Abstract
Inflammatory bowel disease affects millions of individuals; nevertheless, pharmacological treatment is disappointingly unsatisfactory. Cannabidiol, a safe and non-psychotropic ingredient of marijuana, exerts pharmacological effects (e.g., antioxidant) and mechanisms (e.g., inhibition of endocannabinoids enzymatic degradation) potentially beneficial for the inflamed gut. Thus, we investigated the effect of cannabidiol in a murine model of colitis. Colitis was induced in mice by intracolonic administration of dinitrobenzene sulfonic acid. Inflammation was assessed both macroscopically and histologically. In the inflamed colon, cyclooxygenase-2 and inducible nitric oxide synthase (iNOS) were evaluated by Western blot, interleukin-1β and interleukin-10 by ELISA, and endocannabinoids by isotope dilution liquid chromatography–mass spectrometry. Human colon adenocarcinoma (Caco-2) cells were used to evaluate the effect of cannabidiol on oxidative stress. Cannabidiol reduced colon injury, inducible iNOS (but not cyclooxygenase-2) expression, and interleukin-1β, interleukin-10, and endocannabinoid changes associated with 2,4,6-dinitrobenzene sulfonic acid administration. In Caco-2 cells, cannabidiol reduced reactive oxygen species production and lipid peroxidation. In conclusion, cannabidiol, a likely safe compound, prevents experimental colitis in mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The disorders collectively known as inflammatory bowel disease (IBD) include Crohn's disease and ulcerative colitis. It is relatively common in the USA, accounting for disease in approximately one million individuals, with similar numbers in Europe [1]. Although the incidence rates are beginning to stabilize in industrialized countries, rates continue to rise in low-incidence areas such as Asia and most developing countries [2, 3]. IBD can be alleviated with medications that induce and maintain remission—since a cure remains elusive—and steroids, 5-ASA, and biologicals have been a mainstay in its treatment [2, 3]. However, these drugs possess limited beneficial action, thus justifying the continued search for new therapeutic approaches.
The marijuana plant, Cannabis sativa, has a long medical history [4]. Extracts of Cannabis were indicated for the treatment of diarrhea a century ago in the USA, and there are several anecdotal accounts of the effective use of Cannabis-based products against IBD [4]. The limitation of the therapeutic utility of Cannabis and of one of its major components, Δ9-tetrahydrocannabinol, is the occurrence of psychoactive effects due to the activation of brain cannabinoid CB1 receptors [5]. In contrast, cannabidiol (CBD), one of the most abundant plant-derived cannabinoids with reported antioxidant, anti-inflammatory, and immunomodulatory effects [6], is devoid of psychoactive properties and is also well tolerated in humans [7]. CBD, unlike ∆9-THC, has very low affinity for both cannabinoid CB1 and CB2 receptors [8, 9], although it has been proposed that it may modulate endocannabinoid function through its ability to inhibit fatty acid amide hydrolase (FAAH, i.e., the enzyme which hydrolyses the endocannabinoid anandamide) [10]. This is an important observation since FAAH inhibition results in anti-inflammatory effects within the gut [11–14]. Although CBD exerts pharmacological activities (e.g., antioxidant, neuroprotective, and anti-inflammatory actions) and mechanisms (i.e., FAAH inhibition) of potential therapeutic interest in the field of gastrointestinal pharmacology, to date, it has not been extensively evaluated in the digestive tract [15]. Ligresti et al. [16] showed that CBD inhibited cell growth in the human colon adenocarcinoma cell line, Caco-2. More recently, it has been shown that CBD does not modify motility in control animals, but it may inhibit the increased intestinal motility associated with experimental ileitis in mice [17].
Considering these observations, we investigated the effect of CBD on the colitis caused by intracolonic administration of 2,4,6,dinitrobenzene sulfonic acid (DNBS). Specifically, we analyzed both macroscopic and microscopic changes in inflamed animals treated or not with CBD.
To further characterize the action of CBD, we investigated the effect of this Cannabis-derived ingredient on inducible nitric oxide synthase (iNOS) and cyclooxygenase-2 (COX-2) expression as well as on interleukin-1β (IL-1 β), interleukin-10 (IL-10), and endocannabinoid levels in the colon of animals treated with DNBS. Moreover, because impairment of the antioxidant defense of intestinal epithelial cells may lead to gut inflammation [18], we investigated the potential protective effect of CBD against oxidative stress in human colon adenocarcinoma (Caco-2) cells.
Materials and methods
Drugs and reagents
CBD [purity by high-performance liquid chromatography (HPLC), 99.76%] was kindly supplied by GW Pharmaceuticals (Porton Down, Wiltshire, UK). DNBS and 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) were purchased from Sigma (Milan, Italy). CBD was dissolved in ethanol/Tween20/saline (1:1:8; for in vivo experiments) or dimethyl sulfoxide (DMSO; for in vitro experiments). DNBS was dissolved in 50% ethanol (0.15 ml/mouse). The CBD vehicles (60 µl/mouse in vivo or 0.01% DMSO in vitro) had no significant effects on the responses under study.
Animals
Male ICR mice, weighing 35–40 g, were supplied by Harlan Italy (Corezzana, Milan, Italy). All animals, used after 1 week of acclimation (temperature, 23 ± 2°C; humidity, 60%), had free access to water and food. Mice were fed ad libitum with standard food, except for the 24-h period immediately preceding the administration of DNBS and for the 12-h period preceding the killing of the animals. All experiments complied with the Italian D.L. no. 116 of 27 January 1992 and associated guidelines in the European Communities Council Directive of 24 November 1986 (86/609/ECC).
Induction of experimental colitis
Colitis was induced by the intracolonic administration of DNBS [11]. Briefly, mice were anesthetized and DNBS (8 mg/mouse) was inserted into the colon using a polyethylene catheter (1 mm in diameter) via the rectum (4.5 cm from the anus). Three days after DNBS administration, all animals were euthanized by asphyxiation with CO2, the mice abdomen was opened by a midline incision and the colon removed, isolated from surrounding tissues, opened along the antimesenteric border, rinsed, weighed, length measured, and processed for macroscopic evaluation. The colon weight/colon length ratio (mg/cm) was also determined as an indirect marker of inflammation. For histological examination, tissues were fixed in 10% formaldehyde. For biochemistry analysis, the colons were kept at −80°C until use.
