Abstract
Purpose
Severe acute radiation pneumonitis (SARP) is a life-threatening complication of thoracic radiotherapy. Pre-treatment pulmonary function (PF) may influence its incidence. We have previously reported on the incidence of SARP among patients with moderate pulmonary dysfunction who received definitive concurrent chemoradiotherapy (dCCRT) for non-small cell lung cancer (NSCLC).
Methods
The clinical outcomes, dose–volume histograms (DVH), and PF parameters of 122 patients (forced expiratory volume in 1 s [FEV1%]: 60–69%) receiving dCCRT between 2013 and 2019 were recorded. SARP was defined as grade ≥3 RP occurring during or within 3 months after CCRT. Logistic regression, receiver operating characteristics curves (ROC), and hazard ratio (HR) analyses were performed to evaluate the predictive value of each factor for SARP.
Results
Univariate and multivariate analysis indicated that the ratio of carbon monoxide diffusing capacity (DLCO%; odds ratio [OR]: 0.934, 95% confidence interval [CI] 0.896–0.974, p = 0.001) and mean lung dose (MLD; OR: 1.002, 95% CI 1.001–1.003, p = 0.002) were independent predictors of SARP. The ROC AUC of combined DLCO%/MLD was 0.775 (95% confidence interval [CI]: 0.688–0.861, p = 0.001), with a sensitivity and specificity of 0.871 and 0.637, respectively; this was superior to DLCO% (0.656) or MLD (0.667) alone. Compared to the MLD-low/DLCO%-high group, the MLD-high/DLCO%-low group had the highest risk for SARP, with an HR of 9.346 (95% CI: 2.133–40.941, p = 0.003).
Conclusion
The DLCO% and MLD may predict the risk for SARP among patients with pre-treatment moderate pulmonary dysfunction who receive dCCRT for NSCLC. Prospective studies are needed to validate our findings.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Definitive concurrent chemoradiotherapy (dCCRT) is the standard of care in patients diagnosed with locally advanced (stage IIIA–B) non-small cell lung cancer (NSCLC) [1, 2]. Radiation pneumonitis (RP) is a common complication of thoracic radiation therapy, and severe acute radiation pneumonitis (SARP) of grade ≥3 may lead to life-threatening complications in certain cases [3, 4]. Numerous studies have investigated the predictors for RP, including age, smoking status, concurrent chemotherapy, dose–volume histogram (DVH) parameters, and others [5,6,7,8,9,10,11,12].
Reports suggest that the incidence of lung cancer in those with chronic obstructive pulmonary disease (COPD) is three- to four-fold higher than that of those without [13, 14]. Pre-treatment pulmonary dysfunction is common among lung cancer patients with COPD. According to international guidelines, pulmonary dysfunction is defined by forced expiratory volume in the first second to forced vital capacity (FEV1/FVC) ratios of less than 0.70 [15, 16]. Certain researchers have suggested that baseline parameters (FEV1 and others) obtained from pulmonary function (PF) testing may predict the risk of RP [8, 17,18,19]. In a prospective study, FEV1, ratio of carbon monoxide diffusing capacity (DLCO), and the exhaled fraction of nitric oxide (FeNO) prior to CCRT was found to be predictive of the incidence of RP in patients with NSCLC [11].
To date, no studies have evaluated the incidence of SARP among patients with baseline moderate pulmonary dysfunction who received dCCRT for lung cancer. Our study aimed to evaluate the correlation between the incidence of SARP and clinical characteristics, including pre-treatment PF parameters, in this select group of patients.
Materials and methods
Patients
We retrospectively reviewed the data of patients with pathological diagnoses of NSCLC in our hospital between January 2013 and March 2019. Moderate pulmonary dysfunction was defined based on the recommendations of the American Thoracic Society (ATS) and the European Respiratory Society (ERS), with ratios of actual/estimated first second of forced expiration (FEV1%) values in the range of 60–69% [20]. Among 632 patients with locally advanced NSCLC who completed dCCRT, the records of 122 demonstrated evidence of pre-treatment moderate pulmonary dysfunction.
Definition of clinical and DVH factors
The data on the clinical characteristics that were recorded included age, gender, Eastern Cooperative Oncology Group (ECOG) performance status, smoking status, TNM stage, chemotherapy regimens, and radiotherapy techniques. The lung volume was defined as the volume of the total lung excluding the gross tumor volume (GTV) [21, 22]. Vx was defined as the percentage of lung/heart volume receiving ≥x Gy. The DVH parameters recorded included the lung V5/20 and mean lung dose (MLD); they were calculated and obtained from planned dose distributions based on convolution/superposition algorithms.
