Background and Purpose:
Transoral laser microsurgery (TLM) and adjuvant radiotherapy are an established therapy regimen for locally advanced laryngeal cancer at our institution. Aim of the present study was to assess value of quality of life (QoL) data with special regard to organ function under consideration of treatment efficacy in patients with locally advanced laryngeal cancer treated with larynx-preserving TLM and adjuvant radiotherapy.
Patients and Methods:
From 1994 to 2006, 39 patients (ten UICC stage III, 29 UICC stage IVA/B) with locally advanced laryngeal carcinomas were treated with TLM and adjuvant radiotherapy. Data concerning treatment efficacy, QoL (using the VHI [Voice Handicap Index], the EORTC QLQ-C30 and QLQ-H&N35 questionnaires) and organ function (respiration, deglutition, voice quality) were obtained for ten patients still alive after long-term follow-up. Correlations were determined using the Spearman rank test.
Results:
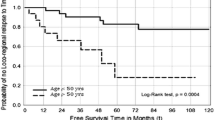
After a median follow-up of 80.8 months, the 5-year overall survival rate was 46.8% and the locoregional control rate 76.5%, respectively. The larynx preservation rate was 89.7% for all patients and 100% for patients still alive after follow-up. Despite some verifiable problems in respiration, speech and swallowing, patients showed a subjectively good QoL.
Conclusion:
TLM and adjuvant radiotherapy is a curative option for patients with locally advanced laryngeal cancer and an alternative to radical surgery. Even if functional deficits are unavoidable in the treatment of locally advanced laryngeal carcinomas, larynx preservation is associated with a subjectively good QoL.
Hintergrund und Ziel:
Lasermikrochirurgie und adjuvante Strahlentherapie sind in der Klinik der Autoren etablierte Behandlungsmethoden lokal fortgeschrittener Larynxkarzinome mit guten onkologischen Ergebnissen und einer hohe Rate an Organerhalt. Bei organerhaltender Therapie sind funktionelle Einschränkungen oft unvermeidbar. Neben den onkologischen Ergebnissen sollten in dieser Studie das objektive Ausmaß solcher Einschränkungen und deren subjektive Wertung durch die Patienten untersucht werden.
Patienten und Methodik:
Von 1994 bis 2006 wurden 39 Patienten (zehn UICC-Stadium III, 29 UICC-Stadium IVA/B) mit lokal fortgeschrittenen Larynxkarzinomen mittels Lasermikrochirurgie und adjuvanter Strahlentherapie behandelt. Bei zehn Patienten erfolgte im Rahmen der Nachsorge in den Jahren 2006/2007 eine Erhebung von Lebensqualitätsdaten. Die Schluckfunktion wurde flexibel endoskopisch überprüft, die Atmung durch eine Bodyplethysmographie. Die Objektivierung der Stimmqualität erfolgte durch das Göttinger Heiserkeitsdiagramm.
Ergebnisse:
Nach einer medianen Beobachtungsdauer von 80,8 Monaten betrugen die 5-Jahres-Überlebensrate 46,8% und die lokoregionale Kontrollrate 76,5%. Eine Salvage-Laryngektomie bei Lokalrezidiv erhielten vier Patienten, so dass im Verlauf eine 89,7%ige Rate an Larynxerhalt erreicht werden konnte. Bei der objektiven Untersuchung der Funktionseinschränkungen zeigte sich bei fünf Patienten eine gelegentliche Aspiration bei kräftigem Hustenreflex. Die übrigen fünf Patienten wiesen keine Schluckstörung auf. Eine Normalstimme lag bei keinem Patienten vor. Es bestand jedoch keine signifikante Korrelation der objektivierten Funktionsstörungen mit den Lebensqualitätsfunktionsskalen: Subjektiv schätzen die Patienten ihre Lebensqualität als gut ein.
Schlussfolgerung:
Lasermikrochirurgie und adjuvante Strahlentherapie sind eine Therapieoption für lokal fortgeschrittene Larynxkarzinome, die neben guten onkologischen Ergebnissen eine hohe Rate an Organerhalt ermöglicht. Die Patienten schätzen ihre Lebensqualität im weiteren Verlauf subjektiv als gut ein. Die tatsächlichen funktionellen Einschränkungen werden durch die Lebensqualitätsdaten allerdings nicht sicher abgebildet. Daher ist zur objektiven Beurteilung posttherapeutischer Funktionsergebnisse die klinische Erhebung funktioneller Befunde erforderlich.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Adelstein DJ, Lavertu P, Saxton JP, et al. Mature results of a phase III randomized trial comparing concurrent chemoradiotherapy with radiation therapy alone in patients with stage III and IV squamous cell carcinoma of the head and neck. Cancer 2000;88:876–83.