The dose of DNBS was selected on the basis of preliminary experiments showing a remarkable colonic damage associated to high reproducibility and low mortality for the 8-mg/kg dose. The time point of damage evaluation (i.e., 3 days after DNBS administration) was chosen because maximal DNBS-induced inflammation has been reported in mice after 3 days [11]. Furthermore, previous studies have shown that 3 days after intracolonic DNBS administration in mice, the inflammatory response may be modulated by administration of cannabinoid drugs such as direct cannabinoid receptor agonists or antagonists [11].
Pharmacological treatment in vivo
CBD (1–10 mg/kg for gross macroscopic evaluations and 5 mg/kg for histology, iNOS, COX-2, interleukin, and endocannabinoid measurements) was injected once a day for six consecutive days starting 3 days before DNBS administration.
Macroscopic and histological evaluation
Macroscopic and histological evaluations were performed 3 days after DNBS administration. Gross macroscopic damage was scored according to the following scale [12]: 0, no damage; 1, hyperemia but no ulcers; 2, fibrosis but no ulcers; 3, ulceration/necrosis <1 cm; 4, ulceration/necrosis <2 cm; 5, ulceration/necrosis >2 cm.
Microscopic damage was assessed on a segment of 1 cm of colon located 4 cm above the anal canal. After fixation for 24 h in saline 10% formaldehyde, samples were dehydrated in graded ethanol and embedded in paraffin. Thereafter, 5-μm sections were deparaffinized with xylene, stained with hematoxylin–eosin, and observed in a DM 4000 B Leica microscope (Leica Microsystems, Milan, Italy). Colon was scored considering (1) the submucosal infiltration (0, none; 1, mild; 2–3, moderate; 4–5 severe) and (2) the crypt abscesses (0, none, 1–2 rare; 3–5, diffuse) [12].
COX-2 and iNOS expression
Full-thickness colons from control and DNBS-treated mice (treated or not with CBD 5 mg/kg) were homogenized in lysis buffer (1:2, w/v) containing 0.5 M β-glycerophosphate, 20 mM MgCl2, 10 mM ethylene glycol tetraacetic acid, and supplemented with 100 mM dithiothreitol and protease/phosphatase inhibitors (100 mM dimethylsulfonyl fluoride, 2 mg/ml apronitin, 2 mM leupeptin, and 10 mM Na3VO4). Homogenates were centrifuged at 600×g for 5 min at 4°C; the supernatants were collected and centrifuged at 16,200×g for 10 min at 4°C. Proteins (50 µg, determined with the Bradford method) were subjected to electrophoresis on a sodium dodecyl sulfate 10% polyacrylamide gel and electrophoretically transferred onto a nitrocellulose transfer membrane (Protran, Schleicher & Schuell, Germany). The immunoblots were developed with 1:2,000 and 1:1,000 dilutions for COX-2 (BD Bioscience, Belgium) and iNOS (Cayman Chemical, USA), respectively, and the signal was detected with the ECL System according to the manufacturer's instructions (Amersham Pharmacia Biotech). The membranes were probed with an anti β-actin antibody to normalize the results, which were expressed as a ratio of densitometric analysis of COX-2/β-actin and iNOS/β-actin bands.
Nitrite measurement
Nitrites, stable metabolites of NO, were measured in full-thickness colonic tissue according to Thomsen et al. [19]. After reducing nitrate to nitrite with the use of acid-washed cadmium powder, homogenate aliquots were centrifuged at 16,200×g for 10 min at 4°C. Then, supernatant aliquots were sequentially incubated with 50 µg/ml 2,3-diaminonaphtalene for 7 min at 4°C (protected from light) and 2.8 N NaOH. Nitrite levels were measured using a fluorescent microplate reader (excitation 365 nm and emission 450 nm; Perkin-Elmer Instruments). The fluorescence intensity obtained was compared with a NaNO2 standard curve (50–2000 nM).
Interleukin-1β and interleukin-10 levels
IL-1β and IL-10 levels in full-thickness colonic tissues were quantified using commercial ELISA kits (R&D Systems and Diaclone, respectively, from Inalco, Italy) according to the manufacturer's instructions.
Endocannabinoid extraction and measurement
Full-thickness colons from control and DNBS-treated mice (treated or not with CBD 5 mg/kg) were removed (3 days after DNBS administration), and tissue specimens were immediately weighed, immersed into liquid nitrogen, and stored at −80°C until extraction of endocannabinoids. Tissues were extracted, purified, and analyzed as described elsewhere [12, 20]. In some experiments, the assay was performed in control mice treated or not with CBD 5 mg/kg.
Quantitative (real-time) RT-PCR analysis
Full-thickness colons from control and DNBS-treated mice were collected in RNA later (Invitrogen) and homogenized by a rotor-stator homogenizer in 1.5 ml of Trizol® (Invitrogen). Total RNA was extracted according to manufacturer recommendations, dissolved in RNAase-free water, and further purified by spin cartridge by the Micro-to-Midi total RNA purification system (Invitrogen). Total RNA was dissolved in RNA storage solution (Ambion), UV-quantified by a Bio-Photometer® (Eppendorf), and stored at −80°C until use. RNA aliquots (6 µ g) were digested by RNAse-free DNAse I (Ambion DNA-free™ kit) in a 20 µ l final volume reaction mixture to remove residual contaminating genomic DNA. After DNAse digestion, concentration and purity of RNA samples were evaluated by the RNA-6000-Nano® microchip assay using a 2100 Bioanalyzer® equipped with a 2100 Expert Software® (Agilent) following the manufacturer’s instructions. For all samples tested, the RNA integrity number was greater than 8 relative to a 0–10 scale. One microgram of total RNA, as evaluated by the 2100 Bioanalyzer, was reverse-transcribed in cDNA by the SuperScript III SuperMix (Invitrogen).
