. NGF-β release was evaluated by ELISA. Values are the mean ± S.E. of triplicate cultures of three independent experiments. c, d Healthy SGEC were pretreated with PD98059 and GW5074, in the presence of EGF [50 ng/ml]. The cultures were treated with TNF-α [20 ng/ml] or IL-6 [50 ng/ml] in the presence of the inhibitors (histograms PD and GW). The culture supernatants were assayed for NGF-β secretion by ELISA and Western blot. Histogram EGF: healthy SGEC cultured in the medium containing EGF without any inhibitors. Histogram C: healthy SGEC treated with TNF-α [20 ng/ml] or IL-6 [50 ng/ml] in the absence of inhibitors. Values are the mean ± S.E. of triplicate cultures of three independent experiments. *P < 0.05, **P < 0.01. e Effects of EGFR gene knockdown on NGF-β gene expression in TNF-α- or IL-6-treated healthy SGEC and pSS SGEC (inflammation grade IV) under full serum growth conditions. After 48 h transfection with either scrambled siRNA (SCRsiRNA) or EGFR-specific siRNA (EGFRsiRNA), NGF-β mRNA expression was analysed by RT-PCR. M = marker. GAPDH served as an internal control for amplification. Results presented are from one experiment and are representative of three independent experiments. f After 48 h transfection with SCRsiRNA or EGFRsiRNA, phospho-ERK1/2 levels in TNF-α- or IL-6-treated healthy SGEC and pSS SGEC was revealed by immunoblotting. Results presented are from one experiment and are representative of three independent experiments. g ELISA of NGF-β protein expression in healthy SGEC and pSS-IV SGEC transfected with SCRsiRNA or EGFRsiRNA and treated with TNF-α or IL-6. Values are the mean ± S.E. of triplicate cultures of three independent experiments. *P < 0.05, **P < 0.01
Discussion
An enhanced production of NGF-β has been reported in inflamed tissues of patients with inflammatory and autoimmune diseases [37], but the reasons why the NGF-β concentration is enhanced and how this can affect inflammatory responses are not yet fully understood. The expression of the signal-transducing NGF-β receptor TrkA demonstrated in several non-nervous cells such as keratinocytes [38] and melanocytes [39] further strengthens the notion that a locally increased expression of the NGF-β/TrkA system might stimulate the release of inflammatory mediators. Earlier reports suggested that NGF-β may influence the proliferative and inflammatory cascades in various diseases, directly by regulating local pathologic events, such as the proliferation of target tissues, promotion of angiogenesis and induction of inflammatory responses, and/or suggested that NGF-β might act indirectly by modulating the synthesis of neuropeptides which, in turn, induce the inflammatory reaction [2]. In the series of experiments described herein, we found that NGF-β synthesis is up-regulated in SGEC from pSS inflamed salivary glands and its synthesis is enhanced after stimulation with pro-inflammatory cytokines. NGF-β acts via its high affinity receptor TrkA on SGEC, key pathologic cells in the inflammatory and proliferative cascades involved in autoimmune pSS. The study focused on pSS SGEC since accumulating data provide support for the role of epithelia in the constitutive or inducible expression of various molecules that are implicated in innate and acquired immune responses [40]. The epithelial cells in the glandular lesions of SS are capable of producing factors directing the chemoattraction of lymphocytes and promoting chronic inflammatory reactions. This evidence supports the proposed definition of Sjögren’s syndrome as an “autoimmune epithelitis” [41]. Immunohistochemical analysis of inflamed salivary gland tissues of SS patients has indicated that ductal and acinar SGEC display high levels of several immunoactive molecules that are known to mediate lymphoid cell homing, antigen presentation, and an increased production of the pro-inflammatory cytokines has been demonstrated in several studies of SS patients [40, 41].