Adelstein DJ, Saxton JP, Lavertu P, et al. A phase III randomized trial comparing concurrent chemotherapy and radiotherapy with radiotherapy alone in resectable stage III and IV squamous cell head and neck cancer: preliminary results. Head Neck 1997;19:567–75.
Ambrosch P. The role of laser microsurgery in the treatment of laryngeal cancer. Curr Opin Otolaryngol Head Neck Surg 2007;15:82–8.
Amdur RJ, Parsons JT, Mendenhall WM, et al. Postoperative irradiation for squamous cell carcinoma of the head and neck: an analysis of treatment results and complications. Int J Radiat Oncol Biol Phys 1989;16:25–36.
Amdur RJ, Parsons JT, Mendenhall WM, et al. Split-course versus continuous-course irradiation in the postoperative setting for squamous cell carcinoma of the head and neck. Int J Radiat Oncol Biol Phys 1989;17: 279–85.
Bachaud JM, Cohen-Jonathan E, Alzieu C, et al. Combined postoperative radiotherapy and weekly cisplatin infusion for locally advanced head and neck carcinoma: final report of a randomized trial. Int J Radiat Oncol Biol Phys 1996;36:999–1004.
Bernier J, Cooper JS. Chemoradiation after surgery for high-risk head and neck cancer patients: how strong is the evidence? Oncologist 2005;10: 215–24.
Bernier J, Domenge C, Ozsahin M, et al. Postoperative irradiation with or without concomitant chemotherapy for locally advanced head and neck cancer. N Engl J Med 2004;350:1945–52.
Bray F, Sankila R, Ferlay J, et al. Estimates of cancer incidence and mortality in Europe in 1995. Eur J Cancer 2002;38:99–166.
Christiansen H, Hermann RM, Martin A, et al. Long-term follow-up after transoral laser microsurgery and adjuvant radiotherapy for advanced recurrent squamous cell carcinoma of the head and neck. Int J Radiat Oncol Biol Phys 2006;65:1067–74.
Christiansen H, Hess CF. Comment on Studer G, et al. Locoregional failure analysis in head-and-neck cancer patients treated with IMRT, in Strahlenther Onkol 2007;183:417–23. Strahlenther Onkol 2007;183:424-5.
Cooper JS, Pajak TF, Forastiere AA, et al. Postoperative concurrent radiotherapy and chemotherapy for high-risk squamous-cell carcinoma of the head and neck. N Engl J Med 2004;350:1937–44.
Department of Veterans’ Affairs Laryngeal Cancer Study Group. Induction chemotherapy plus radiation compared with surgery plus radiation in patients with advanced laryngeal cancer. The Department of Veterans’ Affairs Laryngeal Cancer Study Group. N Engl J Med 1991;324:1685–90.
Eich HT, Löschcke M, Scheer M, et al. Neoadjuvant radiochemotherapy and radical resection for advanced squamous cell carcinoma of the oral cavity. Outcome of 134 patients. Strahlenther Onkol 2008;184:23–9.
Forastiere AA, Goepfert H, Maor M, et al. Concurrent chemotherapy and radiotherapy for organ preservation in advanced laryngeal cancer. N Engl J Med 2003;349:2091–8.
Fortin A, Allard J, Albert M, et al. Outcome of patients treated with cobalt and 6 MV in head and neck cancers. Head Neck 2001;23:181–8.
Fröhlich M, Michaelis D, Strube HW, et al. Acoustic voice analysis by means of the hoarseness diagram. J Speech Lang Hear Res 2000;43:706–20.
International Commission on Radiation Units and Measurements. ICRU report 50: prescribing, recording, and reporting photon beam therapy. Washington: International Commission on Radiation Units and Measurements; 1993.
Kaplan E, Meier P. Nonparametric estimation from incomplete observations. J Am Stat Assoc 1958;58:457–81.
Kennedy JT, Paddle PM, Cook BJ, et al. Voice outcomes following transoral lasermicrosurgery for early glottic squamous cell carcinoma. J Laryngol Otol 2007;20:1–5.
Kessler P, Grabenbauer G, Leher A, et al. Five year survival of patients with primary oral squamous cell carcinoma. Comparison of two treatment protocols in a prospective study. Strahlenther Onkol 2007;183:184–9.