Radiotherapy
Radiotherapy was delivered using intensity-modulated radiation therapy (IMRT) to a total dose of 60–66 Gy at 2.0 Gy per fraction, at five fractions per week. The targets were delineated based on International Commission on Radiation Units and Measurements (ICRU) reports 62 [23] and 83 [24]. Similar to the descriptions in our previous report, [25, 26], the GTV was defined as the macroscopically identifiable tumor including lymph nodes with a margin of more than 1 cm on planning computed tomography images. The clinical tumor volume (CTV) encompassed the GTV with 8‑ and 5‑mm margins around the lung tissue and involved lymph nodes, respectively. For superior or inferior lobe tumors, a 10- or 15-mm margin was added isotropically to the CTV to create the planning target volume (PTV). The planning organ at risk volumes (PRVs) extended for 5 mm around the spinal cord.
The dose–volume constraints for the lungs were set as follows: V5 < 65%, V20 < 35%, and MLD < 20 Gy. The maximum doses allowed to the spinal cord and heart PRVs were 50 Gy and V50 < 25%, respectively, and the mean dose was <20 Gy.
Chemotherapy regimens
All of the patients received concurrent chemotherapy during radiotherapy; the regimens included paclitaxel with carboplatin (PC) and etoposide and cisplatin (EP), in accordance with the National Comprehensive Cancer Network (NCCN) guidelines [27]. The TC and EP regimens were administered weekly and every 28 days, respectively. The chemotherapy dosing and adjustments were performed as per the NCCN panel recommendations.
Pulmonary function parameters
All the enrolled patients underwent both whole-body plethysmography (WBP) and gas (helium) dilution (MBHD) using the full MasterScreen PFT System (Jaeger Corp, Germany), which was equipped with a mixing fan, carbon dioxide (CO2) absorber, oxygen (O2) and helium supply, gas inlet and outlet, and a water vapor absorber.
The pulmonary function parameters recorded included the forced expiratory volume in 1 s% predicted (FEV1%), forced expiratory volume in 1 s/forced vital capacity (FEV1/FVC), peak expiratory flow% predicted (PEF%), maximum expiratory flow% predicted (MMEF%), maximum expiratory flow at 75% of FVC% predicted (MME75%), maximum expiratory flow at 50% of FVC% predicted (MMEF50%), maximum expiratory flow at 25% of FVC% predicted (MMEF25%), maximal voluntary ventilation% predicted (MVV%), vital capacity% predicted (VC%), residual volume/total lung capacity (RV/TLC), diffusing capacity for carbon monoxide% predicted (DLCO%), resistance in airways% predicted (Raw%), and specific airway conductance% predicted (sGaw%).
Endpoint definitions
Any RP of ≥ grade 3 according to the Common Terminology Criteria for Adverse Events (CTCAE), version 4.0 [28], during or within 3 months of completion of CCRT, was recorded as SARP. The diagnosis of SARP was confirmed by at least two experienced radiation oncologists based on the clinical symptoms, synchronous computed tomography scans of the chest (to exclude the possibility of tumor progression), and evidence of administration of inhalational oxygen and corticosteroids in the medical records.
Statistical methods
Univariate logistic regression was performed to evaluate the predictive value of the individual factors for SARP. Factors with p < 0.05 on univariate analyses were included in multivariate analysis. Spearman’s rank correlation analyses were performed to prevent multicollinearity between factors. Area under the receiver operating characteristic (ROC) curve (AUC) analysis was performed to evaluate the optimal cut-off value of the continuous predictive factors. The Cox regression model was used to define the incidence curves of SARP and obtain a hazard ratio. Data analyses were performed using the SPSS (version 25.0, IBM Corp, Armonk, NY, USA) statistical software package. All of the tests were two-sided, and a value of p < 0.05 was considered statistically significant.
Results
Patient characteristics
The baseline characteristics of the study population are summarized in Table 1. Most of the subjects were male and had a history of smoking. Overall, 67 (54.9%) were diagnosed with stage IIIA disease. A total of 48 (39.9%) patients had an ECOG performance status of 0. Overall, 31 (25.4%) patients were recorded to have SARP; 20.5% (25 patients), 3.3% (four patients), and 1.6% (two patients) had developed RP of grades 3, 4, and 5, respectively. The median interval from the completion of RT to the occurrence of SARP was 45 (21–76) days. There were no significant differences in terms of GTV volume between patients with (median: 134.4 cm3 and range: 82.80–285.70 cm3) and without (median: 128.60 cm3 and range: 79.30–266.10 cm3) SARP (p > 0.05).