The NGF-β/TrkA system expression was shown to be correlated with the degree of salivary gland injury and the inflammatory changes in pSS. A particularly interesting observation was that in pSS, the salivary gland NGF-β/TrkA expression levels were found to be significantly increased from low grade to advanced inflammation, and the number of NGF-β+/TrkA+ pSS SGEC was positively correlated with the MSG biopsy focus score. This study was focused on human SGEC since a large volume of literature data in this field reveals the functional participation of these cells during the time course of the immune response in pSS. SGEC appear to be suitably equipped to participate in various aspects of inflammation, including the recruitment and activation of immune cells, and manifest an intriguingly high expression of various immunoactive factors, a fact that strongly suggests the operation of an intrinsic activation mechanism in these cells [42–54]. As yet, the molecular events underlying the involvement of SGEC in exacerbating the chronic inflammatory condition observed in pSS have not been extensively studied, and one question that needs to be answered is what mechanism underlies the correlation between an abnormal expression of the NGF-β/TrkA system and the inflammatory grade in pSS SGEC.
Since pSS is characterized by a dysregulated cytokines production [45–47, 53, 54] and cytokines are strong inducers of NGF-β synthesis [55, 56], we investigated the stimulatory effects of the pro-inflammatory cytokines TNF-α and IL-6 on SGEC from healthy and pSS subjects to mimic the inflammatory environment characteristic of pSS. As expected, these experiments demonstrated that NGF-β/TrkA system expression is significantly enhanced after stimulation with TNF-α and IL-6 both in healthy and in I–IV pSS SGEC, confirming that the elevated expression can be induced by addition of the pro-inflammatory cytokines TNF-α and IL-6. This fact suggests that a strong link may exist between the secretion of cytokines by inflammatory and epithelial cells and the modulation of NGF-β production in the inflamed salivary glands. This finding corroborates previous reports showing that TNF-α and IL-6 regulate NGF-β production from different cell types and tissues [55, 56]. So far, however, there has been little discussion about the signal transduction required to produce NGF-β as a mediator of inflammation. Our study reveals that the TNF-α/IL-6-enhanced NGF-β production in pSS is mediated via the Raf-1/MEK/ERK cascade that has already been demonstrated to be a common mediator of effects induced by IL-6 [57, 58] and TNF-α [58, 59].
We also attempted to identify the mechanism through which the inflammatory condition characterizing pSS boosts NGF-β expression. We verified whether the release of NGF-β can be modulated or inhibited by interrupting signalling of the MEK/ERK pathway. Pretreatment of healthy SGEC with PD98059, which selectively blocks ERK activity, impeded NGF-β secretion in response to pro-inflammatory cytokines stimulation. These data were consistent with the results observed in cultured pSS SGEC, in which the NGF-β secretion was similarly susceptible to inhibition by PD98059 treatment. Therefore, we sought to determine whether Raf-1 kinase activation is a regulatory step in NGF-β release by pro-inflammatory cytokines-treated healthy SGEC through the Raf-1/MEK/ERK pathway, and to establish whether Raf-1 activation also occurs in pSS SGEC. We determined the effects of GW5074, a known inhibitor of Raf-1 kinase, on NGF-β production following TNF-α/IL-6 treatment of healthy SGEC. The data obtained place Raf-1 upstream of the MEK/ERK pathway that leads to NGF-β secretion and further support the potential involvement of this pathway in the pro-inflammatory role of NGF-β. Similar results were observed for GW5074-treated pSS SGEC, supporting the possibility that pSS-related inflammation is linked to an increased NGF-β expression and, although preliminary, support a model in which NGF-β, produced through the activation of the MEK/ERK pathway, plays a key role in the pathogenesis of pSS.
