Abstract
Hormone-resistant (HR) prostate cancers are highly aggressive and respond poorly to treatment. A better understanding of the molecular mechanisms involved in HR should lead to more rational approaches to therapy. The role of IL-6/STAT3 signaling in the transition of HR with aggressive tumor behavior and its possible link with myeloid-derived suppressor cells (MDSCs) were identified. In the present study, murine prostate cancer cell line (TRAMP-C1) and a hormone-resistant cell sub-line (TRAMP-HR) were used. Changes in tumor growth, invasion ability, and the responsible pathway were investigated in vitro and in vivo. We also examined the role of IL-6 in HR tumor progression and the recruitment of MDSCs. As seen in both in vitro and in vivo experiments, HR had aggressive tumor growth compared to TRAMP-C1. From mRNA and protein analysis, a higher expression of IL-6 associated with a more activated STAT3 was noted in HR tumor. When IL-6 signaling in prostate cancer was blocked, aggressive tumor behavior could be overcome. The underlying changes included decreased cell proliferation, less epithelial–mesenchymal transition, and decreased STAT3 activation. In addition to tumor progression, circulating IL-6 levels were significantly correlated with MDSC recruitment in vivo. Inhibition of IL-6 abrogated the recruitment of MDSCs in tumor- bearing mice, associated with slower tumor growth and attenuated angiogenesis. In conclusion, altered IL-6/STAT3 signaling is crucial in HR transition, aggressive behavior, and MDSC recruitment. These findings provide evidence for therapeutically targeting IL-6 signaling in prostate cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inhibiting androgen receptor (AR) signaling by hormone deprivation therapy is initially effective for prostate cancer, but ultimately leads to a hormone-resistant (HR) phenotype [1, 2]. In the clinic, HR cancers are usually highly aggressive and respond poorly to treatment. A better understanding of the molecular mechanisms involved in HR could provide insight into tumor progression and lead to more rational approaches to therapy.
Several mechanisms are implicated in prostate cancer progression and androgen-independent growth [3–5]. We previously reported [6] that constitutional activation of STAT3 is associated with the transition of HR prostate cancer. IL-6 is a major activator of JAK/STAT3 signaling [7, 8]. Moreover, IL-6 signaling is implicated in the regulation of tumor growth and metastatic spread, and its level could be correlated with a poor prognosis in different cancers [8–10]. Accordingly, we hypothesized that IL-6 might be crucial in tumor progression and androgen-independent growth of prostate cancer.
IL-6 is an important pro-inflammatory cytokine and is recognized as a key regulator of immunosuppression with advanced cancer [7, 8, 11]. Evidence supports the concept that chronic inflammation promotes the development and progression of cancers, and immune suppression could be one of the mechanisms underlying the fact that inflammation facilitates tumor progression [11, 12]. Myeloid-derived suppressor cells (MDSCs), a heterogeneous mixture of immature myeloid cells, was reported to markedly expand in tumor-bearing mice and patients with cancer and contribute to an immunosuppressive tumor microenvironment [13, 14]. The expansions of MDSCs are associated with several inflammatory mediators, and STAT3 is arguably the main transcription factor that regulates the expansion of MDSCs [15]. Therefore, the induction of MDSCs by activated IL-6/STAT3 signaling might mediate in part the aggressive tumor behavior of HR prostate cancer.
Although investigations on IL-6 in carcinogenesis were carried out, the role of IL-6 in HR prostate cancer still remains unclear. Moreover, if inflammation-induced MDSC is a significant factor linking inflammation and cancer, then downregulating the inflammation factor should reduce MDSC levels and delay tumor progression. Therefore, in the present study, the links between IL-6 signaling, the expansion of MDSCs, and HR prostate cancer were investigated in vitro and in vivo.
Materials and methods
Cell cultures and reagents
A transgenic adenocarcinoma of the mouse prostate cancer cell line (TRAMP)-C1 was cultured in DMEM and 10 nM dehydroisoandrosterone. TRAMP-C1 cells were passaged serially in androgen-deprived medium to establish androgen-independent growth as TRAMP-HR. TRAMP-C1 and TRAMP-HR cells were stably transfected with IL-6 silencing vectors or a control vector. We also cultured 22RV1-HR and LNCaP- HR cells, as described earlier [2]. Mice recombinant IL-6 and IL-6-neutralized antibodies were purchased from R&D (Minneapolis, MN), and the IL-6 silencing vector and control vector were purchased from Santa Cruz (Santa Cruz, CA). The details were described in Electronic supplementary material (ESM).
Cell growth
For time course studies, cells were seeded in six-well plates at 1 × 104 cells/well in androgen(+) or androgen-deprived medium (ESM). The effects of IL-6 signaling on cell growth rates were assessed using cells incubated in a drug-containing medium for the indicated times following pre-incubation in the presence or absence of 60 ng/ml IL-6 or 5 μg/ml IL-6 Ab for 48 h.
ELISA for IL-6 level in vitro and in vivo
The levels of IL-6 in the cellular supernatants and murine serum samples were analyzed using Mouse IL-6 Quantikine ELISA Kit (R&D System; ESM).
