Abstract
Purpose
We propose a functional treatment strategy for fragility fractures of the pelvis (FFP) in geriatric patients; patients with such fractures normally undergo 10 days of conservative therapy with full-weight bearing within pain limits. Conservative therapy for FFP is continued for patients who can stand with assistance, and surgical stabilization is recommended for patients with difficulty in auxiliary standing at 10 day postadmission. This study aimed to compare the outcomes of functional treatment between geriatric patients with FFP type I/II and those with FFP type III/IV, as described by Rommens et al.
Methods
We conducted a retrospective study of 84 geriatric patients who underwent functional treatment for FFP. Based on the results of the first examination, the patients were allocated to the following FFP types: type I/II (n = 53) and type III/IV (n = 31). Change in functional mobility scale described by Graham et al. from before injury to the final follow-up were compared between the groups.
Results
There was no significant difference in the functional mobility scale (0.25 ± 0.70 vs. 0.23 ± 0.56, p = 0.889) between FFP type I/II and FFP type III/IV.
Conclusion
The outcomes of the functional treatment for FFP for the geriatric patients did not differ significantly between the radiographic classifications. Functional treatment could, therefore, be a treatment option for almost all radiographic types of FFP, especially for geriatric patients. Further investigations are warranted.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Rommens et al. [1, 2] recently developed a radiographic classification for managing fragility fractures of the pelvis (FFP). Conservative therapy is recommended for FFP types I (anterior lesions only) and II (nondisplaced posterior lesions), whereas surgical stabilization is efficacious for FFP types III (displaced unilateral posterior lesions) and IV (displaced bilateral posterior lesions). Nevertheless, the classification of FFP and its management remain a matter of debate [3, 4].
The radiographic classification of FFP and its management as recommended by Rommens et al. [1, 2] may exaggerate the role of surgical interventions for FFP [5,6,7]. Although various minimally invasive surgical stabilizations have been developed [8,9,10,11], postoperative complications (e.g., screw loosening) can occur and require revision surgery [12, 13]. A primary goal of treatment is functional recovery [14]; therefore, radiographs and function are important parameters for determining the optimal FFP treatment [3]. Interestingly, 10 days of bed rest has had no effect on physical performance in geriatric populations [15], and in-hospital complications remain high in patients with FFP, even when treated operatively [16]. We, therefore, propose a functional treatment strategy for FFP in geriatric patients (Fig. 1).
Functional treatment strategy for fragility fractures of the pelvis (FFP). Initially, all patients undergo conservative therapy with full-weight bearing within pain. Continuation of conservative therapy for FFP is recommended for patients who can stand at 10 days after being diagnosed with FFP, and surgical stabilization for FFP is recommended for patients who cannot stand due to permanent pelvic pain at 10 days after being diagnosed with FFP. FFP fragility fractures of the pelvis
In patients with FFP, weight bearing within 12 weeks seems likely to have little impact on fracture displacement in the coronal plane (0.2–0.8 mm), irrespective of FFP type [5], which may be attributable to the fact that weight bearing applies force not only to the hip but also to the intact ligaments [14] and muscles (e.g., adductor, biceps femoris, gluteus, obturator, rectus femoris [17]) [18, 19]. We, therefore, hypothesize that outcomes of functional treatment for FFP might not differ significantly among the radiographic classifications of FFP described by Rommens et al. [1, 2]. This study aimed at comparing the outcomes of functional treatment for FFP type I/II and FFP type III/IV in geriatric patients.
Methods
Study design and participants
We conducted a retrospective study comparing the outcomes of functional treatment for FFP type I/II and FFP type III/IV in geriatric patients. Of the 95 consecutive patients with FFP between February 2013 and December 2019, 84 geriatric patients who had undergone functional treatment for FFP were considered eligible for this study. Those who lacked evaluable data (eight patients) or were younger than 65 years (three patients) were excluded from the study. Table 1 summarizes the patients’ characteristics.
Functional treatment strategy for fragility fractures of the pelvis
First-line treatment
Initially, all patients underwent conservative therapy with full-weight-bearing exercises within pain limits. A rehabilitation therapy program typically consists of 40 min of therapy per day at least 5 days per week. Patients with swallowing ability take 60-mg loxoprofen orally; those without the ability take 25-mg diclofenac sodium as a suppository. Patients who cannot tolerate nonsteroidal anti-inflammatory drugs take 200–400 mg acetaminophen orally. Analgesics are administered on request. Patients are allowed to take analgesics every 6–8 h.