The reaction mixture was incubated in a termocycler iCycler-iQ5® (BioRad) for a 5 min at 60°C step, followed by a rapid chilling for 2 min at 4°C. The protocol was stopped at this step and the reverse transcriptase was added to the samples, except the negative controls (-RT). The incubation was resumed by two thermal steps: 10 min at 25°C followed by 40 min at 50°C. Finally, the reaction was terminated by heating at 95°C for 10 min. Quantitative real-time PCR was performed by an iCycler-iQ5® in a 20 µ l reaction mixture containing 1× SsoFast EVAGreen supermix (BioRad), 10 ng of cDNA (calculated on the basis of the retro-transcribed RNA), and 330 nM for each primer. The amplification profile consisted of an initial denaturation of 2 min at 94°C and 40 cycles of 30 s at 94°C, annealing for 30 s at TaOpt (optimum annealing temperature, see below), and elongation for 45 s at 68°C. Fluorescence data were collected during the elongation step. A final extension of 7 min was carried out at 72°C, followed by melt-curve data analysis. Optimized primers for FAAH analysis (accession: NM_010173) and relative TaOpt were designed by the AlleleID® software 7.0 version (Biosoft International, Palo Alto, CA, USA) and were synthesized (HPLC purification grade) by Eurofins-MWG/Operon, Germany. Assays were performed in quadruplicate (maximum ∆Ct of replicate samples <0.5), and a standard curve from consecutive fivefold dilutions (100 to 0.16 ng) of a cDNA pool representative of all samples was included for PCR efficiency determination. Relative expression calculation—to correct for PCR efficiency and normalized with respect to reference gene β-actin (accession: NM_007393)—and statistical analysis were performed by the IQ5 software.
Cell culture
Caco-2 cells (American Type Culture Collection) were cultured in Dulbecco's modified Eagle’s medium (DMEM) containing 10% fetal bovine serum (FBS), 100 U/ml penicillin, 100 µg/ml streptomycin, 1% non-essential amino acids, 1 M HEPES 2.5%, non-essential amino acid 1X, and 2 mM l-glutamine 1%. Cell viability was evaluated by trypan blue staining.
Cytotoxicity assay
The effect of CBD on cell survival was measured using the MTT assay [21]. Caco-2 cells (passage between 35 and 40) were seeded in 96-well plates at a concentration of 1 × 104 cells/well. After 48 h of culturing, the cells were treated with CBD (10−8–10−5 M) at 37°C for 24 h. Subsequently, cells were washed with 100 µ l/well of PBS and incubated with 200 µl/well of MTT solution (250 µ g/ml) for 1 h at 37°C. Finally, 100 µl/well of DMSO was added and the absorbency was read at a wavelength (λ) of 490 nm (microplate autoreader model EL 311SX; Bio-Tek Instruments Inc., Winooski, VT, USA). Treatments were compared with a positive control, i.e., DMSO 6% (v/v). Results are expressed as percentage of cell viability.
Lipid peroxidation in Caco-2 cells
Lipid peroxidation products from Caco-2 cells were measured by the thiobarbituric acid colorimetric assay [22]. Briefly, Caco-2 cells (passage between 35 and 40) were seeded in Petri dishes (100 mm in diameter) at a density of 1.0 × 106 in DMEM supplemented with 10% FBS and led to the differentiation. Caco-2 cell monolayers, exposed to CBD (10−8–10−5 M) for 24 h, were washed with PBS and incubated with the Fenton's reagent (H2O2/Fe2+ 1 mM) for 3 h at 37°C. Subsequently, cells were washed and scraped on ice with 800 µ l of PBS. Cells were lysed by six cycles of freezing and thawing in PBS and then centrifuged at 12,600×g for 10 min at 4°C. Trichloroacetic acid (300 µl of 10%, w/v) was added to 150 µl of cellular lysate, and after centrifugation at 7,000×g for 10 min, 0.67% (w/v) thiobarbituric acid was added and the mixture was heated at 80°C for 30 min. Malondialdehyde (MDA) production was recorded using a Beckman DU-62 spectrophotometer at a wavelength (λ) of 532 nm. The results are expressed as micromoles of MDA per milligram of proteins contained in the cell lysates, which were determined by the Bio-Rad protein assay.
Intracellular ROS measurement in Caco-2 cells
The generation of intracellular reactive oxygen species (ROS) was estimated using the fluorescence probe 2′,7′-dichlorfluorescein-diacetate (H2DCF-DA) [23]. For the experiments, cells were plated in 96-multiwell black plates (Corning, USA) at the density of 1 × 104 cells per well and led to the differentiation. Caco-2 cell monolayers were incubated for 24 h at 37°C with CBD (10−8–10−5 M). After washing, cells were incubated for 30 min with 200 µl of 100 µM H2DCF-DA in HBSS containing 1% FBS. Finally, cells were rinsed and incubated with the Fenton's reagent (H2O2/Fe2+ 2 mM) for 3 h at 37°C. The DCF fluorescence intensity was detected using a fluorescent microplate reader (excitation 485 nm and emission 538 nm; Perkin-Elmer Instruments). The intracellular ROS levels were expressed as fluorescence intensity (picogreen).
Statistical analysis
Data are expressed as the mean ± SEM of n experiments. To determine statistical significance, Student's t test was used for comparing a single treatment mean with a control mean, and a one-way analysis of variance followed by a Tukey–Kramer multiple comparisons test was used for the analysis of multiple treatment means. Values of p less than 0.05 were considered significant.