Immunofluorescence staining
Cells in exponential growth were seeded on to coverslips for immunofluorescent staining with or without treatment. At the stated times after treatment, they were fixed, permeabilized with 2 % paraformaldehyde for 5 min, and washed in PBST. The slides were incubated for 1 h at room temperature with antibodies against E-cadherin and IL-6. The slides were incubated with FITC or Texas red-conjugated secondary antibody for 1 h and counterstaining with DAPI for nucleus.
SA-β-Gal activity
We determined SA-β-Gal activity using a senescence detection kit from BioVision (Mountain View, CA) according to the manufacturer’s instructions (ESM).
Tumor model in mice (ectopic and orthotopic)
Eight-week-old male C57BL/6J mice and IL-6 knockout mice on a C57BL/6J background (B6.129S2-Il6tm1Kopf/J) (IL-6KO) were used for the tumor implantation model, with the approval of our hospital Experimental Animal Committee. In the ectopic tumor implantation model, TRAMP-C1 and TRAMP-HR transfectants (1 × 106 cells per implantation, five animals per group) were s.c. implanted into the dorsal gluteal region. In the orthotopic tumor implantation model, TRAMP-C1 and TRAMP-HR transfectants (6 × 106 cells per implantation, five animals per group) were intraoperatively implanted into the lateral region of the prostate gland. The extent of orthotopic tumor invasion was measured 2 weeks after implantation. The effects of IL-6 stimulation on tumor growth were also investigated in vivo. For the treated group, an i.p injection of IL-6 (100 ng per mice, thrice a week) was started 1 day before tumor implantation.
FACS for MDSC
Current data suggest that MDSCs are not a defined subset of cells but rather a group of phenotypically heterogeneous myeloid cells that have common biological activity. The co-expression of myeloid cell lineage differentiation antigens Gr1 and CD11b characterizes MDSCs in mice [15, 16]. Therefore, in the present study, MDSCs are defined as CD11b+Gr1+ in mice. Flow cytometric analysis (FACS) was carried out on single-cell suspensions prepared from whole tumors and spleen after the digestion and immunostaining for CD11b and GR1 with fluorescence-labeled monoclonal antibodies (BD PharMingen). The percentage of MDSCs was measured by multicolor flow cytometry with the aforementioned monoclonal antibodies. Isotype-specific antibodies were used as negative controls in FACS.
Immunohistochemical staining and immunofluorescence for tissue specimen
Formalin-fixed, paraffin-embedded tissues were cut into 5-μm sections and mounted on slides for immunohistochemical staining. Frozen tissue specimen was cut into 5- to 8-μm cryostat sections and allowed to reach room temperature for immunofluorescence. The details were described in ESM.
Immunoblot analysis and statistical analysis
The details were described in ESM.
Results
Aggressive tumor growth in HR prostate cancer
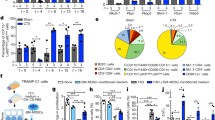
We demonstrated that TRAMP-HR cells showed accelerated tumor growth `compared to TRAMP-C1 cells in culture with or without anti-androgen treatment (Fig. 1a). The finding was confirmed by tumor growth in either male or castrated mice (Fig. 1b). We previously reported that constitutive activation of STAT3 associated with altered DNMT1 and AR expressions can be crucial in human HR prostate cancers [8]. IL-6 is the main activator of STAT3 signaling and the inducer of AR expression [7, 17]. Accordingly, we examined the activation of IL-6/STAT3 signaling in the transition of HR prostate cancer. As shown in Fig. 1c, the levels of IL-6 and p-STAT3 were gradually increased and related to the duration of hormone treatment. The data from IHC, Western blotting, and real-time RT-PCR analysis (Fig. 1d–f and ESM Fig. 1a) show that HR prostate cancer had higher levels of IL-6 and more activated STAT3, AR, and DNMT1 compared to hormone-sensitive prostate cancer cells. When HR was treated with an IL-6-neutralized antibody, the changes were reversed. Furthermore, as shown in ESM Fig. 1b, IL-6 possessed a significant impact on the androgen-independent growth of prostate cancer.