Univariate analysis
As shown in Table 2, univariate analysis indicated that V20 (odds ratio [OR]: 1.082, 95% confidence interval [CI]: 1.023–1.145, p = 0.006) and MLD (OR: 1.002, 95% CI: 1.001–1.003, p = 0.004) were significantly associated with SARP. Among the PF parameters, DLCO% (OR: 0.956, 95% CI: 0.925–0.988, p = 0.007), FEV1/FVC (OR: 1.043, 95% CI: 1.006–1.082, p = 0.022), PEF% (OR: 1.030, 95% CI: 1.004–1.057, p = 0.024), MEF75% (OR: 1.027, 95% CI: 1.005–1.049, p = 0.016), and MEF50% (OR: 1.027, 95% CI: 1.001–1.055, p = 0.045) significantly correlated with the incidence of SARP. None of the clinical and pathological features including gender, age, ECOG performance status, and chemotherapy regimen demonstrated significant correlations with the occurrence of SARP in the study population.
Multivariate analysis
As shown in Table 3, Spearman’s correlation analysis demonstrated relationships between the ventilation parameters. This indicated that the DLCO% was not related to ventilation function. Multivariate logistic regression was performed using the significant factors obtained during univariate analysis; these included the V20, MLD, DLCO%, FEV1/FVC, PEF%, MEF75%, and MEF50%. On multivariate analysis, the DLCO% (OR: 0.934, 95% CI 0.896–0.974, p = 0.001) and MLD (OR: 1.002, 95% CI 1.001–1.003, p = 0.002) were independent predictive factors for SARP in the present cohort (shown in Table 4).
ROC curve analysis
The ROC curves of the DLCO% and MLD are shown in Fig. 1. The ROC curves demonstrated that the AUC of the DLCO% was 0.656 (95% CI: 0.556–0.756, p = 0.010); the optimal cut-off point of 81.10% had a sensitivity of 0.871 and specificity of 0.560. The AUC of the MLD was 0.667 (95% CI: 0.564–0.769, p = 0.042); the optimal cutoff point was 1434.56 cGy (sensitivity/specificity of 0.677/0.648, respectively). On combined analysis of the DLCO% and MLD, the AUC was found to be 0.775 (95% CI: 0.688–0.861, p = 0.001), with a sensitivity and specificity of 0.875 and 0.657, respectively.
Cox regression analysis
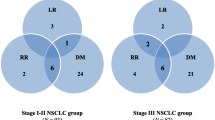
The patients were categorized into different groups based on the average MLD and DLCO% values of the cohort. Compared with patients in the MLD-low group (MLD ≤ average value), those in the MLD-high group (MLD > average value) had a higher risk of SARP, with a hazard ratio (HR) of 2.682 (95% CI: 1.234–5.826, p = 0.013). The incidence of SARP in the patients in the DLCO%-low group (DLCO% ≤ average value) was significantly higher than that of those in the DLCO%-high group (HR: 2.762, 95% CI: 1.271–6.003, p = 0.010). Compared to those in the MLD-low/DLCO%-high group, patients in the MLD-high/DLCO%-low group had the highest risk of SARP, with an HR of 9.346 (95% CI: 2.133–40.941, p = 0.003; Fig. 2).
Discussion
Numerous studies have assessed possible predictors of the risk of SARP. To the best of our knowledge, the present study is the first to evaluate the incidence of SARP among patients with NSCLC who had moderate pulmonary dysfunction. Our findings indicate that the DLCO% and MLD obtained from PF testing and DVH analysis, respectively, had potential predictive value for the occurrence of SARP in this selected population; the combination of these two factors was found to be more meaningful.
Two DVH-based parameters, namely, MLD and Vdose, were previously identified to be important predictive factors for the risk of RP in patients with NSCLC or other tumor types receiving thoracic radiotherapy. Reports from Martel et al.[29], Graham et al.[30], and Hernando et al.[31] suggested that the risk of RP with radical radiotherapy for lung cancer increased significantly in cases where the MLD was ≥20 Gy. After advancements in radiation techniques and the advent of three-dimensional conformal radiotherapy (3D-CRT and IMRT), a number of studies also demonstrated that the MLD is a potential predictor of RP even in cases where the relative values are less than 20 Gy [32,33,34,35,36]. Claude et al. found that in patients with NSCLC, the MLD, V20, and V30 were associated with the risk of severe RP (grade > or = 2) after 3D-CRT [32]. In a study including 84 patients with lung cancer, the MLD showed a clear trend towards statistical significance in the patient group without COPD [33]. In another study on patients with lung cancer, the incidence of symptomatic RP was 15.0%, and the MLD (p = 0.043) was statistically significantly related to RP [34]. Recent findings from the study by Lee et al. that used perfusion single-photon-emission computed tomography and fluorodeoxyglucose positron-emission tomography imaging also suggested that the MLD (also functional MLD) was a significant predictor of grade ≥2 pneumonitis, with a cut-off value of 13.6 Gy (functional MLD: 13.2 Gy) [35]. Our findings concur with those of these studies, indicating that the incidence of SARP definitely increased in cases where the MLD was ≥14.3 Gy.