Results
Animal body weight changes and colon weight/colon length ratio
Three days after intracolonic administration of DNBS (8 mg/mouse), a significant (p < 0.001) body weight loss (weight variation: control 0.02 ± 0.11 g, DNBS −6.55 ± 0.26 g; p < 0.001, n = 8–10 animals) was observed. The treatment of animals with CBD, at the doses of 1–10 mg/kg, significantly reduced DNBS-induced effects on body weight (weight variation: DNBS −6.55 ± 0.26 g; CBD 1 mg/kg, −6.14 ± 0.25 g; CBD 2.5 mg/kg, −5.88 ± 0.54 g; CBD 5 mg/kg, −4.50 ± 0.70 g; CBD 10 mg/kg, −4.85 ± 0.31; p < 0.05 at the 5- and 10-mg/kg doses, n = 8–10 animals). In control mice (i.e., mice not given DNBS), CBD 5 mg/kg caused a significant (p < 0.05) reduction in body weight after a 6-day treatment [weight variation (g): vehicle, +2.82 ± 0.61; +CBD, 0.72 ± 0.56, n = 5].
DNBS administration caused a significant (p < 0.001) increase in colon weight/colon length ratio (Fig. 1a). The exposure of the animals to CBD, at the doses ranging from 1 to 10 mg/kg significantly (p < 0.01) reduced the effects of DNBS (Fig. 1a). The maximal protective effect of CBD in colon weight/colon length ratio was achieved with the 5-mg/kg dose.
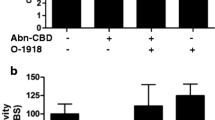
Dinitrobenzene sulfonic acid (DNBS)-induced colitis in mice. Colon weight/colon length ratio and macroscopic score of colons from untreated and DNBS-treated mice in the presence or absence of cannabidiol (CBD). Macroscopic score was assessed 3 days after DNBS (8 mg/mouse, intracolonically) administration. CBD (1–10 mg/kg, IP) was administered once a day for six consecutive days starting 3 days before DNBS administration. Results are mean ± SEM of eight to ten animals. #p < 0.001 vs control (Ctrl), **p < 0.01 and ***p < 0.001 vs DNBS alone
Macroscopic examination
No macroscopic damage was detected in the colon tissues of control mice. In contrast, mice treated with DNBS exhibited macroscopic signs of colitis including mild edema and hyperemia and sometimes adhesions to the small bowel. Treatment with CBD (1–10 mg/kg) significantly (p < 0.001) reduced the macroscopic damage associated with DNBS administration (Fig. 1b). The maximal protective effect was achieved with the 5-mg/kg dose of CBD.
Microscopic examination
Colonic mucosa of healthy control animals showed normal appearance with intact epithelium (Fig. 2a). In the DNBS group, colons showed mucosal injury which was characterized by the absence of epithelium (partially substituted by fibrin and granulocytes) and by mucosal and submucosal infiltration of inflammatory cells with edema (Fig. 2b). CBD (5 mg/kg) reduced the signs of colon injury (microscopic score: control, 0.17 ± 0.17; DNBS, 7.67 ± 0.42; CBD, 3.33 ± 0.21, n = 6, p < 0.001). In the colon of CBD (5 mg/kg)-treated animals, the glands were regenerating, and edema in mucosa and submucosa was reduced (Fig. 2c).
Histological evaluations of inflamed and non-inflamed colons. No histological modification was observed in the mucosa and submucosa of control mice (a). Mucosal injury induced by dinitrobenzene sulfonic acid administration (DNBS, 8 mg/mouse, intracolonically) was characterized by the absence of epithelium and massive mucosal and submucosal inflammatory cell infiltration (b). Treatment with cannabidiol caused a regeneration of the glands and a reduction of edema in mucosa and submucosa (c). Histological analysis was performed 3 days after DNBS administration. CBD (5 mg/kg, IP) was administered once a day for six consecutive days starting 3 days before DNBS administration. Original magnification ×200. The figure is representative of six experiments (see “Results”)
COX-2 and iNOS expression
Western blot analysis revealed the expression of COX-2 in colonic tissues of both normal and DNBS-treated animals (Fig. 3a). However, the densitometric analysis indicated a significant (p < 0.001) increase in the expression of COX-2 in the inflamed tissues (Fig. 3a). CBD (5 mg/kg) did not cause significant changes in the expression of COX-2 (Fig. 3a).
Cyclooxygenase-2 (COX-2) (a) and inducible nitric oxide synthase (iNOS) (b) expression in colonic tissues of animals treated or not with dinitrobenzene sulfonic acid (DNBS, 8 mg/mouse, intracolonically): effect of cannabidiol (CBD). Measurements were performed 3 days after DNBS administration. CBD (5 mg/kg, IP) was administered once a day for six consecutive days starting 3 days before DNBS administration. Results are means ± SEM of four experiments. #p < 0.001 vs control (Ctrl), *p < 0.05 vs DNBS. Insert, representative Western blot
No appreciable detection of iNOS expression was observed in the colon of healthy animals (Fig. 3b). In contrast, in the DNBS-exposed colon, a significant (p < 0.001) induction of iNOS expression was detected (Fig. 3b). CBD treatment (5 mg/kg) significantly (p < 0.05) reduced the overexpression of iNOS induced by DNBS (Fig. 3b).
Nitrite measurement
The levels of nitrites, the stable metabolites of NO, were significantly (p < 0.001) elevated in the colon after intracolonic administration of DNBS (Fig. 4). Treatment with CBD (5 mg/kg) significantly (p < 0.001) attenuated the stimulated nitrite production (Fig. 4).
Effect of cannabidiol (CBD) on nitrite levels in colonic tissues of animals treated with dinitrobenzene sulfonic acid (DNBS). Assay was performed 3 days after DNBS administration (DNBS, 8 mg/mouse, intracolonically). CBD (5 mg/kg, IP) was administered once a day for six consecutive days starting 3 days before DNBS administration. Results are mean ± SEM of four experiments. #p < 0.01 vs control (Ctrl), ***p < 0.001 vs DNBS
IL-1β and IL-10 levels
The levels of interleukin-1β were significantly (p < 0.001) increased by DNBS (Fig. 5a). In contrast, IL-10 production significantly decreased in samples from DNBS-treated mice (Fig. 5b). Treatment with CBD counteracted the changes in IL-1β and IL-10 levels observed in the inflamed colons (Fig. 5a, b).