Since ERK1/2 phosphorylation is dependent on EGFR activation, which then leads to downstream Raf-1 and MEK activation, we then explored whether the EGF/EGFR system cooperates in promoting NGF-β release by pSS SGEC. An augmented expression of the EGF/EGFR system has been noted in biopsied salivary gland samples from SS patients [60]. Recently, several authors demonstrated that the EGF/EGFR system leads to the activation of intracellular kinase cascades such as the phosphatidylinositol 3-kinase (PI3K)-Akt and IkappaB kinase (IKK)-nuclear factor kappaB (NF-κB) pathways [61–64], both of which are well known anti-apoptogenic survival signals [65]. In addition, Nakamura et al. demonstrated that EGF-mediated activation of both PI3K-Akt and IKK-NF-κB is functionally anti-apoptogenic in SS and represents a defence mechanism of epithelial restoration [66]. The Raf-1/MEK/ERK cascade is one of the major and best studied EGFR downstream pathways, which links extracellular signals to the regulation of various cellular behaviours [67, 68]. The possible role of the EGF/EGFR system in the regulation of TNF-α/IL-6-dependent NGF-β secretion in pSS SGEC was therefore examined. We demonstrated that additional TNF-α or IL-6 treatment enhanced NGF-β release by healthy SGEC and, when the Raf-1/MEK/ERK pathway was perturbed using the specific pharmacological MEK and Raf-1 inhibitors, the EGF-dependent NGF-β production was negatively modulated. This would identify EGF as a key molecule in the NGF-β production dependence on the Raf-1/MEK/ERK pathway activation. Interestingly, EGFR-specific gene knockdown caused a substantial reduction in the levels of phosphorylated ERK1/2 and NGF-β in TNF-α- and IL-6-treated healthy SGEC, validating the results obtained with the pathway inhibitors. This prompted us to test whether EGFR activates ERK1/2 phosphorylation and NGF-β production also in pSS SGEC, and we found that EGFR gene silencing inhibited ERK1/2 phosphorylation and NGF-β secretion almost equally in TNF-α/IL-6-treated healthy SGEC and in pSS SGEC. Based on our findings, a possible scheme for the Raf-1/MEK/ERK-enhanced NGF-β production in pSS SGEC is shown in Fig. 7.
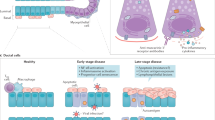
Schematic model of EGFR/Raf-1/MEK/ERK pathway-dependent NGF-β release in pSS SGEC. In pSS SGEC, the chronic inflammatory condition, reflected by the increased levels of the pro-inflammatory cytokines TNF-α and IL-6, determines NGF-β production, mediated through an EGFR-dependent activation of the Raf-1/MEK/ERK pathway
In conclusion, our study suggests a hypothetical scenario in which pro-inflammatory cytokines secreted by infiltrating lymphocytes and pSS SGEC enhance NGF-β production via the EGFR/Raf-1/MEK/ERK pathway in human pSS SGEC, exacerbating the chronic inflammatory condition characterizing pSS disease. These data suggest that modulation of the NGF/EGFR/Raf-1/MEK/ERK pathway may be a plausible strategy for therapeutic intervention to reduce the damaging effects of inflammation in pSS. The results of this work do not resolve the key question of whether NGF is neuroprotective, pro-inflammatory or anti-inflammatory in pSS. Many studies have suggested an intimate correlation between systemic NGF-β concentrations and disease activity, and NGF-β appears to act as a pro-inflammatory neurokine in addition to its neurotrophic effects, even if considerable evidence also points to a protective and regenerative effect of NGF in some diseases. Therefore, depending on the disease and the pathological mechanisms involved, recombinant NGF-β or its antagonists may offer an opportunity for novel therapeutic approaches to inflammatory diseases. The inclusion of regimens targeting neurogenic inflammation is of importance in cases with refractory disease and/or of serious side effects arising with conventional immunosuppressants.