Several studies have investigated the correlation between the DLCO and incidence of RP after thoracic radiotherapy. In 2004, Videtic et al. reported that the DLCO was a strong predictor of treatment-related toxicities after CCRT in patients with small-cell lung cancer. In their cohort of 215 patients, the incidence of toxicity-related interruptions was found to be significant for DLCO values of less than 60% (p = 0.043) [36]. In a prospective study on 53 patients with NSCLC, RP of grade ≥ 2 based on the CTCAE scale was observed in 40% (15/37); the development of RP was significantly associated with several pre-treatment PF parameters including FEV1% (p = 0.02), DLCO (p = 0.02), and FeNO (p = 0.04) [11]. In a study at the MD Anderson Cancer Center, Lopez et al. found that the correlation between the percent reduction in the DLCO and the risk of RP differed significantly between RP of grades ≤1 and ≥2 (p = 0.0004) [37]. In a study using a neural network model, the FEV1 and DLCO% were individually found to be significant risk factors for RP (p < 0.05) [18]. Our findings agreed with those of these reports, and the DLCO% was found to be a potential predictor for SARP. In the present cohort, patients with relatively lower DLCO% had a significantly higher incidence of SARP (HR: 2.762, 95% CI: 1.271–6.003, p = 0.010).
However, different studies have published conflicting reports. Findings from the study by Wang et al. indicated that poor baseline PF did not increase the risk of radiation-induced lung toxicity (RILT) [7]; on multivariate analysis, the MLD and age (≥65 years) were significantly correlated with the development of symptomatic RILT. In contrast to our study, only 50% (130/260) of their cohort received CCRT; this may have had an impact on data analysis. In a large multi-institutional study, Guckenberger et al. found that patients with better DLCO values had longer overall survival; they found no significant association between any parameter of pre-treatment PF and the risk of either grade 2 or 3 radiation pneumonitis [38]. In this cohort of 483 patients, the radiation technique used was image-guided stereotactic body radiotherapy, which differed from the conventionally fractionated radiotherapy technique used in our study. In their systematic review, Chen et al. indicated a relation between interstitial lung disease-specific toxicity and treatment-related mortality; the studied population included patients with early-stage lung cancer [39].
From a physiological perspective, the DLCO reflects the available alveolar surface area, the volume of blood present in the pulmonary capillaries, and the thickness of the alveolar capillary membrane. This parameter is helpful in the evaluation of patients with dyspnea, obstructive lung diseases, and restrictive lung diseases, with or without pulmonary parenchymal involvement; it is also useful for assessing patients with pulmonary vascular diseases. Impaired DLCO% is indicative of hypoxia [40]. Strong evidence from the experimental data indicate that hypoxia may be one of the most important driving forces that initialize and perpetuate radiation-induced pulmonary injury. In a study on rats, early changes in lung perfusion, the development of hypoxia, and chronic oxidative stress after irradiation were found to be associated with a significant increase in the activation of macrophages and the continuous production of reactive oxygen species, which stimulated the production of fibrogenic and angiogenic cytokines [41]. Another study found severe hypoxia to be associated with a significant increase in macrophage activity, collagen deposition, lung fibrosis, and levels of TGF-beta, VEGF, and CD-31 endothelial cell markers, suggestive of hypoxia-mediated activation of the pro-fibrinogenic pathways [42]. Among the PFT parameters including FEV1, DLCO has been found to be a key parameter predictive of post-radiotherapy lung function [43,44,45,46]. In a recent study [46] that prospectively analyzed patient-, dose-, and PFT-related data before and after thoracic radiation therapy, the findings suggested that the DLCO may be the most reliable indicator for lung tissue damage after thoracic radiotherapy. Therefore, the DLCO is likely to play an important role in radiation-induced lung toxicity, including RP.
Unfortunately, we failed to identify any other dosimetric or clinical factors that correlated significantly with the risk of SARP. In a study of the DVH-based parameters of the heart among patients with Hodgkin lymphoma, Cella et al. reported that the heart mass receiving >30 Gy was a predictor for the risk of RP in combination with the V5 of the left lung (Rs = 0.35, AUC = 0.78) [47]. A study from the Memorial Sloan Kettering Cancer Center found that the heart dose correlated strongly with symptomatic RP in a large cohort of patients with malignant pleural mesothelioma, where both lungs were treated with intensity-modulated pleural radiation therapy [48]. In a large cohort of patients with NSCLC, Tucker et al. reported no association between incidental heart exposure during radiotherapy and the occurrence of moderate or severe RP [49]. Although the NCCN panel recommended dose constraints for the normal heart, the results of RTOG 0617 suggested that lower radiation doses also have a negative impact on patient survival after thoracic RT, and more stringent constraints may be appropriate [50].