Second-line treatment
Difficulty in standing, defined as difficulty with auxiliary standing on 1 leg and/or 2 legs due to permanent pelvic pain, was assessed at 10 days after being diagnosed with FFP. Continuing the conservative therapy for FFP is recommended for patients who have no difficulty in standing, and surgical stabilization for FFP is recommended for patients who do have difficulty in standing. The surgical procedure was as minimally invasive as possible. Basically, FFP types II–IV were fixed in a percutaneous procedure (iliosacral and/or trans-sacral screw); however, open reduction and internal fixation were performed in FFP type III/IV, particularly in cases with large fracture displacement.
Radiographic study
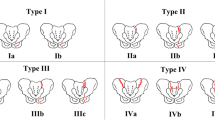
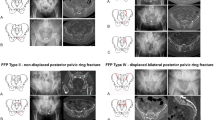
The author (KH) of this study, an orthopedic trauma consultant specialized in pelvic and lower extremity trauma, classified all fractures on radiographs and/or computed tomography (CT) during the first examination (outpatient) and at the final follow-up, according to the Rommens FFP classification [1, 2] (Fig. 2). Based on the results of the first examination, the patients were allocated to FFP type I/II or FFP type III/IV.
Rommens classification of fragility fractures of the pelvis (FFP) [1, 2]; unilateral anterior pelvic ring disruption (FFP type Ia); bilateral anterior pelvic ring disruption (FFP type Ib); dorsal nondisplaced posterior injury only (FFP type IIa); sacral crush with anterior disruption (FFP type IIb); nondisplaced sacral, sacroiliac, or iliac fracture with anterior disruption (FFP type IIc); displaced unilateral ilium fracture and anterior disruption (FFP type IIIa); displaced unilateral sacroiliac disruption and anterior disruption (FFP type IIIb); displaced unilateral sacral fracture together with anterior disruption (FFP type IIIc); bilateral iliac fractures or bilateral sacroiliac disruptions together with anterior disruption (FFP type IVa); spinopelvic dissociation together with anterior disruption (FFP type IVb); and combination of various posterior instabilities together with anterior disruption (FFP type IVc)
Outcome parameters
We collected demographic data, including age, sex, body mass index, time from injury to the first examination, American Society of Anesthesiologists (ASA) physical status score at the time of admission, and Rommens FFP classification at the first examination. The ASA physical status score was defined as follows: grade 1—normal, healthy patient; grade 2—mild systemic disease; grade 3—severe systemic disease that is not incapacitating; grade 4—severely incapacitating, systemic disease that is a constant threat to life; and grade 5—moribund patient [20, 21].
The study’s primary outcomes were functional mobility, which was assessed using the functional mobility scale described by Graham et al. [22, 23] before the injury, at 10 days after being diagnosed with FFP, and at the final follow-up. The change in functional mobility from before the injury to the final follow-up was subsequently calculated. The functional mobility scale is defined as follows [22, 23]: 0—full activity; 1—walking with assistance; 2—walking with assistance for short periods; 3—walking with assistance for activities of daily living/appointments only; 4—confined to a wheelchair; and 5—bedridden.
The study’s secondary outcomes were surgical intervention, fracture progression (FP), bone union, and follow-up period. The FP was defined as a fracture that progressed one or more levels according to the Rommens FFP classification on radiographs at the final follow-up [6, 13]. For instance, a change from FFP type IVb at the first examination to FFP type IVc at the final follow-up was regarded as FP. Bone union was defined as a bridging callus over the fracture site on the radiographs and/or CT. The follow-up period was defined as the time between the initial presentation and last control, at which all patients achieved weight-bearing without pain.
Statistical analysis
We employed Fisher’s exact test to compare the qualitative data between the groups, including sex, ASA physical status score, surgical intervention, and FP. We employed Student’s t test to compare the quantitative data between the groups, including age, body mass index, time from injury to the first examination, functional mobility scale (change, before fracture, at 10 days, and at final follow-up), bone union, and follow-up period. The level of significance (p value) was set at 0.05. Analyses were performed using the Statistical Package for Social Sciences program, version 19 (IBM Corp., Armonk, NY, USA).
Results
Demographic data
Table 2 summarizes the patients’ demographic data. Compared with the patients with FFP type III/IV, patients with FFP type I/II were older (85.0 ± 7.5 vs. 81.0 ± 7.8 years; p = 0.025), had a shorter time from injury to the first examination (2.9 ± 6.6 vs. 21.8 ± 28.2 days; p = 0.002), and had a lower rate of ASA 3 scores [25/53 (47.2%) vs. 23/31 (74.2%) patients; p = 0.022] and a higher rate of ASA two scores [27/53 (50.9%) vs. 8/31 (25.8%) patients; p = 0.038].