References
Barker PA, Murphy RA (1992) The nerve growth factor receptor: a multicomponent system that mediates the actions of the neurotrophin family of proteins. Mol Cell Biochem 110:1–15
Aloe L, Skaper SD, Leon A, Levi-Montalcini R (1994) Nerve growth factor and autoimmune diseases. Autoimmunity 19:141–150
Aloe L, Tuveri MA, Carcassi U, Levi-Montalcini R (1992) Nerve growth factor in the synovial fluid of patients with chronic arthritis. Arth Rheum 35:351–355
Bracci-Laudiero L, Aloe L, Levi-Montalcini R, Galeazzi M, Schilter D, Scully JL, Otten U (1993) Increased levels of NGF in sera of systemic lupus erythematosus patients. NeuroReport 4:563–565
Aalto K, Korhonen L, Lahdenne P, Pelkonen P, Lindholm D (2002) Nerve growth factor in serum of children with systemic lupus erythematosus is correlated with disease activity. Cytokine 20:136–139
Safieh-Garabedian B, Poole S, Allchorne A, Winter J, Woolf CJ (1995) Contribution of interleukin-1 beta to the inflammation-induced increase in nerve growth factor levels and inflammatory hyperalgesia. Br J Pharmacol 115:1265–1275
Manni L, Aloe L (1998) Role of IL-1 beta and TNF-alpha in the regulation of NGF in experimentally induced arthritis in mice. Rheumatol Int 18:97–102
Bracci-Laudiero L, Lundeberg T, Stenfors C, Theodorsson E, Tirassa P, Aloe L (1996) Modification of lymphoid and brain nerve growth factor levels in systemic lupus erythematosus mice. Neurosci Lett 204:13–16
De Simone R, Micera A, Tirassa P, Aloe L (1996) mRNA for NGF and p75 in the central nervous system of rats affected by experimental allergic encephalomyelitis. Neuropathol Appl Neurobiol 22:54–59
Seidel MF, Herguijuela M, Forkert R, Otten U (2010) Nerve growth factor in rheumatic diseases. Semin Arthritis Rheum 40:109–126
Lowe EM, Anand P, Terenghi G, Williams-Chestnut RE, Sinicropi DV, Osborne JL (1997) Increased nerve growth factor levels in the urinary bladder of women with idiopathic sensory urgency and interstitial cystitis. Br J Urol 79:572–577
Jacobs BL, Smaldone MC, Tyagi V, Philips BJ, Jackman SV, Leng WW, Tyagi P (2010) Increased nerve growth factor in neurogenic overactive bladder and interstitial cystitis patients. Can J Urol 17:4989–4994
Bonini S, Lambiase A, Bonini S, Angelucci F, Magrini L, Manni L, Aloe L (1996) Circulating nerve growth factor levels are increased in humans with allergic diseases and asthma. Proc Natl Acad Sci U S A 93:10955–10960
Braun A, Appel E, Baruch R, Herz U, Botchkarev V, Paus R, Brodie C, Renz H (1998) Role of nerve growth factor in a mouse model of allergic airway inflammation and asthma. Eur J Immunol 28:3240–3251
Lambiase A, Bonini S, Bonini S, Micera A, Magrini L, Bracci-Laudiero L, Aloe L (1995) Increased plasma levels of nerve growth factor in vernal keratoconjunctivitis and relationship to conjunctival mast cells. Invest Ophthalmol Vis Sci 36:2127–2132
di Mola FF, Friess H, Zhu ZW, Koliopanos A, Bley T, Di Sebastiano P, Innocenti P, Zimmermann A, Büchler MW (2000) Nerve growth factor and Trk high affinity receptor (TrkA) gene expression in inflammatory bowel disease. Gut 46:670–679
Stanzel RD, Lourenssen S, Blennerhassett MG (2008) Inflammation causes expression of NGF in epithelial cells of the rat colon. Exp Neurol 211:203–213
Fantini F, Magnoni C, Bracci-Laudiero L, Pincelli CTE (1995) Nerve growth factor is increased in psoriatic skin. J Invest Dermatol 105:854–855
Raychaudhuri SP, Jiang WY, Farber EM (1998) Psoriatic keratinocytes express high levels of nerve growth factor. Acta Derm Venereol 78:84–86