The present study has several limitations. First, it was retrospectively designed, and is therefore subject to bias from multiple sources. In particular, the pre-treatment PF may have been influenced by the bulky tumor (stage T3 or T4); this may have indicated bias in certain recruited patients who did not have actual moderate pulmonary dysfunction caused by other comorbidities (such as COPD, among others). In cases where the tumor progressively shrank during treatment, the pulmonary function may have improved, thereby decreasing the risk of RP. Second, the sample size was relatively small and insufficient for obtaining a definitive conclusion. Therefore, the risk factors identified from the present study should be cautiously generalized for routine use, and require validation in another independent data set. Third, among the patients with pre-treatment pulmonary dysfunction, the optimal radiation therapy schedule had not been established. All patients in this cohort had received a prescription dose of 60–66 Gy without any plan adjustments. Several studies have indicated that tumor sizes decrease significantly after the delivery of 45 Gy of fractionated radiotherapy [51, 52]. In a prospective phase II trial using a mid-treatment PET/CT-adapted radiation therapy strategy, only three (7%) patients developed grade 3 RP [53]. Therefore, re-simulation and plan modification may be employed in practice for patients with NSCLC.
The relatively high incidence of SARP in the present study requires further analysis. According to the design of this retrospective study, all patients were evaluated only if their FEV1% was in the range of 60–69%. No previously published prospective or retrospective studies have focused on this select group of patients with NSCLC. In a prospective phase III trial in China [54], RP of grade ≥3 was observed in 7.4% and 8.3% patients with NSCLC who received the EP or PC regimen, respectively. The median FEV1% in the PC group was recorded at 76.0%; this was relatively higher than the FEV1% range in the present cohort. In our opinion, pre-treatment moderate pulmonary dysfunction may explain the high incidence of SARP.
In conclusion, the DLCO% and MLD may be possible predictors of the incidence of SARP in patients with baseline moderate pulmonary dysfunction who receive definitive CCRT for NSCLC. Combining the two parameters may further improve their predictive ability. Future prospective studies are warranted to validate our findings.
References
Sause W, Kolesar P, Taylor S et al (2000) Final results of phase III trial in regionally advanced unresectable non-small cell lung cancer: Radiation Therapy Oncology Group, Eastern Cooperative Oncology Group, and Southwest Oncology Group. Chest 117:358–364. https://doi.org/10.1378/chest.117.2.358
Aupérin A, Le Péchoux C, Rolland E et al (2010) Meta-analysis of concomitant versus sequential radiochemotherapy in locally advanced non-small-cell lung cancer. J Clin Oncol 28:2181–2190. https://doi.org/10.1200/JCO.2009.26.2543
Semrau S, Bier A, Thierbach U et al (2003) Concurrent radiochemotherapy with vinorelbine plus cisplatin or carboplatin in patients with locally advanced non-small-cell lung cancer (NSCLC) and anincreased risk of treatment complications. Strahlenther Onkol 179:823–831. https://doi.org/10.1007/s00066-003-1127-8
Kong F‑M, Hayman JA, Griffith KA et al (2006) Final toxicity results of a radiation-dose escalation study in patients with non-small-cell lung cancer (NSCLC): Predictors for radiation pneumonitis and fibrosis. Int J Radiat Oncol Biol Phys 65:1075–1086. https://doi.org/10.1016/j.ijrobp.2006.01.051
Kong F‑M, Wang S (2015) Nondosimetric risk factors for radiation-induced lung toxicity. Semin Radiat Oncol 25:100–109. https://doi.org/10.1016/j.semradonc.2014.12.003
Tsujino K, Hashimoto T, Shimada T et al (2014) Combined analysis of V20, VS5, pulmonary fibrosis score on baseline computed tomography, and patient age improves prediction of severe radiation pneumonitis after concurrent chemoradiotherapy for locally advanced non-small-cell lung cancer. J Thorac Oncol 9:983–990. https://doi.org/10.1097/JTO.0000000000000187
Wang J, Cao J, Yuan S et al (2013) Poor baseline pulmonary function may not increase the risk of radiation-induced lung toxicity. Int J Radiat Oncol Biol Phys 85:798–804. https://doi.org/10.1016/j.ijrobp.2012.06.040