Primary outcomes
Figure 3 and Table 2 present the primary outcomes. At the final follow-up, there were no significant differences in the functional mobility scale (1.53 ± 1.54 vs. 1.16 ± 1.21, p = 0.231) between FFP type I/II and FFP type III/IV. There were no significant differences in the change in functional mobility scale (0.25 ± 0.70 vs. 0.23 ± 0.56, p = 0.889) between FFP type I/II and FFP type III/IV.
Secondary outcomes
Table 2 lists the secondary outcomes. There were no significant differences in the rate of patients who underwent surgery [6/53 (11.3%) vs. 2/31 (6.5%) patients; p = 0.704], in FP [10/53 (18.9%) vs. 3/31 (9.7%) patients; p = 0.355], or in the follow-up duration (408.7 ± 254.2 vs. 448.3 ± 280.0 days; p = 0.578) between FFP type I/II and FFP type III/IV. Patients with FFP type I/II required less time to achieve bone union (105.0 ± 73.7 vs. 155.7 ± 89.3 days; p = 0.039) than those with FFP type III/IV.
Discussion
We propose a functional treatment strategy for FFP in geriatric patients. Our main findings were that (1) patients with FFP type I/II had a shorter time from injury to the first examination than those with FFP type III/IV; (2) there were no significant differences in functional mobility scale between the patients with FFP type I/II and those with FFP type III/IV; and (3) patients with FFP type I/II required less time to achieve bone union than those with FFP type III/IV, whereas there was no significant difference in the follow-up period between the groups.
We found that late presentation was related to FFP type III/IV. Similarly, Rommens et al. [13] reported that patients who presented late were likely to experience severe FFP types. Indeed, FP from FFP type I/II to type III/IV was observed in 8.7–8.9% of patients with FFP type I/II during conservative therapy [6, 13]. It, therefore, appears likely that FP (i.e., fracture displacement on sagittal plane [13] and/or new fractures) can develop with time (late presentation and/or long-term conservative therapy). A functional treatment strategy for FFP could delay the need for surgery, which could in turn result in FP [13]. However, the time from symptoms to surgery was 11.6 days in our study and 68.4 days in a past study [12], and the rate of FP was 15.5% (13/84 patients) in our study and 14.2% (21/148 patients [13]) to 22.8% (18/79 patients [6]) in past studies. These findings indicate that the surgery was delayed for 11.6 days in a functional treatment strategy for FFP; the delay was not too long to severely impact FP. Therefore, a functional treatment strategy for FFP could not be extremely inferior to the other therapeutic strategies in terms of FP rate.
In our study, there were no significant differences in the change in functional mobility scale between the patients with FFP type I/II and those with FFP type III/IV. Similar to our findings, radiographic FFP types have been reported to not be strongly associated with the patients’ physical function [6]. The inconsistency between radiographic and functional instability could result from the complex structure of the pelvis, including ligaments [14] and muscles [17, 19], suggesting that not all patients with FFP type III/IV require surgical stabilization. Radiographic instability might be useful for deciding whether surgery should be conducted; however, the indication for surgery should be determined comprehensively, based not only on radiographs but also on physical functioning and the risk of surgery. We, therefore, propose a functional treatment strategy for FFP, focusing on physical function treatment and determining the indication for surgical stabilization based on functional instability. The surgical rate of our strategy was 10%, similar to the strategy of Ueda et al. (8%) [6] and lower than those of Rommens et al. (32%) [13] and Osterhoff et al. (42%) [7].
In this study, patients with FFP type I/II required less time to achieve bone union than those with FFP type III/IV. However, there was no significant difference in the follow-up period, which could be due to our follow-up interval that focused on physical function. Therefore, a functional therapeutic strategy for FFP type III/IV might be radiographically inferior but not functionally inferior to that for FFP type I/II.