Aggressive tumor growth in HR cells related to IL-6 expression. a Cell growth of TRAMP-HR cancer cells compared to TRAMP-C1 cells in culture with or without anti-androgen treatment. Equal cell numbers (1 × 104 cells per well) were incubated in androgen(+) or androgen-deprived medium. We counted the number of viable cells after incubation for 2, 4, and 6 days. The Y-axis represents the viable cell number. Each point represents the means of three separate experiments. Bars, SD. b Tumor growth curves of HR compared to TRAMP-C1 tumor in male and castrated mice. We also showed the representative picture of TRAMP-C1 and TRAMP-HR tumors at 18 days after implantation in mice and H&E staining. Each point represents the means of three separate experiments. Bars, SD. *P < 0.05. c The increases of IL-6 expression in the transition of HR cells were evaluated by Western blot analysis in vitro. d The expressions of DNMT1, AR p-STAT3, and IL-6 were evaluated by IHC staining for TRAMP-C1 and TRAMP-HR tumors in vivo. Representative slides are shown, with magnification ×400. e The levels of DNMT1, AR p-STAT3, and IL-6 were evaluated by Western blot analysis in vitro. Proteins were extracted from cells in the presence or absence of 5 μM DNMT inhibitor or 5 μg/ml IL-6 Ab for 24 h (C, TRAMP-C1; HR, TRAMP-HR; DI, DNMT inhibitor; IL-6 Ab, IL-6 neutralized antibody). f Levels of IL-6 were examined by real-time RT-PCR in vitro. The Y-axis shows the ratio of IL-6 to GAPDH normalized by the value of TRAMP-C1 cells under the control condition. Columns represent the means of three separate experiments. Bars, SD. *P < 0.05 (C, TRAMP-C1; HR, TRAMP-HR; DI, DNMT inhibitor; IL-6 Ab, IL-6 neutralized antibody)
IL-6 linked with the aggressive behavior of HR
To determine whether IL-6 was involved in the alteration of aggressive behavior in prostate cancer, we stably transfected TRAMP-C1 and TRAMP-HR with IL-6 silencing vectors. Figure 2a and ESM Fig. 2a demonstrated that the IL-6 silencing vector significantly inhibited IL-6 expression in both TRAMP-C1 and TRAMP-HR cells. In cellular experiments and tumor growth in mice, IL-6 silencing vectors resulted in slower tumor growth, and the inhibition effect was independent of androgen status (Fig. 2b, c and ESM Fig. 2b, c). Additionally, HR prostate cancer cells increased invasion ability, as demonstrated by the migration assay (ESM Fig. 2d) and orthotopic tumor implantation assay (Fig. 2d). The invasiveness of HR prostate cancer was clearly attenuated by IL-6 silencing vectors.
IL-6 linked with the aggressive behavior of HR. a IL-6 silencing vector significantly decreased IL-6 expression demonstrated by Western blot analysis in vitro and IHC in vivo (C-V, control vector; IL-6-SV, IL-6 silencing vector). b IL-6 silencing vector decreased the proliferation rate of TRAMP-C1 and TRAMP-HR cancer cells by viable cell number counting for 6 days (1 × 104 cells on day 0; the Y-axis represents the viable cell number). c IL-6 silencing vector decreased tumor growth demonstrated by ectopic tumor growth curves and the representative pictures in male mice. Each point represents the means of three separate experiments. Bars, SD. *P < 0.05. d The effect of the IL-6 silencing vector on the invasive capacities was evaluated by murine orthotopic tumor implantation. The results are shown by representative slides and quantitative data. The Y-axis represents the relative ratio of prostate tumor invading into adjacent structure 2 weeks after implantation, normalized to the invading number of TRAMP-C1 tumors. *P < 0.05
Mechanisms underlying the effects of IL-6
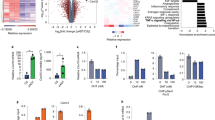
Figure 3a shows that IL-6 silencing vectors increased cell death as measured by FACS and the Annexin V staining data. Furthermore, cell cycle arrest and increases in cell senescence using SA-β-gal staining occurred following IL-6 silencing (ESM Fig. 3a, b). The role of IL-6 in tumor cell proliferation was also evaluated in vivo. Staining for Ki-67 was higher in HR tumor than TRAMP-C1 tumor, and IL-6 silencing vector clearly attenuated the positive staining (ESM Fig. 3c). As shown in Fig. 3b on the expressions of apoptosis- and cell cycle-related proteins, IL-6 inhibition induced the increases of p21, cyclin B1, and p53 associated with the decreases of bcl-2, DNMT1, and p-STAT3. Because epithelial–mesenchymal transition (EMT) is a key event in invasiveness [24], and the activation of IL-6/STAT3 signaling may be an important in the induction of EMT, we determined whether IL-6/STAT3 signaling correlated with EMT changes in prostate cancer. As determined by the expression of E-cadherin, vimentin, MMP-9, and angiogenesis-related proteins, IL-6 silencing vectors attenuated the EMT changes in vitro and in vivo (Fig. 3b–d). Moreover, when we blocked STAT3 activation with a JAK inhibitor, AG490, the tumor growth was inhibited associated with decreased EMT changes in vitro (ESM Fig. 3d).