Palma DA, Senan S, Tsujino K et al (2013) Predicting radiation pneumonitis after chemoradiation therapy for lung cancer: an international individual patient data meta-analysis. Int J Radiat Oncol Biol Phys 85:444–450. https://doi.org/10.1016/j.ijrobp.2012.04.043
Zhang X‑J, Sun J‑G, Sun J et al (2012) Prediction of radiation pneumonitis in lung cancer patients: a systematic review. J Cancer Res Clin Oncol 138:2103–2116. https://doi.org/10.1007/s00432-012-1284-1
Shi A, Zhu G, Wu H et al (2010) Analysis of clinical and dosimetric factors associated with severe acute radiation pneumonitis in patients with locally advanced non-small cell lung cancer treated with concurrent chemotherapy and intensity-modulated radiotherapy. Radiat Oncol 5:35. https://doi.org/10.1186/1748-717X-5-35
Torre-Bouscoulet L, Muñoz-Montaño WR, Martínez-Briseño D et al (2018) Abnormal pulmonary function tests predict the development of radiation-induced pneumonitis in advanced non-small cell lung cancer. Respir Res 19:72. https://doi.org/10.1186/s12931-018-0775-2
Jin H, Tucker SL, Liu HH et al (2009) Dose-volume thresholds and smoking status for the risk of treatment-related pneumonitis in inoperable non-small cell lung cancer treated with definitive radiotherapy. Radiother Oncol 91:427–432. https://doi.org/10.1016/j.radonc.2008.09.009
Papi A, Casoni G, Caramori G et al (2004) COPD increases the risk of squamous histological subtype in smokers who develop non-small cell lung carcinoma. Thorax 59:679. https://doi.org/10.1136/thx.2003.018291
Skillrud DM, Offord KP, Miller RD (1986) Higher risk of lung cancer in chronic obstructive pulmonary disease. A prospective, matched, controlled study. Ann Intern Med 105:503–507. https://doi.org/10.7326/0003-4819-105-4-503
Vogelmeier CF, Criner GJ, Martinez FJ et al (2017) Global strategy for the diagnosis, management, and prevention of chronic obstructive lung disease 2017 report. GOLD executive summary. Am J Respir Crit Care Med 195:557–582. https://doi.org/10.1164/rccm.201701-0218PP
National Clinical Guideline C (2010) National Institute for Health and Clinical Excellence: Guidance. In: Chronic obstructive pulmonary disease: management of chronic obstructive pulmonary disease in adults in primary and secondary care. Royal College of Physicians (UK) National Clinical Guideline Centre—Acute and Chronic Conditions, London
Dehing-Oberije C, De Ruysscher D, van Baardwijk A et al (2009) The importance of patient characteristics for the prediction of radiation-induced lung toxicity. Radiother Oncol 91:421–426. https://doi.org/10.1016/j.radonc.2008.12.002
Chen S, Zhou S, Zhang J et al (2007) A neural network model to predict lung radiation-induced pneumonitis. Med Phys 34:3420–3427. https://doi.org/10.1118/1.2759601
Ferrero C, Badellino S, Filippi AR et al (2015) Pulmonary function and quality of life after VMAT-based stereotactic ablative radiotherapy for early stage inoperable NSCLC: a prospective study. Cancer Treat Res 89:350–356. https://doi.org/10.1016/j.lungcan.2015.06.019
Laszlo G (2006) Standardisation of lung function testing: helpful guidance from the ATS/ERS Task Force. Thorax 61:744–746. https://doi.org/10.1136/thx.2006.061648
Seppenwoolde Y, De Jaeger K, Boersma LJ et al (2004) Regional differences in lung radiosensitivity after radiotherapy for non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 60:748–758. https://doi.org/10.1016/j.ijrobp.2004.04.037
Hope AJ, Lindsay PE, El Naqa I et al (2006) Modeling radiation pneumonitis risk with clinical, dosimetric, and spatial parameters. Int J Radiat Oncol Biol Phys 65:112–124. https://doi.org/10.1016/j.ijrobp.2005.11.046
Morgan-Fletcher SL (2001) Prescribing, Recording and Reporting Photon Beam Therapy (Supplement to ICRU Report 50), ICRU Report 62. ICRU, pp. ix+52, 1999 (ICRU Bethesda, MD) $65.00 ISBN 0‑913394-61‑0. Brit J Radiol 74:294–294. https://doi.org/10.1259/bjr.74.879.740294
Hodapp N (2012) The ICRU Report 83: prescribing, recording and reporting photon-beam intensity-modulated radiation therapy (IMRT). Strahlenther Onkol 188:97–99. https://doi.org/10.1007/s00066-011-0015-x
Jiang X, Li T, Liu Y et al (2011) Planning analysis for locally advanced lung cancer: dosimetric and efficiency comparisons between intensity-modulated radiotherapy (IMRT), single-arc/partial-arc volumetric modulated arc therapy (SA/PA-VMAT). Radiat Oncol 6:140. https://doi.org/10.1186/1748-717x-6-140
Xiao J, Zhang H, Gong Y et al (2010) Feasibility of using intravenous contrast-enhanced computed tomography (CT) scans in lung cancer treatment planning. Radiother Oncol 96:73–77. https://doi.org/10.1016/j.radonc.2010.02.029