Our study has several limitations, the first of which is its retrospective nature, and thus the patients’ functional/radiological data were not always available. However, the outcome parameters were routinely assessed at the first examination (outpatient), at 10 days after being diagnosed with FFP, and at the final follow-up (pain-free ambulatory function) in all patients with FFP in our institution. This limitation might, therefore, not affect the results. Second, the number of participants was small due to the low incidence of FFP, which could have affected the results. With the growing numbers of elderly individuals, there could be an increasing number of patients with FFP. Further investigations on this topic with sufficient statistical power are, therefore, warranted. Third, the study participants were limited to geriatric populations (≥ 65 years); therefore, a functional therapeutic strategy for FFP cannot be generalized for all patients with FFP. Although the majority of those with FFP are reported to be elderly, future studies should investigate the efficacy of this strategy in younger populations (< 65 years). Fourth, the rest pain was within manageable bounds for all patients in the present study. The rest pain without manageable bounds may require early surgery as previously reported [6, 13]; therefore, no rest pain without manageable bounds is a prerequisite for a functional treatment strategy for FFP. Fifth, the quality of life (e.g., pain and anxiety) was not assessed, because a large number of patients could have dementia. Sixth, the present study included patients with FFP type I, which are isolated fractures of the anterior pelvic ring. FFP type II/III/IV are fractures of the posterior pelvic ring. However, FFP type I can experience FP and progress to FFP type II–IV [6, 13] and was, therefore, included. Seventh, a lack of bone union in the follow-up period could influence the radiographic outcome results (e.g., FP and bone union). However, this is unlikely to significantly alter the quality of functional outcomes, given that the follow-up period was determined by achieving pain-free ambulatory function. Eighth, the time from injury to the first examination differed among the participants, which could influence the functional outcome results. As mentioned above, however, FFP types might depend on time (late presentation and/or long-term conservative therapy). Therefore, this limitation might not be avoided in studies comparing radiographic types. Ninth, the complaints of FP were unclear, given that FP was assessed based not on function but on radiographs during the first examination and the final follow-up. Nevertheless, few [2/13 (15%)] patients with FP required surgery in this study, indicating that FP might have a small impact on our therapeutic strategy.
Outcomes for the functional treatment for FFP might not differ by radiographic classification in geriatric patients. Therefore, functional treatment could be an option for treating almost all radiographic types of FFP, especially in geriatric patients. Further investigations are warranted.
Code availability
Not applicable to that section.
References
Rommens PM, Hofmann A. Comprehensive classification of fragility fractures of the pelvic ring: Recommendations for surgical treatment. Injury. 2013;44:1733–44. https://doi.org/10.1016/j.injury.2013.06.023.
Rommens PM, Ossendorf C, Pairon P, Dietz S-O, Wagner D, Hofmann A. Clinical pathways for fragility fractures of the pelvic ring: personal experience and review of the literature. J Orthop Sci. 2015;20:1–11. https://doi.org/10.1007/s00776-014-0653-9.
Krappinger D, Kaser V, Kammerlander C, Neuerburg C, Merkel A, Lindtner RA. Inter- and Intraobserver reliability and critical analysis of the FFP classification of osteoporotic pelvic ring injuries. Injury. 2019;50:337–43. https://doi.org/10.1016/j.injury.2018.11.027.
Berger-Groch J, Thiesen DM, Grossterlinden LG, Schaewel J, Fensky F, Hartel MJ. The intra- and interobserver reliability of the Tile AO, the Young and Burgess, and FFP classifications in pelvic trauma. Arch Orthop Trauma Surg. 2019;139:645–50. https://doi.org/10.1007/s00402-019-03123-9.
Natoli RM, Fogel HA, Holt D, Schiff A, Bernstein M, Summers HD, et al. Advanced imaging lacks clinical utility in treating geriatric pelvic ring injuries caused by low-energy trauma. J Orthop Trauma. 2017;31:194–9. https://doi.org/10.1097/BOT.0000000000000761.
Ueda Y, Inui T, Kurata Y, Tsuji H, Saito J, Shitan Y. Prolonged pain in patients with fragility fractures of the pelvis may be due to fracture progression. Eur J Trauma Emerg Surg. 2019. https://doi.org/10.1007/s00068-019-01150-0.
Osterhoff G, Noser J, Held U, Werner CML, Pape HC, Dietrich M. Early operative versus non-operative treatment of fragility fractures of the pelvis - a propensity matched multicenter study. J Orthop Trauma. 2019. https://doi.org/10.1097/BOT.0000000000001584.
Hopf JC, Krieglstein CF, Müller LP, Koslowsky TC. Percutaneous iliosacral screw fixation after osteoporotic posterior ring fractures of the pelvis reduces pain significantly in elderly patients. Injury. 2015;46:1631–6. https://doi.org/10.1016/j.injury.2015.04.036.
Schmitz P, Baumann F, Grechenig S, Gaensslen A, Nerlich M, Müller MB. The cement-augmented transiliacal internal fixator (caTIFI): an innovative surgical technique for stabilization of fragility fractures of the pelvis. Injury. 2015;46:S114–S12020. https://doi.org/10.1016/S0020-1383(15)30029-2.