Mechanisms underlying the effects of IL-6 on tumor aggressiveness. a Effects of the IL-6 silencing vector on cell death and apoptosis demonstrated by FACS and immunofluorescence with PI and Annexin V staining in vitro. b Effect of IL-6 silencing vector on the expression of apoptosis-, cell aging-, and EMT-related proteins evaluated by Western blot in vitro (C-V, control vector; IL-6-SV, IL-6 silencing vector). c The changes of E-cadherin in prostate cancer cells were evaluated by immunofluorescence in vitro and the results shown by representative slides and quantitative data. The quantification for E-cadherin expression is to calculate the value of the cell number positive for E-cadherin immunofluorescence divided by the total cell number for each condition. Columns are the means of three separate experiments. Bars, SD. *P < 0.05. d Effect of the IL-6 silencing vector on the expression of CD31 evaluated by immunochemical staining and immunofluorescence in vivo. The results are shown by representative slides and quantitative data. The quantification for CD31 expression is to calculate the area of positive for CD31 immunofluorescence divided by the total DAPI positive area for each condition. The Y-axis represents the ratio normalized by the value of TRAMP-C1 cells. Columns are the means of three separate experiments. Bars, SD. *P < 0.05
Effects of circulating IL-6 on tumor growth
We used enzyme-linked immunosorbent assay (ELISA) to test the level of IL-6 in the supernatant of cell culture and the serum of mice bearing tumors. As shown in Fig. 4a and ESM Fig. 4, HR secreted significantly higher IL-6 than TRAMP-C1 tumors, and the IL-6 silencing vector clearly attenuated IL-6 secretion. When cancer cells with IL-6 silencing vectors and those with control vectors were simultaneously inoculated into C57BL/6J mice, the level of circulating IL-6 was similar to that with tumors with control vectors. By our data about tumor aggressiveness, it was seen that there was a trend toward the IL-6 silencing vector inducing a more pronounced tumor inhibition in mice than that noted in the cellular experiments. We assumed that circulating IL-6 plays a role in tumor promotion, in addition to a direct action on malignant cells. To test whether IL-6 increased tumor growth and abrogated the inhibitory effect induced by androgen deprivation in vivo, we examined TRAMP-C1 tumor growth in castrated mice with IL-6 stimulation compared to that with control condition in male mice. Figure 4b shows that IL-6 stimulation could overcome the tumor-inhibiting effect induced by androgen deprivation. When HR prostate cancer cells with control vectors and those with IL-6 silencing vectors were separately implanted into the right and left thighs of mice, the growth-inhibiting effect induced by the IL-6 silencing vector could be overcome by simultaneously implanted tumors with control vectors (Fig. 4c). But the IHC data revealed that tumor with IL-6 silencing vectors still had relatively lower levels of IL-6, DNMT1, and AR and less activated STAT3 (Fig. 4d). Based on the data, we suggested that the level of circulating IL-6 positively linked with tumor growth in mice. To further demonstrate that the level of IL-6 secreted by the tumor is important for tumor progression, we implanted prostate cancer cells with control vectors and/or those with IL-6 silencing vectors into IL-6 knockout (KO) mice to abrogate microenvironment-produced IL-6. As shown in Fig. 4e, tumor growth was still significantly correlated with the IL-6 serum level of mice bearing different types of tumors.
Effects of circulating IL-6 on tumor growth. a The levels of IL-6 in serum of mice bearing tumors with or without IL-6 silencing vectors were examined by ELISA in vivo. Columns are the means of three separate experiments. Bars, SD. *P < 0.05. b Effect of IL-6 on tumor growth evaluated by the tumor growth curves of TRAMP-C1 stimulated with IL-6 in castrated mice compared to that in male mice without IL-6 stimulation. We also showed the representative picture of tumors in the male and castrated mice. Each point represents the means of three separate experiments. Bars, SD. c Tumor growth curves of simultaneous implanted TRAMP-HR cells with control vectors and those with IL-6 silencing vectors in male and castrated mice. We also showed the representative picture of tumors at 18 days after implantation in mice. Each point represents the means of three separate experiments. Bars, SD. d Expressions of DNMT1, AR, p-STAT3, STAT3, and IL-6 were evaluated by IHC for simultaneous implanted TRAMP-HR cells with control vectors and those with IL-6 silencing vectors in the same male mice. Representative slides are shown, with magnification ×100. e Tumor size of TRAMP-C1 cells with control vectors and those with IL-6 silencing vectors at 14 days after simultaneous implantation (5 × 106 cells per implantation) in the same or different IL-6 KO mice. Additionally, the IL-6 serum level of tumor-bearing mice was examined by ELISA and the representative slides of IHC for IL-6 and p-STAT3 demonstrated
Effects of circulating IL-6 on the induction of MDSC
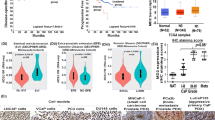
As shown in Fig. 5a, b and ESM Fig. 5a, b, MDSC levels in tumor and spleen of mice inoculated with TRAMP-HR tumor significantly increased compared to mice with TRAMP-C1 tumors. Moreover, IL-6 silencing vectors obviously blocked the accumulation of MDSCs in vivo. When wild-type tumors and those with IL-6 silencing vectors were simultaneously inoculated into the same mice, the level of MDSCs in tumor was similar to that of mice bearing wild-type tumors (Fig. 5c). To further determine whether the accumulation of MDSCs was driven by IL-6 stimulation, we examined the level of MDSCs in mice with TRAMP-C1 tumor with or without IL-6 stimulation. As detected by FACS and immunofluorescence analysis, IL-6 stimulation induced more MDSC accumulation associated with an increased expression of stromal-drived factor-1 alpha (SDF-1α), a chemokine that promotes tissue retention of bone marrow-derived cells (Fig. 5c, d and ESM Fig. 5c). When we implanted prostate cancer cells in IL-6 KO mice to abrogate microenvironment-produced IL-6, the tumor-secreted IL-6 still had a significant impact on the recruitment of MDSCs (Figs. 4e and 5e and ESM Fig. 5d).