Ettinger DS, Wood DE, Aisner DL et al (2017) Non-small cell lung cancer, version 5.2017, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw 15:504–535. https://doi.org/10.6004/jnccn.2017.0050
National Cancer Institute (2010) Common terminology criteria for adverse events (CTCAE) version 4.03. https://evs.nci.nih.gov/ftp1/CTCAE/CTCAE_4.03/CTCAE_4.03_2010-06-14_QuickReference_8.5x11.pdf. Accessed 14 June 2010
Martel MK, Ten Haken RK, Hazuka MB et al (1994) Dose-volume histogram and 3‑D treatment planning evaluation of patients with pneumonitis. Int J Radiat Oncol Biol Phys 28:575–581. https://doi.org/10.1016/0360-3016(94)90181-3
Graham MV, Purdy JA, Emami B et al (1999) Clinical dose-volume histogram analysis for pneumonitis after 3D treatment for non-small cell lung cancer (NSCLC). Int J Radiat Oncol Biol Phys 45:323–329. https://doi.org/10.1016/s0360-3016(99)00183-2
Hernando ML, Marks LB, Bentel GC et al (2001) Radiation-induced pulmonary toxicity: a dose-volume histogram analysis in 201 patients with lung cancer. Int J Radiat Oncol Biol Phys 51:650–659. https://doi.org/10.1016/s0360-3016(01)01685-6
Claude L, Perol D, Ginestet C et al (2004) A prospective study on radiation pneumonitis following conformal radiation therapy in non-small-cell lung cancer: clinical and dosimetric factors analysis. Radiother Oncol 71:175–181. https://doi.org/10.1016/j.radonc.2004.02.005
Rancati T, Ceresoli GL, Gagliardi G et al (2003) Factors predicting radiation pneumonitis in lung cancer patients: a retrospective study. Radiother Oncol 67:275–283. https://doi.org/10.1016/s0167-8140(03)00119-1
Fay M, Tan A, Fisher R et al (2005) Dose-volume histogram analysis as predictor of radiation pneumonitis in primary lung cancer patients treated with radiotherapy. Int J Radiat Oncol Biol Phys 61:1355–1363. https://doi.org/10.1016/j.ijrobp.2004.08.025
Lee HJ Jr., Zeng J, Vesselle HJ et al (2018) Correlation of functional lung heterogeneity and dosimetry to radiation pneumonitis using perfusion SPECT/CT and FDG PET/CT imaging. Int J Radiat Oncol Biol Phys 102:1255–1264. https://doi.org/10.1016/j.ijrobp.2018.05.051
Videtic GM, Stitt LW, Ash RB et al (2004) Impaired diffusion capacity predicts for decreased treatment tolerance and survival in limited stage small cell lung cancer patients treated with concurrent chemoradiation. Cancer Treat Res 43:159–166. https://doi.org/10.1016/j.lungcan.2003.08.026
Lopez Guerra JL, Gomez D, Zhuang Y et al (2012) Change in diffusing capacity after radiation as an objective measure for grading radiation pneumonitis in patients treated for non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 83:1573–1579. https://doi.org/10.1016/j.ijrobp.2011.10.065
Guckenberger M, Kestin LL, Hope AJ et al (2012) Is there a lower limit of pretreatment pulmonary function for safe and effective stereotactic body radiotherapy for early-stage non-small cell lung cancer? J Thorac Oncol 7:542–551. https://doi.org/10.1097/JTO.0b013e31824165d7
Chen H, Senan S, Nossent EJ et al (2017) Treatment-related toxicity in patients with early-stage non-small cell lung cancer and coexisting interstitial lung disease: a systematic review. Int J Radiat Oncol Biol Phys 98:622–631. https://doi.org/10.1016/j.ijrobp.2017.03.010
Plummer AL (2008) The carbon monoxide diffusing capacity: clinical implications, coding, and documentation. Chest 134:663–667. https://doi.org/10.1378/chest.07-1771
Fleckenstein K, Zgonjanin L, Chen L et al (2007) Temporal onset of hypoxia and oxidative stress after pulmonary irradiation. Int J Radiat Oncol Biol Phys 68:196–204. https://doi.org/10.1016/j.ijrobp.2006.12.056
Vujaskovic Z, Anscher MS, Feng QF et al (2001) Radiation-induced hypoxia may perpetuate late normal tissue injury. Int J Radiat Oncol Biol Phys 50:851–855. https://doi.org/10.1016/s0360-3016(01)01593-0
Lopez Guerra JL, Gomez DR, Zhuang Y et al (2012) Changes in pulmonary function after three-dimensional conformal radiotherapy, intensity-modulated radiotherapy, or proton beam therapy for non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 83:e537–543. https://doi.org/10.1016/j.ijrobp.2012.01.019
Stanic S, Paulus R, Timmerman RD et al (2014) No clinically significant changes in pulmonary function following stereotactic body radiation therapy for early- stage peripheral non-small cell lung cancer: an analysis of RTOG 0236. Int J Radiat Oncol Biol Phys 88:1092–1099. https://doi.org/10.1016/j.ijrobp.2013.12.050