Nakayama Y, Suzuki T, Honda A, Yamashita S, Matsui K, Ishii K, et al. Interdigitating percutaneous screw fixation for Rommens type IIIa fragility fractures of the pelvis: technical notes and preliminary clinical results. Int Orthop. 2020. https://doi.org/10.1007/s00264-020-04664-0.
Rommens PM, Wagner D, Hofmann A. Minimal invasive surgical treatment of fragility fractures of the pelvis. Chirurgia (Bucur). 2017;112:524–37. https://doi.org/10.21614/chirurgia.112.5.524.
Eckardt H, Egger A, Hasler RM, Zech CJ, Vach W, Suhm N, et al. Good functional outcome in patients suffering fragility fractures of the pelvis treated with percutaneous screw stabilisation: assessment of complications and factors influencing failure. Injury. 2017;48:2717–23. https://doi.org/10.1016/j.injury.2017.11.002.
Rommens PM, Arand C, Hopf JC, Mehling I, Dietz SO, Wagner D. Progress of instability in fragility fractures of the pelvis: an observational study. Injury. 2019;50:1966–73. https://doi.org/10.1016/j.injury.2019.08.038.
Rommens PM, Wagner D, Hofmann A. Fragility fractures of the pelvis. JBJS Rev. 2017;5:34. https://doi.org/10.2106/JBJS.RVW.16.00057.
Kortebein P, Symons TB, Ferrando A, Paddon-Jones D, Ronsen O, Protas E, et al. Functional impact of 10 days of bed rest in healthy older adults. J Gerontol A Biol Sci Med Sci. 2008;63:1076–81. https://doi.org/10.1093/gerona/63.10.1076.
Noser J, Dietrich M, Tiziani S, Werner CML, Pape HC, Osterhoff G. Mid-term follow-up after surgical treatment of fragility fractures of the pelvis. Injury. 2018;49:2032–5. https://doi.org/10.1016/j.injury.2018.09.017.
Ricci PL, Maas S, Kelm J, Gerich T. Finite element analysis of the pelvis including gait muscle forces: an investigation into the effect of rami fractures on load transmission. J Exp Orthop. 2018;5:33. https://doi.org/10.1186/s40634-018-0151-7.
Khurana B, Sheehan SE, Sodickson AD, Weaver MJ. Pelvic ring fractures: what the orthopedic surgeon wants to know. Radiographics. 2014;34:1317–33. https://doi.org/10.1148/rg.345135113.
Dickenson RP, Hutton WC, Stott JR. The mechanical properties of bone in osteoporosis. J Bone Joint Surg Br. 1981;63:233–8.
Owens WD, Felts JA, Spitznagel EL Jr. ASA physical status classifications: a study of consistency of ratings. Anesthesiology. 1978;49:239–43. https://doi.org/10.1097/00000542-197810000-00003.
Ercin E, Bilgili MG, Sari C, Basaran SH, Tanriverdi B, Edipoglu E, et al. Risk factors for mortality in geriatric hip fractures: a compressional study of different surgical procedures in 785 consecutive patients. Eur J Orthop Surg Traumatol. 2017;27:101–6. https://doi.org/10.1007/s00590-016-1843-2.
Graham HK, Harvey A, Rodda J, Nattrass GR, Pirpiris M. The functional mobility scale (FMS). J Pediatr Orthop. 2004;24:514–20. https://doi.org/10.1097/00004694-200409000-00011.
Gupta AC, Hirsch JA, Chaudhry ZA, Chandra RV, Pulli B, Galinsky JG, et al. Evaluating the safety and effectiveness of percutaneous acetabuloplasty. J Neurointerv Surg. 2012;4:134–8. https://doi.org/10.1136/jnis.2011.004879.
Funding
No funding was available for this manuscript.
Author information
Authors and Affiliations
Contributions
KH is accountable and responsible for designing the study, acquiring data, and approving the final version of the manuscript. TK is accountable and responsible for designing the study, analyzing and interpreting data, writing and revising the manuscript, and approving the final version of the manuscript. KH and TK have contributed equally to this study.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional review board of Karatsu Red Cross Hospital (registration number: 3-1) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Availability of data and material
The datasets used during the current study are not publicly available because of patient confidentiality but are available from the corresponding author on reasonable request.
Consent to participate
Not applicable to that section.
Consent for publication
All authors have seen and approved the final manuscript and have given their consent for publication.
Rights and permissions
About this article
Cite this article
Hotta, K., Kobayashi, T. Functional treatment strategy for fragility fractures of the pelvis in geriatric patients. Eur J Trauma Emerg Surg 47, 21–27 (2021). https://doi.org/10.1007/s00068-020-01484-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01484-0