IL-6 linked with the recruitment of MDSC. a Effect of IL-6 on the recruitment of MDSC in tumor (tumor size, 300–350 mm3) evaluated by FACS using GrI-CD11b staining in mice bearing tumors with or without IL-6 silencing vectors. The results are shown by representative slides. b Effect of IL-6 on the recruitment of MDSC in spleen evaluated by FACS using GrI-CD11b staining in mice bearing tumors for 2 weeks. The results are shown by representative slides. c Effect of IL-6 on the recruitment of MDSC in tumor (tumor size, 300–350 mm3) evaluated by FACS using GrI-CD11b staining in mice bearing different types of tumors (C, TRAMP-C1; HR, TRAMP-HR; IL-6-SV, IL-6 silencing vector). Columns are the means of three separate experiments. Bars, SD. *P < 0.05. d Effect of IL-6 on the expression of CD11b and Gr1 detected by immunofluorescence for mice bearing different types of tumors in vivo. The quantification for CD11b expression is to calculate the value of the cell number positive for CD11b immunofluorescence divided by the total cell number for each condition. The Y-axis represents the ratio normalized by the value of TRAMP-C1 cells. Columns are the means of three separate experiments. Bars, SD. *P < 0.05. e Effect of IL-6 on the recruitment of MDSC in spleen evaluated by FACS using GrI-CD11b staining at 14 days after simultaneous implantation (5 × 106 TRAMP-C1 cells with control vectors and those with IL-6 silencing vectors) in IL-6 KO mice. The results are shown by representative slides
Effects of the induction of MDSC on tumor regrowth
Our data revealed that MDSC recruitment may be responsible for the accelerated tumor growth in mice bearing IL-6-overexpressed tumor. It is reported that local irradiation (LI) could induce the recruitment of immune-suppressor cells to facilitate tumor regrowth [18]. To examine whether the induction of MDSCs underlined the tumor progression, we examined the link between irradiation, tumor regrowth, and MDSC recruitment. Figure 6a demonstrated that LI stimulated the recruitment of MDSCs in tumor associated with increased IL-6 and that IL-6 silencing vector attenuated LI-induced MDSC recruitment. The role of MDSC accumulation in tumor progression was further examined by whole-body irradiation (WBI) 6 Gy with or without infusion of sorted MDSCs to mice bearing 500-mm3 TRAMP-C1 tumors. The dose (6 Gy WBI) is known to damage the bone marrow and depleted leukocytes for 1.5–2 weeks [19]. By observation of the tumor regrowth, the infusion of sorted MDSCs abrogated the growth delay induced by WBI compared to that after LI (Fig. 6b, c). Moreover, we demonstrated that MDSC accumulation was associated with increased CD31 and VEGF (Fig. 6c, d). Therefore, the induction of angiogenesis might be one of the mechanisms responsible for tumor promotion by MDSCs. To further investigate the dual effect of tumor cell and MDSC recruitment on the role of IL-6 in tumor growth in vivo, we simultaneously implanted HR cells and/or those with IL-6 silencing vectors into the mice following 6 Gy WBI to abrogate MDSC recruitment and examined the direct effect of IL-6 on tumor cells. As shown in Fig. 6e, the depletion of MDSCs partially attenuated HR-induced growth stimulation on tumor with an IL-6 silencing vector compared to that noted in Figs. 2c and 4c. Therefore, we suggested that the IL-6-induced growth promotion in vivo was contributed by the dual effect on tumor cells and MDSC recruitment.