Guckenberger M, Klement RJ, Kestin LL et al (2013) Lack of a dose-effect relationship for pulmonary function changes after stereotactic body radiation therapy for early-stage non-small cell lung cancer. Int J Radiat Oncol Biol Phys 85:1074–1081. https://doi.org/10.1016/j.ijrobp.2012.09.016
Schroder C, Engenhart-Cabillic R, Vorwerk H et al (2017) Changes in pulmonary function and influencing factors after high-dose intrathoracic radio(chemo)therapy. Strahlenther Onkol 193:125–131. https://doi.org/10.1007/s00066-016-1067-8
Cella L, D’Avino V, Palma G et al (2015) Modeling the risk of radiation-induced lung fibrosis: Irradiated heart tissue is as important as irradiated lung. Radiother Oncol 117:36–43. https://doi.org/10.1016/j.radonc.2015.07.051
Yorke ED, Jackson A, Kuo LC et al (2017) Heart dosimetry is correlated with risk of radiation pneumonitis after lung-sparing hemithoracic pleural intensity modulated radiation therapy for malignant pleural mesothelioma. Int J Radiat Oncol Biol Phys 99:61–69. https://doi.org/10.1016/j.ijrobp.2017.04.025
Tucker SL, Liao Z, Dinh J et al (2014) Is there an impact of heart exposure on the incidence of radiation pneumonitis? Analysis of data from a large clinical cohort. Acta Oncol 53:590–596. https://doi.org/10.3109/0284186x.2013.831185
Bradley JD, Paulus R, Komaki R et al (2015) Standard-dose versus high-dose conformal radiotherapy with concurrent and consolidation carboplatin plus paclitaxel with or without cetuximab for patients with stage IIIA or IIIB non-small-cell lung cancer (RTOG 0617): a randomised, two-by-two factorial phase 3 study. Lancet Oncol 16:187–199. https://doi.org/10.1016/s1470-2045(14)71207-0
Kong FM, Frey KA, Quint LE et al (2007) A pilot study of [18F] fluorodeoxyglucose positron emission tomography scans during and after radiation-based therapy in patients with non small-cell lung cancer. J Clin Oncol 25:3116–3123. https://doi.org/10.1200/jco.2006.10.3747
Mahasittiwat P, Yuan S, Xie C et al (2013) metabolic tumor volume on PET reduced more than gross tumor volume on ct during radiotherapy in patients with non-small cell lung cancer treated with 3DCRT or SBRT. J Radiat Oncol 2:191–202. https://doi.org/10.1007/s13566-013-0091-x
Kong FM, Ten Haken RK, Schipper M et al (2017) Effect of midtreatment PET/CT-adapted radiation therapy with concurrent chemotherapy in patients with locally advanced non-small-cell lung cancer: a phase 2 clinical trial. JAMA Oncol 3:1358–1365. https://doi.org/10.1001/jamaoncol.2017.0982
Liang J, Bi N, Wu S et al (2017) Etoposide and cisplatin versus paclitaxel and carboplatin with concurrent thoracic radiotherapy in unresectable stage III non-small cell lung cancer: a multicenter randomized phase III trial. Ann Oncol 28:777–783. https://doi.org/10.1093/annonc/mdx009
Funding
This project was supported by a grant from Sichuan Provincial Science and Technology Funding to Youling Gong (2018SZ0184). This work has been selected to be presented partly in digital poster form at the American Society for Radiation Oncology Annual Meeting, 2019.
Author information
Authors and Affiliations
Contributions
Youling Gong conceived and designed the study. Yin Zhou, Tiansheng Yan, Xiaojuan Zhou, Peng Cao, Chunli Luo, and Youling Gong collected the data. Yin Zhou, Tiansheng Yan, and Youling Gong analyzed and interpreted the data and drafted the article. Lin Zhou, Yong Xu, Yongmei Liu, Jianxin Xue, Jin Wang, Yongsheng Wang, You Lu, and Binmiao Liang critically revised the paper. All of the authors approved the final submitted version.
Corresponding author
Ethics declarations
Conflict of interest
Y. Zhou, T. Yan, X. Zhou, P. Cao, C. Luo, L. Zhou, Y. Xu, Y. Liu, J. Xue, J. Wang, Y. Wang, Y. Lu, B. Liang, and Y. Gong declare that they have no competing interests.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee (West China Hospital of Sichuan University Biomedical Research Ethics Committee) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
The authors Ying Zhou and Tiansheng Yan contributed equally to the manuscript.
Rights and permissions
About this article
Cite this article
Zhou, Y., Yan, T., Zhou, X. et al. Acute severe radiation pneumonitis among non-small cell lung cancer (NSCLC) patients with moderate pulmonary dysfunction receiving definitive concurrent chemoradiotherapy: Impact of pre-treatment pulmonary function parameters. Strahlenther Onkol 196, 505–514 (2020). https://doi.org/10.1007/s00066-019-01552-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-019-01552-4