Effect of cannabidiol (CBD) on interleukin-1β (IL-1β) (a) and interleukin-10 (IL-10) (b) levels in mouse colons treated with dinitrobenzene sulfonic acid (DNBS). Assay was performed 3 days after DNBS administration (DNBS, 8 mg/mouse, intracolonically). CBD (5 mg/kg, IP) was administered once a day for six consecutive days starting 3 days before DNBS administration. Results (expressed as picograms per milligram of proteic extract) are mean ± SEM of four experiments. #p < 0.001 vs control (Ctrl), ***p < 0.001 vs DNBS
Endocannabinoid levels
The levels of both anandamide and 2-arachydonylglycerol (2-AG) were significantly increased by treatment with DNBS (p < 0.01). Treatment with CBD (5 mg/kg) significantly counteracted these changes (p < 0.01), although it did not completely restore control levels (Table 1). CBD treatment did not affect endocannabinoid levels in control mice (Table 1).
FAAH mRNA expression
The relative expression analysis, evaluated by quantitative RT-PCR, of FAAH mRNA in colon samples from control, DNBS-, and DNBS + CBD-treated mice is depicted in Fig. 6. Colons from DNBS-treated animals showed a significant decrease in FAAH mRNA expression, which was not significantly further modified by CBD (5 mg/kg)
Relative expression of fatty acid amide hydrolase (FAAH) mRNA in colonic tissues of animals treated or not with dinitrobenzene sulfonic acid (DNBS, 8 mg/mouse, intracolonically): effect of cannabidiol (CBD). Measurements were performed 3 days after DNBS administration. CBD (5 mg/kg, IP) was administered once a day for six consecutive days starting 3 days before DNBS administration. Total RNA extracted from colons of DNBS-treated mice and controls was subjected to quantitative (real-time) RT-PCR analysis as described in “Materials and methods.” Data were analyzed by GENEX software for groupwise comparisons and statistical analysis. The lowest expression value for each target was considered as 1. Results are means ± SEM of three experiments. **p < 0.001 vs control (Ctrl)
Cytotoxicity assay
In the MTT assay, CBD (up to 10−5 M) had no significant cytotoxic effect on Caco-2 cells after a 24-h exposure (% viability: control, 100 ± 0.0; CBD 10−8 M, 102.05 ± 5.2; CBD 3 × 10−8 M, 101.8 ± 6.54; CBD 10−7 M, 104.9 ± 6.83; CBD 3 × 10−7 M, 97.58 ± 7.5; CBD 10−6 M, 98.27 ± 9.4; CBD 3 × 10−6 M, 106.3 ± 5.0; CBD 10−5 M, 97.37 ± 13.2, n = 8). DMSO (6%, v/v), used as positive control, significantly (p < 0.001) reduced the cell viability in Caco-2 cells [control, 100 ± 0.0; DMSO 6% (v/v), 37.85 ± 5.2, n = 8].
Antioxidant assays on Caco-2 cells
Fenton's reagent [hydrogen peroxide (1 mM) plus iron(II) ions (1 mM)] induced an oxidative stress in Caco-2 cells after a 3-h exposure, resulting in MDA production (Fig. 7a). Pre-incubation of Caco-2 cells for 24 h with CBD (10−8–10−5 M) significantly and in a concentration-dependent manner (p < 0.05–0.01) reduced the increase of H2O2/Fe2+-induced MDA cytosolic levels (Fig. 7a).
Intracellular malondialdehyde (MDA) (a) and reactive oxygen species (ROS) production (b) produced by Fenton's reagent (1 mM H2O2/Fe2+ for MDA and 2 mM H2O2/Fe2+ for ROS) in 7 days differentiated Caco-2 cells after 24-h exposure to cannabidiol (CBD, 10−8–10−5 M). Results are mean ± SEM of five experiments. #p < 0.001 vs control (Ctrl), *p < 0.05, and **p < 0.01 vs H2O2/Fe2+ alone
The exposure of the Caco-2 cells to H2O2/Fe2+ (2 mM) produced a significant (p < 0.001) increase in ROS formation (Fig. 7b). A pretreatment for 24 h with CBD (10−8–10−5 M) reduced ROS formation as measured by the inhibition of DCF fluorescence intensity (Fig. 7b). This effect was significant (p < 0.05) at the highest concentration tested (10−5 M).
Discussion
Despite tremendous progress being made in our understanding of the pathobiology of IBD, the pharmacological treatment of this condition continues to be unsatisfactory. Since anecdotal reports suggest that Cannabis extracts may relieve the symptoms of patients with IBD [15], we evaluated the effect of CBD, one of the main non-psychotropic ingredients of marijuana, in the DNBS model of experimental colitis. We found that CBD was profoundly beneficial in vivo and also attenuated the degree of lipid peroxidation and ROS production in intestinal epithelial cells.
We found that CBD reduced the decrease in body weight associated with DNBS administration. In addition, macroscopic evaluations of the colon revealed that the severity of damage was drastically reduced in animals pretreated with CBD. CBD also reduced the wet weight/colon length ratio of the inflamed colonic tissue, which is considered a reliable and sensitive indicator of the severity and extent of the inflammatory response [24], thus further supporting the hypothesis of a beneficial action of CBD in the inflamed gut. In these experiments, we found that the dose of 5 mg/kg exerted an optimal therapeutic effect. Indeed, low doses (1 and 2.5 mg/kg) were weakly active (with non-statistically significant protective effects), while the higher dose (10 mg/kg) did not exert a further beneficial effect compared to the 5-mg/kg dose. Therefore, further experiments and measurements (e.g., histology, enzymes expression, interleukins, and endocannabinoid levels) were performed with the 5-mg/kg dose. Thus, histological examination showed that CBD 5 mg/kg reduced the signs of colon injury; specifically, CBD reduced edema in the mucosa and in the submucosa and caused gland regeneration.
In order to investigate possible molecular changes associated with the beneficial effect of CBD, observed here through macroscopical and histological evaluations, we evaluated enzymes (i.e., iNOS, COX-2) and mediators (i.e., IL-1β, IL10, endocannabinoids) involved in the protection of intestinal mucosa and also performed experiments in isolated intestinal epithelial cells. Such experiments are discussed in detail below.