Link between the induction of MDSC and tumor regrowth. a Effects of local irradiation on the IL-6 expression and MDSC recruitment examined by FACS analysis in male mice bearing tumor 48 h after irradiation. b Tumor size of TRAMP-C1 tumor at 9 days after irradiation. When tumor reaches 500 mm3, we observe tumor growth after whole-body irradiation for 6 Gy with or without intravenous infusion 1 × 106 sorted MDSC compared to that after local tumor irradiation for 6 Gy. We also showed the representative picture of tumors in the male mice. Each point represents the means of three separate experiments. Bars, SD. c Recruitment of MDSC evaluated by FACS using GrI-CD11b staining in tumor-bearing mice at 9 days after whole-body irradiation for 6 Gy with or without intravenous infusion 1 × 106 sorted MDSC or local tumor irradiation for 6 Gy. d Expressions of CD31 and VEGF evaluated by immunochemical staining in tumor-bearing mice at 9 days after whole-body irradiation for 6 Gy with or without intravenous infusion 1 × 106 sorted MDSC or local tumor irradiation for 6 Gy. e Tumor size of TRAMP-HR cells and those with IL-6 silencing vectors at 14 days after simultaneous implantation (5 × 106 cells per implantation) in the same or different mice after WBI. We also showed the representative picture of tumors. Each point represents the means of three separate experiments. Bars, SD (HR, TRAMP-HR; IL-6-SV, IL-6 silencing vector)
Discussion
To perform experiments in an immunocompetent model, TRAMP-C1 prostate cancer cell line, derived from adenocarcinoma of mouse prostate, and TRAMP-HR, derived from TRAMP-C1 cells cultured in an androgen-deprived medium, were used in the present study. The androgen-independent growth noted in the animal model confirmed the hormone resistance of HR prostate cancer induced in vitro. In addition to accelerated tumor growth, HR appeared with increased invasiveness, shown by the migration assay and the orthotopic tumor model. Constitutive activation of STAT3 contributes to oncogenesis in a variety of malignancies including prostate cancer [20]. IL-6 is an important transcription factor regulating oncogenic signaling and inducing STAT3 activation [8, 21]. Moreover, in several experimental models, IL-6 seems to have anti-apoptotic and pro-angiogenic effects [22]. Treatment with anti-IL-6 antibody has been successfully applied in several models representing prostate cancer [23, 24]. In the present study, HR prostate cancer appeared with increased IL-6 expressions compared to hormone-sensitive prostate cancer. We hypothesized that IL-6 is crucial in the transition of HR and could be a promising target for prostate cancer, therefore, looking at the effect of IL-6 on prostate cancer in vitro and in vivo. By our data, inhibiting IL-6 resulted in a slower tumor growth associated with decreased p-STAT3, and the effect was independent of androgen status. The increases of apoptosis, cellular senescence, and cell cycle arrest could be responsible for the slower tumor growth induced by inhibiting IL-6. The invasiveness of prostate cancer cells was also significantly attenuated by the IL-6 silencing vector. EMT appears to be functionally relevant to the invasive characteristics of epithelial tumors [25]. Activated STAT3 signaling is an important pathway responsible for the EMT process [20, 25]. At the molecular marker level, EMT is characterized by the loss of E-cadherin associated with a number of invasion- and angiogenesis-related factors. Our data demonstrated that TRAMP-HR had decreased E-cadherin associated with increased MMP-9 and VEGF compared to TRAMP-C1 in vitro, and IL-6 silencing vectors reversed the EMT-related change. It was reported that IL-6 contributed to the conversion of prostate cancer to an androgen-independent state in xenografts models [17, 23], and anti-IL-6 monoclonal antibodies have been applied to treat metastatic castration-resistant prostate cancer in clinical studies [26]. Our data also showed that IL-6/STAT3 signaling had a significant impact on androgen- independent growth and the aggressive behavior of prostate cancer. Taken together, these findings indicate that endogenous IL-6 plays an important role in the aggressive tumor growth of prostate cancer and is crucial in the transition of HR prostate cancer.
In the clinic, IL-6 serum levels seem to be elevated in a subgroup of patients with metastatic prostate cancer [27, 28]. In the present study, higher IL-6 levels were seen in the supernatant of HR cell culture medium and the serum of mice bearing HR tumors. Moreover, there was a positive correlation between the circulating level of IL-6 and tumor growth in vivo. IL-6 have been known to positively influence tumor development and is recognized as a key regulator of immunosuppression with advanced cancer [7, 8, 11]. A better understanding of systemic immunosuppression, such as the interactions between MDSCs, systemic cytokines, and their signaling pathways, could lead to new strategies for augmenting immune response against tumors. MDSCs are an important cell subset that contributes to an immunosuppressive tumor microenvironment [29, 30]. The expansion of MDSC is associated with inflammation, and the activation of STAT3 is significantly associated with the expansion of MDSC [15]. Based on the hypothesis that MDSC might be the mechanism responsible for tumor promotion by circulating IL-6, we checked for a correlation between the subpopulation of MDSC and the serum level of IL-6 in mice bearing tumors. By our data, it was shown that higher serum levels of IL-6 were significantly linked with more MDSC recruitment associated with increased p-STAT3 and SDF-1α. Furthermore, in experiments with tumor implanted in IL-6 KO mice, the inhibition of tumor-produced IL-6 significantly abrogated the recruitment of MDSC. These findings indicated that IL-6 is a major mediator underlying the more expansion of MDSC noted in HR prostate cancer.
MDSCs are thought to represent an important barrier that limits the full potential of immune-based cancer therapies or endogenous host response to developing tumors [29–31]. Radiotherapy is crucial for the treatment of prostate cancer. The enhancement of antitumor responses following RT was attributed to the ability of RT to alter the tumor microenvironment in a part. The increase in MDSCs induced by local irradiation was reported to facilitate tumor regrowth after irradiation [18]. Accordingly, to further investigate the link between the recruitment of MDSC and tumor progression, we observed tumor regrowth after depletion of MDSC by WBI with or without infusion of sorted CD11b+Gr1+ cells compared to that after LI. In our data, the expansion of MDSC by LI or intravenous infusion was associated with rapid tumor regrowth.