Toyoda M, Nakamura M, Makino T, Hino T, Kagoura M, Morohashi M (2002) Nerve growth factor and substance P are useful plasma markers of disease activity in atopic dermatitis. Br J Dermatol 147:71–79
Fauchais AL, Boumediene A, Lalloue F, Gondran G, Loustaud-Ratti V, Vidal E, Jauberteau MO (2009) Source brain-derived neurotrophic factor and nerve growth factor correlate with T-cell activation in primary Sjogren’s syndrome. Scand J Rheumatol 38:50–57
Peri Y, Agmon-Levin N, Theodor E, Shoenfeld Y (2012) Sjögren’s syndrome, the old and the new. Best Pract Res Clin Rheumatol 26:105–117
Batbayar B, Nagy G, Kövesi G, Zelles T, Fehér E (2004) Morphological basis of sensory neuropathy and neuroimmunomodulation in minor salivary glands of patients with Sjögren’s syndrome. Arch Oral Biol 49:529–538
Ekström J, Ekman R, Håkanson R, Sjögren S, Sundler F (1988) Calcitonin gene-related peptide in rat salivary glands: neuronal localization, depletion upon nerve stimulation, and effects on salivation in relation to substance P. Neuroscience 26:933–949
Lodde BM, Mineshiba F, Wang J, Cotrim AP, Afione S, Tak PP, Baum BJ (2006) Effect of human vasoactive intestinal peptide gene transfer in a murine model of Sjögren’s syndrome. Ann Rheum Dis 65:195–200
Konttinen YT, Hukkanen M, Kemppinen P, Segerberg M, Sorsa T, Malmström M, Rose S, Itescu S, Polak JM (1992) Peptide-containing nerves in labial salivary glands in Sjögren’syndrome. Arthritis Rheum 35:815–820
Santavirta N, Konttinen YT, Törnwall J, Segerberg M, Santavirta S, Matucci-Cerinic M, Björvell H (1997) Neuropeptides of the autonomic nervous system in Sjögren’s syndrome. Ann Rheum Dis 56:737–740
Fehér E, Zelles T, Nagy G (1999) Immunocytochemical localisation of neuropep-tide-containing nerve fibres in human labial glands. Arch Oral Biol 44:S33–S37
Lee HK, Lee KS, Kim HC, Lee SH, Kim EK (2005) Nerve growth factor concentration and implications in photorefractive keratectomy vs laser in situ keratomileusis. Am J Ophthalmol 139:965–971
Lambiase A, Micera A, Sacchetti M, Cortes M, Mantelli F, Bonini S (2011) Alterations of tear neuromediators in dry eye disease. Arch Ophthalmol 129:981–986
Yan F, John SK, Wilson G, Jones DS, Washington MK, Polk DB (2004) Kinase suppressor of Ras-1 protects intestinal epithelium from cytokine-mediated apoptosis during inflammation. J Clin Invest 114:1272–1280
Vitali C, Bombardieri S, Jonsson R, Moutsopoulos HM, Alexander EL, Carsons SE, Daniels TE, Fox PC, Fox RI, Kassan SS et al (2002) Classification criteria for Sjögren’s syndrome: a revised version of the European criteria proposed by the American-European Consensus Group. Ann Rheum Dis 61:554–558
Sens DA, Hintz DS, Rudisill MT, Sens MA, Spicer SS (1985) Explant culture of human submandibular gland epithelial cells: evidence for ductal origin. Lab Invest 52:559–567
Vitali C, Bootsma H, Bowman SJ, Dorner T, Gottenberg JE, Mariette X, Ramos-Casals M, Ravaud P, Seror R, Theander E et al (2013) Classification criteria for Sjogren’s syndrome: we actually need to definitively resolve the long debate on the issue. Ann Rheum Dis 72:476–478
Kapsogeorgou EK, Abu-Helu RF, Moutsopoulos HM, Manoussakis MN (2005) Salivary gland epithelial cell exosomes: a source of autoantigenic ribonucleoproteins. Arthritis Rheum 52:1517–1521
Sisto M, Lisi S, Lofrumento DD, D’Amore M, Frassanito MA, Ribatti D (2012) Sjögren’s syndrome pathological neovascularization is regulated by VEGF-A-stimulated TACE-dependent crosstalk between VEGFR2 and NF-κB. Genes Immun 13:411–420