The inducible form of the iNOS that is responsible for high-output production of NO from the amino acid l-arginine is up-regulated in various forms of mucosal inflammation [25]. It is believed that the level of iNOS-derived NO correlates well with disease activity in ulcerative colitis, and the majority of animal experiments have shown improvement in experimental IBD with iNOS inhibitors [25]. Previous investigators have shown that CBD reduced the overexpression of iNOS both in the inflamed rat paw [26] and in endothelial cells treated with a pro-inflammatory stimulus [27]. Our study demonstrated that CBD attenuated the expression of iNOS in the colon of DNBS-treated mice, which could contribute to the anti-inflammatory effects of this marijuana component. In line with these results, we also observed a reduction of nitrite production (the stable metabolites of NO) in animals treated with CBD.
Similarly to iNOS, colonic COX-2 is markedly elevated in experimental models of IBD [28] as well as in IBD patients’ biopsies [29]. COX-2 inhibitors have been shown both to ameliorate and to exacerbate the severity of experimental colitis [30, 31].We have demonstrated here that the expression of COX-2 protein was increased in the colon of DNBS-treated mice, and such increase was not significantly modified by CBD, thus arguing against an involvement of COX-2 in CBD-induced intestinal anti-inflammatory effects. Consistent with our results, others have shown that COX-2 activity and content were not affected by CBD in glioma tumor tissues [32].
Interleukins are cytokines involved in a variety of biological processes, including cell activation, growth, and differentiation, and they are central to the development of intestinal inflammation [33]. Among various cytokines, IL-1β plays an important pro-inflammatory role in the initiation and amplification of the inflammatory response leading to intestinal injury [33]. In contrast, IL-10 is a regulatory cytokine which inhibits pro-inflammatory cytokines release, resulting in anti-inflammatory effect within the gut [34]. Dysregulation of IL-1β and IL-10 levels (i.e., enhanced IL-1β and decreased IL-10 levels) has been demonstrated in the colon obtained from patients with ulcerative colitis [35], and administration of IL-1Ra antagonists reduces experimentally induced intestinal inflammation [36]. In the present study, we have observed that intracolonic administration of DNBS causes an increase in colonic IL-1β as well as a decrease in IL-10 levels. More importantly, we have shown that CBD counteracted the colonic variation of both IL-1β and IL-10 levels, thus suggesting the possible involvement of these cytokines. Consistent with our results, it has been recently shown that CBD impairs IL-1β protein expression and release induced in the rat dorsal hippocampus by the administration of the Alzheimer β-amyloid peptide [37].
Increased production of endocannabinoids (i.e., anandamide and/or 2-AG) has been observed both experimentally and in IBD patients’ biopsies [15]. In well-established models of IBD in rodents, including the DNBS model of colitis, endocannabinoids may limit intestinal inflammation in vivo via cannabinoid CB1 and/or CB2 receptor activation [14, 15, 38, 39]. This assumption is mainly based on the observation that pharmacological enhancement of intestinal endocannabinoid levels, through inhibition of the degrading enzyme FAAH, has been shown to be protective in experimental models of ulcerative colitis in rodents [12, 13]. In the digestive tract, FAAH inhibition is associated with the increased levels of both anandamide and 2-AG [40, 41]. Because CBD has been shown to inhibit FAAH [10] and may reduce intestinal motility in the inflamed gut through a FAAH-mediated mechanism [17, 42], we investigated the possible involvement of FAAH in CBD mode of action by measuring endocannabinoid levels in inflamed tissues from animals treated or not with CBD. Similar to previous results [12, 13], we found that DNBS administration to mice was accompanied by increased colon levels of endocannabinoids. We also observed down-regulation of FAAH mRNA as compared to control mice. However, contrary to what one would expect from a putative inhibitory effect on FAAH, CBD neither increased colon endocannabinoid levels—and, in fact, significantly decreased them—nor did it change FAAH mRNA expression in DNBS-treated mice. In addition, CBD treatment had no effect on endocannabinoid levels in control mice. These observations rule against an involvement of FAAH in the protective effect of CBD.
A critical event in the development of inflammation in the gut is the impairment of antioxidant defense of intestinal epithelial cells leading to oxidative stress [18]. To evaluate the possible effects of CBD on oxidative stress, we used the human colon adenocarcinoma Caco-2 cell line which has been used to examine a variety of intestinal (dys)functions, including those related to intestinal mucosa inflammation. We showed here for the first time in intestinal cells that CBD reduced, in a concentration-dependent manner, ROS production and lipid peroxidation, a relevant finding in light of the observation that ROS production leading to oxidative stress constitutes a major tissue-destructive force contributing significantly to the pathogenesis of IBD [43]. The antioxidant properties of CBD in intestinal epithelial cells might contribute to the beneficial effect of this plant compound against DNBS-induced colitis observed in vivo in the present study. Others have shown that CBD exerts protective effects against lipid peroxidation and/or ROS production in retinal, pheocromocytoma, and neuronal cells [44–46].
In conclusion, our results show that the degree of intestinal inflammation caused by intracolonic administration of DNBS is substantially reduced by treatment of mice with the Cannabis-derived ingredient CBD. The effect of CBD is associated with the down-regulation of iNOS (but not COX-2) expression and modulation of cytokine (IL-1β and IL-10) levels, whereas it does not involve FAAH inhibition or interference with endocannabinoid inactivation mechanisms in general. Studies on intestinal epithelial cells suggest that CBD prevents oxidative stress, which may be one of the underlying factors leading to mucosal protection in vivo.