In addition to immunosuppression, bone marrow-derived CD11b+ myeloid cells have been shown to mediate many functions of myeloid cells, including migration and angiogenesis [32, 33]. The recruitment of various blood-borne bone marrow-derived cells might be important for tumor neovascularization. Angiogenesis is one of the mechanisms that promote tumor progression, and CD31 mediated endothelial cell–cell interactions involved in angiogenesis [34]. In our data, the induction of MDSC recruitment accelerated tumor growth associated with increased CD31 and VEGF expressions in tumors. These findings indicated that MDSC recruitment might mediate the aggressive tumor growth noted in IL-6-expressing prostate cancer, and the promotion of angiogenesis is one of the underlying mechanisms.
Finally, it is noteworthy that IL-6 is crucial for aggressive tumor growth and the transition of HR process of prostate cancer by the dual effects of IL-6 on tumor cells and MDSC recruitment. These results suggested that the level of IL-6 in cancer patients might be a significant clinical predictor of prostate cancer. Moreover, targeting IL-6 could lead to some promising strategies for the treatment of HR prostate cancer.
Abbreviations
- HR:
-
Hormone-resistant
- HS:
-
Hormone-sensitive
- MDSCs:
-
Myeloid-derived suppressor cells
- AR:
-
Androgen receptor
- EMT:
-
Epithelial–mesenchymal transition
- VEGF:
-
Vascular endothelial growth factor
- WBI:
-
Whole-body irradiation
- LI:
-
Local irradiation
- RT:
-
Irradiation
References
Craft N, Chhor C, Tran C, Belldegrun A, DeKernion J, Witte ON, Said J, Reiter RE, Sawyers CL (1999) Evidence for clonal outgrowth of androgen-independent prostate cancer cells from androgen-dependent tumors through a two-step process. Cancer Res 59:5030–5036
Wu CT, Chen WC, Liao SK, Hsu CL, Lee KD, Chen MF (2007) The radiation response of hormone-resistant prostate cancer induced by long-term hormone therapy. Endocr Relat Cancer 14:633–643
Chen CD, Welsbie DS, Tran C, Baek SH, Chen R, Vessella R, Rosenfeld MG, Sawyers CL (2004) Molecular determinants of resistance to antiandrogen therapy. Nat Med 10:33–39
Edwards J, Bartlett JM (2005) The androgen receptor and signal-transduction pathways in hormone-refractory prostate cancer. Part 1: Modifications to the androgen receptor. BJU Int 95:1320–1326
Kinkade CW, Castillo-Martin M, Puzio-Kuter A, Yan J, Foster TH, Gao H, Sun Y, Ouyang X, Gerald WL, Cordon-Cardo C et al (2008) Targeting AKT/mTOR and ERK MAPK signaling inhibits hormone-refractory prostate cancer in a preclinical mouse model. J Clin Invest 118:3051–3064
Chen MF, Chen WC, Chang YJ, Wu CF, Wu CT (2010) Role of DNA methyltransferase 1 in hormone-resistant prostate cancer. J Mol Med (Berl) 88:953–962
Kishimoto T (2005) Interleukin-6: from basic science to medicine—40 years in immunology. Annu Rev Immunol 23:1–21
Schafer ZT, Brugge JS (2007) IL-6 involvement in epithelial cancers. J Clin Invest 117:3660–3663
Culig Z, Steiner H, Bartsch G, Hobisch A (2005) Interleukin-6 regulation of prostate cancer cell growth. J Cell Biochem 95:497–505
Chen CC, Chen WC, Lu CH, Wang WH, Lin PY, Lee KD, Chen MF (2010) Significance of interleukin-6 signaling in the resistance of pharyngeal cancer to irradiation and the epidermal growth factor receptor inhibitor. Int J Radiat Oncol Biol Phys 76:1214–1224
Coussens LM, Werb Z (2002) Inflammation and cancer. Nature 420:860–867
Balkwill F, Mantovani A (2001) Inflammation and cancer: back to Virchow? Lancet 357:539–545
Bunt SK, Sinha P, Clements VK, Leips J, Ostrand-Rosenberg S (2006) Inflammation induces myeloid-derived suppressor cells that facilitate tumor progression. J Immunol 176:284–290
Suzuki E, Kapoor V, Jassar AS, Kaiser LR, Albelda SM (2005) Gemcitabine selectively eliminates splenic Gr-1+/CD11b+ myeloid suppressor cells in tumor-bearing animals and enhances antitumor immune activity. Clin Cancer Res 11:6713–6721
Gabrilovich DI, Nagaraj S (2009) Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev Immunol 9:162–174
Kusmartsev S, Nefedova Y, Yoder D, Gabrilovich DI (2004) Antigen-specific inhibition of CD8+ T cell response by immature myeloid cells in cancer is mediated by reactive oxygen species. J Immunol 172:989–999
Malinowska K, Neuwirt H, Cavarretta IT, Bektic J, Steiner H, Dietrich H, Moser PL, Fuchs D, Hobisch A, Culig Z (2009) Interleukin-6 stimulation of growth of prostate cancer in vitro and in vivo through activation of the androgen receptor. Endocr Relat Cancer 16:155–169