Bonini S, Rasi G, Bracci-Laudiero ML, Procoli A, Aloe L (2003) Nerve growth factor: neurotrophin or cytokine? Int Arch Allergy Immunol 131:80–84
Terenghi G, Mann D, Kopelman PG, Anand P (1997) TrkA and trkC expression is increased in human diabetic skin. Neurosci Lett 228:33–34
Flørenes VA, Maelandsmo GM, Holm R, Reich R, Lazarovici P, Davidson B (2004) Expression of activated TrkA protein in melanocytic tumors: relationship to cell proliferation and clinical outcome. Am J Clin Pathol 122:412–420
Manoussakis MN, Kapsogeorgou EK (2007) The role of epithelial cells in the pathogenesis of Sjögren’s syndrome. Clin Rev Allergy Immunol 32:225–230
Moutsopoulos HM (1994) Sjögren’s syndrome: autoimmune epithelitis. Clin Immunol Immunopathol 72:162–165
Sisto M, Lisi S, Castellana D, Scagliusi P, D’Amore M, Caprio S, Scagliusi A, Acquafredda A, Panaro MA, Mitolo V et al (2006) Autoantibodies from Sjögren’s syndrome induce activation of both the intrinsic and extrinsic apoptotic pathways in human salivary gland cell line A-253. J Autoimmun 27:38–49
Manoussakis MN, Tsinti M, Kapsogeorgou EK, Moutsopoulos HM (2012) The salivary gland epithelial cells of patients with primary Sjögren’s syndrome manifest significantly reduced responsiveness to 17β-estradiol. J Autoimmun 39:64–68
Sisto M, D’Amore M, Caprio S, Mitolo V, Scagliusi P, Lisi S (2009) Tumor necrosis factor inhibitors block apoptosis of human epithelial cells of the salivary glands. Ann N Y Acad Sci 1171:407–414
Lisi S, Sisto M, Lofrumento DD, Cucci L, Frassanito MA, Mitolo V, D’Amore M (2010) Pro-inflammatory role of anti-Ro/SSA autoantibodies through the activation of Furin-TACE-amphiregulin axis. J Autoimmun 35:160–170
Sisto M, Lisi S, Lofrumento DD, Caprio S, Mitolo V, D’Amore M (2010) TNF blocker drugs modulate human TNF-α-converting enzyme pro-domain shedding induced by autoantibodies. Immunobiology 21:874–883
Sisto M, Lisi S, Lofrumento DD, Ingravallo G, Mitolo V, D’Amore M (2010) Expression of pro-inflammatory TACE-TNF-α-amphiregulin axis in Sjögren’s syndrome salivary glands. Histochem Cell Biol 134:345–353
Sisto M, Lisi S, Lofrumento DD, Ingravallo G, Maiorano E, D’Amore M (2011) A failure of TNFAIP3 negative regulation maintains sustained NF-κB activation in Sjögren’s syndrome. Histochem Cell Biol 135:615–625
Tzioufas AG, Kapsogeorgou EK, Moutsopoulos HM (2012) Pathogenesis of Sjögren’s syndrome: what we know and what we should learn. J Autoimmun 39:4–8
Lisi S, Sisto M, Lofrumento DD, D’Amore M (2012) Sjögren’s syndrome autoantibodies provoke changes in gene expression profiles of inflammatory cytokines triggering a pathway involving TACE/NF-κB. Lab Invest 92:615–624
Sisto M, Lisi S, Lofrumento DD, D’Amore M, Ribatti D (2012) Neuropilin-1 is upregulated in Sjögren’s syndrome and contributes to pathological neovascularization. Histochem Cell Biol 137:669–677
Voulgarelis M, Tzioufas AG (2010) Pathogenetic mechanisms in the initiation and perpetuation of Sjögren’s syndrome. Nat Rev Rheumatol 6:529–537
Nocturne G, Mariette X (2013) Advances in understanding the pathogenesis of primary Sjögren’s syndrome. Nat Rev Rheumatol 9:544–556
Lisi S, Sisto M, D’Amore M, Lofrumento DD, Ribatti D (2013) Emerging avenues linking inflammation, angiogenesis and Sjögren’s syndrome. Cytokine 61:693–703