Abbreviations
- 2-AG:
-
2-Arachydonylglycerol
- CBD:
-
Cannabidiol
- COX-2:
-
Cyclooxygenase-2
- DMEM:
-
Dulbecco's modified Eagle’s medium
- DNBS:
-
2,4,6-Dinitrobenzene sulfonic acid
- ELISA:
-
Enzyme-linked immunosorbent assay
- FAAH:
-
Fatty acid amide hydrolase
- FBS:
-
Fetal bovine serum
- iNOS:
-
Inducible nitric oxide synthase
- H2DCF-DA:
-
2′,7′-Dichlorfluorescein-diacetate
- IL-1β:
-
Interleukin-1β
- IL-10:
-
Interleukin 10
- MDA:
-
Malondialdehyde
- MTT:
-
3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide
- PBS:
-
Phosphate-buffered saline
- ROS:
-
Reactive oxygen species
- TBA:
-
Thiobarbituric acid
References
Lichtenstein GR, Abreu MT, Cohen R, Tremaine W (2006) American Gastroenterological Association Institute technical review on corticosteroids, immunomodulators, and infliximab in inflammatory bowel disease. Gastroenterology 130:940–987
Colombel JF, Watson AJ, Neurath MF (2008) The 10 remaining mysteries of inflammatory bowel disease. Gut 57:429–433
Kozuch PL, Hanauer SB (2008) Treatment of inflammatory bowel disease: a review of medical therapy. World J Gastroenterol 14:354–377
Mechoulam R, Ben-Shabat S (1999) From gan-zi-gun-nu to anandamide and 2-arachidonoylglycerol: the ongoing story of cannabis. Nat Prod Rep 16:131–143
Di Marzo V (2008) Targeting the endocannanbinoid system: to enhance or to reduce. Nat Rev Drug Discov 7:438–455
Mechoulam R, Peters M, Murillo-Rodriguez E, Hanus LO (2007) Cannabidiol—recent advances. Chem Biodivers 4:1678–1692
Cunha JM, Carlini EA, Pereira AE, Ramos OL, Pimentel C, Gagliardi R, Sanvito WL, Lander N, Mechoulam R (1980) Chronic administration of cannabidiol to healthy volunteers and epileptic patients. Pharmacology 21:175–185
McPartland JM, Glass M, Pertwee RG (2007) Meta-analysis of cannabinoid ligand binding affinity and receptor distribution: interspecies differences. Br J Pharmacol 152:583–593
Pertwee RG (2008) The diverse CB1 and CB2 receptor pharmacology of three plant cannabinoids: delta9-tetrahydrocannabinol, cannabidiol and delta9-tetrahydrocannabivarin. Br J Pharmacol 153:199–215
Bisogno T, Hanus L, De Petrocellis L, Tchilibon S, Ponde DE, Brandi I, Moriello AS, Davis JB, Mechoulam R, Di Marzo V (2001) Molecular targets for cannabidiol and its synthetic analogues: effect on vanilloid VR1 receptors and on the cellular uptake and enzymatic hydrolysis of anandamide. Br J Pharmacol 134:845–852
Massa F, Marsicano G, Hermann H, Cannich A, Monory K, Cravatt BF, Ferri GL, Sibaev A, Storr M, Lutz B (2004) The endogenous cannabinoid system protects against colonic inflammation. J Clin Invest 113:1202–1209
D'Argenio G, Valenti M, Scaglione G, Cosenza V, Sorrentini I, Di Marzo V (2006) Up-regulation of anandamide levels as an endogenous mechanism and a pharmacological strategy to limit colon inflammation. FASEB J 20:568–570
Storr MA, Keenan CM, Emmerdinger D, Zhang H, Yüce B, Sibaev A, Massa F, Buckley NE, Lutz B, Göke B, Brand S, Patel KD, Sharkey KA (2008) Targeting endocannabinoid degradation protects against experimental colitis in mice: involvement of CB1 and CB2 receptors. J Mol Med 86:925–936
Di Marzo V, Izzo AA (2006) Endocannabinoid overactivity and intestinal inflammation. Gut 55:1373–1376
Izzo AA, Camilleri M (2008) Emerging role of cannabinoids in gastrointestinal and liver diseases: basic and clinical aspects. Gut 57:1140–1155
Ligresti A, Moriello AS, Starowicz K, Matias I, Pisanti S, De Petrocellis L, Laezza C, Portella G, Bifulco M, Di Marzo V (2006) Antitumor activity of plant cannabinoids with emphasis on the effect of cannabidiol on human breast carcinoma. J Pharmacol Exp Ther 318:1375–1387
Capasso R, Borrelli F, Aviello G, Romano B, Scalisi C, Capasso F, Izzo AA (2008) Cannabidiol, extracted from Cannabis sativa, selectively inhibits inflammatory hypermotility in mice. Br J Pharmacol 154:1001–1008
Xavier RJ, Podolsky DK (2007) Unravelling the pathogenesis of inflammatory bowel disease. Nature 448:427–434
Thomsen LL, Ching LM, Zuang L, Gavin JB, Bagueley BC (1991) Tumor-dependent increased plasma nitrate concentrations as an indication of the antitumor effect of flavone-8-acetic acid and analogues in mice. Cancer Res 51:71–81
Di Marzo V, Capasso R, Matias I, Aviello G, Petrosino S, Borrelli F, Romano B, Orlando P, Capasso F, Izzo AA (2008) The role of endocannabinoids in the regulation of gastric emptying: alterations in mice fed a high fat diet. Br J Pharmacol 153:1272–1280
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65:55–63
Esterbauer H, Cheeseman KH (1990) Determination of aldehydic lipid peroxidation products: malonaldehyde and 4-hydroxynonenal. Methods Enzymol 186:407–421
Yokomizo A, Moriwaki M (2006) Effects of uptake of flavonoids on oxidative stress induced by hydrogen peroxide in human intestinal Caco-2 cells. Biosci Biotechnol Biochem 70:1317–1324
Gálvez J, Garrido M, Merlos M, Torres MI (2000) Zarzuelo A (2000) Intestinal anti-inflammatory activity of UR-12746, a novel 5-ASA conjugate, on acute and chronic experimental colitis in the rat. Br J Pharmacol 130:1949–1959
Kolios G, Valatas V, Ward SG (2004) Nitric oxide in inflammatory bowel disease: a universal messenger in an unsolved puzzle. Immunology 113:427–437