Lefebvre JL, Chevalier D, Luboinski B, et al. Larynx preservation in pyriform sinus cancer: preliminary results of a European Organization for Research and Treatment of Cancer phase III trial. EORTC Head and Neck Cancer Cooperative Group. J Natl Cancer Inst 1996;88:890–9.
Nawka T, Wiesmann U, Gonnermann U. Validation of the German version of the Voice Handicap Index. HNO 2003;51:921–30.
Olthoff A, Mrugalla S, Laskawi R, et al. Assessment of irregular voices after total and laser surgical laryngectomy. Arch Otolaryngol Head Neck Surg 2003;129:994–9.
Olthoff A, Steuer-Vogt MK, Licht K, et al. Quality of life after treatment for laryngeal carcinomas. ORL J Otorhinolaryngol Relat Spec 2006;68:253–8.
Olthoff A, Zeiss D, Laskawi R, et al. Laser microsurgical bilateral posterior cordectomy for the treatment of bilateral vocal fold paralysis. Ann Otol Rhinol Laryngol 2005;114:599–604.
Parkin DM, Bray F, Ferlay J, et al. Global cancer statistics, 2002. CA Cancer J Clin 2005; 55:74–108.
Parsons JT, Mendenhall WM, Stringer SP, et al. An analysis of factors influencing the outcome of postoperative irradiation for squamous cell carcinoma of the oral cavity. Int J Radiat Oncol Biol Phys 1997;39:137–48.
Peters LJ, Goepfert H, Ang KK, et al. Evaluation of the dose for postoperative radiation therapy of head and neck cancer: first report of a prospective randomized trial. Int J Radiat Oncol Biol Phys 1993;26:3–11.
Pradier O, Christiansen H, Schmidberger H, et al. Adjuvant radiotherapy after transoral microlasersurgery for advanced squamous cell carcinoma of the head and neck. Int J Radiat Oncol Biol Phys 2005;63:1368–77.
Rades D, Stoehr M, Meyners T, et al. Evaluation of prognostic factors and two radiation techniques in patients treated with surgery followed by radio(chemo)therapy or definitive radio(chemo)therapy for locally advanced head-and-neck cancer. Strahlenther Onkol 2008;184:198–205.
Regine WF, Valentino J, Sloan DA, et al. Postoperative radiation therapy for primary vs. recurrent squamous cell carcinoma of the head and neck: results of a comparative analysis. Head Neck 1999;21:554–9.
Richard JM, Sancho-Garnier H, Pessey JJ, et al. Randomized trial of induction chemotherapy in larynx carcinoma. Oral Oncol 1998;34:224–8.
Schröter-Morasch H. Klinische Untersuchung des Oropharynx und videoendoskopische Untersuchung der Schluckfunktion. In: Bartolome G., Schröter-Morasch H., Hrsg. Schluckstörungen, Diagnostik und Rehabilitation, 2 Aufl. München-Jena: Urban & Fischer, 1999:132.
Sobin LH, Wittekind C. TNM classification of malignant tumours. New York Toronto: Wiley-Liss, 6th edition 2002.
Steiner W, Ambrosch P. Endoscopic laser surgery of the upper aerodigestive tract. With special emphasis on cancer surgery. Stuttgart-New York: Thieme, 2000.
Studer G, Luetolf UM, Glanzmann C. Locoregional failure analysis in head-and-neck cancer patients treated with IMRT. Strahlenther Onkol 2007;183:417–23, discussion 424-5.
Trotti A, Colevas AD, Setser A, et al. CTCAE v3.0: development of a comprehensive grading system for the adverse effects of cancer treatment. Semin Radiat Oncol 2003;13:176–81.
Tupchong L, Scott CB, Blitzer PH, et al. Randomized study of preoperative versus postoperative radiation therapy in advanced head and neck carcinoma: long-term follow-up of RTOG study 73-03. Int J Radiat Oncol Biol Phys 1991;20:21–8.
Author information
Authors and Affiliations
Corresponding author
Additional information
The study results were reported as oral presentation at the 2008 DEGRO (German Society of Radiooncology) Annual Meeting in Vienna, Austria.
Olivier Pradier and Hans Christiansen share senior authorship.
Rights and permissions
About this article
Cite this article
Olthoff, A., Ewen, A., Wolff, H.A. et al. Organ Function and Quality of Life after Transoral Laser Microsurgery and Adjuvant Radiotherapy for Locally Advanced Laryngeal Cancer. Strahlenther Onkol 185, 303–309 (2009). https://doi.org/10.1007/s00066-009-1967-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-009-1967-y