Kossmann T, Hans V, Imhof HG, Trentz O, Morganti-Kossmann MC (1996) Interleukin-6 released in human cerebrospinal fluid following traumatic brain injury may trigger nerve growth factor production in astrocytes. Brain Res 713:143–152
Kuno R, Yoshida Y, Nitta A, Nabeshima T, Wang J, Sonobe Y, Kawanokuchi J, Takeuchi H, Mizuno T, Suzumura A et al (2006) The role of TNF-alpha and its receptors in the production of NGF and GDNF by astrocytes. Brain Res 1116:12–18
Hattori A, Iwasaki S, Murase K, Tsujiimoto M, Sato M, Hyashi K, Kohno M (1994) Tumor necrosis factor is markedly synergistic with interleukin1 and interferon gamma in stimulating the production of nerve growth factor in fibroblasts. FEBS Lett 340:177–180
Hideshima T, Podar K, Chauhan D, Anderson KC (2005) Cytokines and signal transduction. Best Pract Res Clin Haematol 18:509–524
Müller G, Storz P, Bourteele S, Döppler H, Pfizenmaier K, Mischak H, Kaiser C, Kolch W (1998) Regulation of Raf-1 kinase by TNF via its second messenger ceramide and cross-talk with mitogenic signaling. EMBO J 17:732–742
Gorgoulis V, Giatromanolaki A, Iliopoulos A, Kanavaros P, Aninos D, Ioakeimidis D, Kontomerkos T, Karameris A (1993) EGF and EGF-R immunoexpression in Sjögren’s syndrome secondary to rheumatoid arthritis. Correlation with EBV expression? Clin Exp Rheumatol 11:623–627
Anest V, Cogswell PC, Baldwin AS Jr (2004) IkappaB kinase alpha and p65/RelA contribute to optimal epidermal growth factor-induced c-fos gene expression independent of IkappaBalpha degradation. J Biol Chem 279:31183–31189
Kitagawa K, Hamada Y, Kato Y, Nakai K, Nishizawa M, Ito S, Okumura T (2004) Epidermal growth factor and interleukin-1beta synergistically stimulate the production of nitric oxide in rat intestinal epithelial cells. Am J Physiol Gastrointest Liver Physiol 287:G1188–G1193
Dhar A, Young MR, Colburn NH (2002) The role of AP-1, NF-kappaB and ROS/NOS in skin carcinogenesis: the JB6 model is predictive. Mol Cell Biochem 234–235:185–193
Navolanic PM, Steelman LS, McCubrey JA (2003) EGFR family signaling and its association with breast cancer development and resistance to chemotherapy (review). Int J Oncol 22:237–252
Viatour P, Merville MP, Bours V, Chariot A (2005) Phosphorylation of NF-kappaB and IkappaB proteins: implications in cancer and inflammation. Trends Biochem Sci 30:43–52
Nakamura H, Kawakami A, Ida H, Koji T, Eguchi K (2007) EGF activates PI3K-Akt and NF-kappaB via distinct pathways in salivary epithelial cells in Sjögren’s syndrome. Rheumatol Int 28:127–136
Dunn KL, Espino PS, Drobic B, He S, Davie JR (2005) The Ras-MAPK signal transduction pathway, cancer and chromatin remodeling. Biochem Cell Biol 83:1–14
Yoon S, Seger R (2006) The extracellular signal-regulated kinase: multiple substrates regulate diverse cellular functions. Growth Factors 24:21–24
Acknowledgments
We are grateful to M.V.C. Pragnell, B.A., for language revision and editing of the manuscript.
Conflict of interest
Authors declare no conflict of interest related to this study.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Lisi and Sisto equally contributed to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 106 kb)
Rights and permissions
About this article
Cite this article
Lisi, S., Sisto, M., Ribatti, D. et al. Chronic inflammation enhances NGF-β/TrkA system expression via EGFR/MEK/ERK pathway activation in Sjögren’s syndrome. J Mol Med 92, 523–537 (2014). https://doi.org/10.1007/s00109-014-1130-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-014-1130-9