Costa B, Trovato AE, Comelli F, Giagnoni G, Colleoni M (2007) The non-psychoactive cannabis constituent cannabidiol is an orally effective therapeutic agent in rat chronic inflammatory and neuropathic pain. Eur J Pharmacol 556:75–83
Rajesh M, Mukhopadhyay P, Bátkai S, Haskó G, Liaudet L, Drel VR, Obrosova IG, Pacher P (2007) Cannabidiol attenuates high glucose-induced endothelial cell inflammatory response and barrier disruption. Am J Physiol Heart Circ Physiol 293:H610–H619
Wallace JL (2006) COX-2: a pivotal enzyme in mucosal protection and resolution of inflammation. ScientificWorldJournal 6:577–588
Singer II, Kawka DW, Schloemann S, Tessner T, Riehl T, Stenson WF (1998) Cyclooxygenase 2 is induced in colonic epithelial cells in inflammatory bowel disease. Gastroenterology 115:297–306
Dudhgaonkar SP, Tandan SK, Kumar D, Raviprakash V, Kataria M (2007) Influence of simultaneous inhibition of cyclooxygenase-2 and inducible nitric oxide synthase in experimental colitis in rats. Inflammopharmacology 15:188–195
Reuter BK, Asfaha S, Buret A, Sharkey KA, Wallace JL (1996) Exacerbation of inflammation-associated colonic injury in rat through inhibition of cyclooxygenase-2. J Clin Invest 98:2076–2085
Massi P, Valenti M, Vaccani A, Gasperi V, Perletti G, Marras E, Fezza F, Maccarrone M, Parolaro D (2008) 5-Lipoxygenase and anandamide hydrolase (FAAH) mediate the antitumor activity of cannabidiol, a non-psychoactive cannabinoid. J Neurochem 104:1091–1110
Siegmund B (2002) Interleukin-1beta converting enzyme (caspase-1) in intestinal inflammation. Biochem Pharmacol 64:1–8
Barbara G, Xing Z, Hogaboam CM, Gauldie J, Collins SM (2000) Interleukin 10 gene transfer prevents experimental colitis in rats. Gut 46:344–349
Madsen K (2002) Combining T cells and IL-10: a new therapy for Crohn's disease? Gastroenterology 123:2140–2144
Cominelli F, Nast CC, Duchini A, Lee M (1992) Recombinant interleukin-1 receptor antagonist blocks the proinflammatory activity of endogenous interleukin-1 in rabbit immune colitis. Gastroenterology 103:65–71
Esposito G, Scuderi C, Savani C, Steardo L Jr, De Filippis D, Cottone P, Iuvone T, Cuomo V, Steardo L (2007) Cannabidiol in vivo blunts beta-amyloid induced neuroinflammation by suppressing IL-1beta and iNOS expression. Br J Pharmacol 151:1272–1279
Kimball ES, Schneider CR, Wallace NH, Hornby PJ (2006) Agonists of cannabinoid receptor 1 and 2 inhibit experimental colitis induced by oil of mustard and by dextran sulfate sodium. Am J Physiol Gastrointest Liver Physiol 291:G364–G371
Wright KL, Duncan M, Sharkey KA (2008) Cannabinoid CB2 receptors in the gastrointestinal tract: a regulatory system in states of inflammation. Br J Pharmacol 153:263–270
Capasso R, Matias I, Lutz B, Borrelli F, Capasso F, Marsicano G, Mascolo N, Petrosino S, Monory K, Valenti M, Di Marzo V, Izzo AA (2005) Fatty acid amide hydrolase controls mouse intestinal motility in vivo. Gastroenterology 129:941–951
Izzo AA, Aviello G, Petrosino S, Orlando P, Marsicano G, Lutz B, Borrelli F, Capasso R, Nigam S, Capasso F, Di Marzo V (2008) Increased endocannabinoid levels reduce the development of precancerous lesions in the mouse colon. J Mol Med 86:89–98
De Filippis D, Iuvone T, D'amico A, Esposito G, Steardo L, Herman AG, Pelckmans PA, de Winter BY, de Man JG (2008) Effect of cannabidiol on sepsis-induced motility disturbances in mice: involvement of CB receptors and fatty acid amide hydrolase. Neurogastroenterol Motil 20:919–927
Kruidenier L, Verspaget HW (2002) Review article: oxidative stress as a pathogenic factor in inflammatory bowel disease—radicals or ridiculous? Aliment Pharmacol Ther 16:1997–2015
El-Remessy AB, Al-Shabrawey M, Khalifa Y, Tsai NT, Caldwell RB, Liou GI (2006) Neuroprotective and blood-retinal barrier-preserving effects of cannabidiol in experimental diabetes. Am J Pathol 168:235–244
Esposito G, De Filippis D, Carnuccio R, Izzo AA, Iuvone T (2006) The marijuana component cannabidiol inhibits beta-amyloid-induced tau protein hyperphosphorylation through Wnt/beta-catenin pathway rescue in PC12 cells. J Mol Med 84:253–258
Hampson AJ, Grimaldi M, Axelrod J, Wink D (1998) Cannabidiol and (−)Delta9-tetrahydrocannabinol are neuroprotective antioxidants. Proc Natl Acad Sci USA 95:8268–8273
Acknowledgments
We are grateful to GW Pharmaceuticals (Porton Down, Wiltshire, UK) for providing us cannabidiol.
Author information
Authors and Affiliations
Corresponding author
Additional information
Francesca Borrelli, Gabriella Aviello, Barbara Romano, Pierangelo Orlando, Rafaelle Capasso, Federico Guadagno, Stefania Petrosino, Vincenzo Di Marzo, and Angelo A, Izzo are members of the Endocannabinoid Research Group.
Rights and permissions
About this article
Cite this article
Borrelli, F., Aviello, G., Romano, B. et al. Cannabidiol, a safe and non-psychotropic ingredient of the marijuana plant Cannabis sativa, is protective in a murine model of colitis. J Mol Med 87, 1111–1121 (2009). https://doi.org/10.1007/s00109-009-0512-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-009-0512-x