Kozin SV, Kamoun WS, Huang Y, Dawson MR, Jain RK, Duda DG (2010) Recruitment of myeloid but not endothelial precursor cells facilitates tumor regrowth after local irradiation. Cancer Res 70:5679–5685
Seung LP, Weichselbaum RR, Toledano A, Schreiber K, Schreiber H (1996) Radiation can inhibit tumor growth indirectly while depleting circulating leukocytes. Radiat Res 146:612–618
Levy DE, Darnell JE Jr (2002) Stats: transcriptional control and biological impact. Nat Rev Mol Cell Biol 3:651–662
Rose-John S, Waetzig GH, Scheller J, Grotzinger J, Seegert D (2007) The IL-6/sIL-6R complex as a novel target for therapeutic approaches. Expert Opin Ther Targets 11:613–624
Culig Z, Puhr M (2011) Interleukin-6: a multifunctional targetable cytokine in human prostate cancer. Mol Cell Endocrinol. doi:10.1016/j.mce.2011.05.033
Wallner L, Dai J, Escara-Wilke J, Zhang J, Yao Z, Lu Y, Trikha M, Nemeth JA, Zaki MH, Keller ET (2006) Inhibition of interleukin-6 with CNTO328, an anti-interleukin-6 monoclonal antibody, inhibits conversion of androgen-dependent prostate cancer to an androgen-independent phenotype in orchiectomized mice. Cancer Res 66:3087–3095
Karkera J, Steiner H, Li W, Skradski V, Moser PL, Riethdorf S, Reddy M, Puchalski T, Safer K, Prabhakar U et al (2011) The anti-interleukin-6 antibody siltuximab down-regulates genes implicated in tumorigenesis in prostate cancer patients from a phase I study. Prostate 71:1455–1465
Thiery JP (2002) Epithelial–mesenchymal transitions in tumour progression. Nat Rev Cancer 2:442–454
Fizazi K, De Bono JS, Flechon A, Heidenreich A, Voog E, Davis NB, Qi M, Bandekar R, Vermeulen JT, Cornfeld M et al (2012) Randomised phase II study of siltuximab (CNTO 328), an anti-IL-6 monoclonal antibody, in combination with mitoxantrone/prednisone versus mitoxantrone/prednisone alone in metastatic castration-resistant prostate cancer. Eur J Cancer 48:85–93
Shariat SF, Kattan MW, Traxel E, Andrews B, Zhu K, Wheeler TM, Slawin KM (2004) Association of pre- and postoperative plasma levels of transforming growth factor beta(1) and interleukin 6 and its soluble receptor with prostate cancer progression. Clin Cancer Res 10:1992–1999
George DJ, Halabi S, Shepard TF, Sanford B, Vogelzang NJ, Small EJ, Kantoff PW (2005) The prognostic significance of plasma interleukin-6 levels in patients with metastatic hormone-refractory prostate cancer: results from Cancer and Leukemia Group B 9480. Clin Cancer Res 11:1815–1820
Kao J, Ko EC, Eisenstein S, Sikora AG, Fu S, Chen SH (2011) Targeting immune suppressing myeloid-derived suppressor cells in oncology. Crit Rev Oncol Hematol 77:12–19
Kusmartsev S, Gabrilovich DI (2002) Immature myeloid cells and cancer-associated immune suppression. Cancer Immunol Immunother 51:293–298
Menetrier-Caux C, Montmain G, Dieu MC, Bain C, Favrot MC, Caux C, Blay JY (1998) Inhibition of the differentiation of dendritic cells from CD34(+) progenitors by tumor cells: role of interleukin-6 and macrophage colony-stimulating factor. Blood 92:4778–4791
Ahn GO, Tseng D, Liao CH, Dorie MJ, Czechowicz A, Brown JM (2010) Inhibition of Mac-1 (CD11b/CD18) enhances tumor response to radiation by reducing myeloid cell recruitment. Proc Natl Acad Sci USA 107:8363–8368
Yang L, DeBusk LM, Fukuda K, Fingleton B, Green-Jarvis B, Shyr Y, Matrisian LM, Carbone DP, Lin PC (2004) Expansion of myeloid immune suppressor Gr+CD11b+ cells in tumor-bearing host directly promotes tumor angiogenesis. Cancer Cell 6:409–421
Sharma S, Sharma MC, Sarkar C (2005) Morphology of angiogenesis in human cancer: a conceptual overview, histoprognostic perspective and significance of neoangiogenesis. Histopathology 46:481–489
Acknowledgments
The study was supported by grants from the National Science Council (grants 97-2314-B-182A-079-MY3) and CMRPG 290041.
Competing interests
There is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 1531 kb)
Rights and permissions
About this article
Cite this article
Wu, CT., Hsieh, CC., Lin, CC. et al. Significance of IL-6 in the transition of hormone-resistant prostate cancer and the induction of myeloid-derived suppressor cells. J Mol Med 90, 1343–1355 (2012). https://doi.org/10.1007/s00109-012-0916-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-012-0916-x